Abstract
Background/Objectives
Plasma lipoprotein composition, especially in the postprandial state, could be relevant for cardiovascular risk and could be influenced by eating habits. This study evaluated the effects of a polyphenol-rich diet on postprandial lipoprotein composition in individuals at high cardiometabolic risk.
Subjects/Methods
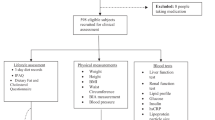
Seventy-eight individuals with high waist circumference and at least another component of the metabolic syndrome were randomized to either a high-polyphenol (HighP) or low-polyphenol (LowP) diet. Before and after the 8-week intervention, chylomicrons, VLDL1, VLDL2, IDL, LDL, HDL particles, and their lipid concentrations were determined over a 6-h high-fat test meal with high or low-polyphenol content, according to the diet assigned.
Results
VLDL1 postprandial areas under the curve (AUCs) were lower for cholesterol (Chol) (1.48 ± 0.98 vs. 1.91 ± 1.13 mmol/L × 6 h, M ± SD, p = 0.014) and triglycerides (Tg) (4.70 ± 2.70 vs. 6.02 ± 3.07 mmol/L × 6 h, p = 0.005) after the HighP than after the LowP diet, with no changes in Chol/Tg ratio. IDL Chol AUCs were higher after the HighP than after the LowP diet (1.29 ± 0.77 vs. 1.01 ± 0.51 mmol/L × 6 h, p = 0.037). LDL Tg AUCs were higher after the HighP than after the LowP diet (1.15 ± 0.33 vs. 1.02 ± 0.35 mmol/L × 6 h, p < 0.001), with a lower Chol/Tg ratio (14.6 ± 4.0 vs. 16.0 ± 3.8, p = 0.007). HDL Tg AUCs were lower after the HighP than after the LowP diet (1.20 ± 0.41 vs. 1.34 ± 0.37 mmol/L × 6 h, p = 0.013).
Conclusions
A high-polyphenol diet reduces the postprandial lipid content of large VLDL and increases IDL cholesterol; it modifies the composition of LDL particles—which become richer in triglycerides, and of HDL—which become instead triglyceride poor. The overall changes in atherogenicity by these effects warrant further investigation on clinical cardiovascular outcomes.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Nakamura K, Miyoshi T, Yunoki K, Ito H. Postprandial hyperlipidemia as a potential residual risk factor. J Cardiol. 2016;67:335–9.
Hyson D, Rutledge JC, Berglund L. Postprandial lipemia and cardiovascular disease. Curr Atheroscler Rep. 2003;5:437–44.
Jackson KG, Poppitt SD, Minihane AM. Postprandial lipemia and cardiovascular disease risk: Interrelationships between dietary, physiological and genetic determinants. Atherosclerosis. 2012;220:22–33.
Wojczynski MK, Glasser SP, Oberman A, Kabagambe EK, Hopkins PN, Tsai MY, et al. High-fat meal effect on LDL, HDL, and VLDL particle size and number in the Genetics of Lipid-Lowering Drugs and Diet Network (GOLDN): an interventional study. Lipids Health Dis. 2011;10:181.
Stefanutti C, Labbadia G, Athyros VG. Hypertriglyceridaemia, postprandial lipaemia and non-HDL cholesterol. Curr Pharm Des. 2014;20:6238–48.
Sabaka P, Kruzliak P, Gaspar L, Caprnda M, Bendzala M, Balaz D, et al. Postprandial changes of lipoprotein profile: effect of abdominal obesity. Lipids Health Dis. 2013;12:179.
Riccardi G, Vaccaro O, Costabile G, Rivellese AA. How well can we control dyslipidemias through lifestyle modifications? Curr Cardiol Rep. 2016;18:66.
Lima GPP, Vianello F, Corrêa CR, da Silva Campos RA, Borguini MG. Polyphenols in fruits and vegetables and its effect on human health. Food Nutr Sci. 2014;5:1065–82.
Del Rio D, Rodriguez-Mateos A, Spencer JP, Tognolini M, Borges G, Crozier A. Dietary (poly)phenolics in human health: structures, bioavailability, and evidence of protective effects against chronic diseases. Antioxid Redox Signal 2013;18:1818–92.
Bladé C, Arola L, Salvado MG. Hypolipidemic effects of proanthocyanidins and their underlying biochemical and molecular mechanisms. Mol Nutr Food Res. 2010;54:37–59.
Amiot MJ, Riva C, Vinet A. Effects of dietary polyphenols on metabolic syndrome features in humans: a systematic review. Obes Rev. 2016;17:573–86.
Fernández-Castillejo S, Valls RM, Castañer O, Rubió L, Catalán U, Pedret A, et al. Polyphenol rich olive oils improve lipoprotein particle atherogenic ratios and subclasses profile: a randomized, crossover, controlled trial. Mol Nutr Food Res. 2016;60:1544–54.
Burton-Freeman B. Postprandial metabolic events and fruit-derived phenolics: a review of the science. Br J Nutr. 2010;104:s1–14.
Annuzzi G, Bozzetto L, Costabile G, Giacco R, Mangione A, Anniballi G, et al. Diets naturally rich in polyphenols improve fasting and postprandial dyslipidemia and reduce oxidative stress: a randomized controlled trial. Am J Clin Nutr. 2014;99:463–71.
National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) final report. Circulation. 2002;106:3143–421.
Bozzetto L, Annuzzi G, Pacini G, Costabile G, Vetrani C, Vitale M, et al. Polyphenol-rich diets improve glucose metabolism in people at high cardiometabolic risk: a controlled randomised intervention trial. Diabetologia 2015;58:1551–60.
USDA special interest databases on flavonoids. Nutrient Data Laboratory Home Page: http://www.ars.usda.gov/nutrientdata/flav.Accessed 13 Sept 2018.
Phenol-Explorer: database on polyphenol content in foods. http://phenolexplorer.eu/. Accessed 13 Sept 2018.
Rivellese AA, De Natale C, Di Marino L, Patti L, Iovine C, Coppola S, et al. Exogenous and endogenous postprandial lipid abnormalities in type 2 diabetic patients with optimal blood glucose control and optimal fasting triglyceride levels. J Clin Endocrinol Metab. 2004;89:2153–9.
Bozzetto L, Annuzzi G, Corte GD, Patti L, Cipriano P, Mangione A, et al. Ezetimibe beneficially influences fasting and postprandial triglyceride-rich lipoproteins in type 2 diabetes. Atherosclerosis 2011;217:142–8.
Vetrani C, Rivellese A, Annuzzi G, Mattila I, Meudec E, Hyotylainen T, et al. Phenolic metabolites as compliance biomarker for polyphenol intake in a randomized controlled human intervention. Food Res Int. 2014;63:233–8.
Buchholz T, Melzig M. Polyphenolic compounds as pancreatic lipase inhibitors. Planta Med. 2015;81:771–83.
Zern TL, West KL, Fernandez ML. Grape polyphenols decrease plasma triglycerides and cholesterol accumulation in the aorta of ovariectomized guinea pigs. J Nutr. 2013;133:2268–72.
Assini JM, Mulvihill EE, Huff MW. Citrus flavonoids and lipid metabolism. Curr Opin Lipidol. 2013;24:34–40.
Baselga-Escudero L, Pascual-Serrano A, Ribas-Latre A, Casanova E, Salvadò MJ, Arola L, et al. Long-term supplementation with a low dose of proanthocyanidins normalized liver miR-33a and miR-122 levels in high-fat diet induced obese rats. Nutr Res. 2015;35:337–45.
Rottiers V, Näär AM. MicroRNAs in metabolism and metabolic disorders. Nat Rev Mol Cell Biol. 2012;13:239–50.
Packard CJ, Shepherd J. Lipoprotein heterogeneity and apolipoprotein B metabolism. Arterioscler Thromb Vasc Biol. 1997;17:3542–56.
Musliner TA, Mc Vicker KM, Iosefa JF, Krauss RM. Metabolism of human intermediate and very low density lipoprotein subfractions from normal and dysbetalipoproteinemic plasma. In vivo studies in rat. Arterioscler. 1987;7:408–20.
Krauss RM. Relationship of intermediate and low density lipoprotein subspecies to risk of coronary artery disease. Am Heart J. 1987;113:578–82.
Qin Y, Xia M, Ma J, Liu J, Mou H, Cao L, et al. Anthocyanin supplementation improves serum LDL- and HDL-cholesterol concentrations associated with the inhibition of cholesteryl ester transfer protein in dyslipidemic subjects. Am J Clin Nutr. 2009;90:485–92.
Chung BH, Liang P, Doran S, Cho BHS, Franklin F. Postprandial chylomicrons: potent vehicles for transporting cholesterol from endogenous LDL+ HDL and cell membranes to the liver via LCAT and CETP. J Lipid Res. 2004;45:1242–55.
Harchaoui KEL, Visser ME, Kastelein JJP, Stroes ES, Dallinga-Thie GM. Triglycerides and cardiovascular risk. Curr Cardiol Rev. 2009;5:216–22.
Zhao W, Haller V, Ritsch A. The polyphenol PGG enhances expression of SR-BI and ABCA1 in J774 and THP-1 macrophages. Atherosclerosis. 2015;242:611–7.
Farràs M, Valls RM, Fernández-Castillejo S, Giralt M, Solà R, Subirana I, et al. Olive oil polyphenols enhance the expression of cholesterol efflux related genes in vivo in humans. A randomized controlled trial. J Nutr Biochem. 2013;24:1334–9.
Masuda D, Yamashita S. Postprandial hyperlipidemia and remnant lipoproteins. J Atheroscler Thromb. 2017;24:95–109.
Kats D, Sharrett AR, Ginsberg HN, Nambi V, Ballantyne CM, Hoogeveen RC, et al. Postprandial lipemia and the risk of coronary heart disease and stroke: the Atherosclerosis Risk in Communities (ARIC) Study. BMJ Open Diabetes Res Care. 2017;5:e000335.
Vergès B. Pathophysiology of diabetic dyslipidaemia: where are we? Diabetologia. 2015;58:886–99.
März W, Scharnagl H, Winkler K, Tiran A, Nauck M, Boehm BO, et al. Low-density lipoprotein triglycerides associated with low-grade systemic inflammation, adhesion molecules, and angiographic coronary artery disease: the Ludwigshafen Risk and Cardiovascular Health study. Circulation. 2004;19:3068–74.
Albers JJ, Slee A, Fleg JL, O’Brien KD, Marcovina SM. Relationship of baseline HDL subclasses, small dense LDL and LDL triglyceride to cardiovascular events in the AIM-HIGH clinical trial. Atherosclerosis. 2016;251:454–9.
Elbaz M, Faccini J, Bongard V, Ingueneau C, Taraszkiewicz D, Perret B, et al. High-density lipoprotein subclass profile and mortality in patients with coronary artery disease: Results from the GENES study. Arch Cardiovasc Dis. 2016;109:607–17.
Martin SS, Khokhar AA, May HT, Kulkarni KR, Blaha MJ, Joshi PH, et al. HDL cholesterol subclasses, myocardial infarction, and mortality in secondary prevention: the Lipoprotein Investigators Collaborative. Eur Heart J. 2015;36:22–30.
Joshi PH, Toth PP, Lirette ST, Griswold ME, Massaro JM, Martin SS, et al. Lipoprotein Investigators Collaborative (LIC) Study Group. Association of high-density lipoprotein subclasses and incident coronary heart disease: The Jackson Heart and Framingham Offspring Cohort Studies. Eur J Prev Cardiol. 2016;23:41–9.
Gebhard C, Rhainds D, Tardif JC. HDL and cardiovascular risk: is cholesterol in particle subclasses relevant? Eur Heart J. 2015;36:10–2.
Vetrani C, Vitale M, Bozzetto L, Della Pepa G, Cocozza S, Costabile G, et al. Association between different dietary polyphenol subclasses and the improvement in cardiometabolic risk factors: evidence from a randomized controlled clinical trial. Acta Diabetol. 2018;55:149–53.
Acknowledgements
Parts of this study were presented at the 86th E-Poster session of the EAS Congress, Lisbon, Portugal, 05–08 May 2018.
Funding
The research leading to these results received funding from the European Community’s Seventh Framework Programme FP7/2009-2012 under grant agreement FP7-KBBE-222639, Etherpaths Project, and the ‘Ministero Istruzione Università e Ricerca’ PRIN 2010-2011-2010JCWWKM.
Author information
Authors and Affiliations
Contributions
LB, GA, GR, and AAR designed the experiment; LB, GDP, and CV collected and analyzed the data; GDP and CV interpreted the data and wrote the paper. GDP, CV, GC, MV, AM, PC, and LP collected the data. GA, GR, and AAR critically revised the paper and contributed to the conclusions. AAR is the guarantor of this work and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. All authors read and approved the final paper.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Trial registered at ClinicalTrials.gov as NCT01154478.
Supplementary information
Rights and permissions
About this article
Cite this article
Della Pepa, G., Vetrani, C., Vitale, M. et al. Effects of a diet naturally rich in polyphenols on lipid composition of postprandial lipoproteins in high cardiometabolic risk individuals: an ancillary analysis of a randomized controlled trial. Eur J Clin Nutr 74, 183–192 (2020). https://doi.org/10.1038/s41430-019-0459-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-019-0459-0
This article is cited by
-
Postprandial glycemic and lipidemic effects of black rice anthocyanin extract fortification in foods of varying macronutrient compositions and matrices
npj Science of Food (2023)
-
Polyphenols mediated attenuation of diabetes associated cardiovascular complications: A comprehensive review
Journal of Diabetes & Metabolic Disorders (2023)
-
Polyphenols: a route from bioavailability to bioactivity addressing potential health benefits to tackle human chronic diseases
Archives of Toxicology (2023)
-
Black chokeberry Aronia melanocarpa extract reduces blood pressure, glycemia and lipid profile in patients with metabolic syndrome: a prospective controlled trial
Molecular and Cellular Biochemistry (2021)
-
Diets naturally rich in polyphenols and/or long-chain n-3 polyunsaturated fatty acids differently affect microbiota composition in high-cardiometabolic-risk individuals
Acta Diabetologica (2020)