Abstract
Physical activity has been known as an essential element to promote human health for centuries. Thus, exercise intervention is encouraged to battle against sedentary lifestyle. Recent rapid advances in molecular biotechnology have demonstrated that both endurance and resistance exercise training, two traditional types of exercise, trigger a series of physiological responses, unraveling the mechanisms of exercise regulating on the human body. Therefore, exercise has been expected as a candidate approach of alleviating a wide range of diseases, such as metabolic diseases, neurodegenerative disorders, tumors, and cardiovascular diseases. In particular, the capacity of exercise to promote tissue regeneration has attracted the attention of many researchers in recent decades. Since most adult human organs have a weak regenerative capacity, it is currently a key challenge in regenerative medicine to improve the efficiency of tissue regeneration. As research progresses, exercise-induced tissue regeneration seems to provide a novel approach for fighting against injury or senescence, establishing strong theoretical basis for more and more “exercise mimetics.” These drugs are acting as the pharmaceutical alternatives of those individuals who cannot experience the benefits of exercise. Here, we comprehensively provide a description of the benefits of exercise on tissue regeneration in diverse organs, mainly focusing on musculoskeletal system, cardiovascular system, and nervous system. We also discuss the underlying molecular mechanisms associated with the regenerative effects of exercise and emerging therapeutic exercise mimetics for regeneration, as well as the associated opportunities and challenges. We aim to describe an integrated perspective on the current advances of distinct physiological mechanisms associated with exercise-induced tissue regeneration on various organs and facilitate the development of drugs that mimics the benefits of exercise.
Similar content being viewed by others
Introduction
Physical activity mainly refers to any bodily movement produced by skeletal muscles and results in energy expenditure, broadly encompassing exercise and sports, which have been done as part of daily living, occupation, leisure, and active transportation.1,2 Over the last few decades, physical activity has been convinced by clinical and experimental studies as an essential element of daily life and crucial to promote health and longevity.3,4,5 Importantly, it is reported that physical inactivity has become the fourth leading cause of death worldwide nowadays.6 According to 2020 World Health Organization (WHO) guidelines, it is stated that 150–300 min of moderate intensity, or 75–150 min of vigorous-intensity physical activity, or some equivalent combination of moderate intensity and vigorous-intensity aerobic physical activity should be undertaken per week.7 However, about one-third of adults worldwide do not meet the minimal intensity or time of physical activity recommended by WHO.8 Substantial evidence has shown that physical inactivity mostly has a negative impact on non-communicable diseases such as coronary heart disease,9 diabetes mellitus,10,11 cancer,12,13 and even mental health,14,15,16 dramatically aggravating the global health burden and shortening the life expectancy of people. Therefore, promotion of physical activity is one of the important methods to improve the quality of human lifespan.
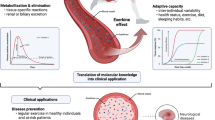
Exercise is theoretically defined as a kind of planned, structured, and repetitive physical activity.1 As a kind of physical education activity and social cultural activity, regular exercise is accepted by more and more people. Basically, there are two types of exercise including endurance (aerobic) training and resistance (anaerobic) training (Fig. 1).17,18,19,20 Physiologically, endurance exercise training refers to the exercise in which glucose metabolism depends on oxygen under aerobic conditions, while resistance exercise training refers to the exercise in which weight or overload is carried out in anaerobic condition and it is a short period of high-intensity or maximal intensity activity.21,22,23 The former usually induces the adaptation of cardiovascular and respiratory systems, while the latter is more likely to result in muscle hypertrophy through increasing myofibrillar volume predominantly in type II fibers and it is accompanied by changes in central nervous system.24,25,26,27 According to the exercise testing and prescription guidelines of the American Academy of Sports Medicine,28 endurance exercise is a wide range of physical activities, such as walking, jogging, dancing, swimming and cycling, its intensity is lower than the maximum intensity and can last for several minutes to several hours.29 Endurance exercise training is based on the FITT (frequency, intensity, time, type)–VP (volume, progression) principle of exercise prescription, while the intensity of exercise can be described in terms of heart rate, oxygen consumption (VO2) and metabolic equivalent.2 Common resistance exercise training includes barbell bench press, barbell overhead squat, dumbbell bicep curl and other strength exercises. The optimal training load for strength training is still being explored.30 It is suggested that performing a single set of 6–12 repetitions with loads ranging from approximately 70–85% one repetition maximum 2–3 times per week may produce sufficient training effect.31 Indeed, the complexity of physical activities makes no such clear boundary between the two types of exercise, as endurance exercise may become anaerobic if the intensity of aerobic exercise exceeds the anaerobic threshold. With a better understanding of the physiological responses triggered by different types of exercise, a variety of exercise strategies have emerged, including high-intensity interval training (HIIT) and moderate-intensity continuous exercise training (MICT). Notably, HIIT is getting more popular among the fitness enthusiasts and athletes because it has demonstrated superiority in cardiorespiratory fitness,32,33,34 weight loss,35,36 and improvement of chronic diseases.37 Overall, the diversity of exercise triggers different physiological adaptations, allowing for the targeted utilization of exercise training to make improvements of the various physical states.
Benefits of exercise-induced tissue regeneration. a Exercise induces physiological hypertrophy of left ventricle and reduction of myocardial infarction area by promoting the proliferation of cardiomyocytes. b Exercise induces muscle hypertrophy by promoting the proliferation of the satellite cells in both physiological and pathological conditions. Angiogenesis and mitochondrial biosynthesis are helpful in delaying muscle fatigue. c Exercise enhances hippocampal neurogenesis, myelin regeneration, axon regeneration, and cerebral angiogenesis to improve the motor, sensory, and cognitive functions. Exercise can also improve the sensory and motor functions after spinal cord injury and promote survival and differentiation of transplanted stem cells. d Exercise increases the branches of nerve fibers in the proximal skin, and promotes axon cross-sectional area (CSA), myelin sheath thickness, Schwann cell’s nucleus area and neurogenesis, so as to relieve the pain, improving sensation and motor function of patients with peripheral neuropathy. e Exercise can change the bone marrow microenvironment, promote the proliferation of hematopoietic stem and progenitor cells and the production of leukocytes. f Exercise regulates skeletal stem cell to differentiate into osteoblasts and chondrocytes, as well as bone angiogenesis, increasing bone mineral density (BMD). Besides, exercise induces the regeneration of post-traumatic cartilage lesions. Exercise is also considered as an effective adjuvant to stem cell-based therapy and the application of biomaterials or devices for cartilage regeneration. g Exercise promotes the regeneration ability of fatty liver, improving its tolerance to ischemia. Besides, exercise can restore liver function by promoting hepatocyte proliferation and mitochondrial biosynthesis in patients with partial hepatectomy. Created with BioRender
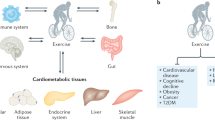
Over the past centuries, exercise training has been regarded as an effective approach to enhance tissue function under normal physiological condition and restore function under diverse pathological conditions, including cardiovascular diseases,38,39,40 chronic metabolic syndromes,41,42 neurological and psychiatric disorders,43,44,45 and cancer,19,46,47,48 which are mainly treated by chemical drugs. However, many diseases with loss of functional cells rely on cell supplement for tissue or organ regeneration. Nowadays, the definition of regeneration has been getting more precise and clearer, known as embryonic regulation, homeostatic regeneration, and restorative regeneration, respectively.49,50 As restorative regeneration stands for the ultimate goal that implantation of regenerated tissue constructs into the body to repair injuries or replace the physiological function, it makes great sense to find out how homeostatic tissues initiate the regeneration program by triggering a coherent immune response, appropriate cell plasticity, as well as stem and stromal cell responses following injury.51 As is well known, the basic process of tissue or organ regeneration should involve various forms of cellular plasticity first, which means that regeneration of tissues damaged by various injury modify tissue architecture through coordinated cell proliferation, differentiation, and apoptosis.52 Regeneration physiologically contributes to homeostasis against cell apoptosis, but it shows so limited ability to repair ischemic or impaired tissue for fully functional recovery in several vital organs, for instance cardiovascular and nervous system.53,54,55,56 Therefore, many approaches are currently applied to tissue regeneration therapy, including activation of endogenous stem cells and supplement with exogenous stem cells.57,58,59,60 Importantly, it has been suggested in recent decades that exercise is also able to contribute to promoting the restoration of damaged tissues, which provides a novel theoretical basis for tissue regeneration.
Since research on restorative regeneration has attracted more and more attention, exercise-induced tissue regeneration provides new therapeutic strategies. Recently it has been reported that only high-intensity training can stimulate changes in markers of mitochondrial respiratory function in skeletal muscle and enhance oxidative phosphorylation levels,61 which proves that there is a dose-dependent response to exercise duration and/or intensity again.3 However, not all individuals are able to achieve the level of exercise needed to experience the wide range of health benefits that exercise provides. Thus, it has been one of the most fascinating topics how exercise affects various organs and promotes injury repair, which drives researchers to mimic these effects with pharmaceuticals. To develop effective therapeutic approaches, it is crucial to understand the underlying mechanisms of the regenerative effects triggered by exercise, at the level of molecules, cells, and systems. This review will summarize recent advances in the benefits of exercise on different vital organs, thereby revealing the underlying molecular mechanisms and the potential mimetics from the perspective of exercise-induced tissue regeneration for further research and clinical applications.
Benefits of exercise on tissue regeneration
Exercise-induced muscle regeneration
The musculoskeletal system is an integral component of mobility and strength in the human body. Skeletal muscles, as the most important component of the musculoskeletal system, are characterized by myofibers and connective tissue, making up more than 35% of the adult body and containing 50–75% of all body proteins.62 The mechanical injury, ischemia injury, inflammatory injury and even congenital or acquired atrophy are described as those that involve disrupted connective tissues, leading to loss of skeletal muscle mass, reduced motor unit discharge rate, and impaired function.63 It has been uncovered that moderate exercise training enhances muscle regeneration after injury, as skeletal muscle mass recovery after extensive injury can be improved by contractile activity. In general, it has been widely convinced that the local adaptations of endurance exercise in skeletal muscle mostly focus on increased mitochondrial biogenesis and capillary density, which aids in the body’s ability to transport and use oxygen to generate energy and therefore delay the onset of muscle fatigue during prolonged aerobic performance.64 However, it has been also shown that endurance exercise training promotes maintenance of muscle mass and recovery after injury.65,66 While in rat models of notexin-induced soleus muscle degeneration, running exercise ensured the full recovery of muscle mass and muscle cross-sectional area during muscle regeneration, and made muscle recovery much faster than sedentary group.67,68 In contrast, resistance exercise training is more conducive to an increase in muscle strength and power as a result of neuromuscular adaptations, increases in muscle cross-sectional area (CSA), and alterations in connective tissue stiffness.69 Strength training significantly improved protracted quadriceps muscle atrophy in anterior cruciate ligament reconstruction patients via increasing muscle fibers CSA and type I fibers.70 Of note, it has been reported that HIIT, the novel combination exercise training strategy, promotes muscle regeneration, innervation, and vascularization in regenerated areas of volumetric muscle loss injury, even enhancing the healing effect of stem cell transplantation with an amniotic membrane scaffold.71 As mentioned about muscle regeneration induced by various exercise training, further studies should seek to assess different loads/modes (uphill vs. flat) with the same volume to confirm whether this affects muscle regeneration following training and provide compound exercise patterns to improve the efficiency of muscle regeneration.
Myogenesis follows after early inflammation and revascularization, and later fibrosis and re-innervation, resulting restoration of muscle mass and function.72 The bona fide tissue-specific stem cell, considered as a key component in myogenesis, in human adult skeletal muscle is the satellite cell.73,74 It has been convinced that the satellite cells are activated, proliferating, and differentiating after muscle fibers get injured, whose mitotic activity can be enhanced by exercise in the forms of endurance or resistance exercise training.75,76 In addition, skeletal muscle regeneration by the modulation of satellite cells is affected by the balance between pro- and anti-inflammatory macrophages.77 Exercise has been confirmed to cause the transition from the M1 to M2 macrophage phenotype, regulating the satellite cells proliferation and differentiation in the injury sites.78,79,80 Moreover, fibro-adipogenic progenitors (FAPs) has also been confirmed to get activated in response to muscle injury and establish functional interactions with the inflammatory cells and the satellite cells to promote muscle repair.81,82,83 More recently, it has been demonstrated that exercise increases and activates satellite cells by promoting FAPs senescence in the mouse models of acute muscle injury and chronic inflammatory myopathy, which provides a new therapeutic strategy for exercise-induced muscle regeneration (Fig. 1b).84
Exercise-induced bone and cartilage regeneration
Briefly, the primary features of an ageing skeleton are loss of bone, degraded articular cartilage, and degenerate, narrowed intervertebral discs, contributing to pain and loss of mobility. Physical activity has long been recognized as an essential factor in the maintenance of skeletal health. An abundance of studies has shown that both endurance and resistance exercise physiologically promote bone growth of teenagers and increase peak bone mass, which contributes to prevention of osteoporosis in adult stages.85,86 Thus, it is convinced that the common decline in bone mass during ageing attenuates, by following specific exercise programs, especially in postmenopausal women.87 Although endurance exercise is important in maintaining overall health, the resistance training may be more applicable to the basic rules of bone adaptation and site-specific effects of exercise.88 Recently an 8-week of exercise protocol of resistance exercise or endurance exercise experiment confirmed resistance exercise, but not endurance exercise, is likely to be effective in increasing bone strength.89 Indeed, it has been confirmed that bone responds more positively to mechanical loads that induce high-magnitude strains at high rates or frequencies, such as quick jumping, which causes the weakness of exercise’s ability to evoke osteogenesis in traditional training patterns.90 Thus, Davison et al.91 established a novel exercise equipment and exercise training patterns to improve the efficiency of osteogenesis, giving hope to those afflicted with bone loss (osteoporosis, or osteopenia) conditions. In addition, bone regeneration also relies on vascularization of the ossifying tissue, called angiogenesis-osteogenesis coupling.92 Yao et al.93 found that treadmill running could physiologically increase vessel number in the proximal metaphysis of rats, and significant changes of bone mineral density (BMD) in response to exercise. Subsequently, a set of researches have clarified that exercise stimulates angiogenesis during bone defect healing, accelerating bone regeneration as well.94,95
Chondral injury is a pathology with high prevalence, reaching as much as 63% of general population and 36% among athletes.96,97 Despite inappropriate or excessive exercise primarily aggravates joint damage, moderate exercise is recognized to exert a beneficial effect on the healing of osteoarthritis. It has been widely reported that both traditional training, such as running and swimming, and non-traditional training, such as pilates and yoga, are effective in the management of knee and hip osteoarthritis, mainly regarding pain and strength improvement.98,99,100 Notably, rodent models have shown that moderate exercise prevents the progression of post-traumatic cartilage lesions.101,102 Additionally, it is suggested that there is a dose–response relationship between loading and intervertebral disc regenerative processes, implying that the loading pattern typically used in the lumbar extension resistance exercise interventions (high load, low volume, and low frequency) may impart the regeneration of the intervertebral discs.103 Actually, cartilage tissue presents limited cellularity and lacks a vascular system, leading to restrained healing capability, which brings more attention to the implantation on promoting regeneration, including stem cell transplantation and the application of biomaterials or devices.104,105,106 Importantly, exercise is also considered as an effective adjuvant to cartilage regeneration therapy. Substantial evidence has shown that exercise enhances the potential of autologous chondrocyte implants, matrix-induced autologous chondrocyte implants, and mesenchymal stem cell (MSC) implants for the successful treatment of damaged articular cartilage and subchondral bone by downregulating osteoclastogenic cytokine production and upregulating antiosteoclastogenic cytokine production by circulating immune cells.107 More recently, Liu et al.108 demonstrated exercise promoted hyalinecartilage regeneration and completely healed cartilage in osteochondral defect rabbits with a biodegradable piezoelectric scaffold implanted, which is potentially applicable to the treatment of osteoarthritis.
As is well known, physical activities induce mechanical stress to the joints and bones, promoting stem cell proliferation and differentiation in the process of regeneration.103,109,110,111 It has been reported that acute exercise increases circulating stem and progenitor cells, including hematopoietic stem cells (HSCs) and MSCs.112 Interestingly, osteoblasts and chondrocytes are derived from multipotent skeletal stem cells of MSCs,113,114 while osteoclasts are derived from the macrophage lineage of HSCs.115 Bone formation is carried out by osteoblasts and resorption is carried out by osteoclasts, which means that bone regeneration relies on the balance of two types of cells. Exercise has been shown to induce skeletal stem cells to differentiate towards osteoblasts. It is found that endurance training increases the total number of bone marrow MSCs in mice, enhances the osteogenic differentiation potential of MSCs, and inhibits the adipogenic potential of MSCs.116 Of note, osteoclast recruitment to the future resorption sites is mainly controlled by osteoblasts. It has been shown that moderate exercise increases the expression of osteoprotegerin and decreases the expression of receptor activator of nuclear factor κB ligand, both of which are expressed by osteoblasts, inhibiting osteoclast differentiation and activity.117,118,119 Thus, the regulatory mechanisms of stem cells responding to mechanical stimuli and biochemical signaling is critical for exercise-induced bone regeneration (Fig. 1f).
Exercise-induced cardiac regeneration
The benefits of exercise on cardiovascular system have been extensively reported.38,120,121 It is widely accepted that both endurance and resistance exercise training contribute to larger left ventricle structures than sedentary controls from the imaging findings, presenting physiological cardiac hypertrophy.122 Thus, one of the most significant exercise-induced adaptations has been described as promoting cardiac growth. However, it has been discovered that the renewal of cardiomyocytes gradually decreases from 1% turning over annually at the age of 20 to 0.3% at the age of 75, implying that adult human cardiomyocytes has a limited self-renewing capacity.53 Importantly, Boström et al.123 demonstrated that adult cardiomyocytes physiologically increased in both size and proliferation rate in response to exercise in mouse models. Meanwhile, it has been identified that endurance exercise increases birth of new cardiomyocytes in adult mice (~4.6-fold) based on incorporation of 15N-thymidine by multi-isotope imaging mass spectrometry.124 Therefore, exercise training provides a new intervention for enhancing the proliferation of cardiomyocytes.
Interestingly, Bei et al.125 stated that cardiomyocyte proliferation was not necessary for exercise-induced cardiac growth but required for its protection against ischemic injury. Ischemic injury, a mismatch of oxygen and substrate supply and demand in the myocardium, is one of the most predominant causes of cardiomyocyte loss. Exercise has been found to reduce adverse ventricular remodeling and cardiac dysfunction when initiated after infarction in animal models126,127 and humans128 for decades. Furthermore, it was found that myocardial infarct size significantly decreased in ischemia injury rats at least 1 week following the cessation of 5 consecutive days HIIT training, implying the sustained capability of exercise in cardiac repair.129 Subsequently, a range of studies have found that exercise increases numerous circulating factors to promote cardiomyocyte proliferation and reverse pathological cardiac remodeling in post-infarction models.130,131,132,133,134 Importantly, Vujic et al.124 demonstrated that exercise induced a robust cardiomyogenic response in an extended border zone of the infarcted area, validating the endogenous cardiomyocyte generation induced by exercise in the process of myocardial injury repair. However, previous studies have been done in the acute phase of cardiomyocyte loss, the effect of exercise on the pathological state of the chronic phase deserves further investigation.
Although exercise has protected against pathological cardiac remodeling, the effect of myocardial restoration after ischemic injury appears to vary from different exercise types.135,136 Interestingly, it has been found that HIIT, the popular exercise strategy, is not superior to MICT in changing left ventricular remodeling or aerobic capacity in the heart failure patients with preserved ejection fraction137 or reduced ejection fraction.138 Additionally, recently it has been reported that moderate heart rate reduction induces cardiomyocytes proliferation under physiological conditions and promotes cardiac regenerative repair after myocardial injury by inducing G1/S transition and increasing the expression of glycolytic enzymes in cardiomyocytes, which is exactly the opposite of the exercise-induced rapid heart rate.139 Thus, the mechanism of exercise-induced myocardial regeneration is quite complex, the effects of different training patterns and training intensities in cardiac regeneration needs further exploration. It is rational to investigate exercise mimetics to balance the benefits and drawbacks of exercise. Furthermore, there are other causes of myocardial injury, such as hypertension140 and cancer,141 leading to cardiomyocyte death, whether exercise training counteracts induced-cell death by promoting cardiomyocyte proliferation also remains unknown (Fig. 1a).
Exercise-induced regeneration in central nervous system
Neural stem and progenitor cells (NSPCs) are major promoters of central nervous system (CNS) regeneration, which migrate and differentiate into highly specified networks of neurons via neurogenesis, while oligodendrocytes and astrocytes are generated via gliogenesis.142 NSPCs response to CNS injury is extraordinarily complex and dependent upon the extent and location of injury, thus the endogenous adult neurogenesis has been highly controversial. Recently, it has been confirmed that the hippocampus contains NSPCs that continue to generate new neurons, called adult hippocampal neurogenesis (AHN), which almost continues across the lifespan, though declining with aging.143,144 Age-related neurodegenerative diseases are probably associated with impaired AHN. These animal studies have shown that voluntary exercise promotes hippocampal neurogenesis and prevents age-related decline in cell-proliferation in this brain structure.145,146 Furthermore, it has also been revealed that exercise induces volumetric retention in the left hippocampus in humans, implying endurance exercise interventions are useful for preventing age-related hippocampal deterioration.147 Besides aging, trauma, ischemic injury, and inflammation often bring about irreversible damage and loss of function to the CNS. Ischemic injury remains an important risk of neuron loss in the CNS. It has been reported that both endurance and resistance exercise training enhance cognitive performance148,149,150 and improve functional performance, such as balance and walking speed,151,152,153 in post-stroke population, implying that exercise promotes the repair of central neurons. Moreover, in the ischemic stroke rodent model, it has been confirmed that early endurance exercise, for instance wheel-running and treadmill training, contributes to functional and neuronal recovery, mainly improving motor function via enhancing synaptic plasticity,154 promoting myelin regeneration154 and neuron survival,155 and facilitating cerebral angiogenesis.156 Multiple sclerosis (MS) is another kind of CNS disorders characterized by oligodendrocyte loss and axonal degeneration/demyelination.157 Recently emerging research suggests that exercise has therapeutic benefits on the outcomes in the CNS for MS patients, including oligodendrogenesis, remyelination, and axonal regeneration.158
Spinal cord injury (SCI) disrupts both axonal pathways and segmental spinal cord circuitry, resulting in permanent loss of motor, sensory, and autonomic function. Exercise has been shown to induce synaptic plasticity and restore motor/sensory function in SCI patients.159 Subsequently, endurance exercise, such as treadmill training, has been reported to enhance axonal regeneration and sprouting in SCI rodent models via multiple ways.160,161,162 Of note, it has been revealed that the cholinergic neurotransmission from spinal locomotor neurons activates spinal NSPCs, leading to neurogenesis in the adult zebrafish. Interference with γ-aminobutyric acid signaling promotes functional recovery after spinal cord injury, which acts in a non-synaptic fashion to maintain NSPCs quiescence.163 Though it provides a new approach for locomotor networks’ activity-dependent neurogenesis during SCI regeneration, whether similar effects can be found in mammals needs to be further investigated. Currently, the multi-faceted regeneration strategies for SCI regeneration have been met with mixed success, however, adult neurogenesis in heterogeneous NSPC populations is still creating barriers to the function recovery of SCI. Indeed, NSPCs proliferate and differentiate into reactive astrocytes in the injured spinal cord, contributing to the glial scar border, which segregates the injury and prevents additional damage.164,165 However, this scar also prevents axonal outgrowth into the site of injury and generation of new cell types within the neural lesion.166 Thus, stem cell-based transplantation, including olfactory ensheathing cells (OECs), MSCs, and NSPCs, has opened an avenue for functional recovery of SCI, which has been enhanced by exercise training as well.167 It has been reported that exercise enhances the effect of OEC grafts in super acute thoracic cord transected rats, inducing a fourfold increase in regenerating axons within the caudal stump of the transected spinal cord.168 Additionally, exercise significantly promoted NSPCs graft survival and differentiation more into neurons and oligodendrocytes, enhancing myelination, and restoration of serotonergic fiber innervation in the lumbar spinal cord via reducing stress caused by active oxygen or active nitrogen through insulin-like growth factor 1 (IGF-1) signaling, which provided more theoretical basis for exercise rehabilitation and pharmacological mimetics169 (Fig. 1c).
Exercise-induced regeneration in peripheral nervous system
The regenerative capacity of the nervous system varies considerably between the peripheral nervous system (PNS) and CNS. On the contrary, the adult human PNS retains the ability of axons to regenerate after injury and successfully reinnervate the intended target.170 In the PNS, injured nerves undergo successful Wallerian degeneration and subsequently the axons upstream of the injury undergo polarized growth toward their target tissues.171 Therefore, enhancing the regeneration of axons is often considered to be a therapeutic target for improving functional recovery after peripheral nerve injury. Several clinical studies have suggested exercise as a non-pharmacological approach to positively affect various aspects of peripheral neuropathy such as diabetic peripheral neuropathy (DPN),172,173 chemotherapy-induced peripheral neuropathy (CIPN),174,175 and even carpal tunnel syndrome.176 Among these studies, a 10-week composite training program of endurance and resistance exercise led to significant reductions in pain and neuropathic symptoms, and increased intraepidermal nerve fiber branching from a proximal skin biopsy in DPN patients.173 Similarly, the positive effects of exercise, including decreasing pain and improving physical function177 as well as improvement of deep sensitivity178 and static balance performance,179 have been confirmed in CIPN patients. The effect of exercise promoting peripheral nerve regeneration is also observed in animal models. Physiologically, ladder-based resistance training effectively induced similar growth in the radial and sciatic nerves (SN) of adult rats including myelinated axons CSA, unmyelinated axons CSA, myelin sheath thickness, and Schwann cells nuclei area.180 Meanwhile, the functional and histological recovery after the mouse SN crush was positively influenced by treatment with eccentric exercise.181 Moderate swimming training was found to promote nerve regeneration in SN ligation or SN transection mice as well.182,183 Additionally, treadmill training accentuated nerve regeneration, accelerated functional recovery and prevented muscle atrophy in median nerve crush injury rat models184 (Fig. 1d).
Exercise-induced regeneration of other tissues
The liver exhibits the unique regenerative capacity that ensures body homeostasis or post-injury repair.185 Experimental models that involve partial hepatectomy or chemical injury have revealed the efforts of exercise that make the liver return to equivalent size and weight to those prior to injury. It has been reported that a 4 weeks endurance exercise program markedly enhances the ischemic tolerance and the regenerative capacity of fatty liver in diet-induced steatosis mice.186 Moreover, Fard-Aghaie et al.187 confirmed that a novel physical prehabilitation of treadmill training promoted hepatocyte proliferation and enhanced mitochondrial biogenesis, restoring liver function after partial hepatectomy operation in rodent models. Although the liver is a solid organ with a high regenerative capacity, the rate of physiological cell turnover is very slow. Thus, the regenerative activities of hepatocytes and cholangiocytes induced by exercise provides new strategies for restoring liver function (Fig. 1g).
The skin, the largest organ of the human body, defends against daily assaults from the external environment. In general, scarring and regeneration are two physiologically opposite endpoints to skin injuries. Thus, scarless regeneration is the ultimate goal in repairing skin injury. Indeed, emerging evidence has shown exercise promotes skin wounds healing. For example, endurance exercise improves cutaneous wound healing rates of different etiologies in mice and humans.188,189,190 Interestingly, a study of mice trained on a motorized treadmill has suggested that different intensities of exercise have different impacts on healing rates.191 In addition, another study has shown that low-intensity exercise accelerates wound healing rates in diabetic mice but high-intensity exercise fails.192 However, promoting wound healing is not the same as promoting skin regeneration, as there are few studies for further cellular mechanisms. Whether exercise promotes resident skin stem cell proliferation remains unclear.
Exercise offers regenerative effects to the hematopoietic system as well. In this regard, preclinical studies of treadmill exercise training in mouse models have demonstrated endurance exercise is able to modify the bone marrow microenvironment, alter hematopoiesis, and accelerate hematopoietic regeneration.193,194 Leukocytes derive from hematopoietic stem and progenitor cells (HSPCs), acting as a major responder of exercise. Recently it has been reported that running exercise diminishes leptin production in adipose tissue to regulate HSPCs proliferation and leukocyte production in mice.195 The impact of exercise on leukocyte production and on HSPC epigenome and transcriptome persists for several weeks. Curiously, it was also showed that ultra-endurance exercise contributed to an increase in circulating leukocytes and induced an inflammatory response that resulted in a highly significant decline of circulating hematopoietic progenitor cells functionality in humans.196 This may be the result of different inflammatory effects of the organism in response to different exercise intensities and patterns. Hematopoietic stem cell transplantation (HSCT) is increasingly used for hematological malignancies or severe non-malignant hematological disorders. Since exercise is convinced to affect HSPC, HSCT combined with exercise therapy is also a topic worth being explored to improve prognosis.197 Lisio et al.198 demonstrated a survival benefit and increased total blood reconstitution in mice that were pre-conditioned with endurance exercise after bone marrow transplantation. However, as implementation varies across studies in terms of timing of exercise initiation, exercise types and duration of exercise according to potential benefits of exercise reported by previous studies, the efficacy of exercise program among HSCT patients varies.199,200 The efficacy of exercise promoting HSCT is worthy of recognition, however, further mechanistic studies are needed (Fig. 1e).
Molecular mechanisms of tissue regeneration induced by exercise
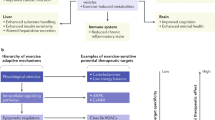
In response to exercise, the organism will have both structural and functional adaptive changes which confer the beneficial effect of exercise. However, the mechanisms by which exercise initiates cellular responses involved in tissue repair/regeneration are still inadequately understood. Generally, exercise predominantly leads to an increase in mechanical signals such as fluid flow, dynamic tension, compression, and hydrostatic pressure. Thus, mechanotransduction, the process by which the organism converts mechanical loading into cellular responses, is regarded as one kind of potent signaling pathways for adaptive responses to exercise.201 Besides mechanical signals, numerous studies have shown that a range of bioactive substances regulated by exercise (namely, exerkines) contribute to maintaining homeostasis and improving the impaired function of diverse organs.202,203 These exerkines can be secreted by a variety of cells, including satellite cells, osteoblasts, immune cells, endothelial cells, fibroblasts, macrophages, and even adipocytes, which act as autocrine, paracrine, or circulating regulators in response to exercise.204,205 Notably, it has been extensively investigated that both mechanical stress and biochemical signals are involved in promoting cell proliferation and renewal induced by exercise.206,207,208,209,210 Since the complicated mechanism of exercise-induced tissue regeneration advances rapidly, we will discuss in detail the substantial novel progress in the regulation of tissue regeneration from multiple aspects.
Mechanotransduction
Indeed, a variety of cell surface proteins and structures, named mechanosensors, has been proposed to convert these mechanical stimuli into electrical or biochemical signals. The Piezo family, one of the mechanically activated ion channel, has emerged as the critical mechanosensors in many cell types, responding to various forms of mechanical forces, including membrane stretch, static pressure, and fluid shear stress.211,212,213 Of note, Piezo1 is also highly expressed in osteocytes and can be upregulated by mechanical stretching, involved in stem cell differentiation and bone formation.214,215,216 In addition, Piezo1 channels, working as non-selective cationic channels in endothelial cells, had profound importance for shear stress-evoked Ca2+ signaling, sensing the exercise induced changes in blood flow.217 Focal adhesions, one type of integrin-based adhesion complex, is another important mechanosensor of transmitting mechanical signals and promoting protein biosynthesis.218,219,220 Unlike integrin-based adhesions that receive mechanical stimuli from the extracellular matrix, gap junctions, two juxtaposed connexons on the surfaces of adjacent cells, are bridges for mechanical signaling communication between cells. Multiple types of connexins play a role in responding to the mechanotransduction, among which connexin 43 was shown that its knockout in early osteoblasts caused impaired muscle formation in mice.221,222 Moreover, low density lipoprotein receptor-related proteins 5/6 (LRP5/6), the single-pass transmembrane protein, have been found to act as the receptor of Wnt ligands and be indispensable for Wnt/β-catenin signaling transduction, which has been shown to affect bone mass by regulating osteoblast proliferation and activity.223,224,225 Besides these canonical membrane structures, novel mechanosensitive proteins are regularly discovered, such as the recent discovery of plexin D1 as a mechanosensitive receptor,226 with more likely awaiting discovery. Taken together, these important membrane structures are the cornerstone of various cellular responses to external mechanical stimuli, and may be another prelude to unlocking the secrets of exercise induced regeneration.
Within the help of the mechanosensors, the activation of sequential signaling cascades and expression of downstream target genes exhibit some common features, even in various cell types, including osteocytes,227 myocytes,228 neurons,229,230 liver cells,231,232 and cardiomyocytes.233,234 Basically, signal transduction can occur through the direct physical connections between the membrane, the cytoskeleton, and the nucleus, triggering gene expression and protein synthesis.235 Importantly, the transmission of information still involves facilitating biochemical signals via intracellular signaling molecules and secondary messengers. The activation of Wnt/β-catenin pathway has been proven to be a key regulator of cell growth. Recently a multi-omic analysis of stretched osteocytes has uncovered mechanically stimulated osteocytes support bone regeneration via ossification and extracellular matrix remodeling, focusing on the activation of Wnt/β-catenin pathway in both human and murine cells, showing the conservation of mechanotransduction mechanisms.236 It has been established that exercise-induced loading reduces expression of sclerostin (SOST) and Dickkopf-related protein 1 (Dkk1), the inhibitors of the Wnt pathway, in osteocytes, thus stimulating new bone formation.237 Focal adhesion kinase (FAK), an attachment protein associated integrin-based adhesion complex, has also been a key component of transmitters of mechanical signals. FAK was reported to be required for IGF-1-induced muscle hypertrophy, through tuberous sclerosis complex 2 (TSC2)/mammalian target of rapamycin (mTOR)/ribosomal S6 kinase 1 (S6K1)-dependent signaling pathway.238 Interestingly, fluid flow shear stress could trigger FAK dephosphorylation, driving class IIa histone deacetylase 5 (HDAC5) nuclear translocation, which demonstrated a role for HDAC5 in loading-induced SOST suppression.239 Another most described mediators are the transcriptional coactivators yes-associated protein (YAP) and transcriptional coactivator with PDZ-binding motif (TAZ).240 Generally, YAP and TAZ, known to be regulated by FAK through RhoA-mediated contractile force, translocate from the cytoplasm to the nucleus in cells perceiving high levels of mechanical signaling.241,242 Notably, nuclear translocation of YAP/TAZ has been also regulated by Hippo signaling pathway.243,244 Multiple mechanical stimuli mostly inhibit the Hippo pathway, promoting YAP/TAZ to enter the nucleus to activate genes involved in the cell cycle and cell proliferation.245,246 Thus, suppression of Hippo signaling play an important role in promotion of tissue regeneration as well, suggesting a new intervention mechanism for exercise-induced regeneration.247,248 Furthermore, Notch signaling has been shown to be another associated pathway of mechanotransduction as well.249 Generally, mechanical loading sensed by integrins or mechanosensitive Piezo results in the transcription of ligands of sending cell, regulating Notch signaling of receiving cell, which modulates cell proliferation and differentiation.250 It has been reported that Notch signaling is impaired in regenerating aged skeletal muscle, which can be restored by physiological stimuli of exercise.251,252,253 Therefore, further researches should be carried out to demonstrate the underlying mechanisms of mechanotransduction mediated tissue regeneration with different exercise types, which may provide the novel targets for clinical interventions (Fig. 2).
Mechanotransduction regulating regenerative responses. The signaling transduction of exercise-induced regeneration are generally initiated by mechanical signals. A series of membrane receptors or channels can respond to mechanical signals, thereby converting mechanical signals into chemical molecular signals. Piezo1 channels, working as non-selective cationic channels, sense the exercise-induced stress, converting into mechanical stress-evoked Ca2+ signaling. Integrin-based adhesion complex activates FAK, promoting YAP/TAZ translocation via inhibiting Hippo signaling. FAK can drive HDAC5 nuclear translocation and suppress SOST. Integrins or Piezo channels activate the transcription of ligands of Notch receptor in sending cell, triggering Notch signaling of receiving cell. Wnt/β-catenin pathway is important in osteogenesis, which can be inhibited by SOST. Connexin 43 responds to the mechanotransduction for cell-to-cell communication. Created with BioRender
PI3K/Akt signaling pathway
Emerging evidence has revealed the essential contribution of PI3K/Akt signaling pathway to exercise-induced regeneration.254,255 An array of growth factors has been reported to act as exerkines, such as IGF-1,256 brain-derived neurotrophic factor (BDNF),257 epidermal growth factor (EGF)258 and their associated family, triggering the cellular responses via PI3K/Akt pathway. Amongst all the growth factors induced by exercise, the most widely studied is IGF-1. Notably, circulating IGF-1 is primarily secreted by the liver, while peripheral tissues, including bone and muscle, produce IGF-1 as well, acting in a paracrine/autocrine fashion. Exercise-induced IGF-1 locally leads to the sequential activation of PI3K/Akt signaling pathways with consequent induction of myoblasts,259,260 osteocytes261,262 and cardiomyocytes263,264 proliferation and differentiation. Meanwhile, neuregulin 1 (NRG1), a member of EGF family, and its tyrosine kinase receptor ErbB family is found to promote cell growth and differentiation physiologically and pathologically by targeting PI3K/Akt pathway.265,266,267 Moreover, BDNF and its receptor, tropomyosin-related kinase B (TrkB) mediate PI3K/Akt pathway as well, sharing the similar effects.268,269 BDNF has been discovered to be time-dependently upregulated in rat skeletal muscle after acute endurance exercise, which is convinced to be involved in exercise-induced skeletal muscle regeneration.257 Briefly, exercise-induced BDNF expression also plays a crucial role in neuronal survival, proliferation, maturation, and outgrowth in both the brain,270,271,272,273 spinal cord,274,275 and PNS.276,277 Angiogenesis has also played a vital role in human physiology of tissue repair, since oxygen supply and nutrients constitute important primitive materials for tissue anabolic activity.278,279,280 The transcription of vascular endothelial growth factor (VEGF) a kind of pro-angiogenic factor, is mainly activated by exercise-induced hypoxia and mechanical stress, which plays a crucial role in endothelial cell survival and promotion of capillary sprouting via PI3K/Akt pathway.281,282 Several studies have revealed that both endurance and resistance exercise increase the expression of VEGF in the brain, heart, skeletal muscle, and bones.95,283,284 HIIT training contributed to an overall increase in the expression levels of VEGF and VEGF receptor-2 (VEGFR2) in skeletal muscle of subjects with peripheral myopathy associated with heart failure, promoting muscle capillarization,285 and differentially expressed genes of the skeletal muscle showed the PI3K/Akt signaling pathway was activated in response to HIIT.286 Of note, it has been found that the PI3K/Akt axis is not only activated by a range of exerkines mentioned above, but also in response to mechanical stress.287,288,289 Exercise frequently mediates crosstalk between mechanoregulation of regeneration and canonical regenerative signaling pathways. While Akt has been reported to be activated by Notch, a important role in mechanotransduction, in EPCs after endurance exercise in hypertension patients, targeting endothelial nitric oxide synthase, for restoration of impaired angiogenesis capacity of late EPCs.290
The downstream responses of PI3K/Akt pathway are also varied. One of the significant targets of Akt is mTOR, an evolutionarily conserved serine/threonine kinase. Actually, mTOR exists in two distinct complexes: mTOR complex 1 and mTOR complex 2 (mTORC1 and 2).291 The activation of mTORC1 is frequently spotted in the adaptive response to exercise.292 Importantly, the activation of mTOR-axis has been the critical process of exercise-induced regeneration in different tissues, including muscle,293,294 heart,295 brain296 and spinal cord.297 Mostly, mTORC1 phosphorylates and activates S6K1/2 and eukaryotic translation initiation factor 4E (eIF4E)-binding proteins 1 and 2 (4E-BP1/2), which contribute to stimulation of mRNA translation, thereby regulating increases or decreases in anabolic and catabolic processes.298 Additionally, the activation of mTORC1 suppresses autophagy and perhaps other lysosomal functions.299 For instance, NRG1 activated PI3K/Akt axis, targeting mTOR-pathway in hippocampal neurogenesis, which was confirmed by exercise-induced expression of autophagy-related proteins.300 Moreover, CCAAT/enhancer binding protein β (C/EBPβ)-Cbp/p300-interacting transactivator with ED-rich carboxy-terminal domain 4 (CITED4) axis has been identified as critical modulator in the cardiomyocyte proliferation in adult exercised hearts, which has also been shown to be regulated by Akt.123,301 It has been confirmed that C/EBPβ is downregulated by endurance exercise to enhance cardiomyocyte proliferation via negatively regulating CITED4 in vitro.123 C/EBPβ and CITED4 has been reported to be regulated in myocardial ischemia or transverse aortic constriction murine models after exercise training.39,302,303 Overall, CITED4 acts as downstream of C/EBPβ, thereby activating the mTOR pathway, promoting exercise-induced cardiomyocyte proliferation and protecting from adverse cardiac remodeling.303,304,305 Another potential downstream mediator of the cell proliferation and development induced by exercise are forkhead box class O family (FOXOs). Akt/FOXO3a signaling pathway is activated in exercise-induced autophagy, which is beneficial for remedying sarcopenia.306 Akt is also likely to mediate FOXO family inhibition in the regulation of stem cell proliferation.307 Inhibition of FOXOs activity decreases myostatin expression and increases satellite cell proliferation, and fusion, and leads to muscle hypertrophy308,309 (Fig. 3).
PI3K/Akt signaling pathway. The PI3K/Akt pathway is mainly activated by an array of growth factors, such as IGF-1, NRG1, VEGF, and BDNF. Akt can be directly activated by Notch signaling. The PI3K/Akt pathway mainly acts as the upstream of mTOR activation. The activation of mTOR promotes cardiomyogenesis, myogenesis, and neurogenesis via various signaling. Importantly, PI3K/Akt axis inhibits C/EBPβ, thus upregulating CITED4 to activate mTOR and promoting myogenesis. Additionally, the PI3K/Akt axis inhibits FOXOs, promoting myogenesis. eNOS is upregulated by the PI3K/Akt axis, promoting angiogenesis. Created with BioRender
MAPK signaling pathways
The extracellular signal-regulated kinases 1 and 2 (ERK1/2), p38 mitogen-activated protein kinase (MAPK), and c-Jun N-terminal kinase (JNK), as key members of MAPK family, are also serine/threonine protein kinases that are irreplaceable players participating in diverse biological activities.310 Similar to PI3K/Akt signaling, MAPK signaling can be activated by a range of growth factors, thus playing an important role in exercise-induced tissue regeneration. More recently, it has been investigated that NRG1/ErbB2 signaling mediates the interaction of YAP with nuclear-envelope and cytoskeletal components for cardiomyocytes regeneration via the activation of ERK.311 Besides, MAPK/ERK signaling is also targeting the regulation of the cell cycle. Postnatal cell cycle exit is often accompanied by reduced expression of cyclins and cyclin-dependent kinases.312,313,314 Endurance exercise up-regulated cyclin-dependent kinase 4 and Cyclin D1 by ERK signaling, inducing the proliferation and differentiation of endogenous neural stem cells, and improving neural function of rats with cerebral infarction.315 Exercise was also reported to activate MAPK/ERK signaling to promote cycling of satellite cells.294 Furthermore, running exercise accelerated muscle regeneration in aged mice, suppressing transforming growth factor-β (TGF-β)/Smad3 signaling in quiescent muscle stem cells via the restoration of Cyclin D1.316 Additionally, it has also been well-known that bone morphogenetic proteins (BMPs), members of TGF-β super family, are upregulated in bones and cartilages after exercise.317,318,319 Mostly, the regulation of downstream networks of BMPs signaling is specifically though canonical Smad-dependent pathways.320 Importantly, BMP signaling has played a vital role in osteoblast differentiation, which promotes osteoblastogenesis through p38 MAPK pathway as well.321,322,323 Furthermore, following repeated bouts of eccentric cycling, it was reported that phosphorylation of JNK and p38 MAPK were also activated in skeletal muscle, inducing the overexpression of MyoD, myogenic regulatory factors (MRFs) and Myogenin324 (Fig. 4).
MAPK signaling pathway. The MAPKs signaling can be activated by exercise-induced mechanical stress and a range of growth factors, including NRG1, TGF-β and BMP, thus playing an important role in exercise-induced tissue regeneration. MAPK/ERK signaling activates YAP translocation into nucleus, promoting cardiomyogenesis. The activation of ERK also promotes neurogenesis and cycling of satellite cells. The restoration of cyclin D1 inhibits TGF-β/Smad signaling. The p38 MAPK and JNK can activate the transcription factors that initiate the expression of osteogenetic and myogenetic genes, including Myod, MRF, and Myogenin, promoting osteogenesis and myogenesis. Created with BioRender
AMPK/SIRT1/PGC-1α signaling pathway
Peroxisome proliferator-activated receptor (PPAR)-γ coactivator-1α (PGC-1α) is commonly expressed in high-energy-demanding tissues such as heart, muscle, and brown adipose tissue, which is already considered as the core regulator of metabolic regulating pathways such as the adenosine monophosphate-activated protein kinase (AMPK)-sirtuin 1 (SIRT1)-PGC-1α pathway.325 Undoubtedly, exercise leads to the activation of AMPK in vivo through the modulation of the AMP-to-ATP ratio.326,327 Though PGC-1α mainly involved in mitochondrial biosynthesis and cellular respiration, has been reported to act as a vital regulator in cell proliferation and differentiation as well.67,328 Exercise strongly induces overexpression of PGC-1α in both human and rodent muscle,329,330 which may trigger a remodeling of the satellite cells niche by altering the extracellular matrix composition, including the levels of fibronectin, thus affecting the proliferative output of satellite cells.331 While in terms of osteogenesis, PGC-1α has already been shown to play an important role in skeletal homeostasis by coactivating a range of transcription factors.332 Overexpression of PGC-1α was sufficient to enhance osteocytic gene expression in IDG-SW3 cells, murine primary osteoblasts, and osteocytes, and ex vivo bone cultures.333 In addition, deletion of PGC-1α suppressed differentiation and activity of osteoblast, resulting in a significant decrease of cortical thickness and trabecular thickness.334 Recently, it has been found that running exercise increases the expression of PGC-1α in the hippocampus of depressed mice, targeting for antidepressant treatment via promoting the proliferation parvalbumin-positive interneurons.335 Mechanically, PGC-1α activates a variety of metabolic programs in different tissues through its ability to form heteromeric complexes with many nuclear hormone receptors, such as PPARs336 and estrogen-related receptors (ERRs).337 Interestingly, PGC-1α is regulated by AMPK/SIRT1 axis, promoting exercise-induced tissue regeneration, as well as involved in mitochondrial signaling,338,339 Thus PGC-1α has acted as a vital regulator in the adaptive response to exercise, which may be the key regulator of the cross-talk between mitochondrial biogenesis and exercise-induced regeneration (Fig. 5).
AMPK/SIRT1/PGC-1α signaling pathway. Exercise changes the energy status, consuming a large amount of ATP, which elevates AMP-to-ATP ratio. Consequently, AMPK/SIRT1/PGC-1α signaling pathway is activated. PGC-1α is very important in the anabolic process of exercise-induced response. PGC-1α and PPAR/ERR form co-transcriptional complexes that initiate the overexpression of target genes, thereby promoting tissue regeneration and repair, including neurogenesis, myogenesis, and osteogenesis. Created with BioRender
Noncoding RNAs and their regulated signaling pathways
Recently emerging evidences support the critical role of noncoding RNAs, another important cluster of exerkines, in the regulation of exercise-induced tissue regeneration. Among them, microRNAs (miRNAs) have shown significant changes in the musculoskeletal system after exercise training.340 It was reported that in healthy untrained males, miR-1, miR-133, and miR-181a were increased in skeletal muscle samples collected 3 h following 60 min of cycling at 70% of VO2 peak.341 Similarly, the former two were shown to decrease in skeletal muscle miRNA profiles of muscle atrophy mice.342,343 Indeed, miR-1 promotes myoblast differentiation, whereas miR-133 stimulates myoblast proliferation. Mechanically, miR-1 modulated myocyte enhancer factor 2 (MEF2) via suppressing HDAC4 and miR-133 inhibited serum response factor (SRF), promoting myogenesis in different stages.344 Of note, miR-1 also positively promoted the protein synthesis and myogenesis by targeting IGF-1/Akt/FOXO3 signaling pathway.345,346 More recently, liver-derived extracellular vesicle miR-122-5p after treadmill training was reported to promote angiogenesis through shifting substrate preference to fatty acids in endothelial cells by targeting 1-acyl-sn-glycerol-3-phosphate acyltransferase (AGPAT1), increasing capillary density in the quadriceps, and accelerating wound healing in mice.347 In addition, treadmill exercise training has been also reported to influence the miRNA profiles of bone tissue, such as miR-190a-5p, miR-203-5p, miR-27a-5p, and miR-5118.348 Importantly, miR-27a-5p is confirmed as a member of miR-23a cluster. The components of the miR-23a cluster regulated osteoblast differentiation by targeting the modulation of SOST via TGF-β signaling pathway, which may explain the regulation of exercise-induced osteogenesis by miRNAs.349 Moreover, more miRNAs have been identified to involve in the different process of fracture healing, thus, whether these miRNAs are regulated by exercise still deserves further exploration.350
Likewise, a wide range of miRNAs have been found to increase in exercised heart as well, acting as vital regulators of exercise-induced cardiomyocyte proliferation and involving in myocardial injury repair. Expression of the protein kinase HIPK1 was identified as a direct target of miR-222 with anti-proliferative effects in cardiomyocytes, contributing to exercise-induced cardiomyogenesis.124,131 MiR-17-3p positively regulated cardiomyocytes proliferation and hypertrophy by targeting tissue inhibitor metallopeptidase 3 (TIMP3) and acting upstream of the phosphatase and tensin homolog deleted on chromosome 10 (PTEN)/Akt signaling pathway, protecting against myocardial ischemia–reperfusion injury.133 Additionally, aerobic exercise training increased miR-26 and decreased miR-16, significantly promoting cardiomyocyte hypertrophy and proliferation via Akt/mTOR signaling pathway.351 Furthermore, miR-34a, regulated by adenosine deaminases acting on RNA 2 (ADAR2), contributed to exercise-induced cardiomyocyte proliferation, targeting SIRT1, Cyclin D1 and Bcl2.352
While in terms of exercise-induced adult neurogenesis, it was reported that running exercise downregulated miR-135a-5p, targeting inositol 1,4,5-trisphosphate (IP3) signaling, thus increasing proliferation of neural precursor cells of the mouse dentate gyrus.353 It was also shown that miR-199a-3p increased in spinal cord after SCI and miR-21 increased in SCI animals that had undergone exercise.354 It was confirmed that miR-21 promoted and miR-199a-3p attenuated neurite growth in sciatic nerve injury rats via targeting PTEN in the regulation of Akt/mTOR pathway.297
Similarly, long noncoding RNAs (lncRNAs) have been shown to respond to exercise as well, promoting cell proliferation and differentiation during tissue regeneration.355 A set of lncRNAs have been reported to play key roles in myogenesis and adult skeletal muscle regeneration.356 Amongst them, the overexpression of lncRNA CYTOR, responding to exercise in both human and rodents, in mouse myogenic progenitor cells enhanced myogenic differentiation by sequestering the transcription factor Tead1, which was a regulatory mechanism of fast-twitch myogenesis in aging.357 Meanwhile, lncRNA CPhar358 and lncExACT1359 have been found to be regulated in exercised heart. Notably, lncRNA CPhar, characterized to be increased with exercise, triggered exercise-induced cardiac physiological hypertrophy via sequestering C/EBPβ and downregulating activating transcription factor 7 (ATF7), thus preventing myocardial ischemic injury-induced cardiac remodeling and dysfunction.358 Whereas lncExACT1 increased in heart failure but decreased in exercised hearts, inhibition of which induced cardiomyogenesis and protected against cardiac fibrosis and dysfunction as well.359 Dachsous cadherin-related 2 (DCHS2) had a role in the heart as a downstream effector of lncExACT1, mainly targeting Hippo/YAP signaling.359 Although evidence is still lacking to support the comprehensive functionality of most lncRNAs, the high tissue-specificity and regulation of specific facets of cellular networks have suggested that lncRNAs are superior to proteins in terms of potential, undesired toxic effects associated with their targeting360 (Fig. 6).
Noncoding RNA regulating the exercise-induced regeneration. Exercise induces many noncoding RNAs in the regulation of physiological response. MiR-17-3p acts as the upstream of PTEN by inhibiting TIMP3, promoting cardiomyocyte proliferation and hypertrophy through Akt/mTOR pathway. Another two miRNAs, miR-26, and miR-16, also involve in the Akt/mTOR pathway. ADAR2 inhibits miR-34a, targeting SIRT1, CyclinD1, and Bcl2 and leading to cardiomyocyte proliferation. Exercise-induced miR-222 decreases the expression of HIPK1, promoting cardiomyogenesis. Furthermore, miR-1 and miR-133 promote myogenesis via inhibiting HDAC4 and SRF, respectively. MiR-122-5p can promote angiogenesis through AGPAT1 pathway. Additionally, miR-27a-5p upregulates the expression of SOST to achieve osteogenesis. Of note, miR-21 and miR-199a-3p are also regulated by exercise, which is involved in PTEN/Akt signaling pathway. While miR-135a-5p promotes neurogenesis via inhibiting IP3 pathway. Exercise also modulates the effect of lncRNA on tissue regeneration. LncRNA CYTOR can achieve myogenesis through sequestering Tead1. LncExACT1 induces pathological myocardial hypertrophy, which is downregulated by exercise. While lncRNA CPhar promotes cardiomyogenesis through decreasing ATF7 by sequestering C/EBPβ. Created with BioRender
Potential exercise mimetics contributing to tissue regeneration
As is mentioned that exercise induces a set of physiological responses that benefit regeneration on various organs, it has gained great potential for use in patients having low exercise compliance or in those for whom regular exercise is not feasible. Consequently, exercise mimetics may have therapeutic applications across a variety of diseases. The following part reviews candidate exercise mimetics with emerging therapeutic targets and strategies for the development of exercise mimetics.
Pharmaceuticals
Indeed, AMPK/SIRT1/PGC-1α pathway acts as an important role of exercise-induced physiological responses. Given it, AMPK agonists are proposed as the promising exercise mimetics.361,362,363 However, it is widely recognized that AMPK activation induces a switch of cellular metabolism from anabolic to catabolic, promoting ATP conservation by inhibiting cell growth and proliferation, which makes AMPK agonists specialize in anti-tumor therapy rather than regeneration.364,365,366,367 Nevertheless, 5-aminoimidazole-4-carboxamide ribonucleotide (AICAR), one of the AMPK agonists, promotes angiogenesis in muscle by activating AMPK signaling in endothelial cells, mimicking the effects of exercise.368,369 Interestingly, though the majority of the effects of AICAR on skeletal muscles are AMPK-dependent, it may have indirect effect of AMPK activation in other organs. For example, AICAR has been suggested to increase hippocampus neuron number via activating the overexpression of BDNF, improving spatial memory; however, it cannot maintain a sustained positive effect as well as running due to the poor permeability through the blood–brain barrier.370,371,372 In addition, AICAR acts as an exercise mimetic in settings of fatty liver disease, enhancing the ischemic tolerance and the regenerative capacity of fatty liver.186 Likewise, another AMPK agonist exhibiting impressive exercise mimicking capability is metformin, which is extensively used as a first-line antiglycemic drug.373 Metformin showed positive cognitive effects or increased memory function via promoting angiogenesis, AHN, and remyelination in aged or stroke rodent models.374,375,376 Besides neurogenesis, metformin also has exhibited capability of osteogenesis, inducing the similar effects on femoral BMD gains compared to plyometric exercise in ovariectomized rats.377
PPARs are proposed to interact with PGC-1α, promoting a series of exercise-induce responses. Deficiency of PPARδ has been reported to result in a reduction of satellite cell number and the regenerative capacity.378 PPARδ increased the proliferation and differentiation of myoblasts through FOXO1, whereas GW501516, a kind of synthetic PPARδ agonist, promoted the processes of myogenesis.379,380 More recently, GW501516 was also reported to limit muscle tissue damage and restores muscle tetanic contraction in mice via mimicking localized exercise-induced inflammation by upregulating Forkhead box A2.381 Notably, GW0742, another synthetic PPARδ agonist, promoted angiogenesis and cell proliferation in muscle382 and heart383 via activation of calcineurin. Similar to AICAR and metformin, GW501516 and GW0742 increased memory performance and enhanced hippocampal neurogenesis as well.370,384 Thus, a phase IIa clinical study was carried out to test T3D-959, a newly synthetic PPARδ agonist, in subjects with mild to moderate Alzheimer’s disease, which suggests that PPARδ agonists are also moving towards clinical translation.385
Angiotensin II receptor blockade, an anti-hypertensive agent, is also an impressive replacement of exercise-induced regeneration. Losartan, a classical angiotensin-receptor blockade, was reported to limit post-infarct ventricular remodeling in rats, predominantly mimicking the protective effect of exercise on the heart.386 More recently, losartan reversed allodynia, reduced muscle fibrosis, and improved muscle regeneration in a murine model of orthopedic trauma combining tibia fracture and pin fixation with muscle damage, recapitulating the exercise-induced regeneration on post-injury recovery387 (Fig. 7).
Emerging pharmaceuticals mimicking exercise-induced tissue regeneration. AMPK/SIRT1/PGC-1α/PPARδ pathway has been selected as an important intervention of exercise-induced physiological responses. AICAR, metformin, GW501516, and GW0742, used to mimic exercise-induced physiological responses, demonstrate the ability to promote damaged tissue repair. Additionally, losartan is used to promote muscle regeneration. Created with BioRender
Natural molecular mediators
As mentioned above, the organism will release various natural molecular mediators involved in signaling pathways that promote regeneration during exercise. The regulatory mechanisms of these biomolecules are being understood by a wide range of researchers, which allows biosynthetic agents or genetic drugs to mimic the effects of exercise as well.
Irisin, a novel myokine, cleaved from membrane precursor fibronectin type III domain-containing 5 (FNDC5) in response to exercise, and acts as a linkage between muscles and other tissues.388 Besides inducing browning of white adipose tissue, irisin was discovered to promote proliferation and differentiation of osteoblasts through activating the p38 and ERK signaling.389,390 In the meantime, recombinant irisin positively regulated osteoblast differentiation under simulated microgravity via the overexpression of β-catenin, successfully providing a prevention strategy for bone loss and muscle atrophy induced by microgravity.391 Interestingly, irisin was also reported to bind to the proteins of the αV class of integrins, increasing production of SOST involved in bone resorption by increasing osteoclasts activity, which implied the two-sided effects of irisin on the therapeutic potential of skeletal remodeling.392 In terms of neuroprotection, circulating irisin crossed the blood-brain barrier and elevated BDNF level in the hippocampus, thereby promoting neurogenesis, enhancing synaptic plasticity, and modulating inflammation, which was demonstrated in models of neurodegenerative disease and cerebral ischemia.393,394,395 Furthermore, a recent study showed that recombinant adenovirus containing the irisin sequence improved burn-related neuropathy by ameliorating neuroinflammation-induced neuronal apoptosis, which demonstrated the protective effect of irisin on the PNS as well.396 Therefore, the therapeutic mechanism of irisin is not fully understood but has strong potential.
Adiponectin, one of the emerging adipokines, is also modulated by exercise, thus exerting a regenerative effect. Chronic exercise training imposed to rodents increased circulating adiponectin levels and AdipoR1 (adiponectin specific muscle receptor) expression.397,398 Thus, adiponectin was found to be responsible for the exercise-induced restoration of satellite cell mobilization, regenerative capacity in aged mice via the AMPK/SIRT1/PGC-1α axis.399 Moreover, adiponectin is capable of crossing the blood-brain barrier and affecting the CNS. Adiponectin mimicked exercise-induced effects in stress-elicited depression mice by retaining the normal proliferation of neural progenitors and dendritic morphology of neurons in the hippocampal dentate gyrus.400 In addition, AdipoRon (adiponectin receptor agonist), which mimicked the effects of running, rescued impaired cognitive function by improving hippocampal neurogenesis via adiponectin-Notch pathway.401 Similarly, AdipoRon treatment confirmed the exercise-induced hippocampal neuroplasticity in diabetic mice as well, which provides another promising candidate exercise mimetics.402,403
There are a set of immunomodulatory cytokines secreted into the circulation during exercise, such as interleukin-6 (IL-6) and IL-15, which are also integrated into the list of candidate exercise mimetics. IL-6 has been found to be synthesized and secreted into circulating by skeletal muscle during exercise, activating PI3K/Akt signaling, MAPK signaling and AMPK signaling in targeting cells.404,405,406 IL-6 was shown to promote proliferation of post-natal murine neural stem cell numbers.407 Thus, administration of recombinant IL-6 in a low-dose pulsatile strategy might directly modulate Schwann and nerve cells as a regenerative response to exercise in diabetic peripheral neuropathy.408 Notably, tocilizumab, one of the IL-6 receptor antibodies, has been used to treat some forms of arthritis.409 The side effect, such as blocking of exercise-mediated loss of visceral adipose tissue mass, has been confirmed recently.410,411 Whether the application of IL-6 receptor antibodies will block exercise-induced regenerative capacity is also a topic worthy of further investigation. While IL-15 is also a myokine of the IL-2 family responding to exercise.412 IL-15 has been reported to have local effects on skeletal muscles, such as promoting myoblast differentiation.413,414 Furthermore, exercise-mediated improvements in the healing of aged skin depend upon circulating IL-15. Exercise-mimicking recombinant IL-15 directly enhanced the growth of the aged mouse fibroblasts and keratinocytes, promoting impaired wound healing via activation of signal transducer and activator of transcription 3 signaling pathway, even though it was barely scarless regeneration415 (Fig. 8).
Natural molecular mediators. A set of exerkines are considered as candidate exercise mimetics, including irisin, adiponectin and interleukin, which can be used as gene therapy. These emerging target molecules provide new insights into the mechanisms of injured tissue regeneration and facilitate the efficiency of clinical translation. Created with BioRender
Discussion and perspective
Application of exercise intervention under aging condition
With the progress of society, the average human life expectancy has increased significantly. In parallel with longer lifespan, aging-specific health problem have emerged, which makes a growing global burden. Although it is brought to light that aging can not to be abolished, it is still expected to be able to attenuate the process and greatly ameliorate its effects, which implies the ultimate goal is not only longer lifespan, but also a better quality of life.416 Indeed, besides trauma and inflammation, aging is a vital process in the lifespan, whose essence is replicative cellular senescence.417 Senescent cells accumulate at sites of age-related pathologies and have an impact on the normal physiology of the tissues, causing a progressive functional deterioration.418 Exercise training is considered as a promising regenerative intervention for aged tissues, contributing to prevention and management of the challenging chronic diseases faced by elderly population.
Dementia is characterized by impairment of cognitive abilities and memory. Alzheimer’s disease (AD), a main and common type of dementia, is probably identified as age-related impairment of AHN.143 It has been reported that exercise not only reduces the risk of developing AD in aged population, but also improves the cognitive function of individuals with mild cognitive impairment and AD.419 Increasing evidence suggests that a variety of bioactive substances induced by exercise exert neuroprotective effects in mouse models via restoration of AHN and regulation of synaptic plasticity as well.420,421 In addition, numerous studies have shown that exercise can improve the poor prognosis of other age-related neurodegeneration via promoting neuronal survival and plasticity, or neurogenesis.422 Interestingly, endurance exercise has been reported to enhance the secretion of an enzyme, called glycosylphosphatidylinositol-specific phospholipase D1, derived from liver, ameliorating impaired neurogenesis and cognition in the aged hippocampus of mice.423 It is a new approach to explore the influence of other organs on the aged brain, providing new targets for the treatment of neurodegenerative diseases.
The level of bone loss increases with age, leading to osteoporosis in the elderly, particularly postmenopausal woman, which increases risk of fractures. Exercise training is considered as an effective method to stimulate bone osteogenesis in osteoporotic patients. As is mentioned, bone is a force-receptive organ, which needs to achieve sufficient mechanical intensity to effectively trigger the response of osteogenesis. As a result, not all types of exercise have the same positive effect on BMD. High intensity aerobic or resistance exercises are confirmed to be more effective in promoting the increase of BMD.424,425 In addition, several meta-analyses have shown that exercise appears extremely site-specific, increasing BMD only in the stimulated body regions.426,427 Thus, more composite exercises of diverse patterns and intensities need to be explored in order to more effective bone regeneration in whole body of aging adults.
Sarcopenia, the loss of skeletal muscle mass and strength, is an inevitable event during the aging process, which reduces physical capacity and enhances the problems associated with disabilities.428 Capelli et al.429 indicated that decay of maximal aerobic power and anaerobic capacity occurred with aging in cycling athletes, confirming age-related loss of muscle mass. Accumulating evidence supports that exercise training represents an effective intervention strategy to reduce or even reverse age-related loss of muscle mass as well.430 A meta-analysis, including 1,328 adults, demonstrated that resistance exercise training was effective in eliciting gains in lean body mass among the older people, particularly if they performed higher volume programs.431 Thus, as an effect of the independent exercise regimes on muscle mass, resistance exercise programs seem to be mostly effective in increasing muscle strength in sarcopenic frail elderly people.432,433 In regard of the cellular level, both resistance and endurance exercise training have shown to increase the number of satellite cells for regeneration in old animals and humans.434,435,436,437 The key role for muscle regeneration may be the intensity and frequency of exercise stimulation, however, the specific mechanisms responsible for re-trigger of growth capacity by exercise are not of comprehensive recognition yet.
Limitation and prospects of exercise intervention
Although remarkable progress has been made in the treatment of exercise interventions over the past few decades (Table 1), the side effects of over exercise are also being recognized. It is common to visualize that excessive-exercise or inappropriate exercise leads to sport-related injuries, ranging from the ankle and the knee, to the face and even the brain, which has ruined the careers of most athletes.438,439,440,441 Notably, chronic excessive exercise might adversely impact cardiovascular health. The increased incidence of atrial fibrillation seen in endurance athletes is one of the best documented cardiac maladaptations, which is related to exercise-induced changes in autonomic tone alongside the development of an arrhythmogenic atrial substrate.442 Myocardial fibrosis and coronary artery calcification have also been detected in ultra-endurance races.443,444 In addition, the marked suppression of growth factors and hormones, including testosterone, IGF-1, and leptin, after ultra-endurance exercise has also reported, which is strongly associated with the magnitude of the energy deficit.445 It has been realized that excessive exercise leads to immune imbalance and decrease in reactive oxygen species scavenging capacity, which has deleterious effects on health as well.446 Fortunately, with a better understanding of the adaptive responses of the organism to exercise gained, it has been found that we all carry our own “endogenous medicine box”. We have the opportunity to take the most applicable pills from the box to target a variety of different diseases. Thus, how to explore and make good use of the body’s own endogenous health resources, especially how to develop personalized rehabilitation exercise prescriptions for different diseases and different patients, has attracted more and more researchers to explore this field.
As a matter of fact, the knowledge of the adaptive responses to exercise is still only the tip of the iceberg. There are still three major points in the current researches on exercise for regeneration requiring further exploration. Firstly, the organism responds differently to diverse exercise patterns and intensities with great individual variability, resulting in instability and poor reproducibility of the exercise test. Therefore, the design of a rational exercise intervention is helpful to investigate the mechanisms of exercise regeneration, which is more effectively applied in clinical treatment further. Secondly, although the role of exercise for tissue regeneration undoubtedly brings new ideas and strategies, exercise mimetics need in-depth exploration. Notably, exercise mimetics may have utility across a wide range of human disorders, which is a gift for patients who are subjectively or objectively unable to achieve exercise benefits. However, as individual variability in exercise, exercise mimetics are not going to work as a universal panacea for divergent disorders but are more likely to be most effective for specific disorders, or even subtypes of such disorders. Thus, exploration of multi-target exercise mimetics is a key step in broadening the range of applications and improving the value of clinical translation. Thirdly, regeneration is indeed an anti-aging remedy, but it also often goes hand in hand with tumors. Whether exercise mimetics have a carcinogenic risk while promoting cell proliferation deserves more research to prove, which means a higher demand on the administration and dose of the drugs.
Beyond any doubt, exercise-induced regenerative medicine is an emerging and promising discipline. Currently, a variety of signaling pathways and related novel biomolecules have been identified in exercise adaptive regeneration, exhibiting more potential perspectives for disease prevention and treatment.
References
Caspersen, C. J. & Christenson, P. G. M. Physical activity, exercise, and physical fitness: definitions and distinctions for health-related research. Public Health Rep. 100, 126–131 (1985).
Garber, C. E. et al. American college of sports medicine position stand. Quantity and quality of exercise for developing and maintaining cardiorespiratory, musculoskeletal, and neuromotor fitness in apparently healthy adults: guidance for prescribing exercise. Med. Sci. Sports Exerc 43, 1334–1359 (2011).
Arem, H. et al. Leisure time physical activity and mortality. JAMA Intern. Med. 175, 959–967 (2015).
Bauman, A. E. et al. An evidence-based assessment of the impact of the Olympic Games on population levels of physical activity. Lancet 398, 456–464 (2021).
Lieberman, D. E., Kistner, T. M., Richard, D., Lee, I. & Baggish, A. L. The active grandparent hypothesis: physical activity and the evolution of extended human healthspans and lifespans. Proc. Natl Acad. Sci. USA 118, e2107621118 (2021).
Kohl, H. W. et al. The pandemic of physical inactivity: global action for public health. Lancet 380, 294–305 (2012).
Bull, F. C. et al. World Health Organization 2020 guidelines on physical activity and sedentary behaviour. Br. J. Sports Med. 54, 1451–1462 (2020).
Hallal, P. C. et al. Global physical activity levels: surveillance progress, pitfalls, and prospects. Lancet 380, 247–257 (2012).
Lavie, C. J., Ozemek, C., Carbone, S., Katzmarzyk, P. T. & Blair, S. N. Sedentary behavior, exercise, and cardiovascular health. Circ. Res. 124, 799–815 (2019).
Lee, C., Han, K., Yoo, J. & Kwak, M. Synergistic harmful interaction between sustained physical inactivity and hypertension/diabetes mellitus on the risk of all-cause mortality: a retrospective observational cohort study. J. Hypertens. 39, 2058–2066 (2021).
Medina, C. et al. Cardiovascular and diabetes burden attributable to physical inactivity in Mexico. Cardiovasc. Diabetol. 19, 99 (2020).
Patterson, R. et al. Sedentary behaviour and risk of all-cause, cardiovascular and cancer mortality, and incident type 2 diabetes: a systematic review and dose response meta-analysis. Eur. J. Epidemiol. 33, 811–829 (2018).
Lee, I. et al. Effect of physical inactivity on major non-communicable diseases worldwide: an analysis of burden of disease and life expectancy. Lancet 380, 219–229 (2012).
Rodriguez-Ayllon, M. et al. Role of physical activity and sedentary behavior in the mental health of preschoolers, children and adolescents: a systematic review and meta-analysis. Sports Med. 49, 1383–1410 (2019).
Kandola, A., Ashdown-Franks, G., Hendrikse, J., Sabiston, C. M. & Stubbs, B. Physical activity and depression: towards understanding the antidepressant mechanisms of physical activity. Neurosci. Biobehav. Rev. 107, 525–539 (2019).
Nooijen, C., Blom, V., Ekblom, O., Ekblom, M. M. & Kallings, L. V. Improving office workers’ mental health and cognition: a 3-arm cluster randomized controlled trial targeting physical activity and sedentary behavior in multi-component interventions. BMC Public Health 19, 266 (2019).
Erguson, B. F. ACSM’s guidelines for exercise testing and prescription 9th Ed. 2014. J. Can. Chiropr. Assoc. 58, 328 (2014).
Lamberti, N. et al. Effects of low-intensity endurance and resistance training on mobility in chronic stroke survivors: a pilot randomized controlled study. Eur. J. Phys. Rehab. Med. 53, 228–239 (2017).
Wehrle, A., Kneis, S., Dickhuth, H., Gollhofer, A. & Bertz, H. Endurance and resistance training in patients with acute leukemia undergoing induction chemotherapy—a randomized pilot study. Support. Care Cancer 27, 1071–1079 (2019).
Garcia-Pinillos, F., Laredo-Aguilera, J. A., Munoz-Jimenez, M. & Latorre-Roman, P. A. Effects of 12-week concurrent high-intensity interval strength and endurance training program on physical performance in healthy older people. J. Strength Cond. Res. 33, 1445–1452 (2019).
Gibala, M. J., Little, J. P., MacDonald, M. J. & Hawley, J. A. Physiological adaptations to low-volume, high-intensity interval training in health and disease. J. Physiol. 590, 1077–1084 (2012).
Knuiman, P., Hopman, M. T. E. & Mensink, M. Glycogen availability and skeletal muscle adaptations with endurance and resistance exercise. Nutr. Metab. 12, 59 (2015).
Gabriele et al. Muscle stem cell and physical activity: what point is the debate at? Open Med. 12, 144–156 (2017).
Folland, J. P. & Williams, A. G. The adaptations to strength training: morphological and neurological contributions to increased strength. Sports Med. 37, 145–168 (2007).
Hoppeler, H., Baum, O., Lurman, G. & Mueller, M. Molecular mechanisms of muscle plasticity with exercise. Compr. Physiol. 1, 1383–1412 (2011).
Farup, J., Sørensen, H. & Kjølhede, T. Similar changes in muscle fiber phenotype with differentiated consequences for rate of force development: endurance versus resistance training. Hum. Mov. Sci. 34, 109–119 (2014).
McGee, S. L. & Hargreaves, M. Exercise adaptations: molecular mechanisms and potential targets for therapeutic benefit. Nat. Rev. Endocrinol. 16, 495–505 (2020).
Garber, C. E. et al. Quantity and quality of exercise for developing and maintaining cardiorespiratory, musculoskeletal, and neuromotor fitness in apparently healthy adults. Med. Sci. Sports Exerc. 43, 1334–1359 (2011).
Wilder, R. P. et al. Physical fitness assessment: an update. J. Long. Term. Eff. Med. Implants 16, 193–204 (2006).
Swift, D. L., Johannsen, N. M., Lavie, C. J., Earnest, C. P. & Church, T. S. The role of exercise and physical activity in weight loss and maintenance. Prog. Cardiovasc. Dis. 56, 441–447 (2014).
Androulakis-Korakakis, P., Fisher, J. P. & Steele, J. The minimum effective training dose required to increase 1RM strength in resistance-trained men: a systematic review and meta-analysis. Sports Med. 50, 751–765 (2020).
Martin-Smith, R. et al. High intensity interval training (HIIT) improves cardiorespiratory fitness (CRF) in healthy, overweight and obese adolescents: a systematic review and meta-analysis of controlled studies. Int. J. Environ. Res. Public Health 17, 2955 (2020).
CHIN, E. C. et al. Low-frequency HIIT improves body composition and aerobic capacity in overweight men. Med. Sci. Sports Exerc. 52, 56–66 (2020).
Grace, F. et al. High intensity interval training (HIIT) improves resting blood pressure, metabolic (MET) capacity and heart rate reserve without compromising cardiac function in sedentary aging men. Exp. Gerontol. 109, 75–81 (2018).
Su, L. et al. Effects of HIIT and MICT on cardiovascular risk factors in adults with overweight and/or obesity: a meta-analysis. PLoS ONE 14, e210644 (2019).
Wewege, M., van den Berg, R., Ward, R. E. & Keech, A. The effects of high-intensity interval training vs. moderate-intensity continuous training on body composition in overweight and obese adults: a systematic review and meta-analysis. Obes. Rev. 18, 635–646 (2017).
Ross, L. M., Porter, R. R. & Durstine, J. L. High-intensity interval training (HIIT) for patients with chronic diseases. J. Sport Health Sci. 5, 139–144 (2016).
Fiuza-Luces, C. et al. Exercise benefits in cardiovascular disease: beyond attenuation of traditional risk factors. Nat. Rev. Cardiol. 15, 731–743 (2018).
Nasim et al. High-intensity interval training increase GATA4, CITED4 and c-Kit and decreases C/EBPβ in rats after myocardial infarction. Life Sci. 221, 319–326 (2019).
Eskandari, A., Soori, R., Choobineh, S. & Tirani, Z. M. Exercise promotes heart regeneration in aged rats by increasing regenerative factors in myocardial tissue. Physiol. Int. 107, 166–176 (2020).
Gulsin, G. S. et al. Cardiovascular determinants of aerobic exercise capacity in adults with type 2 diabetes. Diabetes Care 43, 2248–2256 (2020).
Zhang, H. et al. Pre-operative exercise therapy triggers anti-inflammatory trained immunity of Kupffer cells through metabolic reprogramming. Nat. Metab. 3, 843–858 (2021).
De Miguel, Z. et al. Exercise plasma boosts memory and dampens brain inflammation via clusterin. Nature 600, 494–499 (2021).
Wilson, R. J. et al. Voluntary running protects against neuromuscular dysfunction following hindlimb ischemia-reperfusion in mice. J. Appl. Physiol. 126, 193–201 (2019).
Li, C. et al. Early wheel-running promotes functional recovery by improving mitochondria metabolism in olfactory ensheathing cells after ischemic stroke in rats. Behav. Brain Res. 361, 32–38 (2019).
Kehm, R. D. et al. Recreational physical activity is associated with reduced breast cancer risk in adult women at high risk for breast cancer: a cohort study of women selected for familial and genetic risk. Cancer Res. 80, 116–125 (2020).
Padr O, A. I. et al. Exercise training protects against cancer-induced cardiac remodeling in an animal model of urothelial carcinoma. Arch. Biochem. Biophys. 645, 12–18 (2018).
Hagar, A. et al. Endurance training slows breast tumor growth in mice by suppressing Treg cells recruitment to tumors. BMC Cancer 19, 536 (2019).
Vervoort, M. Regeneration and development in animals. Biol. Theory 6, 25–35 (2011).
Poss, K. D. Advances in understanding tissue regenerative capacity and mechanisms in animals. Nat. Rev. Genet. 11, 710–722 (2010).
Galliot, B., Crescenzi, M., Jacinto, A. & Tajbakhsh, S. Trends in tissue repair and regeneration. Development 144, 357–364 (2017).
Fu, X. Repair cell first, then regenerate the tissues and organs. Mil. Med. Res. 8, 2 (2021).
Bergmann, O. et al. Evidence for cardiomyocyte renewal in humans. Science 324, 98–102 (2009).
He, L. & Zhou, B. Cardiomyocyte proliferation: remove brakes and push accelerators. Cell Res. 27, 959–960 (2017).
Nakada, D., Levi, B. P. & Morrison, S. J. Integrating physiological regulation with stem cell and tissue homeostasis. Neuron 70, 703–718 (2011).
Armada-da-Silva, P. A., Pereira, C., Amado, S. & Veloso, A. P. Role of physical exercise for improving posttraumatic nerve regeneration. Int. Rev. Neurobiol. 109, 125–149 (2013).
Zarei-Kheirabadi, M. et al. Human embryonic stem cell-derived neural stem cells encapsulated in hyaluronic acid promotes regeneration in a contusion spinal cord injured rat. Int. J. Biol. Macromol. 148, 1118–1129 (2020).
Kim, S. G. A cell-based approach to dental pulp regeneration using mesenchymal stem cells: a scoping review. Int. J. Mol. Sci. 22, 4357 (2021).
Čamernik, K. et al. Mesenchymal stem cells in the musculoskeletal system: from animal models to human tissue regeneration? Stem Cell Rev. Rep. 14, 346–369 (2018).
Spitzhorn, L. et al. Transplanted human pluripotent stem cell-derived mesenchymal stem cells support liver regeneration in Gunn rats. Stem Cells Dev. 27, 1702–1714 (2018).
Granata, C. et al. High-intensity training induces non-stoichiometric changes in the mitochondrial proteome of human skeletal muscle without reorganisation of respiratory chain content. Nat. Commun. 12, 7056 (2021).
Janssen, I., Heymsfield, S. B., Wang, Z. & Ross, R. Skeletal muscle mass and distribution in 468 men and women aged 18–88 yr. J. Appl. Physiol. 89, 81–88 (2000).
Jarvinen, T. A. et al. Muscle injuries: optimising recovery. Best. Pract. Res. Clin. Rheumatol. 21, 317–331 (2007).
Joyner, M. J. & Coyle, E. F. Endurance exercise performance: the physiology of champions. J. Physiol. 586, 35–44 (2008).
Qaisar, R., Bhaskaran, S. & Van Remmen, H. Muscle fiber type diversification during exercise and regeneration. Free Radic. Biol. Med. 98, 56–67 (2016).
Konopka, A. R. & Harber, M. P. Skeletal muscle hypertrophy after aerobic exercise training. Exerc. Sport Sci. Rev. 42, 53–61 (2014).
Koulmann, N. et al. Physical exercise during muscle regeneration improves recovery of the slow/oxidative phenotype. Muscle Nerve 55, 91–100 (2016).
Richard-Bulteau, H., Serrurier, B., Crassous, B., Banzet, S. & Koulmann, N. Recovery of skeletal muscle mass after extensive injury: positive effects of increased contractile activity. Am. J. Physiol. Cell Physiol. 294, C467–C476 (2008).
Hughes, D. C., Ellefsen, S. & Baar, K. Adaptations to endurance and strength training. Cold Spring Harb. Perspect. Med. 8, a29769 (2018).
Friedmann-Bette et al. Strength training effects on muscular regeneration after ACL reconstruction. Med. Sci. Sports Exerc. 50, 1152–1161 (2018).
Izadi, M. R., Habibi, A., Khodabandeh, Z. & Nikbakht, M. Synergistic effect of high-intensity interval training and stem cell transplantation with amniotic membrane scaffold on repair and rehabilitation after volumetric muscle loss injury. Cell Tissue Res. 383, 765–779 (2021).
Grounds, M. D. The need to more precisely define aspects of skeletal muscle regeneration. Int. J. Biochem. Cell Biol. 56, 56–65 (2014).
Kaczmarek, A. et al. The role of satellite cells in skeletal muscle regeneration—the effect of exercise and age. Biology 10, 1056 (2021).
Yin, H., Price, F. & Rudnicki, M. A. Satellite cells and the muscle stem cell niche. Physiol. Rev. 93, 23–67 (2013).
Fukada, S. & Nakamura, A. Exercise/resistance training and muscle stem cells. Endocrinol. Metab. 36, 737–744 (2021).
Murach, K. A., Fry, C. S., Dupont Versteegden, E. E., McCarthy, J. J. & Peterson, C. A. Fusion and beyond: satellite cell contributions to loading‐induced skeletal muscle adaptation. FASEB J. 35, e21893 (2021).
Perandini, L. A., Chimin, P., Lutkemeyer, D. D. S. & Câmara, N. O. S. Chronic inflammation in skeletal muscle impairs satellite cells function during regeneration: can physical exercise restore the satellite cell niche? FASEB J. 285, 1973–1984 (2018).
Wang, H. et al. Altered macrophage phenotype transition impairs skeletal muscle regeneration. Am. J. Pathol. 184, 1167–1184 (2014).
Walton, R. G. et al. Human skeletal muscle macrophages increase following cycle training and are associated with adaptations that may facilitate growth. Sci. Rep. 9, 969 (2019).
Minari, A. L. A., Oyama, L. M. & Dos Santos, R. V. T. Downhill exercise-induced changes in gene expression related with macrophage polarization and myogenic cells in the triceps long head of rats. Inflammation 38, 209–217 (2015).
Madaro, L. et al. Denervation-activated STAT3–IL-6 signalling in fibro-adipogenic progenitors promotes myofibres atrophy and fibrosis. Nat. Cell Biol. 20, 917–927 (2018).
Farup, J., Madaro, L., Puri, P. L. & Mikkelsen, U. R. Interactions between muscle stem cells, mesenchymal-derived cells and immune cells in muscle homeostasis, regeneration and disease. Cell Death Dis. 6, e1830 (2015).
Joe, A. W. B. et al. Muscle injury activates resident fibro/adipogenic progenitors that facilitate myogenesis. Nat. Cell Biol. 12, 153–163 (2010).
Saito, Y., Chikenji, T. S., Matsumura, T., Nakano, M. & Fujimiya, M. Exercise enhances skeletal muscle regeneration by promoting senescence in fibro-adipogenic progenitors. Nat. Commun. 11, 889 (2020).
Specker, B. & Minett, M. Can physical activity improve peak bone mass? Curr. Osteoporos. Rep. 11, 229–236 (2013).
Kemmler, W., Bebenek, M., von Stengel, S. & Bauer, J. Peak-bone-mass development in young adults: effects of study program related levels of occupational and leisure time physical activity and exercise. A prospective 5-year study. Osteoporos. Int. 26, 653–662 (2015).
Gomez-Cabello, A., Ara, I., Gonzalez-Aguero, A., Casajus, J. A. & Vicente-Rodriguez, G. Effects of training on bone mass in older adults: a systematic review. Sports Med. 42, 301–325 (2012).
Suominen, H. Muscle training for bone strength. Aging Clin. Exp. Res. 18, 85–93 (2006).
Shahabi, S. et al. The effects of 8-week resistance and endurance trainings on bone strength compared to irisin injection protocol in mice. Adv. Biomed. Res. 10, 40 (2021).
Turner, C. H. Three rules for bone adaptation to mechanical stimuli. Bone 23, 399–407 (1998).
Davison, S. et al. Exercise-based correlates to calcaneal osteogenesis produced by a chronic training intervention. Bone 128, 115049 (2019).
Maes, C. Role and regulation of vascularization processes in endochondral bones. Calcif. Tissue Int. 92, 307–323 (2013).
Yao, Z. et al. Increase of both angiogenesis and bone mass in response to exercise depends on VEGF. J. Bone Miner. Res. 19, 1471–1480 (2004).
Holstein, J. H. et al. Exercise enhances angiogenesis during bone defect healing in mice. J. Orthop. Res. 29, 1086–1092 (2011).
Wazzani, R. et al. Physical activity and bone vascularization: a way to explore in bone repair context? Life 11, 783 (2021).
Flanigan, D. C., Harris, J. D., Trinh, T. Q., Siston, R. A. & Brophy, R. H. Prevalence of chondral defects in athletes’ knees: a systematic review. Med. Sci. Sports Exerc. 42, 1795–1801 (2010).
Perera, J. R., Gikas, P. D. & Bentley, G. The present state of treatments for articular cartilage defects in the knee. Ann. R. Coll. Surg. Engl. 94, 381–387 (2012).
Wellsandt, E. & Golightly, Y. Exercise in the management of knee and hip osteoarthritis. Curr. Opin. Rheumatol. 30, 151–159 (2018).
Raposo, F., Ramos, M. & Lúcia Cruz, A. Effects of exercise on knee osteoarthritis: a systematic review. Musculoskelet. Care 19, 399–435 (2021).
Vincent, K. R., Vasilopoulos, T., Montero, C. & Vincent, H. K. Eccentric and concentric resistance exercise comparison for knee osteoarthritis. Med. Sci. Sports Exerc. 51, 1977–1986 (2019).
Iijima, H. et al. Exercise intervention increases expression of bone morphogenetic proteins and prevents the progression of cartilage-subchondral bone lesions in a post-traumatic rat knee model. Osteoarthr. Cartil. 24, 1092–1102 (2016).
Assis, L. et al. Aerobic exercise training and low-level laser therapy modulate inflammatory response and degenerative process in an experimental model of knee osteoarthritis in rats. Osteoarthr. Cartil. 24, 169–177 (2016).
Steele, J., Bruce-Low, S., Smith, D., Osborne, N. & Thorkeldsen, A. Can specific loading through exercise impart healing or regeneration of the intervertebral disc? Spine J. 15, 2117–2121 (2015).
Fernandes, T. L. et al. Macrophage: a potential target on cartilage regeneration. Front. Immunol. 11, 111 (2020).
Kubosch, E. J. et al. The potential for synovium-derived stem cells in cartilage repair. Curr. Stem Cell Res. Ther. 13, 174–184 (2018).
Benmassaoud, M. M., Gultian, K. A., DiCerbo, M. & Vega, S. L. Hydrogel screening approaches for bone and cartilage tissue regeneration. Ann. NY Acad. Sci. 1460, 25–42 (2019).
Smith, J. K. Exercise as an adjuvant to cartilage regeneration therapy. Int. J. Mol. Sci. 21, 9471 (2020).
Liu, Y. et al. Exercise-induced piezoelectric stimulation for cartilage regeneration in rabbits. Sci. Transl. Med. 14, eabi7282 (2022).
Yokota, H., Leong, D. J. & Sun, H. B. Mechanical loading: bone remodeling and cartilage maintenance. Curr. Osteoporos. Rep. 9, 237–242 (2011).
Tong, X. et al. The effect of exercise on the prevention of osteoporosis and bone angiogenesis. Biomed. Res. Int. 2019, 8171897 (2019).
Qi, M. C., Zou, S. J., Han, L. C., Zhou, H. X. & Hu, J. Expression of bone‐related genes in bone marrow MSCs after cyclic mechanical strain: implications for distraction osteogenesis. Int. J. Oral Sci. 1, 143–150 (2009).
Schmid, M., Kröpfl, J. M. & Spengler, C. M. Changes in circulating stem and progenitor cell numbers following acute exercise in healthy human subjects: a systematic review and meta-analysis. Stem Cell Rev. Rep. 17, 1091–1120 (2021).
Chan, C. K. F. et al. Identification of the human skeletal stem cell. Cell 175, 43–56 (2018).
Ortinau, L. C. et al. Identification of functionally distinct Mx1+αSMA+ periosteal skeletal stem cells. Cell Stem Cell 25, 784–796 (2019).
Kylmaoja, E., Nakamura, M. & Tuukkanen, J. Osteoclasts and remodeling based bone formation. Curr. Stem Cell Res. Ther. 11, 626–633 (2016).
Marędziak, M., Śmieszek, A., Chrząstek, K., Basinska, K. & Marycz, K. Physical activity increases the total number of bone-marrow-derived mesenchymal stem cells, enhances their osteogenic potential, and inhibits their adipogenic properties. Stem Cells Int. 2015, 379093 (2015).
Kreja, L., Liedert, A., Hasni, S., Claes, L. & Ignatius, A. Mechanical regulation of osteoclastic genes in human osteoblasts. Biochem. Biophys. Res. Commun. 368, 582–587 (2008).
Kish, K., Mezil, Y., Ward, W. E., Klentrou, P. & Falk, B. Effects of plyometric exercise session on markers of bone turnover in boys and young men. Eur. J. Appl. Physiol. 115, 2115–2124 (2015).
Udagawa, N. et al. Osteoclast differentiation by RANKL and OPG signaling pathways. J. Bone Miner. Metab. 39, 19–26 (2021).
Sanchis-Gomar, F., Fiuza-Luces, C. & Lucia, A. Exercise as the master polypill of the 21st century for the prevention of cardiovascular disease. Int. J. Cardiol. 181, 360–361 (2015).
Lavie, C. J. et al. Exercise and the cardiovascular system. Circ. Res. 117, 207–219 (2015).
Utomi, V. et al. Systematic review and meta-analysis of training mode, imaging modality and body size influences on the morphology and function of the male athlete’s heart. Heart 99, 1727–1733 (2013).
Boström, P. et al. C/EBPβ controls exercise-induced cardiac growth and protects against pathological cardiac remodeling. Cell 143, 1072–1083 (2010).
Vujic, A. et al. Exercise induces new cardiomyocyte generation in the adult mammalian heart. Nat. Commun. 9, 1659 (2018).
Bei, Y. et al. Cardiac cell proliferation is not necessary for exercise-induced cardiac growth but required for its protection against ischaemia/reperfusion injury. J. Cell. Mol. Med. 21, 1648–1655 (2017).
Bansal, A. et al. Proteomic analysis reveals late exercise effects on cardiac remodeling following myocardial infarction. J. Proteomics 73, 2041–2049 (2010).
Yengo, C. M., Zimmerman, S. D., McCormick, R. J. & Thomas, D. P. Exercise training post-MI favorably modifies heart extracellular matrix in the rat. Med. Sci. Sports Exerc. 44, 1005–1012 (2012).
Haykowsky, M. et al. A meta-analysis of the effects of exercise training on left ventricular remodeling following myocardial infarction: start early and go longer for greatest exercise benefits on remodeling. Trials 12, 92 (2011).
Rahimi, M. et al. The effect of high intensity interval training on cardioprotection against ischemia-reperfusion injury in wistar rats. EXCLI J. 14, 237–246 (2015).
Jia, D., Hou, L., Lv, Y., Xi, L. & Tian, Z. Postinfarction exercise training alleviates cardiac dysfunction and adverse remodeling via mitochondrial biogenesis and SIRT1/PGC‐1α/PI3K/Akt signaling. J. Cell. Physiol. 234, 23705–23718 (2019).
Liu, X. et al. miR-222 is necessary for exercise-induced cardiac growth and protects against pathological cardiac remodeling. Cell Metab. 21, 584–595 (2015).
Otaka, N. et al. Myonectin is an exercise-induced myokine that protects the heart from ischemia-reperfusion injury. Circ. Res. 123, 1326–1338 (2018).
Shi, J. et al. miR-17-3p contributes to exercise-induced cardiac growth and protects against myocardial ischemia-reperfusion injury. Theranostics 7, 664–676 (2017).
Bei, Y. et al. Exercise-induced circulating extracellular vesicles protect against cardiac ischemia–reperfusion injury. Basic Res. Cardiol. 112, 38 (2017).
Garza, M. A. Cardiac remodeling and physical training post myocardial infarction. World J. Cardiol. 7, 52–64 (2015).
Garza, M. A., Wason, E. A., Cruger, J. R., Chung, E. & Zhang, J. Q. Strength training attenuates post-infarct cardiac dysfunction and remodeling. J. Physiol. Sci. 69, 523–530 (2019).
Mueller, S. et al. Effect of high-intensity interval training, moderate continuous training, or guideline-based physical activity advice on peak oxygen consumption in patients with heart failure with preserved ejection fraction. JAMA 325, 542–551 (2021).
Ellingsen, Ø. et al. High-intensity interval training in patients with heart failure with reduced ejection fraction. Circulation 135, 839–849 (2017).
Tan, J. et al. Moderate heart rate reduction promotes cardiac regeneration through stimulation of the metabolic pattern switch. Cell Rep. 38, 110468 (2022).
Sharman, J. E., La Gerche, A. & Coombes, J. S. Exercise and cardiovascular risk in patients with hypertension. Am. J. Hypertens. 28, 147–158 (2015).
Antunes, J. M. M., Ferreira, R. M. P. & Moreira-Gonçalves, D. Exercise training as therapy for cancer-induced cardiac cachexia. Trends Mol. Med. 24, 709–727 (2018).
Bond, A. M. et al. Differential timing and coordination of neurogenesis and astrogenesis in developing mouse hippocampal subregions. Brain Sci. 10, 909 (2020).
Moreno-Jiménez, E. P. et al. Adult hippocampal neurogenesis is abundant in neurologically healthy subjects and drops sharply in patients with Alzheimer’s disease. Nat. Med. 25, 554–560 (2019).
Boldrini, M. et al. Human hippocampal neurogenesis persists throughout aging. Cell Stem Cell 22, 589–599 (2018).
van Praag, H. Neurogenesis and exercise: past and future directions. Neuromol. Med. 10, 128–140 (2008).
Nam, S. M. et al. Effects of treadmill exercise on neural stem cells, cell proliferation, and neuroblast differentiation in the subgranular zone of the dentate gyrus in cyclooxygenase-2 knockout mice. Neurochem. Res. 38, 2559–2569 (2013).
Firth, J. et al. Effect of aerobic exercise on hippocampal volume in humans: a systematic review and meta-analysis. Neuroimage 166, 230–238 (2018).
Batcho, C., Stoquart, G. & Thonnard, J. Brisk walking can promote functional recovery in chronic stroke patients. J. Rehabil. Med. 45, 854–859 (2013).
Cumming, T. B., Tyedin, K., Churilov, L., Morris, M. E. & Bernhardt, J. The effect of physical activity on cognitive function after stroke: a systematic review. Int. Psychogeriatr. 24, 557–567 (2012).
Marzolini, S., Oh, P., McIlroy, W. & Brooks, D. The effects of an aerobic and resistance exercise training program on cognition following stroke. Neurorehab. Neural Repair. 27, 392–402 (2013).
Pang, M. Y. C., Charlesworth, S. A., Lau, R. W. K. & Chung, R. C. K. Using aerobic exercise to improve health outcomes and quality of life in stroke: evidence-based exercise prescription recommendations. Cerebrovasc. Dis. 35, 7–22 (2013).
Vahlberg, B., Cederholm, T., Lindmark, B., Zetterberg, L. & Hellström, K. Short-term and long-term effects of a progressive resistance and balance exercise program in individuals with chronic stroke: a randomized controlled trial. Disabil. Rehabil. 39, 1615–1622 (2016).
Mehta, S. et al. Resistance training for gait speed and total distance walked during the chronic stage of stroke: a meta-analysis. Top. Stroke Rehabil. 19, 471–478 (2014).
Hu, J. et al. Constraint-induced movement therapy enhances AMPA receptor-dependent synaptic plasticity in the ipsilateral hemisphere following ischemic stroke. Neural Regen. Res. 16, 319 (2021).
Shabanzadeh, A. P. et al. Modifying PTEN recruitment promotes neuron survival, regeneration, and functional recovery after CNS injury. Cell Death Dis. 10, 567 (2019).
Tang, Y. et al. Effects of treadmill exercise on cerebral angiogenesis and MT1-MMP expression after cerebral ischemia in rats. Brain Behav. 8, e1079 (2018).
Chang, A. et al. Neurogenesis in the chronic lesions of multiple sclerosis. Brain 131, 2366–2375 (2008).
Guo, L. Y., Lozinski, B. & Yong, V. W. Exercise in multiple sclerosis and its models: focus on the central nervous system outcomes. J. Neurosci. Res. 98, 509–523 (2020).
Sandrow-Feinberg, H. R. & Houlé, J. D. Exercise after spinal cord injury as an agent for neuroprotection, regeneration and rehabilitation. Brain Res. 1619, 12–21 (2015).
Chew, C. & Sengelaub, D. Exercise promotes recovery after motoneuron injury via hormonal mechanisms. Neural Regen. Res. 15, 1373 (2020).
Davaa, G. et al. Exercise ameliorates spinal cord injury by changing DNA methylation. Cells 10, 143 (2021).
Jung, S., Seo, T. & Kim, D. Treadmill exercise facilitates recovery of locomotor function through axonal regeneration following spinal cord injury in rats. J. Exerc. Rehabil. 12, 284–292 (2016).
Chang, W. et al. Locomotion dependent neuron-glia interactions control neurogenesis and regeneration in the adult zebrafish spinal cord. Nat. Commun. 12, 4857 (2021).
Hesp, Z. C. et al. Proliferating NG2-cell-dependent angiogenesis and scar formation alter axon growth and functional recovery after spinal cord injury in mice. J. Neurosci. 38, 1366–1382 (2018).
Stenudd, M., Sabelström, H. & Frisén, J. Role of endogenous neural stem cells in spinal cord injury and repair. JAMA Neurol. 72, 235–237 (2015).
Hackett, A. R. et al. Injury type-dependent differentiation of NG2 glia into heterogeneous astrocytes. Exp. Neurol. 308, 72–79 (2018).
Tashiro, S. et al. Current progress of rehabilitative strategies in stem cell therapy for spinal cord injury: a review. NPJ Regen. Med. 6, 81 (2021).
Takeoka, A. et al. Axon regeneration can facilitate or suppress hindlimb function after olfactory ensheathing glia transplantation. J. Neurosci. 31, 4298–4310 (2011).
Hwang, D. H. et al. Survival of neural stem cell grafts in the lesioned spinal cord is enhanced by a combination of treadmill locomotor training via insulin-like growth factor-1 signaling. J. Neurosci. 34, 12788–12800 (2014).
Benowitz, L. I. & Popovich, P. G. Inflammation and axon regeneration. Curr. Opin. Neurol. 24, 577–583 (2011).
Conforti, L., Gilley, J. & Coleman, M. P. Wallerian degeneration: an emerging axon death pathway linking injury and disease. Nat. Rev. Neurosci. 15, 394–409 (2014).
Kluding, P. M. et al. The effect of exercise on neuropathic symptoms, nerve function, and cutaneous innervation in people with diabetic peripheral neuropathy. J. Diabetes Complicat. 26, 424–429 (2012).
Allet, L. et al. The gait and balance of patients with diabetes can be improved: a randomised controlled trial. Diabetologia 53, 458–466 (2010).
Zimmer, P. et al. Eight-week, multimodal exercise counteracts a progress of chemotherapy-induced peripheral neuropathy and improves balance and strength in metastasized colorectal cancer patients: a randomized controlled trial. Support. Care Cancer 26, 615–624 (2018).
Dhawan, S., Andrews, R., Kumar, L., Wadhwa, S. & Shukla, G. A randomized controlled trial to assess the effectiveness of muscle strengthening and balancing exercises on chemotherapy-induced peripheral neuropathic pain and quality of life among cancer patients. Cancer Nurs. 43, 269–280 (2020).
Ballestero-Pérez, R. et al. Effectiveness of nerve gliding exercises on carpal tunnel syndrome: a systematic review. J. Manip. Physiol. Ther. 40, 50–59 (2017).
Streckmann, F. et al. Exercise program improves therapy-related side-effects and quality of life in lymphoma patients undergoing therapy. Ann. Oncol. 25, 493–499 (2014).
Kleckner, I. R. et al. Effects of exercise during chemotherapy on chemotherapy-induced peripheral neuropathy: a multicenter, randomized controlled trial. Support. Care Cancer 26, 1019–1028 (2018).
Bland, K. A. et al. Effect of exercise on taxane chemotherapy–induced peripheral neuropathy in women with breast cancer: a randomized controlled trial. Clin. Breast Cancer 19, 411–422 (2019).
Neto, W. K. et al. Ladder-based resistance training elicited similar ultrastructural adjustments in forelimb and hindlimb peripheral nerves of young adult Wistar rats. Exp. Brain Res. 239, 2583–2592 (2021).
Martins, D. F. et al. Long-term regular eccentric exercise decreases neuropathic pain-like behavior and improves motor functional recovery in an axonotmesis mouse model: the role of insulin-like growth factor-1. Mol. Neurobiol. 55, 6155–6168 (2018).
de Moraes, A. A., de Almeida, C. A. S., Lucas, G., Thomazini, J. A. & DeMaman, A. S. Effect of swimming training on nerve morphological recovery after compressive injury. Neurol. Res. 40, 955–962 (2018).
Liao, C. et al. Effects of swimming exercise on nerve regeneration in a rat sciatic nerve transection model. Biomedicine 7, 3 (2017).
Coelho Ferreira, M. et al. Effects of two intensities of treadmill exercise on neuromuscular recovery after median nerve crush injury in Wistar rats. J. Exerc. Rehabil. 15, 392–400 (2019).
Michalopoulos, G. K. & Bhushan, B. Liver regeneration: biological and pathological mechanisms and implications. Nat. Rev. Gastroenterol. Hepatol. 18, 40–55 (2021).
Linecker, M. et al. Exercise improves outcomes of surgery on fatty liver in mice. Ann. Surg. 271, 347–355 (2020).
Fard Aghaie, M. H. et al. The effects of physical prehabilitation: Improved liver regeneration and mitochondrial function after ALPPS operation in a rodent model. J. Hepatobiliary Pancreat. Sci. 28, 692–702 (2021).
Emery, C. F., Kiecolt-Glaser, J. K., Glaser, R., Malarkey, W. B. & Frid, D. J. Exercise accelerates wound healing among healthy older adults: a preliminary investigation. J. Gerontol. A Biol. Sci. Med. Sci. 60, 1432–1436 (2005).
Keylock, K. T. et al. Exercise accelerates cutaneous wound healing and decreases wound inflammation in aged mice. Am. J. Physiol. Regul. Integr. Comp. Physiol. 294, R179–R184 (2008).
Mutlak, O., Aslam, M. & Standfield, N. The influence of exercise on ulcer healing in patients with chronic venous insufficiency. Int. Angiol. 37, 160–168 (2018).
Zogaib, F. G. & Monte-Alto-Costa, A. Moderate intensity physical training accelerates healing of full-thickness wounds in mice. Braz. J. Med. Biol. Res. 44, 1025–1035 (2011).
Keylock, T., Meserve, L. & Wolfe, A. Low-intensity exercise accelerates wound healing in diabetic mice. Wounds 30, 68–71 (2018).
Emmons, R., Niemiro, G. M., Owolabi, O. & De Lisio, M. Acute exercise mobilizes hematopoietic stem and progenitor cells and alters the mesenchymal stromal cell secretome. J. Appl. Physiol. 120, 624–632 (2016).
Emmons, R., Ngu, M., Xu, G., Hernández-Saavedra, D. & Lisio, M. D. Effects of obesity and exercise on bone marrow progenitor cells following radiation. Med. Sci. Sports Exerc. 51, 1126–1136 (2019).
Frodermann, V. et al. Exercise reduces inflammatory cell production and cardiovascular inflammation via instruction of hematopoietic progenitor cells. Nat. Med. 25, 1761–1771 (2019).
Stelzer, I. et al. Ultra-endurance exercise induces stress and inflammation and affects circulating hematopoietic progenitor cell function. Scand. J. Med. Sci. Sports 25, e442–e450 (2015).
Appelbaum, F. R. Hematopoietic-cell transplantation at 50. N. Engl. J. Med. 357, 1472–1475 (2007).
De Lisio, M., Baker, J. M. & Parise, G. Exercise promotes bone marrow cell survival and recipient reconstitution post-bone marrow transplantation, which is associated with increased survival. Exp. Hematol. 41, 143–154 (2013).
Wiskemann, J. & Huber, G. Physical exercise as adjuvant therapy for patients undergoing hematopoietic stem cell transplantation. Bone Marrow Transplant. 41, 321–329 (2008).
Baumann, F. T. et al. Physical activity for patients undergoing an allogeneic hematopoietic stem cell transplantation: benefits of a moderate exercise intervention. Eur. J. Haematol. 87, 148–156 (2011).
Khan, K. M. & Scott, A. Mechanotherapy: how physical therapists’ prescription of exercise promotes tissue repair. Br. J. Sports Med. 43, 247–252 (2009).
Magliulo, L., Bondi, D., Pini, N., Marramiero, L. & Di Filippo, E. S. The wonder exerkines—novel insights: a critical state-of-the-art review. Mol. Cell. Biochem. 477, 105–113 (2022).
Safdar, A., Saleem, A. & Tarnopolsky, M. A. The potential of endurance exercise-derived exosomes to treat metabolic diseases. Nat. Rev. Endocrinol. 12, 504–517 (2016).
Hoffmann, C. & Weigert, C. Skeletal muscle as an endocrine organ: the role of myokines in exercise adaptations. Csh. Perspect. Med. 7, a29793 (2017).
Han, Y., You, X., Xing, W., Zhang, Z. & Zou, W. Paracrine and endocrine actions of bone—the functions of secretory proteins from osteoblasts, osteocytes, and osteoclasts. Bone Res. 6, 16 (2018).
Henriksen, T., Green, C. & Pedersen, B. K. Myokines in myogenesis and health. Recent Pat. Biotechnol. 6, 167–171 (2012).
Herrmann, M. et al. Interactions between muscle and bone—where physics meets biology. Biomolecules 10, 432 (2020).
Monemian, E. A. et al. Tissue regeneration from mechanical stretching of cell-cell adhesion. Tissue Eng. C Methods 25, 631–640 (2019).
Castillo, A. B. & Leucht, P. Bone homeostasis and repair: forced into shape. Curr. Rheumatol. Rep. 17, 58 (2015).
Dolan, C. P. et al. Digit specific denervation does not inhibit mouse digit tip regeneration. Dev. Biol. 486, 71–80 (2022).
Murthy, S. E., Dubin, A. E. & Patapoutian, A. Piezos thrive under pressure: mechanically activated ion channels in health and disease. Nat. Rev. Mol. Cell Biol. 18, 771–783 (2017).
Gudipaty, S. A. et al. Mechanical stretch triggers rapid epithelial cell division through Piezo1. Nature 543, 118–121 (2017).
Kefauver, J. M., Ward, A. B. & Patapoutian, A. Discoveries in structure and physiology of mechanically activated ion channels. Nature 587, 567–576 (2020).
He, L., Si, G., Huang, J., Samuel, A. D. T. & Perrimon, N. Mechanical regulation of stem-cell differentiation by the stretch-activated Piezo channel. Nature 555, 103–106 (2018).
Sun, W. et al. The mechanosensitive Piezo1 channel is required for bone formation. ELife 8, e47454 (2019).
Li, X. et al. Stimulation of Piezo1 by mechanical signals promotes bone anabolism. ELife 8, e49631 (2019).
Beech, D. J. Endothelial Piezo1 channels as sensors of exercise. J. Physiol. 596, 979–984 (2018).
Rozo, M., Li, L. & Fan, C. Targeting β1-integrin signaling enhances regeneration in aged and dystrophic muscle in mice. Nat. Med. 22, 889–896 (2016).
Boppart, M. D. & Mahmassani, Z. S. Integrin signaling: linking mechanical stimulation to skeletal muscle hypertrophy. Am. J. Physiol. Cell Physiol. 317, C629–C641 (2019).
Geiger, B., Spatz, J. P. & Bershadsky, A. D. Environmental sensing through focal adhesions. Nat. Rev. Mol. Cell Biol. 10, 21–33 (2009).
Plotkin, L. I., Davis, H. M., Cisterna, B. A. & Sáez, J. C. Connexins and pannexins in bone and skeletal muscle. Curr. Osteoporos. Rep. 15, 326–334 (2017).
Shen, H., Grimston, S., Civitelli, R. & Thomopoulos, S. Deletion of Connexin43 in osteoblasts/osteocytes leads to impaired muscle formation in mice. J. Bone Miner. Res. 30, 596–605 (2015).
Ren, Q., Chen, J. & Liu, Y. LRP5 and LRP6 in Wnt signaling: similarity and divergence. Front. Cell Dev. Biol. 9, 670960 (2021).
Williams, B. O. LRP5: from bedside to bench to bone. Bone 102, 26–30 (2017).
Zhao, L., Shim, J. W., Dodge, T. R., Robling, A. G. & Yokota, H. Inactivation of Lrp5 in osteocytes reduces Young’s modulus and responsiveness to the mechanical loading. Bone 54, 35–43 (2013).
Mehta, V. et al. The guidance receptor plexin D1 is a mechanosensor in endothelial cells. Nature 578, 290–295 (2020).
Li, X., Kordsmeier, J. & Xiong, J. New advances in osteocyte mechanotransduction. Curr. Osteoporos. Rep. 19, 101–106 (2021).
Wackerhage, H., Schoenfeld, B. J., Hamilton, D. L., Lehti, M. & Hulmi, J. J. Stimuli and sensors that initiate skeletal muscle hypertrophy following resistance exercise. J. Appl. Physiol. 126, 30–43 (2019).
Song, Y. et al. The mechanosensitive ion channel Piezo inhibits axon regeneration. Neuron 102, 373–389 (2019).
Li, F. et al. The Atr-Chek1 pathway inhibits axon regeneration in response to Piezo-dependent mechanosensation. Nat. Commun. 12, 3845 (2021).
Song, Z. et al. Mechanosensing in liver regeneration. Semin. Cell Dev. Biol. 71, 153–167 (2017).
Lorenz, L. et al. Mechanosensing by β1 integrin induces angiocrine signals for liver growth and survival. Nature 562, 128–132 (2018).
Lyon, R. C., Zanella, F., Omens, J. H. & Sheikh, F. Mechanotransduction in cardiac hypertrophy and failure. Circ. Res. 116, 1462–1476 (2015).
Jiang, F. et al. The mechanosensitive Piezo1 channel mediates heart mechano-chemo transduction. Nat. Commun. 12, 869 (2021).
Tsata, V. & Beis, D. In full force. Mechanotransduction and morphogenesis during homeostasis and tissue regeneration. J. Cardiovasc. Dev. Dis. 7, 40 (2020).
Santos, L., Ugun-Klusek, A., Coveney, C. & Boocock, D. J. Multiomic analysis of stretched osteocytes reveals processes and signalling linked to bone regeneration and cancer. NPJ Regen. Med. 6, 32 (2021).
Tanaka, S. & Matsumoto, T. Sclerostin: from bench to bedside. J. Bone Miner. Metab. 39, 332–340 (2021).
Crossland, H. et al. Focal adhesion kinase is required for IGF-1-mediated growth of skeletal muscle cells via a TSC2/mTOR/S6K1-associated pathway. Am. J. Physiol. Endocrinol. Metab. 305, E183–E193 (2013).
Sato, T. et al. A FAK/HDAC5 signaling axis controls osteocyte mechanotransduction. Nat. Commun. 11, 3282 (2020).
Dupont, S. et al. Role of YAP/TAZ in mechanotransduction. Nature 474, 179–183 (2011).
Aragona, M. et al. A mechanical checkpoint controls multicellular growth through YAP/TAZ regulation by actin-processing factors. Cell 154, 1047–1059 (2013).
Wang, L. et al. Integrin-YAP/TAZ-JNK cascade mediates atheroprotective effect of unidirectional shear flow. Nature 540, 579–582 (2016).
Zheng, Y. & Pan, D. The Hippo signaling pathway in development and disease. Dev. Cell 50, 264–282 (2019).
Piccolo, S., Dupont, S. & Cordenonsi, M. The biology of YAP/TAZ: Hippo signaling and beyond. Physiol. Rev. 94, 1287–1312 (2014).
Ma, S., Meng, Z., Chen, R. & Guan, K. The Hippo pathway: biology and pathophysiology. Annu. Rev. Biochem. 88, 577–604 (2019).
Chang, Y., Wu, J., Wang, C. & Jang, A. C. C. Hippo signaling-mediated mechanotransduction in cell movement and cancer metastasis. Front. Mol. Biosci. 6, 157 (2020).
Liu, Q. et al. Suppressing Hippo signaling in the stem cell niche promotes skeletal muscle regeneration. Stem Cells 39, 737–749 (2021).
Gabriel, B. M., Hamilton, D. L., Tremblay, A. M. & Wackerhage, H. The Hippo signal transduction network for exercise physiologists. J. Appl. Physiol. 120, 1105–1117 (2016).
Ziouti, F. et al. NOTCH signaling is activated through mechanical strain in human bone marrow-derived mesenchymal stromal cells. Stem Cells Int. 2019, 5150634 (2019).
Stassen, O. M. J. A., Ristori, T. & Sahlgren, C. M. Notch in mechanotransduction–from molecular mechanosensitivity to tissue mechanostasis. J. Cell Sci. 133, jcs250738 (2020).
Arthur, S. T. & Cooley, I. D. The effect of physiological stimuli on sarcopenia; impact of Notch and Wnt signaling on impaired aged skeletal muscle repair. Int. J. Biol. Sci. 8, 731–760 (2012).
Bi, P. et al. Stage-specific effects of Notch activation during skeletal myogenesis. ELife 5, e17355 (2016).
Fujimaki, S. et al. Functional overload enhances satellite cell properties in skeletal muscle. Stem Cells Int. 2016, 7619418 (2016).
Lin, J. et al. Swimming exercise stimulates IGF1/PI3K/Akt and AMPK/SIRT1/PGC1α survival signaling to suppress apoptosis and inflammation in aging hippocampus. Aging 12, 6852–6864 (2020).
Feng, L., Li, B., Xi, Y., Cai, M. & Tian, Z. Aerobic exercise and resistance exercise alleviate skeletal muscle atrophy through IGF-1/IGF-1R-PI3K/Akt pathway in mice with myocardial infarction. Am. J. Physiol. Cell Physiol. 322, C164–C176 (2022).
Kraemer, W. J., Ratamess, N. A. & Nindl, B. C. Recovery responses of testosterone, growth hormone, and IGF-1 after resistance exercise. J. Appl. Physiol. 122, 549–558 (2017).
Yu, T., Chang, Y., Gao, X., Li, H. & Zhao, P. Dynamic expression and the role of BDNF in exercise-induced skeletal muscle regeneration. Int. J. Sports Med. 38, 959–966 (2017).
Li, S. et al. MOTS-c and exercise restore cardiac function by activating of NRG1-ErbB signaling in diabetic rats. Front. Endocrinol. 13, 812032 (2022).
Yoshida, T. & Delafontaine, P. Mechanisms of IGF-1-mediated regulation of skeletal muscle hypertrophy and atrophy. Cells 9, 1970 (2020).
Fink, J., Schoenfeld, B. J. & Nakazato, K. The role of hormones in muscle hypertrophy. Phys. Sportsmed. 46, 129–134 (2018).
Guntur, A. R. & Rosen, C. J. IGF-1 regulation of key signaling pathways in bone. Bonekey Rep. 2, 437 (2013).
Bikle, D. D. et al. Role of IGF-I signaling in muscle bone interactions. Bone 80, 79–88 (2015).
McMullen, J. R. et al. Phosphoinositide 3-kinase(p110α) plays a critical role for the induction of physiological, but not pathological, cardiac hypertrophy. Proc. Natl Acad. Sci. USA 100, 12355–12360 (2003).
Kim, J. et al. Insulin-like growth factor i receptor signaling is required for exercise-induced cardiac hypertrophy. Mol. Endocrinol. 22, 2531–2543 (2008).
Gumà, A., Martínez-Redondo, V., López-Soldado, I., Cantó, C. & Zorzano, A. Emerging role of neuregulin as a modulator of muscle metabolism. Am. J. Physiol. Endocrinol. Metab. 298, E742–E750 (2010).
D Uva, G. et al. ERBB2 triggers mammalian heart regeneration bypromoting cardiomyocyte dedifferentiation andproliferation. Nat. Cell Biol. 17, 627–638 (2015).
Cai, M. X. et al. Exercise training activates neuregulin 1/ErbB signaling and promotes cardiac repair in a rat myocardial infarction model. Life Sci. 149, 1–9 (2016).
Gubert, C. & Hannan, A. J. Exercise mimetics: harnessing the therapeutic effects of physical activity. Nat. Rev. Drug Discov. 20, 862–879 (2021).
Li, Y. et al. Protection against acute cerebral ischemia/reperfusion injury by Leonuri Herba Total Alkali via modulation of BDNF-TrKB-PI3K/Akt signaling pathway in rats. Biomed. Pharmacother. 133, 111021 (2021).
Chang, M., Park, C., Rhie, S., Shim, W. & Kim, D. Early treadmill exercise increases macrophage migration inhibitory factor expression after cerebral ischemia/reperfusion. Neural Regen. Res. 14, 1230–1236 (2019).
Zhang, Q., Deng, X., Sun, X., Xu, J. & Sun, F. Exercise promotes axon regeneration of newborn striatonigral and corticonigral projection neurons in rats after ischemic stroke. PLoS ONE 8, e80139 (2013).
Kowiański, P. et al. BDNF: A key factor with multipotent impact on brain signaling and synaptic plasticity. Cell. Mol. Neurobiol. 38, 579–593 (2018).
Liu, P. Z. & Nusslock, R. Exercise-mediated neurogenesis in the hippocampus via BDNF. Front. Neurosci. 12, 52 (2018).
Bilchak, J. N., Caron, G. & Cote, M. P. Exercise-induced plasticity in signaling pathways involved in motor recovery after spinal cord injury. Int. J. Mol. Sci. 22, 4858 (2021).
Weishaupt, N., Blesch, A. & Fouad, K. BDNF: the career of a multifaceted neurotrophin in spinal cord injury. Exp. Neurol. 238, 254–264 (2012).
McGregor, C. E. & English, A. W. The role of BDNF in peripheral nerve regeneration: activity-dependent treatments and Val66Met. Front. Cell. Neurosci. 12, 522 (2019).
English, A. W., Wilhelm, J. C. & Ward, P. J. Exercise, neurotrophins, and axon regeneration in the PNS. Physiology 29, 437–445 (2014).
Reddy, L. V. K., Murugan, D., Mullick, M., Begum Moghal, E. T. & Sen, D. Recent approaches for angiogenesis in search of successful tissue engineering and regeneration. Curr. Stem Cell Res. Ther. 15, 111–134 (2020).
Hu, K. & Olsen, B. R. The roles of vascular endothelial growth factor in bone repair and regeneration. Bone 91, 30–38 (2016).
Zhang, J. et al. Endothelial lactate controls muscle regeneration from ischemia by inducing M2-like macrophage polarization. Cell Metab. 31, 1136–1153 (2020).
Shibuya, M. Differential roles of vascular endothelial growth factor receptor-1 and receptor-2 in angiogenesis. J. Biochem. Mol. Biol. 39, 469–478 (2006).
Melincovici, C. S. et al. Vascular endothelial growth factor (VEGF)-key factor in normal and pathological angiogenesis. Rom. J. Morphol. Embryol. 59, 455–467 (2018).
Tang, K., Xia, F. C., Wagner, P. D. & Breen, E. C. Exercise-induced VEGF transcriptional activation in brain, lung and skeletal muscle. Respir. Physiol. Neurobi. 170, 16–22 (2010).
Pourheydar, B., Biabanghard, A., Azari, R., Khalaji, N. & Chodari, L. Exercise improves aging-related decreased angiogenesis through modulating VEGF-A, TSP-1 and p-NF-Ƙb protein levels in myocardiocytes. J. Cardiovasc. Thorac. Res. 12, 129–135 (2020).
Tryfonos, A. et al. Exercise training enhances angiogenesis-related gene responses in skeletal muscle of patients with chronic heart failure. Cells 10, 1915 (2021).
Chen, L., Bai, J. & Li, Y. miR-29 mediates exercise-induced skeletal muscle angiogenesis by targeting VEGFA, COL4A1 and COL4A2 via the PI3K/Akt signaling pathway. Mol. Med. Rep. 22, 661–670 (2020).
Da, Y. et al. Mechanical stress promotes biological functions of C2C12 myoblasts by activating PI3K/AKT/mTOR signaling pathway. Mol. Med. Rep. 21, 470–477 (2019).
Song, F. et al. Mechanical stress regulates osteogenesis and adipogenesis of rat mesenchymal stem cells through PI3K/Akt/GSK-3β/β-Catenin signaling pathway. Biomed. Res. Int. 2017, 6027402 (2017).
Liu, M. et al. Phosphorylated GSK-3β protects stress-induced apoptosis of myoblasts via the PI3K/Akt signaling pathway. Mol. Med. Rep. 22, 317–327 (2020).
Liang, J. et al. Promotion of aerobic exercise induced angiogenesis is associated with decline in blood pressure in hypertension. Hypertension 77, 1141–1153 (2021).
Laplante, M. & Sabatini, D. M. mTOR signaling in growth control and disease. Cell 149, 274–293 (2012).
Watson, K. & Baar, K. mTOR and the health benefits of exercise. Semin. Cell Dev. Biol. 36, 130–139 (2014).
Baraldo, M. et al. Skeletal muscle mTORC1 regulates neuromuscular junction stability. J. Cachexia Sarcopenia Muscle 11, 208–225 (2020).
Chen, Z. et al. Exercise protects proliferative muscle satellite cells against exhaustion via the Igfbp7-Akt-mTOR axis. Theranostics 10, 6448–6466 (2020).
Liao, J., Li, Y., Zeng, F. & Wu, Y. Regulation of mTOR pathway in exercise-induced cardiac hypertrophy. Int. J. Sports Med. 36, 343–350 (2015).
Chen, K. et al. Exercise training improves motor skill learning via selective activation of mTOR. Sci. Adv. 5, w1888 (2019).
Kar, A. N. et al. MicroRNAs 21 and 199a-3p regulate axon growth potential through modulation of Pten and mTor mRNAs. eNeuro 8, 121–155 (2021).
Valvezan, A. J. & Manning, B. D. Molecular logic of mTORC1 signalling as a metabolic rheostat. Nat. Metab. 1, 321–333 (2019).
Deleyto-Seldas, N. & Efeyan, A. The mTOR-autophagy axis and the control of metabolism. Front. Cell Dev. Biol. 9, 655731 (2021).
Jang, Y. Endurance exercise-induced expression of autophagy-related protein coincides with anabolic expression and neurogenesis in the hippocampus of the mouse brain. Neuroreport 31, 442–449 (2020).
Ding, S. et al. C/EBPB-CITED4 in exercised heart. Adv. Exp. Med. Biol. 1000, 247–259 (2017).
Lerchenmüller, C. et al. CITED4 protects against adverse remodeling in response to physiological and pathological stress. Circ. Res. 127, 631–646 (2020).
Bezzerides, V. J. et al. CITED4 induces physiologic hypertrophy and promotes functional recovery after ischemic injury. JCI Insight 1, e85904 (2016).
Bahramian, A., Mirzaei, B., Karimzadeh, F., Ramhmaninia, F. & Hemmatinafar, M. The effects of exercise training intensity on the expression of C/EBPβ and CITED4 in rats with myocardial infarction. Asian J. Sports Med. 9, e59300 (2018).
Ryall, K. A., Bezzerides, V. J., Rosenzweig, A. & Saucerman, J. J. Phenotypic screen quantifying differential regulation of cardiac myocyte hypertrophy identifies CITED4 regulation of myocyte elongation. J. Mol. Cell. Cardiol. 72, 74–84 (2014).
Zeng, Z. et al. Exercise-induced autophagy suppresses sarcopenia through Akt/mTOR and Akt/FoxO3a signal pathways and AMPK-mediated mitochondrial quality control. Front. Physiol. 11, 583478 (2020).
Sanchez, A. M. J., Candau, R. B. & Bernardi, H. FoxO transcription factors: their roles in the maintenance of skeletal muscle homeostasis. Cell. Mol. Life Sci. 71, 1657–1671 (2014).
Rathbone, C. R., Booth, F. W. & Lees, S. J. FoxO3a preferentially induces p27Kip1 expression while impairing muscle precursor cell-cycle progression. Muscle Nerve 37, 84–89 (2008).
Liu, C. et al. Effect of RNA oligonucleotide targeting Foxo-1 on muscle growth in normal and cancer cachexia mice. Cancer Gene Ther. 14, 945–952 (2007).
Wen, X., Jiao, L. & Tan, H. MAPK/ERK pathway as a central regulator in vertebrate organ regeneration. Int. J. Mol. Sci. 23, 1464 (2022).
Aharonov, A. et al. ERBB2 drives YAP activation and EMT-like processes during cardiac regeneration. Nat. Cell Biol. 22, 1346–1356 (2020).
Tane, S. et al. CDK inhibitors, p21Cip1 and p27Kip1, participate in cell cycle exit of mammalian cardiomyocytes. Biochem. Biophys. Res. Commun. 443, 1105–1109 (2014).
Mohamed, T. et al. Regulation of cell cycle to stimulate adult cardiomyocyte proliferation and cardiac regeneration. Cell 173, 104–116 (2018).
Zhu, L. et al. Remifentanil preconditioning promotes liver regeneration via upregulation of β-arrestin 2/ERK/cyclin D1 pathway. Biochem. Biophys. Res. Commun. 557, 69–76 (2021).
Liu, W. et al. Physical exercise promotes proliferation and differentiation of endogenous neural stem cells via ERK in rats with cerebral infarction. Mol. Med. Rep. 18, 1455–1464 (2018).
Brett, J. O. et al. Exercise rejuvenates quiescent skeletal muscle stem cells in old mice through restoration of Cyclin D1. Nat. Metab. 2, 307–317 (2020).
Kwon, J. H., Moon, K. M. & Min, K. W. Exercise-induced myokines can explain the importance of physical activity in the elderly: an overview. Healthcare 8, 378 (2020).
Zhang, L. et al. Medium-intensity treadmill exercise exerts beneficial effects on bone modeling through bone marrow mesenchymal stromal cells. Front. Cell Dev. Biol. 8, 600639 (2020).
Iijima, H. et al. Physiological exercise loading suppresses post-traumatic osteoarthritis progression via an increase in bone morphogenetic proteins expression in an experimental rat knee model. Osteoarthr. Cartil. 25, 964–975 (2017).
Zou, M. et al. The Smad dependent TGF-β and BMP signaling pathway in bone remodeling and therapies. Front. Mol. Biosci. 8, 593310 (2021).
Zuo, C. et al. Osteoblastogenesis regulation signals in bone remodeling. Osteoporos. Int. 23, 1653–1663 (2012).
Wu, M., Chen, G. & Li, Y. TGF-β and BMP signaling in osteoblast, skeletal development, and bone formation, homeostasis and disease. Bone Res. 4, 16009 (2016).
Chen, G., Deng, C. & Li, Y. TGF-β and BMP signaling in osteoblast differentiation and bone formation. Int. J. Biol. Sci. 8, 272–288 (2012).
Valladares-Ide, D. et al. Activation of protein synthesis, regeneration, and MAPK signaling pathways following repeated bouts of eccentric cycling. Am. J. Physiol. Endocrinol. Metab. 317, E1131–E1139 (2019).
Fan, W. & Evans, R. M. Exercise mimetics: impact on health and performance. Cell Metab. 25, 242–247 (2017).
Herzig, S. & Shaw, R. J. AMPK: guardian of metabolism and mitochondrial homeostasis. Nat. Rev. Mol. Cell Biol. 19, 121–135 (2018).
Garcia, D. & Shaw, R. J. AMPK: mechanisms of cellular energy sensing and restoration of metabolic balance. Mol. Cell 66, 789–800 (2017).
Chen, H., Fan, W., He, H. & Huang, F. PGC-1: a key regulator in bone homeostasis. J. Bone Miner. Metab. 40, 1–8 (2022).
Norrbom, J. et al. PGC-1alpha mRNA expression is influenced by metabolic perturbation in exercising human skeletal muscle. J. Appl. Physiol. 96, 189–194 (2004).
Koves, T. R. et al. Peroxisome proliferator-activated receptor-gamma co-activator 1alpha-mediated metabolic remodeling of skeletal myocytes mimics exercise training and reverses lipid-induced mitochondrial inefficiency. J. Biol. Chem. 280, 33588–33598 (2005).
Dinulovic, I., Furrer, R., Beer, M. & Ferry, A. Muscle PGC-1α modulates satellite cell number and proliferation by remodeling the stem cell niche. Skelet. Muscle 6, 39 (2016).
Handschin, C. The biology of PGC-1alpha and its therapeutic potential. Trends Pharmacol. Sci. 30, 322–329 (2009).
Sánchez-de-Diego, C. et al. Glucose restriction promotes osteocyte specification by activating a PGC-1α-dependent transcriptional program. iScience 15, 79–94 (2019).
Colaianni, G. et al. Deletion of the transcription factor PGC-1alpha in mice negatively regulates bone mass. Calcif. Tissue Int. 103, 638–652 (2018).
Wang, J. et al. Hippocampal PGC-1α-mediated positive effects on parvalbumin interneurons are required for the antidepressant effects of running exercise. Transl. Psychiatry 11, 222 (2021).
Wang, S., Dougherty, E. J. & Danner, R. L. PPARγ signaling and emerging opportunities for improved therapeutics. Pharmacol. Res. 111, 76–85 (2016).
McMeekin, L. J. et al. Estrogen-related receptor alpha (ERRα) is required for PGC-1α-dependent gene expression in the mouse brain. Neuroscience 479, 70–90 (2021).
Wang, L. et al. mTORC1-PGC1 axis regulates mitochondrial remodeling during reprogramming. FEBS J. 287, 108–121 (2020).
Thirupathi, A. & de Souza, C. T. Multi-regulatory network of ROS: the interconnection of ROS, PGC-1 alpha, and AMPK-SIRT1 during exercise. J. Physiol. Biochem. 73, 487–494 (2017).
Silva, F. C. D. et al. Effects of physical exercise on the expression of microRNAs: a systematic review. J. Strength Cond. Res. 34, 270–280 (2020).
Russell, A. P. et al. Regulation of miRNAs in human skeletal muscle following acute endurance exercise and short-term endurance training. J. Physiol. 591, 4637–4653 (2013).
Allen, D. L. et al. Effects of spaceflight on murine skeletal muscle gene expression. J. Appl. Physiol. 106, 582–595 (2009).
Mytidou, C. et al. Age-related exosomal and endogenous expression patterns of miR-1, miR-133a, miR-133b, and miR-206 in skeletal muscles. Front. Physiol. 12, 708278 (2021).
Chen, J. et al. The role of microRNA-1 and microRNA-133 in skeletal muscle proliferation and differentiation. Nat. Genet. 38, 228–233 (2006).
Elia, L. et al. Reciprocal regulation of microRNA-1 and insulin-like growth factor-1 signal transduction cascade in cardiac and skeletal muscle in physiological and pathological conditions. Circulation 120, 2377–2385 (2009).
Matheny, R. W. et al. RNA transcript expression of IGF-I/PI3K pathway components in regenerating skeletal muscle is sensitive to initial injury intensity. Growth Horm. IGF Res. 32, 14–21 (2017).
Lou, J. et al. Exercise promotes angiogenesis by enhancing endothelial cell fatty acid utilization via liver-derived extracellular vesicle miR-122-5p. J. Sport Health Sci. 11, 495–508 (2022).
Yang, H. et al. Treadmill exercise influences the microRNA profiles in the bone tissues of mice. Exp. Ther. Med. 22, 1035 (2021).
Zeng, H. et al. MicroRNA miR-23a cluster promotes osteocyte differentiation by regulating TGF-β signalling in osteoblasts. Nat. Commun. 8, 15000 (2017).
Groven, R. V. M., van Koll, J., Poeze, M., Blokhuis, T. J. & van Griensven, M. miRNAs related to different processes of fracture healing: an integrative overview. Front. Surg. 8, 786564 (2021).
Pelozin, B. R. A., Soci, U. P. R., Gomes, J. L. P., Oliveira, E. M. & Fernandes, T. mTOR signaling-related microRNAs as cardiac hypertrophy modulators in high-volume endurance training. J. Appl. Physiol. 132, 126–139 (2022).
Wu, X. et al. ADAR2 increases in exercised heart and protects against myocardial infarction and doxorubicin-induced cardiotoxicity. Mol. Ther. 30, 400–414 (2022).
Pons-Espinal, M. et al. MiR-135a-5p is critical for exercise-induced adult neurogenesis. Stem Cell Rep. 12, 1298–1312 (2019).
Liu, G., Detloff, M. R., Miller, K. N., Santi, L. & Houle, J. D. Exercise modulates microRNAs that affect the PTEN/mTOR pathway in rats after spinal cord injury. Exp. Neurol. 233, 447–456 (2012).
Bonilauri, B. & Dallagiovanna, B. Long non-coding RNAs are differentially expressed after different exercise training programs. Front. Physiol. 11, 567614 (2020).
Li, Y., Chen, X., Sun, H. & Wang, H. Long non-coding RNAs in the regulation of skeletal myogenesis and muscle diseases. Cancer Lett. 417, 58–64 (2018).
Wohlwend, M. et al. The exercise-induced long noncoding RNA CYTOR promotes fast-twitch myogenesis in aging. Sci. Transl. Med. 13, c7367 (2021).
Gao, R. et al. Long noncoding RNA cardiac physiological hypertrophy-associated regulator induces cardiac physiological hypertrophy and promotes functional recovery after myocardial ischemia-reperfusion injury. Circulation 144, 303–317 (2021).
Li, H. et al. lncExACT1 and DCHS2 regulate physiological and pathological cardiac growth. Circulation 145, 1218–1233 (2022).
Statello, L., Guo, C., Chen, L. & Huarte, M. Gene regulation by long non-coding RNAs and its biological functions. Nat. Rev. Mol. Cell Biol. 22, 96–118 (2021).
Vincent, E. E. et al. Differential effects of AMPK agonists on cell growth and metabolism. Oncogene 34, 3627–3639 (2015).
Narkar, V. A. et al. AMPK and PPARδ agonists are exercise mimetics. Cell 134, 405–415 (2008).
Ehrenborg, E. & Krook, A. Regulation of skeletal muscle physiology and metabolism by peroxisome proliferator-activated receptor δ. Pharmacol. Rev. 61, 373–393 (2009).
Hardie, D. G. AMP-activated protein kinase: a cellular energy sensor with a key role in metabolic disorders and in cancer. Biochem. Soc. Trans. 39, 1–13 (2011).
Višnjić, D., Lalić, H., Dembitz, V., Tomić, B. & Smoljo, T. AICAr, a widely used AMPK activator with important AMPK-independent effects: a systematic review. Cells 10, 1095 (2021).
Chiang, C. et al. Metformin-treated cancer cells modulate macrophage polarization through AMPK-NF-κB signaling. Oncotarget 8, 20706–20718 (2017).
Mallik, R. & Chowdhury, T. A. Metformin in cancer. Diabetes Res. Clin. Pract. 143, 409–419 (2018).
Ouchi, N., Shibata, R. & Walsh, K. AMP-activated protein kinase signaling stimulates VEGF expression and angiogenesis in skeletal muscle. Circ. Res. 96, 838–846 (2005).
Zibrova, D. et al. GFAT1 phosphorylation by AMPK promotes VEGF-induced angiogenesis. Biochem. J. 474, 983–1001 (2017).
Kobilo, T., Yuan, C. & van Praag, H. Endurance factors improve hippocampal neurogenesis and spatial memory in mice. Learn. Mem. 18, 103–107 (2011).
Guerrieri, D. & van Praag, H. Exercise-mimetic AICAR transiently benefits brain function. Oncotarget 6, 18293–18313 (2015).
Wrann, C. D. et al. Exercise induces hippocampal BDNF through a PGC-1α/FNDC5 pathway. Cell Metab. 18, 649–659 (2013).
Giaccari, A., Solini, A., Frontoni, S. & Del Prato, S. Metformin benefits: another example for alternative energy substrate mechanism? Diabetes Care 44, 647–654 (2021).
Liu, Y., Tang, G., Zhang, Z., Wang, Y. & Yang, G. Metformin promotes focal angiogenesis and neurogenesis in mice following middle cerebral artery occlusion. Neurosci. Lett. 579, 46–51 (2014).
Zhu, X. et al. Metformin improves cognition of aged mice by promoting cerebral angiogenesis and neurogenesis. Aging 12, 17845–17862 (2020).
DiTacchio, K. A., Heinemann, S. F. & Dziewczapolski, G. Metformin treatment alters memory function in a mouse model of Alzheimer’s disease. J. Alzheimers Dis. 44, 43–48 (2015).
Stunes, A. K. et al. Skeletal effects of plyometric exercise and metformin in ovariectomized rats. Bone 132, 115193 (2020).
Chandrashekar, P. et al. Inactivation of PPARβ/δ adversely affects satellite cells and reduces postnatal myogenesis. Am. J. Physiol. Endocrinol. Metab. 309, E122–E131 (2015).
Angione, A. R., Jiang, C., Pan, D., Wang, Y. & Kuang, S. PPARδ regulates satellite cell proliferation and skeletal muscle regeneration. Skelet. Muscle 1, 33 (2011).
Nahlé, Z. et al. CD36-dependent regulation of muscle FoxO1 and PDK4 in the PPARδ/β-mediated adaptation to metabolic stress. J. Biol. Chem. 283, 14317–14326 (2008).
Phua, W. W. T. et al. PPARβ/δ agonism upregulates Forkhead Box A2 to reduce inflammation in C2C12 myoblasts and in skeletal muscle. Int. J. Mol. Sci. 21, 1747 (2020).
Gaudel, C., Schwartz, C., Giordano, C., Abumrad, N. A. & Grimaldi, P. A. Pharmacological activation of PPARβ promotes rapid and calcineurin-dependent fiber remodeling and angiogenesis in mouse skeletal muscle. Am. J. Physiol. Endocrinol. Metab. 295, E297–E304 (2008).
Wagner, N. et al. Peroxisome proliferator-activated receptor β stimulation induces rapid cardiac growth and angiogenesis via direct activation of calcineurin. Cardiovasc. Res. 83, 61–71 (2009).
Strosznajder, A. K., Wójtowicz, S., Jeżyna, M. J., Sun, G. Y. & Strosznajder, J. B. Recent insights on the role of PPAR-β/δ in neuroinflammation and neurodegeneration, and its potential target for therapy. Neuromol. Med. 23, 86–98 (2021).
Chamberlain, S., Gabriel, H., Strittmatter, W. & Didsbury, J. An exploratory phase IIa study of the PPAR delta/gamma agonist T3D-959 assessing metabolic and cognitive function in subjects with mild to moderate Alzheimer’s disease. J. Alzheimers Dis. 73, 1085–1103 (2020).
Xu, X. et al. Exercise training combined with angiotensin II receptor blockade limits post-infarct ventricular remodelling in rats. Cardiovasc. Res. 78, 523–532 (2008).
Tawfik, V. L. et al. Angiotensin receptor blockade mimics the effect of exercise on recovery after orthopaedic trauma by decreasing pain and improving muscle regeneration. J. Physiol. 598, 317–329 (2020).
Bostrom, P. et al. A PGC1-alpha-dependent myokine that drives brown-fat-like development of white fat and thermogenesis. Nature 481, 463–468 (2012).
Ma, Y. et al. Irisin promotes proliferation but inhibits differentiation in osteoclast precursor cells. FASEB J. 32, 5813–5823 (2018).
Qiao, X. et al. Irisin promotes osteoblast proliferation and differentiation via activating the MAP kinase signaling pathways. Sci. Rep. 6, 18732 (2016).
Chen, Z. et al. Recombinant irisin prevents the reduction of osteoblast differentiation induced by stimulated microgravity through increasing β-Catenin expression. Int. J. Mol. Sci. 21, 1259 (2020).
Kim, H. et al. Irisin mediates effects on bone and fat via αV integrin receptors. Cell 175, 1756–1768 (2018).
Jodeiri Farshbaf, M. & Alviña, K. Multiple roles in neuroprotection for the exercise derived myokine irisin. Front. Aging Neurosci. 13, 649929 (2021).
Lourenco, M. V. et al. Exercise-linked FNDC5/irisin rescues synaptic plasticity and memory defects in Alzheimer’s models. Nat. Med. 25, 165–175 (2019).
Waseem, R. et al. FNDC5/irisin: physiology and pathophysiology. Molecules 27, 1118 (2022).
Huang, S., Yang, S., Lo, J., Wu, S. & Tai, M. Irisin gene delivery ameliorates burn-induced sensory and motor neuropathy. Int. J. Mol. Sci. 21, 7798 (2020).
Garekani, E. T., Mohebbi, H., Kraemer, R. R. & Fathi, R. Exercise training intensity/volume affects plasma and tissue adiponectin concentrations in the male rat. Peptides 32, 1008–1012 (2011).
Zeng, Q. et al. Effects of exercise on adiponectin and adiponectin receptor levels in rats. Life Sci. 80, 454–459 (2007).
Inoue, A. et al. Exercise restores muscle stem cell mobilization, regenerative capacity and muscle metabolic alterations via adiponectin/AdipoR1 activation in SAMP10 mice. J. Cachexia Sarcopenia Muscle 8, 370–385 (2017).
Wang, P. et al. Potential involvement of adiponectin signaling in regulating physical exercise-elicited hippocampal neurogenesis and dendritic morphology in stressed mice. Front. Cell. Neurosci. 14, 189 (2020).
You, J. et al. Role of adiponectin-Notch pathway in cognitive dysfunction associated with depression and in the therapeutic effect of physical exercise. Aging Cell 20, e13387 (2021).
Lee, T. H. et al. Chronic AdipoRon treatment mimics the effects of physical exercise on restoring hippocampal neuroplasticity in diabetic mice. Mol. Neurobiol. 58, 4666–4681 (2021).
Li, A., Yau, S. Y., Machado, S., Yuan, T. F. & So, K. F. Adult neurogenic and antidepressant effects of adiponectin: a potential replacement for exercise? CNS Neurol. Disord. Drug Targets 14, 1129–1144 (2015).
Pedersen, B. K. & Febbraio, M. A. Muscles, exercise and obesity: skeletal muscle as a secretory organ. Nat. Rev. Endocrinol. 8, 457–465 (2012).
Peake, J. M., Della, G. P., Suzuki, K. & Nieman, D. C. Cytokine expression and secretion by skeletal muscle cells: regulatory mechanisms and exercise effects. Exerc. Immunol. Rev. 21, 8–25 (2015).
Reihmane, D. & Dela, F. Interleukin-6: possible biological roles during exercise. Eur. J. Sport Sci. 14, 242–250 (2014).
Storer, M. A. et al. Interleukin-6 regulates adult neural stem cell numbers during normal and abnormal post-natal development. Stem Cell Rep. 10, 1464–1480 (2018).
Cox, A. A. et al. Low-dose pulsatile interleukin-6 as a treatment option for diabetic peripheral neuropathy. Front. Endocrinol. 8, 89 (2017).
Schmitt, C., Kuhn, B., Zhang, X., Kivitz, A. J. & Grange, S. Disease-drug-drug interaction involving tocilizumab and simvastatin in patients with rheumatoid arthritis. Clin. Pharmacol. Ther. 89, 735–740 (2011).
Wedell-Neergaard, A. et al. Exercise-induced changes in visceral adipose tissue mass are regulated by IL-6 signaling: a randomized controlled trial. Cell Metab. 29, 844–855 (2019).
Trinh, B. et al. Blocking endogenous IL-6 impairs mobilization of free fatty acids during rest and exercise in lean and obese men. Cell Rep. Med. 2, 100396 (2021).
Furuichi, Y., Manabe, Y., Takagi, M., Aoki, M. & Fujii, N. L. Evidence for acute contraction-induced myokine secretion by C2C12 myotubes. PLoS ONE 13, e206146 (2018).
O. Leary, M. F., Wallace, G. R., Bennett, A. J., Tsintzas, K. & Jones, S. W. IL-15 promotes human myogenesis and mitigates the detrimental effects of TNFα on myotube development. Sci. Rep. 7, 12997 (2017).
Yoshida, S. et al. Interleukin‐15 receptor subunit alpha regulates interleukin‐15 localization and protein expression in skeletal muscle cells. Exp. Physiol. 107, 222–232 (2022).
Wong, W., Crane, E. D., Kuo, Y., Kim, A. & Crane, J. D. The exercise cytokine interleukin-15 rescues slow wound healing in aged mice. J. Biol. Chem. 294, 20024–20038 (2019).
Partridge, L., Deelen, J. & Slagboom, P. E. Facing up to the global challenges of ageing. Nature 561, 45–56 (2018).
Muñoz-Espín, D. & Serrano, M. Cellular senescence: from physiology to pathology. Nat. Rev. Mol. Cell Biol. 15, 482–496 (2014).
Calcinotto, A. et al. Cellular senescence: aging, cancer, and injury. Physiol. Rev. 99, 1047–1078 (2019).
De la Rosa, A. et al. Physical exercise in the prevention and treatment of Alzheimer’s disease. J. Sport Health Sci. 9, 394–404 (2020).
Liang, Y. et al. All roads lead to Rome-a review of the potential mechanisms by which exerkines exhibit neuroprotective effects in Alzheimer’s disease. Neural Regen. Res. 17, 1210–1227 (2022).
Choi, S. H. et al. Combined adult neurogenesis and BDNF mimic exercise effects on cognition in an Alzheimer’s mouse model. Science 361, eaan8821 (2018).
Sujkowski, A., Hong, L., Wessells, R. J. & Todi, S. V. The protective role of exercise against age-related neurodegeneration. Ageing Res. Rev. 74, 101543 (2022).
Horowitz, A. M. et al. Blood factors transfer beneficial effects of exercise on neurogenesis and cognition to the aged brain. Science 369, 167–173 (2020).
Watson, S. L. et al. High-intensity resistance and impact training improves bone mineral density and physical function in postmenopausal women with osteopenia and osteoporosis: the LIFTMOR randomized controlled trial. J. Bone Miner. Res. 33, 211–220 (2018).
Anupama, D. S., Norohna, J. A., Acharya, K. K., Ravishankar & George, A. Effect of exercise on bone mineral density and quality of life among postmenopausal women with osteoporosis without fracture: a systematic review. Int. J. Orthop. Trauma Nurs. 39, 100796 (2020).
Martyn-St James, M. & Carroll, S. Meta-analysis of walking for preservation of bone mineral density in postmenopausal women. Bone 43, 521–531 (2008).
Ma, D., Wu, L. & He, Z. Effects of walking on the preservation of bone mineral density in perimenopausal and postmenopausal women: a systematic review and meta-analysis. Menopause 20, 1216–1226 (2013).
Cruz-Jentoft, A. J. et al. Sarcopenia: revised European consensus on definition and diagnosis. Age Ageing 48, 16–31 (2019).
Capelli, C., Rittveger, J., Bruseghini, P., Calabria, E. & Tam, E. Maximal aerobic power and anaerobic capacity in cycling across the age spectrum in male master athletes. Eur. J. Appl. Physiol. 116, 1395–1410 (2016).
Landi, F., Marzetti, E., Martone, A. M., Bernabei, R. & Onder, G. Exercise as a remedy for sarcopenia. Curr. Opin. Clin. Nutr. 17, 25–31 (2013).
Peterson, M. D., Sen, A. & Gordon, P. M. Influence of resistance exercise on lean body mass in aging adults: a meta-analysis. Med. Sci. Sports Exerc. 43, 249–258 (2011).
Giallauria, F., Cittadini, A., Smart, N. A. & Vigorito, C. Resistance training and sarcopenia. Monaldi Arch. Chest Dis. 84, 51–53 (2016).
Papa, E. V., Dong, X. & Hassan, M. Resistance training for activity limitations in older adults with skeletal muscle function deficits: a systematic review. Clin. Interv. Aging 12, 955–961 (2017).
Joanisse, S. et al. Exercise conditioning in old mice improves skeletal muscle regeneration. FASEB J. 30, 3256–3268 (2016).
Leenders, M. et al. Elderly men and women benefit equally from prolonged resistance-type exercise training. J. Gerontol. A Biol. Sci. Med. Sci. 68, 769–779 (2013).
Cisterna, B. et al. Adapted physical exercise enhances activation and differentiation potential of satellite cells in the skeletal muscle of old mice. J. Anat. 228, 771–783 (2016).
Zacharewicz, E. et al. Identification of MicroRNAs linked to regulators of muscle protein synthesis and regeneration in young and old skeletal muscle. PLoS ONE 9, e114009 (2014).
Arnold, M. J. & Moody, A. L. Common running injuries: evaluation and management. Am. Fam. Physician 97, 510–516 (2018).
Fagher, K. & Lexell, J. Sports-related injuries in athletes with disabilities. Scand. J. Med. Sci. Sports 24, e320–e331 (2014).
Murphy, C., O. Connell, J. E., Kearns, G. & Stassen, L. Sports-related maxillofacial injuries. J. Craniofac. Surg. 26, 2120–2123 (2015).
Pierpoint, L. A. & Collins, C. Epidemiology of sport-related concussion. Clin. Sports Med. 40, 1–18 (2021).
Elliott, A. D., Linz, D., Verdicchio, C. V. & Sanders, P. Exercise and atrial fibrillation: prevention or causation? Heart Lung Circ. 27, 1078–1085 (2018).
O’Keefe, E. L., Torres-Acosta, N., O’Keefe, J. H. & Lavie, C. J. Training for longevity: the reverse J-Curve for exercise. Mo. Med. 117, 355–361 (2020).
Dockerill, C., Lapidaire, W., Lewandowski, A. J. & Leeson, P. Cardiac remodelling and exercise: what happens with ultra-endurance exercise? Eur. J. Prev. Cardiol. 27, 1464–1466 (2020).
Geesmann, B., Gibbs, J. C., Mester, J. & Koehler, K. Association between energy balance and metabolic hormone suppression during ultraendurance exercise. Int. J. Sports Physiol. Perform. 12, 984–989 (2017).
Turner, J. E., Bennett, S. J., Bosch, J. A., Griffiths, H. R. & Aldred, S. Ultra-endurance exercise: unanswered questions in redox biology and immunology. Biochem. Soc. Trans. 42, 989–995 (2014).
Seo, M. et al. Effects of 16 weeks of resistance training on muscle quality and muscle growth factors in older adult women with sarcopenia: a randomized controlled trial. Int. J. Environ. Res. Public Health 18, 6762 (2021).
Kemmler, W. et al. Effects of high‐intensity resistance training on osteopenia and sarcopenia parameters in older men with osteosarcopenia—one‐year results of the randomized controlled Franconian Osteopenia and Sarcopenia Trial (FrOST). J. Bone Miner. Res. 35, 1634–1644 (2020).
Aamann, L. et al. Resistance training increases muscle strength and muscle size in patients with liver cirrhosis. Clin. Gastroenterol. Hepatol. 18, 1179–1187 (2020).
Lichtenberg, T., von Stengel, S., Sieber, C. & Kemmler, W. The favorable effects of a high-intensity resistance training on sarcopenia in older community-dwelling men with osteosarcopenia: the randomized controlled FrOST study. Clin. Interv. Aging 14, 2173–2186 (2019).
FilipoviC, T. N. et al. A 12-week exercise program improves functional status in postmenopausal osteoporotic women: randomized controlled study. Eur. J. Phys. Rehabil. Med. 57, 120–130 (2021).
Harding, A. T. et al. Exploring thoracic kyphosis and incident fracture from vertebral morphology with high-intensity exercise in middle-aged and older men with osteopenia and osteoporosis: a secondary analysis of the LIFTMOR-M trial. Osteoporos. Int. 32, 451–465 (2021).
Harding, A. T. et al. Effects of supervised high-intensity resistance and impact training or machine-based isometric training on regional bone geometry and strength in middle-aged and older men with low bone mass: the LIFTMOR-M semi-randomised controlled trial. Bone 136, 115362 (2020).
Otero, M., Esain, I., Gonzalez-Suarez, A. M. & Gil, S. M. The effectiveness of a basic exercise intervention to improve strength and balance in women with osteoporosis. Clin. Interv. Aging 12, 505–513 (2017).
Pandey, A. et al. Frailty status modifies the efficacy of exercise training among patients with chronic heart failure and reduced ejection fraction: an analysis from the HF-ACTION trial. Circulation 146, 80–90 (2022).
Hieda, M. et al. One-year committed exercise training reverses abnormal left ventricular myocardial stiffness in patients with stage B heart failure with preserved ejection fraction. Circulation 144, 934–946 (2021).
Liu-Ambrose, T. et al. Aerobic exercise and vascular cognitive impairment. Neurology 87, 2082–2090 (2016).
Bo, W. et al. Effects of combined intervention of physical exercise and cognitive training on cognitive function in stroke survivors with vascular cognitive impairment: a randomized controlled trial. Clin. Rehabil. 33, 54–63 (2019).
Nave, A. H. et al. Physical Fitness Training in Patients with Subacute Stroke (PHYS-STROKE): multicentre, randomised controlled, endpoint blinded trial. BMJ 366, l5101 (2019).
Sobol, N. A. et al. Effect of aerobic exercise on physical performance in patients with Alzheimer’s disease. Alzheimers Dement. 12, 1207–1215 (2016).
Lautenschlager, N. T. et al. Effect of physical activity on cognitive function in older adults at risk for Alzheimer disease. JAMA 300, 1027–1037 (2008).
Lamb, S. E. et al. Dementia And Physical Activity (DAPA) trial of moderate to high intensity exercise training for people with dementia: randomised controlled trial. BMJ 361, k1675 (2018).
Acknowledgements
This work is supported by National Natural Science Foundation of China (92068101, 31871498), Project from Shanghai Municipal Health Commission (2022XD050), Shanghai Municipal Education Commission-Gaofeng Clinical Medicine Grant Support (828313), Project from National Research Center for Translational Medicine at Shanghai (TMSK-2021–106), Shanghai Collaborative Innovation Program on Regenerative Medicine and Stem Cell Research (2019CXJQ01), and Innovative Research Team of High-level Local Universities in Shanghai.
Author information
Authors and Affiliations
Contributions
L.C. and Y.F. conceived and revised the paper. J.C. and R.Z. wrote the paper and organized the figures. All authors have read and approved the article.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Chen, J., Zhou, R., Feng, Y. et al. Molecular mechanisms of exercise contributing to tissue regeneration. Sig Transduct Target Ther 7, 383 (2022). https://doi.org/10.1038/s41392-022-01233-2
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41392-022-01233-2
This article is cited by
-
Mechanosensitive channel of large conductance enhances the mechanical stretching-induced upregulation of glycolysis and oxidative metabolism in Schwann cells
Cell Communication and Signaling (2024)
-
Non invasive techniques for direct muscle quality assessment after exercise intervention in older adults: a systematic review
BMC Geriatrics (2024)
-
The Effect of Exercise on Mesenchymal Stem Cells and their Application in Obesity Treatment
Stem Cell Reviews and Reports (2024)
-
Spatiotemporal multi-omics: exploring molecular landscapes in aging and regenerative medicine
Military Medical Research (2024)
-
Short term effects of a novel combined approach compared with physical therapy alone among older patients with temporomandibular degenerative joint disease: a prospective cohort study
BMC Oral Health (2023)