Abstract
Ferroptosis, a novel mode of cell death dependent on iron and reactive oxygen species, has been extensively explored during malignant tumors metastasis. Ferroptosis can interact with multiple components of the tumor microenvironment to regulate metastasis. These interactions generally include the following aspects: (1) Epithelial-mesenchymal transformation, which can help cancer cells increase their sensitivity to ferroptosis while they have multiple mechanisms to fight against it; (2) Disorder of iron metabolism in cancer stem cells which maintains their stem characteristics; (3) Polarization of M0 macrophages to M2. (4) The paradoxical effects of iron metabolism and CD8 + T cells induced by ferroptosis (5) Regulation of angiogenesis. In addition, ferroptosis can be regulated by miRNAs through the reprogramming of various intracellular metabolism processes, including the regulation of the glutathione- glutathione peroxidase 4 pathway, glutamic acid/cystine transport, iron metabolism, lipid metabolism, and oxidative stress. Therefore, there are many potential interactions between ferroptosis-related miRNAs and tumor metastasis, including interaction with cancer cells and immune cells, regulating cytokines, and angiogenesis. This review focuses on the role of ferroptosis-related miRNA in tumor metastasis, aiming to help readers understand their relationship and provide a new perspective on the potential treatment strategies of malignant tumors.
Similar content being viewed by others
Facts
-
1.
Ferroptosis can interact with multiple components of the tumor microenvironment to regulate metastasis.
-
2.
miRNAs can influence the progression of ferroptosis through different pathways.
-
3.
There is a potential link between miRNA, ferroptosis and tumor metastasis.
-
4.
Ferroptosis-related miRNAs are used as biomarkers for the diagnosis and prediction of tumor diseases.
Open question
-
1.
How does ferroptosis-related miRNA affect tumor progression, especially tumor metastasis?
-
2.
Can ferroptosis-related miRNA be used for targeted therapy of tumor diseases?
-
3.
Can we summarize the association of ferroptosis-related miRNAs with tumor metastasis through specific mechanisms?
Introduction
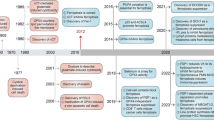
Ferroptosis was first discovered in 2012 and has widely attracted attention as a novel mode of cell death. Pathological characteristics of ferroptosis are mainly reflected in mitochondria, including smaller size, reduced or disappeared cristae, membrane concentration, and outer membrane rupture [1,2,3]. On the molecular level, ferroptosis needs to be triggered by intracellular iron overload and reactive oxygen species (ROS) production and accumulation [4].
The relationship between ferroptosis and tumor metastasis has received extensive attention. At present, studies have found lipid peroxidation and iron overload in cancer cells [5]. Theoretically, ferroptosis is an anti-tumor mechanism. However, the current research has found that cancer cells can escape from ferroptosis through a variety of mechanisms, which is conducive to the progression and metastasis of cancer [6].
MicroRNAs (miRNAs) are small, non-coding RNAs that downregulate gene expression by targeting the 3’UTR of mRNA during transcription [7]. Notably, studies have found that miRNA can also regulate ferroptosis by combining with mRNA [8, 9]. The effects of miRNAs include targeting glutamate/cystine transport to regulate glutathione synthesis [10], iron metabolism to regulate intracellular iron content, lipid metabolism to regulate reactive oxygen species (ROS) generation, and other oxidative stress pathways [11]. Ferroptosis-associated miRNA has multiple roles in the process of tumor metastasis, including regulating tumor cells, immune cells, angiogenesis, and cytokine secretion, etc. [12].
In this review, we discussed the relationship between ferroptosis and tumor metastasis, analyzed the mechanisms of miRNA regulating ferroptosis, and finally summarized the new roles of ferroptosis-related miRNAs in tumor metastasis. We hope this review could provide new suggestions and references for future research, and the treatment of malignant cancer.
Ferroptosis and metastasis in the tumor microenvironment (TME)
Metastasis is one of the prominent features of malignant tumors. It mainly contains the following steps. First, cancer in situ grows larger, and then invades the local blood vessels, lymph duct, or spreads directly. Then cancer cells can move with lymph or blood, gathering, adhering, and proliferating in the appropriate pre-metastatic niche of the secondary site where the structure of vessels or lymphatic ducts in the secondary site is changed and their permeability is increased, allowing the cancer cells to penetrate out of the circulatory system to invade and proliferate [13,14,15]. Recent studies have found that ferroptosis plays a regulatory role in the metastasis of malignant tumors, which mainly includes the regulation of tumor cells, cancer stem cells (CSCs), immune cells, epithelial-mesenchymal transition (EMT), tumor angiogenesis and so on.
Ferroptosis and cancer cells
Cancer in situ show the resistance to ferroptosis due to the high cell density and tight cell junctions. For most malignant tumors, EMT is the first procedure for the metastasis. Studies have found that cancer cells are connected by E-cadherin (ECAD), which is also increased in tumors with high cell density, inhibiting ferroptosis through the Ecad-NF2-Hippo-YAP signaling axis. After EMT, the reduction of ECAD could cause the increased sensitivity to ferroptosis [16,17,18]. Some studies used histone deacetylase (HDAC) inhibitors to induce EMT of human adrenal cortical cancer. In this process, the decreased expression of iron-exporting protein and antioxidant genes in cancer cells resulted in increased intracellular iron accumulation and the expression of ROS which indicates that cancer cells going through EMT have a greater possibility and sensitivity to ferroptosis [18]. Some other studies have found that some EMT transcription factors (EMT-TFs) (TWIST/SNAIL) can induce discoidin domain receptor2 (DDR2) expression thus increasing the sensitivity to ferroptosis through the Hippo pathway [19]. Cancer cells have an increased sensitivity to ferroptosis after EMT, which appears to be detrimental to tumor metastasis. In fact, they also have a variety of mechanisms to combat ferroptosis. It is reported that α6β4 integrin is involved in the anti-ferroptosis process [20, 21]. α6β4 integrin is an important component of type I hemidesmosomes (HD), which is found in the epithelium of various tissue types and participating in initiating HD assembly and mediating cell adhesion [22]. Once detached from ECM, α6β4 integrin on cancer cells inhibited the expression of long polyunsaturated fatty acid-rich enzyme acyl-CoA synthetase long-chain family member 4 (ACSL4) (essential for ferroptosis) through Src and signal transducer and activator of transcription 3 (STAT3) pathways [20]. The adhesion protein poliovirus receptor-related protein 4 (PVRL4) could also participate in this process which facilitate the accumulation of cancer cells isolated from ECM spontaneously and inhibit ferroptosis through PVRL4/α6β4/Src signaling pathway [21]. It also stimulates and maintains the expression of glutathione peroxidase 4 (GPX4), which can convert lipid hydroperoxides to lipid alcohols and inhibit the formation of ROS, thereby inhibiting ferroptosis [23]. In recent studies, it has been found that the interaction of cell migration-inducing protein (CEMIP) with inositol 1/4 in prostate cancer cells activates the nuclear factor erythroid 2-related factor 2 (NRF2) and promotes the transcription of solute Carrier Family 7, Member 11 (SLC7A11), (a glutamate/cysteine antiporter solute family 7 member). Promoting cystine uptake by cancer cells could increase ferroptosis resistance after ECM detachment [24]. This sensitization to ferroptosis after EMT and the anti-ferroptosis effect of cancer cells is a contradictory relationship that results in the release of large numbers of cancer cells from the carcinoma in situ tissue, but only some of them could successfully colonize (Fig. 1A).
A Some EMT-TFS can induce the expression of DDR2 to increase the ferroptosis sensitivity of cancer cells after EMT through the Hippo pathway, and inhibit the expression of iron export proteins to maintain intracellular iron overload and higher levels of ROS. The α6β4 integrin located on the cell membrane can activate the Src and STAT3 pathways to inhibit the expression of the long polyunsaturated fatty acid-rich enzyme ACSL4. The adhesion protein PVRL4 inhibits ferroptosis through the PVRL4/α6β4/Src signaling pathway. CEMIP interacts with inositol 1/4 to activate NRF2 to increase SLC7A11 transcription, and cancer cells uptake cystine to increase ferroptosis resistance after ECM detachment. B Iron overload can increase intracellular ROS, and activate macrophages to M1 phenotype by enhancing P300 /CBP acetyltransferase activity and promoting p53 acetylation, thereby promoting the progression of inflammation. At the same time, RRM2 gene expression can inhibit ferroptosis, promote the polarization of M2 macrophages, and inhibit the polarization of M1 macrophages to promote cancer progression and metastasis. The increased expression of NOX4 can activate the PI3K/Akt signaling pathway through the increase of ROS, causing the increased secretion of various cytokines such as VEGF-C, IL-8, and CCL7, and promoting the polarization of M2 phenotype macrophages. In cancer cells, M1 macrophages can activate CD8 + T cells to cause ferroptosis and play a killing role. CD8 + T cells downregulate the expression of SLC3A2 and SLC7A11, two subunits of XC—by releasing INFγ, which affects the uptake of cystine and promotes the production of ROS and ferroptosis. INFγ could also activate ACSL4 expression through the STAT1-IRF1 signaling pathway and trigger ACSL4-dependent ferroptosis. Cholesterol can increase the expression of CD36 in CD8 + T cells, increase the uptake of fatty acids by T cells, induce lipid peroxidation and ferroptosis of CD8 + T cells, and cause tumor-killing ability dysfunction.
CSCs exist in the primary tumor site of the TME, which are associated with strong differentiation and proliferation ability, and they are considered to be critical for metastasis [25]. Some stem cell markers and signaling pathways in CSCs are also related to iron, and the high density of intracellular iron is involved in maintaining CSC stem characteristics, protecting [26, 27]. The phenotype of CSCs is plastic and can be influenced by various signals in the TME, such as the Wnt signal and nuclear factor kappa-B (NF-κB) signal to transform between stem cell type and non-stem cell type [25]. Recently, the phenotypic plasticity of CSCs has been found to protect metastatic breast cancer cells from ferroptosis. Screening the secretome of breast cancer stem cells (BCSCs) revealed that dickkopf-related protein 1 (DKK1) reduced the stem cell phenotype by inhibiting Wnt signaling in metastatic cancer cells. DKK1 also reduced SLC7A11 expression and lipid peroxidation, and increased glutathione, thereby reducing ferroptosis [28].
Ferroptosis and immune cells
Ferroptosis and tumor-associated macrophages (TAMs)
TAMs are one of the most significant regulatory cells in the TME. Among them, M2-phenotype macrophages account for the majority in the late stage of malignant tumors, which promote tumor progression and angiogenesis, mediating malignant tumor immunosuppression, and metastasis [29, 30]. Studies found that there are many types of receptors on the surface of TAMs, which can trigger ferroptosis of tumor cells through a variety of signaling pathways, and affect the polarization state of macrophages [31]. For instance, iron overload can increase the expression of ROS in macrophages. Then, they are activated to the M1 phenotype by enhancing P300/cAMP-response element binding protein (CREB)-binding protein (CBP) acetyltransferase activity and promoting p53 acetylation, thereby improving the progression of inflammation [32]. In cancer cells, M1 macrophages are the main cause of ferroptosis through the activation of CTL.
At late stages of cancer, macrophages with M2 phenotype are increased. Ribonucleoside-Diphosphate reductase subunit M2 (RRM2), one of the regulatory factors related to ferroptosis, affects the prognosis of lung adenocarcinoma through database analysis. Subsequent experiments showed that RRM2 could inhibit ferroptosis, promote the polarization of M2 macrophages, and inhibit the polarization of M1 macrophages to facilitate cancer progression and metastasis [33, 34]. In non-small cell lung cancer, NADPH oxidase 4 (NOX4) expression is increased, which can activate the PI3K/Akt signaling pathway through ROS increase. It upregulates the secretion of various cytokines such as vascular endothelial growth factor-C (VEGF-C), IL-8, and chemokine (C-C motif) ligand 7 (CCL7), which promote M2 macrophage polarization and metastasis (Fig. 1B) [35].
At present, the direct link between ferroptosis and TAM as well as the related mechanisms and pathways are still not clear. However, it is undeniable that clarifying the relationship is promising for the treatment. Studies have used nanomaterials equipped with ferroptosis inducers to increase the anti-inflammatory response of tumor cells through ferroptosis stress, induce the polarization of M1 phenotype macrophages, and regulate inflammatory and metabolic functions for tumor treatment [36].
Ferroptosis and T cell
Ferroptosis also interacts with various immune cells in the TME, and the relationship with CD8 + T cells has been most deeply explored. The traditional view is that CD8 + T cells kill tumor cells through perforin-granzyme and Fas-Fasl mechanisms [37,38,39]. With a deeper understanding of ferroptosis, researchers found that CD8 + T cells can also induce cancer cells ferroptosis. CD8 + T cells downregulate the expression of SLC3A2 and SLC7A11, two subunits of the glutamate-cystine antiporter system Xc- by releasing interferon-γ (INF-γ), which affects cystine uptake and promotes ROS production and ferroptosis [38]. Recent studies have found that INF-γ could activate ACSL4 expression through the signal transducer and activator of transcription 1 -interferon regulatory factor 1 (STAT1-IRF1) signaling pathway, leading to ACSL4-dependent ferroptosis [38, 40]. However, this killing effect could not be maintained for long, after which cholesterol in the TME could induce CD36 expression on CD8 + T cells. This increases the uptake of fatty acids by T cells, resulting lipid peroxidation, and ferroptosis of CD8 + T cells themselves. Leading the loss of tumor-killing function and anti-tumor ability gradually, thus increasing tumor metastasis (Fig. 1B) [41,42,43].
Ferroptosis and other immune cells
The TME can cause metabolic reprogramming in other different types of immune cells, including abnormal iron metabolism and lipid peroxidation. But there are few studies on the direct relationship between them. At present, omics studies have found that the ferroptosis regulatory gene SLC7A11 can reduce the abundance of NK cells and inhibit anti-tumor immunity [44]. Experiments in vitro revealed that the mitochondrial iron transport protein ATP-binding cassette transporter 7 (ABCB7) is essential for B cell development, proliferation, class switching, and recombination [45]. Minghua Yang et al. discovered that granulocytes in glioblastoma can trigger cancer cell ferroptosis. Neutrophils can transfer myeloperoxidase into cancer cells, inducing iron-dependent accumulation of lipid peroxides [46]. The interaction between ferroptosis and immune cells needs more deeper research to analyze the mechanism, pathway, and effect on tumor progression and metastasis.
Ferroptosis and angiogenesis
Angiogenesis is one of the significant features of malignant tumors. Although the direct role of ferroptosis in this process has not been fully investigated, ROS production has been shown to participate in tumor angiogenesis [47]. In endothelial cells, ROS can be derived from NADPH oxidase in mitochondria. Under the stimulation of inflammation and tumor substances, it can cause the expression of angiogenic cytokines such as VEGF. Activated NOX and ROS could change local vascular endothelial cells from a static to a proliferative state, which is conducive to angiogenesis [48]. At present, the relationship between ferroptosis and angiogenesis is not clear. Recent studies have reported that miR-539 can activate the stress-activated protein kinase/jun N-terminal kinases (SAPK/JNK) signaling pathway by targeting tumor necrosis factor (TNF) -α-induced protein 8 (TIPE) and reduce the expression of GPX4 to inhibit ferroptosis in colorectal cancer cells [49]. Meanwhile, TIPE promotes vascular endothelial growth factor receptor 2 (VEGFR2)-mediated angiogenesis by upregulating the expression and phosphorylation of pyruvate dehydrogenase kinase 1 (PDK1) in cancer cells [50], thus promoting metastasis.
miRNAs and ferroptosis
The emerging evidence suggests that miRNAs are involved in regulating multiple key steps of ferroptosis, including glutathione-GPX4 pathway, glutamate/cystine transport, iron metabolism, and lipid metabolism.
miRNAs regulate the glutathione-GPX4 pathway
GPX4 is a glutathione-dependent enzyme that transforms toxic lipid hydroperoxides to nontoxic lipoalcohol (L-OH), thereby reducing the conversion of iron-induced lipid hydroperoxides to highly reactive lipid alkoxyl radicals, and restraining ferroptosis. The inhibition of GPX4 promotes the progression of ferroptosis. For example, miR-15 can inhibit GPX4 expression by interacting with the 3’-UTR of GPX4 mRNA [51], which blocks the conversion of glutathione (GSH) to L-glutathione Oxidized (GSSG), hinders the conversion of hazardous lipid peroxides into nontoxic L-OH, increases GSH, ROS levels and malondialdehyde (MDA), and accelerates the progress of ferroptosis. miR-15a-3p [52], miR-1287-5p [53], and miR-324-3p have similar roles in cancer by directly targeting GPX4 to positively regulate ferroptosis [54].
What’s more, activating transcription factor 4 (ATF4) is a member of the CREB / ATF family, and acts as a transcriptional activator and repressor in ferroptosis. MicroRNA-214-3p plays a regulatory role in hepatocarcinogenesis, and the inhibition of miR-214 can directly promote the expression of ATF4 [55]. ATF4 binds with an amino acid reaction element in the promoter region of the SLC7A11, promoting the transcription of SLC7A11. On the other hand, ATF4, a key point of endoplasmic reticulum stress affecting ferroptosis, promotes heat shock 70 kDa protein 5 (HSPA5) expression through the PERK-ATF4-CHOP pathway, increases GPX4 expression, hinders ROS generation, and suppresses ferroptosis.
miRNAs regulate glutamate/cystine transport
It has been confirmed that the regulation of the glutamate/cysteine reverse transport system key proteins can affect ferroptosis in tumor cells, such as SLC38A1, SLC1A5, SLC3A2, and SLC7A11. System Xc-(SLC3A2 and SLC7A11) pumps glutamate away from the cell in a 1:1 ratio while transferring the extracellular cystine to the cell [56]. When System Xc-function is inhibited or deactivated, it leads to cysteine depletion, lipid peroxidation, and ferroptosis [10]. miR-5096 [57], miR-27a-3p [58], miR-375 [59], and miR-34c-3p can inhibit cysteine and GSH generation by directly targeting SLC7A11 [60], which increase ROS and iron accumulation levels, thus promoting ferroptosis. Acting as a chaperone of SLC7A11, SLC3A2 contributes to the stability of SLC7A11 protein. miR-142-3p has been found to highly express in the M1 macrophages of hepatocarcinoma tissue, which could affect the production of GSH, Fe2+, and MDA, promoting ferroptosis of the M1 macrophages by targeting SLC3A2, thus facilitating tumor metastasis [61]. SLC1A5 and SLC38A1 can mediate the uptake of neutral amino acids such as glutamine (Gln). Direct targeting of SLC1A5 to inhibit Gln uptake by miR-137 resulted in a decrease in the generation of glutamate (Glu) and ROS, thereby inhibiting ferroptosis. Although α -ketoglutarate (α-KG) can enhance insensitive ferroptosis of miR-137 to rescue the overall inhibitory effect, it also suggests that SLC1A5 is located upstream in the Gln decomposition process [62].
Furthermore, β-mercaptoethanol can convert the incoming cystine into cysteine without relying on systemic XC-. Cystethiane β-synthase (CBS) acts as a marker of transsulfuration activity, participates in ferroptosis and protects hepatocellular carcinoma, lung cancer, and breast cancer cells from ferroptosis [63]. miR-6852 can directly bind to CBS, reduce cysteine uptake, increase the intracellular concentrations of lipid ROS, reduce the cellular mitochondrial membrane potential and promote ferroptosis [63].
miRNAs regulate iron metabolism
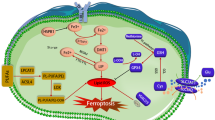
Excessive iron accumulation is the basis of ferroptosis. Iron bind to transferrin and exist in the form of Fe3+, after entering the cells through the transferrin receptor (TFR1) on the cell membrane, it is converted to the Fe2+ under the function of six-transmembrane epithelial antigen of the prostate 3 (STEAP3) [64]. Later, the divalent metal ion transporter 1 (DMT1) transports it to the cytoplasm of the unstable iron pool. The intracellular accumulation of excessive Fe2+ can trigger Fenton reactions to generate Fe and hydroxyl radicals, thus producing a large amount of ROS. It has shown that miR-148a [65], miR-107 [66], and miR-378g can downregulate TFR1 expression by binding to TFR1 3’UTR [67], affecting intracellular iron homeostasis and promoting the proliferation of hepatocarcinoma (HCC), colorectal cancer, and laryngeal cancer cells, respectively.
Excessive intracellular Fe3+ can be stored in ferritin, and the unbound part is excreted outside by membrane ferroportin 1 (FPN1), thereby maintaining intracellular iron metabolism homeostasis. Ferritin heavy chain 1 (FTH1) and ferritin light chain (FTL) both are the components of ferritin [68]. It has been shown that lncRNA H19 can enhance the transcriptional activity of the endogenous FTH1 by sponging miRNA-19b-3p, which increases the storage of ferric ions to reduce the intracellular free iron content and inhibits ROS generation and ferroptosis [69]. miR-147a [70], miR-302a-3p [71], and miR-153-5p can directly bind to the 3’-untranslated region of FPN1 and inhibit iron export, thereby promoting iron overload, lipid peroxidation, and ferroptosis [72]. What’s more, Nrf2 can increase the transcription level of FPN1, thereby increasing the extracellular output of intracellular iron and reducing the Fe2+ levels in the intracellular labile iron pool (LIP). In myeloma cells, Nrf2 directly trans-activates FPN1 or promotes FPN1 expression by inhibiting miR-17-5p, promoting iron export, reducing the intracellular ferric ion concentration and ROS production, and inhibiting ferroptosis [73]. This provides a new direction to target the iron mechanism.
miRNAs regulate lipid metabolism
One of the characteristics of ferroptosis is the accumulation of ROS through polyunsaturated fatty acid (PUFA) peroxidation [74]. For example, arachidonic acid (AA) and adrenal acid (AdA) are the main free PUFAs, and ACSL4 uses coenzyme A to catalyze the AA/AdA for the generation of AA / AdA-CoA, then esterifying to AA/AdA-PE under the influence of lysophosphatidylcholine acyltransferase 3 (LPCAT3), and finally oxidized to lipid peroxides by ALOXs. The downregulated miR-424-5p can directly bind to the 3’-UTR of ACSL4 to improve the expression of ACSL4 [75], promote the accumulation of lipid peroxides, destroy the integrity of cell membrane and the release of cell contents, which triggers ferroptosis [76]. Similarly, the downregulation of miR-670-3p [77] and miR-23a-3p also accelerate ferroptosis by targeting ACSL4 [78]. Cisplatin and paclitaxel can increase miR-522 secretion of fibroblast exosomes by activating the USP7/hnRNPA1 axis, while miR-522 can directly interact with arachidonate 15-lipoxygenase (ALOX15), reduce the conversion of PUFA to PUFAs-OOH, suppress lipid peroxidation and ROS production, and ultimately reduce chemosensitivity [79].
Tumor cells prefer to synthesize fatty acids de novo than normal cells that tend to uptake them from exogenous sources. When lipid synthesis increases in cancer cells, more lipid biosynthetic enzymes are needed to produce different fatty acids [11]. Stearyl-coenzyme A desaturase 1 (SCD1) is an essential enzyme for the de novo synthesis of FA, which catalyzes the desaturation of saturated fatty acid to monounsaturated fatty acid (MUFA). LINC01606 promotes SCD1 expression and functions through interaction with miR-423-5p to control intracellular MUFA synthesis and activate Wnt/β-catenin signaling [80]. This signaling enhances LINC01606 expression to promote MUFA synthesis continuously, while MUFA competitively affects PUFA peroxidation [56], thereby inhibiting ferroptosis. (Fig. 2 and Table 1).
The role of the ferroptosis-related miRNAs in tumor metastasis
Ferroptosis can play a regulatory role in the process of tumor metastasis, including regulating tumor cells, tumor stem cells, immune-related cells, tumor angiogenesis and so on. Considering that miRNAs could participate in the process of ferroptosis, the ferroptosis-related miRNAs could affect tumor metastasis, as well.
Ferroptosis-related miRNAs regulate tumor cells
The miRNA can promote metastasis by regulating morphological transition. miR-15a-3p is significantly downregulated in ovarian cancer [81], gastric cancer, and small-cell lung cancer [82]. It directly boosts the expression of E-cadherin, N-cadherin, and c-fos through Twist1, which induces EMT and enhances tumor migration and metastasis [83]. Interestingly, Twist1 is an inhibitor of ATF4, which activates the ATF4/CHAC1 pathway to induce GSH degradation, affecting ferroptosis [84]. Moreover, miR-15a-3p can inhibit pancreatic cancer cell proliferation, invasion, EMT, and stemness characteristics by suppressing the SLC39A7-mediated Wnt/β-catenin pathway [85]. What’s more, Wnt/β-catenin pathway can inhibit PUFA peroxidation by enhancing MUFA, which is associated with the downregulation of ferroptosis [80], which is a disadvantage for ferroptosis. Notably, ferroptosis-associated miR-5096 can not only target SLC7A11 to increase ROS and iron accumulation directly, but also regulate EMT marker expression and inhibits the metastatic potential of the cells [57], thus hindering tumor metastasis.
CSCs are the source of cancer initiation, recurrence, and metastasis. The specific miRNAs have regulatory effects on CSCs. Moreover, EMT and CSC formation have a strong correlation with tumor invasion and metastasis, and they are associated with tumor cell chemoresistance [86]. The level of miR-214-3p is significantly low in LSCC tissues while the level of yes-associated protein 1 is high, and it maintains CSC properties by activating the Hippo signaling pathway [87]. While downregulation of YAP/TAZ activity after DDR2 knockdown may contribute to ferroptosis protection.
miRNA can regulate tumor metastasis through intercellular communication with the tumor cells. Exosomes are a subset of membrane-bound extracellular vesicles ranging from 50 to 150 nm in diameter and contain multiple molecules, such as miRNA, leading to the miRNA transition to other tumor cells through exosomes. miR-9 secreted by tumor cells can be transferred to normal fibroblasts through exosomes, thus improving cell motility in breast cancer by reducing the expression of E-cadherin and calcium-dependent cell-cell adhesion glycoproteins [88]. USP7 promotes the secretion of miR-522 derived from cancer-associated fibroblasts (CAFs) exosome by regulating hnRNPA1 deubiquitination, targeting ALOX15 in tumor cells to inhibit the production of ROS, and increasing the chemoresistance of gastric cancer cells [79].
Ferroptosis-related miRNAs regulate immune cells
miRNA regulates the function of immune cells and tumor metastasis through several mechanisms, such as regulating metabolic reprogramming and macrophage phenotype. Leukemia cell-derived sEV-associated miR-19a-3p alters the metabolic reprogramming of CD8 + T cells by targeting SLC6A8-mediated creatine import, causing immune evasion and tumor metastasis [89]. CD8 + T cells are reduced by releasing IFN-γ, resulting in attenuated downregulation of SLC7A11. Besides, PD-L1 inhibits T-cell proliferation by binding to programmed death 1 (PD-1). It has been shown that ER-stressed HCC cells deliver miR-23a-3p in exosomes to macrophages, which activates the PI3K-AKT pathway by inhibiting phosphatase and tensin homolog (PTEN) to increase PD-L1 expression, reducing the CD8 + T cell ratio and IL-2 production, thereby resulting in tumor escape [90]. Similarly, miR-424-5p actively rescues the exhaustion of T cells by downregulating PD-L1 expression [91]. Furthermore, lncRNA FENDRR upregulates GADD45B to inhibit Treg-mediated immune escape of HCC cells by sponging miR-423-5p [92]. However, its effects on tumor metastasis meed to be further studied.
miRNA can promote tumor progression by regulating macrophage phenotype. miR-153-5p directly targets FPN1 to promote iron overload, lipid peroxidation, and ferroptosis. In addition, studies have shown that iron overload can increase the levels of M1 markers (e.g., IL-6, TNF-α, and IL-1β) and reduce M2 polarization, which restrains the tumor progression and metastasis [93]. Moreover, lncRNA FYVE, RhoGEF and PH domain containing 5 antisense RNA 1 (FGD5-AS1) upregulates bone marrow stromal cell antigen 2 (BST2) by sponging miR-129-5p, suppressing M1 macrophage polarization, and simultaneously inducing M2 macrophage polarization, thus increasing the development of cervical cancer [94]. A similar effect has been observed in miR-17-5p, whose over-expression could promote M2 polarization and enhance gastric cancer cell metastasis [95].
Ferroptosis-related miRNAs regulate cytokines
Ferroptosis-related miRNA influences tumor metastasis by regulating the expression of cytokines (e.g., transforming growth factor-β 1 (TGF-β1), CCL5, and IL-8). TGF-β could regulate cell proliferation and differentiation through a series of signal pathways. In the SMAD pathway, TGF-β signaling activates drosophila mothers against decapentaplegic protein 2 (Smad2) and Smad3 via TβRI and TβRII to form the SMAD complex, which is transferred to the nuclear to promote EMT progression [96]. For example, miR-9 can directly target the 3’UTR of SOX7 and inhibit the transcriptional activity of SOX7 mRNA, thereby promoting TGF-β1-induced non small-cell lung cancer (NSCLC) cell metastasis [97]. miR-19a can induce EMT under the upregulation of TNF-α, thus promoting colorectal cancer (CRC) invasion and metastasis. However, the underlying molecular mechanisms are not fully cleared [98]. miR-129-5p could inhibit the metastasis of gastric cancer cells by downregulating IL-8 expression, which is known as the chemokine ligand (CXCL) 8 and plays a pivotal role in angiogenesis and metastasis [99].
Ferroptosis-related miRNAs regulate angiogenesis
Tumor angiogenesis could be regulated by ferroptosis-related miRNAs from different types of cells in the TME. miRNA-17-92, a miRNA cluster that promotes cancer progression, has been found to target zinc lipoprotein A20-ACSL4 axis, which protects endothelial cells from ferroptosis [100] and facilitates angiogenesis. LncRNA SNHG11 is highly expressed in pancreatic cancer patients, which promotes VEGFA expression by miR-324-3p, thus increasing tumor angiogenesis and facilitating metastasis [101]. In glioma, miR-9 is increased by the paracrine secretion of cancer cells. After being absorbed by endothelial cells, miR-9 acts on multiple targets and promotes angiogenesis [102]. Meanwhile, some ferroptosis-related miRNAs have an inhibitory effect on tumor angiogenesis. One study identified the role of miR-214 in inhibiting angiogenesis and promoting apoptosis in HCC by using a miRNAs mimetic and inhibitor transfection manner [103], while miR-214 is frequently downregulated in HCC, and the paracrine activation of hepatoma-derived growth factor (HDGF) promotes tumor angiogenesis. miR-375 inhibits the platelet-derived growth factor C (PDGFC) and then inhibits the tumor angiogenesis [104]. Therefore, ferroptosis-related miRNA can play a promoting or inhibitory role in the process of tumor angiogenesis, thus affecting the occurrence and development of tumor metastasis. (Fig. 3 and Table 2).
Ferroptosis-related miRNA relates to tumor metastasis by influencing tumor cells (EMT, CSCs, and exosome), immune cells, cytokines, and angiogenesis. A miR-15a-3p targets Twist1 to regulate E-cadherin, N-cadherin, and c-fos expression, which induces mesenchymal cell morphology and enhances tumor migration and metastasis. B miR-214-3p suppresses CSC by directly targeting the yes-associated protein 1 (YAP1) and activating the Hippo signaling pathway. C miR-522 derived from CAFs exosome targets ALOX15 in tumor cells to inhibit the production of ROS, and increasing the chemoresistance of cancer cells. D miR-19a-3p alters the metabolic reprogramming of CD8 + T cells by targeting SLC6A8-mediated creatine import, causing immune evasion. E miR-129-5p targets BST2 and suppress M2 macrophage polarization, thus increasing the development of cervical cancer. F miR-9 can directly target the 3’UTR of SOX7 and inhibit the transcriptional activity of SOX7 mRNA, thereby promoting TGF-β1-induced NSCLC cell metastasis. G miR-129-5p could inhibit the metastasis of gastric cancer cells by downregulating IL-8 expression. H miRNA-17-92 targets zinc lipoprotein A20-ACSL4 axis, protects endothelial cells from ferroptosis and facilitates angiogenesis. (I) miR-375 inhibits PDGFC and then inhibits the tumor angiogenesis.
Application of ferroptosis-related miRNAs in tumor therapy
miRNAs could affect ferroptosis and regulate the metastatic process of tumors, which provides a new direction for the subsequent tumor diagnosis and drug development [105]. Currently, there are already ferroptosis-related miRNAs used as biomarkers for tumor diagnosis or prediction, like miR-214, miR-17-92, and miR-324-3p [106], etc. Moreover, targeted therapy of miRNAs in tumor metastasis is also under explored. Icariside II is a flavonoid with antitumor properties [107], which directly suppresses the GPX4 through miR-324-3p to induce ferroptosis, thus inhibiting the migration and invasion of renal cell carcinoma (RCC) [108]. This natural extract may be an effective drug for the treatment of RCC. As an analgesic, ketamine is ideal for managing cancer-related pain in clinical practice. Ketamine could significantly inhibit HCC progression by targeting lnvPVT1/miR-214-3p axis and decreasing GPX4 [109], thereby promoting the ferroptosis, both in vitro and in vivo. However, due to the possibility of abuse of ketamine, it is may not available for clinical use yet. In addition to drugs, nanotechnology is also being used in the treatment of tumors. Luo Y et al. used nanoparticle-coated miR-101-3p to target TBLR1, promoting ferroptosis and inhibiting lung cancer progression [110]. These indicate that miRNAs have promising prospects in future clinical diagnosis and treatment (Table 3).
Conclusion
Current basic research on ferroptosis is growing exponentially. miRNA is thought to play a different regulatory role in the ferroptosis process, but there are still some problems in this field. With too few existing studies, the specific mechanisms by which ferroptosis regulates the tumor metastasis process are still being explored. Moreover, although it is relatively clear that miRNA regulates ferroptosis and tumor metastasis, respectively, it is ambiguous how miRNA regulates tumor metastasis through ferroptosis. Nonetheless, we illustrate the new role of ferroptosis-related miRNA on the regulation of tumor metastasis, and the potential link between miRNA, ferroptosis, and tumor metastasis, thus providing new perspectives and thoughts for future experimental research. In the future, further extensive exploration of the relationship of miRNA in tumor metastasis and ferroptosis is needed, and it provides new targets and directions for the treatment of cancer by developing appropriate model systems to help in the diagnosis, treatment, and prognosis of cancer.
References
Qiu Y, Cao Y, Cao W, Jia Y, Lu N. The application of ferroptosis in diseases. Pharm Res. 2020;159:104919.
Chen X, Kang R, Kroemer G, Tang D. Broadening horizons: the role of ferroptosis in cancer. Nat Rev Clin Oncol. 2021;18:280–96.
Mou Y, Wang J, Wu J, He D, Zhang C, Duan C, et al. Ferroptosis, a new form of cell death: opportunities and challenges in cancer. J Hematol Oncol. 2019;12:34.
Wang H, Liu C, Zhao Y, Gao G. Mitochondria regulation in ferroptosis. Eur J Cell Biol. 2020;99:151058.
Ye L, Jin F, Kumar SK, Dai Y. The mechanisms and therapeutic targets of ferroptosis in cancer. Expert Opin Ther Targets. 2021;25:965–86.
Lei G, Zhuang L, Gan B. Targeting ferroptosis as a vulnerability in cancer. Nat Rev Cancer. 2022;22:381–96.
Ding C, Ding X, Zheng J, Wang B, Li Y, Xiang H, et al. miR-182-5p and miR-378a-3p regulate ferroptosis in I/R-induced renal injury. Cell Death Dis. 2020;11:929.
Zhang H, Ge Z, Wang Z, Gao Y, Wang Y, Qu X. Circular RNA RHOT1 promotes progression and inhibits ferroptosis via mir-106a-5p/STAT3 axis in breast cancer. Aging. 2021;13:8115–26.
Wu ZH, Tang Y, Yu H, Li HD. The role of ferroptosis in breast cancer patients: a comprehensive analysis. Cell Death Discov. 2021;7:93.
Xie Y, Hou W, Song X, Yu Y, Huang J, Sun X, et al. Ferroptosis: process and function. Cell Death Differ. 2016;23:369–79.
Liu M, Kong XY, Yao Y, Wang XA, Yang W, Wu H, et al. The critical role and molecular mechanisms of ferroptosis in antioxidant systems: a narrative review. Ann Transl Med. 2022;10:368.
Brown RAM, Richardson KL, Kabir TD, Trinder D, Ganss R, Leedman PJ. Altered iron metabolism and impact in cancer biology, metastasis, and immunology. Front Oncol. 2020;10:476.
Steeg PS. Tumor metastasis: mechanistic insights and clinical challenges. Nat Med. 2006;12:895–904.
Valastyan S, Weinberg RA. Tumor metastasis: molecular insights and evolving paradigms. Cell 2011;147:275–92.
Wan L, Pantel K, Kang Y. Tumor metastasis: moving new biological insights into the clinic. Nat Med. 2013;19:1450–64.
Sun T, Chi J-T. Regulation of ferroptosis in cancer cells by YAP/TAZ and Hippo pathways: The therapeutic implications. Genes Dis. 2021;8:241–9.
Juan WC, Hong W. Targeting the hippo signaling pathway for tissue regeneration and cancer therapy. Genes. 2016;7:55
Oliveira T, Hermann E, Lin D, Chowanadisai W, Hull E, Montgomery M. HDAC inhibition induces EMT and alterations in cellular iron homeostasis to augment ferroptosis sensitivity in SW13 cells. Redox Biol. 2021;47:102149.
Lin C-C, Yang W-H, Lin Y-T, Tang X, Chen P-H, Ding C-KC, et al. DDR2 upregulation confers ferroptosis susceptibility of recurrent breast tumors through the Hippo pathway. Oncogene. 2021;40:2018–34.
Brown CW, Amante JJ, Goel HL, Mercurio AM. The α6β4 integrin promotes resistance to ferroptosis. J Cell Biol. 2017;216:4287–97.
Brown CW, Amante JJ, Mercurio AM. Cell clustering mediated by the adhesion protein PVRL4 is necessary for α6β4 integrin-promoted ferroptosis resistance in matrix-detached cells. J Biol Chem. 2018;293:12741–8.
de Pereda L, Sonnenberg JM. A. Regulation of hemidesmosome dynamics and cell signaling by integrin α6β4. J Cell Sci. 2021;134:jcs259004.
Forcina GC, Dixon SJ. GPX4 at the Crossroads of Lipid Homeostasis and Ferroptosis. Proteomics 2019;19:e1800311.
Liu B, Li X, Wang D, Yu Y, Lu D, Chen L, et al. CEMIP promotes extracellular matrix-detached prostate cancer cell survival by inhibiting ferroptosis. Cancer Sci. 2022;113:2056–70.
Batlle E, Clevers H. Cancer stem cells revisited. Nat Med. 2017;23:1124–34.
Cosialls E, El Hage R, Dos Santos L, Gong C, Mehrpour M, Hamaï A. Ferroptosis: cancer stem cells rely on iron until "to die for" it. Cells. 2021;10:2981.
Szymonik J, Wala K, Górnicki T, Saczko J, Pencakowski B, Kulbacka J. The impact of iron chelators on the biology of cancer stem cells. Int J Mol Sci. 2021;23:89.
Wu M, Zhang X, Zhang W, Chiou YS, Qian W, Liu X, et al. Cancer stem cell regulated phenotypic plasticity protects metastasized cancer cells from ferroptosis. Nat Commun. 2022;13:1371.
Cassetta L, Pollard JW. Targeting macrophages: therapeutic approaches in cancer. Nat Rev Drug Discov. 2018;17:887–904.
Mantovani A, Marchesi F, Malesci A, Laghi L, Allavena P. Tumour-associated macrophages as treatment targets in oncology. Nat Rev Clin Oncol. 2017;14:399–416.
Zhou Z, Xu B, Hu N, Guo Z, Bao W, Shao B, et al. Targeting the macrophage-ferroptosis crosstalk: a novel insight into tumor immunotherapy. Front Biosci. 2022;27:203.
Zhou Y, Que K-T, Zhang Z, Yi ZJ, Zhao PX, You Y, et al. Iron overloaded polarizes macrophage to proinflammation phenotype through ROS/acetyl-p53 pathway. Cancer Med. 2018;7:4012–22.
Tang B, Xu W, Wang Y, Zhu J, Wang H, Tu J, et al. Identification of critical ferroptosis regulators in lung adenocarcinoma that RRM2 facilitates tumor immune infiltration by inhibiting ferroptotic death. Clin Immunol. 2021;232:108872.
Jin C-Y, Du L, Nuerlan AH, Wang X-L, Yang Y-W, Guo R. High expression of RRM2 as an independent predictive factor of poor prognosis in patients with lung adenocarcinoma. Aging. 2020;13:3518–35.
Zhang J, Li H, Wu Q, Chen Y, Deng Y, Yang Z, et al. Tumoral NOX4 recruits M2 tumor-associated macrophages via ROS/PI3K signaling-dependent various cytokine production to promote NSCLC growth. Redox Biol. 2019;22:101116.
Gu Z, Liu T, Liu C, Yang Y, Tang J, Song H, et al. Ferroptosis-strengthened metabolic and inflammatory regulation of tumor-associated macrophages provokes potent tumoricidal activities. Nano Lett. 2021;21:6471–9.
Wang W, Green M, Choi JE, Gijón M, Kennedy PD, Johnson JK, et al. CD8(+) T cells regulate tumour ferroptosis during cancer immunotherapy. Nature. 2019;569:270–4.
Liao P, Wang W, Wang W, Kryczek I, Li X, Bian Y, et al. CD8(+) T cells and fatty acids orchestrate tumor ferroptosis and immunity via ACSL4. Cancer Cell. 2022;40:365–78.e6.
Tang R, Xu J, Zhang B, Liu J, Liang C, Hua J, et al. Ferroptosis, necroptosis, and pyroptosis in anticancer immunity. J Hematol Oncol. 2020;13:110.
Friedmann Angeli JP, Xavier da Silva TN, Schilling B. CD8 T cells PUF(A)ing the flames of cancer ferroptotic cell death. Cancer Cell. 2022;40:346–8.
Ma X, Xiao L, Liu L, Ye L, Su P, Bi E, et al. CD36-mediated ferroptosis dampens intratumoral CD8 T cell effector function and impairs their antitumor ability. Cell Metabolism. 2021;33.
Xu S, Chaudhary O, Rodr¡guez-Morales P, Sun X, Chen D, Zappasodi R, et al. Uptake of oxidized lipids by the scavenger receptor CD36 promotes lipid peroxidation and dysfunction in CD8 T cells in tumors. Immunity. 2021;54:1561–77.e7.
Ma X, Xiao L, Liu L, ye L, Su P, Bi E, et al. CD36-mediated ferroptosis dampens intratumoral CD8+ T cell effector function and impairs their antitumor ability. Cell Metab. 2021;33:1001–12.e5.
Xu F, Guan Y, Xue L, Zhang P, Li M, Gao M, et al. The roles of ferroptosis regulatory gene SLC7A11 in renal cell carcinoma: a multi-omics study. Cancer Med. 2021;10:9078–96.
Lehrke MJ, Shapiro MJ, Rajcula MJ, Kennedy MM, McCue SA, Medina KL, et al. The mitochondrial iron transporter ABCB7 is required for B cell development, proliferation, and class switch recombination in mice. ELife. 2021;10:e69621.
Yee PP, Wei Y, Kim S-Y, Lu T, Chih SY, Lawson C, et al. Neutrophil-induced ferroptosis promotes tumor necrosis in glioblastoma progression. Nat Commun. 2020;11:5424.
Kirtonia A, Sethi G, Garg M. The multifaceted role of reactive oxygen species in tumorigenesis. Cell Mol Life Sci. 2020;77:4459–83.
Fukai T, Ushio-Fukai M. Cross-talk between NADPH oxidase and mitochondria: role in ROS signaling and angiogenesis. Cells. 2020;9:1849
Yang Y, Lin Z, Han Z, Wu Z, Hua J, Zhong R, et al. miR-539 activates the SAPK/JNK signaling pathway to promote ferropotosis in colorectal cancer by directly targeting TIPE. Cell Death Discov. 2021;7:272.
Zhong M, Li N, Qiu X, Ye Y, Chen H, Hua J, et al. TIPE regulates VEGFR2 expression and promotes angiogenesis in colorectal cancer. Int J Biol Sci. 2020;16:272–83.
Xu P, Wang Y, Deng Z, Tan Z, Pei X. MicroRNA-15a promotes prostate cancer cell ferroptosis by inhibiting GPX4 expression. Oncol Lett. 2022;23:67.
Liu L, Yao H, Zhou X, Chen J, Chen G, Shi X, et al. MiR-15a-3p regulates ferroptosis via targeting glutathione peroxidase GPX4 in colorectal cancer. Mol Carcinogenesis. 2022;61:301–10.
Xu Z, Chen L, Wang C, Zhang L, Xu W. MicroRNA-1287-5p promotes ferroptosis of osteosarcoma cells through inhibiting GPX4. Free Radic Res. 2021;55:1119–29.
Deng SH, Wu DM, Li L, Liu T, Zhang T, Li J, et al. miR-324-3p reverses cisplatin resistance by inducing GPX4-mediated ferroptosis in lung adenocarcinoma cell line A549. Biochem Biophys Res Commun. 2021;549:54–60.
Bai T, Liang R, Zhu R, Wang W, Zhou L, Sun Y. MicroRNA-214-3p enhances erastin-induced ferroptosis by targeting ATF4 in hepatoma cells. J Cell Physiol. 2020;235:5637–48.
Chen X, Li J, Kang R, Klionsky DJ, Tang D. Ferroptosis: machinery and regulation. Autophagy. 2021;17:2054–81.
Yadav P, Sharma P, Sundaram S, Venkatraman G, Bera AK, Karunagaran D. SLC7A11/ xCT is a target of miR-5096 and its restoration partially rescues miR-5096-mediated ferroptosis and anti-tumor effects in human breast cancer cells. Cancer Lett. 2021;522:211–24.
Lu X, Kang N, Ling X, Pan M, Du W, Gao S. MiR-27a-3p promotes non-small cell lung cancer through SLC7A11-mediated-ferroptosis. Front Oncol. 2021;11:759346.
Ni H, Qin H, Sun C, Liu Y, Ruan G, Guo Q, et al. MiR-375 reduces the stemness of gastric cancer cells through triggering ferroptosis. Stem Cell Res Ther. 2021;12:325.
Sun K, Ren W, Li S, Zheng J, Huang Y, Zhi K, et al. MiR-34c-3p upregulates erastin-induced ferroptosis to inhibit proliferation in oral squamous cell carcinomas by targeting SLC7A11. Pathol, Res Pract. 2022;231:153778.
Hu Z, Yin Y, Jiang J, Yan C, Wang Y, Wang D, et al. Exosomal miR-142-3p secreted by hepatitis B virus (HBV)-hepatocellular carcinoma (HCC) cells promotes ferroptosis of M1-type macrophages through SLC3A2 and the mechanism of HCC progression. J Gastrointest Oncol. 2022;13:754–67.
Luo M, Wu L, Zhang K, Wang H, Zhang T, Gutierrez L, et al. miR-137 regulates ferroptosis by targeting glutamine transporter SLC1A5 in melanoma. Cell Death Differ. 2018;25:1457–72.
Wang M, Mao C, Ouyang L, Liu Y, Lai W, Liu N, et al. Long noncoding RNA LINC00336 inhibits ferroptosis in lung cancer by functioning as a competing endogenous RNA. Cell Death Differ. 2019;26:2329–43.
Stockwell BR, Jiang X. The chemistry and biology of ferroptosis. Cell Chem Biol. 2020;27:365–75.
Babu KR, Muckenthaler MU. miR-148a regulates expression of the transferrin receptor 1 in hepatocellular carcinoma. Sci Rep. 2019;9:1518.
Fu Y, Lin L, Xia L. MiR-107 function as a tumor suppressor gene in colorectal cancer by targeting transferrin receptor 1. Cell Mol Biol Lett. 2019;24:31.
Cui P, Dai X, Liu R, Cao H. LncRNA LINC00888 upregulation predicts a worse survival of laryngeal cancer patients and accelerates the growth and mobility of laryngeal cancer cells through regulation of miR-378g/TFRC. J Biochem. Mol Toxicol. 2021;35:e22878.
Shi ZZ, Fan ZW, Chen YX, Xie XF, Jiang W, Wang WJ, et al. Ferroptosis in carcinoma: regulatory mechanisms and new method for cancer therapy. OncoTargets Ther. 2019;12:11291–304.
Zhang R, Pan T, Xiang Y, Zhang M, Xie H, Liang Z, et al. Curcumenol triggered ferroptosis in lung cancer cells via lncRNA H19/miR-19b-3p/FTH1 axis. Bioact Mater. 2022;13:23–36.
Xu P, Ge FH, Li WX, Xu Z, Wang XL, Shen JL, et al. MicroRNA-147a targets SLC40A1 to induce ferroptosis in human glioblastoma. Anal Cell Pathol. 2022;2022:2843990.
Wei D, Ke YQ, Duan P, Zhou L, Wang CY, Cao P. MicroRNA-302a-3p induces ferroptosis of non-small cell lung cancer cells via targeting ferroportin. Free Radic Res. 2021;55:821–30.
Zhu C, Song Z, Chen Z, Lin T, Lin H, Xu Z, et al. MicroRNA-4735-3p facilitates ferroptosis in clear cell renal cell carcinoma by targeting SLC40A1. Anal Cell Pathol. 2022;2022:4213401.
Kong Y, Hu L, Lu K, Wang Y, Xie Y, Gao L, et al. Ferroportin downregulation promotes cell proliferation by modulating the Nrf2-miR-17-5p axis in multiple myeloma. Cell Death Dis. 2019;10:624.
Su LJ, Zhang JH, Gomez H, Murugan R, Hong X, Xu D, et al. Reactive oxygen species-induced lipid peroxidation in apoptosis, autophagy, and ferroptosis. Oxid Med Cell Longev. 2019;2019:5080843.
Ma LL, Liang L, Zhou D, Wang SW. Tumor suppressor miR-424-5p abrogates ferroptosis in ovarian cancer through targeting ACSL4. Neoplasma. 2021;68:165–73.
Sun W, Wu X, Yu P, Zhang Q, Shen L, Chen J, et al. LncAABR07025387.1 enhances myocardial ischemia/reperfusion injury via miR-205/ACSL4-mediated ferroptosis. Front Cell Dev Biol. 2022;10:672391.
Bao C, Zhang J, Xian SY, Chen F. MicroRNA-670-3p suppresses ferroptosis of human glioblastoma cells through targeting ACSL4. Free Radic Res. 2021;55:853–64.
Lu Y, Chan YT, Tan HY, Zhang C, Guo W, Xu Y, et al. Epigenetic regulation of ferroptosis via ETS1/miR-23a-3p/ACSL4 axis mediates sorafenib resistance in human hepatocellular carcinoma. J Exp Clin Cancer Res. 2022;41:3.
Zhang H, Deng T, Liu R, Ning T, Yang H, Liu D, et al. CAF secreted miR-522 suppresses ferroptosis and promotes acquired chemo-resistance in gastric cancer. Mol Cancer. 2020;19:43.
Luo Y, Huang S, Wei J, Zhou H, Wang W, Yang J, et al. Long noncoding RNA LINC01606 protects colon cancer cells from ferroptotic cell death and promotes stemness by SCD1-Wnt/β-catenin-TFE3 feedback loop signalling. Clin Transl Med. 2022;12:e752.
Fan B, Chen LP, Yuan YH, Xiao HN, Lv XS, Xia ZY. MiR-15a-3p suppresses the growth and metastasis of ovarian cancer cell by targeting Twist1. Eur Rev Med Pharmacol Sci. 2019;23:1934–46.
Wang D, Wu W, Huang W, Wang J, Luo L, Tang D. LncRNA LUADT1 sponges miR-15a-3p to upregulate Twist1 in small cell lung cancer. BMC Pulm Med. 2019;19:246.
Wang T, Hou J, Li Z, Zheng Z, Wei J, Song D, et al. miR-15a-3p and miR-16-1-3p negatively regulate Twist1 to repress gastric cancer cell invasion and metastasis. Int J Biol Sci. 2017;13:122–34.
Wang J, Wang T, Zhang Y, Liu J, Song J, Han Y, et al. CPEB1 enhances erastin-induced ferroptosis in gastric cancer cells by suppressing twist1 expression. IUBMB Life. 2021;73:1180–90.
Cui Y, Yang Y, Ren L, Yang J, Wang B, Xing T, et al. miR-15a-3p suppresses prostate cancer cell proliferation and invasion by targeting SLC39A7 via downregulating Wnt/β-catenin signaling pathway. Cancer Biotherapy Radiopharmaceuticals. 2019;34:472–9.
Tanabe S, Quader S, Cabral H, Ono R. Interplay of EMT and CSC in cancer and the potential therapeutic strategies. Front Pharmacol. 2020;11:904.
Lu T, Yang Y, Li Z, Lu S. MicroRNA-214-3p inhibits the stem-like properties of lung squamous cell cancer by targeting YAP1. Cancer Cell Int. 2020;20:413.
Baroni S, Romero-Cordoba S, Plantamura I, Dugo M, D’Ippolito E, Cataldo A, et al. Exosome-mediated delivery of miR-9 induces cancer-associated fibroblast-like properties in human breast fibroblasts. Cell Death Dis. 2016;7:e2312.
Peng M, Ren J, Jing Y, Jiang X, Xiao Q, Huang J, et al. Tumour-derived small extracellular vesicles suppress CD8+ T cell immune function by inhibiting SLC6A8-mediated creatine import in NPM1-mutated acute myeloid leukaemia. J Extracell Vesicles. 2021;10:e12168.
Liu J, Fan L, Yu H, Zhang J, He Y, Feng D, et al. Endoplasmic reticulum stress causes liver cancer cells to release exosomal miR-23a-3p and up-regulate programmed death ligand 1 expression in macrophages. Hepatology. 2019;70:241–58.
Dastmalchi N, Hosseinpourfeizi MA, Khojasteh SMB, Baradaran B, Safaralizadeh R. Tumor suppressive activity of miR-424-5p in breast cancer cells through targeting PD-L1 and modulating PTEN/PI3K/AKT/mTOR signaling pathway. Life Sci. 2020;259:118239.
Yu Z, Zhao H, Feng X, Li H, Qiu C, Yi X, et al. Long non-coding RNA FENDRR acts as a miR-423-5p sponge to suppress the Treg-mediated immune escape of hepatocellular carcinoma cells. Mol Ther Nucleic Acids. 2019;17:516–29.
Yang Y, Wang Y, Guo L, Gao W, Tang TL, Yan M. Interaction between macrophages and ferroptosis. Cell Death Dis. 2022;13:355.
Liu G, Du X, Xiao L, Zeng Q, Liu Q. Activation of FGD5-AS1 promotes progression of cervical cancer through regulating BST2 to Inhibit macrophage M1 polarization. J Immunol Res. 2021;2021:5857214.
Song J, Xu X, He S, Wang N, Bai Y, Li B, et al. Exosomal hsa_circ_0017252 attenuates the development of gastric cancer via inhibiting macrophage M2 polarization. Hum Cell. 2022;35:1499–511.
Ma J, Kong FF, Yang D, Yang H, Wang C, Cong R, et al. lncRNA MIR210HG promotes the progression of endometrial cancer by sponging miR-337-3p/137 via the HMGA2-TGF-β/Wnt pathway. Mol Ther Nucleic Acids. 2021;24:905–22.
Han L, Wang W, Ding W, Zhang L. MiR-9 is involved in TGF-β1-induced lung cancer cell invasion and adhesion by targeting SOX7. J Cell Mol Med. 2017;21:2000–8.
Huang L, Wang X, Wen C, Yang X, Song M, Chen J, et al. Hsa-miR-19a is associated with lymph metastasis and mediates the TNF-α induced epithelial-to-mesenchymal transition in colorectal cancer. Sci Rep. 2015;5:13350.
Jiang Z, Wang H, Li Y, Hou Z, Ma N, Chen W, et al. MiR-129-5p is down-regulated and involved in migration and invasion of gastric cancer cells by targeting interleukin-8. Neoplasma. 2016;63:673–80.
Xiao FJ, Zhang D, Wu Y, Jia QH, Zhang L, Li YX, et al. miRNA-17-92 protects endothelial cells from erastin-induced ferroptosis through targeting the A20-ACSL4 axis. Biochem Biophys Res Commun. 2019;515:448–54.
Fang X, Cai Y, Xu Y, Zhang H. Exosome-mediated lncRNA SNHG11 regulates angiogenesis in pancreatic carcinoma through miR-324-3p/VEGFA axis. Cell Biol Int. 2022;46:106–17.
Chen X, Yang F, Zhang T, Wang W, Xi W, Li Y, et al. MiR-9 promotes tumorigenesis and angiogenesis and is activated by MYC and OCT4 in human glioma. J Exp Clin Cancer Res. 2019;38:99.
Shih TC, Tien YJ, Wen CJ, Yeh TS, Yu MC, Huang CH, et al. MicroRNA-214 downregulation contributes to tumor angiogenesis by inducing secretion of the hepatoma-derived growth factor in human hepatoma. J Hepatol. 2012;57:584–91.
Mirzaei HR, Sahebkar A, Mohammadi M, Yari R, Salehi H, Jafari MH, et al. Circulating microRNAs in Hepatocellular Carcinoma: Potential Diagnostic and Prognostic Biomarkers. Curr Pharm Des. 2016;22:5257–69.
Zhang X, Wang L, Li H, Zhang L, Zheng X, Cheng W. Crosstalk between noncoding RNAs and ferroptosis: new dawn for overcoming cancer progression. Cell Death Dis. 2020;11:580.
Dai SM, Li FJ, Long HZ, Zhou ZW, Luo HY, Xu SG, et al. Relationship between miRNA and ferroptosis in tumors. Front Pharmacol. 2022;13:977062.
Chen M, Wu J, Luo Q, Mo S, Lyu Y, Wei Y, et al. The anticancer properties of herba epimedii and its main bioactive componentsicariin and icariside II. Nutrients. 2016;8:563.
Yu R, Zhou Y, Shi S, Wang X, Huang S, Ren Y. Icariside II induces ferroptosis in renal cell carcinoma cells by regulating the miR-324-3p/GPX4 axis. Phytomedicine: Int J Phytother Phytopharmacol. 2022;102:154182.
He GN, Bao NR, Wang S, Xi M, Zhang TH, Chen FS. Ketamine induces ferroptosis of liver cancer cells by targeting lncRNA PVT1/miR-214-3p/GPX4. Drug Des, Dev Ther. 2021;15:3965–78.
Luo Y, Niu G, Yi H, Li Q, Wu Z, Wang J, et al. Nanomedicine promotes ferroptosis to inhibit tumour proliferation in vivo. Redox Biol. 2021;42:101908.
Zhang K, Wu L, Zhang P, Luo M, Du J, Gao T, et al. miR-9 regulates ferroptosis by targeting glutamic-oxaloacetic transaminase GOT1 in melanoma. Mol Carcinogenesis. 2018;57:1566–76.
Liao Y, Jia X, Ren Y, Deji Z, Gesang Y, Ning N, et al. Suppressive role of microRNA-130b-3p in ferroptosis in melanoma cells correlates with DKK1 inhibition and Nrf2-HO-1 pathway activation. Hum Cell. 2021;34:1532–44.
Fan H, Ai R, Mu S, Niu X, Guo Z, Liu L. MiR-19a suppresses ferroptosis of colorectal cancer cells by targeting IREB2. Bioengineered. 2022;13:12021–9.
Luo W, Wang J, Xu W, Ma C, Wan F, Huang Y, et al. LncRNA RP11-89 facilitates tumorigenesis and ferroptosis resistance through PROM2-activated iron export by sponging miR-129-5p in bladder cancer. Cell Death Dis. 2021;12:1043.
Song Z, Jia G, Ma P, Cang S. Exosomal miR-4443 promotes cisplatin resistance in non-small cell lung carcinoma by regulating FSP1 m6A modification-mediated ferroptosis. Life Sci. 2021;276:119399.
Jiang X, Yuan Y, Tang L, Wang J, Zhang D, Duan L. Systematic analysis and validation of the prognosis, immunological role and biology function of the ferroptosis-related lncRNA GSEC/miRNA-101-3p/CISD1 axis in lung adenocarcinoma. Front Mol Biosci. 2021;8:793732.
Salah A, Wang H, Li Y, Ji M, Ou W-B, Qi N. Insights into dendritic cells in cancer immunotherapy: from bench to clinical applications. Front Cell Dev Biol. 2021;9:1422.
Liu C, Li G, Yang N, Su Z, Zhang S, Deng T, et al. miR-324-3p suppresses migration and invasion by targeting WNT2B in nasopharyngeal carcinoma. Cancer Cell Int. 2017;17:2.
Sun GL, Li Z, Wang WZ, Chen Z, Zhang L, Li Q, et al. miR-324-3p promotes gastric cancer development by activating Smad4-mediated Wnt/beta-catenin signaling pathway. J Gastroenterol. 2018;53:725–39.
Qi W, Chen J, Cheng X, Huang J, Xiang T, Li Q, et al. Targeting the Wnt-regulatory protein CTNNBIP1 by microRNA-214 enhances the stemness and self-renewal of cancer stem-like cells in lung adenocarcinomas. Stem Cells. 2015;33:3423–36.
He Z, Guo X, Tian S, Zhu C, Chen S, Yu C, et al. MicroRNA-137 reduces stemness features of pancreatic cancer cells by targeting KLF12. J Exp Clin Cancer Res. 2019;38:126.
Shui Y, Yu X, Duan R, Bao Q, Wu J, Yuan H, et al. miR-130b-3p inhibits cell invasion and migration by targeting the Notch ligand Delta-like 1 in breast carcinoma. Gene. 2017;609:80–7.
Doğanlar O, Doğanlar ZB, Delen E, Doğan A. The role of melatonin in angio-miR-associated inhibition of tumorigenesis and invasion in human glioblastoma tumour spheroids. Tissue Cell. 2021;73:101617.
Bonafé GA, Dos Santos JS, Ziegler JV, Marson FAL, Rocha T, Ortega MM. Dipotassium glycyrrhizinate on melanoma cell line: inhibition of cerebral metastases formation by targeting NF-kB genes-mediating microRNA-4443 and microRNA-3620-dipotassium Glycyrrhizinate Effect on melanoma. Int J Mol Sci. 2022;23:7251.
Long J, Menggen Q, Wuren Q, Shi Q, Pi X. Long noncoding RNA taurine-upregulated gene1 (TUG1) promotes tumor growth and metastasis through TUG1/Mir-129-5p/astrocyte-elevated gene-1 (AEG-1) axis in malignant melanoma. Med Sci Monit. 2018;24:1547–59.
Zhang Y, Wang S, Lai Q, Fang Y, Wu C, Liu Y, et al. Cancer-associated fibroblasts-d erived exosomal miR-17-5p promotes colorectal cancer aggressive phenotype by initiating a RUNX3/MYC/TGF-β1 positive feedback loop. Cancer Lett. 2020;491:22–35.
Lu Y, Luan XR. miR-147a suppresses the metastasis of non-small-cell lung cancer by targeting CCL5. J Int Med Res. 2020;48:300060519883098.
Zeng A, Yin J, Wang Z, Zhang C, Li R, Zhang Z, et al. miR-17-5p-CXCL14 axis related transcriptome profile and clinical outcome in diffuse gliomas. Oncoimmunology. 2018;7:e1510277.
Srivastava A, Goldberger H, Dimtchev A, Ramalinga M, Chijioke J, Marian C, et al. MicroRNA profiling in prostate cancer-the diagnostic potential of urinary miR-205 and miR-214. PLoS ONE. 2013;8:e76994.
Lyu J, Zhao L, Wang F, Ji J, Cao Z, Xu H, et al. Discovery and validation of serum microRNAs as early diagnostic biomarkers for prostate cancer in Chinese population. BioMed Res Int. 2019;2019:9306803.
Xu X, Lu J, Wang F, Liu X, Peng X, Yu B, et al. Dynamic changes in plasma microRNAs have potential predictive values in monitoring recurrence and metastasis of nasopharyngeal carcinoma. BioMed Res Int. 2018;2018:7329195.
Fan B, Shen C, Wu M, Zhao J, Guo Q, Luo Y. miR-17-92 cluster is connected with disease progression and oxaliplatin/capecitabine chemotherapy efficacy in advanced gastric cancer patients: a preliminary study. Medicine. 2018;97:e12007.
Zhang W, Fu T, Guo Z, Zhang Y, Zhang L, Su H, et al. Serum miR-375 levels are closely related to disease progression from HBV infection to HBV-related hepatocellular carcinoma. BioMed Res Int. 2020;2020:5819385.
Wen Y, Han J, Chen J, Dong J, Xia Y, Liu J, et al. Plasma miRNAs as early biomarkers for detecting hepatocellular carcinoma. Int J Cancer. 2015;137:1679–90.
Dai X, Chiang Y, Wang Z, Song Y, Lu C, Gao P, et al. Expression levels of microRNA-375 in colorectal carcinoma. Mol Med Rep. 2012;5:1299–304.
Visani M, de Biase D, Marucci G, Cerasoli S, Nigrisoli E, Bacchi Reggiani ML, et al. Expression of 19 microRNAs in glioblastoma and comparison with other brain neoplasia of grades I-III. Mol Oncol. 2014;8:417–30.
Guo W, Wu Z, Chen J, Guo S, You W, Wang S. et al. Nanoparticle delivery of miR-21-3p sensitizes melanoma to anti-PD-1 immunotherapy by promoting ferroptosis. J Immunotherapy Cancer. 2022;10:e004381.
Han B, Liu Y, Zhang Q, Liang L. Propofol decreases cisplatin resistance of non-small cell lung cancer by inducing GPX4-mediated ferroptosis through the miR-744-5p/miR-615-3p axis. J Proteom. 2022;274:104777.
Funding
This work was partially supported by the National Natural Science Foundation of China (No. 81602167), the Hunan Provincial Natural Science Foundation of China (No. 2017JJ3494 and 2021JJ31100), and the Science and Technology Program Foundation of Changsha City (No. kq2004085).
Author information
Authors and Affiliations
Contributions
ZJ and JZ wrote the manuscript and drew the figures. LL, DJ, and WR collected the related papers, HY, PL, TR, and WD created the Tables, HT, JZ, and YY helped to revise the manuscript. ZZ, LJ, DO, and WJ designed and revised the manuscript. All the authors read and approved the final version of the review.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Consent for publication
All authors approved the final manuscript and the submission to this journal.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Jiang, Z., Zhou, J., Deng, J. et al. Emerging roles of ferroptosis-related miRNAs in tumor metastasis. Cell Death Discov. 9, 193 (2023). https://doi.org/10.1038/s41420-023-01486-y
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41420-023-01486-y