Abstract
Background
Weight cycling is the repeated episodes manifesting intentional weight loss and subsequent unintentional weight gain. Whether the frequency and magnitude of weight cycling is associated with colorectal cancer risk independent of body mass index (BMI) remains unknown.
Methods
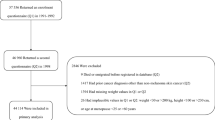
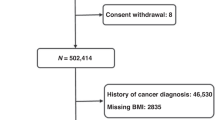
Two prospective cohort studies, Nurses’ Health Study I and Health Professionals Follow-up Study, followed 85,562 participants from 1992 to 2014. Participants completed a questionnaire regarding the frequency and magnitude of intentional weight loss in the past 4 years at the baseline. Hazard ratios (HRs) and 95% confidence intervals (CIs) were estimated using Cox proportional hazard model.
Results
We identified 1626 colorectal cancer cases during up to 22 years of follow-up. In the pooled analysis of HPFS and NHS, compared to non-weight cycling, moderate weight cycling (≥3 times of intentional weight loss of ≥2.3–4.4 kg) was associated with a reduced risk of colorectal cancer after adjustment for confounders, including attained BMI after weight cycling (HR = 0.82, 95% CI 0.69, 0.97). However, no significant association was observed in mild weight cyclers and in severe weight cyclers.
Conclusions
Moderate weight cycling was associated with a lower risk of colorectal cancer independent of BMI. This finding needs further studies for replication and putative biological mechanisms.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
The data underlying this article cannot be shared for the privacy of individuals who participated in Nurses’ Health Study I and Health Professionals Follow-up study.
Code availability
Codes are not shared.
References
Fryar CD, Carroll MD, Afful J. Prevalence of overweight, obesity, and severe obesity among adults aged 20 and over: United States, 1960–1962 through 2017–2018. NCHS Health E-Stats. 2020.
Lobstein T, Brinsden H, Neveux M. World Obesity Atlas 2022; World Obesity Federation: London, UK, 2022.
Yaemsiri S, Slining MM, Agarwal SK. Perceived weight status, overweight diagnosis, and weight control among US adults: the NHANES 2003–2008 Study. Int J Obes. 2011;35:1063–70.
Kraschnewski J, Boan J, Esposito J, Sherwood N, Lehman E, Kephart D, et al. Long-term weight loss maintenance in the United States. Int J Obes. 2010;34:1644–54.
Stevens VL, Jacobs EJ, Patel AV, Sun J, McCullough ML, Campbell PT, et al. Weight cycling and cancer incidence in a large prospective US cohort. Am J Epidemiol. 2015;182:394–404.
Thompson HJ, McTiernan A. Weight cycling and cancer: weighing the evidence of intermittent caloric restriction and cancer risk. Cancer Prev Res. 2011;4:1736–42.
Stevens VL, Jacobs EJ, Sun J, Patel AV, McCullough ML, Teras LR, et al. Weight cycling and mortality in a large prospective US study. Am J Epidemiol. 2012;175:785–92.
Morois S, Mesrine S, Josset M, Clavel-Chapelon F, Boutron-Ruault MC. Anthropometric factors in adulthood and risk of colorectal adenomas. Am J Epidemiol. 2010;172:1166–80.
Colditz GA, Manson JE, Hankinson SE. The Nurses’ Health Study: 20-year contribution to the understanding of health among women. J Women’s Health. 1997;6:49–62.
Rimm EB, Giovannucci EL, Willett WC, Colditz GA, Ascherio A, Rosner B, et al. Prospective study of alcohol consumption and risk of coronary disease in men. Lancet. 1991;338:464–8.
Lee DH, Keum NN, Rezende LFM, Tabung FK, Hong SE, Giovannucci EL. Association between weight cycling and risk of kidney cancer: a prospective cohort study and meta-analysis of observational studies. Cancer Causes Control. 2021;32:1029–38.
Field AE, Malspeis S, Willett WC. Weight cycling and mortality among middle-aged or older women. Arch Intern Med. 2009;169:881–6.
Nurses’ Health Study. NHS Questionnaire 1992 (long). 2023. https://nurseshealthstudy.org/participants/questionnaires.
Health Professionals Follow-Up Study. HPFS Questionnaire 1992 (long). 2023. https://www.hsph.harvard.edu/hpfs/hpfs-questionnaires/.
World Cancer Research Fund/American Institute for Cancer Research. World Cancer Research Fund international systematic literature review: the associations between food, nutrition and physical activity and the risk of colorectal cancer. World Cancer Research Fund; 2017. https://www.wcrf.org/sites/default/files/colorectal-cancer-slr.pdf.
U.S. Cancer Statistics Working Group. Cancer Statistics Data Visualizations Tool, based on 2022 submission data (1999–2020): U.S. Department of Health and Human Services, Centers for Disease Control and Prevention and National Cancer Institute; 2023. https://www.cdc.gov/cancer/dataviz.
Butterworth AS, Higgins JPT, Pharoah P. Relative and absolute risk of colorectal cancer for individuals with a family history: a meta-analysis. Eur J Cancer. 2006;42:216–27.
PDQ Screening and Prevention Editorial Board. Colorectal Cancer Screening (PDQ®): Health Professional Version. In: PDQ Cancer Information Summaries. Bethesda: National Cancer Institute (US); 2002. https://www.ncbi.nlm.nih.gov/books/NBK65825/.
Liang PS, Chen TY, Giovannucci E. Cigarette smoking and colorectal cancer incidence and mortality: systematic review and meta-analysis. Int J Cancer. 2009;124:2406–15.
Rothwell PM, Wilson M, Elwin CE, Norrving B, Algra A, Warlow CP, et al. Long-term effect of aspirin on colorectal cancer incidence and mortality: 20-year follow-up of five randomised trials. Lancet. 2010;376:1741–50.
Sun Z, Liu L, Wang PP, Roebothan B, Zhao J, Dicks E, et al. Association of total energy intake and macronutrient consumption with colorectal cancer risk: results from a large population-based case-control study in Newfoundland and Labrador and Ontario, Canada. Nutr J. 2012;11:18.
Steck SE, Guinter M, Zheng J, Thomson CA. Index-based dietary patterns and colorectal cancer risk: a systematic review. Adv Nutr. 2015;6:763–73.
Zervoudakis A, Strickler HD, Park Y, Xue X, Hollenbeck A, Schatzkin A, et al. Reproductive history and risk of colorectal cancer in postmenopausal women. J Natl Cancer Inst. 2011;103:826–34.
Mackie GM, Samocha-Bonet D, Tam CS. Does weight cycling promote obesity and metabolic risk factors? Obes Res Clin Pract. 2016;11:131–9.
Carey KJ, Vitek W. Weight cycling in women: adaptation or risk? Semin Reprod Med. 2022;40:277–82.
Trentham-Dietz A, Nichols HB, Hampton JM, Newcomb PA. Weight change and risk of endometrial cancer. Int J Epidemiol. 2006;35:151–8.
Schwalb ME, Smith-Warner SA, Hou J, Rohan TE, Snetselaar L, Luo J, et al. Sustained weight loss, weight cycling, and weight gain during adulthood and pancreatic cancer incidence in the Women’s Health Initiative. Am J Epidemiol. 2022;191:1009–20.
Yokomichi H, Ohde S, Takahashi O, Mochizuki M, Takahashi A, Yoda Y, et al. Weight cycling and the subsequent onset of type 2 diabetes mellitus: 10-year cohort studies in urban and rural Japan. BMJ Open. 2017;7:e014684.
Jeffery RW, Wing RR, French SA. Weight cycling and cardiovascular risk factors in obese men and women. Am J Clin Nutr. 1992;55:641–4.
Bairey Merz CN, Olson MB, Kelsey SF, Bittner V, Reis SE, Reichek N, et al. Weight cycling and cardiovascular outcome in women with suspected ischemia: a report from the NHLBI-sponsored WISE Study. PLoS ONE. 2018;13:e0207223.
Premoselli F, Sesca E, Binasco V, Caderni G, Tessitore L. Fasting/re-feeding before initiation enhances the growth of aberrant crypt foci induced by azoxymethane in rat colon and rectum. Int J Cancer. 1998;77:286–94.
Guffey CR, Fan D, Singh UP, Murphy EA. Linking obesity to colorectal cancer: recent insights into plausible biological mechanisms. Curr Opin Clin Nutr Metab Care. 2013;16:595–600.
Vargas AJ, Quackenbush J, Glass K. Diet-induced weight loss leads to a switch in gene regulatory network control in the rectal mucosa. Genomics. 2016;108:126–33.
Byers T, Sedjo RL. Does intentional weight loss reduce cancer risk? Diabetes Obes Metab. 2011;13:1063–72.
Lakhdar N, Denguezli M, Zaouali M, Zbidi A, Tabka Z, Bouassida A. Diet and diet combined with chronic aerobic exercise decreases body fat mass and alters plasma and adipose tissue inflammatory markers in obese women. Inflammation. 2013;36:1239–47.
Nicklas BJ, Ambrosius W, Messier SP, Miller GD, Penninx BWJH, Loeser RF, et al. Diet-induced weight loss, exercise, and chronic inflammation in older, obese adults: a randomized controlled clinical trial. Am J Clin Nutr. 2004;79:544–51.
Pendyala S, Neff LM, Suárez-Fariñas M, Holt PR. Diet-induced weight loss reduces colorectal inflammation: implications for colorectal carcinogenesis. Am J Clin Nutr. 2011;93:234–42.
Breininger SP, Malcomson FC, Afshar S, Turnbull DM, Greaves L, Mathers JC. Effects of obesity and weight loss on mitochondrial structure and function and implications for colorectal cancer risk. In: Proceedings of the Nutrition Society. Cambridge University Press; 2019. p. 426–37.
Beeken RJ, Croker H, Heinrich M, Obichere A, Finer N, Murphy N, et al. The impact of diet-induced weight loss on biomarkers for colorectal cancer: an exploratory study (INTERCEPT). Obesity. 2017;25:S95–101.
Field AE, Manson JE, Laird N, Williamson DF, Willett WC, Colditz GA. Weight cycling and the risk of developing type 2 diabetes among adult women in the United States. Obes Res. 2004;12:267–74.
Marinac CR, Suppan CA, Giovannucci E, Song M, Kværner AS, Townsend MK, et al. Elucidating under-studied aspects of the link between obesity and multiple myeloma: weight pattern, body shape trajectory, and body fat distribution. JNCI Cancer Spectr. 2019;3:pkz044.
Rimm EB, Stampfer MJ, Colditz GA, Chute CG, Litin LB, Willett WC. Validity of self-reported waist and hip circumferences in men and women. Epidemiology. 1990;1:466–73.
Acknowledgements
The authors would like to acknowledge the contribution to this study from the Channing Division of Network Medicine, Department of Medicine, Brigham and Women’s Hospital and central cancer registries supported through the Centers for Disease Control and Prevention’s National Program of Cancer Registries (NPCR) and/or the National Cancer Institute’s Surveillance, Epidemiology, and End Results (SEER) Program. Central registries may also be supported by state agencies, universities, and cancer centres. Participating central cancer registries include the following: Alabama, Alaska, Arizona, Arkansas, California, Colorado, Connecticut, Delaware, Florida, Georgia, Hawaii, Idaho, Indiana, Iowa, Kentucky, Louisiana, Massachusetts, Maine, Maryland, Michigan, Mississippi, Montana, Nebraska, Nevada, New Hampshire, New Jersey, New Mexico, New York, North Carolina, North Dakota, Ohio, Oklahoma, Oregon, Pennsylvania, Puerto Rico, Rhode Island, Seattle SEER Registry, South Carolina, Tennessee, Texas, Utah, Virginia, West Virginia, Wyoming.
Funding
The Nurses’ Health Study I was funded by the National Cancer Institute, National Institutes of Health (UM1 CA176726, P01 CA87969) Health Professionals Follow-up Study was funded by the National Cancer Institute, National Institutes of Health (U01 CA167552). This work was funded by the National Institutes of Health (R03 CA204825) and the Yonsei University Research Grant of 2023-22-0351.
Author information
Authors and Affiliations
Contributions
DHL, NK and ELG conceived and designed the study. DHL conducted data analyses. SK prepared the first draft. DHL, NK and ELG aided in interpreting the results. All authors contributed to the critical revision of the manuscript for important intellectual content. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
The protocol of this study was approved by the institutional review boards of Harvard T.H. Chan School of Public Health, the Brigham and Women’s Hospital, Boston, USA, and those of participating registries according to need. Completion of the questionnaire was considered to imply informed consent.
Consent for publication
Not applicable.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kim, S., Lee, D.H., Giovannucci, E.L. et al. Association between weight cycling and risk of colorectal cancer: a prospective cohort study. Br J Cancer 130, 496–503 (2024). https://doi.org/10.1038/s41416-023-02529-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41416-023-02529-y