Abstract
Study design
Systematic review of qualitative studies.
Objective
To synthesise qualitative research exploring the experiences and perspectives of persons with spinal cord injury (SCI), relatives and health professionals concerning goal setting in SCI rehabilitation.
Methods
Five electronic databases were searched. A search strategy was constructed with key concepts identified using PICo (Population, phenomena of Interest and Context). Peer reviewed studies complying with the inclusion criteria were selected. Interpretive Description methodology guided analysis and synthesis of the findings.
Results
The search yielded 427 records. Of 12 full text studies assessed for eligibility, four were included describing goal setting in SCI rehabilitation from the perspective of persons with SCI and health professionals. Persons with SCI described a need for goal setting to be related to their everyday life, whereas the health professionals tended to use the hospital setting as their point of reference. Persons with SCI emphasised the importance of being self-directed and taking an active role in goal setting and rehabilitation. No studies presented the perspective of relatives.
Conclusions
This review illuminates the divergence in the understanding of goal setting between persons with SCI and health professionals. Goal setting in SCI rehabilitation often directly reflects physical functioning goals set by the health professionals, which does not prepare persons with SCI for everyday life and emotional issues. There is lack of focus on goals addressing psychosocial components such as family issues and change of roles. A shared process with goal setting relevant to persons with SCI and their everyday life is needed.
Similar content being viewed by others
Introduction
Spinal cord injury (SCI) is a complex and life-changing condition with physical, social and psychological consequences affecting participation and health-related quality of life [1]. Comprehensive multidisciplinary inpatient specialist rehabilitation is essential to support rehabilitation of persons with SCI [1]. Effective rehabilitation requires goal setting using a collaborative process during which the person with SCI and/or the relatives negotiate goals with the rehabilitation team [2]. Goal setting helps to identify the person’s needs, values and expectations regarding rehabilitation [3]. Active involvement in goal setting promotes autonomy, and improves treatment adherence and rehabilitation satisfaction [4, 5]. Furthermore, goal setting has a therapeutic effect beyond the goal itself, such as improved awareness of and adaption to disability [6]. During the last decade, person-centred goal setting has gained ground as a central principle in rehabilitation. However, there is a lack of consensus on how to implement it in clinical practice [4].
Previous reviews related to experiences of goal setting in rehabilitation have focused on stroke survivors, of whom many experience cognitive dysfunction [6, 7]. Evidence shows that experiences might be different in persons without cognitive dysfunction, such as persons with SCI [8]. One review described the experience in rehabilitation in persons with SCI but did not include goal setting [9]. As evidence is sparse on the experiences and perspectives of persons with SCI, health professionals or relatives regarding goal setting in rehabilitation, it is important to gather information and identify gaps in relation to this issue in both research and clinical practice. In this way, we can ensure a more person-centred approach and improve SCI rehabilitation. The aim of this study was to gain insight into experiences with and perspectives on goal setting in SCI rehabilitation from persons with SCI, their relatives and health professionals.
Materials and methods
This review was performed systematically and guided by a pre-defined protocol registered with the International Prospective Register of Systematic Reviews (PROSPERO) [registration number: CRD42018110408]; in reporting it follows PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines [10, 11]. The PICo framework (Population, phenomena of Interest and Context) used defined the inclusion criteria for study selection [12]. Studies were assessed for relevance using the inclusion criteria listed in Table 1.
The review team consisted of four persons. TM is an associate professor and physiotherapist with specialist knowledge of rehabilitation and goal setting. CMJ is a nurse and Master of health science with knowledge of SCI, rehabilitation and goal setting. LSM is an anthropologist and PhD student with knowledge of rehabilitation and Interpretive Description. CH is a senior researcher and nurse with specialist knowledge of rehabilitation and Interpretive Description.
Search and selection process
The PICo framework for qualitative searches was used to develop a search algorithm [12]. Keywords related to ‘SCI’ [AND] ‘Goal’ [AND] ‘Rehabilitation’ were used. Based on PICo, keywords were identified, and a preliminary PubMed search was undertaken to ensure identification of potentially relevant studies regarding experiences with and perspectives on goal setting in SCI rehabilitation. Additional keywords were derived from relevant titles and abstracts. Moreover, the index terms used by PubMed to describe each study were analysed to identify more relevant keywords. A search strategy was then developed and refined through discussions within the review team and with a specialised librarian. The search strategy developed for PubMed was then modified to search CINAHL, Embase, and PsycINFO (Supplemental table S1). No restrictions on publication dates were applied. The databases were searched from the earliest date available until October 2018. The search results were processed using the review management tool Covidence©. After removing duplicates, screening of the titles and abstracts according to the inclusion criteria was performed independently by two reviewers (CMJ, LSM). Full-text screening was completed for all studies that met the inclusion criteria by two reviewers (CMJ, LSM). Disagreements were resolved through discussion with a third reviewer (TM).
To ensure all relevant publications were identified, other publications by the authors included in the review were screened. To identify additional literature, the reference lists of included studies were reviewed and titles of studies that cited included studies were screened.
Critical appraisal and data extraction
Included studies were assessed using the Critical Appraisal Skills Programme (CASP) checklist for qualitative studies [13]. CASP is widely used to assess strengths and weaknesses of qualitative studies. It consists of ten key areas: clear aim, appropriate methodology, research design, data collection, ethical issues, rigour of data analysis and statement of findings [13]. Three reviewers (CMJ, LSM, CH) independently assessed methodological quality. Disagreements were resolved by lengthy and thorough discussions until consensus was reached in each area. As there is no published standard on when to exclude a study, no studies were excluded based on the quality assessment [14, 15]. Data from the included studies were extracted using a data extraction template developed and pilot tested by the reviewers. The template contained details about author(s), year of publication, country, setting, methodological approach, primary study aim(s), population, findings and perspectives; CMJ and LSM extracted the data and the extraction were discussed and agreed upon by all four authors (see Table 2).
Data synthesis
The analysis approach was informed by Interpretive Description, an inductive research methodology designed to address challenges that arise in practise [15]. The methodology seeks to develop a coherent conceptual description that represents associations, relationships and patterns within the phenomenon that is being researched (in this study: goal setting) in order to improve practice [15].
The analysis consisted of a four-step strategy [15]. First, data were scrutinised by all four authors for meaning components and immediate impressions. Data in this review consist of Results sections, Implications for practice sections and Conclusions from the included studies. These were extracted and imported to NVivo™. Second, these data were coded into initial themes reflecting particular circumstances and generalised patterns in relation to the study aim. Third, a more thorough coding based on the initial themes from step two was performed by CH and TM and the coding was discussed thoroughly by all four authors. Themes, patterns and relationships in the data material were then critically analysed by TM and CH. Finally, the study findings were summarised by extracting final themes and key insights across studies representing experiences with and perspectives on goal setting in SCI rehabilitation; this was performed by CH, TM and LSM.
Results
Study selection
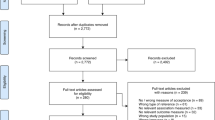
The initial search identified 586 records; one study was included based on the reference lists of included studies. Once duplicates were removed, 427 titles and abstracts were screened. Twelve studies were assessed in full text, of which three were discussed with a third reviewer; eight were excluded (Supplemental Table S2). Thus, four studies were included in the final review [16,17,18,19] (Fig. 1).
Study characteristics
Only perspectives of persons with SCI and health professionals were reported. No studies were found presenting relatives’ perspectives.
The included studies were conducted in Canada [17, 18] and Australia [16, 19] and published between 2001 and 2012 (Table 2). Time since injury varied for persons with SCI in the included studies; from months [16, 18] to years [17]. The purpose was to explore the process of goal setting [16, 19], to examine the perceptions of persons with SCI of the role in goal setting [18] and to understand the components of person-centred rehabilitation [17, 18].
Data were collected using individual semi-structured interviews [16, 18] or focus groups [17, 19]. Two studies used a theoretical approach to explore the topic, King’s theory of goal attainment [18] and symbolic interactionism [17]. One study used the Canadian Occupational Performance Measure (COPM), to set goals [19]. The participants in three studies comprised health professionals [16, 19] persons with SCI [16, 18, 19] or a mixed diagnostic population with SCI-specific data presented separately [17]. The number of study participants ranged from 1 to 13.
Overall, the studies were conducted in rehabilitation units [16, 17] and specialised SCI rehabilitation units [18, 19].
Quality assessment
According to CASP, all studies were appraised as contributing important insights and knowledge that extend our understanding of the experience with and perspectives on goal setting in rehabilitation (Table 3).
Synthesis of findings
Persons with SCI and health professionals have different and at times conflicting experiences with and perspectives on goal setting, mainly because the health professionals’ approach to goal setting primarily targets physical functioning rather than everyday life goals, which in turn is the most important concern for persons with SCI (Fig. 2).
Conflicting experiences with and perspectives on goal setting between persons with SCI and health professionals
The findings illustrated how important it was to persons with SCI that the goal setting process was related to their everyday life outside the hospital [16,17,18]. They explained that they constantly had discharge in mind and the difficulties they might experience when returning to their own home. Their concerns included issues such as education, family and employment [16,17,18]. It was important for persons with SCI that they worked towards the same goals as the health professionals. These were not necessarily goal attainment of which could be measured within the clinical setting, but goals that would apply to their everyday life [16]. The persons with SCI explained that goal setting as used by their therapists mostly addressed physical elements such as walking on stairs and managing basic care needs, which only partly prepared them for everyday life after discharge [16,17,18]. However, they wished for more relevant goals that addressed the psychosocial components of their everyday life such as family issues, employment, change of roles and independence in life outside the hospital [16,17,18].
These people with SCI emphasised that it was important for rehabilitation, including goal setting, to be individualised and tailored to their particular needs. They reported feeling that goal setting often revolved around whether the goals fit into the care plan developed by the health professionals [16,17,18]. They stated that the health professionals mainly applied their specific professional outlook when setting goals, meaning that they sometimes failed to involve the perspectives and wishes for life after discharge of the person with SCI [16, 17]. The relationship or power balance between health professionals and persons with SCI thus felt unequal, and patients explained how they suppressed their individual needs and goals, causing them to worry how that might affect their life after discharge [16]. For instance, patients expressed a need for the goal setting process to leave room for hope regarding their future [17, 18].
Furthermore, persons with SCI found it difficult to participate in goal setting on equal terms with health professionals, particularly in the early stages of the rehabilitation process [17, 18]. They explained that they were often not ready to play a role in goal setting, being too ill, incapacitated, and/or uninformed about their condition [17].
Patients explained how goals sometimes tended to drift away from their originally set targets towards goals set by the health professionals [18]. They explained that they occasionally felt they were perceived as being passive by the health professionals, and emphasised the importance of being self-directed and taking an active role in the goal setting and rehabilitation in order for it to be successful [17]. Moreover, they emphasised that regardless of their ‘stage’ in the rehabilitation process, it was important for them to be actively involved in goal setting and decision making [16, 17]. One study moreover underlined the importance of involving relatives in goal setting, which was perceived as a major help and support for persons with SCI [17].
Health professionals’ approach to goal setting in the hospital setting
The findings illustrated how health professionals’ understanding of goal setting was influenced by the hospital setting. They were experts in SCI and had a profound professional knowledge of the physical challenges and rehabilitation needs of persons with SCI [16,17,18]. The health professionals expressed clear opinions on what persons with SCI needed, referring to their professional knowledge and experiences within the field [16, 17, 19]. Furthermore, they applied technical terms to guide the person with SCI in the ‘right’ direction, if the latter had a different opinion or an opinion that was considered unrealistic by the health professionals [16, 17, 19]. The hospital setting became important because the person with SCI was a ‘visitor’ from outside [16]. Health professionals explained that the context of the hospital and the content of the goal setting process was familiar territory for them, and therefore they could predict what persons with SCI could expect and what knowledge or goal was of relevance. Nevertheless, some found that goal-setting tools could facilitate more involvement of persons with SCI, and some health professionals explained how tools could facilitate discussions with persons with SCI and enable the formulation of joint goals [16, 19].
These health professionals sought an equal relationship with the persons with SCI and aimed for a shared goal-setting process [16,17,18]. But, they still expressed feeling somewhat superior to persons with SCI, due to their professional knowledge of the expected consequences of SCI, and the effects these limitations might have on the future lives for the person with SCI [16,17,18]. Thus, the professionals often ended up taking the lead in defining the needs and goals of persons with SCI [16,17,18].
The health professionals had opinions on what could realistically be expected in relation to achieving goals, and they explained that they sometimes shared this knowledge with the person with SCI in order to speed up the goal-setting process [16, 19]. They described a ‘well-formed idea’ when persons with SCI were aiming to set goals that were not realistic, stating that ultimately it was their responsibility to decide whether working towards a given goal was appropriate [16, 19]. Therefore, the roles were divided and health professionals actively provided answers posed by the more passive person with SCI [16, 19].
They expected patients to be actively involved in the goal-setting process, while simultaneously aligning these goals with their own expert knowledge more than with the needs expressed by the patients [16, 19]. The professionals clearly stated that they strived to set goals as objectively as possible and in a way that made it possible to measure the achievement of the goals [16, 19]. If the person with SCI was not ready for goal setting as quickly as expected, some professionals suggested or even wrote down the goals that they found were appropriate and then asked the person with SCI to approve these goals [16, 17, 19]. This was in contrast to the health professionals’ statement on the importance of giving persons with SCI as much influence as possible to set realistic goals [16, 17, 19].
Discussion
This synthesis highlights the differences in experiences with and perspectives on goal setting for persons with SCI and the health professionals who treat them.
Strengths and limitations
A clear strength of this review is the systematic and judicious approach, involving at least two authors in all steps. The process was guided by the protocol registered in the PROSPERO register, the PRISMA guidelines and the PICo framework for qualitative studies, ensuring transparency and a systematic approach [10,11,12]. The CASP checklist for qualitative studies was used for critical appraisal of the included studies [13]. The studies were generally of high quality with good methodological rigour. Some quality issues were raised such as item #6 and item #8 of the CASP Checklist were answered ‘No’ or ‘unclear’ for all included studies [13]. None of the studies critically addressed the researcher(s) own role(s) (item #6). The researchers were occupational therapists [16, 19], nurses [18] and physiotherapist [17], this could have affected the interpretation findings, as the relationship between researcher and participants might have an unequal power balance and could influence what was expressed about goal setting [20, 21]. The question of sufficiently rigorous analysis (item #8) can be hard to resolve in qualitative research and is not considered a general weakness of the included studies. One study did not report the method of analysis [16]. All four studies had a clear aim and they all contributed to the understanding of the experience of goal setting in SCI rehabilitation.
Interpretive Description was chosen as the methodology for this review because it is an inductive methodology with a stringent and transparent analysis method [15]. The inductive four-step analysis guided by the Interpretive Description method ensured a systematic approach and transparency to the analysis, which would not have been possible using a deductive approach [15]. However, as this is a review based on data consisting of Results sections, Implications for practice sections and Conclusions from four studies, the interpretive part of the analysis has not been possible to unfold to the same extent as in an Interpretive Description analysis with “raw” empirical data [15]. Nevertheless, the included studies covered data from different settings collected using different methods and methodological traditions, adding strength to the review.
Even though generalisability is not formally expected in qualitative studies, we find that the insights derived from this study concerning diverging views between persons with SCI and health professionals may be transferable to similar SCI settings or possibly even to illnesses other than SCI [15].
Discussion of characteristics of included studies
Goal setting in rehabilitation might differ between countries and health systems [3, 20]. The included studies were conducted in two countries only (Australia and Canada), which could influence the relevance of the review’s conclusions, although studies on SCI rehabilitation from other countries have reported similar findings [5, 22,23,24]. The varying contexts included in this review highlight possible gaps in the body of evidence concerning experiences with and perspectives on goal setting in rehabilitation from the perspectives of persons with SCI, their relatives and health professionals.
One of the studies implies that time since the person suffered SCI has importance for goal setting [16]. This is supported by evidence suggesting that goals change over time [4, 24]. Given this, explicit exploration of goal setting in SCI rehabilitation at different points post-injury could be useful in producing data to guide future practice in SCI rehabilitation. On the other hand, the included studies represent different stages in rehabilitation (from sub-acute to long-term). They identify some of the same themes, implying that certain themes may be consistent in rehabilitation goal setting for persons with SCI.
Recent evidence on goal setting in rehabilitation suggests different approaches depending on whether persons have cognitive dysfunctions or not [8]. In one of the included studies, persons with acquired brain damage were interviewed in addition to persons with SCI [17]. The study did not suggest a different approach to persons with brain damage compared with persons with SCI [17]. Goal setting in SCI rehabilitation must take high number of factors into account [22, 25] one of them being cognitive functioning.
The health professionals in the four studies were occupational therapists, who base their practice within a goal-setting framework [26] and their experiences may not reflect those of other health professionals. Literature finds occupational therapists to base their practice around person-centred goal setting while medical doctors are more directive and less person-centred [24]. Goal setting and shared decision making are gaining ground in rehabilitation, and health professionals are becoming more aware of the importance of and challenges in goal setting [3, 4, 24]. Therefore, health professionals need to develop and ensure good clinical competences in goal setting. Furthermore, it is important to develop and describe goal-setting methods with focus on the everyday life after discharge.
Discussion of the synthesis
The synthesis highlights the differences in experiences and perspectives of goal setting for persons with SCI and health professionals. Our findings that goal setting in SCI rehabilitation encompasses a complex collaboration between patients and health professionals are supported by a Cochrane review [4]. Professionals need to share evidence and clinical knowledge with persons with SCI whilst being flexible in terms of when and how much information they provide, depending on the progress of the rehabilitation process. This review sheds light on challenges related to knowledge sharing among health professionals and persons with SCI in goal setting. This highlights the need for a shared goal setting process with involvement and consideration of needs and preferences of persons with SCI.
Although a person-centred approach to SCI rehabilitation practice is advocated [27], health professionals’ lack of compliance with this approach can leave patients unsupported and on their own [22,23,24]. Some studies highlight that persons with SCI are not adequately prepared for everyday life following SCI and that professionals’ focus on physical rehabilitation could reduce community reintegration for persons with SCI [22, 23, 27, 28]. Although a person with SCI is successfully rehabilitated in the hospital context, there are still long term challenges following SCI [22, 23, 25, 27, 28]. These challenges go beyond physical functioning and have vocational, financial and social consequences [23, 25]. Given the traumatic and long-term nature of SCI affecting the total life situation of the person, there is a need to reframe traditional rehabilitation practices [22, 27, 29]. In this review, it is argued that person-centred goal setting is important in order to improve SCI rehabilitation. By increasing attention to person-centred goal setting, professionals can use empowerment in rehabilitation and possibly strengthen autonomy and self-efficacy of persons living with SCI [5, 16, 22].
This is needed to enable transfer rehabilitation knowledge to the persons with SCI and their everyday life after discharge which is supported by studies in other areas than SCI rehabilitation [5, 6, 8, 21].
The ideal goal setting process is often dominated by health professionals taking the lead in setting the goals. Even though there has been a focus on shared decision making since the last studies in this review were published (2012), this challenge still exists [5, 24]. Goal setting must focus on the everyday life of persons with SCI, not just on goals that can be achieved and measured in a clinical setting. This review highlights a divergence between health professionals’ aim to set objective goals measurable in the hospital context such as being able to walk on stairs [17, 18], and the requests of patients for goals related to challenges in after-discharge everyday life such as family issues, education, employment or social challenges [16,17,18]. This discrepancy in perspectives may lead to interactions in goal setting to be conducted in an authoritarian approach, in deviation from practice guidelines for SCI rehabilitation [1]. Ideally, the health professional and the patient should draw upon each other’s knowledge, experience and preferences to enhance the relevance of the goal setting [5]. Therefore, to achieve a shared goal setting process and to strengthen patient autonomy, a change in power relations is essential [5].
Even though relatives should play a role in goal setting [2] none of the included studies explored the perspectives of relatives; however, one study emphasised the importance of support from relatives and peers in the goal setting process [17]. The lack of perspectives of relatives in the literature is similar to the findings in a recent review on goal setting in stroke rehabilitation [7].
Goal-setting tools such as SMART or COPM are well known and generally recommended for use in clinical practice [4]. However, this review highlights that health professionals find it difficult to use goal-setting tools and to incorporate them in clinical practice [15, 18]. This is supported by other authors who recommend ongoing focus on goal setting and use of different tools and approaches, as no tool will fit all individuals and situations [3, 5].
Goal setting in rehabilitation has been discussed more intensely over the last few years, in a Cochrane review from 2015 [4] and in more recent quantitative reviews [8, 30], and the approach to goal setting may have changed since the last of the four studies was published. There are no qualitative studies on goal setting in SCI rehabilitation after 2012; this underpins the need for more research within this area. A study from 2017 on shared decision making supported the need for a focus on the goal setting process and goals relevant to everyday life [24].
There is a need for further exploration of shared goal setting in different settings and time points post-injury, particularly goal setting in non-acute settings where persons with SCI have been out of hospital for some time.
Conclusions
This review provides insight into goal setting in SCI rehabilitation based on the experiences and perspectives of persons with SCI and health professionals. We found important differences between the understanding of goal setting of persons with SCI and that of health professionals, as persons with SCI seeks goals in relation to everyday life and professionals’ more often tend to set objective goals measurable in the hospital context.
Setting goals leaning on professional knowledge and at the same time involving the person with SCI and focusing on their everyday life challenges is a complex and difficult process that requires skilled and well-trained health professionals.
Future studies are required to further develop goal setting methods in multidisciplinary rehabilitation focusing on how to optimise involvement of persons with SCI in a shared goal setting process. Goal setting focusing on everyday life after discharge is important for persons with SCI. It would be beneficial to explore this further in qualitative studies identifying what the necessary professional skills are for successful goal setting and how these may be taught to health professionals. Furthermore, the role in goal setting of relatives of persons with SCI needs further attention.
References
Nas K, Yazmalar L, Sah V, Aydin A, Ones K. Rehabilitation of spinal cord injuries. World J Orthop. 2015;6:8–16.
Wade DT. Goal setting in rehabilitation: an overview of what, why and how. Clin Rehabilit. 2009;23:291–5.
Siegert RJ, Levack W. Rehabilitation goal setting: theory, practice, and evidence. Boca Raton: CRC Press, Taylor & Francis Group; 2015.
Levack WM, Weatherall M, Hay-Smith EJ, Dean SG, McPherson K, Siegert RJ. Goal setting and strategies to enhance goal pursuit for adults with acquired disability participating in rehabilitation. Cochrane Database Syst Rev. 2015:CD009727.
Lenzen SA, Daniels R, van Bokhoven MA, van der Weijden T, Beurskens A. Disentangling self-management goal setting and action planning: A scoping review. PLoS ONE. 2017;12:e0188822.
Rosewilliam S, Roskell CA, Pandyan AD. A systematic review and synthesis of the quantitative and qualitative evidence behind patient-centred goal setting in stroke rehabilitation. Clin Rehabilit. 2011;25:501–14.
Lloyd A, Bannigan K, Sugavanam T, Freeman J. Experiences of stroke survivors, their families and unpaid carers in goal setting within stroke rehabilitation: a systematic review of qualitative evidence. JBI Database Syst Rev Implement Rep. 2018;16:1418–53.
Smit EB, Bouwstra H, Hertogh CM, Wattel EM, van der Wouden JC. Goal-setting in geriatric rehabilitation: a systematic review and meta-analysis. Clin Rehabilit. 2019;33:395–407.
Whalley Hammell K. Experience of rehabilitation following spinal cord injury: a meta-synthesis of qualitative findings. Spinal Cord. 2007;45:260–74.
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6:e1000097.
International prospective register of systematic reviews United Kingdom Centre for Reviews and Dissemination. University of York [Internet]. [cited 27-03-2019]. https://www.crd.york.ac.uk/prospero/.
Stern C, Jordan Z, McArthur A. Developing the review question and inclusion criteria. Am J Nurs. 2014;114:53–6.
Critical Appraisal Skills Programme. CASP Qualitative Checklist. [Internet]. [cited 27-09-2019] Available at: https://casp-uk.net/casp-toolschecklists/. 2018.
Dixon-Woods M, Shaw RL, Agarwal S, Smith JA. The problem of appraising qualitative research. Qual Saf Health Care. 2004;13:223–5.
Thorne SE. Interpretive description: qualitative research for applied practice. 2 ed. New York, NY: Routledge; 2016. p. 336.
Barclay L. Exploring the factors that influence the goal setting process for occupational therapy intervention with an individual with spinal cord injury. Aust Occup Ther J. 2002;49:3–13.
Cott CA. Client-centred rehabilitation: client perspectives. Disabil Rehabilit. 2004;26:1411–22.
Draaistra H, Singh MD, Ireland S, Harper T. Patients’ perceptions of their roles in goal setting in a spinal cord injury regional rehabilitation program. Can J Neurosci Nurs. 2012;34:22–30.
Gustafsson, L, Mitchell, MG, Fleming, J, Price, G. Clinical utility of the Canadian Occupational Performance Measure in spinal cord injury rehabilitation. Brit J Occupational Therapy. 2012;75:337–42.
Siegert RJ, Taylor WJ. Theoretical aspects of goal-setting and motivation in rehabilitation. Disabil Rehabilit. 2004;26:1–8.
Yun D, Choi J. Person-centered rehabilitation care and outcomes: A systematic literature review. Int J Nurs Stud. 2019;93:74–83.
Angel S, Kirkevold M, Pedersen BD. Rehabilitation after spinal cord injury and the influence of the professional’s support (or lack thereof). J Clin Nurs. 2011;20:1713–22.
Nunnerley JL, Hay-Smith EJ, Dean SG. Leaving a spinal unit and returning to the wider community: an interpretative phenomenological analysis. Disabil Rehabilit. 2013;35:1164–73.
Scheel-Sailer A, Post MW, Michel F, Weidmann-Hugle T, Baumann Holzle R. Patients’ views on their decision making during inpatient rehabilitation after newly acquired spinal cord injury-A qualitative interview-based study. Health Expect. 2017;20:1133–42.
Barclay L, Lalor A, Migliorini C, Robins L. A comparative examination of models of service delivery intended to support community integration in the immediate period following inpatient rehabilitation for spinal cord injury. Spinal Cord. 2019:528–36.
Northen JG, Rust DM, Nelson CE, Watts JH. Involvement of adult rehabilitation patients in setting occupational therapy goals. Am J Occup Ther. 1995;49:214–20.
Beringer A. Spinal cord injury and outdoor experiences. Int J Rehabilit Res. 2004;27:7–15.
Lysack C, Komanecky M, Kabel A, Cross K, Neufeld S. Environmental factors and their role in community integration after spinal cord injury. Can J Occup Ther. 2007;74(Spec No.):243–54.
Dorsett P, Geraghty T. Health-related outcomes of people with spinal cord injury-a 10 year longitudinal study. Spinal cord. 2008;46:386–91.
Plant SE, Tyson SF, Kirk S, Parsons J. What are the barriers and facilitators to goal-setting during rehabilitation for stroke and other acquired brain injuries? A systematic review and meta-synthesis. Clin Rehabilit. 2016;30:921–30.
Acknowledgements
The authors would like to thank research librarian Camilla Meyer at Aarhus University Library for help, advice and guidance with the literature search. We would also like to thank senior researcher Anne-Mette Momsen for help with the initial searches and associate professor Merete Bjerrum for advice and input.
Funding
This work was supported by DEFACTUM, Central Denmark Region, Aarhus, Denmark and the Specialised Hospital for Polio and Accident Victims, Denmark.
Author information
Authors and Affiliations
Contributions
TM was responsible for designing the review protocol, screening potentially eligible studies, interpreting results, and writing the report. CMJ was responsible for designing the review protocol, registering the protocol, conducting the search, screening potentially eligible studies, extracting data, performing quality assessment of the included studies, interpreting results and provide feedback on the report. LSM was responsible for extracting data, performing quality assessment of the included studies, interpreting results and provide feedback on the report. CH was responsible for extracting data, performing quality assessment of the included studies, interpreting results and provide feedback on the report.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Maribo, T., Jensen, C.M., Madsen, L.S. et al. Experiences with and perspectives on goal setting in spinal cord injury rehabilitation: a systematic review of qualitative studies. Spinal Cord 58, 949–958 (2020). https://doi.org/10.1038/s41393-020-0485-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41393-020-0485-8
This article is cited by
-
Determination of cut-off points in the Trunk control test for spinal cord injury to assess the ability to perform different activities of daily living
Spinal Cord (2024)
-
Performance of the Dutch clinical prediction rule for the ambulation outcome after spinal cord injury in a middle-income country clinical setting: an external validation study in the Thai retrospective cohort
Spinal Cord (2023)
-
Cross-sectorial collaboration on policy-driven rehabilitation care models for persons with neuromuscular diseases: reflections and behavior of community-based health professionals
BMC Health Services Research (2022)
-
Strategies used by providers to support individuals with spinal cord injury in weight management: a qualitative study of provider perspectives
Spinal Cord Series and Cases (2021)