Abstract
Background
To develop a simple scoring system to predict either any or severe IVH in VLBW infants.
Methods
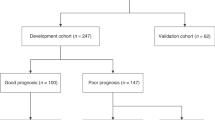
In this retrospective cohort study, 923 VLBW infants were randomly divided into derivation (n = 431) and validation (n = 492) cohorts. After stepwise multivariable logistic regression analyses, a risk score was assigned to independent predictors.
Results
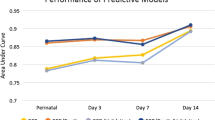
The overall rates of any and severe IVH were 22.9% and 9.9%. Gestational age, maternal race, location of birth and sex were independent predictors of any IVH (AUC 0.75 in derivation cohort and 0.69 for validation cohort). Birth weight, Apgar score at 1 minute, location of birth and sex were independent predictors of severe IVH (AUC 0.84 in derivation cohort and 0.77 for validation cohort). For any IVH, infants in the high-risk category (total score 4 or 5) had > 50% likelihood of any IVH with a negative predictive value of 82.6%. For severe IVH, the total risk score ranged from 0–8, and infants in high-risk category (total score 6–8) had 30% likelihood of severe IVH with a negative predictive value of 94.9%.
Conclusion
We report an easy to calculate, validated scoring system with a high NPV to identify VLBW infants at highest risk of IVH.
Impact
-
We report a simple validated scoring system with a high NPV for prediction of IVH in VLBW infants.
-
The variables in the proposed model are available at birth and unlikely to be influenced by provider bias.
-
This scoring system can identify infants at risk of any and severe IVH, while most previous models predict only severe IVH.
-
This scoring system does not require access to web-based resources.
-
This scoring system can help in employing prevention strategies only for infants at highest risk of IVH and thus eliminate the risks of interventions in a large majority of VLBW infants.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 14 print issues and online access
$259.00 per year
only $18.50 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Stoll, B. J. et al. Eunice Kennedy Shriver National Institute of Child Health and Human Development Neonatal Research Network. Neonatal outcomes of extremely preterm infants from the NICHD Neonatal Research Network. Pediatrics 126, 443–456 (2010).
Patra, K., Wilson-Costello, D., Taylor, H. G., Mercuri-Minich, N. & Hack, M. Grades I–II intraventricular hemorrhage in extremely low birth weight infants: effects on neurodevelopment. J. Pediatr. 149, 169–173 (2006).
Bolisetty, S. et al. Intraventricular hemorrhage and neurodevelopmental outcomes in extreme preterm infants. Pediatrics 133, 55–62 (2014).
Mukerji, A., Shah, V. & Shah, P. S. Periventricular/Intraventricular Hemorrhage and Neurodevelopmental Outcomes: A Meta-analysis. Pediatrics 136, 1132–1143 (2015).
Ballabh, P. Pathogenesis and Prevention of Intraventricular hemorrhage. Clin. Perinatol. 41, 47–67 (2014).
Shankaran, S. et al. Maternal race, demography, and health care disparities impact risk for intraventricular hemorrhage in preterm neonates. J. Pediatr. 164, 1005–1011 (2014).
McGoldrick, E., Stewart, F., Parker, R. & Dalziel, S. R. Antenatal corticosteroids for accelerating fetal lung maturation for women at risk of preterm birth. Cochrane Database Syst. Rev. 12, CD004454 (2020).
Smit, E., Odd, D. & Whitelaw, A. Postnatal phenobarbital for the prevention of intraventricular haemorrhage in preterm infants. Cochrane Database Syst. Rev. 8, CD001691 (2013).
Fowlie, P. W., Davis, P. G. & McGuire, W. Prophylactic intravenous indomethacin for preventing mortality and morbidity in preterm infants. Cochrane Database Syst. Rev. 7, CD000174 (2010).
Carteaux, P. et al. Evaluation and development of potentially better practices for the prevention of brain hemorrhage and ischemic brain injury in very low birth weight infants. Pediatrics 111, e489–e496 (2003).
Jasani, B., Torgalkar, R., Ye, X. Y., Syed, S. & Shah, P. S. Association of umbilical cord management strategies with outcomes of preterm infants: A systematic review and network meta-analysis. JAMA Pediatr. 175, e210102 (2021).
Tarnow-Mordi, W. et al. Delayed versus immediate cord clamping in preterm infants. N. Engl. J. Med. 377, 2445–2455 (2017).
Fogarty, M. et al. Delayed vs early umbilical cord clamping for preterm infants: a systematic review and meta-analysis. Am. J. Obstet. Gynecol. 218, 1–18 (2018).
Yao, S. L., Smit, E. & Odd, D. The effectiveness of interventions to prevent intraventricular haemorrhage in premature infants: A systematic review and network meta-analysis. J. Neonatal Perinat. Med. 16, 5–20 (2023).
Romantsik, O., Calevo, M. G. & Bruschettini, M. Head midline position for preventing the occurrence or extension of germinal matrix-intraventricular haemorrhage in preterm infants. Cochrane Database Syst. Rev. 7, CD012362 (2020).
Kumar, P. et al. Elevated supine midline head position for prevention of intraventricular hemorrhage in VLBW and ELBW infants: a retrospective multicenter study. J. Perinatol. 41, 278–285 (2021).
Papile, L. A., Burstein, J., Burstein, R. & Koffler, H. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J. Pediatr. 92, 529–534 (1978).
Gursoy, T., Hayran, M., Derin, H. & Ovali, F. A clinical scoring system to predict the development of bronchopulmonary dysplasia. Am. J. Perinatol. 32, 659–666 (2015).
Heuchan, A. M., Evans, N., Henderson, D. J. & Simpson, J. M. Perinatal risk factors for major intraventricular haemorrhage in the Australian and New Zealand Neonatal. Netw., 1995-97. Arch. Dis. Child. Fetal Neonatal Ed. 86, F86–F90 (2002).
Singh, R. et al. A predictive model for SIVH risk in preterm infants and targeted indomethacin therapy for prevention. Sci. Rep. 3, 2539 (2013).
Luque, M. J. et al. A risk prediction model for severe intraventricular hemorrhage in very low birth weight infants and the effect of prophylactic indomethacin. J. Perinatol. 34, 43–48 (2014).
Coskun, Y. et al. A clinical scoring system to predict the development of intraventricular hemorrhage (IVH) in premature infants. Childs Nerv. Syst. 34, 129–136 (2018).
Lee, J., Hong, M., Yum, S. K. & Lee, J. H. Perinatal prediction model for severe intraventricular hemorrhage and the effect of early postnatal acidosis. Childs Nerv. Syst. 34, 2215–2222 (2018).
Chawla, S. et al. Model for severe intracranial hemorrhage and role of early indomethacin in extreme preterm infants. Pediatr. Res. 92, 1648–1656 (2022).
Poryo, M. et al. Ante-, peri- and postnatal factors associated with intraventricular hemorrhage in very premature infants. Early Hum. Dev. 116, 1–8 (2018).
Ancel, P. Y. et al. Are maternal hypertension and small-for-gestational age risk factors for severe intraventricular hemorrhage and cystic periventricular leukomalacia? Results of the EPIPAGE cohort study. Am. J. Obstet. Gynecol. 193, 178–184 (2005).
Bossung, V. et al. Neonatal Outcome after Preeclampsia and HELLP Syndrome: A Population-Based Cohort Study in Germany. Front Pediatr. 12, 579293 (2020).
Sloane, A. J. et al. Hypertensive disorders during pregnancy are associated with reduced severe intraventricular hemorrhage in very-low-birth-weight infants. J. Perinatol. 39, 1125–1130 (2019).
Acknowledgements
Authors thank Dr Preetha Prasad for sharing data from patients in her institution for this study.
Author information
Authors and Affiliations
Contributions
P.K. conceptualized and designed the study, drafted the initial manuscript, and critically reviewed and revised the manuscript. M.P. carried out the initial analyses, and critically reviewed and revised the manuscript. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kumar, P., Polavarapu, M. A simple scoring system for prediction of IVH in very-low-birth-weight infants. Pediatr Res 94, 2033–2039 (2023). https://doi.org/10.1038/s41390-023-02744-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-023-02744-6