Abstract
Food-triggered anaphylaxis can encompass a variety of systemic and intestinal symptoms. Murine-based and clinical studies have revealed a role for histamine and H1R and H2R-pathway in the systemic response; however, the molecular processes that regulate the gastrointestinal (GI) response are not as well defined. In the present study, by utilizing an IgE-mast cell (MC)-dependent experimental model of oral antigen-induced anaphylaxis, we define the intestinal epithelial response during a food-induced anaphylactic reaction. We show that oral allergen-challenge stimulates a rapid dysregulation of intestinal epithelial transcellular and paracellular transport that was associated with the development of secretory diarrhea. Allergen-challenge induced (1) a rapid intestinal epithelial Cftr-dependent Cl− secretory response and (2) paracellular macromolecular leak that was associated with modification in epithelial intercellular junction proteins claudin-1, 2, 3 and 5, E-cadherin and desmosomal cadherins. OVA-induced Cftr-dependent Cl− secretion and junctional protein degradation was rapid occurring and was sustained for 72 h following allergen-challenge. Blockade of both the proteolytic activity and Cl− secretory response was required to alleviate intestinal symptoms of food-induced anaphylaxis. Collectively, these data suggest that the GI symptom of food-induced anaphylactic reaction, secretory diarrhea, is a consequence of CFTR-dependent Cl− secretion and proteolytic activity.
Similar content being viewed by others
Introduction
Severe food allergy-related reactions, termed food-triggered anaphylaxis, are serious life threatening reactions responsible for 30,000–120,000 emergency department visits, 2000–3000 hospitalizations, and ~150 deaths per year in the United States.1,2 The onset of symptoms are variable, occurring within seconds to a few hours following exposure to the casual dietary allergen, and often affects multiple organ systems including gastrointestinal (GI), cutaneous, respiratory, and cardiovascular.3 Cutaneous symptoms (urticaria and angioedema) are the most common, occurring in ~80% of cases and GI symptoms occur in as much as 40% cases, which include cramping, abdominal pain, nausea, emesis and diarrhea.4 Recently, there has been emerging clinical data indicating a link between GI manifestations with the more severe anaphylactic phenotype including hypotension and hypoxia.5,6,7,8,9 Clinical and experimental analyses have identified a central role for IgE/FcεRI cross linking on the surface on mast cells (MC) in promoting the clinical manifestations associated with food-triggered anaphylaxis.10,11,12,13,14,15,16 MCs upon IgE cross linking release an array of preformed mediators including histamine, PAF, serotonin, proteases (tryptase and chymase), and lipid-derived mediators (prostaglandins [PGD2] and leukotrienes [LTC4, LTD4 and LTE4]) which are thought to drive the systemic and GI symptoms.11,12,14,15,17 Genetic or pharmacological blockade of MC activity prevents the GI and systemic involvement in oral antigen-induced anaphylaxis.18,19 Notably, experimental investigations have revealed that histamine via histamine receptor (HR) HR1, HR2 and HR4 signaling drives the systemic manifestations of IgE-mediated anaphylaxis in mice,18,20,21 however, the GI symptoms while MC and IgE-dependent, remain unabated by HR1 and HR2 antagonism18 indicating a role for other MC-derived mediators in the induction of the GI symptoms of oral antigen-induced anaphylaxis.
Herein, we describe the temporal molecular processes associated with GI symptoms of food-induced anaphylaxis in mice. We show that oral antigen-challenge induces a rapid dysregulation of small intestine (SI) transcellular Cftr-dependent Cl− secretion and paracellular macromolecular leak. The paracellular macromolecular flux was linked with modification of transmembrane proteins in the tight junction (claudin-1,2,3,5 and junctional adhesion molecule-A) and epithelial cadherins in the adherens junction (E-cadherin) and desmosomes (DM) (Desmoglein-2 (Dsg-2) and desmocollin-2 (Dsc-2)), and was mediated by IgE/MC activation. We show that GI manifestations such as secretory diarrhea was antigen-induced and persisted for 72 h and was abated by abrogation of proteolytic activity and Cl− secretion. Collectively, these studies suggest that MC-driven proteolytic activity and Cl− secretory response is required for the development of secretory diarrhea response during a food-induced anaphylactic reaction in mice.
Results
Food antigen exposure is restricted to the SI during a food-induced anaphylactic reaction
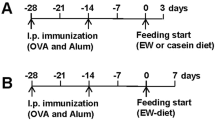
We have previously shown that ovalbumin (OVA)-sensitized mice demonstrate systemic and GI symptoms including diarrhea within 30 min of the 7th oral OVA challenge.22,23 To ascertain the localization of dietary antigen in the GI tract during the onset of the symptoms of food-induced anaphylaxis, mice received o.g. of fluorescent OVA and the transit of dietary antigen along the GI tract was monitored for 30 min (Fig. 1a). We show that dietary antigen was predominantly localized in the SI, in particularly the jejunum-ileum region, with the highest concentration localized to the proximal ileum region (Fig. 1b). We observe minimal evidence of dietary antigen in the cecum and colon from the ileocecal junction to distal colon. OVA-sensitized and challenged mice possess a heightened GI CD4+ Th2 and ILC2 immune response in the SI, which can alter GI peristalsis.24,25,26,27,28 To determine the localization of antigen in the GI compartment following IgE-MC activation independent of the Type-2 immune response we employed the passive-oral IgE-mediated model of anaphylaxis using transgenic mice with intestinal mastocytosis and no Th2 activation (iIL-9Tg).19,22 Notably, fluorescent OVA in iIL-9Tg mice 30 min following MC activation was similar to that observed in wild-type (WT) mice that experienced food-induced anaphylaxis (Fig. 1b). Furthermore, the dietary antigen was restricted to the distal jejunum and jejunoileal region in naive WT mice and iIL-9Tg mice that received isotype control and did not experience anaphylaxis, suggesting that anaphylaxis does not significantly alter dietary antigen translocation (Fig. 1b). These studies indicate that the eliciting dietary antigen is predominantly restricted to the murine jejunoileal region and not in the caecum or colon at the corresponding time these mice experience symptoms of anaphylaxis.
a Experimental regimen, b Localization of OVA-fluorescence in the GI tract segments of naive or food allergic WT and iIL-9Tg mice following anti-IgE treatment. OVA-sensitized BALB/c mice were repeatedly challenged with OVA and on the 7th challenge received 5 × 105 FITC-labeled FluoSpheres™ Polystyrene Microspheres and localization of FluoSpheres in the GI segments were examined by fluorescence within 30 min. Naive mice and iIL-9Tg mice challenged with either anti-IgE (20 μg/200 μl i.v.) or vehicle received oral gavage of 5 × 105 FITC-labelled FluoSpheres™ Polystyrene Microspheres and localization of FluoSpheres in the GI segments were examined within 30 min. Data are represented as the mean fluorescence signal detected in luminal contents (per mg) of the respective GI segments from n = 5 mice.
Antigen challenge stimulated intestinal epithelial CFTR-dependent Cl− transport and paracellular leak
Given our observation that dietary antigen was restricted to the SI, we examined epithelial ion transport (Short-circuit current; Isc) of the SI from control and food-allergic mice (within 30 min of food-challenge) to determine whether anaphylaxis was associated with altered intestinal epithelial permeability. Basal Isc and forskolin-induced ΔIsc of the SI of food allergic mice was significantly increased compared to vehicle-treated mice (Fig. 2a, b). Pre-exposure of the SI epithelium to the CFTR inhibitor (CFTRinh172) and not DIDS, a potent inhibitor of calcium activated Cl− transporters (Cl−/HCO3− exchanger and potassium/chloride co-transporter), abrogated the Forskolin-induced ΔIsc indicating that increased current is predominantly mediated by CFTR-dependent Cl− transport activity (Fig. 2c). Assessment of the paracellular epithelial function of the jejunum from OVA-treated mice revealed decreased transepithelial resistance (TER) and increased macromolecular flux (FITC-Dextran flux; apical to basolateral) compared with jejunal preparations from vehicle-treated mice (Fig. 2d, e). Collectively, these studies suggest that dietary antigen induced a rapid SI epithelial CFTR-dependent Cl− secretory response and paracellular permeability within 30 min of oral antigen challenge.
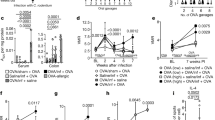
a Isc baseline, b Forskolin-induced short-circuit current response (ΔIsc) of jejunum segments from vehicle- and OVA-treated BALB/c WT mice within 60 min of the 7th OVA challenge. c Forskolin-induced short-circuit current response of jejunum segments from vehicle- and OVA-treated mice following exposure to the ion channel blockers DIDS (100 μM) or CFTRInh172 (20 μM) in the mucosal reservoir inside Ussing chambers system. d TER and e FITC-dextran flux of jejunum segments from vehicle- and OVA-treated BALB/c WT mice within 60 min of the 7th OVA challenge. OVA-treated mice were sensitized with OVA-alum and received seven o.g. OVA challenges. vehicle-treated mice are OVA-sensitized mice that were challenged with vehicle (Saline) and did not develop anaphylaxis symptoms. Data are represented as the mean ± SD; n = 3–7 mice per group from 2–3 representative experiments (a–e). ****P < 0.0001, ***P < 0.001, **P < 0.01, *P < 0.05, ns > 0.05.
Direct exposure of OVA to jejunal SI preparations is sufficient to promote epithelial transcellular and paracellular dysfunction
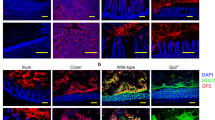
Next, we examined whether the food-induced macromolecular leak was associated with changes in intercellular junctional proteins (JP). To do this, we examined SI epithelial AJ and TJ proteins from naive mice and mice that demonstrated symptoms of anaphylaxis (≥1.5 °C Temperature loss and diarrhea) 30 min following the 7th food allergen challenge. We observed a significant reduction in the level of full length transmembrane proteins in the TJ, Claudin-1, -2, -3 and -5 AJ, E-cadherin and DM, Dsg-2, and Dsc-2 in SI epithelial extracts from food allergic mice compared with naive mice (Fig. 3a, b, control (CTL) vs. food-challenge #7). Intriguingly, we identified the presence of cleaved fragments of the AJ protein, E-cadherin (~55 kDa), Dsg-2 (22 kDa) and Dsc-2 (75 kDa) in SI epithelial extracts from anaphylactic mice (Fig. 3b, food-challenge #7). The food allergic reaction was not associated with a decrease in all intestinal JP as the SI TJ protein occludin was unaffected by repeated dietary food challenge (Fig. 3a challenge #7). Keratin-8 (CK-8) immunoblotting reveals comparable level of intestinal epithelial cells and Actin and GAPDH shows similar protein loading (Fig. 3a, b). Immunofluorescence analyses of the jejunum revealed a similar pattern of decreased proteins in the TJ, Claudin-1, Claudin-2, and E-cadherin in the apical junctional complex of the intestinal epithelium of allergic mice within 30 min of antigen challenge as compared with untreated mice (Fig. 3d). Notably, we observed no change in the expression of the transmembrane protein ZO-1 in jejunum of allergic mice following allergen exposure (Fig. 3d).
Assessment of intestinal junctional proteins expression: western protein analysis of a Claudin-1, Claudin-2, Claudin-3, Claudin-5, Occludin, Keratin-8, GADPH, and Actin and b E-cadherin, Dsg-2, Dsc-2, and GADPH in isolated jejunal epithelial cells from untreated (CTL) and OVA-sensitized mice 30 min following the 5th and 7th oral challenge. c Western protein analysis of Dsg-2 in isolated jejunal epithelial cells from untreated (CTL) and OVA-sensitized mice prior to (Pre-) and 30 min following the 7th oral challenge (Post-) (a–c). Actin and GAPDH were used as a loading control. Colonic tissue was used as a positive control. MW, molecular weight. Each column represents a single mouse. d Immunofluorescence analysis of E-cadherin, ZO-1, Claudin-1 and Claudin-2 (white) in jejunum segments from untreated (vehicle)- and OVA-treated BALB/c WT mice within 30 min of the 7th OVA challenge. Nuclei are visualized with DAPI (blue). d Representative photomicrographs of n = 5–7 mice per group and five serial SI sections per mouse.
To determine whether the cleaved intestinal JP in the TJ, AJ, and DM was associated with development of GI symptoms of food-induced anaphylaxis, we performed analyses on mice following the fifth food-challenge that do not demonstrate symptoms of food-induced anaphylaxis following challenge (food-challenge #5). We show that the level of TJ proteins, Claudin-1, -2, -3 and -5 were similar to that observed in naive mice (Fig. 3a; CTL compared to food-challenge #5). Furthermore, we observed full length E-cadherin and Dsg-2 and Dsc-2 in SI epithelial extracts from asymptomatic mice following 5th challenge (Fig. 3b), albeit we detected the presence of cleaved cadherin fragments (E-cadherin and Dsg-2 and Dsc-2) (Fig. 3b). Collectively these data suggest that cleavage of intestinal JP in the TJ, AJ, and DM was associated with development of GI symptoms of food-induced anaphylaxis.
Given that we were able to detect cleaved cadherin fragments, we utilized the Dsg-2 western blot analyses as a surrogate marker to determine whether a single dietary antigen-challenge induced rapid SI cadherin cleavage. To do this, we examined SI epithelial Dsg-2 in mice prior to (Pre-) and following (Post-) the 7th food-challenge. Notably, we observed the loss of the native full-length Dsg-2 following the 7th challenge (Fig. 3c). In addition, we also observed decreased levels of the 50 kDa Dsg-2 cleavage fragment and accumulation of lower molecular weight (30 kDa) Dsg-2 fragment (Fig. 3c). These data indicate that a single allergen challenge is sufficient to induce a pronounced and rapid decrease in the full length high molecular weight Dsg-2 protein levels and increasing low molecular weight Dsg-2 cleavage products in mice that develop food-induced anaphylaxis.
To determine whether direct antigen exposure of the SI epithelium can induce the GI epithelial dysfunction, we exposed the apical surface of SI segments from unsensitized and food-allergic mice ex vivo to OVA in an Ussing chamber system and assessed Isc and TER. Ex vivo exposure of OVA to the SI segment of a naive animal did not induce any significant change in Isc or TER (Fig. 4a, b). In contrast, OVA exposure of the SI segment from allergic mice stimulated an increase in Isc and a decrease in TER within 30 min (Fig. 4a, b). The baseline Isc and TER of the SI segments from allergic mice was trending lower than that observed from naive mice, however, levels were not statistically significant (Fig. 4a, b). These studies show that a single allergen challenge is sufficient to induce a pronounced and rapid decrease in intestinal epithelial barrier function that is related to the enhanced ion transport and the loss of intestinal epithelial paracellular integrity. To get insight into the temporal nature of the paracellular and transcellular epithelial dysfunction following allergen challenge, we monitored Isc and TER of SI segments from food allergic mice following the 7th OVA challenge. We show that OVA-induced intestinal epithelial barrier dysfunction was maintained for at least 48 h following dietary antigen challenge and returned to baseline levels by 72 h (Fig. 4c, d). Collectively, these studies demonstrate that dietary antigen exposure of the SI mucosal epithelium is sufficient to induce SI barrier dysfunction that can be sustained for up to 48 h following allergen exposure.
a Isc baseline and b TER of ex vivo jejunal segments from unsensitized (naive) and OVA-sensitized and oral challenged mice (allergic) apically exposed to vehicle (PBS) or OVA in Ussing chamber system. c Isc and d TER of ex vivo jejunal segments from unsensitized (Ctrl) and OVA-sensitized and oral challenged mice 24–96 h following the seventh oral challenge. (a, b) Jejunum was removed from unsensitized (naive) and OVA-sensitized and oral challenged mice (allergic- following 6th oral challenge) and mounted in a Ussing chamber system and exposed to either PBS (−) or 1% OVA on the apical side and Isc and TER were recorded as described in the “Materials and methods” section. c, d Jejunum from unsensitized (Ctrl) and OVA-sensitized and oral challenged mice were removed 24, 48, 72, and 96 h following seventh challenge and mounted in a Ussing chamber system and Isc and TER were recorded as described in the “Material and methods” section. Data are represented as the mean ± SD, n = 3 mice per group. ****P < 0.0001, ***P < 0.001, **P < 0.01, *P < 0.05, ns > 0.05.
Dissection of mechanisms of oral antigen-induced transcellular and paracellular permeability
To define the relationship between SI epithelial transcellular and paracellular barrier dysfunction and the development of the dietary antigen-induced GI symptom, secretory diarrhea, we examined the SI from allergic mice that did and did not develop diarrhea following the 7th challenge. The SI segment from mice that developed secretory diarrhea within 30 min of food allergen challenge had a significant increase in Isc (~3-fold) and dramatically decreased TER (~60% reduction) compared to vehicle-treated mice (Fig. 5a, b). In contrary, the SI from mice that received antigen that failed to develop secretory diarrhea did not demonstrate evidence of altered Isc but did show a significant reduction in TER (~26% reduction) compared to vehicle-treated mice (Fig. 5a, b). These studies demonstrate a relationship between altered SI transcellular and paracellular permeability and the development of the food-induced symptom secretory diarrhea in food allergic mice.
a Isc baseline and b TER measurements of jejunal segments from OVA-sensitized mice following vehicle (Saline) or OVA oral challenge (7th challenge) and stratified according to secretory diarrhea development (60 min). OVA-sensitized mice were challenged with OVA (7th Challenge) and evidence of profuse liquid stool (diarrhea-positive) was examined. Following the 60 min diarrhea observation period, jejunal segments were removed and mounted in a Ussing chamber system and Isc and TER were recorded as described in the “Material and methods” section. Data are represented as the mean ± SD, n = 4–7 mice per group. ****P < 0.0001, ***P < 0.001, **P < 0.01, *P < 0.05, ns > 0.05.
Given our demonstration of dietary antigen-induced enhanced Cl− transport, and also paracellular barrier dysfunction associated with JP protein degradation and that this was associated with the GI symptom diarrhea, we hypothesized that the secretory diarrhea response was a consequence of CFTR-dependent Cl− secretion and proteolytic-activity. To test this hypothesis, mice that demonstrated a history of food-induced anaphylaxis (as confirmed by the 6th challenge) received either a chloride channel blocker (GlyH101) (o.g 15 min before OVA) or a protease inhibitor (AEBSF) (i.v. 2 h before OVA) alone or in combination prior to the 7th challenge and food allergen-induced SI epithelial transcellular and paracellular function was assessed (Fig. 6a). As previously demonstrated, OVA-challenge of OVA-sensitized mice increased SI basal Isc, forskolin-induced ΔIsc response and FITC-dextran flux and reduced the TER compared to non-allergic (vehicle) mice (Figs. 2 and 6b, c). Pretreatment with GlyH101 alone, significantly attenuated OVA-induced amplification of forskolin-induced ΔIsc, TER and FITC-dextran flux (Fig. 6b–e). Pretreatment with AEBSF alone, also significantly attenuated OVA-mediated reduction in TER, and increase in FITC-dextran flux, however, SI forskolin-induced ΔIsc was unaffected (Fig. 6b–e). Pretreatment with both GlyH101 and AEBS prior to the 7th OVA-challenge significantly attenuated OVA-induced dysregulation of both SI epithelial transcellular and paracellular function compared with OVA-treated mice that received vehicle (Fig. 6b, c). Importantly, pretreatment of food allergic mice with GlyH101 and AEBSF dramatically reduced the incidence of diarrhea in mice following the 7th OVA-challenge (Fig. 7). Moreover, 10 of 10 of food allergic mice that received OVA developed secretory diarrhea following the 7th challenge. In contrast, only 8 of 18 mice who received GlyH101 and AEBSF developed secretory diarrhea following the 7th challenge (Fig. 7). Collectively, the GI symptom of dietary antigen-induced anaphylaxis, secretory diarrhea, is a consequence of food antigen-induced transcellular and paracellular SI epithelial barrier function.
a Experimental regimen, b Isc baseline and c Forskolin-induced Isc responses (ΔIsc), d TER, e FITC-dextran flux of jejunal segments from OVA-sensitized and oral challenged mice (7th challenge) following pretreatment with GlyH101 and protease inhibitor (AEBSF) alone or in combination. OVA-sensitized mice received repeated OVA challenge (six challenges) and mice that demonstrated evidence of food allergy were stratified into indicated groups. Mice received either 0.5 mM GlyH101 (oral gavage) 15 min prior to the 7th OVA-challenge or 500 μg AEBSF (i.v.) 2 h prior to 7th OVA-challenge, alone or in combination and subsequently received oral gavage (OVA). Following the 60 min observational period, jejunal segments were removed and mounted in a Ussing chamber system and physiological measurements were recorded as described in the Material and methods section. Vehicle represents unsensitized mice that received vehicle oral gavage challenge. c–e Data are represented as the mean ± SD, n = 3–7 mice per group. ****P < 0.0001, ***P < 0.001, **P < 0.01, *P < 0.05, ns > 0.05.
Chi-square analysis of number of mice with/without secretory diarrhea. OVA-sensitized mice received repeated OVA challenge (six challenges) and mice that demonstrated evidence of food allergy were stratified into either vehicle or GlyH101 + AEBSF groups. Mice received 500 μg AEBSF (i.v.) 2 h prior to 7th OVA challenge and 0.5 mM GlyH101 (oral gavage) 15 min prior to the 7th OVA challenge and subsequently received oral gavage (OVA) and evidence for diarrhea was examined for a 60 min observational period.
Discussion
In the present study, we show that: (1) the onset of GI symptoms of dietary antigen-induced anaphylaxis occurred with dietary antigen localized to the SI; (2) the symptom of diarrhea was associated with increased SI epithelial CFTR-dependent Cl− secretion and epithelial JP degradation; (3) The transcellular and paracellular SI dysfunction occurred rapidly following food antigen exposure and persisted for up to 72 h; (4) development of the intestinal symptom diarrhea in dietary antigen-induced anaphylaxis was linked to SI transcellular and paracellular dysfunction and (5) blockade of chloride channel and proteolytic activity attenuated the GI symptoms in dietary antigen-induced anaphylaxis.
The association between food allergy and diarrhea dates back to the 1930s.29,30,31 Rowe reported cases of diarrhea in 15% of 150 cases of GI allergy. Whether or not the symptom of diarrhea was associated with and acute-IgE-mediated reaction or part of some other allergic condition (e.g., allergic colitis or FPIES) was inconclusive; however, the diarrhea phenotype was food-dependent, acute and often associated with other clinical signs and symptoms of food-induced anaphylaxis, such as fatigue, toxemia and nervousness.29,30 More recent reports indicate that IgE-mediated anaphylactic reactions involving the GI tract including diarrhea occur in 30 to 45% of cases anaphylaxis.32,33 Interestingly, antidotal data supports a role for GI symptoms in the severity of food-induced anaphylaxis.4,9 Retrospective chart analyses of clinical features of acute generalized hypersensitivity reactions in 1149 patients revealed that features of anaphylaxis, including vomiting and nausea, strongly correlated with anaphylaxis severity.9 In contrast, common skin features, including urticaria, erythema and angioedema, did not correlate with hypoxia and hypotension.9 Similarly, examination of the clinical history of 163 pediatric patients with food-induced anaphylaxis showed that relapsing GI symptoms increased the risk of hypotension and bradycardia or cardiac arrest.8
The molecular basis by which an eliciting dietary antigen induces GI symptoms in food-induced anaphylaxis is unclear. We have previously shown that oral antigen-induced anaphylaxis in mice is MC-dependent18 and that heightened GI MC numbers correlate with intestinal and systemic anaphylaxis severity.19,22 Similarly, systemic mastocytosis patients can present with increased GI symptoms and have increased risk of severe anaphylaxis34,35 and administration of the MC stabilizing agent sodium cromoglycate protected food allergic individuals from food provocation-induced GI permeability and altered GI function.36 Herein, we demonstrate that the food allergen-induced GI symptom of diarrhea was associated with a rapid SI secretory response and epithelial barrier dysfunction and that suppression of the GI symptom required inhibition of both Cl− channel activity and proteolysis. Several MC-derived mediators are known to modulate discrete components of the intestinal epithelial secretory and barrier function including histamine, prostaglandins and mast cell-derived proteases.37,38 Secretory diarrhea is generally a result of dysregulation of the coordinated GI epithelial secretory or absorptive processes leading to excessive accumulation of GI luminal fluid.39 The SI epithelial fluid secretion is predominantly mediated by transepithelial Cl− flux from the basolateral to apical surface of the epithelium via coordinated chloride channels and transporters including Na/K/Cl symporter (NKCC1), Basolateral K+ channels (KCNQ1/KNE3 and KCNN4), the cyclic-nucleotide-activated cystic fibrosis transmembrane conductance regulator (CFTR) and Ca2+-activated Cl− channels (CaCCs).40 We show that dietary exposure of the SI of food-sensitized mice promoted an increase in basolateral to apical Cl− secretion via CFTR-dependent mechanism. Histamine signaling through the H1R stimulates CFTR Cl− ion secretion through cAMP/PKA pathway.41,42 Similarly, prostaglandins and serotonin increase Cl− secretion in human colon and jejunum samples, respectively.43,44 However, experimental studies in in vivo animal model systems have demonstrated that while antihistamines may impact systemic symptoms, they do not impact the secretory diarrhea phenotype in food-induced anaphylaxis, and clinically, antihistamines have been shown to be effective for the treatment of the cutaneous symptoms but not the GI symptoms.3,18 A recent study reported an important role for MC-derived PGD2 in the suppression of systemic symptom of shock (hypotension and hypothermia) during an anaphylactic reaction in mice45; however, as the anaphylaxis model employed by the investigators did not induce GI symptoms, they were unable to assess the contribution of MC-derived PGD2 to the secretory diarrhea response. Mast cell-derived cytokines such as IL-6, IL-8, IL-13 and TNF alpha have been shown to activate secondary messenger cascades including Ca2+ and cyclic nucleotides such as cAMP and cGMP to stimulate CFTR-dependent Cl− transport and inhibit the absorptive capacity of apical Na+ transporters and promote a secretory diarrhea phenotype.39,46 Furthermore, the pro-Type-2 cytokines associated with food-induced anaphylaxis such as IL-4 and IL-13 regulate SI CFTR expression and enhanced CFTR activity.46,47,48 However, IgE-FcεRI-induced release of cytokines from MCs generally occurs up to 1 h following activation and we show that the dietary antigen-induced CFTR-dependent response occurred rapidly within min of allergen exposure suggesting that the CFTR-dependent Cl− transport is not likely MC-derived cytokine-mediated. We predict that the repetitive oral allergen challenge and stimulation of the SI CD4+ Th2 and ILC2 response is likely to drive SI CFTR mRNA and protein induction in the intestinal epithelium and that cAMP-inducing mast cell-derived mediators stimulate exaggerated intestinal epithelial CFTR activity and CFTR-dependent Cl− secretion and as a consequence development of secretory diarrhea acutely following allergen exposure. The physiological significance of increased fluid secretion in the SI of food allergic mice is likely related to efforts to remove the food allergen from the SI surface epithelium and promote elimination of the food allergen from the host GI compartment. Analogous to this, helminth infestation of the GI tract is known to promote an anti-helminth host immune response known as the “weep and sweep”. The “weep and sweep” response involves induction of a GI CFTR-dependent secretory response to increased luminal fluid (weep) and increased peristaltic contractility (sweep), which is thought to lead to detachment of the helminth parasite from the surface epithelia and promote parasite expulsion from the host.49 Intriguingly, the anti-helminth host “weep and sweep” response is driven by a CD4+ Th2 and ILC2-dependent immune response similar to that observed in food allergic reactions.49,50
The dietary antigen-induced SI epithelial barrier dysfunction was also associated with rapid degradation in the SI epithelial TJ and AJ proteins and increased paracellular leak. AJ and TJ proteins expressed by intestinal epithelial cells are critical for the establishment and maintenance of intestinal epithelial paracellular permeability and barrier function.51,52 Previous studies in rats have revealed increased intestinal permeability during an intestinal hypersensitivity reaction that was dependent on MC activation and release of MC proteases.53,54,55 IgE-cross linking of FcεRI on MC promotes the rapid release of several proteases in both mouse and man.56,57,58,59 In mice, IgE-mediated reactions are associated with the prodigious release of the chymotrypsin-like serine protease MCPT-1; however, connective and mucosal MCs are known to express many additional proteases, including MCPT-4 (chymotrypsin-like), MCPT-5 (Elastase-like), MCPT-6, MCPT-7 (trypsin-like tryptases), and carboxypeptidase 3 (CPA3).60 Several of the MC proteases can disrupt TJ proteins and increase cellular permeability. MCPT-4, which possesses chymotryptic proteolytic activity, and the elastase-like MCPT-5 have been shown to disrupt epidermal TJ function, in particularly Claudin-4.61 Studies in MCPT-1-deficient mice have revealed a role for MCPT-1 in the proteolytic degradation of Occludin62 and MCPT-4 induces disruption of SI epithelial Claudin-3 function via PAR-2-dependent process and altering SI intestinal permeability.63,64 Similarly, human tryptase has been shown to regulate GI permeability via PAR-2-β-arrestin-dependent mechanism causing disruption of TJ, Claudin-1, ZO-1 and Occludin and perijunctional F-actin.65,66 Given that food-induced anaphylaxis in mice is associated with the accumulation and degranulation of intestinal mucosal MCs, and not connective tissue MCs, it is likely that mucosal MCs proteases such as MCPT-1 and MCPT-2 may drive the SI epithelial barrier dysfunction.18,19 Employing a rat model of anaphylaxis, investigators have previously reported a role for the mucosal mast cell granule chymase, rat mast cell protease-II (RMCP-II), in increased jejunal paracellular permeability.55,67 Notably, RMCP-II induces the loss of ZO-1 and Occludin in MDCK-II monolayers.55,67 Examination of Mcpt1−/– mice on the BALB/c background, revealed no role for MCPT-1 in the incidence of diarrhea or severity of food-induced anaphylaxis (Incidence of Diarrhea; 8/10 vs 9/14; following the 7th oral (OVA) challenge of OVA-sensitized WT vs Mcpt1−/– mice; n = 10 and 14 mice, respectively.), suggesting that other mucosal MC-derived proteases are likely to drive the SI epithelial barrier dysfunction.
In summary, by employing a murine model of dietary antigen-induced anaphylaxis with intestinal and systemic symptoms, we show that the dietary antigen-induced anaphylaxis is associated with an increase in SI transcellular and paracellular permeability. We show that the altered intestinal permeability and secretory diarrheal phenotype is rapidly induced by MC degranulation and can be inhibited by pharmacological blockade of proteolytic and CFTR-dependent Cl− transport activity.
Materials and methods
Animals
Six-to-eight-week-old BALB/c WT mice were obtained from the National Cancer Institute (Bethesda, MD, USA) and bred in-house at Cincinnati Children’s Hospital Medical Center (CCHMC) (Cincinnati, OH, USA) and at the University of Michigan (UM) (Ann Arbor, MI, USA). Intestinal IL-9 transgenic (iIL-9Tg) mice were generated as previously described.19 Age-, sex-, weight-matched littermates were used as controls in all experiments. The mice were maintained and bred in a clean barrier facility and were handled under an approved Institutional Animal Care and Use Committee protocols at CCHMC and University of Michigan animal facility.
Oral antigen-induced intestinal anaphylaxis
Four-to-eight--week-old mice were sensitized to OVA (50 µg of OVA/1 mg of alum in sterile saline by intraperitoneal (i.p.) injection) and received repeated oral gavage (o.g.) challenge with OVA (250 µl of OVA (50 mg) in saline or 250 μl of saline (vehicle)) as previously described.22 Prior to each o.g. challenge, mice were deprived of food for 4–5 h. Rectal temperatures were measured prior to challenge and then every 15 min for 60 min. Diarrhea was assessed by visually monitoring mice for up to 60 min following o.g. challenge and mice demonstrating profuse liquid stool were recorded as diarrhea-positive. Evidence of secretory diarrhea was assessed by determination of short-circuit current (Isc) of SI segments ex vivo in a Ussing chamber system up to 60 min following o.g. challenge. Mice were considered allergic if they demonstrated symptoms of anaphylaxis (hypothermia > 1.5 °C temperature loss and diarrhea) following the 6th or 7th challenge. In Some experiments, mice were o.g. with 0.5 mM N-(2-naphthalenyl)-[(3,5-dibromo-2,4-dihydroxyphenyl) methylene] glycine hydrazide (GlyH101) (EMD Millipore #219671) 15 min before the 7th OVA-challenge. 500 μg 4-benzenesulfonyl fluoride hydrochloride (AEBSF) (Sigma# A8456) were giving intravenous (i.v.) 2 h prior to the 7th OVA the challenge. To track food allergen passage in the GI tract, Mice were administered OVA (200 mg/ml) with 5 × 105 FITC-labelled FluoSpheres™ Polystyrene Microspheres (10 µM size) (Thermo Fisher, Waltham, MA, USA) by oral gavage and monitored for 30 min. The mice were euthanized, the GI tract surgically removed and segmented into anatomical compartments of the GI tract (stomach, duodenum, jejunum, ileum, caecum and colon). The duodenum was divided into 1.5-cm segments, jejunum into 4-cm segments, ileum into 2-cm segments and colon into 4-cm segments. The duodenum was defined as 3-cm GI segment distal to pyloric sphincter. The jejunum was defined as the ~16-cm GI segment distal of the duodenum and 10-cm proximal from the ileocecal valve. The ileum was defined as the GI segment 10-cm proximal from the ileocecal valve. The caecum was defined as the pouch connecting to the junction of the proximal ileum and distal colon. The colon segment was ~8 cm connecting the proximal caecum to the distal rectum. The luminal contents of the segments were flushed with phosphate-buffered saline (PBS) centrifuged, weighed and suspended in 200 µl PBS and the fluorescence of the total contents of each segment was measured using a Bioteck multi-mode plater reader (Synergy H1) with Gen5 software. Data presented as the mean fluorescence signal detected per mg of luminal contents.
Passive anaphylaxis
Mice were injected i.v. with 20 μg/200 μL of anti-IgE (IgG2a mAb to mouse IgE; EM-95) and evidence of anaphylaxis was examined as previously described.11,68
Solutions and drugs
The Krebs buffer used on each side of the Ussing chamber contained 4.70 mM KCl, 2.52 mM CaCl2, 118.5 mM NaCl, 1.18 mM NaH2PO4, 1.64 mM MgSO4 and 24.88 mM NaHCO3. The tissues were allowed to equilibrate for 15 min in Krebs buffer containing 5.5 mM glucose. All reagents were obtained from Sigma-Aldrich (St. Louis, MO, USA) unless stated otherwise.
Ussing chambers
One centimeter, freshly isolated, serosal-stripped segments of jejunum was mounted between the hemi-chambers of an Ussing apparatus (U2500 Dual Ussing chamber, Warner instruments, Hamden, CT), and 0.112 cm2 of tissue was exposed to 10 ml Krebs buffer at 37 °C. The transepithelial potential difference (PD) was detected with two paired electrodes that contained 4% agar in 3 M KCl. The electrodes were connected to a voltage clamp amplifier (EC-800, Epithelial voltage clamp, Warner Instruments, Hamden, CT). The electrode PD and fluid resistance were compensated before mounting tissue segments into the chamber. To establish equilibrium, PD was continuously monitored under open-circuit conditions for 15 min. Thereafter, the tissues were voltage-clamped at 0 mV while continuously measuring short-circuit current (Isc). Voltage pulses (3-mV square waves sustained for 5 s) were delivered every 50 s to yield a current response for calculation of TER from the Ohm's law. For ion conductance experiments, changes in Isc were determined for the cumulative addition of forskolin to the serosal reservoir. After the peak response to the final concentration of each agonist was recorded, the Krebs buffer on each side of the chamber was replaced, and the tissue was allowed to equilibrate for 30 min Immediately following re-equilibration, tissue was pre-incubated with ion channel blockers 4,4′-Diisothiocyanatostilbene-2,2′-disulfonate (DIDS) (100 μM) or CFTRInh172 (20 μM) to mucosal reservoir. Changes in Isc were measured in response to the addition of forskolin to the mucosal side. To study effects of direct allergen application, 1% OVA or equal volume of PBS was directly added into apical side of the dissected jejunum mounted in the Ussing chamber and Isc, TER were recorded as previously described.19
Intestinal epithelial cells (IEC) preparation
Five centimeters segment of the jejunum was washed with cold PBS and 2% fetal bovine serum (FBS) and 5 mM DTT (20 min at 37 °C with shaking). Afterward, IEC were isolated by washing tissue three times with PBS and 2% FBS and 5 mM EDTA (10 min at 37 °C with shaking), then the washing solution was collected then centrifuged (400 × g for 10 min at 4 °C) and pellet was suspended in PBS for cells quantification and lysis. For cell lysis, isolated IEC were resuspended in RIPA buffer (0.5% Triton X-100, 0.5% NP-40, 0.5% deoxycholic acid, 0.1% SDS, 150 mM NaCl, 1 mM EGTA [pH 8.0], 1 mM EDTA, 0.2 mM sodium orthovanadate, 20 mM Tris [pH 7.4]) supplemented with protease and phosphatase inhibitors. Immunoblotting was performed as previously described.69
Immunofluorescence
Five centimeters segment of the jejunum was fresh frozen in O.C.T. Tissues were fixed in 95% cold ethanol for 30 min, followed by 1 min of pure acetone fixation at room temperature. For ZO-1 staining, tissues were fixed in 4% PFA, followed by permeabilization with 0.5% Triton X-100. Primary antibody staining was performed in Hank’s balanced salt solution with 3% bovine serum albumin (BSA) for overnight. Secondary antibodies were incubated in 3% BSA and for 1 h. Antibodies for WB were as follows: Rabbit anti-claudin-1 #51–9100 (Thermo Fisher, Waltham, MA, USA), rabbit anti-claudin-2 #51-6100 (Thermo Fisher, Waltham, MA, USA), rabbit anti-claudin-3 #SAB4500434 (Sigma-Aldrich, St. Louis, MO, USA), mouse anti-claudin-5 #35–2500, rabbit anti-ZO-1 #617300 (Thermo Fisher, Waltham, MA, USA), goat anti-E-Cadherin #AF748, goat anti-mouse JAM-A #AF1077 (R&D Systems, Minneapolis, MN, USA), rabbit anti-cytokeratin-8 #ab53280, rabbit anti-dsg-2 #ab124683 (Abcam, Cambridge, UK), mouse anti-dsc-2 #32–6200 (Thermo Fisher, Waltham, MA, USA), rabbit anti-GADPH #G9545 (Sigma-Aldrich, St. Louis, MO, USA), rabbit anti-calnexin #C4731 (Sigma-Aldrich, St. Louis, MO, USA). Antibodies for immunofluorescence were as following: rat anti-E-cadherin #53-3249-82, rabbit anti-claudin-1 #51-9000, rabbit anti-claudin-2 #516100 (Thermo Fisher, Waltham, MA, USA). Nucleus were detected with DAPI. Confocal microscopy was performed using a Leica SP5 inverted microscope (Wetzlar, Germany) Leica SP5 software.
Statistical analysis
Data are expressed as mean ± standard deviation (SD), unless otherwise stated. Statistical significance comparing different sets of mice was determined by Student’s t test. In experiments comparing multiple experimental groups, statistical differences between groups were analyzed using the one-way, nonparametric ANOVA and a Bonferroni post-test. P < 0.05 was considered significant. All analyses were performed using Prism 7.0 software (GraphPad Software Inc., San Diego, CA, USA).
References
Sampson, H. A. Anaphylaxis and emergency treatment. Pediatrics 111, 1601–1608 (2003).
Ross, M. P. et al. Analysis of food-allergic and anaphylactic events in the national electronic injury surveillance system. J. Allergy Clin. Immunol. 121, 166–171 (2008).
Wang, J. & Sampson, H. A. Food anaphylaxis. Clin. Exp. Allergy 37, 651–660 (2007).
Sampson, H. A., Mendelson, L. & Rosen, J. P. Fatal and near-fatal anaphylactic reactions to food in children and adolescents. N. Engl. J. Med. 327, 380–384 (1992).
Schrander, J. J., Unsalan-Hooyan, R. W., Forget, P. P. & Jansen, J. [51Cr]EDTA intestinal permeability in children with cow’s milk tolerance. J. Pediatr. Gastroenterol. Nutr. 10, 189–192 (1990).
Troncone, R., Caputo, N., Florio, G. & Finelli, E. Increased intestinal sugar permeability after challenge in children with cow’s milk allergy or intolerance. Allergy 49, 142–146 (1994).
Van Elburg, R., Heymans, H. S. & De, M. J. Effect of disodiumcromoglycate on intestinal permeability changes and clinical response during cow’s milk challenge. Pediatr. Allergy Immunol. 4, 79–85 (1993).
Calvani, M. et al. Risk factors for severe pediatric food anaphylaxis in Italy. Pediatr. Allergy Immunol. 22, 813–819 (2011).
Brown, S. G. A. Clinical features and severity grading of anaphylaxis. J. Allergy Clin. Immunol. 114, 371–376 (2004).
Galli, S. J. et al. Mast cells as “tunable” effector and immunoregulatory cells: recent advances. Annu. Rev. Immunol. 23, 749–786 (2005).
Strait, R. T., Morris, S. C., Yang, M., Qu, X. W. & Finkelman, F. D. Pathways of anaphylaxis in the mouse. J. Allergy Clin. Immunol. 109, 658–668 (2002).
Dombrowicz, D., Flamand, V., Brigman, K. K., Koller, B. H. & Kinet, J. P. Abolition of anaphylaxis by targeted disruption of the high affinity immunoglobulin E receptor alpha chain gene. Cell 75, 969–976 (1993).
Lorentz, A., Schwengberg, S., Mierke, C., Manns, M. P. & Bischoff, S. C. Human intestinal mast cells produce IL-5 in vitro upon IgE receptor cross-linking and in vivo in the course of intestinal inflammatory disease. Eur. J. Immunol. 29, 1496–1503 (1999).
Santos, J., Benjamin, M., Yang, P. C., Prior, T. & Perdue, M. H. Chronic stress impairs rat growth and jejunal epithelial barrier function: role of mast cells. Am. J. Physiol. Gastrointest. Liver Physiol. 278, G847–G854 (2000).
Kelefiotis, D. & Vakirtzi-Lemonias, C. In vivo responses of mouse blood cells to platelet-activating factor (PAF): role of the mediators of anaphylaxis. Agents Actions 40, 150–156 (1993).
Strait, R. T., Morris, S. C., Smiley, K., Urban, J. F. Jr. & Finkelman, F. D. IL-4 exacerbates anaphylaxis. J. Immunol. 170, 3835–3842 (2003).
Lorentz, A., Schwengberg, S., Sellge, G., Manns, M. P. & Bischoff, S. C. Human intestinal mast cells are capable of producing differnt cytokine profiles: role of igE receptor cross-linking and IL-4. J. Immunol. 164, 43–48 (2000).
Brandt, E. B. et al. Mast cells are required for experimental oral allergen-induced diarrhea. J. Clin. Investig. 112, 1666–1677 (2003).
Forbes, E. E. et al. IL-9- and mast cell-mediated intestinal permeability predisposes to oral antigen hypersensitivity. J. Exp. Med. 205, 897–913 (2008).
Wechsler, J. B., Schroeder, H. A., Byrne, A. J., Chien, K. B. & Bryce, P. J. Anaphylactic responses to histamine in mice utilize both histamine receptors 1 and 2. Allergy 68, 1338–1340 (2013).
Wang, M. et al. Combined blockade of the histamine H1 and H4 receptor suppresses peanut-induced intestinal anaphylaxis by regulating dendritic cell function. Allergy 71, 1561–1574 (2016).
Ahrens, R. et al. Intestinal mast cell levels control severity of oral antigen-induced anaphylaxis in mice. Am. J. Pathol. 180, 1535–1546 (2012).
Sledd, J. et al. Loss of IL-4Ralpha-mediated PI3K signaling accelerates the progression of IgE/mast cell-mediated reactions. Immun. Inflamm. Dis. 3, 420–430 (2015).
Akiho, H., Blennerhassett, P., Deng, Y. & Collins, S. M. Role of IL-4, IL-13, and STAT6 in inflammation-induced hypercontractility of murine smooth muscle cells. Am. J. Physiol. Gastrointest. Liver Physiol. 282, G226–G232 (2002).
Akiho, H., Ihara, E., Motomura, Y. & Nakamura, K. Cytokine-induced alterations of gastrointestinal motility in gastrointestinal disorders. World J. Gastrointest. Pathophysiol. 2, 72–81 (2011).
Akiho, H. et al. Interleukin-4- and -13-induced hypercontractility of human intestinal muscle cells-implication for motility changes in Crohn’s disease. Am. J. Physiol. Gastrointest. Liver Physiol. 288, G609–G615 (2005).
Khan, W. I. et al. Modulation of intestinal muscle contraction by interleukin-9 (IL-9) or IL-9 neutralization: correlation with worm expulsion in murine nematode infections. Infect. Immun. 71, 2430–2438 (2003).
Zhao, A. et al. Dependence of IL-4, IL-13, and nematode-induced alterations in murine small intestinal smooth muscle contractility on Stat6 and enteric nerves. J. Immunol. 171, 948–954 (2003).
Rowe, A. Jr., Rowe, A. H., Uyeyama, K. & Young, E. J. Diarrhea caused by food allergy. J. Allergy 27, 424–436 (1956).
Rowe, A. H. [Food allergy and its clinical manifestations]. Rev. Clin. Espanola 62, 366–373 (1956).
Rowe, A. H. Abdominal food allergy: its history, symptomatology, diagnosis and treatment. Calif. West. Med. 29, 317–322 (1928).
Simons, F. E. & Sheikh, A. Anaphylaxis: the acute episode and beyond. BMJ 346, f602 (2013).
Lieberman, P. et al. The diagnosis and management of anaphylaxis practice parameter: 2010 update. J. Allergy Clin. Immunol. 126, 477–480 (2010). e471-442.
Soter, N. A., Austen, K. F. & Wasserman, S. I. Oral disodium cromoglycate in the treatment of systemic mastocytosis. N. Engl. J. Med. 301, 465–469 (1979).
Horan, R. F., Sheffer, A. L. & Austen, K. F. Cromolyn sodium in the management of systemic mastocytosis. J. Allergy Clin. Immunol. 85, 852–855 (1990).
Andre, C., Andre, F., Colin, L. & Cavagna, S. Measurement of intestinal permeability to mannitol and lactulose as a means of diagnosing food allergy and evaluating therapeutic effectiveness of disodium cromoglycate. Ann. Allergy 59, 127–130 (1987).
Perdue, M. H., Masson, S., Wershil, B. K. & Galli, S. J. Role of mast cells in ion transport abnormalities associated with intestinal anaphylaxis. Correction of the diminished secretory response in genetically mast cell-deficient W/Wv mice by bone marrow transplantation. J. Clin. Investig. 87, 687–693 (1991).
Crowe, S. E., Sestini, P. & Perdue, M. H. Allergic reactions of rat jejunal mucosa. Ion transport responses to luminal antigen and inflammatory mediators. Gastroenterology 99, 74–82 (1990).
Thiagarajah, J. R., Donowitz, M. & Verkman, A. S. Secretory diarrhoea: mechanisms and emerging therapies. Nature reviews. Gastroenterol. Hepatol. 12, 446–457 (2015).
Barrett, K. E. & Keely, S. J. Chloride secretion by the intestinal epithelium: molecular basis and regulatory aspects. Ann. Rev. Physiol. 62, 535–572 (2000).
Homaidan, F. R., Tripodi, J., Zhao, L. & Burakoff, R. Regulation of ion transport by histamine in moue cecum. Eur. J. Pharmacol. 331, 199–204 (1997).
Kim, Y. S. et al. Histamine 1 receptor-Gbetagamma-cAMP/PKA-CFTR pathway mediates the histamine-induced resetting of the suprachiasmatic circadian clock. Mol. Brain 9, 49 (2016).
Kellum, J. M., Budhoo, M. R., Siriwardena, A. K., Smith, E. P. & Jebraili, S. A. Serotonin induces Cl− secretion in human jejunal mucosa in vitro via a nonneural pathway at a 5-HT4 receptor. Am. J. Physiol. 267, G357–G363 (1994).
Collins, D., Hogan, A. M., Skelly, M. M., Baird, A. W. & Winter, D. C. Cyclic AMP-mediated chloride secretion is induced by prostaglandin F2alpha in human isolated colon. Br. J. Pharmacol. 158, 1771–1776 (2009).
Nakamura, T. et al. Mast cell-derived prostaglandin D2 attenuates anaphylactic reactions in mice. J. Allergy Clin. Immunol. 140, 630–632.e639 (2017).
Wu, D. et al. Interleukin-13 (IL-13)/IL-13 receptor α1 (IL-13Rα1) signaling regulates intestinal epithelial cystic fibrosis transmembrane conductance regulator channel-dependent Cl− secretion. J. Biol. Chem. 286, 13357–13369 (2011).
Galietta, L. J. et al. IL-4 is a potent modulator of ion transport in the human bronchial epithelium in vitro. J. Immunol. 168, 839–845 (2002).
Zund, G., Madara, J. L., Dzus, A. L., Awtrey, C. S. & Colgan, S. P. Interleukin-4 and Interleukin-13 differentially regulate epithelial chloride secretion. J. Biol. Chem. 271, 7460–7464 (1996).
Anthony, R. M., Rutitzky, L. I., Urban, J. F. Jr., Stadecker, M. J. & Gause, W. C. Protective immune mechanisms in helminth infection. Nat. Rev. Immunol. 7, 975–987 (2007).
Lee, J. B. et al. IL-25 and CD4(+) TH2 cells enhance type 2 innate lymphoid cell-derived IL-13 production, which promotes IgE-mediated experimental food allergy. J. Allergy Clin. Immunol. 137, 1216–1225.e1215 (2016).
Groschwitz, K. R. & Hogan, S. P. Intestinal barrier function: molecular regulation and disease pathogenesis. J. Allergy Clin. Immunol. 124, 3–20 (2009).
Turner, J. R. Intestinal mucosal barrier function in health and disease. Nat. Rev. Immunol. 9, 799–809 (2009).
Turner, M. W. et al. Intestinal hypersensitivity reactions in the rat. I. Uptake of intact protein, permeability to sugars and their correlation with mucosal mast-cell activation. Immunology 63, 119–124 (1988).
King, S. J., Miller, H. R., Newlands, G. F. & Woodbury, R. G. Depletion of mucosal mast cell protease by corticosteroids: effect on intestinal anaphylaxis in the rat. Proc. Natl Acad. Sci. USA 82, 1214–1218 (1985).
Scudamore, C. L., Thornton, E. M., McMillan, L., Newlands, G. F. & Miller, H. R. Release of the mucosal mast cell granule chymase, rat mast cell protease-II, during anaphylaxis is associated with the rapid development of paracellular permeability to macromolecules in rat jejunum. J. Exp. Med. 182, 1871–1881 (1995).
Yu, L. C. & Perdue, M. H. Role of mast cells in intestinal mucosal function: studies in models of hypersensitivity and stress. Immunol. Rev. 179, 61–73 (2001).
Bischoff, S. C. Mucosal allergy: role of mast cells and eosinophil granulocytes in the gut. Bailliere’s Clin. Gastroenterol. 10, 443–459 (1996).
Gurish, M. F. & Austen, K. F. The diverse roles of mast cells. J. Exp. Med. 194, F1–F5 (2001).
Galli, S. J., Maurer, M. & Lantz, C. S. Mast cells as sentinels of innate immunity. Curr. Opin. Immunol. 11, 53–59 (1999).
Pejler, G., Abrink, M., Ringvall, M. & Wernersson, S. Mast cell proteases. Adv. Immunol. 95, 167–255 (2007).
Bankova, L. G. et al. Mouse mast cell proteases 4 and 5 mediate epidermal injury through disruption of tight junctions. J. Immunol. 192, 2812–2820 (2014).
Lawrence, C. E., Paterson, Y. Y., Wright, S. H., Knight, P. A. & Miller, H. R. Mouse mast cell protease-1 is required for the enteropathy induced by gastrointestinal helminth infection in the mouse. Gastroenterology 127, 155–165 (2004).
Groschwitz, K. R. et al. Mast cells regulate homeostatic intestinal epithelial migration and barrier function by a chymase/Mcpt4-dependent mechanism. Proc. Natl Acad. Sci. USA 106, 22381–22386 (2009).
Groschwitz, K. R., Wu, D., Osterfeld, H., Ahrens, R. & Hogan, S. P. Chymase-mediated intestinal epithelial permeability is regulated by a protease-activating receptor/matrix metalloproteinase-2-dependent mechanism. Am. J. Physiol. Gastrointest. Liver Physiol. 304, G479–G489 (2013).
Jacob, C. et al. Mast cell tryptase controls paracellular permeability of the intestine. Role of protease-activated receptor 2 and beta-arrestins. J. Biol. Chem. 280, 31936–31948 (2005).
Wilcz-Villega, E. M., McClean, S. & O’Sullivan, M. A. Mast cell tryptase reduces junctional adhesion molecule-A (JAM-A) expression in intestinal epithelial cells: implications for the mechanisms of barrier dysfunction in irritable bowel syndrome. Am. J. Gastroenterol. 108, 1140–1151 (2013).
Scudamore, C. L. et al. Basal secretion and anaphylactic release of rat mast cell protease-II (RMCP-II) from ex vivo perfused rat jejunum: translocation of RMCP-II into the gut lumen and its relation to mucosal histology. Gut 37, 235–241 (1995).
Baniyash, M. & Eshhar, Z. Inhibition of IgE binding to mast cells and basophils by monoclonal antibodies to murine IgE. Eur. J. Immunol. 14, 799–807 (1984).
Capaldo, C. T. et al. Proinflammatory cytokine-induced tight junction remodeling through dynamic self-assembly of claudins. Mol. Biol. Cell 25, 2710–2719 (2014).
Acknowledgements
This work was supported by National Institutes of Health grants DK073553, DK090119, AI138177, and AI112626; Food Allergy Research & Education (FARE); Department of Defense grant W81XWH-15-1-051730; M-FARA; and the Mary H. Weiser Food Allergy Center supported (to S.P.H.).
Author information
Authors and Affiliations
Contributions
D.W., R.A., L.W., and A.Y. performed experiments. S.P.H. and A.Y. analyzed the data, and wrote the manuscript. V.G. and A.N. designed and assisted with some experiments. T.N., N.W.L., C.P., A.N., C.A.P. manuscript revision and discussion. S.P.H study supervision and funding acquisition.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yamani, A., Wu, D., Ahrens, R. et al. Dysregulation of intestinal epithelial CFTR-dependent Cl− ion transport and paracellular barrier function drives gastrointestinal symptoms of food-induced anaphylaxis in mice. Mucosal Immunol 14, 135–143 (2021). https://doi.org/10.1038/s41385-020-0306-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41385-020-0306-6
This article is cited by
-
Orally desensitized mast cells form a regulatory network with Treg cells for the control of food allergy
Mucosal Immunology (2021)