Abstract
Background
The prognosis for high-risk childhood acute leukaemias remains dismal and established treatment protocols often cause long-term side effects in survivors. This study aims to identify more effective and safer therapeutics for these patients.
Methods
A high-throughput phenotypic screen of a library of 3707 approved drugs and pharmacologically active compounds was performed to identify compounds with selective cytotoxicity against leukaemia cells followed by further preclinical evaluation in patient-derived xenograft models.
Results
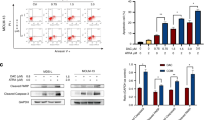
Auranofin, an FDA-approved agent for the treatment of rheumatoid arthritis, was identified as exerting selective anti-cancer activity against leukaemia cells, including patient-derived xenograft cells from children with high-risk ALL, versus solid tumour and non-cancerous cells. It induced apoptosis in leukaemia cells by increasing reactive oxygen species (ROS) and potentiated the activity of the chemotherapeutic cytarabine against highly aggressive models of infant MLL-rearranged ALL by enhancing DNA damage accumulation. The enhanced sensitivity of leukaemia cells towards auranofin was associated with lower basal levels of the antioxidant glutathione and higher baseline ROS levels compared to solid tumour cells.
Conclusions
Our study highlights auranofin as a well-tolerated drug candidate for high-risk paediatric leukaemias that warrants further preclinical investigation for application in high-risk paediatric and adult acute leukaemias.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Pui, C. H. in Childhood Leukemias. 3rd edn, Chapter 13, Acute lymphoblastic leukemia, 332–366 (Cambridge University Press, 2012).
Pui, C. H., Yang, J. J., Hunger, S. P., Pieters, R., Schrappe, M., Biondi, A. et al. Childhood acute lymphoblastic leukemia: progress through collaboration. J. Clin. Oncol. 33, 2938–2948 (2015).
Coustan-Smith, E., Mullighan, C. G., Onciu, M., Behm, F. G., Raimondi, S. C., Pei, D. et al. Early T-cell precursor leukaemia: a subtype of very high-risk acute lymphoblastic leukaemia. Lancet Oncol. 10, 147–156 (2009).
Boer, J. M. & den Boer, M. L. BCR-ABL1-like acute lymphoblastic leukaemia: from bench to bedside. Eur. J. Cancer 82, 203–218 (2017).
Adams, M. J. & Lipshultz, S. E. Pathophysiology of anthracycline- and radiation-associated cardiomyopathies: implications for screening and prevention. Pediatr. Blood Cancer 44, 600–606 (2005).
Ness, K. K., Armenian, S. H., Kadan-Lottick, N. & Gurney, J. G. Adverse effects of treatment in childhood acute lymphoblastic leukemia: general overview and implications for long-term cardiac health. Expert Rev. Hematol. 4, 185–197 (2011).
Green, D. M., Kawashima, T., Stovall, M., Leisenring, W., Sklar, C. A., Mertens, A. C. et al. Fertility of female survivors of childhood cancer: a report from the childhood cancer survivor study. J. Clin. Oncol. 27, 2677–2685 (2009).
Green, D. M., Kawashima, T., Stovall, M., Leisenring, W., Sklar, C. A., Mertens, A. C. et al. Fertility of male survivors of childhood cancer: a report from the Childhood Cancer Survivor Study. J. Clin. Oncol. 28, 332–339 (2010).
Mody, R., Li, S., Dover, D. C., Sallan, S., Leisenring, W., Oeffinger, K. C. et al. Twenty-five-year follow-up among survivors of childhood acute lymphoblastic leukemia: a report from the Childhood Cancer Survivor Study. Blood 111, 5515–5523 (2008).
Robison, L. L. Late effects of acute lymphoblastic leukemia therapy in patients diagnosed at 0–20 years of age. Hematology Am. Soc. Hematol. Educ. Program 2011, 238–242 (2011).
Pieters, R., Schrappe, M., De Lorenzo, P., Hann, I., De Rossi, G., Felice, M. et al. A treatment protocol for infants younger than 1 year with acute lymphoblastic leukaemia (Interfant-99): an observational study and a multicentre randomised trial. Lancet 370, 240–250 (2007).
Kotecha, R. S., Gottardo, N. G., Kees, U. R. & Cole, C. H. The evolution of clinical trials for infant acute lymphoblastic leukemia. Blood Cancer J. 4, e200 (2014).
Li, Y. Y. & Jones, S. J. Drug repositioning for personalized medicine. Genome Med. 4, 27 (2012).
Ashburn, T. T. & Thor, K. B. Drug repositioning: identifying and developing new uses for existing drugs. Nat. Rev. Drug Disco. 3, 673–683 (2004).
Somers, K., Chudakova, D. A., Middlemiss, S. M. C., Wen, V. W., Clifton, M., Kwek, A. et al. CCI-007, a novel small molecule with cytotoxic activity against infant leukemia with MLL rearrangements. Oncotarget 7, 46067–46087 (2016).
Khaw, S. L., Suryani, S., Evans, K., Richmond, J., Robbins, A., Kurmasheva, R. T. et al. Venetoclax responses of pediatric ALL xenografts reveal sensitivity of MLL-rearranged leukemia. Blood 128, 1382–1395 (2016).
Somers, K., Wen, V. W., Middlemiss, S. M. C., Osborne, B., Forgham, H., Jung, M. et al. A novel small molecule that kills a subset of MLL-rearranged leukemia cells by inducing mitochondrial dysfunction. Oncogene 38, 3824–3842 (2019).
Bliss, C. I. The calculation of microbial assays. Bacteriol. Rev. 20, 243–258 (1956).
Zhao, W., Sachsenmeier, K., Zhang, L., Sult, E., Hollingsworth, R. E. & Yang, H. A new bliss independence model to analyze drug combination data. J. Biomol. Screen 19, 817–821 (2014).
Goswami, C. P., Cheng, L., Alexander, P. S., Singal, A. & Li, L. A new drug combinatory effect prediction algorithm on the cancer cell based on gene expression and dose-response curve. Pharmacomet. Syst. Pharm. 4, e9 (2015).
Di Veroli, G. Y., Fornari, C., Wang, D., Mollard, S., Bramhall, J. L., Richards, F. M. et al. Combenefit: an interactive platform for the analysis and visualization of drug combinations. Bioinformatics 32, 2866–2868 (2016).
Rahman, I., Kode, A. & Biswas, S. K. Assay for quantitative determination of glutathione and glutathione disulfide levels using enzymatic recycling method. Nat. Protoc. 1, 3159–3165 (2006).
Gana, C. C., Hanssen, K. M., Yu, D. M. T., Flemming, C. L., Wheatley, M. S., Conseil, G. et al. MRP1 modulators synergize with buthionine sulfoximine to exploit collateral sensitivity and selectively kill MRP1-expressing cancer cells. Biochem Pharm. 168, 237–248 (2019).
Somers, K., Evans, K., Cheung, L., Karsa, M., Pritchard, T., Kosciolek, A. et al. Effective targeting of NAMPT in patient-derived xenograft models of high-risk pediatric acute lymphoblastic leukemia. Leukemia. 34, 1524–1539 (2020).
Richmond, J., Carol, H., Evans, K., High, L., Mendomo, A., Robbins, A. et al. Effective targeting of the P53-MDM2 axis in preclinical models of infant MLL-rearranged acute lymphoblastic leukemia. Clin. Cancer Res. 21, 1395–1405 (2015).
Kees, U. R., Ford, J., Watson, M., Murch, A., Ringńer, M., Walker, R. J. et al. Gene expression profiles in a panel of childhood leukemia cell lines mirror critical features of the disease. Mol. Cancer Ther. 2, 671–677 (2003).
Saletta, F., Wadham, C., Ziegler, D. S., Marshall, G. M., Haber, M., McCowage, G. et al. Molecular profiling of childhood cancer: Biomarkers and novel therapies. BBA Clin. 1, 59–77 (2014).
Brown, P. Treatment of infant leukemias: challenge and promise. Hematology Am. Soc. Hematol. Educ. Program 2013, 596–600 (2013).
Parker, C., Waters, R., Leighton, C., Hancock, J., Sutton, R., Moorman, A. V. et al. Effect of mitoxantrone on outcome of children with first relapse of acute lymphoblastic leukaemia (ALL R3): an open-label randomised trial. Lancet 376, 2009–2017 (2011).
Burkhardt, B., Mueller, S., Khanam, T. & Perkins, S. L. Current status and future directions of T-lymphoblastic lymphoma in children and adolescents. Br. J. Haematol. 173, 545–559 (2016).
Kuhlen, M., Klusmann, J.-H. & Hoell, J. I. Molecular approaches to treating pediatric leukemias. Front Pediatr. 7, 356 (2019).
Hijiya, N., Stewart, C. F., Zhou, Y., Campana, D., Coustan-Smith, E., Rivera, G. K. et al. Phase II study of topotecan in combination with dexamethasone, asparaginase, and vincristine in pediatric patients with acute lymphoblastic leukemia in first relapse. Cancer 112, 1983–1991 (2008).
Conticello, C., Martinetti, D., Adamo, L., Buccheri, S., Giuffrida, R., Parrinello, N. et al. Disulfiram, an old drug with new potential therapeutic uses for human hematological malignancies. Int. J. Cancer 131, 2197–2203 (2012).
Deng, M., Jiang, Z., Li, Y., Zhou, Y., Li, J., Wang, X. et al. Effective elimination of adult B-lineage acute lymphoblastic leukemia by disulfiram/copper complex in vitro and in vivo in patient-derived xenograft models. Oncotarget 7, 82200–82212 (2016).
Fiskus, W., Saba, N., Shen, M., Ghias, M., Liu, J., Gupta, S. D. et al. Auranofin induces lethal oxidative and endoplasmic reticulum stress and exerts potent preclinical activity against chronic lymphocytic leukemia. Cancer Res 74, 2520–2532 (2014).
Hwang-Bo, H., Jeong, J. W., Han, M. H., Park, C., Hong, S. H., Kim, G. Y. et al. Auranofin, an inhibitor of thioredoxin reductase, induces apoptosis in hepatocellular carcinoma Hep3B cells by generation of reactive oxygen species. Gen. Physiol. Biophys. 36, 117–128 (2017).
Zitka, O., Skalickova, S., Gumulec, J., Masarik, M., Adam, V., Hubalek, J. et al. Redox status expressed as GSH:GSSG ratio as a marker for oxidative stress in paediatric tumour patients. Oncol. Lett. 4, 1247–1253 (2012).
Lock, R. B., Liem, N., Farnsworth, M. L., Milross, C. G., Xue, C., Tajbakhsh, M. et al. The nonobese diabetic/severe combined immunodeficient (NOD/SCID) mouse model of childhood acute lymphoblastic leukemia reveals intrinsic differences in biologic characteristics at diagnosis and relapse. Blood 99, 4100–4108 (2002).
Liem, N. L., Papa, R. A., Milross, C. G., Schmid, M. A., Tajbakhsh, M., Choi, S. et al. Characterization of childhood acute lymphoblastic leukemia xenograft models for the preclinical evaluation of new therapies. Blood 103, 3905–3914 (2004).
Geller, H. M., Cheng, K. Y., Goldsmith, N. K., Romero, A. A., Zhang, A. L., Morris, E. J. et al. Oxidative stress mediates neuronal DNA damage and apoptosis in response to cytosine arabinoside. J. Neurochem 78, 265–275 (2001).
Houghton, P. J., Morton, C. I., Gorlick, R., Lock, R. B., Carol, H., Reynolds, C. P. et al. Stage 2 combination testing of rapamycin with cytotoxic agents by the Pediatric preclinical testing program. Mol. Cancer Ther. 9, 101–112 (2010).
Cruickshank, M. N., Ford, J., Cheung, L. C., Heng, J., Singh, S., Wells, J. et al. Systematic chemical and molecular profiling of MLL-rearranged infant acute lymphoblastic leukemia reveals efficacy of romidepsin. Leukemia 31, 40–50 (2017).
Furst, D. E. Mechanism of action, pharmacology, clinical efficacy and side effects of auranofin. An orally administered organic gold compound for the treatment of rheumatoid arthritis. Pharmacotherapy 3, 284–298 (1983).
Roder, C. & Thomson, M. J. Auranofin: repurposing an old drug for a golden new age. Drugs R. D. 15, 13–20 (2015).
Kean, W. F. & Kean, I. R. Clinical pharmacology of gold. Inflammopharmacology 16, 112–125 (2008).
Liu, N., Li, X., Huang, H., Zhao, C., Liao, S., Yang, C. et al. Clinically used antirheumatic agent auranofin is a proteasomal deubiquitinase inhibitor and inhibits tumor growth. Oncotarget 5, 5453–5471 (2014).
Hrabe, J. E., O’Leary, B. R., Fath, M. A., Rodman, S. N., Button, A. M., Domann, F. E. et al. Disruption of thioredoxin metabolism enhances the toxicity of transforming growth factor β-activated kinase 1 (TAK1) inhibition in KRAS-mutated colon cancer cells. Redox Biol. 5, 319–327 (2015).
Fan, C., Zheng, W., Fu, X., Li, X., Wong, Y. S. & Chen, T. Enhancement of auranofin-induced lung cancer cell apoptosis by selenocystine, a natural inhibitor of TrxR1 in vitro and in vivo. Cell Death Dis. 5, e1191 (2014).
Simon, T. M., Kunishima, D. H., Vibert, G. J. & Lorber, A. Screening trial with the coordinated gold compound auranofin using mouse lymphocyte leukemia P388. Cancer Res 41, 94–97 (1981).
Chen, X., Shi, X., Zhao, C., Li, X., Lan, X., Liu, S. et al. Anti-rheumatic agent auranofin induced apoptosis in chronic myeloid leukemia cells resistant to imatinib through both Bcr/Abl-dependent and -independent mechanisms. Oncotarget 5, 9118–9132 (2014).
Lewandowski, D., Barroca, V., Ducongé, F., Bayer, J., Van Nhieu, J. T., Pestourie, C. et al. In vivo cellular imaging pinpoints the role of reactive oxygen species in the early steps of adult hematopoietic reconstitution. Blood 115, 443–452 (2010).
Battisti, V., Maders, L. D., Bagatini, M. D., Santos, K. F., Spanevello, R. M., Maldonado, P. A. et al. Measurement of oxidative stress and antioxidant status in acute lymphoblastic leukemia patients. Clin. Biochem. 41, 511–518 (2008).
Jones, L., Richmond, J., Evans, K., Carol, H., Jing, D., Kurmasheva, R. T. et al. Bioluminescence imaging enhances analysis of drug responses in a patient-derived xenograft model of pediatric ALL. Clin. Cancer Res. 23, 3744–3755 (2017).
Acknowledgements
Patient samples and related clinical information for this study were kindly provided by Sydney Children’s Tumour Bank Network. Children’s Cancer Institute Australia is affiliated with UNSW Sydney and The Sydney Children’s Hospitals Network.
Author information
Authors and Affiliations
Contributions
M.K., A.K., A.B., A.M. and A.J.G. conducted the experiments and analysed the data; U.R.K., L.C.C. and R.S.K. provided guidance and access to the cell lines and patient material used in the study; K.S. and M.J.H. conceived the project and designed the experiments. T.F., G.M.A., M.H., M.D.N., R.S. and R.B.L. provided crucial suggestions and support with study design; M.K. wrote the manuscript under the guidance of K.S. and M.J.H. who critically reviewed the manuscript; All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Animal studies were conducted with approval from the Animal Care and Ethics Committee of the University of New South Wales (Sydney, Australia).
Consent to publish
Not applicable.
Data availability
All data generated or analysed during this study are included in this published article and its Supplementary information files.
Competing interests
The authors declare no competing interests.
Funding information
This research was supported by grants from the Anthony Rothe Memorial Trust, the Cancer Council NSW, the Tenix Foundation, the Kids Cancer Alliance, the ISG Foundation, the National Health and Medical Research Council of Australia (NHMRC Fellowships APP1059804 and APP1157871) to R.B.L. and the Children’s Leukaemia & Cancer Research Foundation (Perth, Western Australia) to U.R.K.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Karsa, M., Kosciolek, A., Bongers, A. et al. Exploiting the reactive oxygen species imbalance in high-risk paediatric acute lymphoblastic leukaemia through auranofin. Br J Cancer 125, 55–64 (2021). https://doi.org/10.1038/s41416-021-01332-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41416-021-01332-x
This article is cited by
-
Pharmacological Insights: Mitochondrial ROS Generation by FNC (Azvudine) in Dalton’s Lymphoma Cells Revealed by Super Resolution Imaging
Cell Biochemistry and Biophysics (2024)
-
FDA-approved disulfiram as a novel treatment for aggressive leukemia
Journal of Molecular Medicine (2024)
-
The gold complex auranofin: new perspectives for cancer therapy
Discover Oncology (2021)