Abstract
The most common chemogenetic neuromodulatory system, designer receptors exclusively activated by designer drugs (DREADDs), uses a non-endogenous actuator ligand to activate a modified muscarinic acetylcholine receptor that is insensitive to acetylcholine. It is crucial in studies using these systems to test the potential effects of DREADD actuators prior to any DREADD transduction, so that effects of DREADDs can be attributed to the chemogenetic system rather than the actuator drug, particularly in experiments using nonhuman primates. We investigated working memory performance after injections of three DREADD actuators, clozapine, olanzapine, and deschloroclozapine, in four male rhesus monkeys tested in a spatial delayed response task before any DREADD transduction took place. Performance at 0.1 mg/kg clozapine and 0.1 mg/kg deschloroclozapine did not differ from vehicle in any of the four subjects. 0.2 mg/kg clozapine impaired working memory function in three of the four monkeys. Two monkeys were impaired after 0.1 mg/kg olanzapine and two were impaired after 0.3 mg/kg deschloroclozapine. We speculate that the unique neuropharmacology of prefrontal cortex function makes the primate prefrontal cortex especially vulnerable to off-target effects of DREADD actuator drugs with affinity for endogenous monoaminergic receptor systems. These findings underscore the importance of within-subject controls for DREADD actuator drugs in the specific tasks under study to confirm that effects following DREADD receptor transduction are not owing to the actuator drug itself. They also suggest that off-target effects of DREADD actuators may limit translational applications of chemogenetic neuromodulation.
Similar content being viewed by others
Introduction
Chemogenetic technologies are widely used to reversibly targetspecific neuronal populations and circuitry in awake, behaving animals [1,2,3,4,5]. The most common chemogenetic system uses designer receptors exclusively activated by designer drugs (DREADDs) composed of a modified muscarinic acetylcholine receptor that is no longer sensitive to acetylcholine but is responsive to an otherwise inert drug [6]. Clozapine-N-oxide (CNO), a metabolite of the antipsychotic clozapine, was initially the primary actuator drug used with DREADDs [7]. However, drawbacks of CNO include poor brain penetrance, action as a substrate for P-glycoprotein, and reverse metabolism to its parent compound [8,9,10,11]. Together these shortcomings have sparked the need for new actuator drugs to use with DREADDs [12,13,14,15].
Three of these new actuators—low-dose clozapine, low-dose olanzapine, and deschloroclozapine—possess better brain penetrance and higher affinity and potency for DREADD receptors than CNO. All of these actuators have been tested in rodent systems [8, 13, 16] and low-dose clozapine [17] and deschloroclozapine [18] have been tested in nonhuman primates. Clozapine and olanzapine are atypical antipsychotics designed for clinical use, and deschloroclozapine is a metabolite of clozapine; each has high affinity for DREADD receptors [8, 13, 18]. Importantly, these drugs can activate DREADD receptors at doses lower than those associated with their therapeutic effects [19,20,21,22].
In this study, we tested two doses each of these three different DREADD actuators on a spatial working memory task in rhesus monkeys that had not yet received DREADD transduction. We tested all of these actuators so that we could select drugs to use as part of a subsequent study of DREADD neuromodulation in nonhuman primates. Published studies of monkeys do not always include these controls, sometimes because of experimental constraints (for example, developmental studies, ref. [17]). Most rodent studies do not include within-subject comparisons, yet these data would be necessary to account for any individual differences in response to DREADD actuators. It is important in studies using any actuator with these chemogenetic systems to test the potential effects of the actuator prior to DREADD transduction in the behavioral task, so that effects of DREADDs can be attributed to the chemogenetic system and not the actuator drug itself.
Materials and methods
Subjects
Four male rhesus macaques, noted as Cases A, J, Ro, and Ru, aged between 5 and 6 years and weighing 5.5–7.9 kg at the time of injection, were used for this study. Case A in this study is a different monkey than Case A from [3]. Monkeys were socially housed indoors in single-sex groups. Daily meals consisted of monkey chow and a variety of fruits and vegetables, and were distributed within transport cages once testing was completed. On weekends, monkeys were fed in their home cages. Within the home cage, water was available ad libitum. Environmental enrichment, in the form of play objects and small food items, was provided daily in the home cage. All procedures were approved by the Icahn School of Medicine Institutional Animal Care and Use Committee and conform to NIH guidelines on the use of nonhuman primates in research.
Apparatus
Testing was performed within a Wisconsin General Testing Apparatus (WGTA). The WGTA is a small enclosed testing area where the experimenter can manually interact with the monkey during testing. Monkeys were trained to move from the home cage to a metal transport cage, which was then wheeled into the WGTA. The experimenter was hidden from the monkey’s view by a one-way mirror, with only the experimenter’s hands visible. A sliding tray with two food wells could be maneuvered back-and-forth between the experimenter and the monkey. A pulley-operated opaque black screen could be lowered by the experimenter to separate the tray from the monkey during testing.
Behavioral testing
Training on the delayed response task followed [23, 24]. Monkeys were first shown a small food reward (craisin or M&M) that was placed in one of two food wells on a sliding tray. The left/right location of the reward was chosen across trials based on a pseudorandomly, counterbalanced sequence. Both wells were then covered with flat, gray tiles and a black opaque screen was lowered between the tray and the monkey for a predefined delay period. The screen was subsequently raised, and the test tray was advanced to the monkey, allowing the monkey to displace one of the well covers (Fig. 1). During initial shaping, monkeys were taught to displace the tiles covering the wells and select the reward. Once monkeys readily displaced the tiles, they progressed through three stages of training with 24 trials per session. Once a monkey reached criterion on the third stage of training, experimental training began. In the experimental task, each trial consisted of one of five possible delays (5, 10, 15, 20, or 30 s) and left or right well location. These delay/location pairings were varied pseudorandomly across trials such that each delay occurred six times and each well location occurred fifteen times in each testing session. Drug injections began once a monkey had achieved stable performance on the task. Monkeys continued with this variable delay design of the delayed response task for ~1 year during the remainder of the experiment, through vehicle injections and injection of all drug conditions. All monkeys completed three sessions of each dose condition for olanzapine and deschloroclozapine, except for Case J who completed two sessions after injection of the 0.05 mg/kg dose of olanzapine. Monkeys completed between 4 and 5 sessions each for the 0.2 mg/kg clozapine condition and between 6 and 9 sessions each after 0.1 mg/kg clozapine.
Drugs
Pharmacology
Clozapine, marketed as the prototype atypical antipsychotic Clozaril™, is FDA-approved and treats psychosis related to schizophrenia and Parkinson’s disease [25, 26]. It is a dopamine receptor antagonist with an affinity for D4 receptors (Ki = 39 nm) and shows high affinity for serotonin 5-HT2A receptors (Ki = 13 nm) and muscarinic M1 and M3 receptors (Ki = 14 nm and 25 nm, respectively) [25, 27, 28]. A dose of 0.1 mg/kg clozapine is effective at activating DREADD receptors in vivo in monkeys [17]. Olanzapine, a second-generation atypical antipsychotic and also FDA-approved, has been documented as a potentially safer, yet not as effective, alternative to clozapine. Olanzapine displays potent antagonism for dopamine D1/D2 receptors (Ki = 58 nm and 21 nm, respectively) and serotonin 5-HT2A receptors (Ki = 2.65 nm) [20, 25, 29]. It has recently been shown that olanzapine is a potent actuator at the inhibitory hM4D(Gi) DREADD receptor in vivo [13]. Both actuators are FDA-approved which could facilitate their application for chemogenetic technologies in a clinical setting. Deschloroclozapine is a dual dopamine and serotonin receptor antagonist with some selectivity for D1 (Ki = 200 nm), 5-HT2A (Ki = 87 nm), and M5 receptors (Ki = 55 nm) [18]. A dose of 0.1 mg/kg i.m. of deschloroclozapine is effective at activating DREADD receptors in vivo and reversibly inducing behavioral effects in monkeys [18].
Preparation
Drugs were prepared fresh daily, at concentrations so that monkeys received 0.1 ml/kg for injection (e.g., for a 0.2 mg/kg dose of drug, drug solution was prepared at a concentration of 2.0 mg/ml). Solutions were filtered through a 0.22 µm syringe filter and pH was determined before injection. Acetic acid, sodium acetate, and sodium hydroxide (NaOH) were all obtained from Fisher Scientific. Concentrations used for glacial acetic acid, sodium acetate, and NaOH were 99.7% (v/v), 1 m, and 0.2 m, respectively. Clozapine (Tocris, Minneapolis, MN) was stored at room temperature. Clozapine was given at 0.1 or 0.2 mg/kg, intramuscularly. For 0.1 mg/kg, clozapine powder was first dissolved in acetic acid and sodium acetate then diluted with NaOH to a final concentration in 0.25/50/49.75 acetic acid/sodium acetate/NaOH (v/v/v). For 0.2 mg/kg, the same reagents were used but the final concentration was 0.5/50/49.5 acetic acid/sodium acetate/NaOH (v/v/v). Olanzapine (Tocris, Minneapolis, MN) was stored at room temperature and given at 0.05 or 0.1 mg/kg, intramuscularly. Olanzapine solutions were made using the same method as above for the 0.1 mg/kg clozapine dose. Deschloroclozapine (DCZ; Medchemexpress, Monmouth Junction, NJ) was stored at 4 °C and was given at 0.1 mg/kg and 0.3 mg/kg, intramuscularly. Low dose of deschloroclozapine was made using the same method as low-dose clozapine and high-dose deschloroclozapine was made using the same method as the higher dose of clozapine. Vehicle injections consisted of 0.25/50/49.75 acetic acid, sodium acetate, and NaOH and were given at 0.1 ml/kg. Actuator injections were never administered more than twice in 1 week and never on adjacent test days to allow for a washout period, accounting for the half-life of clozapine (14.2 h on average) and olanzapine (33 h on average) [30]. There were vehicle or no-injection test days on other days of the test week. Actuators were not counterbalanced; we tested clozapine, olanzapine, and deschloroclozapine in that order in each monkey. Within drug conditions, however, doses were shuffled in order across drug test days. We also interpolated additional clozapine test days during testing with the other two actuators. Throughout the study, we did not observe any order effects or obvious effects on behavior on the days following actuator injections. Clozapine and olanzapine were given in the home cage 10 min before the start of testing and deschloroclozapine was given in the home cage 30 min before the start of testing. Clozapine and olanzapine both get into the brain fairly quickly and previous DREADD studies using these actuators have started behavior 10 min post injection [13, 17]. Deschloroclozapine shows a slightly slower timescale with higher plasma concentration ~15–30 min after intramuscular injection and CSF concentration continues to rise between 30 min to 90 min post injection [18]. Accordingly, beginning the delayed response task 30 min post injection for deschloroclozapine would allow sufficient time for the actuator to get into the brain.
Statistical analysis
Analyses were performed in RStudio with R 3.5 [31] using the lme4, lmerTest, and emmeans packages [32, 33]. Data were analyzed with a generalized linear mixed model and binomial distribution, with trial outcome (correct or incorrect) as the outcome variable, injection and delay as fixed effects, and case as a random effect to account for repeated sessions across time for each monkey. Two models were estimated for each drug condition (CLZ, OLZ, and DCZ) across all four cases comparing the two drug doses in each condition to vehicle (VEH). A “full” model included a two-way interaction term between Injection (VEH, 0.1 mg/kg CLZ, 0.2 mg/kg CLZ for clozapine; VEH, 0.05 mg/kg OLZ, 0.1 mg/kg OLZ for olanzapine; VEH, 0.1 mg/kg DCZ, 0.3 mg/kg DCZ for deschloroclozapine) and delay (5–30 sec) to examine how actuator injection affected working memory performance over delay intervals during the delayed response task. A “reduced” model with delay alone as a fixed effect was estimated and, using a hierarchical approach, we assessed model fit between the two models. If Injection significantly improved model fit (i.e., there was a significant effect of injection on task performance) we calculated estimated marginal means from the “full” fitted model for each drug condition across all four cases. We analyzed pairwise comparisons and contrasts to determine differences in performance between VEH and each actuator drug dose as well as differences between the two doses of each actuator drug themselves. Owing to inter-case variability across monkeys in response to actuator drug, a generalized linear model for each drug condition was also computed for each case regardless of the outcome of the overall model. We next calculated estimated marginal means from the “full” fitted model for each case and analyzed pairwise contrasts to determine any differences in performance between (1) VEH and each actuator drug dose and (2) two doses of each actuator drug themselves. Interaction analyses were calculated using the estimated marginal means to examine whether a dose of an actuator drug modified the working performance over delay for each monkey. Reported confidence intervals are given on a log odds ratio scale. P values and confidence intervals were adjusted using the Tukey method for multiple comparisons. Because three out of four monkeys had no variability at a particular delay or delays during actuator drug sessions, the five levels for the Delay factor were collapsed into “short delay” and “long delay” levels for some analyses (noted for each monkey). Full models, those for each drug condition across all four cases and those for individual cases, were tested for over/underdispersion of residuals using simulation-based tests to measure deviation of residuals and dispersion of residual standard deviations [34]. All evaluations of model residuals returned no significant over/underdispersion (two-sided nonparametric test, p > 0.05). We recorded the total time to complete each behavioral session to use as a proxy for motivation during the delayed response task. Data were analyzed in a linear mixed model for each actuator condition (CLZ, OLZ, and DCZ) across all four cases with total session time as the outcome variable, Injection as a fixed effect, and case as a random effect. After each model was generated, we calculated the estimated marginal means and analyzed the pairwise contrasts to determine any differences in total session time between VEH and each actuator at both tested doses.
Results
Effect of clozapine on working memory performance
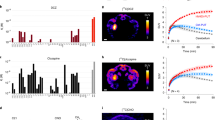
Comparison of our full and reduced models showed that including injection and injection×delay interaction terms significantly improved our model fit (X2(10) = 32.209, p = 0.0003695). Analysis of the estimated marginal means comparisons from our full model across all four cases revealed that monkeys showed significant working memory impairment after 0.2 mg/kg clozapine compared with vehicle (Fig. 2a; p = 0.0007, 95% confidence interval of (0.173, 0.779)). We found a significant effect on working memory performance between the two doses of clozapine (p = 0.001, (0.222, 1.058)). Pairwise comparisons of each vehicle-clozapine dose pair across all four monkeys revealed a significant effect of the higher 0.2 mg/kg clozapine dose relative to vehicle and 0.1 mg/kg clozapine at the 30 second delay interval only (p = 0.0002).
a Performance after clozapine injection for each case across all tested delay intervals. b Performance after administration of olanzapine. c Performance after administration of deschloroclozapine. Data are represented as mean performance ± sem. VEH vehicle, CLZ clozapine, OLZ olanzapine, DCZ deschloroclozapine.
For the analysis of pairwise contrasts for each case, delays were binned into “short” (5–20 s) and “long” (30 s) groups. Comparisons of estimated marginal means for each monkey showed that Cases A, Ro, and Ru were significantly impaired in the spatial delayed response task after 0.2 mg/kg clozapine compared witih performance after vehicle (Table 1). Interestingly, Case A also showed a significant difference in working memory performance between the two doses of clozapine. Case A had a significant interaction between Injection and Delay terms (p = 0.0103). This interaction was primarily driven by the longer delay period with worsening delayed response performance with the higher clozapine dose and the long 30 s delay group (p = 0.0005). No monkey showed impairment in working memory performance after the 0.1 mg/kg clozapine dose compared with vehicle performance.
Effect of olanzapine on working memory performance
Analysis of our full and reduced models revealed that inclusion of Injection and Injection x Delay terms did not significantly improve model fit (X2(10) = 6.558, p = 0.7664) indicating there was no consistent difference across the four cases. To examine variability within our cases, we also computed a full model for each monkey. For Case Ro, delays were binned into the same “short” (5–20 s) and “long” (30 s) groups. We found that Cases A and Ro were significantly impaired in working memory performance after administration of the higher 0.1 mg/kg dose of olanzapine (Fig. 2b). Case Ro also had significantly more incorrect trials in the delayed response task after the lower 0.05 mg/kg dose of olanzapine compared to vehicle.
Effect of deschloroclozapine on working memory performance
Including injection and injection×delay interaction terms significantly improved our deschloroclozapine model compared with delay alone (X2(10) = 19.686, p = 0.03237). Comparison of estimated marginal means for our full fitted model across all four cases revealed a significant contrast between vehicle and the higher 0.3 mg/kg dose of deschloroclozapine (p = 0.0058, 95% confidence interval of (0.1093, 0.802)). Analysis of the estimated marginal means for the full model for each case showed Cases A and Ro were significantly impaired in delayed response performance after 0.3 mg/kg dose compared with performance after vehicle (Table 1). Owing to no variability at two delays, Case Ro again had binned “short” and “long” delays. Case Ro also had a significant difference between the two doses of deschloroclozapine with greater working memory deficit after the 0.3 mg/kg dose. No monkey showed a significant impairment in working memory performance after the lower 0.1 mg/kg dose of deschloroclozapine (Fig. 2c).
Effect of DREADD actuators on time to complete behavioral testing and other behaviors
For testing sessions (each composed of 30 trials; all monkeys completed 30 trials during all test sessions), we calculated the total time to complete the delayed response task and used this measure as a proxy for motivation. After comparing the estimated marginal means from the model for each actuator condition, we found that there was no significant difference in total session time between vehicle and any actuator drug and tested dose (p > 0.05, across all four cases for clozapine, olanzapine, and deschloroclozapine). Actuator conditions did not affect monkeys’ ability to complete the 30 trials in each session on all testing days. It was also apparent during testing that Cases A, J, and Ro displayed an increased amount of lachrymation and cooing behaviors during each olanzapine testing session; no noticeable increase in these behaviors was noted for vehicle or other actuator drugs. These behaviors were scored as present or absent during test sessions. The increase in cooing behavior in olanzapine sessions did not lead to a difference in time to complete the delayed response task, and we did not observe this behavior with the other two actuators.
Discussion
We found that some monkeys showed deficits in the delayed response task after administration of actuator drugs prior to any DREADD transduction. For clozapine, three out of four monkeys were impaired in working memory function by the higher 0.2 mg/kg dose, which is far less than doses tested for therapeutic effects (ranging 2.5–6 mg/kg) [19,20,21,22]. Two out of four monkeys showed working memory deficits after the higher 0.1 mg/kg dose of olanzapine and one of those monkeys, Case Ro, additionally showed significant impairment compared with vehicle after the 0.05 mg/kg dose. Similar to clozapine, both of the tested doses for olanzapine are below a therapeutic dose of 0.35 mg/kg yet have been shown to effectively activate DREADDs [13, 20]. The two monkeys impaired by doses of olanzapine were also impaired by the higher 0.3 mg/kg dose of deschloroclozapine. We found that no monkey was impaired in delayed response performance after 0.1 mg/kg clozapine or 0.1 mg/kg deschloroclozapine and we plan on moving forward with those actuators and doses for our future neuromodulatory studies.
We speculate that the delayed response task may be particularly sensitive to the actuators used in this study owing to the neuropharmacology of the prefrontal cortex, a region heavily involved in working memory function [35,36,37,38]. Indeed, dopamine and serotonin receptor subtypes antagonized by these three actuator drugs are enriched in primate prefrontal cortex, and D1/D2 and 5-HT2A specifically have been heavily implicated in working memory function [20, 25, 39,40,41]. We found a slight dependence of impairment on delay with the higher doses of clozapine and deschloroclozapine on delayed response performance with greater impairment at higher delay intervals (20–30 s). This behavioral deficit at higher delay periods would point to a working memory effect and demonstrate that antagonism of these receptors did not impair delayed response performance overall, but instead performance where memory of reward location in the task must be maintained for the longest periods. Our goal for this study was not to examine the receptor mechanisms of these drugs, and in the absence of pharmacokinetic data on each monkey we do not know whether individual differences in drug response were related to individual differences in drug distribution and/or metabolism. Nevertheless, these findings indicate significant individual differences in response to DREADD actuator drugs in the absence of DREADD receptor expression, putting limits on dosing and indicating that testing with actuator drugs prior to DREADD receptor transduction is an essential component of experimental design.
A recent study also investigated the role of acute systemic low-dose clozapine on a battery of behaviors in wild-type rats [42]. Low-dose clozapine (0.1 mg/kg) did not affect working memory function measured as performance in a delayed alternation task, but did affect other behaviors such as locomotion, anxiety, and cognitive flexibility. Thus, similar to our findings in nonhuman primates, actuator drugs can have DREADD-independent effects at a high enough dose. We stress that our findings demonstrate that these behavioral effects can occur in a cognitive task with doses far below the therapeutic range tested in nonhuman primates (clozapine: 6 mg/kg; olanzapine: 0.35 mg/kg) that would normally not be expected to have any effects on their own.
We selected these three actuator drugs owing to their affinity and efficacy at DREADD receptors and their evidence in rodent and nonhuman primate behavioral models. Two recently developed compounds, JHU37152 (J52) and JHU37160 (J60), also display high in vivo occupancy and potency for DREADD receptors in mice and monkeys [14]. These drugs exhibit greater DREADD activation than clozapine at lower concentrations, indicating that they are more potent agonists at DREADD receptors. In contrast, another actuator drug, Compound 21, exhibits similar potency to CNO at the DREADD receptor; however, this potency is lower than both J52 and J60 and thus may not be practical for applications in nonhuman primates [12, 14, 16]. Recently, it was reported that low-dose compound 21 also produced metabolic changes in brain activity (FDG uptake), whereas an equipotent dose of clozapine produced no changes [14].
Although the most commonly used form of DREADDs uses the modified G-protein coupled receptor, other chemogenetic technologies, including the KORD DREADD derived from a modified κ-opioid receptor [43] and the recently reported pharmacologically selective actuator modules (PSAMs) [44], are available to modulate neuronal regions and circuitry. For our study, we selected the muscarinic acetylcholine receptor-based DREADDs owing to their extensive application in nonhuman primates in both our own behavioral studies as well as several others [1,2,3, 17]. There has been limited evidence of PSAMs in nonhuman primates and the low solubility of Salvanorin B, the actuator for KORD DREADD, makes dosing monkeys difficult. Any actuator drug or technology employed should be scrutinized as those in this study and similar preoperative experiments should be conducted for any planned doses.
For studies using DREADDs, particularly those in nonhuman primates, it would be critical to obtain an upper limit of an actuator dose for each animal prior to DREADD transduction and determine individual variability with dosages. After DREADDs are expressed, it is not possible to ascertain whether a “low” dose of actuator has any effect on its own. Our findings also indicate that different potential DREADD actuators, even at “low” doses, may have different patterns of off-target effects in different behavioral paradigms, as in the case of olanzapine here. Therefore, we stress the importance of validating each drug and dosage in the context of the planned behavioral testing post-DREADD transduction and in a within-subjects design when possible. It may not be adequate to confirm in a subset of monkeys that chosen doses of actuators used to activate DREADD receptors are ineffective on their own, given the presence of marked individual differences that we observed, or to use blanket dosing recommendations across different behavioral settings. Including these experiments in chemogenetic studies will ensure that any behavioral output post transduction can be attributed to the activated chemogenetic system and not administration of the actuator drug itself. In DREADD experiments using rodents, a common control to account for potential effects of an actuator alone is to express eGFP in two groups and test injections of vehicle in one group and actuator drug in the other. The within-subject design in this study testing effects of an actuator prior to transduction of any vector system could provide the same control and importantly reduce the number of animals used compared with that in a between-subject design.
These findings also indicate caution as chemogenetic neuromodulation strategies start to move toward potential clinical applications. A significant strength of these approaches is the potential to manipulate neural activity in a circuit-specific manner that is not possible with electrical stimulation. However, the requirement to use a pharmacological actuator to activate the DREADD receptors has the potential for unintended off-target effects, as seen here. As these strategies continue to be refined, as much attention needs to be paid to design of the “key” as to the “lock” [6].
Funding and disclosure
Authors have no conflicts of interest to report. This work was supported by R21NS096936 (MGB) and T32AG049688 (NAU).
References
Eldridge MAG, Lerchner W, Saunders RC, Kaneko H, Krausz KW, Gonzalez FJ, et al. Chemogenetic disconnection of monkey orbitofrontal and rhinal cortex reversibly disrupts reward value. Nat Neurosci 2016;19:37–39.
Grayson DS, Bliss-Moreau E, Machado CJ, Bennett J, Shen K, Grant KA, et al. The rhesus monkey connectome predicts disrupted functional networks resulting from pharmacogenetic inactivation of the amygdala. Neuron 2016;91:453–66.
Upright NA, Brookshire SW, Schnebelen W, Damatac CG, Hof PR, Browning PGF, et al. Behavioral effect of chemogenetic inhibition is directly related to receptor transduction levels in rhesus monkeys. J Neurosci. 2018;38:7969–75.
Malvaez M, Shieh C, Murphy MD, Greenfield VY, Wassum KM. Distinct cortical–amygdala projections drive reward value encoding and retrieval. Nat Neurosci. 2019;22:685–6.
Vetere G, Tran LM, Moberg S, Steadman PE, Restivo L, Morrison FG, et al. Memory formation in the absence of experience. Nat Neurosci. 2019;22:933–40.
Armbruster BN, Li X, Pausch MH, Herlitze S, Roth BL. Evolving the lock to fit the key to create a family of G protein-coupled receptors potently activated by an inert ligand. Proc Natl Acad Sci 2007;104:5163–8.
Roth BL. DREADDs for Neuroscientists. Neuron 2016;89:683–94.
Gomez JL, Bonaventura J, Lesniak W, Mathews WB, Sysa-Shah P, Rodriguez LA, et al. Chemogenetics revealed: DREADD occupancy and activation via converted clozapine. Science 2017;357:503–7.
Raper J, Morrison RD, Daniels JS, Howell L, Bachevalier J, Wichmann T, et al. Metabolism and distribution of clozapine-n-oxide: implications for nonhuman primate chemogenetics. ACS Chem Neurosci. 2017;8:1570–76.
Mahler SV, Aston-Jones G. CNO Evil? Considerations for the Use of DREADDs in Behavioral Neuroscience. Neuropsychopharmacology. 2018;43:934–36.
Manvich DF, Webster KA, Foster SL, Farrell MS, Ritchie JC, Porter JH, et al. The DREADD agonist clozapine N-oxide (CNO) is reverse-metabolized to clozapine and produces clozapine-like interoceptive stimulus effects in rats and mice. Sci Rep. 2018;8:3840.
Chen X, Choo H, Huang X-P, Yang X, Stone O, Roth BL, et al. The first structure–activity relationship studies for designer receptors exclusively activated by designer drugs. ACS Chem Neurosci. 2015;6:476–84.
Weston M, Kaserer T, Carpenter JC, Snowball A, Knauss S, Lignani G, et al. Olanzapine: a full and potent agonist at the hM4D(Gi) DREADD amenable to clinical translation of chemogenetics. BioRxiv. 2018; https://doi.org/10.1101/477513.
Bonaventura J, Eldridge MAG, Hu F, Gomez JL, Sanchez-Soto M, Abramyan AM, et al. High-potency ligands for DREADD imaging and activation in rodents and monkeys. Nat Commun. 2019;10:4627.
Goutaudier R, Coizet V, Carcenac C, Carnicella S. DREADDs: the power of the lock, the weakness of the key. favoring the pursuit of specific conditions rather than specific ligands. ENeuro. 2019;6:ENEURO.0171-19.2019.
Thompson KJ, Khajehali E, Bradley SJ, Navarrete JS, Huang XP, Slocum S, et al. DREADD agonist 21 is an effective agonist for muscarinic-based DREADDs in vitro and in vivo. ACS Pharmacol Transl Sci. 2018;1:61–72.
Raper J, Murphy L, Richardson R, Romm Z, Kovacs-Balint Z, Payne C, et al. Chemogenetic inhibition of the amygdala modulates emotional behavior expression in infant rhesus monkeys. Eneuro. 2019;6:ENEURO.0360-19.2019.
Nagai Y, Miyakawa N, Takuwa H, Hori Y, Oyama K, Ji B, et al. Deschloroclozapine: a potent and selective chemogenetic actuator enables rapid neuronal and behavioral modulations in mice and monkeys. BioRxiv. 2019. https://doi.org/10.1101/854513.
Casey DE. Serotonergic and dopaminergic aspects of neuroleptic-induced extrapyramidal syndromes in nonhuman primates. Psychopharmacology 1993;112:S55–S59.
Lidow MS, Goldman-Rakic PS. Differential regulation of D2 and D4 dopamine receptor mrnas in the primate cerebral cortex vs. neostriatum: effects of chronic treatment with typical and atypical antipsychotic. Drugs 1997;283:8.
Murphy B. Clozapine reverses the spatial working memory deficits induced by FG7142 in monkeys. Neuropsychopharmacology 1997;16:433–7.
Linn GS, Negi SS, Gerum SV, Javitt DC. Reversal of phencyclidine-induced prepulse inhibition deficits by clozapine in monkeys. Psychopharmacology 2003;169:234–9.
Bachevalier J, Mishkin M. Visual recognition impairment follows ventromedial but not dorsolateral prefrontal lesions in monkeys. Behavioural Brain Res. 1986;20:249–61.
Croxson PL, Kyriazis DA, Baxter MG. Cholinergic modulation of a specific memory function of prefrontal cortex. Nat Neurosci 2011;14:1510–2.
Tauscher J, Hussain T, Agid O, Verhoeff NPLG, Wilson AA, Houle S, et al. Equivalent occupancy of dopamine D1 and D2 receptors with clozapine: differentiation from other atypical antipsychotics. Am J Psychiatry. 2004;161:1620–5.
Zhang H, Wang L, Fan Y, Yang L, Wen X, Liu Y, et al. Atypical antipsychotics for Parkinson’s disease psychosis: a systematic review and meta-analysis. Neuropsychiatr Dis Treat. 2019;15:2137–49.
Wenthur CJ, Lindsley CW. Classics in chemical neuroscience: clozapine. ACS Chem Neurosci. 2013;4:1018–25.
Li P, L. Snyder G, E. Vanover K. Dopamine targeting drugs for the treatment of schizophrenia: past, present and future. Curr Top Medicinal Chem. 2016;16:3385–403.
Bymaster FP, Nelson DL, DeLapp NW, Falcone JF, Eckols K, Truex LL, et al. Antagonism by olanzapine of dopamine D1, serotonin2, muscarinic, histamine H1, and alpha1-adrenergic receptors in vitro. Schizophrenia Res 1999;37:107–22.
Callaghan JT, Bergstrom RF, Ptak LR, Beasley CM. Olanzapine: pharmacokinetic and pharmacodynamic profile. Clin Pharmacokinetics 1999;37:177–93.
R Core Team. R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria; 2018.
Kuznetsova A, Brockhoff P, Christensen R. lmerTest package: tests in linear mixed effects models. J Stat Softw. 2017;82:1–26.
Lenth R emmeans: Estimated Marginal Means, aka Least-Squares Means. 2019.
Hartig F DHARMa: Residual Diagnostics for Hierarchical (Multi-Level/Mixed) Regression Models. 2019.
Goldman-Rakic PS. Cellular basis of working memory. Neuron 1995;14:477–85.
Fuster JM. The prefrontal cortex—an update: time is of the essence. Neuron 2001;30:319–33.
Arnsten AFT, Wang MJ, Paspalas CD. Neuromodulation of thought: flexibilities and vulnerabilities in prefrontal cortical network synapses. Neuron 2012;76:223–39.
Barbey AK, Koenigs M, Grafman J. Dorsolateral prefrontal contributions to human working memory. Cortex 2013;49:1195–205.
Puig MV, Gulledge AT. Serotonin and prefrontal cortex function: neurons, networks, and circuits. Mol Neurobiol 2011;44:449–64.
Ott T, Nieder A. Dopamine D2 receptors enhance population dynamics in primate prefrontal working memory circuits. Cereb Cortex. 2016;27:4423–35.
Sawaguchi T, Goldman-Rakic PS. The role of D1-dopamine receptor in working memory: local injections of dopamine antagonists into the prefrontal cortex of rhesus monkeys performing an oculomotor delayed-response task. J Neurophysiol. 1994;71:515–28.
Ilg A-K, Enkel T, Bartsch D, Bähner F. Behavioral effects of acute systemic low-dose clozapine in wild-type rats: Implications for the use of DREADDs in behavioral neuroscience. Front Behav Neurosci. 2018;12:173.
Vardy E, Robinson JE, Li C, Olsen RHJ, DiBerto JF, Giguere PM, et al. A new DREADD facilitates the multiplexed chemogenetic interrogation of behavior. Neuron 2015;86:936–46.
Magnus CJ, Lee PH, Bonaventura J, Zemla R, Gomez JL, Ramirez MH, et al. Ultrapotent chemogenetics for research and potential clinical applications. Science;2019:15364:pii: eaav5282.
Acknowledgements
We thank Jared Boyce for technical assistance.
Author information
Authors and Affiliations
Contributions
MGB designed the research; NAU performed the research; NAU and MGB analyzed the data; NAU wrote the paper; MGB edited the paper.
Corresponding author
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Upright, N.A., Baxter, M.G. Effect of chemogenetic actuator drugs on prefrontal cortex-dependent working memory in nonhuman primates. Neuropsychopharmacol. 45, 1793–1798 (2020). https://doi.org/10.1038/s41386-020-0660-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41386-020-0660-9