Abstract
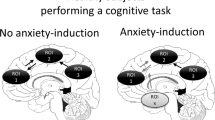
Myelination subserves efficient neuronal communication, and alterations in white matter (WM) microstructure have been implicated in numerous psychiatric disorders, including pathological anxiety. Recent work in rodents suggests that muscarinic antagonists may enhance myelination with behavioral benefits; however, the neural and behavioral effects of muscarinic antagonists have yet to be explored in non-human primates (NHP). Here, as a potentially translatable therapeutic strategy for human pathological anxiety, we present data from a first-in-primate study exploring the effects of the muscarinic receptor antagonist solifenacin on anxious behaviors and WM microstructure. 12 preadolescent rhesus macaques (6 vehicle control, 6 experimental; 8F, 4M) were included in a pre-test/post-test between-group study design. The experimental group received solifenacin succinate for ~60 days. Subjects underwent pre- and post-assessments of: 1) anxious temperament (AT)-related behaviors in the potentially threatening no-eye-contact (NEC) paradigm (30-min); and 2) WM and regional brain metabolism imaging metrics, including diffusion tensor imaging (DTI), quantitative relaxometry (QR), and FDG-PET. In relation to anxiety-related behaviors expressed during the NEC, significant Group (vehicle control vs. solifenacin) by Session (pre vs. post) interactions were found for freezing, cooing, and locomotion. Compared to vehicle controls, solifenacin-treated subjects exhibited effects consistent with reduced anxiety, specifically decreased freezing duration, increased locomotion duration, and increased cooing frequency. Furthermore, the Group-by-Session-by-Sex interaction indicated that these effects occurred predominantly in the males. Exploratory whole-brain voxelwise analyses of post-minus-pre differences in DTI, QR, and FDG-PET metrics revealed some solifenacin-related changes in WM microstructure and brain metabolism. These findings in NHPs support the further investigation of the utility of antimuscarinic agents in targeting WM microstructure as a means to treat pathological anxiety.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 13 print issues and online access
$259.00 per year
only $19.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Kessler RC, Petukhova M, Sampson NA, Zaslavsky AM, Wittchen HU. Twelve-month and lifetime prevalence and lifetime morbid risk of anxiety and mood disorders in the United States. Int J methods Psychiatr Res. 2012;21:169–84.
Konnopka A, König H. Economic burden of anxiety disorders: a systematic review and meta-analysis. Pharmacoeconomics. 2020;38:25–37.
Bandelow B, Michaelis S. Epidemiology of anxiety disorders in the 21st century. Dialogues Clin Neurosci. 2015;17:327–35.
Yang X, Fang Y, Chen H, Zhang T, Yin X, Man J, et al. Global, regional and national burden of anxiety disorders from 1990 to 2019: results from the Global Burden of Disease Study 2019. Epidemiol Psych Sci. 2021;30:e36.
Bandelow B, Michaelis S, Wedekind D. Treatment of anxiety disorders. Dialogues Clin Neurosci. 2017;19:93–107.
Ginsburg GS, Becker-Haimes EM, Keeton C, Kendall PC, Iyengar S, Sakolsky D, et al. Results from the child/adolescent anxiety multimodal extended long-term study (CAMELS): primary anxiety outcomes. J Am Acad Child Adolesc Psychiatry. 2018;57:471–80.
Ginsburg GS, Becker EM, Keeton CP, Sakolsky D, Piacentini J, Albano AM, et al. Naturalistic follow-up of youths treated for pediatric anxiety disorders. JAMA Psychiatry. 2014;71:310–8.
Scholten W, Have M ten, Geel C van, Balkom A van, Graaf R de, Batelaan N. Recurrence of anxiety disorders and its predictors in the general population. Psychol Med. 2023;53:1334–42.
Barnea-Goraly N, Menon V, Eckert M, Tamm L, Bammer R, Karchemskiy A, et al. White matter development during childhood and adolescence: a cross-sectional diffusion tensor imaging study. Cereb Cortex. 2005;15:1848–54.
Lebel C, Beaulieu C. Longitudinal development of human brain wiring continues from childhood into adulthood. J Neurosci. 2011;31:10937–47.
Costello EJ, Mustillo S, Erkanli A, Keeler G, Angold A. Prevalence and development of psychiatric disorders in childhood and adolescence. Arch Gen Psychiatry. 2003;60:837–44.
Aggarwal N, Williams LE, Tromp DPM, Pine DS, Kalin NH. A dynamic relation between whole-brain white matter microstructural integrity and anxiety symptoms in preadolescent females with pathological anxiety. Transl Psychiatry. 2022;12:57.
Tromp DPM, Williams LE, Fox AS, Oler JA, Roseboom PH, Rogers GM, et al. Altered uncinate fasciculus microstructure in childhood anxiety disorders in boys but not girls. Am J Psychiatry. 2019;176:208–16.
Fields RD. Myelin formation and remodeling. Cell. 2014;156:15–7.
Miron VE, Kuhlmann T, Antel JP. Cells of the oligodendroglial lineage, myelination, and remyelination. Biochim Biophys Acta 2011;1812:184–93.
Friedrich P, Fraenz C, Schlüter C, Ocklenburg S, Mädler B, Güntürkün O, et al. The relationship between axon density, myelination, and fractional anisotropy in the human corpus callosum. Cereb Cortex. 2020;30:2042–56.
Roberts TPL, Liu F, Kassner A, Mori S, Guha A. Fiber density index correlates with reduced fractional anisotropy in white matter of patients with glioblastoma. Am J Neuroradiol. 2005;26:2183–6.
Beaulieu C. The basis of anisotropic water diffusion in the nervous system—a technical review. NMR Biomed. 2002;15:435–55.
Lazari A, Lipp I. Can MRI measure myelin? systematic review, qualitative assessment, and meta-analysis of studies validating microstructural imaging with myelin histology. Neuroimage. 2021;230:117744.
Song SK, Yoshino J, Le TQ, Lin SJ, Sun SW, Cross AH, et al. Demyelination increases radial diffusivity in corpus callosum of mouse brain. Neuroimage. 2005;26:132–40.
Tromp DPM, Grupe DW, Oathes DJ, McFarlin DR, Hernandez PJ, Kral TRA, et al. Reduced structural connectivity of a major frontolimbic pathway in generalized anxiety disorder. Arch Gen psychiatry. 2012;69:925–34.
Baur V, Hänggi J, Rufer M, Delsignore A, Jäncke L, Herwig U, et al. White matter alterations in social anxiety disorder. J Psychiatr Res. 2011;45:1366–72.
Kim MJ, Whalen PJ. The structural integrity of an amygdala-prefrontal pathway predicts trait anxiety. J Neurosci. 2009;29:11614–8.
Liao M, Yang F, Zhang Y, He Z, Su L, Li L. White matter abnormalities in adolescents with generalized anxiety disorder: a diffusion tensor imaging study. BMC Psychiatry. 2014;14:41.
Westlye LT, Bjørnebekk A, Grydeland H, Fjell AM, Walhovd KB. Linking an anxiety-related personality trait to brain white matter microstructure: diffusion tensor imaging and harm avoidance. Arch Gen Psychiatry. 2011;68:369–77.
Tromp DPM, Fox AS, Oler JA, Alexander AL, Kalin NH. The relationship between the uncinate fasciculus and anxious temperament is evolutionarily conserved and sexually dimorphic. Biol Psychiatry. 2019;86:890–8.
Aggarwal N, Moody JF, Dean IDC, Tromp DPM, Kecskemeti SR, Oler JA, et al. Spatiotemporal dynamics of nonhuman primate white matter development during the first year of life. Neuroimage. 2021;231:117825.
Dimond D, Rohr CS, Smith RE, Dhollander T, Cho I, Lebel C, et al. Early childhood development of white matter fiber density and morphology. Neuroimage. 2020;210:116552.
Scholz J, Klein MC, Behrens TEJ, Johansen-Berg H. Training induces changes in white-matter architecture. Nat Neurosci. 2009;12:1370–1.
Sampaio-Baptista C, Khrapitchev AA, Foxley S, Schlagheck T, Scholz J, Jbabdi S, et al. Motor skill learning induces changes in white matter microstructure and myelination. J Neurosci. 2013;33:19499–503.
Liu J, Dupree JL, Gacias M, Frawley R, Sikder T, Naik P, et al. Clemastine enhances myelination in the prefrontal cortex and rescues behavioral changes in socially isolated mice. J Neurosci. 2016;36:957–62.
Abiraman K, Pol SU, O’Bara MA, Chen GD, Khaku ZM, Wang J, et al. Anti-muscarinic adjunct therapy accelerates functional human oligodendrocyte repair. J Neurosci. 2015;35:3676–88.
Welliver RR, Polanco JJ, Seidman RA, Sinha AK, O’Bara MA, Khaku ZM, et al. Muscarinic receptor m3r signaling prevents efficient remyelination by human and mouse oligodendrocyte progenitor cells. J Neurosci. 2018;38:6921–32.
Fields RD, Dutta DJ, Belgrad J, Robnett M. Cholinergic signaling in myelination. Glia. 2017;65:687–98.
Pan S, Mayoral SR, Choi HS, Chan JR, Kheirbek MA. Preservation of a remote fear memory requires new myelin formation. Nat Neurosci. 2020;23:487–99.
Du W, Deng Y, Jiang R, Tong L, Li R, Jiang X. Clemastine enhances myelination, delays axonal loss and promotes functional recovery in spinal cord injury. Neurochem Res. 2022;47:503–15.
Li Z, He Y, Fan S, Sun B. Clemastine rescues behavioral changes and enhances remyelination in the cuprizone mouse model of demyelination. Neurosci Bull. 2015;31:617–25.
Green AJ, Gelfand JM, Cree BA, Bevan C, Boscardin WJ, Mei F, et al. Clemastine fumarate as a remyelinating therapy for multiple sclerosis (ReBUILD): a randomised, controlled, double-blind, crossover trial. Lancet. 2017;390:2481–9.
Drug Approval Package: VesiCare (Solifenacin Succinate) NDA #021518 [Internet]. Available from: https://www.accessdata.fda.gov/drugsatfda_docs/nda/2004/21-518_VesiCare.cfm. Accessed 25 Dec 2022.
Kalin NH, Shelton SE. Defensive behaviors in infant rhesus monkeys: environmental cues and neurochemical regulation. Science. 1989;243:1718–21.
Kalin NH. The neurobiology of fear. Sci Am. 1993;268:94–101.
Fox AS, Oler JA, Shackman AJ, Shelton SE, Raveendran M, McKay DR, et al. Intergenerational neural mediators of early-life anxious temperament. Proc Natl Acad Sci. 2015;112:9118–22.
Rosenbaum JF, Biederman J, Bolduc-Murphy EA, Faraone SV, Chaloff J, Hirshfeld DR, et al. Behavioral inhibition in childhood: a risk factor for anxiety disorders. Harv Rev Psychiatry. 1993;1:2–16.
Shackman AJ, Fox AS, Oler JA, Shelton SE, Oakes TR, Davidson RJ, et al. Heightened extended amygdala metabolism following threat characterizes the early phenotypic risk to develop anxiety-related psychopathology. Mol Psychiatry. 2017;22:724–32.
Goldsmith HH, Hilton EC, Phan JM, Sarkisian KL, Carroll IC, Lemery-Chalfant K, et al. Childhood inhibition predicts adolescent social anxiety: findings from a longitudinal twin study. Dev Psychopathol. 2022;34:1666–85.
Birn RM, Shackman AJ, Oler JA, Williams LE, McFarlin DR, Rogers GM, et al. Evolutionarily conserved prefrontal-amygdalar dysfunction in early-life anxiety. Mol Psychiatry. 2014;19:915–22.
Nair AB, Jacob S. A simple practice guide for dose conversion between animals and human. J Basic Clin Pharm. 2016;7:27–31.
Nair A, Morsy MA, Jacob S. Dose translation between laboratory animals and human in preclinical and clinical phases of drug development. Drug Dev Res. 2018;79:373–82.
Fox AS, Shelton SE, Oakes TR, Davidson RJ, Kalin NH. Trait-like brain activity during adolescence predicts anxious temperament in primates. PLoS One. 2008;3:e2570.
Kecskemeti S, Samsonov A, Hurley SA, Dean DC, Field A, Alexander AL. MPnRAGE: a technique to simultaneously acquire hundreds of differently contrasted MPRAGE images with applications to quantitative T1 mapping. Magn Reson Med. 2015;75:1040–53.
Kecskemeti S, Samsonov A, Velikina J, Field AS, Turski P, Rowley H, et al. Robust motion correction strategy for structural mri in unsedated children demonstrated with three-dimensional radial MPnRAGE. Radiology. 2018;289:509–16.
Avants BB, Epstein CL, Grossman M, Gee JC. Symmetric diffeomorphic image registration with cross-correlation: Evaluating automated labeling of elderly and neurodegenerative brain. Med Image Anal. 2008;12:26–41.
Camino: Open-Source Diffusion-MRI Reconstruction and Processing − 02759.pdf [Internet]. Available from: https://afni.nimh.nih.gov/sscc/staff/rwcox/ISMRM_2006/ISMRM%202006%20-%203340/files/02759.pdf. Accessed 24 Jan 2021.
Zhang H, Yushkevich P, Alexander D, Gee J. Deformable registration of diffusion tensor MR images with explicit orientation optimization. Med Image Anal. 2006;10:764–85.
Jenkinson M, Beckmann CF, Behrens TEJ, Woolrich MW, Smith SM. FSL. Neuroimage. 2012;62:782–90.
Brauer M, Curtin JJ. Linear mixed-effects models and the analysis of nonindependent data: a unified framework to analyze categorical and continuous independent variables that vary within-subjects and/or within-items. Psychol Methods. 2018;23:389–411.
Cox RW. AFNI: software for analysis and visualization of functional magnetic resonance neuroimages. Comput Biomed Res. 1996;29:162–73.
Cherubini A, Péran P, Hagberg GE, Varsi AE, Luccichenti G, Caltagirone C, et al. Characterization of white matter fiber bundles with T2* relaxometry and diffusion tensor imaging. Magn Reson Med. 2009;61:1066–72.
Moody JF, Aggarwal N, Dean DC, Tromp DPM, Kecskemeti SR, Oler JA, et al. Longitudinal assessment of early-life white matter development with quantitative relaxometry in nonhuman primates. Neuroimage. 2022;251:118989.
Marisca R, Hoche T, Agirre E, Hoodless LJ, Barkey W, Auer F, et al. Functionally distinct subgroups of oligodendrocyte precursor cells integrate neural activity and execute myelin formation. Nat Neurosci. 2020;23:363–74.
Levine JM, Reynolds R, Fawcett JW. The oligodendrocyte precursor cell in health and disease. Trends Neurosci. 2001;24:39–47.
Crawford AH, Stockley JH, Tripathi RB, Richardson WD, Franklin RJM. Oligodendrocyte progenitors: adult stem cells of the central nervous system? Exp Neurol. 2014;260:50–5.
Fernandez-Castaneda A, Gaultier A. Adult oligodendrocyte progenitor cells – multifaceted regulators of the CNS in health and disease. Brain Behav Immun. 2016;57:1–7.
Clayton BLL, Tesar PJ. Oligodendrocyte progenitor cell fate and function in development and disease. Curr Opin Cell Biol. 2021;73:35–40.
Zhang SC, Ge B, Duncan ID. Adult brain retains the potential to generate oligodendroglial progenitors with extensive myelination capacity. Proc Natl Acad Sci. 1999;96:4089–94.
Deoni SCL. Quantitative relaxometry of the brain. Top Magn Reson Imaging. 2010;21:101–13.
O’Muircheartaigh J, Vavasour I, Ljungberg E, Li DKB, Rauscher A, Levesque V, et al. Quantitative neuroimaging measures of myelin in the healthy brain and in multiple sclerosis. Hum Brain Mapp. 2019;40:2104–16.
Kumar R, Nguyen HD, Macey PM, Woo MA, Harper RM. Regional brain axial and radial diffusivity changes during development. J Neurosci Res. 2012;90:346–55.
Winklewski PJ, Sabisz A, Naumczyk P, Jodzio K, Szurowska E, Szarmach A. Understanding the physiopathology behind axial and radial diffusivity changes—what do we know? Front Neurol. 2018;9:92.
Alexander AL, Lee JE, Lazar M, Field AS. Diffusion tensor imaging of the brain. Neurotherapeutics. 2007;4:1–14.
Kalin NH, Fox AS, Kovner R, Riedel MK, Fekete EM, Roseboom PH, et al. Overexpressing corticotropin-releasing factor in the primate amygdala increases anxious temperament and alters its neural circuit. Biol Psychiatry. 2016;80:345–55.
Furey ML, Drevets WC. Antidepressant efficacy of the antimuscarinic drug scopolamine: a randomized, placebo-controlled clinical trial. Arch Gen Psychiatry. 2006;63:1121–9.
Sipos ML, Burchnell V, Galbicka G. Dose-response curves and time-course effects of selected anticholinergics on locomotor activity in rats. Psychopharmacology 1999;147:250–6.
Scarr E. Muscarinic receptors: their roles in disorders of the central nervous system and potential as therapeutic targets. CNS Neurosci Ther. 2012;18:369–79.
Yamada M, Miyakawa T, Duttaroy A, Yamanaka A, Moriguchi T, Makita R, et al. Mice lacking the M3 muscarinic acetylcholine receptor are hypophagic and lean. Nature. 2001;410:207–12.
Cerghet M, Skoff RP, Swamydas M, Bessert D. Sexual dimorphism in the white matter of rodents. J Neurol Sci. 2009;286:76–80.
Yasuda K, Maki T, Kinoshita H, Kaji S, Toyokawa M, Nishigori R, et al. Sex-specific differences in transcriptomic profiles and cellular characteristics of oligodendrocyte precursor cells. Stem Cell Res. 2020;46:101866.
Swamydas M, Bessert D, Skoff R. Sexual dimorphism of oligodendrocytes is mediated by differential regulation of signaling pathways. J Neurosci Res. 2009;87:3306–19.
Fox AS, Kalin NH. A translational neuroscience approach to understanding the development of social anxiety disorder and its pathophysiology. Am J Psychiatry. 2014;171:1162–73.
Acknowledgements
We thank Dr. Jason F. Moody for his expertize and assistance with the quantitative relaxometry analyses, and Carissa Boettcher for assisting with the animal care and experimentation protocols. We also thank the many other members of the staffs of the Harlow Center for Biological Psychology and Wisconsin National Primate Research Center. This work was supported by grants from the National Institutes of Health: R01-MH081884 (NHK); R01-MH046729 (NHK)—includes NIH Bench-to-Bedside supplement (Award ID: 654199; MAB, NHK); T32-GM140935 (NA); T32-MH018931 (NA). The funding sources played no role in the conceptualization, design, execution, or analysis of any part of the study.
Author information
Authors and Affiliations
Contributions
NA, JAO, DPMT, PHR, MKR, VRE, MAB, and NHK all made substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data for the work. NA and NHK drafted the work, and all authors contributed to critically revising the draft for important intellectual content and provided final approval of the version to be published. NA and NHK agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Competing interests
NHK reported receiving grants from the National Institute of Mental Health; consulting to CME Outfitters, the Pritzker Neuropsychiatric Disorders Research Consortium, the Skyland Trail Advisory Board, the Early Life Adversity Research External Scientific Advisory Board at the University of Texas at Austin, and Corcept Therapeutics Incorporated; and serving as editor-in-chief of The American Journal of Psychiatry during the conduct of the study. The other authors report no potential conflicts of interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Aggarwal, N., Oler, J.A., Tromp, D.P.M. et al. A preliminary study of the effects of an antimuscarinic agent on anxious behaviors and white matter microarchitecture in nonhuman primates. Neuropsychopharmacol. 49, 405–413 (2024). https://doi.org/10.1038/s41386-023-01686-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41386-023-01686-1