Abstract
PTSD patients show alterations of the immune system, mainly a ‘low-grade inflammation’. Psychotherapeutic treatments are meant to reduce symptom burden of PTSD patients but 30–50% of PTSD patients do not benefit from psychotherapy. Therefore, in this study, the predictive effect of cytokine levels on therapy outcome are investigated. Pro- (IL-6) and anti-inflammatory (IL-10) cytokines in female PTSD patients (N = 17) were assessed under acute stress during a Trier social stress test (TSST) before therapeutic treatment. The predictive effects of IL-6 and IL-10 on therapy outcome (SCL_GSI, BDI) after an inpatient psychotherapeutic treatment at the University Medical Center Carl Gustav Carus, Technische Universität Dresden was investigated. Areas under the curve with respect to ground (AUCG) and increase (AUCI) for IL-6 and IL-10 levels during the TSST were calculated and used as predictors in regression analyses with pre-treatment scores. Models including all three predictors show good model fits (R2 = 0.255 to 0.744). Models including AUCG and AUCI scores show superior fits compared with models including pre-treatment scores alone (ΔR2 = 0.196 to 0.444). IL-6 AUCG and AUCI scores are significant predictors for post-treatment SCL-GSI and BDI (β = −0.554 to 0.853), whereas IL-10 AUCG significantly predicts SCL-GSI and BDI (β = −0.449 to −0.509). Therefore, pro- and anti-inflammatory IL-6 and IL-10 levels under acute stress before therapy predict therapy outcome of female PTSD patients regarding general symptom burden and depressive symptoms. Future studies should further address the link between inflammation and therapy outcome, especially underlying mechanisms and influencing factors.
Similar content being viewed by others
Introduction
Post-traumatic stress disorder (PTSD) develops after being exposed to or having witnessed a life-threatening event. Symptoms of PTSD are re-experiencing the event or parts of it in flashbacks or nightmares, hyperarousal and avoiding aspects related to the traumatic event [1]. Somatically, PTSD patients often show various diseases such as cardiovascular, respiratory, gastrointestinal and autoimmune diseases [2]. Even when controlling for risk factors for somatic diseases such as smoke status or somatic conditions such as hypertension, PTSD patients still show an elevated risk for somatic diseases [2, 3].
Based on these findings, a direct link between psychological disorders and somatic diseases is hypothesized. It is assumed that an alteration of the hypothalamus pituitary adrenal-axis (HPA-axis) and the immune system might promote the development of somatic diseases via cytokines [4]. Cytokines, a family of proteins, mediate immune responses to injury, infection or other organismal stress and are associated with inflammatory diseases, e. g. cardiovascular diseases, cancer, or autoimmune disorders [4, 5]. As described in past studies, an activation of the HPA-axis because of stress triggers a cascade resulting in an immunoregulatory function by inhibiting inflammatory cytokines such as Interleukin (IL-) 6 and increasing production of anti-inflammatory cytokines such as IL-10 [6]. Different studies investigated these mechanisms and found alterations of the HPA-axis and the immune system in PTSD patients showing a blunted HPA-axis stress reactivity compared with healthy controls [7, 8]. Regarding the immune system, mainly a so-called ‘low-grade inflammation’ was found in PTSD patients showing increased inflammatory cytokine levels compared with healthy controls [4]. These elevated levels of IL-6 were found to be associated with worse cognitive functioning of PTSD patients [9]. Therefore, it is supposed that these altered mechanisms of the HPA-axis and the immune system might lead to inflammatory body states in PTSD patients promoting the development of the mentioned diseases.
What remains unclear is, if cytokine levels also influence therapy outcome. 30% of patients with psychological disorders during clinical trials and 65% of patients in routine care do not respond to psychotherapy [10]. 30–50% of PTSD patients do not benefit from trauma-focused therapy sufficiently but show substantial residual symptoms after the end of the therapy [11, 12]. For this reason, past studies investigated aspects influencing therapy outcome and found various predictive factors [13, 14]. Regarding therapy outcome of PTSD patients, neuroimaging data and data of pre-treatment biomarkers among others were used for predicting therapy outcome [12, 15]. Higher bedtime salivary cortisol and lower urinary cortisol before treatment predicted greater symptom reduction [15, 16]. Studies examining the predictive character of cytokine levels on treatment outcome are rather rare. Rhein et al. (2021) assessed IL-6 levels of PTSD patients after a psychosocial stress test before therapy and the severity of depressive, trauma-related, and somatic symptoms 8 weeks after treatment. It was shown that patients with a high reactivity to the stress test, reflected by high IL-6 levels, showed a more negative therapy outcome. This study first showed an association between cytokine levels and therapy outcome [17].
The mentioned studies show that different biomarkers such as cortisol and cytokines influence therapy outcome of PTSD patients [14,15,16]. Nevertheless, the role of anti-inflammatory cytokines remains unclear and studies addressing the influence of cytokines on therapy outcome are very rare in general. Therefore, in this study, we assess the predictive character of pro-inflammatory IL-6 and anti-inflammatory IL-10 levels after a psychosocial stress test at the beginning of psychotherapeutical treatment regarding therapy outcome in female PTSD patients.
Methods
Study sample
Patients were recruited consecutively at the University Medical Center Carl Gustav Carus of the Technische Universität Dresden during the beginning of their inpatient treatment. 17 female PTSD patients between 28 and 58 years old (M = 47.12, SD = 8.52) with fluent German language skills were included in this sample. Exclusion criteria were a lifetime history of substance use disorder, psychotic or bipolar disorder, psychopharmacological or glucocorticoid-containing medication intake (e. g. asthma inhaler, topical cortisone creams), severe medical illnesses (e. g. cancer, autoimmune diseases, diabetes) and pregnancy. The Structured Clinical Interview (SCID-IV) [18] was conducted by trained interviewers for assessing mental disorders based on the DSM-IV-TR. All of the participants did at least show one comorbidity, n = 1 showed the maximum of 5 additional diagnosis to PTSD, most of the patients (n = 9) showed 3 comorbidities. N = 16 PTSD patients did additionally suffer from a major depressive disorder, n = 6 from panic disorder with/ without agoraphobia, n = 9 from social anxiety disorder, n = 8 from somatoform disorder. None of the participants did use contraceptives, n = 14 took medication and n = 10 of them were taking psychotropic drugs. N = 8 patients were married, 3 were divorced, 4 were single and 2 were widowed. 3 of the patients were uncapable for work and 6 of them did smoke. All of the participants provided written informed consent and the study procedure was conducted in accordance with the Declaration of Helsinki and approved by the local Ethics Committee of the Medical Faculty of the Technische Universität Dresden, Germany.
Psychosocial stress induction and hormone sampling
At the beginning of the inpatient treatment, patients participated in a standardized stress test, the Trier social stress test (TSST). The TSST reliably induces acute moderate psychosocial stress under laboratory conditions [19, 20]. It requires a mock job interview (5 min) and a mental arithmetic task (5 min) of the participants, which are performed in front of a mock selection committee. The TSST took place after 2 pm in the afternoon to account for the circadian rhythm of cytokine secretion. The female participants were tested in the luteal phase of their menstrual cycle. Blood samples were collected via a venous catheter 15 min and 1 min prior to the TSST as well as 1 min, 10 min, 20 min, 30 min, 45 min and 60 min after the TSST and set to coagulate for 30 min at room temperature. Afterwards, the blood samples were centrifuged at 20 °C for 10 minutes at 2500xG RCF. Blood samples were stored at −80 °C before being assayed for cytokines. Serum cytokine concentrations (IL-6 and IL-10) were determined using highly-sensitive ELISA enzyme-linked immunosorbent assays (IBL International GmbH, Germany).
Therapy procedure
PTSD patients received a multimodal trauma-focused psychotherapy, the mean duration of treatment was 9 weeks (SD = 3.44). Each week, patients participated in two sessions of individual therapy, which included trauma-focused elements such es Eye Movement Desensitization and Reprocessing or trauma-focused cognitive behavioural therapy. Individual therapy sessions were either offered by board-certified psychotherapists or experienced psychologists and were all supervised by an experienced psychotherapist. Furthermore, each week patients received two sessions of group therapy, two sessions of communicative movement therapy, two sessions of art therapy, one session of progressive muscle relaxation, one session of psychoeducation group, one session of training in social competences group and one session of trauma-stabilization group or skills training. If indicated, daily brief sessions with a nurse took place.
Clinical assessment
Two German language self-report questionnaires were handed out to the study participants for a clinical characterization in the beginning of the therapy and as a measure of therapy outcome at the end of therapy. In both, higher questionnaire scores indicate higher symptom burden. The Symptom Checklist (SCL-90-R) [21, 22] assesses the general psychological symptom burden within the last seven days and consists of 90 items. The global severity index (GSI) reflects the degree of general impairment. The SCL-90-R meets high internal consistencies with Cronbach’s α = 0.97 for the global index. Depressiveness was evaluated with the Beck Depression Inventory II (BDI-II) [23] including 21 items that match the DSM-IV-TR major depression criteria. Internal consistencies (Cronbach’s alpha) are high with α = 0.90 to 0.93.
Statistical analyses
A power analysis was conducted with StataIC 16 V5 to calculate an appropriate sample size. Therefore, based on a power of 80%, α = 0.05 and R2 = 0.50 were assumed. Based on this calculation, a sample size N = 18 was proposed and implemented. One patient had to be excluded because of missing data in the clinical assessment resulting in N = 17. As IL-6 and IL-10 values were skewed, they were subjected to ln-transformations [24]. For IL-10 values, there were in total 5.88% of missing data for different patients and time points. Therefore, missing cytokine values were imputed using predictive means matching over 10 iterations using R with the package mice [25]. Pre-/ post-differences in subjective symptom burden (SCL-90_R GSI, BDI) were calculated using paired t-tests. Results were considered significant when p < 0.05. Area under the curve with respect to ground (AUCG) and increase (AUCI) [26] were calculated for cytokine levels (IL-6, IL-10) during the TSST using StataIC 16 V5. To check for multicollinearity before regression analyses, AUC scores and pre-treatment scores were correlated using Pearson correlations. No correlation exceeded 0.7, so no evidence of multicollinearity was found. At first, in regression analyses pre-treatment scores were used as predictors for therapy outcome. Then, values for AUCG and AUCI were additionally added as predictors for therapy outcome (SCL-90 GSI, BDI). R2 greater than | 0.26| indicate a high goodness-of-fit [27]. ΔR2 was computed to assess additional benefit from including AUC scores in the regression analyses.
Results
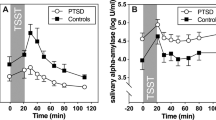
PTSD patients did show significant lower symptom burden on the BDI after therapy (M = 21.94, SD = 14.87) compared with BDI scores at the beginning (M = 29.81, SD = 11.72; t(15) = 2.50, p = 0.024, d = 1.16). Regarding the SCL-GSI score, there were no significant differences (beginning: M = 1.85, SD = 0.72, end: M = 1.46, SD = 0.97; t(15) = 1.84, p = 0.086). Figure 1 shows cytokine levels (IL-6, IL-10) in PTSD patients for different time points before and after the TSST, Table 1 includes means and standard deviations of IL-6 and IL-10 levels for each time point before and after the TSST. Further analyses of these patterns in comparison with depressive patients and healthy controls can be derived from a former article [28]. Results of Pearson correlation of AUC scores and pre-treatment scores can be derived from Table 2.
In regression analyses, when predicting therapy outcome by pre-treatment scores, SCL-GSI pre-treatment scores significantly predict SCL post-treatment scores (F(1,15) = 5.13, p = 0.039, R2 = 0.255) and also BDI pre-treatment scores significantly predict BDI scores after treatment (F(1,15) = 8.05, p = 0.013, R2 = 0.349). Results from regression analyses including pre-treatment scores and AUC scores as predictors for therapy outcome can be derived from Table 3. Model fits are consistently higher than R2 = 0.26, reflecting good model fits. 69.9% of the variance of SCL-GSI post-treatment scores is explained by IL-6 AUC scores and pre-treatment SCL-GSI scores. In this model, AUCG (β = 0.853, p = 0.001) and AUCI (β = −0.554, p = 0.024) are significant predictors for SCL-GSI post-treatment scores whereas SCL-GSI pre-treatment scores are not (β = 0.204, p = 0.287). 74.4% of the variance of BDI post-treatment scores is explained by IL-6 AUC scores and pre-treatment BDI scores. Also in this model, BDI pre-treatment scores do not significantly predict therapy outcome (β = 0.302, p = 0.104) whereas AUCG (β = 0.814, p = 0.001) and AUCI (β = −0.449, p = 0.044) coefficients show significant predictions. For IL-10, explained variances are smaller but the models still show a good model fit (SCL-GSI: R2 = 0.571, BDI: R2 = 0.545). Regarding SCL-GSI, AUCG-IL10 (β = −0.509, p = 0.018) and SCL-GSI pre-treatment scores (β = 0.686, p = 0.005) show significant regression coefficients, whereas AUCI-IL10 does not significantly predict SCL-GSI post-treatment scores (β = 0.686, p = 0.319). The same pattern was found in the regression model predicting BDI post-treatment scores (AUCG-IL10 β = −0.449, p = 0.036; AUCI-IL10 β = −0.158, p = 0.425; BDI pre-treatment scores β = 0.572, p = 0.009). ΔR2 were between 0.196 for predicting BDI post-treatment scores with IL-10 AUC scores and pre-treatment scores as predictors and 0.444 for predicting SCL_GSI post-treatment scores with IL-6 AUC scores and pre-treatment scores.
Discussion
In this study, the predictive value of IL-6 and IL-10 cytokine levels with regard on therapy outcome was assessed. It was found that IL-6 and IL-10 levels under acute stress in the beginning of the therapy predict therapy outcome regarding general symptom burden and depressive symptoms. Higher levels of IL-6 under acute stress before therapy are associated with higher general symptom burden and more severe depressive symptoms after therapy, whereas higher levels of IL-10 under acute stress before therapy are associated with reduced general symptom burden and less depressive symptoms after therapy. A high reactivity of IL-6 during acute stress before therapy predicts reduced general symptom burden and less depressive symptoms after therapy. The finding of predictive effects of IL-6 regarding therapy outcome is in line with the rarely existing literature [17] and adds further evidence to the predictive role of IL-6 and new insights in the predictive role of IL-10 regarding therapy outcome in female PTSD patients.
These results seem to emphasize the pro-inflammatory role of IL-6 suggested to promote inflammatory body states and the anti-inflammatory role of IL-10 [6]. Whereas higher levels of IL-6 seem to predict worse therapy outcome in this study, higher levels of IL-10 before therapy predict better therapy outcome. Additionally, the reactivity to an acute stressor plays an important role as a high IL-6 reactivity under acute stress predicts an advantageous therapy outcome. Therefore, as past studies show, the immune system of PTSD patients shows alterations compared with healthy controls and this altered immune system also seems to influence therapy outcome as results in this study suggest. One possible link might be the influence of elevated IL-6 levels on cognitive functioning of PTSD patients [29]. PTSD patients showed significantly higher IL-6 levels compared with healthy controls and significantly worse performance in memory, language and attention tasks [29]. As these functions also play an important role during psychotherapeutic treatment, an impairment could influence the therapy process and outcome, which is why this link should be investigated in future studies. As the role of IL-10 was rarely examined in past studies, this study again emphasizes the importance to also take anti-inflammatory cytokines such as IL-10 into account when assessing the role of the immune system in PTSD patients.
Based on these findings, the question arises how the immune system can be influenced and if this ‘low-grade inflammation’ of PTSD patients can be reduced or normalized. In a meta-analysis it was found that especially cognitive behavioral therapy (CBT) lowers levels of pro-inflammatory cytokines, increase immune cells and increase natural killer cell activity. Moreover, CBT was still associated with enhanced immunity six months after treatment [30]. Therefore, CBT seems to have a positive long-term effect on inflammatory states. If this influence is also present in PTSD patients, needs to be addressed in future studies. Another possibility of influencing elevated cytokine levels of PTSD patients is psychopharmacological treatment. Here, several new approaches targeting cytokine levels as alternatives to the known serotonin-reuptake-inhibitor treatments are discussed. For example, glucocorticoids could inhibit the expression of cytokines such as IL-6 [31, 32]. Also, endocannabinoid signaling was shown to have anti-inflammatory effects, which is why an elevation of endocannabinoid signaling with synthetic cannabinoids is discussed to be effective. Studies already found positive effects of endocannabinoids on trauma-associated nightmares and general PTSD symptoms [33, 34].
This study shows predictive effects of elevated IL-6 and IL-10 levels under acute stress on therapy outcome of PTSD patients. Nevertheless, there are some limitations. The study is slightly underpowered as one patient needed to be excluded because of missing data. Therefore, interpretation of the results needs to be made with caution. In this study, only female participants were assessed. On one hand, the prevalence of PTSD is higher among women compared with men and more women seek for trauma-related treatment [35]. On the other hand, it is known that there are gender differences in the immune response of individuals under acute stress [36]. As the sample size is quite small, we tried to control for as many influencing factors as possible (e. g. differences in immune response between genders, menstruation) in advance to not include too many control variables in the calculations and therefore reduce power of our study. 16 out of 17 patients suffered from a major depression additionally to PTSD. In general, PTSD patients often suffer from other mental disorders [37] which makes it difficult to include patients only suffering from PTSD and would affect the generalizability of the results. The general symptom burden assessed via the SCL-GSI did not change significantly through therapy. On one hand, the 9-week treatment is quite short for significantly reducing symptom burden of patients with multiple diagnosis. On the other hand, patients received a trauma-focused therapy addressing the traumatic symptoms and making the patients more aware of their traumatic experiences. This often leads to a higher symptom burden at first, which does not necessarily decrease through therapy to a smaller symptom burden than before treatment. Additionally, in this study one representative for pro- and anti-inflammatory cytokines was assessed, which gives a first insight of predictive effects of these cytokines regarding therapy outcome but for more general conclusions and further insights, additional parameters of the immune system should be assessed.
To our knowledge this is the first study investigating predictive effects of pro- and anti-inflammatory cytokines on therapy outcome in female PTSD patients. The present study showed that pro-inflammatory IL-6 and anti-inflammatory IL-10 levels under acute stress before therapy predict therapy outcome of female PTSD patients regarding general symptom burden and depressive symptoms. These findings emphasize the importance of the often-shown inflammatory state of PTSD patients and its influence on therapy outcome. Future studies should address underlying mechanisms of the link between inflammation and therapy outcome and find ways to ensure a greater benefit from psychotherapy for PTSD patients with low-grade inflammations.
References
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th edn (American Psychiatric Association, 2013).
Boscarino JA. Posttraumatic stress disorder and physical illness: results from clinical and epidemiologic studies. Ann N. Y Acad Sci. 2004;1032:141–53.
Giesinger I, Li J, Takemoto E, Cone JE, Farfel MR, Brackbill RM. Association between posttraumatic stress disorder and mortality among responders and civilians following the September 11, 2001, disaster. JAMA Netw Open. 2020;3:e1920476.
Speer K, Upton D, Semple S, McKune A. Systemic low-grade inflammation in post-traumatic stress disorder: a systematic review. J Inflamm Res. 2018;ume 11:111–21.
Hoge EA, Brandstetter K, Moshier S, Pollack MH, Wong KK, Simon NM. Broad spectrum of cytokine abnormalities in panic disorder and posttraumatic stress disorder. Depression Anxiety. 2009;26:447–55.
Petrovsky N. Towards a unified model of neuroendocrine-immune interaction. Immunol Cell Biol. 2001;79:350–7.
Metz S, Duesenberg M, Hellmann-Regen J, Wolf OT, Roepke S, Otte C, et al. Blunted salivary cortisol response to psychosocial stress in women with posttraumatic stress disorder. J Psychiatr Res. 2020;130:112–9.
Meewisse ML, Reitsma JB, Vries GJ, Gersons BPR, Olff M. Cortisol and post-traumatic stress disorder in adults: systematic review and meta-analysis. Br J Psychiatry: J Ment Sci. 2007;191:387–92.
Hori H, Kim Y. Inflammation and post-traumatic stress disorder. Psychiatry Clin Neurosci. 2019;73:143–53.
Lambert MJ. Maximizing psychotherapy outcome beyond evidence-based medicine. Psychother Psychosom. 2017;86:80–89.
Bradley R, Greene J, Russ E, Dutra L, Westen D. A multidimensional meta-analysis of psychotherapy for PTSD. Am J Psychiatry. 2005;162:214–27.
Zhutovsky P, Thomas RM, Olff M, van Rooij SJH, Kennis M, van Wingen GA, et al. Individual prediction of psychotherapy outcome in posttraumatic stress disorder using neuroimaging data. Transl Psychiatry. 2019;9:326.
Khayyat-Abuaita U, Paivio S, Pascual-Leone A, Harrington S. Emotional processing of trauma narratives is a predictor of outcome in emotion-focused therapy for complex trauma. Psychotherapy. 2019;56:526–36.
Brady F, Warnock-Parkes E, Barker C, Ehlers A. Early in-session predictors of response to trauma-focused cognitive therapy for posttraumatic stress disorder. Behav Res Ther. 2015;75:40–7.
Colvonen PJ, Glassman LH, Crocker LD, Buttner MM, Orff H, Schiehser DM, et al. Pretreatment biomarkers predicting PTSD psychotherapy outcomes: a systematic review. Neurosci Biobehav Rev. 2017;75:140–56.
Yehuda R, Pratchett LC, Elmes MW, Lehrner A, Daskalakis NP, Koch E, et al. Glucocorticoid-related predictors and correlates of post-traumatic stress disorder treatment response in combat veterans. Interface Focus. 2014;4:20140048.
Rhein C, Hepp T, Kraus O, Majewski K, Lieb M, Rohleder N, et al. Interleukin-6 secretion upon acute psychosocial stress as a potential predictor of psychotherapy outcome in posttraumatic stress disorder. J Neural Transm. 2021;128:1301–10.
First, MB & Gibbon, M. The Structured Clinical Interview for DSM-IV Axis I Disorders (SCID-I) and the Structured Clinical Interview for DSM-IV Axis II (SCID-II; John Wiley & Sons, Inc., 2004).
Foley P, Kirschbaum C. Human hypothalamus-pituitary-adrenal axis responses to acute psychosocial stress in laboratory settings. Neurosci Biobehav Rev. 2010;35:91–96.
Kirschbaum C, Pirke KM, Hellhammer DH. The ‘Trier Social Stress Test’-a tool for investigating psychobiological stress responses in a laboratory setting. Neuropsychobiology. 1993;28:76–81.
Derogatis, LR, Savitz, KL. The SCL-90-R, Brief Symptom Inventory, and Matching Clinical Rating Scales (American Psychological Association, 1999).
Hessel A, Schumacher J, Geyer M, Brähler E. Symptom-checkliste SCL-90-R. Diagnostica. 2001;47:27–39.
Beck, AT, Steer, R-A, & Brown, GK. Beck Depressions-Inventar Revision (Pearson, 2009).
Rohleder N. Stimulation of systemic low-grade inflammation by psychosocial stress. Psychosom Med. 2014;76:181–9.
van Buuren S. Groothuis-Oudshoorn K mice: multivariate imputation by chained equations in R. J. Stat. Softw. 2011 https://doi.org/10.18637/jss.v045.i03.
Pruessner JC, Kirschbaum C, Meinlschmid G, Hellhammer DH. Two formulas for computation of the area under the curve represent measures of total hormone concentration versus time-dependent change. Psychoneuroendocrinology. 2003;28:916–31.
Cohen J. Statistical Power Analysis For The Behavioral Sciences (Erlbaum Associates, 1988).
Renner V, Schellong J, Bornstein S, Petrowski K. Stress-induced pro-and anti-inflammatory cytokine concentrations in female PTSD and depressive patients. Transl Psychiatry. 2022;12:158.
Imai R, Hori H, Itoh M, Lin M, Niwa M, Ino K, et al. Inflammatory markers and their possible effects on cognitive function in women with posttraumatic stress disorder. J Psychiatr Res. 2018;102:192–200. https://doi.org/10.1016/j.jpsychires.2018.04.009.
Shields GS, Spahr CM, Slavich GM. Psychosocial Interventions and Immune System Function: A Systematic Review and Meta-analysis of Randomized Clinical Trials. JAMA Psychiatry. 2020;77:1031–43. https://doi.org/10.1001/jamapsychiatry.2020.0431.
Aerni A, Traber R, Hock C, Roozendaal B, Schelling G, Papassotiropoulos A, et al. Low-dose cortisol for symptoms of posttraumatic stress disorder. Am J Psychiatry. 2004;161:1488–90. https://doi.org/10.1176/appi.ajp.161.8.1488.
Yehuda R, Bierer LM, Pratchett LC, Lehrner A, Koch EC, van Manen JA, et al. Cortisol augmentation of a psychological treatment for warfighters with posttraumatic stress disorder: Randomized trial showing improved treatment retention and outcome. Psychoneuroendocrinology. 2015;51:589–97. https://doi.org/10.1016/j.psyneuen.2014.08.004.
Cameron C, Watson D, Robinson J. Use of a synthetic cannabinoid in a correctional population for posttraumatic stress disorder-related insomnia and nightmares, chronic pain, harm reduction, and other indications: A retrospective evaluation. J Clin Psychopharmacol. 2014;34:559–64. https://doi.org/10.1097/JCP.0000000000000180.
Jetly R, Heber A, Fraser G, Boisvert D. The efficacy of nabilone, a synthetic cannabinoid, in the treatment of PTSD-associated nightmares: A preliminary randomized, double-blind, placebo-controlled cross-over design study. Psychoneuroendocrinology. 2015;51:585–8. https://doi.org/10.1016/j.psyneuen.2014.11.002.
Kilpatrick DG, Resnick HS, Milanak ME, Miller MW, Keyes KM, Friedman MJ. National estimates of exposure to traumatic events and PTSD prevalence using DSM‐IV and DSM‐5 criteria. J Trauma stress. 2013;26:537–47. https://doi.org/10.1002/jts.21848.
Rohleder N, Schommer N, Hellhammer DH, Engel R, Kirschbaum C. Sex Differences in Glucocorticoid Sensitivity of Proinflammatory Cytokine Production After Psychosocial Stress. Psychosom Med. 2001;63:966–72.
Galatzer‐Levy IR, Nickerson A, Litz BT, Marmar CR. Patterns of lifetime PTSD comorbidity: A latent class analysis. Depression Anxiety. 2013;30:489–96. https://doi.org/10.1002/da.22048.
Acknowledgements
We like to thank the therapists of the University Medical Center Carl Gustav Carus of the Technische Universität Dresden conducting therapy sessions in this study as well as all patients who participated in this study.
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Contributions
JS, PJ and KP were involved in recruiting the sample and data collection. CK contributed his expertise regarding cytokines and analyzed cytokine levels. VR contributed to data processing, data analyzes and writing the manuscript. All of the authors contributed to finalizing the article.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Renner, V., Joraschky, P., Kirschbaum, C. et al. Pro- and anti-inflammatory cytokines Interleukin-6 and Interleukin-10 predict therapy outcome of female patients with posttraumatic stress disorder. Transl Psychiatry 12, 472 (2022). https://doi.org/10.1038/s41398-022-02230-3
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41398-022-02230-3
This article is cited by
-
Paradoxical effect of anti-inflammatory drugs on IL-6 mRNA expression in patients with PTSD during treatment
Journal of Neural Transmission (2024)