Abstract
Background
Pulmonary hypertension (PH) in patients with bronchopulmonary dysplasia (BPD) results from vasoconstriction and/or vascular remodeling, which can be regulated by mitogen-activated protein kinases (MAPKs). MAPKs are deactivated by dual-specificity phosphatases (DUSPs). We hypothesized that single-nucleotide polymorphisms (SNPs) in DUSP genes could be used to predict PH in BPD.
Methods
Preterm infants diagnosed with BPD (n = 188) were studied. PH was defined by echocardiographic criteria. Genomic DNA isolated from patient blood samples was analyzed for 31 SNPs in DUSP genes. Clinical characteristics and minor allele frequencies were compared between BPD-PH (cases) and BPD-without PH (control) groups. Biomarker models to predict PH in BPD using clinical and SNP data were tested by calculations of area under the ROC curve.
Results
In our BPD cohort, 32% (n = 61) had PH. Of the DUSP SNPs evaluated, DUSP1 SNP rs322351 was less common, and DUSP5 SNPs rs1042606 and rs3793892 were more common in cases than in controls. The best fit biomarker model combines clinical and DUSP genetic data with an area under the ROC curve of 0.76.
Conclusion
We identified three DUSP SNPs as potential BPD-PH biomarkers. Combining clinical and DUSP genetic data yields the most robust predictor for PH in BPD.
Similar content being viewed by others
Introduction
Bronchopulmonary dysplasia (BPD is a chronic lung disease most commonly seen in preterm infants who require prolonged, positive pressure ventilation and supplemental oxygen. Recent studies have shown that preterm infants who go on to develop BPD have disrupted alveolar and vascular growth, as demonstrated by persistent hypoplasia of lung microvasculature and alveolar simplification.1,2 The resultant decrease in vascular surface area reduces the lung’s capacity for gas exchange and affects perfusion throughout the pulmonary vascular network. Subsequent hypoxia-induced vasoconstriction, elevated pulmonary vascular resistance, and remodeling with intimal hyperplasia of small pulmonary arteries have been implicated in the pathogenesis of BPD-associated pulmonary hypertension (PH).1 Approximately 25–40% of preterm infants with BPD will develop PH and there is an increased risk of mortality with the diagnosis of PH in BPD patients.3 Previously identified clinical risk factors for PH in BPD include low birth weight, necrotizing enterocolitis, retinopathy of prematurity, and patent ductus arteriosus.3,4
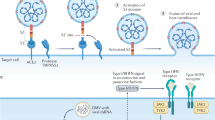
Mitogen-activated protein kinases (MAPKs) play an important role in regulating gene expression, cell proliferation and differentiation, apoptosis, and the synthesis of pro-inflammatory cytokines in response to extracellular stimulation.5,6 MAPKs are activated by phosphorylation of the threonine and tyrosine residues in the Thr-Xaa-Tyr motif in the activation loop domain and inactivated by dephosphorylation catalyzed by dual-specificity phosphatases (DUSPs). Members of the typical DUSP subfamily contain an N-terminal MAPK-binding motif and are critical for the termination of the MAPK cascades.7 Thus they are also referred to as MAP kinase phosphatases (MKPs). These typical DUSPs exhibit differences in expression patterns, subcellular localization, and substrate preferences.
Studies from patients with pulmonary arterial hypertension have observed dysregulated pulmonary artery smooth muscle cell growth that is dependent on both p38 MAPK and c-Jun N-terminal kinase (JNK).8 Inhibiting p38 MAPK in mice with right ventricular (RV) failure resulted in improved RV function and inhibition of RV fibrosis.9 We have previously shown that DUSP1 (MKP-1) knockout mice exposed to chronic hypoxia had greater thickening of their pulmonary arteries as well as evidence of RV hypertrophy compared to wild-type (WT) mice.10 Similarly, DUSP (MKP-1) was found to inhibit hypoxic proliferation of human pulmonary arterial smooth muscle cells.11 The role of the DUSP family in BPD-PH, however, remains unknown. Therefore, we postulate that the development of PH in BPD may be influenced by the regulatory actions of the DUSP family of genes. In the present study, we hypothesized that mutations in the DUSP gene family are involved in the pathogenesis of BPD-PH and therefore that single-nucleotide polymorphisms (SNPs) within the DUSP gene family will be differentially distributed in cohorts of BPD patients with and without PH. We also sought to determine whether SNPs in the DUSP family of genes could be combined with clinical data to serve as a useful biomarker to predict which BPD patients will develop PH.
Methods
The Institutional Review Board at Nationwide Children’s Hospital approved this study. Preterm infants diagnosed with BPD were enrolled from the neonatal intensive care unit at Nationwide Children’s Hospital (level 4, all referral) after September 1, 2009. Diagnostic criteria for BPD were determined according to the NICHD consensus statement as a supplemental oxygen requirement at 28 days of life.12 Consistent with the physiologic definition of BPD established by Walsh et al. in 2003,13 in order to standardize and reduce the variation in observed rates of BPD, Nationwide Children’s Hospital NICU maintains oxygen saturation goals of 90–95% for patients <36 weeks postmenstrual age (PMA) and >94% for patients >36 weeks PMA. Enrollment, clinical data abstraction, and specimen collection were completed through the Ohio Perinatal Research Network and Perinatal Research Repository at The Research Institute at Nationwide Children’s Hospital, Columbus, OH. BPD patients with congenital heart disease, congenital diaphragmatic hernia, and lung hypoplasia were excluded from this study. We did not exclude BPD patients with isolated atrial septal defect, ventricular septal defect, or patent ductus arteriosus. Clinical characteristics were obtained from systematic medical chart review. Both postnatal steroids prior to admission and steroids during admission, as well as caffeine, were all given systemically.
Pulmonary hypertension
PH was diagnosed after 28 days of life by echocardiogram. Evidence of elevated pulmonary arterial pressure on echocardiogram included intraventricular septal flattening, right ventricular hypertrophy and/or dilation, tricuspid regurgitant jet velocity >3 m/s, and/or pulmonary regurgitation.3,14,15,16,17 From a BPD study cohort of 188 preterm infants with BPD, 61 (32%) of these patients were diagnosed with PH based on these echocardiographic parameters and were therefore considered cases. Controls were defined as patients with BPD who did not have PH by these echocardiographic criteria. Some patients in this study have been enrolled previously in research studies.14,17,18,19
Single-nucleotide polymorphisms
As described in previous studies,17,18 patient blood samples were collected after parent consent and study enrollment. Blood samples were collected and stored by the Perinatal Research Repository at the Abigail Wexner Research Institute at Nationwide Children’s Hospital. DNA was isolated from blood leucocytes and SNPs were genotyped by Agena MassArray (Agena, San Diego, CA). For each loci, the SNP (minor allele) was defined as the allele with a minor allele frequency (MAF) <0.5. SNPs were selected for their putative functionality, which was determined by SNP location within the gene loci and potential for altering protein structure and expression as determined from the NCBI/SNP database. PubMed literature searches were conducted to focus on DUSP genes that had known associations with cardiopulmonary disease. This selection process yielded a total of 31 SNPs on 9 out of the 12 DUSP family of genes, which included typical DUSP family members: DUSP1, DUSP2, DUSP4, DUSP5, DUSP6, DUSP7, DUSP9, DUSP10, and DUSP16. Each of these nine typical DUSP family members have a MAPK-binding motif that interacts with the common domain of MAPKs.7
Statistics
This was a case–control study. Clinical characteristics were compared using chi-squared tests for categorical variables and Student’s t test for continuous variables. Statistical significance was considered at p < 0.05. This study was designed to test a specific hypothesis and only candidate DUSP family genes were included in the study. Given the limitation of study sample size, less conservative values are also of interest and may be hypothesis generating. Therefore, no correction was made for multiple testing. Calculated MAF for cases and controls were compared using chi-squared test with one degree of freedom, similar to previous studies.17,18,20 Univariate and multivariate logistic regression was employed to assess clinical and genetic predictors of PH in BPD. Chi-square, t test, and logistic regression analyses were completed with STATA/IC 12.0 (STATA Corp., College Station, TX, USA). Biomarker analyses utilizing the area under the curve (AUC) of receiver operating characteristic (ROC) curves were completed using the GraphPad Prism 7 Software (La Jolla, CA). Clinical and SNP AUC models were constructed after analysis by t test revealed six possible early clinical predictors of PH in BPD (birth weight, gestational age, small for gestational age (SGA), surfactant, postnatal steroids prior to admission, and mechanical ventilation). However, since birth weight, gestational age, and SGA are interdependent variables, we chose to exclude gestational age and SGA and include only four possible early clinical predictors. Similarly, analysis by t test revealed three possible genetic predictors (rs322351, rs1042606, rs3793892). These AUC models were based on data resubstitution method, which uses the same data to construct and evaluate the model. Although data resubstitution can underestimate the classifier error, it has less variability than other methods, such as cross-validation, especially for small sample sizes.21
In order to better evaluate the data in the absence of an external validation cohort, we also completed the cross-validation analysis. Cross-validation has the advantage of producing a less biased result; however, for small sample sizes such as the present study, cross-validation has greater variability than resubstitution. Both methods of prediction have been shown to be comparable in terms of ranking accuracy.21 Cross-validation was achieved by 100 splits of all clinical and SNP data into 2/3 training and 1/3 test sets. Each iteration of training/test set split divided the data into a different 2/3 training and 1/3 test set. For each split, the training data were used to identify the top three DUSP SNPs and the top four clinical covariates based on statistical significance from univariable associations. Logistic regression models were built using the top three SNPs, the top four clinical variables, and the top three SNPs and top four clinical variables combined. The AUC was evaluated on test data, averaged across test data sets, and presented as median and interquartile range (IQR).22,23
Results
Clinical characteristics for the entire cohort, BPD-PH patients (cases), and BPD without PH patients (controls) are shown in Table 1. We found that birth weight and gestational age were lower in cases than in controls (Table 1). There was also a greater rate of SGA in cases than in the controls (Table 1). We did not find any sex or race differences. There was a trend toward a greater rate of African Americans with BPD-PH compared to BPD-without PH. To further explore this, a chi-squared analysis comparing African American and Caucasian groups was conducted and found no significant difference (p = 0.34) between cases and controls. APGARs were similar between the two groups. Although rates of respiratory distress syndrome were similar among cases and controls, we found that surfactant was given less frequently in cases than in controls (Table 1). Postnatal steroids prior to admission were more common in cases than in controls. More cases were treated with mechanical ventilation than were controls. We found no differences in the use of nasal continuous positive airway pressure (nCPAP), >30% oxygen at 36 weeks PMA, or in the common co-morbidities of prematurity between cases and controls. For hospital medications, we found that steroid treatment given during hospital admission occurred more frequently in cases than in controls. As expected, cases of BPD-PH received more inhaled nitric oxide (iNO) treatment than BPD-without PH controls. We found no differences in rates of infection or use of a central line between cases and controls.
We evaluated 31 SNPs in 9 out of the 12 typical DUSP genes that are known to interact with MAPKs7 and found that SNPs in DUSP1 and DUSP5 were significantly different between cases and controls (Table 2). These SNPs remained significantly different even after exclusion of BPD patients requiring <30% oxygen at 36 weeks PMA. DUSP1 SNP rs322351 had MAF that was lower in cases than in controls. Conversely, two SNPs in DUSP5, rs1042606 and rs3793892, had MAF that were greater in cases than in controls.
We next used logistic regression analysis to examine various dependent variables in the probability of developing PH in BPD (Table 3). For the clinical variables, we found that birth weight <700 g, postnatal steroids prior to admission, steroids during admission, total endotracheal tube ventilation >70 days, mechanical ventilation, iNO therapy, and no surfactant, all increased probability of developing PH. After adjusting for all other clinical variables in the table, only postnatal steroids prior to admission increased probability of developing PH (odds ratio 4.7 [1.76, 12.59], p = 0.002). Therefore, if a BPD patient was exposed to postnatal steroids prior to admission, the odds of PH in BPD were 4.7 times greater than if the BPD patient had not been exposed to treatment. When examining the three DUSP SNPs that were significantly different between groups, independent logistic regression of each DUSP SNP resulted in significant predictive modeling of PH in BPD. DUSP1 SNP rs322351 was associated with a 41% decrease in the odds of developing PH in BPD (p = 0.020), and this finding persisted even after adjustment for the other two DUSP5 SNPs (p = 0.023) (Table 3). Both DUSP5 SNPs rs1042606 and rs3793892 were associated with an approximately 1.6 times greater risk of developing PH in BPD (p = 0.036 and p = 0.042, respectively); however, this finding did not persist after adjustment for the other two DUSP SNPs (Table 3).
We next calculated AUC of the ROC curve for several clinical and SNP models, keeping in mind that a perfect biomarker is 100% sensitive and 100% specific, resulting in an AUC of 1. For the clinical models (Table 4), we included early significant clinical predictors as identified by Tables 1 and 3: birth weight <700 g, postnatal preadmission steroids, mechanical ventilation, and no surfactant. When these clinical predictors were analyzed separately, birth weight <700 g had the largest AUC for the ROC curve, although it was only 0.612 (Table 4). We next examined various combinations of these clinical factors using ROC curves, and the largest AUC for PH in BPD was 0.729 when birth weight <700 g+postnatal preadmission steroids+mechanical ventilation+no surfactant were analyzed together. For the genetic data, the ROC curve with the largest AUC was for the DUSP1 WT rs322351, which was modeled as a 0–2 variable dependent on the number of WT alleles present at the rs322351 locus (Table 3). We found that combining the SNPs improved the AUC of the ROC curve slightly, and there was little difference in the AUC of the ROC curve when combining all three SNPs or two of the three SNPs. The best AUC of the ROC curve for genetic data (DUSP1 SNP rs322351+DUSP5 SNP rs1042606) was only 0.632.
We were interested to know whether we could improve the AUC of the ROC curve by including both clinical and SNP data. Figure 1 shows the ROC curves of the best AUC (0.729) from the combined clinical data (from Table 4) and the best AUC (0.632) from the combined SNP data (from Table 4). When we combined these clinical and SNP data together, we found a small increase in the AUC of the ROC curve to 0.755 (Fig. 1). We compared each of the AUCs generated in Fig. 1 and found that the clinical+SNP AUC of 0.755 was significantly greater than the SNP AUC of 0.632 (p = 0.035). Cross-validation analysis found a lower median AUC for all groups (clinical median AUC 0.657 [IQR 0.603–0.704], SNP median AUC 0.543 [IQR 0.512–0.584], clinical+SNP median AUC 0.642 [IQR 0.589–0.701]), the clinical median AUC was slightly greater than the clinical+SNP median AUC, and there continued to be a difference between SNP and clinical+SNP median AUC.
The best fit biomarker model to predict pulmonary hypertension (PH) in bronchopulmonary dysplasia (BPD) combines clinical and single-nucleotide polymorphism (SNP) data. Area under the curve (AUC) calculated for BPD cohort (BPD alone, n = 127 and BPD-PH, n = 61). Combining the best fit independent clinical biomarker model (birth weight <700 g+postnatal, pre-admission steroids+mechanical ventilation+no surfactant) with the best fit independent SNP biomarker model (DUSP1 WT rs322351+DUSP5 SNP rs1042606) yields a 0–8 variable with an AUC 0.755. *AUC Clinical+SNP data different from AUC SNP data (p = 0.035)
Discussion
In this biomarker study of clinical factors and DUSP loci for the prediction of PH in BPD, we have several novel findings: (1) BPD-PH patients had a lower birth weight and gestational age and a greater percentage of SGA than in BPD-without PH controls, (2) BPD-PH patients received less surfactant, more postnatal pre-admission steroids, and more mechanical ventilation than did BPD-without PH controls, (3) BPD-PH patients received more steroids during admission and iNO treatment than did BPD-without PH controls, (4) DUSP1 SNP rs322351 was less common, and DUSP5 SNPs rs1042606 and rs3793892 were more common in cases than in controls, (5) the overall best fit biomarker combines clinical and DUSP genetic data with an area under the ROC curve of 0.76, which is significantly greater than DUSP genetic data alone area under the ROC curve of 0.63.
Previous clinical studies by our group did not detect a difference in SGA between BPD-PH and BPD-without PH controls,14,17,18 while in the present study we recruited our largest BPD cohort to date of 188 patients, thus improving power, and were able detect a greater percentage of SGA in cases than in controls. SGA is indicative of an early and poorly developed vascular network in these premature neonates, thus contributing to both their lung disease (BPD) and PH. Consistent with previous clinical studies, we observed lower birth weight and gestational age.14 Similar distribution of sex and race were observed. The largest minority group in our cohort, African American, had a trend toward greater rates of BPD-PH compared to BPD-without PH. Since SNP distribution can be dependent on racial background, the observation that the African American group trended toward more severe disease (BPD-PH) warrants future study. In our cohort, BPD-PH patients received less surfactant, a novel finding, indicating that in the premature neonate, early surfactant administration prior to nCPAP may be an important preventative strategy against PH in BPD. We also found greater steroid treatment in BPD-PH patients than in BPD-without PH patients, with similar distribution of BPD severity among groups. This is consistent with our study in 2014, where we found a trend toward greater postnatal steroid use in BPD-PH compared to BPD-without patients.18 The time course of steroid treatment and diagnosis of BPD and/or PH requires further study, since 75% of BPD-PH patients received steroids during admission and this could in part explain why severe BPD (>30% oxygen at 36 weeks PMA) was not statistically greater in BPD-PH compared to that in BPD-without PH patients. Inflammatory processes are downregulated by steroids by way of DUSP1 (MKP-1).24 Therefore, treatment with steroids, or perhaps more specifically targeting overexpression of DUSP1 could potentially ameliorate PH in BPD, however, this has yet to be studied. Mechanical ventilation use was greater in BPD-PH patients than BPD-without PH patients, consistent with previous studies.14,17,25 As expected, iNO treatment was greater in BPD-PH patients, and its role as a potent vasodilator26,27 likely improved PH but did not prevent PH in BPD.
We found that DUSP1 SNP rs322351 was less common, and DUSP5 SNPs rs1042606 and rs3793892 were more common, in cases than in controls. Both DUSP1 (MKP-1) and DUSP5 are typical DUSPs with a MAPK-binding motif7 and are also a part of a subset group of DUSPs that are inducible nuclear phosphatases.28 A difference between DUSP1 (MKP-1) and DUSP5 is that DUSP5 is MAPK extracellular signal-regulated kinases 1/2 (ERK1/2) specific, whereas DUSP1 (MKP-1) has phosphatase activity toward both ERK1/2 and the stress-activated kinases p38 and JNK.28,29,30,31,32 However, only DUSP1 (MKP-1) can act as both a phosphatase of MAPK and a MAPK substrate. MAPK ERK-mediated phosphorylation of DUSP1 (MKP-1) can lead to ubiquitination/protein degradation or increased protein stability, depending on the DUSP1 (MKP-1) phosphorylation site.28,33,34 Similar to DUSP1 (MKP-1), DUSP5 protein can be stabilized by MAPK ERK, thus reinforcing respective phosphatase activities in a positive feedback loop.28 Future studies could determine whether DUSP1 SNP rs322351, DUSP5 SNP rs1042606, and/or DUSP5 SNP rs3793892 modify DUSP protein function to contribute to the pathophysiology of PH in BPD. MAPKs phosphorylate and activate numerous downstream targets, including transcription factors and protein kinases that play a key role in fundamental cellular processes that are influenced by inflammation, including cellular survival, proliferation, and apoptosis.35 We speculate that the effect of MAPK is to promote cellular proliferation of the pulmonary vascular wall, contributing to PH, while DUSP1/5, by negatively regulating MAPKs, would prevent PH.
Human studies of DUSP1 (MKP-1) have shown that the antiproliferative effect of sildenafil on pulmonary artery smooth muscle cells is mediated by the upregulation of DUSP1 (MKP-1).36 These findings suggest that DUSP1 (MKP-1) may be protective against hallmark features in the progression of PH in patients with BPD. MAPK ERK1/2-mediated cell proliferation has been specifically implicated in the pathophysiology of PH,37,38 and thus DUSP5, with its characteristic MAPK ERK1/2 specificity, is a promising therapeutic target for MAPK ERK1/2-mediated PH. Future clinical studies evaluating MAPK ERK1/2, JNK, and p38 profile in our BPD cohort with and without PH could determine whether a MAPK ERK1/2-specific inhibitor, such as DUSP5, might serve as a targeted and effective therapy for BPD-PH patients.
This study was limited by small cohort size. BPD is considered a rare disease by NIH, and we have expanded our single-center cohort to include as many BPD patients as possible. However, the relatively small sample size limited the power of this study to detect potentially important differences. We have immediate plans to replicate this study in a larger and independent BPD cohort. Another major limitation has been the difficulty of diagnosing PH in neonates and infants; however, bedside echocardiography is now the standard of care and serves as a useful and less-invasive tool to reliably diagnose neonatal PH.39
Taken together, these clinical and DUSP SNP data produce the best area under the ROC curve to date for BPD-PH (0.76). The most predictive clinical biomarkers, birth weight <700 g, postnatal preadmission steroids, mechanical ventilation, and no surfactant, also contribute to the pathophysiology of PH. We found that DUSP1 and DUSP5 SNPs are predictive of PH in BPD. Future studies are needed to combine and add biomarkers to further improve the AUC in order to create a clinically applicable biomarker panel for BPD-PH.
References
Baker, C. D., Abman, S. H. & Mourani, P. M. Pulmonary hypertension in preterm infants with bronchopulmonary dysplasia. Pediatr. Allergy Immunol. Pulmonol. 27, 8–16 (2014).
Kalikkot Thekkeveedu, R., Guaman, M. C. & Shivanna, B. Bronchopulmonary dysplasia: a review of pathogenesis and pathophysiology. Respir. Med. 132, 170–177 (2017).
Berkelhamer, S. K., Mestan, K. K. & Steinhorn, R. H. Pulmonary hypertension in bronchopulmonary dysplasia. Semin. Perinatol. 37, 124–131 (2013).
Arjaans, S. et al. Identification of gaps in the current knowledge on pulmonary hypertension in extremely preterm infants: a systematic review and meta-analysis. Paediatr. Perinat. Epidemiol. 32, 258–267 (2018).
Li, L., Chen, S. F. & Liu, Y. MAP kinase phosphatase-1, a critical negative regulator of the innate immune response. Int. J. Clin. Exp. Med. 2, 48–67 (2009).
Dickinson, R. J. & Keyse, S. M. Diverse physiological functions for dual-specificity MAP kinase phosphatases. J. Cell Sci. 119, 4607–4615 (2006).
Huang, C. Y. & Tan, T. H. DUSPs, to MAP kinases and beyond. Cell Biosci. 2, 1–10 (2012).
Wilson, J. L., Yu, J., Taylor, L. & Polgar, P. Hyperplastic growth of pulmonary artery smooth muscle cells from subjects with pulmonary arterial hypertension is activated through JNK and p38 MAPK. PLoS ONE 10, e0123662 (2015).
Kojonazarov, B. et al. p38 MAPK inhibition improves heart function in pressure-loaded right ventricular hypertrophy. Am. J. Respir. Cell Mol. Biol. 57, 603–614 (2017).
Jin, Y. et al. Mice deficient in Mkp-1 develop more severe pulmonary hypertension and greater lung protein levels of arginase in response to chronic hypoxia. Am. J. Physiol. Heart Circ. Physiol. 298, H1518–H1528 (2010).
Jin, Y. et al. MKP-1 is a target of miR-210 and mediate the negative regulation of miR-210 inhibitor on hypoxic hPASMC proliferation. Cell Biol. Int. 39, 113–120 (2015).
Jobe, A. H. & Bancalari, E. Bronchopulmonary dysplasia. Am. J. Respir. Crit. Care Med. 163, 1723–1729 (2001).
Walsh, M. C., Wilson-Costello, D., Zadell, A., Newman, N. & Fanaroff, A. Safety, reliability, and validity of a physiologic definition of bronchopulmonary dysplasia. J. Perinatol. 23, 451–456 (2003).
Trittmann, J. K. et al. Using clinical and genetic data to predict pulmonary hypertension in bronchopulmonary dysplasia. Acta Paediatr. 107, 2158–2164 (2018).
Bui, C. B. et al. Pulmonary hypertension associated with bronchopulmonary dysplasia in preterm infants. J. Reprod. Immunol. 124, 21–29 (2017).
Slaughter, J. L., Pakrashi, T., Jones, D. E., South, A. P. & Shah, T. A. Echocardiographic detection of pulmonary hypertension in extremely low birth weight infants with bronchopulmonary dysplasia requiring prolonged positive pressure ventilation. J. Perinatol. 31, 635–640 (2011).
Trittmann, J. K. et al. A single nucleotide polymorphism in the dimethylarginine dimethylaminohydrolase gene is associated with lower risk of pulmonary hypertension in bronchopulmonary dysplasia. Acta Paediatr. 105, e170–e175 (2016).
Trittmann, J. K. et al. Arginase I gene single-nucleotide polymorphism is associated with decreased risk of pulmonary hypertension in bronchopulmonary dysplasia. Acta Paediatr. 103, e439–e443 (2014).
Trittmann, J. K. et al. Plasma asymmetric dimethylarginine levels are increased in neonates with bronchopulmonary dysplasia-associated pulmonary hypertension. J. Pediatr. 166, 230–233 (2015).
Pearson, D. L. et al. Neonatal pulmonary hypertension-urea-cycle intermediates, nitric oxide production, and carbamoyl-phosphate synthetase function. N. Engl. J. Med. 344, 1832–1838 (2001).
Braga-Neto, U., Hashimoto, R., Dougherty, E. R., Nguyen, D. V. & Carroll, R. J. Is cross-validation better than resubstitution for ranking genes? Bioinformatics 20, 253–258 (2004).
Andres, S. A., Brock, G. N. & Wittliff, J. L. Interrogating differences in expression of targeted gene sets to predict breast cancer outcome. BMC Cancer 13, 1–18 (2013).
Garbett, N. C. & Brock, G. N. Differential scanning calorimetry as a complementary diagnostic tool for the evaluation of biological samples. Biochim. Biophys. Acta 1860, 981–989 (2016).
Lasa, M., Abraham, S. M., Boucheron, C., Saklatvala, J. & Clark, A. R. Dexamethasone causes sustained expression of mitogen-activated protein kinase (MAPK) phosphatase 1 and phosphatase-mediated inhibition of MAPK p38. Mol. Cell Biol. 22, 7802–7811 (2002).
Trittmann, J. K. et al. An arginase-1 SNP that protects against the development of pulmonary hypertension in bronchopulmonary dysplasia enhances NO-mediated apoptosis in lymphocytes. Physiol. Rep. 4, 1–11 (2016).
Furchgott, R. F. & Zawadzki, J. V. The obligatory role of endothelial cells in the relaxation of arterial smooth muscle by acetylcholine. Nature 288, 373–376 (1980).
Morris, S. M. Jr. & Billiar, T. R. New insights into the regulation of inducible nitric oxide synthesis. Am. J. Physiol. 266, E829–E839 (1994).
Kucharska, A., Rushworth, L. K., Staples, C., Morrice, N. A. & Keyse, S. M. Regulation of the inducible nuclear dual-specificity phosphatase DUSP5 by ERK MAPK. Cell Signal 21, 1794–1805 (2009).
Owens, D. M. & Keyse, S. M. Differential regulation of MAP kinase signalling by dual-specificity protein phosphatases. Oncogene 26, 3203–3213 (2007).
Mandl, M., Slack, D. N. & Keyse, S. M. Specific inactivation and nuclear anchoring of extracellular signal-regulated kinase 2 by the inducible dual-specificity protein phosphatase DUSP5. Mol. Cell Biol. 25, 1830–1845 (2005).
Franklin, C. C. & Kraft, A. S. Constitutively active MAP kinase kinase (MEK1) stimulates SAP kinase and c-Jun transcriptional activity in U937 human leukemic cells. Oncogene 11, 2365–2374 (1995).
Franklin, C. C. & Kraft, A. S. Conditional expression of the mitogen-activated protein kinase (MAPK) phosphatase MKP-1 preferentially inhibits p38 MAPK and stress-activated protein kinase in U937 cells. J. Biol. Chem. 272, 16917–16923 (1997).
Brondello, J. M., Pouyssegur, J. & McKenzie, F. R. Reduced MAP kinase phosphatase-1 degradation after p42/p44MAPK-dependent phosphorylation. Science 286, 2514–2517 (1999).
Lin, Y. W. & Yang, J. L. Cooperation of ERK and SCFSkp2 for MKP-1 destruction provides a positive feedback regulation of proliferating signaling. J. Biol. Chem. 281, 915–926 (2006).
Talavera, M. M. et al. Mitogen-activated protein kinase phosphatase-1 prevents lipopolysaccharide-induced apoptosis in immature rat intestinal epithelial cells. Pediatr. Res. 78, 128–136 (2015).
Li, B., Yang, L., Shen, J., Wang, C. & Jiang, Z. The antiproliferative effect of sildenafil on pulmonary artery smooth muscle cells is mediated via upregulation of mitogen-activated protein kinase phosphatase-1 and degradation of extracellular signal-regulated kinase 1/2 phosphorylation. Anesth. Analg. 105, 1034–1041 (2007).
Kovacs, L. et al. Activation of Calpain-2 by mediators in pulmonary vascular remodeling of pulmonary arterial hypertension. Am. J. Respir. Cell Mol. Biol. 54, 384–393 (2016).
Nelin, L. D. et al. The Src family tyrosine kinases src and yes have differential effects on inflammation-induced apoptosis in human pulmonary microvascular endothelial cells. Am. J. Physiol. Lung Cell Mol. Physiol. 310, L880–L888 (2016).
McCrary, A. W. et al. Agreement of an echocardiogram-based diagnosis of pulmonary hypertension in infants at risk for bronchopulmonary dysplasia among masked reviewers. J. Perinatol. 39, 248–255 (2018).
Acknowledgements
The authors would like to thank the patients and their families for participating in this study and the research staff of the Ohio Perinatal Research Network (OPRN) and the Perinatal Research Respository (PRR). This work was supported in part by The Ohio State University College of Medicine Roessler Medical Student Research Scholarship awarded to L.L.C. This study was funded by an intramural grant from the Center for Clinical and Translational Research at The Research Institute, Nationwide Children’s Hospital (CTSA grant UL1TR001070) and an NIH grant (K08HL129080) from NHLBI.
Author information
Authors and Affiliations
Contributions
Substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data: all authors. Drafting the article or revising it critically for important intellectual content: L.L.C., J.K.T. Final approval of the version to be published: all authors.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, L.L., Zmuda, E.J., Talavera, M.M. et al. Dual-specificity phosphatase (DUSP) genetic variants predict pulmonary hypertension in patients with bronchopulmonary dysplasia. Pediatr Res 87, 81–87 (2020). https://doi.org/10.1038/s41390-019-0502-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-019-0502-9
This article is cited by
-
Hyperoxia exposure upregulates Dvl-1 and activates Wnt/β-catenin signaling pathway in newborn rat lung
BMC Molecular and Cell Biology (2023)