Abstract
Background
The arguments about whether intermittent or continuous tube feeding was preferred in patients with hemorrhagic stroke exist yet. This study aimed to examine the effects of intermittent versus continuous tube feeding on its intolerance performance and efficiency of calorie intake.
Method
A convenience sample was selected from January 2018 to January 2019 in the Neurosurgery Department of West China Hospital, Sichuan Province. The participants were randomly allocated to either intermittent or continuous tube feeding group, fed four times or 24 h a day using electric feeding pump, respectively. The incidence of the intolerance and calorie intake were recorded and analyzed.
Results
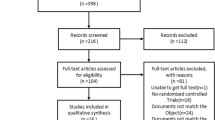
78 patients took part in this study: 40 in the intermittent group and 38 in the continuous group. The incidence of the diarrhea was significantly lower in the continuous group (7.9 vs 37.5%, p = 0.002). The total intolerance rate was significantly lower in the continuous group compared with the intermittent group (63.2 vs 85.0%, p = 0.027). There was no significant difference in calorie intake between the intermittent and continuous group during the first 3 days (2595.4 ± 394.5 kcal vs 2317.8 ± 645.1 kcal, p = 0.099). No significant difference in total calorie intake was found between two groups (6265.6 ± 1261.3 kcal vs 6429.4 ± 1452.4 kcal, p = 0.597).
Conclusion
Continuous tube feeding was an effective way to improve the tolerance of enteral nutrition. But no enough evidence was found to support the advantage in calorie intake of continuous tube feeding in this study.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Feigin VL, Krishnamurthi RV, Priya P, Bo N, Mensah GA, Bennett DA, et al. Update on the global burden of ischemic and hemorrhagic stroke in 1990–2013: the GBD 2013 Study. Neuroepidemiology. 2015;45:161–76.
Global Health Estimates 2016: Deaths by cause, age, sex, by country and by region, 2000–2016. 2018. http://www.who.int/healthinfo/global_burden_disease/estimates/en/.
Zhou M, Wang H, Zhu J, Chen W, Wang L, Liu S, et al. Cause-specific mortality for 240 causes in China during 1990–2013: a systematic subnational analysis for the Global Burden of Disease Study 2013. Lancet. 2016;387:251–72.
Delong W, Jianming Y, Yi Y, Bin P, Yilong W. Prevention and treatment of stroke in China is still facing enormous challenges-summary of the report on stroke prevention and treatment in China in 2018. Chin Circ J. 2019;34:6–20.
Naghavi M, Abajobir AA, Abbafati C, Abbas K, Abdallah F, Abera SF, et al. Global, regional, and national age-sex specific mortality for 264 causes of death, 1980–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet. 2017;390:1151–210.
Global health data exchange. GBD results tool. 2018. http://ghdx.healthdata.org/gbd-results-tool.
Fu X, Wong KS, Wei JW, Chen X, Lin Y, Zeng J, et al. Factors associated with severity on admission and in-hospital mortality after primary intracerebral hemorrhage in China. Int J Stroke. 2013;8:73–9.
Guan T, Ma J, Li M, Xue T, Lan Z, Guo J, et al. Rapid transitions in the epidemiology of stroke and its risk factors in China from 2002 to 2013. Neurology. 2017;89:53–61.
Mcclave SA, Martindale RG, Vanek VW, Mccarthy MC, Roberts PR, Taylor B, et al. Guidelines for the provision and assessment of nutrition support therapy in the adult critically Ill patient. J Parenter Enter Nutr. 2016;33:277–316.
Kudsk KA. Current aspects of mucosal immunology and its influence by nutrition. Am J Surg. 2002;183:390–8.
Windsor ACJ, Kanwar S, Li AGK, Barnes E, Guthrie JA, Spark JI, et al. Compared with parenteral nutrition, enteral feeding attenuates the acute phase response and improves disease severity in acute pancreatitis. Gut. 1998;42:431–5.
Taylor SJ, Fettes SB, Jewkes C, Nelson RJ. Prospective, randomized, controlled trial to determine the effect of early enhanced enteral nutrition on clinical outcome in mechanically ventilated patients suffering head injury. Crit Care Med. 1999;27:2525–31.
Mcclave SA, Martindale RG, Vanek VW, Mccarthy M, Roberts P, Taylor B, et al. Guidelines for the provision and assessment of nutrition support therapy in the adult critically ill patient: Society of Critical Care Medicine (SCCM) and American Society for Parenteral and Enteral Nutrition (A.S.P.E.N.). J Parenter Enter Nutr. 2009;33:277–316.
Rongcai J, Guangzhi S, Wei C, Junji W, Lihong L. Expert consensus on digestive and nutrition management of severe neurosurgical patients in China (2016). Natl Med J China. 2016;96:1643–7.
Aquilani R, Scocchi M, Boschi F, Viglio S, Iadarola P, Pastoris O, et al. Effect of calorie-protein supplementation on the cognitive recovery of patients with subacute stroke. Nutr Neurosci. 2008;11:235–40.
Aquilani R, Scocchi M, Iadarola P, Franciscone P, Verri M, Boschi F, et al. Protein supplementation may enhance the spontaneous recovery of neurological alterations in patients with ischaemic stroke. Clin Rehabilit. 2008;22:1042–50.
Zheng T, Zhu X, Liang H, Huang H, Yang J, Wang S. Impact of early enteral nutrition on short term prognosis after acute stroke. J Clin Neurosci. 2015;22:1473–6.
Wang SS, Zheng TH, Chen ZL, Yang JD, Zhou XY, Liu CF. The impact of early alimentary nutrition on short-term prognosis after acute stroke. Chin J Intern Med. 2007;46:366–9.
Ichimaru S, Amagai T. Intermittent and bolus methods of feeding in critical care. New York: Springer; 2015.
Bear DE, Hart N, Puthucheary Z. Continuous or intermittent feeding: pros and cons. Curr Opin Crit Care. 2018;24:1.
Patel JJ, Rosenthal MD, Heyland DK. Intermittent versus continuous feeding in critically ill adults. Curr Opin Clin Nutr Metab Care. 2017;21:1.
Bowling TE, Silk DB. Colonic responses to enteral tube feeding. Gut. 1998;42:147–51.
Duncan H, Cole S, Bowling T, Silk D. Does a nasogastric tube adversely affect distal colonic motility and contribute to pathogenesis of enteral feeding-related diarrhea? Gastroenterology. 1998;114:A876–A7.
Chowdhury AH, Murray K, Hoad CL, Costigan C, Marciani L, Macdonald IA, et al. Effects of bolus and continuous nasogastric feeding on gastric emptying, small bowel water content, superior mesenteric artery blood flow, and plasma hormone concentrations in healthy adults: a randomized crossover study. Ann Surg. 2016;263:450.
Ciocon JO, Galindociocon DJ, Tiessen C, Galindo D. Continuous compared with intermittent tube feeding in the elderly. J Parenter Enter Nutr. 1992;16:525–8.
Hiebert J, Brown A, Anderson R, Halfacre S, Rodeheaver G, Edlich R. Comparison of continuous vs intermittent tube feedings in adult burn patients. J Parenter Enter Nutr. 1981;5:73–5.
Zheru J, Yanyan Z, Na G. A study on different nasal feeding methods in stroke patients with dysphagia. Chin Foreign Med Res. 2014;12:24–5.
Gezhen Z. The application of continuous enteral nutrition in ICU patients. J Clin Med Pract. 2017;21:171–2.
Serpa LF, Kimura M, Faintuch J, Ceconello I. Effects of continuous versus bolus infusion of enteral nutrition in critical patients. Clinics 2003;58:9.
Vm TDA, Gomes PC, Caporossi C. Enteral nutrition in critical patients; should the administration be continuous or intermittent? Nutrición Hospitalaria. 2014;29:563.
Kocan MJ, Hickisch SM. A comparison of continuous and intermittent enteral nutrition in NICU patients. J Neurosci Nurs. 1986;18:333–7.
Desley H, Wendy C. Gastric feeding in critically ill children: a randomized controlled trial. Am J Crit Care. 2003;12:461–8.
Lee JSW, Tung Wai A. A comparison of two feeding methods in the alleviation of diarrhoea in older tube-fed patients: a randomised controlled trial. Age Ageing. 2003;32:388–93.
Macleod JBA, Jennifer L, Doug H, Christina R, James D, Cohn SM, et al. Prospective randomized control trial of intermittent versus continuous gastric feeds for critically ill trauma patients. J Trauma Acute Care Surg. 2007;63:57–61.
Forbes R, Jones C, Njoku C, Tulman D, Evans DC, Bergese S, et al. Continuous versus bolus tube feeds: does the modality affect glycemic variability or insulin requirements? J Am Coll Surg. 2013;217:S57–S8.
Metersky M, Skiest D. Intermittent enteral feeding: the influence on respiratory and digestive tract colonization in mechanically ventilated intensive-care-unit patients. Am J Respiratory Crit Care Med. 1996;154:394.
Li D, Yongjun W, Shaoshi W, Ning W, Yilong W. Chinese expert consensus on dysphagia and nutrition management in stroke patients. Chin J Stroke. 2013;8:973–83.
Su YY, Gao DQ, Zeng XY, Sha RJ, Niu XY, Wang CQ, et al. A survey of the enteral nutrition practices in patients with neurological disorders in the tertiary hospitals of China. Asia Pac J Clin Nutr. 2016;25:521–8.
Kao CC, Chiu HL, Liu D, Chan PT, Tseng IJ, Chen R, et al. Effect of interactive cognitive motor training on gait and balance among older adults: a randomized controlled trial. Int J Nurs Stud. 2018;82:121–8.
Kocan MJ, Hickisch SM. A comparison of continuous and intermittent enteral nutrition in NICU patients. J Neurosci Nurs. 1986;18:333–7.
Michelle K, Rebecca F. Enteral nutrition for adults in the hospital setting. Nutr Clin Pract. 2015;30:634–51.
Chapman MJ, Nguyen NQ, Deane AM. Gastrointestinal dysmotility: evidence and clinical management. Curr Opin Clin Nutr Metab Care. 2013;16:209–16.
Rhoney DH, Dennis P, Formea CM, Christina Y, Coplin WM. Tolerability of bolus versus continuous gastric feeding in brain-injured patients. Neurological Res. 2002;24:613–20.
Taylor SJ, Manara AR, Brown J. Treating delayed gastric emptying in critical illness: metoclopramide, erythromycin, and bedside (Cortrak) nasointestinal tube placement. J Parenter Enter Nutr. 2010;34:289–94.
Ibrahim K, Mustafa I, Eman Z, Nadia T. Incidence of aspiration and gastrointestinal complications in critically ill patients using continuous versus bolus infusion of enteral nutrition: a pseudo-randomised controlled trial. Aust Crit Care. 2014;27:188–93.
Hong Z, Guangjun Z, Wen C, Cuihua L. The research progress of the abdominal compartment syndrome monitoring. Med Inf. 2007;20:1715–7.
Jeremy PT. Nutritional interventions in critical illness. Proc Nutr Soc. 2007;66:16.
Ting C, Xueling C, Dan W. Effect of continuous enteral nutrition on the treatment effect and quality of life in stroke patients with dysphagia. J Qilu Nurs. 2015;21:16–8.
Bonten MJ, Gaillard CA, Van dHR, de Leeuw PW, Van dGS, Stobberingh EE, et al. Intermittent enteral feeding: the influence on respiratory and digestive tract colonization in mechanically ventilated intensive-care-unit patients. Am J Respiratory Crit Care Med. 1996;154:394.
Gazzaneo MC, Suryawan A, Orellana RA, Torrazza RM, Elkadi SW, Wilson FA, et al. Intermittent bolus feeding has a greater stimulatory effect on protein synthesis in skeletal muscle than continuous feeding in neonatal pigs. J Nutr. 2011;141:2152–8.
Stoll B, Puiman P, Cui L, Chang X, Benight NM, Bauchartthevret C, et al. Continuous parenteral and enteral nutrition induces metabolic dysfunction in neonatal pigs. J Parenter Enter Nutr. 2012;36:538–50.
Marik PE. Feeding critically ill patients the right ‘whey’: thinking outside of the box. A personal view. Ann Intensive Care. 2015;5:11.
Acknowledgements
Thanks for the support from all participants and their legal guardians. And we will give our thanks for the clinical practice help to RN Yan Wang and RN Min Tang from Neurosurgery Department in West China Hospital, Sichuan University.
Funding
This study was funded by Health Commission of Sichuan Province (18ZD032).
Author information
Authors and Affiliations
Contributions
WZ was responsible for study design, screening potentially eligible patients, data analysis, and paper drafting. YJ was responsible for study design, funding application, revising manuscript, and correspondence to editor. JPL was responsible for study design, funding application, revising manuscript, and correspondence to editor.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhu, W., Jiang, Y. & Li, J. Intermittent versus continuous tube feeding in patients with hemorrhagic stroke: a randomized controlled clinical trial. Eur J Clin Nutr 74, 1420–1427 (2020). https://doi.org/10.1038/s41430-020-0579-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-020-0579-6