Abstract
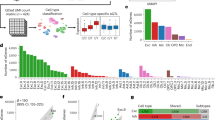
BRAT1 biallelic variants are associated with rigidity and multifocal seizure syndrome, lethal neonatal (RMFSL), and neurodevelopmental disorder associating cerebellar atrophy with or without seizures syndrome (NEDCAS). To date, forty individuals have been reported in the literature. We collected clinical and molecular data from 57 additional cases allowing us to study a large cohort of 97 individuals and draw phenotype-genotype correlations. Fifty-nine individuals presented with BRAT1-related RMFSL phenotype. Most of them had no psychomotor acquisition (100%), epilepsy (100%), microcephaly (91%), limb rigidity (93%), and died prematurely (93%). Thirty-eight individuals presented a non-lethal phenotype of BRAT1-related NEDCAS phenotype. Seventy-six percent of the patients in this group were able to walk and 68% were able to say at least a few words. Most of them had cerebellar ataxia (82%), axial hypotonia (79%) and cerebellar atrophy (100%). Genotype-phenotype correlations in our cohort revealed that biallelic nonsense, frameshift or inframe deletion/insertion variants result in the severe BRAT1-related RMFSL phenotype (46/46; 100%). In contrast, genotypes with at least one missense were more likely associated with NEDCAS (28/34; 82%). The phenotype of patients carrying splice variants was variable: 41% presented with RMFSL (7/17) and 59% with NEDCAS (10/17).
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Data availability
The datasets generated and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Aglipay JA, Martin SA, Tawara H, Lee SW, Ouchi T. ATM activation by ionizing radiation requires BRCA1-associated BAAT1. J Biol Chem. 2006;281:9710–8.
Ouchi M, Ouchi T. Regulation of ATM/DNA-PKcs phosphorylation by BRCA1-associated BAAT1. Genes Cancer. 2010;1:1211–4.
So EY, Ouchi T. The potential role of BRCA1-associated ATM activator-1 (BRAT1) in regulation of mTOR. J Cancer Biol Res. 2013;1:1001.
So EY, Ouchi T. BRAT1 deficiency causes increased glucose metabolism and mitochondrial malfunction. BMC Cancer. 2014;14:548.
Puffenberger EG, Jinks RN, Sougnez C, Cibulskis K, Willert RA, Achilly NP, et al. Genetic mapping and exome sequencing identify variants associated with five novel diseases. PLoS ONE. 2012;7:e28936.
Hanes I, Kozenko M, Callen DJA. Lethal neonatal rigidity and multifocal seizure syndrome—a misnamed disorder? Pediatr Neurol. 2015;53:535–40.
Valence S, Cochet E, Rougeot C, Garel C, Chantot-Bastaraud S, Lainey E, et al. Exome sequencing in congenital ataxia identifies two new candidate genes and highlights a pathophysiological link between some congenital ataxias and early infantile epileptic encephalopathies. Genet Med. 2019;21:553–63.
Colak FK, Guleray N, Azapagasi E, Yazıcı MU, Aksoy E, Ceylan N. An intronic variant in BRAT1 creates a cryptic splice site, causing epileptic encephalopathy without prominent rigidity. Acta Neurol Belg. 2020;120:1425–32.
Saunders CJ, Miller NA, Soden SE, Dinwiddie DL, Noll A, Alnadi NA, et al. Rapid whole-genome sequencing for genetic disease diagnosis in neonatal intensive care units. Sci Transl Med. 2012;4:154ra135.
Saitsu H, Yamashita S, Tanaka Y, Tsurusaki Y, Nakashima M, Miyake N, et al. Compound heterozygous BRAT1 mutations cause familial Ohtahara syndrome with hypertonia and microcephaly. J Hum Genet. 2014;59:687–90.
Straussberg R, Ganelin-Cohen E, Goldberg-Stern H, Tzur S, Behar DM, Smirin-Yosef P, et al. Lethal neonatal rigidity and multifocal seizure syndrome – report of another family with a BRAT1 mutation. Eur J Paediatr Neurol. 2015;19:240–2.
van de Pol LA, Wolf NI, van Weissenbruch MM, Stam CJ, Weiss JM, Waisfisz Q, et al. Early-onset severe encephalopathy with epilepsy: the BRAT1 gene should be added to the list of causes. Neuropediatrics. 2015;46:392–400.
Fernández-Jáen A, Álvarez S, So EY, Ouchi T, de la Peña MJ, Duat A, et al. Mutations in BRAT1 cause autosomal recessive progressive encephalopathy: report of a Spanish patient. Eur J Paediatr Neurol. 2016;20:421–5.
Horn D, Weschke B, Knierim E, Fischer‐Zirnsak B, Stenzel W, Schuelke M, et al. BRAT1 mutations are associated with infantile epileptic encephalopathy, mitochondrial dysfunction, and survival into childhood. Am J Med Genet A. 2016;170:2274–81.
Mundy SA, Krock BL, Mao R, Shen JJ. BRAT1-related disease—identification of a patient without early lethality. Am J Med Genet A. 2016;170:699–702.
Smith NJ, Lipsett J, Dibbens LM, Heron SE. BRAT1-associated neurodegeneration: intra-familial phenotypic differences in siblings. Am J Med Genet A. 2016;170:3033–8.
Srivastava S, Olson HE, Cohen JS, Gubbels CS, Lincoln S, Davis BT, et al. BRAT1 mutations present with a spectrum of clinical severity. Am J Med Genet A. 2016;170:2265–73.
Srivastava S, Naidu S. Epileptic encephalopathy due to BRAT1 pathogenic variants. Pediatr Neurol Briefs. 2016;30:45.
Celik Y, Okuyaz C, Arslankoylu AE, Ceylaner S. Lethal neonatal rigidity and multifocal seizure syndrome with a new mutation in BRAT1. Epilepsy Behav Case Rep. 25 mai. 2017;8:2.
Oatts JT, Duncan JL, Hoyt CS, Slavotinek AM, Moore AT. Inner retinal dystrophy in a patient with biallelic sequence variants in BRAT1. Ophthalmic Genet. 2017;38:559–61.
Van Ommeren RH, Gao AF, Blaser SI, Chitayat DA, Hazrati LN. BRAT1 mutation: the first reported case of Chinese origin and review of the literature. J Neuropathol Exp Neurol. 2018;77:1071–8.
Szymańska K, Laure-Kamionowska M, Szczałuba K, Koppolu A, Furmanek M, Kuśmierska K, et al. Clinico-pathological correlation in case of BRAT1 mutation. Folia Neuropathol. 2018;56:362–71.
Mahjoub A, Cihlarova Z, Tétreault M, MacNeil L, Sondheimer N, Caldecott KW, et al. Homozygous pathogenic variant in BRAT1 associated with nonprogressive cerebellar ataxia. Neurol Genet. 2019;5:e359.
Scheffer IE, Boysen KE, Schneider AL, Myers CT, Mehaffey MG, Rochtus AM, et al. BRAT1 encephalopathy: a recessive cause of epilepsy of infancy with migrating focal seizures. Dev Med Child Neurol. 2020;62:1096–9.
Burgess R, Wang S, McTague A, Boysen KE, Yang X, Zeng Q, et al. The genetic landscape of epilepsy of infancy with migrating focal seizures. Ann Neurol. 2019;86:821–31.
Pourahmadiyan A, Heidari M, Ardakani HS, Noorian S, Savad S. A novel pathogenic variant of BRAT1 gene causes rigidity and multifocal seizure syndrome, lethal neonatal. Int J Neurosci. 2021;131:875–8.
Skafi O, Fawaz F, Merhi B, Jouni H, MMansour S, Harb R, et al. Rigidity with multifocal seizure syndrome, lethal neonatal in a lebanese neonate. A rare case report. J Pediatr Disord Neonatal Care. 2018;1:106.
Li W, Wu S, Xu H, Zhao X, Pan Y, Huang H, et al. Novel variant in BRAT1 with the lethal neonatal rigidity and multifocal seizure syndrome. Pediatr Res. 2021;1:7.
Balasundaram P, Fijas M, Nafday S. A rare case of lethal neonatal rigidity and multi-focal seizure syndrome. Cureus. 2021;13:e13600.
Sobreira N, Schiettecatte F, Valle D, Hamosh A. GeneMatcher: a matching tool for connecting investigators with an interest in the same gene. Hum Mutat. 2015;36:928–30.
Nuovo S, Baglioni V, De Mori R, Tardivo S, Caputi C, Ginevrino M, et al. Clinical variability at the mild end of BRAT1-related spectrum: evidence from two families with genotype-phenotype discordance. Hum Mutat. 2022;43:67–73.
Cornet MC, Morabito V, Lederer D, Glass HC, Santos SF, Numis AL, et al. Neonatal presentation of genetic epilepsies: early differentiation from acute provoked seizures. Epilepsia. 2021;62:1907–20.
Low LH, Chow YL, Li Y, Goh CP, Putz U, Silke J, et al. Nedd4 family interacting protein 1 (Ndfip1) is required for ubiquitination and nuclear trafficking of BRCA1-associated ATM activator 1 (BRAT1) during the DNA damage response. J Biol Chem. 2015;290:7141–50.
Smith ED, Blanco K, Sajan SA, Hunter JM, Shinde DN, Wayburn B, et al. A retrospective review of multiple findings in diagnostic exome sequencing: half are distinct and half are overlapping diagnoses. Genet Med. 2019;21:2199–207.
AlAbdi L, Alrashseed S, Alsulaiman A, Helaby R, Imtiaz F, Alhamed M, et al. Residual risk for additional recessive diseases in consanguineous couples. Genet Med Off J Am Coll Med Genet. 2021;23:2448–54.
Bunod R, Doummar D, Whalen S, Keren B, Chantot-Bastaraud S, Maincent K, et al. Congenital immobility and stiffness related to biallelic ATAD1 variants. Neurol Genet. 2020;6:e520.
Martin S, Chamberlin A, Shinde DN, Hempel M, Strom TM, Schreiber A, et al. De novo variants in GRIA4 lead to intellectual disability with or without seizures and gait abnormalities. Am J Hum Genet. 2017;101:1013–20.
Chong JX, McMillin MJ, Shively KM, Beck AE, Marvin CT, Armenteros JR, et al. De novo mutations in NALCN cause a syndrome characterized by congenital contractures of the limbs and face, hypotonia, and developmental delay. Am J Hum Genet. 2015;96:462–73.
Patak J, Gilfert J, Byler M, Neerukonda V, Thiffault I, Cross L, et al. MAGEL2-related disorders: a study and case series. Clin Genet. 2019;96:493–505.
Aldaz CM, Hussain T. WWOX loss of function in neurodevelopmental and neurodegenerative disorders. Int J Mol Sci. 2020;21:8922.
Piard J, Hawkes L, Milh M, Villard L, Borgatti R, Romaniello R, et al. The phenotypic spectrum of WWOX-related disorders: 20 additional cases of WOREE syndrome and review of the literature. Genet Med. 2019;21:1308–18.
Gatti M, Magri S, Nanetti L, Sarto E, Bella DD, Salsano E, et al. From congenital microcephaly to adult onset cerebellar ataxia: distinct and overlapping phenotypes in patients with PNKP gene mutations. Am J Med Genet A. 2019;179:2277–83.
Riso V, Galatolo D, Barghigiani M, Galosi S, Tessa A, Ricca I, et al. A NGS-based analysis on a large cohort of ataxic patients refines the clinical spectrum associated with SCA21. Eur J Neurol. 2021;28:2784–8.
Acknowledgements
The authors would like to thank the families for their participation in this study. Funding: SS received funding from National Institute of Health/National Institute of Neurological Disorders and Stroke (NIH/NINDS) (K23NS119666). FSA acknowledges the support of King Salman Center for Disability Research through Research Group no RG-2022-011.
Author information
Authors and Affiliations
Contributions
CE, SV, GD, RM collected clinical and molecular data. CE, JP analyzed and interpreted data and wrote the manuscript. JP, LVM designed the study. SV, RM, AA, EA, FSA, VB, IB, MB-L, EB, IB, EB-B, A-LB, AB, DKB, CC, MRC, M-CC, CC, OD, VD, A-SD-P, MCDG, MD-F, HE, KC, MG, JGG, DH, JG, AG, FLH, HH, MI, RK, BK, EGK, DK, PK, KK, DL, LM, CM, DM-R, LN, SO, CO, JNP, LP, LP, CP, GP, CP, AP, MR, CR, VS, IS, AS, SS, RS, PS, EMV, PV, LV, AV, JW, MW, MSZ, FZ, GL, VRY, MM, FH-G, MB, FA, HG, CW, AN, MT, DS, YM, KK, CS, VC, MZ, LVM, LB characterized the clinical and molecular features of the disease. All the authors edited or commented the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
Individuals were referred by clinical geneticists for genetic testing as part of routine clinical care. All patients enrolled and/or their legal representative have signed informed consent for use of data and/or photographs. This study has been performed in accordance with the Declaration of Helsinki.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Engel, C., Valence, S., Delplancq, G. et al. BRAT1–related disorders: phenotypic spectrum and phenotype-genotype correlations from 97 patients. Eur J Hum Genet 31, 1023–1031 (2023). https://doi.org/10.1038/s41431-023-01410-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41431-023-01410-z
This article is cited by
-
Why donât we all use genomic testing?
European Journal of Human Genetics (2023)