Abstract
According to the adenosine hypothesis of schizophrenia, the classically associated hyperdopaminergic state may be secondary to a loss of function of the adenosinergic system. Such a hypoadenosinergic state might either be due to a reduction of the extracellular levels of adenosine or alterations in the density of adenosine A2A receptors (A2ARs) or their degree of functional heteromerization with dopamine D2 receptors (D2R). In the present study, we provide preclinical and clinical evidences for this latter mechanism. Two animal models for the study of schizophrenia endophenotypes, namely the phencyclidine (PCP) mouse model and the A2AR knockout mice, were used to establish correlations between behavioural and molecular studies. In addition, a new AlphaLISA-based method was implemented to detect native A2AR-D2R heteromers in mouse and human brain. First, we observed a reduction of prepulse inhibition in A2AR knockout mice, similar to that observed in the PCP animal model of sensory gating impairment of schizophrenia, as well as a significant upregulation of striatal D2R without changes in A2AR expression in PCP-treated animals. In addition, PCP-treated animals showed a significant reduction of striatal A2AR-D2R heteromers, as demonstrated by the AlphaLISA-based method. A significant and pronounced reduction of A2AR-D2R heteromers was next demonstrated in postmortem caudate nucleus from schizophrenic subjects, even though both D2R and A2AR were upregulated. Finally, in PCP-treated animals, sub-chronic administration of haloperidol or clozapine counteracted the reduction of striatal A2AR-D2R heteromers. The degree of A2AR-D2R heteromer formation in schizophrenia might constitute a hallmark of the illness, which indeed should be further studied to establish possible correlations with chronic antipsychotic treatments.
Similar content being viewed by others
Introduction
Schizophrenia is a complex psychiatric disorder with a heterogeneous genetic and neurobiological background, which influence early brain development [1]. The most accepted mechanistic hypothesis of schizophrenia is based on a simultaneous deregulation of glutamatergic and dopaminergic systems [1, 2]. In 1967, Van Rossum [3] proposed a dopaminergic basis of schizophrenia, an increase in dopaminergic neurotransmission. Indeed, most individuals with schizophrenia are behaviourally supersensitive to drugs inducing activation of dopamine receptors [4] and the positive symptoms are thought to be associated with hyperactivation of the dopaminergic system. Early work analyzing postmortem brains from patients with schizophrenia revealed a higher striatal density of dopamine D2 receptors (D2Rs) [5]. Recent neuroimaging studies indicate that striatal D2R are augmented by about 5.8 ± 2.7% in schizophrenic subjects [6] and it has been postulated that the D2R population with higher affinity for dopamine are preferentially involved [7], although with some considerations [8]. Thus, a meta-analysis of imaging studies supported the elevation in the D2R availability but gave more significance to a presynaptic component of dopamine release [8]. In agreement with the involvement of dopamine and D2R in schizophrenia, classical antipsychotics such as haloperidol [9] are D2R antagonists or weak partial agonists [10]. However, although efficacious against positive symptoms, haloperidol and related compounds induce severe side effects, including motor impairments [11].
The purinergic system may also be involved in the biology of psychiatric disorders, including schizophrenia [12]. Indeed, the adenosine hypothesis of schizophrenia [13, 14] posits that dysregulation of both glutamatergic and dopaminergic signalling are secondary to a hypoadenosinergic state. The adenosinergic control of the striatal dopaminergic system largely depends on the existence of complexes (i.e., heteromers) formed by adenosine and dopamine receptors, more specifically heteromers of adenosine A2A receptors (A2Rs) and D2R [15]. Accordingly, a hypoadenosinergic state, with a decline in extracellular adenosine concentration or a relative downregulation of A2AR vs. D2R, would reduce the well-established tonic A2AR-mediated inhibition of D2R function in the A2AR–D2R heteromer [15]. It has therefore been postulated that increasing A2AR-mediated allosteric inhibition of D2R within the striatopallidal GABA pathway might represent a promising strategy for schizophrenia management [15,16,17]. In line with this, administration of a selective A2AR agonist effectively antagonized phencyclidine (PCP)-induced locomotor activity in rats [18], an animal model of schizophrenic symptomatology [19]. Similarly, the non-selective adenosine receptor antagonist caffeine has been described to exacerbate psychosis in schizophrenic patients [20].
The present study aimed at exploring potential alterations of A2AR and D2R striatal expression and their degree of heteromerization in mice treated sub-chronically with PCP and in postmortem striatal tissue from schizophrenic subjects, using our recently developed AlphaLISA-based approach [21]. Furthermore, we evaluated whether sub-chronic treatment with the typical antipsychotic haloperidol and the atypical antipsychotic clozapine could modify these alterations in PCP-treated mice.
Methods and materials
Human brain samples
Postmortem human brain samples were obtained at autopsy in the Basque Institute of Legal Medicine, Bilbao, Spain. The study was carried out in compliance with the policies of research and ethical review boards for postmortem brain studies at the moment of sample collection (Basque Institute of Legal Medicine, Bilbao). After a retrospective search for antemortem medical information, ten brain samples of subjects diagnosed with schizophrenia according to DSM-IV, DSM-IV-R or CIE-10 criteria were matched to ten control subjects in a paired design. Mean age, postmortem interval, RNA integrity number, brain pH or tissue storage time did not differ significantly between controls and schizophrenic subjects (Supplementary Table S1). Samples from the caudate nucleus were dissected at autopsy following standard procedures and were immediately stored at −70 °C until assay. For every experimental procedure, each subject ascribed to the schizophrenia group was processed in parallel to a matched control subject.
Animals
A2AR−/− and D2R−/− mice generated on a CD-1 genetic background [22, 23] and the corresponding littermates weighing 20–25 g were used. The animal protocol (#7085) was approved by the University of Barcelona Committee on Animal Use and Care. Animals were housed and tested in compliance with the guidelines provided by the Guide for the Care and Use of Laboratory Animals [24] and following the European Union directives (2010/63/EU). Mice were housed in groups of five in standard cages with ad libitum access to food and water and maintained under a 12 h dark/light cycle (starting at 7:30 a.m.), 22 °C temperature and 66% humidity (standard conditions).
Drug administration
PCP (10 mg/kg, subcutaneously; Tocris, Bristol, UK), haloperidol (0.1 mg/kg, intraperitoneally (i.p.); Tocris) and clozapine (10 mg/kg, i.p.; Tocris) were dissolved in physiological saline (NaCl 0.9%) and administered for 5 consecutive days. At the end of treatment (2–3 h after the final drug administration) animals were used for behavioural assessments and biochemical experiments.
Prepulse inhibition of the acoustic startle response
Mice aged 2–3 months were first handled for 5 days prior to behavioural tests. All the tests were performed during the light phase of the circadian cycle (between 8:30 and 14:00 h) by a researcher blind to drug treatments. At the end of the trial, mice were briefly returned to their home cage before being used in biochemical experiments. Prepulse inhibition (PPI) test was performed using the StartFear System (Panlab, Cornellà de Llobregat, Spain), as described in detailed elsewhere [25] and in the Supplementary Information.
Determination of ribonucleosides and monoamines in mouse striatum
Mice were rapidly killed by cervical dislocation and 400 μm brain coronal sections were obtained in carbogen (95% O2 and 5% CO2) bubbled artificial cerebrospinal fluid buffer (127 mM NaCl, 1 mM KCl, 1.2 mM KH2PO4, 26 mM NaHCO3, 10 mM d-glucose, 2.4 mM CaCl2 and 1.3 mM MgCl2, pH 7.4). Next, the striatum was dissected from the slice and homogenized in 200 μl of acetonitrile (Sigma-Aldrich) containing 2% CH3COOH (Sigma-Aldrich) and dC-d3 (1 ng/µl) at 4 °C in a 1 ml Potter–Elvehjem glass tube using a homogenizer stirrer HS-30E (Witeg Labortechnik GmbH, Wertheim, Germany) with 10 strokes at 700–900 rotations per min. Finally, samples were centrifuged at 13,200 r.p.m. at 4 °C for 20 min and the supernatants were stored at −80 °C until analysis. Quantitative analysis of ribonucleosides (i.e., adenosine, cytidine, guanosine and uridine) and monoamines (i.e., dopamine and serotonin) was carried out by liquid chromatography technique coupled with tandem mass spectrometry and is described in detail in the Supplementary Information.
Immunohistofluorescence analysis
Mice were anaesthetized and perfused intracardially with 100–200 ml ice-cold 4% paraformaldehyde (PFA) in phosphate-buffered saline (PBS; 8.07 mM Na2HPO4, 1.47 mM KH2PO4, 137 mM NaCl, 0.27 mM KCl, pH 7.2). Brains were post-fixed in the same solution of PFA at 4 °C during 12 h. Coronal sections (50 μm) were obtained using a vibratome (Leica Lasertechnik GmbH, Heidelberg, Germany). Slices were collected in Walter’s Antifreezing solution (30% glycerol, 30% ethylene glycol in PBS, pH 7.2) and kept at −20 °C until processing. For immunohistofluorescence analysis, the slices were washed three times with PBS, permeabilized with 0.5% Triton X-100 in PBS for 2 h and rinsed again three times with washing solution (0.05% Triton X-100 in PBS). The slices were then incubated with washing solution containing 10% normal donkey serum (NDS; Jackson ImmunoResearch Laboratories, Inc., West Grove, PA, USA) for 2 h at room temperature. Subsequently, slices were incubated with goat anti-A2AR (3 µg/ml; Santa Cruz Biotechnology, Inc., Dallas, TX, USA), rabbit anti-D2R (3 µg/ml; Frontier Institute Co. Ltd, Hokkaido, Japan) or goat anti-DAT (0.5 µg/ml; Santa Cruz Biotechnology, Inc.) in washing solution containing 10% NDS for 24 h at 4 °C. Next, slices were washed with washing solution containing 1% NDS before the incubation with Cy3-conjugated donkey anti-goat or Cy2-conjugated donkey anti-rabbit IgG antibody (1 : 200; Jackson ImmunoResearch Laboratories, West Grove, PA, USA) in washing solution for 2 h at room temperature. Finally, slices were washed twice with washing solution containing 10% NDS and then mounted with Vectashield immunofluorescence medium (Vector Laboratories, Peterborough, UK) in glass slides. Fluorescence striatal images were captured using a Leica TCS 4D confocal scanning laser microscope (Leica Lasertechnik GmbH).
Gel electrophoresis and immunoblotting
Mouse striatum or frozen human caudate were homogenized in ice-cold 10 mM Tris HCl, pH 7.4, 1 mM EDTA, 300 mM KCl buffer containing a protease inhibitor cocktail (Roche Molecular Systems, USA) using a Polytron for three periods of 10 s each. The homogenate was centrifuged for 10 min at 1000 × g. The resulting supernatant was centrifuged for 30 min at 12,000 × g. The membranes were dispersed in 50 mM Tris HCl (pH 7.4) and 10 mM MgCl2, washed, and resuspended in the same medium as described previously [26]. Protein concentration was determined using the BCA protein assay kit (Thermo Fisher Scientific, Inc., Rockford, IL, USA) and 50–80 μg of protein was used for immunoblotting.
Sodium dodecyl sulfate-polyacrylamide gel electrophoresis was performed using 10% polyacrylamide gels. Proteins were transferred to Hybond®-LFP polyvinylidene difluoride (PVDF) membranes (GE Healthcare, Chicago, IL, USA) using a Trans-Blot® SD Semi-Dry Transfer Cell (Bio-Rad, Hercules, CA, USA). PVDF membranes were blocked with 5% (wt/vol) dry non-fat milk in PBS containing 0.05% Tween-20 (PBS-T) during 45 min and immunoblotted using goat polyclonal anti-A2AR (0.5 μg/ml; Santa Cruz Biotechnology, Inc.), rabbit polyclonal anti-D2R (1 μg/ml; Frontier Institute Co. Ltd), guinea pig polyclonal anti-A2AR (1 μg/ml; Frontier Institute Co. Ltd), goat anti-DAT (0.5 μg/ml; Santa Cruz Biotechnology, Inc.) and rabbit polyclonal anti-α-actinin (0.5 μg/ml; Santa Cruz Biotechnology, Inc.) antibodies in blocking solution overnight at 4 °C. PVDF membranes were washed with PBS-T three times (5 min each) before incubation with either a horseradish peroxidase (HRP)-conjugated goat anti-rabbit IgG (1/30,000; Pierce Biotechnology, Rockford, IL, USA), HRP-conjugated rabbit anti-goat IgG (1/10,000; Pierce Biotechnology) or HRP-conjugated rabbit anti-guinea pig IgG (1/3,000; Pierce Biotechnology) in blocking solution at 20 °C during 2 h. After washing the PVDF membranes with PBS-T three times (5 min each), the immunoreactive bands were developed using a chemiluminescent detection kit (Thermo Fisher Scientific, Waltham, MA, USA) and were detected with an Amersham Imager 600 (GE Healthcare Europe GmbH, Barcelona, Spain).
AlphaLISA method
Mouse striatal and human caudate membranes were homogenized in AlphaLISA buffer (AlphaLISA HiBlock Buffer, PerkinElmer, Waltham, MA, EEUU) and protein concentration determined. Thus, 5 μg of protein/well was placed in white 384 well-plates (384 Well Small Volume™ HiBase Microplates, Greiner Bio-one, Kremsmünster, Austria). Subsequently, membranes were incubated with 5 μl of 10 nM donor primary antibody plus 5 μl of 10 nM acceptor primary antibody (rabbit anti-D2R and guinea pig anti-A2AR, respectively) overnight at 4 °C. As a negative control, samples were also incubated in the absence of either the acceptor or donor primary antibody (Supplementary Fig. S1a). In addition, striatal membranes from A2AR−/− and D2R−/− mice were used negative controls to further validate the new AlphaLISA method implemented here for the detection of A2AR–D2R heteromers in native tissue (Supplementary Fig. S1b). All reagents were mixed by pipetting up and down before incubation. After the overnight incubation, plates were tempered at 22 °C before acceptor beads were added. Anti-guinea pig conjugated acceptor beads were generated by covalent binding of AffiniPure F(ab’)2 Fragment Donkey Anti-Guinea Pig IgG (H + L) (Jackson ImmunoResearch Laboratories, Inc., West Grove, PA, USA) to acceptor beads (AlphaLisa acceptor beads, 6772001; PerkinElmer) following the manufacturer’s instructions. Subsequently, acceptor beads were diluted in AlphaLISA buffer and 5 μL added to each well (final concentration 40 μg/mL). The reagents were mixed by pipetting. After 1 h incubation (in darkness at 22 °C), donor beads (anti-rabbit IgG AlphaLISA Donor beads, AS105D, PerkinElmer) were diluted in AlphaLISA buffer and 5 μL of diluted beads added to each well (final concentration 10 μg/mL). The final reaction volume was 30 μL. The reagents were mixed by pipetting. Finally, after 24 h incubation (in darkness at 4 °C), the microplate was read using a CLARIOstar plate-reader (BMG Labtech, Durham, NC, USA). The plate was left in the dark at room temperature and read again at 48 h. A background signal (B) was determined in wells where all reagents were added without sample. For each membrane brain sample a negative control (Cn) was determined by incubating in the absence of acceptor primary antibody (i.e., guinea pig anti-A2AR antibody). Therefore, for each sample the specific AlphaLISA signal (i.e., ∆AlphaLISA) was calculated as follows:
Statistics
Data are represented as mean ± SEM. The number of samples/animals (n) in each experimental condition is indicated in the corresponding figure legend. Data normality was assessed by the Shapiro–Wilk normality test. Outliers were assessed by the Grubbs’ test; thus, data from any animal found to be an outlier was excluded. Comparisons among experimental groups were performed by Student’s t-test, one-way analysis of variance (ANOVA) with Dunnett’s post hoc test or two-way ANOVA with Sidak’s post hoc test using GraphPad Prism 6.01 (San Diego, CA, USA), as indicated. Statistical difference was accepted when P < 0.05.
Results
Alterations in sensorimotor gating in PCP-treated animals and in mice lacking A2AR
The adenosine hypothesis of schizophrenia [13, 14] was recently bolstered by the observation that A2AR deletion (A2AR−/−) prompts behaviours that mimic symptoms of psychosis and molecular/anatomical alterations in mice, resembling the relevant phenotype features of the human disorder [23, 27, 28]. We first validated the A2AR−/−-based animal model of psychotic symptoms by comparing it with the well-established PCP animal model of sensory gating impairment of schizophrenia [19, 29, 30]. A2AR−/− and A2AR+/+ saline- and PCP-treated mice were evaluated with the PPI test, a classically accepted behavioural assessment of sensorimotor processing altered in schizophrenic patients and in PCP-treated rodents [19, 29]. As previously reported [23, 28], A2AR−/− mice showed a significant reduction in basal PPI at 70 dB (P = 0.0156), 75 dB (P = 0.0023) and 80 dB (P = 0.0001) (Fig. 1). PCP administration to A2AR+/+ mice also induced a significant PPI reduction, up to half of basal values, at 70 dB (P = 0.0068), 75 dB (P = 0.0025) and 80 dB (P = 0.0119) (Fig. 1). These results demonstrated that sensorimotor processing alterations in A2AR−/− mice were comparable to those observed in PCP-treated wild-type (WT) animals.
The prepulse inhibition (PPI) impairment of the acoustic startle response (ASR) was assessed and expressed as percentage mean ± SEM (n = 10–15 animals) of inhibition of ASR at the indicated prepulse acoustic stimulus amplitudes (i.e., 70, 75 and 80 dB). *P < 0.05, **P < 0.01 and ***P < 0.001, one-way ANOVA followed by Dunnett’s post hoc test compared with WT (A2AR+/+) group. Two-way ANOVA (PP × phenotype/PCP) revealed a significant main effect of phenotype/PCP (F(2,117) = 22.65, P < 0.0001) and a nonsignificant effect of PP (F(2,117) = 2.616, P = 0.0774) or the interaction between both factors (F(4,117) = 0.5762, P = 0.6804).
Striatal A2AR and D2R expression profiles in A2AR−/− and PCP-treated mice
Next, we aimed at determining possible alterations in striatal A2AR content in the PCP animal model, as well as possible alterations in striatal D2R densities in PCP-treated and in A2AR−/− mice groups, by performing immunoblotting and immunocytochemistry experiments. First, we assessed A2AR and D2R expression by immunoblot analysis. A2AR and D2R expression was ascertained by the presence of protein bands of molecular weight ~45 kDa and ~70–80 kDa, respectively (Fig. 2a, d), which were absent in A2AR- and D2R-knockout mice samples as previously demonstrated [23] In addition, we assessed the dopamine transporter (DAT), as alterations in DAT expression have been recently described in another rodent model of psychosis [31]. Importantly, although A2AR and DAT expression were not altered in the striatum of PCP-treated animals, the expression of D2R was significantly increased (P = 0.0006) (Fig. 2a, b). Immunohistofluorescence analysis of A2AR, D2R and DAT in coronal slices at the level of the anterior commissure from PCP-treated mice also revealed higher D2R immunoreactivity in the striatum (Fig. 2c). Overall, these results indicate that PCP treatment raised D2R expression in the striatum, while A2AR and DAT were unaffected.
a, d Representative immunoblots showing the expression of A2AR, D2R and DAT in striatal membranes from saline and PCP-treated mice (a) and striatal membranes from WT (A2AR+/+) and A2AR−/− mice (d); striatal membranes were analyzed by SDS-PAGE (50 μg of protein/lane) and immunoblotted using goat anti-A2AR, rabbit anti-D2R, goat anti-DAT and rabbit anti-α-actinin antibodies (see Methods). b, e) Relative quantification of A2AR, D2R and DAT expression. The immunoblot protein bands corresponding to A2AR, D2R, DAT and α-actinin from saline and PCP-treated mice (b; n = 6–9) and from WT and A2AR−/− mice (e; n = 5–7) were quantified by densitometric scanning; values were normalized to the respective amount of α-actinin in each lane to correct for protein loading; results are expressed as percentage (mean ± SEM) of the corresponding saline-treated or WT animals; *P < 0.05, **P < 0.01 and ***P < 0.001 two-way ANOVA with Sidak’s post hoc test. c, f Representative images of A2AR, D2R and DAT immunoreactivities in the dorsal striatum of saline and PCP-treated mice (c) or WT and A2AR−/− mice (f); scale bar: 350 μm. Cx, cortex; St, striatum.
Subsequently, we analyzed A2AR, D2R and DAT expression in WT and A2AR−/− mice. Similar to what was observed in PCP-treated mice, immunoblotting analysis revealed that deletion of A2AR induced a significative increase in D2R (P = 0.0433) but also in DAT (P = 0.0014) expression in the striatum (Fig. 2d, e). As expected, A2AR expression was abolished in A2AR−/− (Fig. 2d, e). In addition, immunohistofluorescence detection of A2AR, D2R and DAT in WT mice also revealed increased D2R and DAT immunoreactivity in the striatum (Fig. 2f). As expected, A2AR immunoreactivity could not be detected in A2AR−/− mice (Fig. 2f). Collectively, these results indicate that the expression of D2R in the striatum of A2AR−/− mice is increased, similar to what was observed in the PCP-based animal model of schizophrenic symptomatology.
Striatal levels of ribonucleosides and monoamines in A2AR−/− and PCP-treated mice
To determine a possible presynaptic imbalance, striatal levels of adenosine and dopamine were determined in A2AR+/+, A2AR−/− and PCP-treated mice. The levels of the ribonucleosides cytidine, guanosine and uridine, and the monoamine serotonin were also determined (Supplementary Table S2). Interestingly, although the levels of dopamine and serotonin were not altered in A2AR−/− or in PCP-treated animals, the amounts of adenosine and cytidine were significantly increased in A2AR−/− mice (Supplementary Table S2). Also, the levels of uridine were significantly raised both in A2AR−/− and PCP-treated animals (Supplementary Table S2). These results indicate that purine metabolism is altered in the A2AR−/− mouse model, which displays a striatal neurochemical pattern different from that observed in the PCP model of schizophrenic symptomatology. Altogether, the results (i.e., density of striatal A2AR and D2R, and neurotransmitter levels) obtained from PCP-treated and A2AR−/− mouse models do not support a presynaptic adenosine–dopamine imbalance, but rather support a postsynaptic A2AR–D2R density imbalance in schizophrenia.
A2AR, D2R and DAT expression profiles in the caudate nucleus from postmortem schizophrenic subjects
As mentioned in the introductory section, previous postmortem and imaging studies suggested the presence of an increased D2R expression in the striatum of schizophrenic subjects [5, 6]. Conversely, the results with DAT and A2AR are inconsistent. A recent meta-analysis indicates that there is a significantly greater interindividual variability of striatal DAT availability in patients with schizophrenia, compared to control subjects. These data suggest that altered DAT expression may occur only in a group of patients [32]. Inconsistent results have also been obtained in relation to striatal A2AR expression in schizophrenia, with reports of either upregulation or downregulation [33, 34]. Therefore, we aimed at determining whether the relative expression of D2R, A2AR and DAT were altered in postmortem caudate from a group of schizophrenic subjects (Supplementary Table S1). From immunoblot analysis of postmortem caudate nucleus membranes obtained from a cohort of ten healthy controls and ten subjects diagnosed with paranoid schizophrenia (Supplementary Table S1), we found that D2R, DAT and A2AR expression was significantly (P < 0.05) increased in the caudate nucleus from subjects with schizophrenia (Fig. 3a, b).
a Representative immunoblot showing the expression of A2AR, D2R and DAT in postmortem caudate membranes from healthy control (HC) and schizophrenic (SCZ) subjects; membranes from human postmortem caudate were analyzed by SDS-PAGE (50 μg of protein/lane) and immunoblotted using goat anti-A2AR, rabbit anti-D2R, goat anti-DAT and rabbit anti-α-actinin antibodies (see ‘Methods’). b Relative quantification of A2AR, D2R and DAT expression; the immunoblot protein bands corresponding to A2AR, D2R, DAT and α-actinin from healthy control (n = 10) and schizophrenic (n = 10) individuals were quantified by densitometric scanning; values were normalized to the respective amount of α-actinin in each lane to correct for protein loading. Results are expressed as percentage (mean ± SEM) of the control. *P < 0.05, **P < 0.01, two-way ANOVA with Sidak’s post hoc test.
Decrease in A2AR–D2R heteromerization in the caudate nucleus of schizophrenic subjects and the striatum of PCP-treated mice
We next interrogated whether the postulated hypoadenosinergic state in schizophrenia could be dependent on a significant change in the interactions between A2AR and D2R, i.e., in their well-established ability to form functional heteromers [15]. To this end, we used our recently engineered AlphaLISA-based method to assess A2AR–D2R interactions in human postmortem brain [21] (Fig. 4a). The AlphaLISA approach revealed a strong and specific energy transfer between the donor and acceptor beads coupled to specific receptor antibodies (Supplementary Fig. 1). This energy transfer confirmed that the intermolecular interaction between A2AR and D2R, i.e., A2AR–D2R heteromers, can be detected in postmortem membrane extracts (Fig. 4b), as recently reported [21]. A significant and pronounced reduction of 59 ± 11% (P = 0.0076) in A2AR–D2R heteromerization was observed in the human caudate membrane extracts from schizophrenic subjects as compared to controls (Fig. 4b, right panel). Similarly, when striatal membrane extracts from PCP-treated animals were assessed, a comparable significant reduction of 75 ± 7% (P = 0.0001) in A2AR–D2R heteromerization was detected as compared to controls (Fig. 4b, left panel). Overall, these results indicate that striatal A2AR–D2R heteromerization was reduced both in schizophrenic subjects and in the PCP-based animal model of schizophrenic symptoms, thus predicting a role for alterations in the formation of the striatal A2AR–D2R heteromers in the pathophysiology of schizophrenia.
a Illustration of the specific AlphaLISA protein–protein interaction assay designed for A2AR–D2R heteromer identification and quantification in native tissue; anti-guinea pig-coated acceptor beads (red sphere) were generated to capture a guinea pig anti-A2AR antibodies bound to the receptors within the membrane extract; anti-rabbit coated donor beads (blue sphere) capture the immune complexes between the rabbit anti-D2R antibodies and the receptors within the membrane extract; A2AR–D2R heteromerization brings donor beads into close proximity (<200 nm) to the acceptor beads. The excitation of the donor beads at 680 nm generates singlet oxygen (1O2) molecules triggering a chemical reaction within the acceptor beads, which results in a sharp peak of fluorescent emission at 615 nm (figure designed using image templates from Servier Medical Art https://smart.servier.com/image-set-download/). b The A2AR–D2R interaction capacity in membranes from saline- (n = 10) and PCP- (n = 10) treated mouse striatum (left panel) or from postmortem control (n = 10) and schizophrenic (n = 10; SCZ) caudate (right panel) was determined by AlphaLISA method (see ‘Methods’); the specific AlphaLISA signal (i.e., ∆AlphaLISA) was calculated as described in the ‘Methods’ section and expressed as percentage (mean ± SEM) of either the saline-treated mice or control subjects. **P < 0.01 and ***P < 0.001, Student’s t-test.
Counteracting effects of sub-chronic antipsychotic treatment on PCP-induced reduction of A2AR–D2R heteromerization
In view that schizophrenic patients showed a reduced A2AR–D2R heteromer formation, we next aimed at determining whether antipsychotic medications may prevent PCP-mediated A2AR–D2R heteromer downregulation in mice. Interestingly, previous preclinical experiments evaluating the effects of neuroleptics on A2AR–D2R interactions found that chronic haloperidol treatment induced an increase in functional A2AR–D2R interactions. More specifically, chronic treatment with haloperidol (administered in drinking water for 30 consecutive days, adjusted to 1.5 mg/kg) in rats led to an increased potency of A2AR agonists in reducing the affinity of D2R agonists in striatal membrane preparations and to an increase in the locomotor-activating effects of the adenosine receptor antagonist theophylline [35]. However, we could not evaluate a possible effect of antipsychotics on striatal A2AR–D2R heteromerization in our cohort sample, since it was limited to ten subjects with paranoid schizophrenia treated with different compounds (Supplementary Table S1). Therefore, we aimed at ascertaining the impact of neuroleptic treatment on A2AR–D2R heteromer formation in PCP-treated mice. We evaluated the possible modification of striatal A2AR–D2R heteromerization upon administration of haloperidol or clozapine in mice repeatedly administered with PCP. We could first confirm that sub-chronic treatment with haloperidol or clozapine did not modify PPI in control mice. Conversely, they both counteracted PCP-induced disruption of PPI (Fig. 5a). On the other hand, the AlphaLISA approach revealed that neither haloperidol nor clozapine modified A2AR–D2R heteromerization in control mice but prevented the reduction of A2AR–D2R heteromerization in PCP-treated animals (Fig. 5b). Finally, when the density of striatal A2AR and D2R was assessed by immunoblotting, we confirmed that PCP produced a significant increase in the density of D2R (Fig. 5c, d). This effect was not modified by haloperidol or clozapine treatment (Fig. 5c, d). Similarly, in the absence of PCP, neither haloperidol nor clozapine treatment significantly modified A2AR and D2R densities (Fig. 5c, d). These results imply that sub-chronic treatment with haloperidol or clozapine does not lead to an increase in A2AR–D2R heteromerization in healthy subjects. However, antipsychotics are able to reverse PCP-induced reduction in striatal A2AR–D2R heteromerization and, as previously reported [36], PCP-induced disruption of PPI.
a PPI impairment in saline- (n = 10) and PCP-treated animals (n = 10) with or without chronic treatment with haloperidol (Halo, 0.1 mg/kg/day for 5 days) or clozapine (Clz, 10 mg/kg/day for 5 days); results are expressed as percentage (mean ± SEM) of inhibition of ASR at the 75 dB amplitude prepulse acoustic stimulus; * P < 0.05, one-way ANOVA followed by Dunnett’s post hoc test compared to saline-treated mice. b A2AR–D2R heteromerization in striatal membranes from the same animals shown in a determined by AlphaLISA method (see ‘Methods’); the specific AlphaLISA signal (i.e., ∆AlphaLISA) was calculated as described in the ‘Methods’ section and expressed as percentage (mean ± SEM) of the saline-treated mice. *P < 0.05 one-way ANOVA with Dunnett’s post hoc test when compared to saline-treated mice. c Representative immunoblot showing the expression of A2AR, D2R and DAT in striatal membranes from animals from the same groups shown in a; striatal membranes from PCP-treated mice were analyzed by SDS-PAGE (50 μg of protein/lane) and immunoblotted using guinea pig anti-A2AR, rabbit anti-D2R, goat anti-DAT and rabbit anti-α-actinin antibodies (see ‘Methods’). d Relative quantification of A2AR, D2R and DAT expression; the immunoblot protein bands corresponding to A2AR, D2R, DAT and α-actinin from the same animals shown in a were quantified by densitometric scanning; values were normalized by the respective amount α-actinin in each lane to correct for protein loading. Results are expressed as percentage (mean ± SEM) of the corresponding saline-treated animal; ***P < 0.001, two-way ANOVA with Sidak’s post hoc test.
Discussion
Targeting D2R-containing heteromers (i.e., A2AR–D2R) represents a new strategy for psychosis management [16]. Our results indicate that the presence of sensitized D2R in schizophrenia may be concomitant to a reduction in A2AR activity secondary to a deficiency in A2AR–D2R heteromer formation. Indeed, we observed a reduction of PPI in A2AR−/− mice, similar to the PPI deficits in PCP-treated mice. In addition, these animals showed a significant upregulation of striatal D2R without concomitant changes in the expression of A2AR (a relative downregulation of A2AR vs. D2R). More importantly, we could establish a correlation between striatal A2AR–D2R heteromer downregulation and PCP-induced sensory gating impairment in mice. Finally, in schizophrenic subjects, A2AR–D2R heteromers were also reduced, even though the expression of both A2AR and D2R was increased.
Apart from the already supported antipsychotic potential for A2AR agonists [18], drugs promoting A2AR–D2R heteromer formation might constitute an alternative strategy for the treatment of schizophrenia. In fact, we could demonstrate that, in the PCP animal model of schizophrenic symptomatology, sub-chronic treatment with either the typical antipsychotic, haloperidol, or the atypical antipsychotic, clozapine, counteracted PCP-induced PPI disruption and PCP-induced reduction in striatal A2AR–D2R heteromerization. Conversely, antipsychotics did not change the degree of A2AR–D2R heteromerization in control animals, without PCP treatment. A more sustained treatment with antipsychotics could therefore lead to further increase in striatal A2AR–D2R heteromerization, as suggested from previous experiments in rats chronically treated with haloperidol [35]. Upregulation of striatal A2AR–D2R heteromers could therefore represent a protective mechanism associated with chronic neuroleptic treatment.
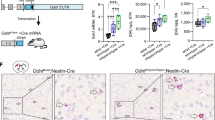
Schizophrenia has a strong heritable component and some genetic risk factors have been already established. Accordingly, genetic animal models are important tools to study the mechanisms underlying this disease. Based on the evidence that striatal D2R are upregulated in schizophrenic patients [6], an animal model of schizophrenia based on D2R overexpression in the striatum (i.e., D2R-OE mice) was created using an artificial transcription factor system [37]. However, although D2R-OE mice showed deficits in working memory tasks and behavioural flexibility, they did not present deficits in PPI [37]. Several gene knockouts, including those of the metabotropic glutamate mGlu2 and mGlu3 receptors, PSD95 (postsynaptic density protein 95), GPRK6 (G-protein receptor kinase 6), the Trace Amine-1 receptor, and RGS9-2 (regulator of G-protein signalling 9-2), have also been proposed as animal model of psychosis, which may represent different aspects of the disease [38, 39]. Our results support the validity of a novel genetic model; A2AR−/− mice. Thus, similar to what is observed in the widely used PCP animal model schizophrenic symptomatology, A2AR−/− mice display PPI deficits and increased striatal D2R and DAT densities.
Altogether, the results of the present study provide strong support to the adenosine hypothesis of schizophrenia [13, 14]. However, rather than pointing to adenosine itself, our data highlight A2ARs and their fundamental role in controlling striatal D2R function [15, 16, 40]. Overall, apart from presynaptic mechanisms [8, 32], the pathophysiology of schizophrenia seems to involve postsynaptic mechanisms which, rather than be related to D2R upregulation, it involves the loss of the control of D2R by A2AR in the striatum. Changes in the density of striatal A2AR-D2R heteromers should then be expected to contribute to the changes observed in positron emission tomography (PET) imaging studies that use D2R ligands in patients with schizophrenia. Those changes would then depend on the complex allosteric interactions between A2AR and D2R agonists and antagonists that occur in the A2AR–D2R heteromer, where any orthosteric A2AR ligand, agonist or antagonist, exerts a negative allosteric modulation on the affinity of any orthosteric D2R ligand, agonist or antagonist [41]. Those allosteric interactions provided a plausible mechanism for the reported increase of [11C]raclopride binding in humans induced by caffeine [42], due to a its ability to antagonize the effect of endogenous adenosine on the binding of the exogenous D2R antagonist [41]. It can thus be predicted that a decrease in A2AR–D2R heteromerization should lead to a reduced effect of endogenous adenosine on exogenous antagonist binding, which might be mainly responsible for the increased striatal D2R antagonist binding of schizophrenic patients.
Funding and disclosure
This work was supported by FEDER/Ministerio de Ciencia, Innovación y Universidades–Agencia Estatal de Investigación (SAF2017-87349-R and MDM-2017-0729) and ISCIII (PIE14/00034), the Catalan government (2017 SGR 1604), Fundació la Marató de TV3 (Grant 20152031), FWO (SBO-140028) to FC, the Basque Government (IT616/13 and IT-1211-19) and the intramural funds of the National Institute on Drug Addiction. The authors declare no conflict of interest.
References
Kahn RS, Sommer IE, Murray RM, Meyer-Lindenberg A, Weinberger DR, Cannon TD, et al. Schizophrenia. Nat Rev Dis Prim. 2015;1:15067.
Freedman R. Schizophrenia. N. Engl J Med. 2003;349:1738–49.
Van Rossum JM. The significance ofdopamine-receptor blockade for the action of neuro-leptic drugs. In: Brill H, Cole J, Deniker P, Hippius H, Bradley P, editors. Neuro-Psycho-Pharmacology, Proceedings of the Fifth International Congress of the Collegium Internationale Neuro-Psycho-pharmacologicum, Washington, March, 1966., Amsterdam: Excerpta Medica Foundation; 1967. p. 321–329.
Lieberman JA, Kane JM, Alvir J. Provocative tests with psychostimulant drugs in schizophrenia. Psychopharmacology. 1987;91:415–33.
Seeman P, Bzowej NH, Guan HC, Bergeron C, Reynolds GP, Bird ED, et al. Human brain D1 and D2 dopamine receptors in schizophrenia, Alzheimer’s, Parkinson’s, and Huntington’s diseases. Neuropsychopharmacology. 1987;1:5–15.
Seeman P. Schizophrenia and dopamine receptors. Eur Neuropsychopharmacol. 2013;23:999–1009.
Seeman P. Are dopamine D2 receptors out of control in psychosis? Prog Neuro-Psychopharmacol Biol Psychiatry. 2013;46:146–52.
Howes OD, Kambeitz J, Kim E, Stahl D, Slifstein M, Abi-Dargham A, et al. The nature of dopamine dysfunction in schizophrenia and what this means for treatment: Meta-analysisof imaging studies. Arch Gen Psychiatry. 2012;69:776–86.
Granger B, Albu S. The haloperidol story. Ann Clin Psychiatry. 2005;17:137–40.
Seeman P. Targeting the dopamine D2 receptor in schizophrenia. Expert Opin Ther Targets. 2006;10:515–31.
Miyamoto S, Miyake N, Jarskog LF, Fleischhacker WW, Lieberman JA. Pharmacological treatment of schizophrenia: a critical review of the pharmacology and clinical effects of current and future therapeutic agents. Mol Psychiatry. 2012;17:1206–27.
Cheffer A, Castillo ARG, Corrêa-Velloso J, Gonçalves MCB, Naaldijk Y, Nascimento IC, et al. Purinergic system in psychiatric diseases. Mol Psychiatry. 2018;23:94–106.
Lara DR, Souza DO. Schizophrenia: a purinergic hypothesis. Med Hypotheses. 2000;54:157–66.
Boison D, Singer P, Shen HY, Feldon J, Yee BK. Adenosine hypothesis of schizophrenia - opportunities for pharmacotherapy. Neuropharmacology. 2012;62:1527–43.
Ferré S, Bonaventura J, Zhu W, Hatcher-Solis C, Taura J, Quiroz C, et al. Essential control of the function of the striatopallidal neuron by pre-coupled complexes of adenosine A2A-dopamine D2 receptor heterotetramers and adenylyl cyclase. Front Pharmacol. 2018;9:243.
Ferré S. Adenosine-dopamine interactions in the ventral striatum. Implications for the treatment of schizophrenia. Psychopharmacology. 1997;133:107–20.
Domenici MR, Ferrante A, Martire A, Chiodi V, Pepponi R, Tebano MT, et al. Adenosine A2A receptor as potential therapeutic target in neuropsychiatric disorders. Pharmacol Res. 2019;147:104338.
Rimondini R, Ferre S, Ogren SO, Fuxe K. Adenosine A2A agonists: a potential new type of atypical antipsychotic. Neuropsychopharmacology. 1997;17:82–91.
Jentsch JD, Roth RH. The neuropsychopharmacology of phencyclidine: from NMDA receptor hypofunction to the dopamine hypothesis of schizophrenia. Neuropsychopharmacology. 1999;20:201–25.
Wang HR, Woo YS, Bahk W-M. Caffeine-induced psychiatric manifestations. Int Clin Psychopharmacol. 2015;30:179–82.
Fernández-Dueñas V, Gómez-Soler M, Valle-León M, Watanabe M, Ferrer I, Ciruela F. Revealing adenosine A2A-dopamine D2 receptor heteromers in Parkinson’s disease post-mortem brain through a new AlphaScreen-based assay. Int J Mol Sci. 2019;20:3600.
Ledent C, Vaugeois JM, Schiffmann SN, Pedrazzini T, El Yacoubi M, Vanderhaeghen JJ, et al. Aggressiveness, hypoalgesia and high blood pressure in mice lacking the adenosine A2a receptor. Nature. 1997;388:674–8.
Taura J, Valle-León M, Sahlholm K, Watanabe M, Van Craenenbroeck K, Fernández-Dueñas V, et al. Behavioral control by striatal adenosine A2A-dopamine D2 receptor heteromers. Genes Brain Behav. 2018;17:e12432.
Clark JD, Gebhart GF, Gonder JC, Keeling ME, Kohn DF. Special report: the 1996 guide for the care and use of laboratory animals. ILAR J. 1997;38:41–48.
Moscoso-Castro M, Gracia-Rubio I, Ciruela F, Valverde O. Genetic blockade of adenosine A2A receptors induces cognitive impairments and anatomical changes related to psychotic symptoms in mice. Eur Neuropsychopharmacol. 2016;26:1227–40.
Andrés-Benito P, Fernández-Dueñas V, Carmona M, Escobar LA, Torrejón-Escribano B, Aso E, et al. Locus coeruleus at asymptomatic early and middle Braak stages of neurofibrillary tangle pathology. Neuropathol Appl Neurobiol. 2017;43:373–92.
Moscoso-Castro M, López-Cano M, Gracia-Rubio I, Ciruela F, Valverde O. Cognitive impairments associated with alterations in synaptic proteins induced by the genetic loss of adenosine A 2A receptors in mice. Neuropharmacology. 2017;126:48–57.
Wang JH, Short J, Ledent C, Lawrence AJ, van den Buuse M. Reduced startle habituation and prepulse inhibition in mice lacking the adenosine A2A receptor. Behavioural Brain Res. 2003;143:201–7.
Castañé A, Santana N, Artigas F. PCP-based mice models of schizophrenia: differential behavioral, neurochemical and cellular effects of acute and subchronic treatments. Psychopharmacology. 2015;232:4085–97.
Jones C, Watson D, Fone K. Animal models of schizophrenia. Br J Pharmacol. 2011;164:1162–94.
Dahoun T, Trossbach SV, Brandon NJ, Korth C, Howes OD. The impact of Disrupted-in-Schizophrenia 1 (DISC1) on the dopaminergic system: a systematic review. Transl Psychiatry. 2017;7:e1015–1015.
Brugger SP, Angelescu I, Abi-Dargham A, Mizrahi R, Shahrezaei V, Howes OD. Heterogeneity of striatal dopamine function in schizophrenia: meta-analysis of variance. Biol Psychiatry. 2019. https://doi.org/10.1016/j.biopsych.2019.07.008.
Deckert J, Brenner M, Durany N, Zöchling R, Paulus W, Ransmayr G, et al. Up-regulation of striatal adenosine A(2A) receptors in schizophrenia. Neuroreport. 2003;14:313–6.
Villar-Menéndez I, Díaz-Sánchez S, Blanch M, Albasanz JL, Pereira-Veiga T, Monje A, et al. Reduced striatal adenosine A2A receptor levels define a molecular subgroup in schizophrenia. J Psychiatr Res. 2014;51:49–59.
Ferré S, Schwarcz R, Li XM, Snaprud P, Ögren SO, Fuxe K. Chronic haloperidol treatment leads to an increase in the intramembrane interaction between adenosine A2 and dopamine D2 receptors in the neostriatum. Psychopharmacology. 1994;116:279–84.
Martinez ZA, Oostwegel J, Geyer MA, Ellison GD, Swerdlow NR. ‘Early’ and ‘late’ effects of sustained haloperidol on apomorphine- and phencyclidine-induced sensorimotor gating deficits. Neuropsychopharmacology. 2000;23:517–27.
Kellendonk C, Simpson EH, Polan HJ, Malleret G, Vronskaya S, Winiger V, et al. Transient and selective overexpression of dopamine D2 receptors in the striatum causes persistent abnormalities in prefrontal cortex functioning. Neuron. 2006;49:603–15.
Simpson EH, Kellendonk C. Insights about striatal circuit function and schizophrenia from a mouse model of dopamine D2 receptor upregulation. Biol Psychiatry. 2017;81:21–30.
Seeman P. All roads to schizophrenia lead to dopamine supersensitivity and elevated dopamine D2(high) receptors. CNS Neurosci Ther. 2011;17:118–32.
Ferré S, O’Connor WT, Snaprud P, Ungerstedt U, Fuxe K. Antagonistic interaction between adenosine A2A receptors and dopamine D2 receptors in the ventral striopallidal system. Implications for the treatment of schizophrenia. Neuroscience. 1994;63:765–73.
Bonaventura J, Navarro G, Casadó-Anguera V, Azdad K, Rea W, Moreno E, et al. Allosteric interactions between agonists and antagonists within the adenosine A2A receptor-dopamine D2 receptor heterotetramer. Proc Natl Acad Sci USA. 2015;112:E3609–18.
Volkow ND, Wang GJ, Logan J, Alexoff D, Fowler JS, Thanos PK, et al. Caffeine increases striatal dopamine D2/D3 receptor availability in the human brain. Transl Psychiatry. 2015;5:e549.
Acknowledgements
We thank Centres de Recerca de Catalunya (CERCA) Programme/Generalitat de Catalunya for IDIBELL institutional support. We thank Esther Castaño and Benjamín Torrejón from the Scientific and Technical Services (SCT) group at the Bellvitge Campus of the University of Barcelona for their technical assistance.
Author information
Authors and Affiliations
Contributions
Substantial contributions to the conception or design of the work (all authors), or the acquisition (MV-L, MMC-M and C.S.), analysis (MV-L, LFC and ML-C), or interpretation of data for the work (LFC and KS). Drafting the work or revising it critically for important intellectual content (all authors). Final approval of the version to be published (all authors). Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved (all authors).
Corresponding authors
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, and provide a link to the Creative Commons license. You do not have permission under this license to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Valle-León, M., Callado, L.F., Aso, E. et al. Decreased striatal adenosine A2A-dopamine D2 receptor heteromerization in schizophrenia. Neuropsychopharmacol. 46, 665–672 (2021). https://doi.org/10.1038/s41386-020-00872-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41386-020-00872-9
This article is cited by
-
Reinstatement of nicotine conditioned place preference in a transgenerational model of drug abuse vulnerability in psychosis: Impact of BDNF on the saliency of drug associations
Psychopharmacology (2023)
-
Adenosine A2A receptor in schizophrenia: an in vivo brain PET imaging study
Psychopharmacology (2022)
-
Chemical biology-based approaches to study adenosine A2A − dopamine D2 receptor heteromers
Purinergic Signalling (2022)