Abstract
There continues to be a major need for more effective inflammatory bowel disease (IBD) therapies. IL-13Rα2 is a decoy receptor that binds the cytokine IL-13 with high affinity and diminishes its STAT6-mediated effector functions. Previously, we found that IL-13Rα2 was necessary for IBD in mice deficient in the anti-inflammatory cytokine IL-10. Here, we tested for the first time a therapeutic antibody specifically targeting IL-13Rα2. We also used the antibody and Il13ra2−/− mice to dissect the role of IL-13Rα2 in IBD pathogenesis and recovery. Il13ra2−/− mice were modestly protected from induction of dextran sodium sulfate (DSS)-induced colitis. Following a 7-day recovery period, Il13ra2−/− mice or wild-type mice administered the IL-13Rα2-neutralizing antibody had significantly improved colon health compared to control mice. Neutralizing IL-13Rα2 to increase IL-13 bioavailability promoted resolution of IBD even if neutralization occurred only during recovery. To link our observations in mice to a large human cohort, we conducted a phenome-wide association study of a more active variant of IL-13 (R130Q) that has reduced affinity for IL-13Rα2. Human subjects carrying R130Q reported a lower risk for Crohn’s disease. Our findings endorse moving anti-IL-13Rα2 into preclinical drug development with the goal of accelerating recovery and maintaining remission in Crohn’s disease patients.
Similar content being viewed by others
Introduction
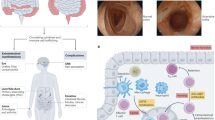
Crohn’s disease (CD) and ulcerative colitis (UC) are inflammatory bowel diseases (IBD) usually characterized by periods of exacerbation and remission.1,2 IBD pathogenesis has been attributed to multiple factors including genetic predispositions, microbial dysbiosis, excessive innate and adaptive immune responses, and breakdown of epithelial barrier function. A common treatment option for patients suffering from IBD is the administration of antitumor necrosis factor alpha (TNFα) agents; however, up to 40% of patients with active IBD do not respond to this treatment for unknown reasons.3 Thus, further exploration of the mechanisms that underlie IBD pathogenesis is necessary to develop improved therapies.
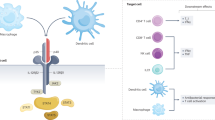
Previous studies identified elevated transcripts of IL13RA2 mRNA in mucosal biopsies of patients with active UC and CD who were nonresponders to anti-TNFα compared to responders.4,5 The immunology literature to date largely indicates that IL-13Rα2 is a nonsignaling decoy receptor for interleukin (IL)-13 that does not exhibit canonical JAK-STAT signaling activity6,7,8,9,10,11,12,13,14. There are a few reports that IL-13Rα2 can alternatively signal through activator protein-1, but in which contexts this happens remains controversial.15,16 It is widely accepted that IL-13 signaling occurs through the IL-4Rα/IL-13Rα1 heterodimer to promote type 2 immunity and that IL-13 signaling induces IL-13Rα2 expression.7,17,18 IL-13Rα2 binds IL-13 with an affinity >400-fold higher than IL-4Rα/IL-13Rα1.18 As a result, IL-13Rα2 can function as a physiological rheostat of type 2 immunity by limiting the amount of IL-13 available to drive STAT6-dependent signaling.19,20 Epithelial cells, fibroblasts, and smooth muscle cells of mice and humans constitutively express IL-13Rα2.21
As a potent type 2 cytokine, IL-13 is a critical suppressor of type 1 and type 17 inflammation associated with IBD pathogenesis 22,23 as well as an integral promotor of wound repair.24,25 In spite of this, the role of IL-13 in IBD is still not well understood. Although IL-13 has been reported to be an inflammatory stimulus in UC,26,27 recent clinical studies found that anti-IL-13 therapy was not effective for UC patients.28,29 While IL-13 is not known to be an initial driver of CD, it has been implicated in tissue remodeling and fibrosis in CD.30,31 IL-13 and other type 2 cytokines are upregulated in response to tissue injury and are important for dampening inflammation and promoting wound resolution and repair,23,32,33,34 requirements for recovery from both UC and CD.
We have hypothesized that the function of IL-13Rα2 as a decoy receptor for IL-13 could be detrimental in the setting of IBD by limiting the protective anti-inflammatory and pro-repair functions of type 2 immunity. Previously, we have shown that the proinflammatory drivers of IBD, TNFα and IL-17A, can reinforce their inflammatory signal by synergizing to induce the expression of IL13RA2 in fibroblasts in vitro.9 We have also previously demonstrated that Il10/Il13ra2 double knockout mice were protected from piroxicam- and Trichuris muris-induced colitis due to the broad anti-inflammatory functions of IL-13 compensating for the absence of IL-10.20 This study left several important questions unanswered. First, it prompted us to test the potential of IL-13Rα2 as a therapeutic target. Second, while IL10 and IL10R deficiencies are rare with few human cases published,35 the role of IL-13 and IL-13Rα2 in IBD pathogenesis remained unclear in an immunocompetent setting. Third, whether IL-13Rα2 was influential during active disease and/or recovery from IBD was unclear. Lastly, we sought data to link our findings in mice to IBD in humans.
With our new studies, we first found evidence that increased IL-13 activity is associated with protection against IBD in humans. We conducted a phenome-wide association study (PheWAS) on a common IL-13 gain-of-function variant. We show here that subjects carrying this variant had a significantly lower odds ratio for CD, but not UC. Next, we aimed to specify the role of IL-13Rα2 in an immune-competent mouse model that was amenable to study the relapsing and remitting characteristics of CD. We chose to use a model of colitis induced by dextran sodium sulfate (DSS)36 and followed by a recovery period. DSS causes epithelial damage that results in type 1 and type 17 immune responses, which have been associated with the pathogenesis of CD in humans.37,38 We also designed a neutralizing antibody against IL-13Rα2 to test IL-13Rα2 blockade as a novel therapeutic strategy during the recovery period of disease. Data from our murine model indicate that neutralizing IL-13Rα2 provides significant therapeutic benefit by diminishing type 1 and 17 inflammation and accelerating recovery by bolstering the endogenous bioactivity of IL-13.
Results
IL-13 gain-of-function variant is protective for CD in human subjects
The common IL-13 variant, R130Q, has increased activity compared to wild-type IL-13.39 R130Q has reduced affinity for IL-13Rα2, but it has a similar affinity for IL-13Rα1 as wild-type IL-13 does.40,41 We performed a PheWAS analysis on the 23andMe database, which contains genetic and self-reported health status information from over 600,000 subjects and evaluated the association of R130Q across a panel of immunological diseases. As expected, our results confirmed strong associations between R130Q and increased risk of allergy, asthma, and eczema (Fig. 1). The same IL-13 variant has been shown to protect against psoriasis,42 and we also found this association in our PheWAS analysis. No genome-wide association between IL-13 and IBD has been reported previously. For the first time, our results revealed a significantly lower odds ratio for CD in subjects carrying R130Q (Fig. 1). In contrast, we found no significant change in the odds ratio of UC in those subjects. Our PheWAS findings provide evidence that increased IL-13 activity is protective against the pathogenesis of human CD and also indicate that protection can be antagonized by IL-13Rα2.
Decreased Crohn’s disease risk for subjects carrying R130Q. A PheWAS analysis was performed on the 23andMe database and evaluated the effect of the R130Q IL-13 variant across a select panel of immunological diseases. Associations between the R130Q IL-13 variant and the immunological diseases are represented as the odds ratios per increase in IL-13 (R130Q) allele number (center of solid square), the number of cases (area of the square), and 95% confidence intervals (extended lines) on a forest plot. The association test p-value reported was computed using a likelihood ratio test
DSS acutely activates type 1 and type 17 pathways
We hypothesized that IL-13Rα2 contributes to CD pathogenesis by sustaining type 1 and type 17 inflammation through its ability to diminish IL-13 signaling. To test this further, we chose a mouse model of colitis induced by DSS because the model shares many characteristics with human CD.37,43,44 The pathology associated with acute DSS-induced colitis has been reported to be mediated by type 1 and type 17 immune responses that are also associated with CD.37 We first determined whether DSS induced type 1 and type 17 inflammatory pathways in our model. DSS exposure for 7 days resulted in a significant increase in the total number of leukocytes in the colonic lamina propria (Supplemental Fig. 1a), which was characterized by an influx of Ly6ChighMHCII− monocytes and CD11b+Ly6G+ neutrophils into the colonic tissue compared to untreated controls (Supplemental Fig. 1b, c). We also measured a significant increase in IFNγ+ and IL-17A+ CD4+TCRβ+ T cells isolated from the colon following 7 days of DSS administration (Supplemental Fig. 1d–f). In parallel with the T-cell data, we measured significant increases in the protein levels of the proinflammatory cytokines TNFα, IL-12p70, IL-1β, IL-6, IFNγ, and IL-17A in colon tissue after 7 days of DSS administration in wild-type mice (Supplemental Fig. 2a–f). In contrast, anti-inflammatory mediators were not increased (Supplemental Fig. 2g–j). Together, these findings support that DSS administration upregulates type 1 and 17 inflammatory mediators in the colonic tissue.
DSS-induced intestinal injury leads to increased expression of IL-13Rα2
We have previously reported that TNFα (a type 1 inflammatory mediator) and IL-17 (a type 17 inflammatory mediator) can synergistically increase IL-13Rα2 expression in both mouse and human fibroblasts in vitro.9 We next aimed to determine whether DSS induced the expression of IL-13Rα2. Wild-type mice were administered 5% DSS in drinking water for 7 days (Fig. 2a). IL-13Rα2 protein levels both in the colon homogenates and serum of wild-type mice administered DSS were significantly higher than those of untreated control mice (Fig. 2b, c). We hypothesized that the type 1 and type 17 inflammatory responses were contributing to the upregulation of IL-13Rα2 in vivo. To test this, we neutralized TNFα, IL-17A, or both TNFα and IL-17A in wild-type mice during the 7 days of DSS administration (Fig. 2d). Neutralization of only TNFα or IL-17A during DSS administration did not significantly reduce the protein levels of IL-13Rα2 in either the colon or serum (Fig. 2e, f). Neutralization of both TNFα and IL-17A significantly reduced IL-13Rα2 protein levels compared to IgG1 isotype control-treated mice. These data suggest that the proinflammatory mediators TNFα and IL-17A induced by DSS administration contribute to the expression of IL-13Rα2 protein in vivo. IL-13Rα2 levels were not decreased to levels found in naïve water-treated mice, however, indicating that other mediators also can contribute to the induction of IL-13Rα2 in the absence of IL-17A and TNFα signaling.
Increased production of IL-13Rα2 protein following DSS administration is partially dependent on TNFα and IL-17A in vivo. a Wild-type mice were administered 5% DSS drinking water or normal drinking water for 7 days. On day 7, mice were euthanized and IL-13Rα2 protein levels were measured in the b colon homogenates and c serum by ELISA. d Wild-type mice were given 5% DSS drinking water or normal drinking water for 7 days. During the induction period of DSS-colitis, groups of mice were administered two intraperitoneal injections (250 μg/mouse) of IgG1 isotype control (MOPC-21), anti-TNFα (XT22.11), anti-IL-17A (17F3), or anti-TNFα (XT22.11)/anti-IL-17A (17F3) antibodies. On day 7, mice were euthanized and IL-13Rα2 protein levels were measured in the e colon homogenates and f serum by ELISA. Experimental results are displayed showing the geometric mean. Statistical significance was determined by Student’s t test (b, c) or one-way ANOVA (e, f), where **p < 0.01, **p < 0.001, and ****p < 0.0001. Data are pooled from two independent experiments. (b, c, n = 4–10 mice/group; e, f, n = 10 mice/group)
IL-13Rα2 deficiency provides modest protection from the initiation of DSS-induced colitis
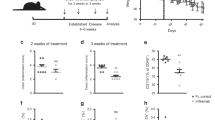
We next investigated whether the DSS-induced IL-13Rα2 expression is contributing to disease pathogenesis. Weight-matched (Supplemental Fig. 3) wild-type mice and Il13ra2−/− mice were administered 5% DSS drinking water or normal drinking water for 7 days (Fig. 3a). Wild-type mice lost a significant percentage of body weight compared to Il13ra2−/− mice after 7 days on DSS drinking water (Fig. 3b). Il13ra2−/− mice appeared markedly less hunched and scruffy compared to wild-type mice (Fig. 3c). Shortening of the colon length has been widely used as a surrogate measure for increased colon pathology in the DSS-induced colitis model.45 As expected, wild-type mice administered DSS had significantly shorter colon lengths compared to untreated wild-type control mice (Fig. 3d). Similarly, Il13ra2−/− mice administered DSS had a significant reduction in their colon lengths compared to untreated Il13ra2−/− control mice (Fig. 3d). On average, wild-type mice had roughly a 26% reduction in colon length, while Il13ra2−/− mice had a 19% reduction in colon length compared to untreated controls (Fig. 3e). DSS-administered wild-type and Il13ra2−/− mice both exhibited increased leukocyte infiltration, submucosal inflammation, and goblet cell depletion in the distal colon compared to untreated controls (Fig. 3f), in agreement with the observed shortening in colon length. While the pathology in Il13ra2−/− mice administered DSS tended to be less severe, the differences did not reach statistical significance (Fig. 3f). Although the inflammation in DSS administered Il13ra2−/− mice was not statistically different compared to wild-type controls, we measured a significant reduction in IL-17A, IL-1β, and IFNγ protein concentrations in the colon homogenates of DSS treated Il13ra2−/− mice compared to DSS administered wild-type controls (Fig. 3g–i). Together, these observations show that the absence of IL-13Rα2 results in modest protection from the initiation of DSS-induced colitis.
Il13ra2−/− mice are modestly protected from the induction of acute DSS-induced colitis. a Wild-type and Il13ra2−/− mice were administered normal drinking water or 5% DSS drinking water for 7 days. b The body weights of all mice were monitored daily. After 7 days of DSS administration, c the physical appearance was scored prior to euthanizing mice and harvesting colons. d The colon lengths were measured and e the average percent reduction in colon lengths of DSS treated mice over normal drinking water controls were calculated. Distal colon was embedded in paraffin, sectioned, and f stained with H&E and the pathology was scored. Colon homogenates were generated and protein concentrations of g IL-17A, h IL-1β, and i IFNγ were measured by multiplex assay. Experimental results are displayed as the geometric mean except (d) is represented as the mean ± S.E.M. Statistical significance was determined by one-way ANOVA, where *p < 0.05, **p < 0.01, and ****p < 0.0001. Data are pooled from two independent experiments (b–i, n = 10–20 mice per group)
Il13ra2 −/− mice recover faster from acute DSS-induced colitis
Both CD and UC are relapsing and remitting inflammatory disorders. To model this in mice, we added a 7-day recovery period. Wild-type mice and Il13ra2−/− mice were administered DSS for 7 days, after which all mice were placed on normal drinking water for an additional 7 days (Fig. 4a). Il13ra2−/− mice administered DSS lost less body weight compared to wild-type mice administered DSS mice; however, following the subsequent recovery period, no significant differences in weight loss were observed between the two groups of mice (Fig. 4b). Although Il13ra2−/− mice appeared less hunched and scruffy compared to wild-type mice (Fig. 4c). Following 7 days of recovery, wild-type mice administered DSS had significantly shorter colons compared to untreated wild-type controls (Fig. 4d). In contrast, the colon lengths of Il13ra2−/− mice administered DSS had increased to the extent that they were not statistically different from those of untreated Il13ra2−/− mice. The average percent reduction in colon length of DSS-administered wild-type mice was nearly 15%, whereas the average percent reduction in colon length of the DSS-administered Il13ra2−/− mice was ~6% (Fig. 4e). Following 7 days of recovery, leukocyte infiltration, submucosal inflammation, and goblet cell depletion were still appreciable in the colons of wild-type mice administered DSS (Fig. 4f, g). There were no significant differences in these measures between Il13ra2−/− mice administered DSS and untreated Il13ra2−/− mice following 7 days of recovery, however (Fig. 4f, g). Collectively, our findings demonstrate that Il13ra2−/− mice may recover faster from DSS-induced colitis. It is important to note that these data do not allow for a controlled comparison of the contributions of IL-13Rα2 during active disease and the recovery period. We address this uncertainty with studies using an anti-IL-13Rα2 antibody described later in Fig. 6.
The absence of IL-13Rα2 promotes tissue injury recovery following DSS-induced colitis. a Wild-type and Il13ra2−/− mice were given normal drinking water or 5% DSS drinking water for 7 days. Then all mice were administered normal drinking water for 7 days. b The body weights of mice were measured daily. On day 14, c the physical appearance of mice was scored. Then all mice were euthanized and d colon lengths were measured and e the average colon length reduction compared to untreated mice after 7 days of recovery was calculated. Distal colons were paraffin embedded, sectioned, and stained with f H&E and g the pathology was scored. Experimental results are displayed showing the geometric mean except b is represented as the mean ± S.E.M. Statistical significance was determined by one-way ANOVA, where *p < 0.05, **p < 0.01, and ****p < 0.0001. Data are pooled from three independent experiments (b, d–g, n = 10–20 mice per group; c, n = 5–10 mice per group)
Recovery of Il13ra2 −/− mice is characterized by increased type 2 immunity in the colon
We next sought to investigate the mediators of the reduced colitis in Il13ra2−/− mice following 7 days of recovery. Analogous with our histological observations, the total number of leukocytes isolated from the colonic lamina propria of Il13ra2−/− mice was significantly lower than the number isolated from wild-type mice (Fig. 5a). Amongst those leukocytes, we observed an increase in both the frequency and total number of CD11b+Siglec-F+ eosinophils in the colonic lamina propria of Il13ra2−/− mice compared to wild-type mice after 7 days of recovery (Supplemental Fig. 4a and Fig. 5b). The frequency and total number of CD206+CD163+ macrophages were also higher in Il13ra2−/− mice than wild-type mice (Supplemental Fig. 4b and Fig. 5c). In agreement with decreased overall inflammation in the colons of Il13ra2−/− mice, we measured a decreased frequency and total number of Ly6ChighMHCII– monocytes (Supplemental Fig. 4c and Fig. 5d). IL-13 has also been shown to induce mucus production by goblet cells.46 Colon sections were stained with alcian blue periodic acid Schiff (AB/PAS) to identify mucus and the staining intensity was quantitated. Again, in accordance with the predicted increase in type 2 signaling, following 7 days of recovery, colon tissue from Il13ra2−/− mice exhibited significantly more AB/PAS staining than colon tissue from wild-type mice (Fig. 5e).
Increased type 2 immune cells and mucus production in the colon of Il13ra2−/− mice following recovery. Wild-type and Il13ra2−/− mice were administered 5% DSS-drinking water or normal drinking water for 7 days. Then all mice were placed on normal drinking water for a 7-day recovery period. On day 14, a leukocytes from the colonic lamina propria were isolated from wild-type and Il13ra2−/− mice, and the b frequency and number of CD11b+Siglec-F+ eosinophils were determined by flow cytometry. c The frequency and total number of CD206+CD163+ macrophages were determined by flow cytometry. d The frequency and total number of Ly6C+MHCII– monocytes were determined by flow cytometry. e Colons from wild-type and Il13ra2−/− mice were stained with Alcian Blue Periodic Acid-Schiff and quantitated on day 14. On day 14, freshly isolated leukocytes from the colonic lamina propria were stimulated ex vivo with PMA (50 ng/mL)/ionomycin (500 ng/mL) for 3 h at 37 °C and f the frequency and total numbers of IL-13+ CD4+TCRβ+ T cells and g ILC2s (gated on CD90.2+CD4− cells) were determined by flow cytometry. Experimental results are displayed showing the geometric mean. Statistical significance was determined by one-way ANOVA, where *p < 0.05, **p < 0.01, ***p < 0.001, and ****p < 0.0001. Data are pooled from two independent experiments (a, n = 9–17 mice per group; b, n = 6–15 mice per group; c, n = 5–6 mice per group; d, n = 6 mice per group; e, n = 20 mice per group; f, g, n = 3–6 mice per group)
One possible consequence of unregulated IL-13 signaling in the absence of IL-13Rα2 is the development of excessive matrix deposition or fibrosis.24 To monitor for the development of fibrosis, colon sections from wild-type and Il13ra2−/− mice on days 0, 7, and 14 of our model were stained with picrosirius red (PSR), a dye that specifically binds to collagen. No significant differences in PSR quantitation were observed at any time point (Supplemental Fig. 5a). In addition, no significant changes in the gene expression of collagen genes, Tgfb1, Tgfbr1, Thbs1, or Thbs4, were observed (Supplemental Fig. 5b–j). These results reveal that despite the increased type 2 immune environment in Il13ra2−/− mice, tissue healing did not result in excess scarring but rather resulted in a general decrease in proinflammatory cytokine-driven tissue injury.
Because we measured many parameters in the colonic tissue indicative of increased IL-13 signaling, we next aimed to identify which cell type was the source of IL-13 in the colon during recovery. After 7 days of recovery, we detected a similar increase in the frequency and total number of IL-13-producing CD4+TCRβ+ T cells in both wild-type and Il13ra2−/− mice compared to naive controls (Fig. 5f). ILC2s produced some IL-13 at baseline, but the frequency and total number of IL-13+ ILC2s remained unchanged after DSS administration and recovery in both strains (Fig. 5g).
Therapeutic blockade of IL-13Rα2 during the recovery period accelerates recovery from acute colitis pathogenesis
While it was evident that IL-13Rα2 ablation in Il13ra2−/− mice ameliorated DSS-induced IBD, it remained unclear whether this phenotype was due to the slightly less severe induction of DSS-colitis or if IL-13Rα2 hindered recovery from DSS-induced colitis. To specifically address this, we targeted IL-13Rα2 in wild-type mice only during the recovery period. We designed a neutralizing antibody specific for murine IL-13Rα2 (Supplemental Fig. 6a) and not IL-13Rα1 (Supplemental Fig. 6b) that blocks the binding of IL-13 to IL-13Rα2 (Supplemental Fig. 6c, d). Groups of wild-type mice were administered DSS for 7 days followed by 7 days of recovery. On days 7 and 11, groups of mice were administered anti-IL-13Rα2 or IgG1 isotype control by intraperitoneal injection (Fig. 6a). In addition, one group of mice received anti-TNFα. Lastly, one group of mice was administered a combination of anti-IL-13Rα2/anti-TNFα. Mice receiving anti-IL-13Rα2 or the anti-IL-13Rα2/anti-TNFα combination therapy rapidly gained weight after the start of therapy (Fig. 6b, c). Mice that received anti-TNFα gradually recovered body weight, but never gained as much weight as the mice receiving anti-IL-13Rα2 or anti-IL-13Rα2/anti-TNFα. On day 14, mice were euthanized and colon lengths were measured. Mice administered anti-TNFα, anti-IL-13Rα2, or anti-IL-13Rα2/anti-TNFα had significantly longer colon lengths compared to IgG1 isotype control treated mice (Fig. 6d). All three treatment groups also had significantly lower colon pathology scores compared to IgG1 isotype control-treated controls (Fig. 6e). In parallel with decreased colonic inflammation, mice treated with anti-IL-13Rα2 had significantly lower colonic protein levels of TNFα, IL-6, IL-12p70, and IL-17A compared to IgG1 isotype treated control mice (Supplemental Fig. 7a–d). The pathology scores of mice treated with anti-TNFα were higher than the groups treated with anti-IL-13Rα2 or anti-IL-13Rα2/anti-TNFα. Wild-type mice administered anti-IL-13Rα2 during the recovery period of one cycle or two cycles of DSS (Supplemental Fig. 8a) were not more susceptible to fibrosis than wild-type mice administered the IgG1 isotype control (Supplemental Fig. 8b, c). Taken together, these results demonstrate that neutralizing IL-13Rα2 with an antibody only during recovery from DSS-induced colitis accelerates recovery. Furthermore, it accelerates recovery at least as well or better than anti-TNFα.
Therapeutic blockade of IL-13Rα2 promotes recovery from colitis. Wild-type mice were administered 5% DSS-drinking water or normal drinking water for 7 days. Then all mice were placed on normal drinking water for 7 days. a On days 7 and 11, mice were administered 250 μg/mouse of anti-TNFα, anti-IL-13Rα2, or both anti-TNFα/anti-IL-13Rα2. Mice were assessed for disease severity by b monitoring body weight daily, c relative change in body weight compared to water controls 24 h post injection, d length of the colon and the average percent reduction in colon length. Distal colons were stained with e H&E and the pathology was scored. Experimental results are represented as the geometric mean. Statistical significance was determined by one-way ANOVA, where **p < 0.01 and ****p < 0.0001. Data are pooled from two independent experiments (n = 20 mice per group)
Anti-IL-13Rα2-mediated accelerated recovery is both IL-13- and eosinophil-dependent
While we found that neutralizing IL-13Rα2 during recovery improves outcomes, it remained uncertain to what degree IL-13 was responsible for the improvement. To test this, wild-type mice that had been administered DSS were treated with anti-IL-13Rα2, anti-IL-13Rα2/anti-IL-13, or an IgG1 isotype control antibody during the recovery week (Fig. 7a). Wild-type mice administered DSS and then anti-IL-13Rα2 regained body weight comparable to untreated control mice, while wild-type mice administered DSS and neutralized of IL-13 failed to regain body weight to the levels of mice that did not receive DSS (Fig. 7b). Wild-type mice with neutralized IL-13 had significantly shorter colon lengths compared to mice administered only anti-IL-13Rα2 (Fig. 7c). The average percent reduction in colon lengths of mice treated with IgG1, anti-IL-13Rα2, or anti-IL-13Rα2/anti-IL-13 were 22%, 11%, and 21%, respectively (Fig. 7d). The colon histology score of mice depleted of IL-13 were comparable to the IgG1 control groups, while the anti-IL-13Rα2 administered group had lower histology scores (Fig. 7e, f). Together, these data confirm that the accelerated recovery from anti-IL-13Rα2 treatment is dependent on IL-13. We observed that the frequency and total number of eosinophils were higher in the colons of Il13ra2−/− mice compared to wild-type mice that did not recover as quickly from DSS-induced colitis (Fig. 5b). To test if eosinophils are important for anti-IL-13Rα2-mediated recovery, we treated wild-type mice with anti-IL-13Rα2 and anti-IL-5 to deplete eosinophils during the 7-day recovery period to effectively deplete eosinophils (Supplemental Fig. 9a, b). Wild-type mice that were depleted of eosinophils during anti-IL-13Rα2 treatment failed to improve their colon lengths unlike those with intact eosinophils (Supplemental Fig. 9c). Eosinophil depletion completely eliminated the improved pathology score found in the colons of anti- IL-13Rα2 treated mice with intact eosinophils (Supplemental Fig. 9d). These results demonstrate that eosinophils play a critical role in anti-IL-13Rα2-mediated recovery along with IL-13.
Recovery from acute DSS-induced colitis is mediated by IL-13. Wild-type mice were administered 5% DSS drinking water or normal drinking water for days. Then all mice were placed on normal drinking water for a 7-day recovery period. a On days 7 and 11, mice were administered 250 μg/mouse of anti-IL-13Rα2, anti-IL-13Rα2/anti-IL-13, or IgG1 isotype control. b Body weights of mice were recorded daily throughout the induction and recovery periods. Mice were euthanized on day 14 and c colons were harvested and the lengths were measured. d The average percent reduction in colon length were calculated. Distal colons were stained with e H&E and the pathology was f scored. Experimental results are represented as the geometric mean. Statistical significance was determined by one-way ANOVA, where *p < 0.05, **p < 0.01, and ****p < 0.0001. Data are pooled from two independent experiments (n = 5–10 mice per group)
Discussion
Despite a number of recent studies of IL-13 in IBD, the role of IL-13 remains unclear and the findings so far indicate its role may vary in different diseases and different stages of disease. There is evidence that the character of the inflammatory response changes over the course of IBD. Type 1 and type 17 immune responses are known to be involved in the induction of CD colitis,47,48 while type 2 cytokines have been associated with tissue remodeling and more chronic fibrotic pathology.30,31 Kugathasan et al. found that a strong type 1 immune profile exhibited by the gut mucosa of CD patients experiencing their first symptoms shifts to a more type 2 polarized milieu in patients with long-standing disease.49 These kinetics align with established roles for IL-13 as anti-inflammatory and pro-tissue repair.23 In contrast, type 2 cytokines like IL-13 have been associated with the pathogenesis of UC.27,50 However, clinical trials of anti-IL-13 monoclonal antibodies anrukinzumab and tralokinumab did not show improved outcomes of patients with active UC.28,29 Given the varied patterns of immune pathway activation, perhaps it is not surprising that another study could not detect different levels of IL-13 production by mucosal explants and activated lamina propria mononuclear cells between CD, UC, and control subjects.51 Collectively, the recent data indicate that immunoregulation during CD and UC is more heterogenous than simply type 1/type 17 polarized and type 2 polarized, respectively.
Analysis of immune modulation during the DSS-induced model of colitis revealed a similar pattern to the one found in early and long-term CD.37 Type 1 and type 17 cytokines were strongly upregulated during the development of acute DSS-induced colitis, and a type 2 response was strongly upregulated later during periods of recovery from injury or during more chronic disease. These kinetics supports our hypothesis that type 2 signaling is detrimentally low when type 1 and type 17 inflammation drives DSS-induced colitis and human CD. The findings also suggest that IL-13Rα2 neutralization may be most effective during recovery because IL-13 is more highly expressed during that period.
Wang et al. have also demonstrated that the IL-13 that is expressed during active DSS-induced colitis does mitigate disease.52 They found IL-13-deficient mice to be moderately more susceptible to DSS-induced colitis at least in part due to increased type 1 and type 17 cytokines. This result parallels our observation that ablating IL-13Rα2 during active disease further mitigates disease, albeit moderately, by incrementally increasing IL-13 signaling above the amount found in wild-type mice. It is important to note that IL-13 is not protective in all settings, however. Targeting IL-13 reduced the severity of murine oxazolone-induced colitis, a model that more closely resembles UC.26,53 Mice overexpressing GATA-3 and type 2 cytokines exhibited worse disease in a DSS-colitis model.54,55 These findings emphasize that too much type 2 inflammation is also detrimental and that balancing IL-13 and type 2 immunity is essential for managing IBD. As we show in our model, exploiting the ability of IL-13Rα2 to be a rheostat for IL-13 provides a powerful therapeutic tool. Achieving the best outcomes requires finding the right balance of type 1, type 17, and type 2 immune responses.
Elevated expression of IL13RA2 has been previously identified in patients suffering from IBD, and its expression is highly upregulated in patients who do not respond to the current standard therapy, anti-TNFα.4,5 IL-13Rα2 has yet to be tested as a therapeutic target and questions remained about how and when IL-13Rα2 promotes IBD. Using a murine model of DSS-induced colitis, we provide evidence that IL-13Rα2 slows the recovery from IBD by limiting the anti-inflammatory functions of IL-13. We also find that therapeutic neutralization of IL-13Rα2 using a novel anti-IL-13Rα2 mAb accelerates recovery from DSS-induced colitis and demonstrate that enhanced IL-13-mediated signaling is responsible for the improvement.
The DSS-induced model has been well characterized.43 We preferred it to other murine models for several reasons. First, it can be used in immunocompetent mice. Second, its acute proinflammatory immune profile is consistent with that found in CD.37 Third, while it causes inflammation limited to the colon similarly to human UC, the inflammation is transmural similar to CD.44 Lastly, by taking the mice off of DSS and administering water for a period, we could model the injury and recovery periods seen in human disease. This allowed us to interrogate the role of IL-13Rα2 during both periods of disease.
The initiation of DSS-induced colitis is characterized by robust production of type 1 and type 17 proinflammatory mediators,37 which we have previously shown to induce the expression of IL-13Rα2 in vitro.9 We demonstrated that administration of drinking water with 5% DSS induces production of colonic and systemic IL-13Rα2 protein. The increased murine IL-13Rα2 production is consistent with human data showing increased expression of IL13RA2 in inflamed colon tissue of IBD patients.4,5 We found that the upregulation of IL-13Rα2 following 7 days of DSS administration is at least partly dependent on type 1 and type 17 mediators as neutralization of TNFα and IL-17A significantly reduced the protein concentrations of both colonic and systemic IL-13Rα2. Neutralization of TNFα and IL-17A did not reduce IL-13Rα2 to levels found in naïve controls, suggesting that other proinflammatory mediators induce IL-13Rα2 production in the absence of TNFα and IL-17A signaling during inflammation in vivo. Neutralizing TNFα alone did not reduce colonic or serum IL-13Rα2 protein levels. This suggests that repair and recovery that we observed in the colons of mice administered anti-TNFα/anti-IL-13Rα2 is due to the increased activity of IL-13 when IL-13Rα2 is neutralized, rather than anti-TNFα reducing the amount of IL-13Rα2 protein in the colon.
We next aimed to investigate the role of IL-13Rα2 in DSS-induced colitis. While both Il13ra2−/− and wild-type mice administered DSS had a significant reduction in their colon lengths and extensive colonic inflammation, mice in which IL-13Rα2 was ablated were modestly protected from disease induction compared to wild-type controls. Il13ra2−/− mice showed significantly accelerated improvement when an additional 7-day recovery period was added, suggesting that IL-13Rα2 plays a prominent role in recovery after tissue injury. Another recently published study also drew this conclusion.56 Verstockt et al. found that IL-13Rα2 ablation did not significantly ameliorate pathology during the induction of colitis by DSS. Three days after removing DSS, Il13ra2−/− mice observed decreased inflammation and promoted goblet cell regeneration.56 While these findings suggested that IL-13Rα2 ablation was more effective during recovery than active disease, they did not allow for a controlled comparison of the respective contributions of IL-13Rα2 during active disease and recovery. To address this, we neutralized IL-13Rα2 with an antibody during only the recovery phase. The results confirmed that IL-13Rα2 neutralization promotes tissue recovery. Our data support that abrogating IL-13Rα2 during the induction period of DSS-induced colitis is less effective at preventing the severity of colitis because of the low levels of IL-13 that are induced compared to untreated control mice. Previous studies of the immune kinetics of DSS-induced colitis and human CD have demonstrated that the immune response shifts from that proinflammatory milieu during pathogenesis toward an anti-inflammatory and pro-wound healing milieu.37,49 This is likely particularly true after DSS is removed and severe tissue injury has already occurred. In this environment, type 2 cytokines like IL-13 potently contribute to tissue remodeling.23,32,33,34,37
We also investigated the mechanisms that contributed to the decreased colonic inflammation in Il13ra2−/− mice. We observed many parameters indicative of increased IL-13 activity, including increased mucus production in colon tissue of Il13ra2−/− mice compared to wild-type mice after the recovery period. Eosinophils have been shown to be both pathogenic and protective in the induction of DSS-induced colitis.57,58 We identified an increase in the frequency and total number of eosinophils in the rapidly recovering colons of Il13ra2−/− mice. In this setting, eosinophils can suppress type 1 and type 17 inflammation by polarizing T cells toward a TH2 phenotype, reducing neutrophilia, boosting immune tolerance, and secreting IL-13.58,59,60 In addition, eosinophils have been shown to have a proregenerative function following liver injury and play an anti-inflammatory role in a mouse model of arthritis.51,61,62 Our findings support a critical repair function of eosinophils during the recovery from DSS-induced colitis, as mice depleted of eosinophils specifically during anti-IL-13Rα2-mediated recovery failed to resolve colonic inflammation. Eosinophils can suppress type 1 inflammatory responses, restrict bacteria-induced gut inflammation,63 and stimulate fibrogenic progenitors to promote muscle regeneration.64 We also identified elevated frequency and total numbers of macrophages expressing both CD206 and CD163. CD206 and CD163 are scavenger receptors for mannose found on the surface of microorganisms and hemoglobin-haptoglobin complexes, respectively.65,66 The upregulation of scavenger receptors specific for inflammatory stimuli correlates with decreased inflammation in and quicker recovery observed in the Il13ra2−/− mice.
To date, genome-wide association studies have associated many genetic loci with IBD;67 however, the association of IL-13 with IBD at genome-wide significance has not been reported. The R130Q IL-13 gain-of-function variant has reduced affinity for IL-13Rα2 because of the substitution of a glutamine residue at position 130 located in the D α-helix.39 Alanine scanning experiments have demonstrated that this substitution is important for IL-13 binding to IL-13Rα2.68 R130Q is also the causal variant for positive associations with asthma and psoriasis. We rationalized that the R130Q IL-13 served as the best genetic tool to analyze the association of IL-13 and IL-13Rα2 with IBD. Increased IL-13 activity in human subjects had no association with the occurrence of UC. We found this surprising given the previous reports connecting IL-13 with UC pathogenesis. As we discussed above, however, anti-IL-13 therapy recently failed to improve outcomes in a clinical trial of UC patients. The size of our PheWAS cohort adds to the mounting evidence that the pathogenesis of UC may be more immunologically heterogenous than originally thought. On the other hand, our PheWAS analysis provided perhaps the strongest evidence to date that increased IL-13 activity is protective against CD pathogenesis. R130Q likely has a greater propensity to downregulate type 1 and type 17 inflammation and promote tissue remodeling because less of it is bound to IL-13Rα2 than unmutated IL-13. Our PheWAS findings also support our observations in mice. In both cases, increased IL-13 activity is protective against colitis resembling CD.
Our final experiments were intended to confirm that IL-13 activity was also responsible for the therapeutic effects in the mouse model. In contrast to the rapid recovery observed in animals treated with anti-IL-13Rα2, mice treated with anti-IL-13Rα2 in combination with anti-IL-13 to neutralize IL-13 during the recovery period failed to regain their body weight and had comparable colon lengths and colonic inflammation as IgG1 isotype control treated mice. These findings also provide strong evidence that targeting IL-13 as a therapy for CD could be problematic. In contrast, the data show that IL-13 plays a protective role by promoting broad anti-inflammatory activity during the recovery period.
In this study, we provide compelling evidence that the increased production of IL-13Rα2 during type 1/type 17 colitis plays a pathogenic role by impeding IL-13-mediated recovery. Our results argue that targeting IL-13Rα2 to bolster endogenous IL-13 bioactivity could represent a highly efficacious therapy to promote resolution of IBD-mediated damage and may be especially useful as an alternative therapy for patients who have failed or developed resistance to anti-TNFα agents.
Methods
Human subjects
All research participants included in the phenome-wide association analyses provided informed consent and answered surveys online according to 23andMe’s human subjects protocol, which was reviewed and approved by Ethical & Independent Review Services, a private institutional review board (http://www.eandireview.com).
Phenome-wide association study
A phenome-wide association analysis of the European 23andMe cohort of the SNP, rs20541, the genetic polymorphism of the IL-13 R130Q variant, was performed. The association was conducted for disease case control endpoints via logistic regression, assuming additive allelic effects, and included covariates for age, gender, and the top four principal components to account for residual population structure. The association test p-value we report was computed using a likelihood ratio test.
Mice
Age and weight-matched female wild-type and Il13ra2−/− mice on a BALB/c genetic background between the ages of 8 and 12 weeks were used in experiments and purchased from Taconic Biosciences. Some studies were repeated in males to confirm that there were no gender biases. Mice were housed under specific pathogen-free conditions at the National Institutes of Health in an Association for Assessment and Accreditation of Laboratory Animal Care approved facility. The National Institute of Allergy and Infectious Diseases Animal Care and Use Committee approved all experimental procedures.
DSS-induced colitis
Acute colitis was induced by 5% (w/v) DSS (MW 40,000–50,000 Da; Alfa Aesar) added to drinking water. The 5% dose of DSS was chosen based on the genetic background of the mice used in our studies, and the cleanliness of our housing facility. Mice were left on DSS water for 7 days and then were placed on normal drinking water for 7 days. Colitis severity was determined by measuring body weight and colon length. Alternatively, mice were subjected to 5% DSS drinking water for 7 days, followed by 7 days on normal drinking water for two cycles.
Antibody administration
Mice were injected intraperitoneally with 250 μg/mouse of anti-IL-17A (17F3), anti-TNFα (XT22.11), or IgG1 isotype control (MOPC-21) on days 0 and 4. For studies where antibodies were administered during the recovery, mice were injected intraperitoneally with 250 μg/mouse of anti-IL-13Rα2 (6D5), anti-TNFα (XT22.11), anti-IL-13Rα2 (6D5)/anti-TNFα (XT22.11), anti-IL-13Rα2 (6D5)/anti-IL-13 (262A-5-1), anti-IL-13Rα2 (6D5)/anti-IL-5 (TRFK5), or IgG1 isotype control (HPRN) on day 7, 11, 21, or 25.
Physical appearance
For physical appearance, mice were scored on the following three-point scale: 0 is equal to normal; 1 is a scruffy appearance; 2 is a scruffy and hunched appearance; and 3 is a scruffy, hunched appearance with no motility.
Histopathology
For histopathological analysis, distal colons were flushed with 1× phosphate-buffered saline and a 6 mm piece of distal colon was harvested, fixed in 10% phosphate-buffered formalin, and embedded in paraffin. Five micrometers sections were cut and stained with hematoxylin and eosin (H&E) and PSR, and counterstained with fast green or ABPAS. Sections were scored by a blinded scorer based on goblet cell depletion, leukocyte infiltration, and submucosal inflammation on a point scale of 0–3, where 0 is no pathology and 3 is the most severe pathology.
Histological quantification
Slides stained with ABPAS or PSR with fast green counterstain were digitized using an Aperio Scanscope® CS system. The percentage of total area positive for ABPAS or PSR was quantitated using the Aperio ImageScope Positive Pixel Count v9 algorithm. Positive pixel area percentages were exported to GraphPad Prism 7 for statistical analyses.
Colon lysates
Preweighed colons were placed into a Precellys tubes containing 500 μL radioimmunoprecipitation assay buffer with protease inhibitor. Tissues were homogenized using a Precellys homogenizer and centrifuged at 10,000 RPM for 10 min at 4 °C. Colon lysate supernatants were frozen at −80 °C until used.
IL-13Rα2 ELISA
Colonic and systemic IL-13Rα2 protein concentrations were determined by ELISA assay as previously described.69 High protein binding 96-well plates were coated with anti-IL-13Rα2 (1 μg/mL; R&D) in PBS overnight and a biotinylated anti-mouse IL-13 (2 μg/mL; Centocor) was used for detection.
Luminex analysis of cytokine expression
TNFα, IL-12p70, IL-1β, IL-6, IFNγ, IL-17A, IL-13, IL-4, IL-10, and IL-5 cytokine concentrations in the colon homogenates were determined using an enzyme-linked immunosorbent assay using the MILLIPLEX MAP Mouse TH17 Magnetic Bead Panel (Millipore Sigma) according to the manufacture’s protocol. Analytes were read using a Bio-Rad Bio-Plex 200 system. Concentrations of cytokines were determined by standard curve using recombinant proteins.
RNA capture and purification
Colons were harvested and placed in a Precellys tube containing 500 μL Trizol. Tissues were then homogenized using a Precellys homogenizer. RNA capture and purification were performed using MagMAX-96 Total RNA Isolation Kit (Thermo Fisher). RNA concentration (ng/μL) was determined using a DeNovix DS-11 Spectrophotometer.
RNA expression profiling
Preparation, hybridization, and detection of RNA samples were carried out by following Nanostring manufacturer’s instructions (Nanostring Technologies). Subsequent analyses were performed using nCounter Analysis System and TM4 MeV microarray software suite.
Isolation of colonic lamina propria leukocytes
Murine colonic lamina propria leukocytes were isolated as previously described.70
Intracellular cytokine staining
Lymphocytes isolated from the colonic lamina propria were restimulated ex vivo with PMA (50 ng/mL) and ionomycin (500 ng/mL) in the presence of brefeldin A for 3 h at 37 °C. Cells were then stained with fluorescently labeled antibodies for surface antigens, followed by permeabilization with Cytofix/Cytoperm (BD), and stained for intracellular cytokines in Perm/Wash (BD).
Antibodies and FACS analysis
Fluorescently labeled antibodies purchased from eBioscience (Waltham, MA) include the following: TCRβ (biotin; 1:200), TCRγδ (biotin; 1:200), CD19 (biotin; 1:200), TCRβ (H57-597; 1:200), CD19 (eBio1D3; 1:200), TCRγδ (EbioGL3; 1:200), CD45.2 (104; 1:400), CD163 (TNKUPJ; 1:100), and IFNγ (XMG1.2; 1:100). Antibodies purchased from Biolegend (San Diego, CA) include the following: CD16/CD32 (93; 1:500), Streptavidin, CD11b (M1/70; 1:500), F4/80 (BM8; 1:200), CD206 (CO68C2; 1:200), and IL-17A (TC11-18H10.1, 1:100). Antibodies purchased from BD Pharmingen (Billerica, MA) include the following: Siglec-F (E50-2440; 1:800), CD64 (X54-5/7.1; 1:200), and CD4 (RM4.5; 1:200). Antibodies purchased from Life Technologies (Washington, DC) include the following: LIVE/DEAD Fixable Blue Viability Dye (1:500). Cells were collected on an LSR Fortessa I flow cytometer equipped with FACSDIVA (BD Biosciences) software and data were analyzed with FlowJo software (Tree Star, Ashland, OR).
Statistical analysis
Experimental results are represented as mean ± standard error or geometric mean. Statistical differences were determined by using Mann–Whitney, two-tailed Student t test, or one-way ANOVA. For both statistical tests, a p-value< 0.05 was deemed statistically significant. Graphing and statistical analysis were performed using GraphPad Prism 7 software. *p < 0.05, **p < 0.01, ***p < 0.001, and ****p < 0.0001; ns denotes not significant. Data are pooled from 2–3 independent experiments.
References
Lee, J. M. & Lee, K. M. Endoscopic diagnosis and differentiation of inflammatory bowel disease. Clin. Endosc. 49, 370–375 (2016).
Loftus, E. V. Jr. Clinical epidemiology of inflammatory bowel disease: incidence, prevalence, and environmental influences. Gastroenterology 126, 1504–1517 (2004).
Rubbert-Roth, A. & Finckh, A. Treatment options in patients with rheumatoid arthritis failing initial TNF inhibitor therapy: a critical review. Arthritis Res. Ther. 11(Suppl. 1), S1 (2009).
Arijs, I. et al. Mucosal gene signatures to predict response to infliximab in patients with ulcerative colitis. Gut 58, 1612–1619 (2009).
Arijs, I. et al. Predictive value of epithelial gene expression profiles for response to infliximab in Crohn’s disease. Inflamm. Bowel Dis. 16, 2090–2098 (2010).
Lupardus, P. J., Birnbaum, M. E. & Garcia, K. C. Molecular basis for shared cytokine recognition revealed in the structure of an unusually high affinity complex between IL-13 and IL-13Ralpha2. Structure 18, 332–342 (2010).
Chandriani, S. et al. Endogenously expressed IL-13Ralpha2 attenuates IL-13-mediated responses but does not activate signaling in human lung fibroblasts. J. Immunol. 193, 111–119 (2014).
Kawakami, K., Taguchi, J., Murata, T. & Puri, R. K. The interleukin-13 receptor alpha2 chain: an essential component for binding and internalization but not for interleukin-13-induced signal transduction through the STAT6 pathway. Blood 97, 2673–2679 (2001).
Badalyan, V. et al. TNF-alpha/IL-17 synergy inhibits IL-13 bioactivity via IL-13Ralpha2 induction. J. Allergy Clin. Immunol. 134, 975–978 (2014). e975.
Yasunaga, S. et al. The negative-feedback regulation of the IL-13 signal by the IL-13 receptor alpha2 chain in bronchial epithelial cells. Cytokine 24, 293–303 (2003).
Mentink-Kane, M. M. & Wynn, T. A. Opposing roles for IL-13 and IL-13 receptor alpha 2 in health and disease. Immunol. Rev. 202, 191–202 (2004).
Chiaramonte, M. G. et al. Regulation and function of the interleukin 13 receptor alpha 2 during a T helper cell type 2-dominant immune response. J. Exp. Med. 197, 687–701 (2003).
Andrews, A. L. et al. IL-13 receptor alpha 2: a regulator of IL-13 and IL-4 signal transduction in primary human fibroblasts. J. Allergy Clin. Immunol. 118, 858–865 (2006).
Feng, N. et al. The interleukin-4/interleukin-13 receptor of human synovial fibroblasts: overexpression of the nonsignaling interleukin-13 receptor alpha2. Lab. Investig. 78, 591–602 (1998).
Fichtner-Feigl, S., Strober, W., Kawakami, K., Puri, R. K. & Kitani, A. IL-13 signaling through the IL-13alpha2 receptor is involved in induction of TGF-beta1 production and fibrosis. Nat. Med. 12, 99–106 (2006).
Rahaman, S. O., Vogelbaum, M. A. & Haque, S. J. Aberrant Stat3 signaling by interleukin-4 in malignant glioma cells: involvement of IL-13Ralpha2. Cancer Res. 65, 2956–2963 (2005).
Wynn, T. A. IL-13 effector functions. Annu. Rev. Immunol. 21, 425–456 (2003).
Andrews, A. L., Holloway, J. W., Puddicombe, S. M., Holgate, S. T. & Davies, D. E. Kinetic analysis of the interleukin-13 receptor complex. J. Biol. Chem. 277, 46073–46078 (2002).
Wilson, M. S. et al. IL-13Ralpha2 and IL-10 coordinately suppress airway inflammation, airway-hyperreactivity, and fibrosis in mice. J. Clin. Investig. 117, 2941–2951 (2007).
Wilson, M. S. et al. Colitis and intestinal inflammation in IL10-/- mice results from IL-13Ralpha2-mediated attenuation of IL-13 activity. Gastroenterology 140, 254–264 (2011).
Tabata, Y. & Khurana Hershey, G. K. IL-13 receptor isoforms: breaking through the complexity. Curr. Allergy Asthma Rep. 7, 338–345 (2007).
Abbas, A. K., Murphy, K. M. & Sher, A. Functional diversity of helper T lymphocytes. Nature 383, 787–793 (1996).
Wynn, T. A. Type 2 cytokines: mechanisms and therapeutic strategies. Nat. Rev. Immunol. 15, 271–282 (2015).
Gieseck, R. L. 3rd et al. Interleukin-13 activates distinct cellular pathways leading to ductular reaction, steatosis, and fibrosis. Immunity 45, 145–158 (2016).
Gieseck, R. L. 3rd, Wilson, M. S. & Wynn, T. A. Type 2 immunity in tissue repair and fibrosis. Nat. Rev. Immunol. 18, 62–76 (2018).
Heller, F., Fuss, I. J., Nieuwenhuis, E. E., Blumberg, R. S. & Strober, W. Oxazolone colitis, a Th2 colitis model resembling ulcerative colitis, is mediated by IL-13-producing NK-T cells. Immunity 17, 629–638 (2002).
Fuss, I. J. et al. Nonclassical CD1d-restricted NK T cells that produce IL-13 characterize an atypical Th2 response in ulcerative colitis. J. Clin. Investig. 113, 1490–1497 (2004).
Reinisch, W. et al. Anrukinzumab, an anti-interleukin 13 monoclonal antibody, in active UC: efficacy and safety from a phase IIa randomised multicentre study. Gut 64, 894–900 (2015).
Danese, S. et al. Tralokinumab for moderate-to-severe UC: a randomised, double-blind, placebo-controlled, phase IIa study. Gut 64, 243–249 (2015).
Scharl, M. et al. Interleukin-13 and transforming growth factor beta synergise in the pathogenesis of human intestinal fistulae. Gut 62, 63–72 (2013).
Curciarello, R., Docena, G. H. & MacDonald, T. T. The role of cytokines in the fibrotic responses in Crohn’s disease. Front. Med. (Lausanne) 4, 126 (2017).
Dalessandri, T., Crawford, G., Hayes, M., Castro Seoane, R. & Strid, J. IL-13 from intraepithelial lymphocytes regulates tissue homeostasis and protects against carcinogenesis in the skin. Nat. Commun. 7, 12080 (2016).
Bosurgi, L. et al. Macrophage function in tissue repair and remodeling requires IL-4 or IL-13 with apoptotic cells. Science 356, 1072–1076 (2017).
Gause, W. C., Wynn, T. A. & Allen, J. E. Type 2 immunity and wound healing: evolutionary refinement of adaptive immunity by helminths. Nat. Rev. Immunol. 13, 607–614 (2013).
Glocker, E. O. et al. Inflammatory bowel disease and mutations affecting the interleukin-10 receptor. N. Engl. J. Med. 361, 2033–2045 (2009).
Okayasu, I. et al. A novel method in the induction of reliable experimental acute and chronic ulcerative colitis in mice. Gastroenterology 98, 694–702 (1990).
Alex, P. et al. Distinct cytokine patterns identified from multiplex profiles of murine DSS and TNBS-induced colitis. Inflamm. Bowel Dis. 15, 341–352 (2009).
Siakavellas, S. I. & Bamias, G. Role of the IL-23/IL-17 axis in Crohn’s disease. Discov. Med. 14, 253–262 (2012).
Vladich, F. D. et al. IL-13 R130Q, a common variant associated with allergy and asthma, enhances effector mechanisms essential for human allergic inflammation. J. Clin. Investig. 115, 747–754 (2005).
Yoshida, Y. et al. Analysis of internal motions of interleukin-13 variant associated with severe bronchial asthma using (15)N NMR relaxation measurements. Biochem. Biophys. Res. Commun. 358, 292–297 (2007).
Lacy, E. R. Equilibrium and kinetic analysis of human interleukin-13 and IL-13 receptor alpha-2 complex formation. J. Mol. Recognit. 25, 184–191 (2012).
Lee, Y. H., Choi, S. J., Ji, J. D. & Song, G. G. Genome-wide pathway analysis of a genome-wide association study on psoriasis and Behcet’s disease. Mol. Biol. Rep. 39, 5953–5959 (2012).
Wirtz, S. et al. Chemically induced mouse models of acute and chronic intestinal inflammation. Nat. Protoc. 12, 1295–1309 (2017).
Melgar, S. et al. Validation of murine dextran sulfate sodium-induced colitis using four therapeutic agents for human inflammatory bowel disease. Int. Immunopharmacol. 8, 836–844 (2008).
Chassaing, B., Aitken, J. D., Malleshappa, M. & Vijay-Kumar, M. Dextran sulfate sodium (DSS)-induced colitis in mice. Curr. Protoc. Immunol. 104, 25 (2014). Unit 15.
Birchenough, G. M., Johansson, M. E., Gustafsson, J. K., Bergstrom, J. H. & Hansson, G. C. New developments in goblet cell mucus secretion and function. Mucosal Immunol. 8, 712–719 (2015).
Fuss, I. J. et al. Disparate CD4+ lamina propria (LP) lymphokine secretion profiles in inflammatory bowel disease. Crohn’s disease LP cells manifest increased secretion of IFN-gamma, whereas ulcerative colitis LP cells manifest increased secretion of IL-5. J. Immunol. 157, 1261–1270 (1996).
Fujino, S. et al. Increased expression of interleukin 17 in inflammatory bowel disease. Gut 52, 65–70 (2003).
Kugathasan, S. et al. Mucosal T-cell immunoregulation varies in early and late inflammatory bowel disease. Gut 56, 1696–1705 (2007).
Heller, F. et al. Interleukin-13 is the key effector Th2 cytokine in ulcerative colitis that affects epithelial tight junctions, apoptosis, and cell restitution. Gastroenterology 129, 550–564 (2005).
Biancheri, P. et al. Absence of a role for interleukin-13 in inflammatory bowel disease. Eur. J. Immunol. 44, 370–385 (2014).
Wang, A. J. et al. Genetic deletion of IL-25 (IL-17E) confers resistance to dextran sulfate sodium-induced colitis in mice. Cell Biosci. 4, 72 (2014).
Kasaian, M. T. et al. Therapeutic activity of an interleukin-4/interleukin-13 dual antagonist on oxazolone-induced colitis in mice. Immunology 143, 416–427 (2014).
Okamura, M., Yoh, K., Ojima, M., Morito, N. & Takahashi, S. Overexpression of GATA-3 in T cells accelerates dextran sulfate sodium-induced colitis. Exp. Anim. 63, 133–140 (2014).
Zhu, J. et al. IL-33 aggravates DSS-induced acute colitis in mouse colon lamina propria by enhancing Th2 cell responses. Mediat. Inflamm. 2015, 913041 (2015).
Verstockt, B. et al. Effects of epithelial IL-13Rα2 expression in inflammatory bowel disease. Front. Immunol. 9, 2983 (2018).
Ahrens, R. et al. Intestinal macrophage/epithelial cell-derived CCL11/eotaxin-1 mediates eosinophil recruitment and function in pediatric ulcerative colitis. J. Immunol. 181, 7390–7399 (2008).
Masterson, J. C. et al. Eosinophil-mediated signalling attenuates inflammatory responses in experimental colitis. Gut 64, 1236–1247 (2015).
Jacobsen, E. A. et al. Allergic pulmonary inflammation in mice is dependent on eosinophil-induced recruitment of effector T cells. J. Exp. Med. 205, 699–710 (2008).
Odemuyiwa, S. O. et al. Cutting edge: human eosinophils regulate T cell subset selection through indoleamine 2,3-dioxygenase. J. Immunol. 173, 5909–5913 (2004).
Yao, Y. et al. Increased expression of TIPE2 in alternatively activated macrophages is associated with eosinophilic inflammation and disease severity in chronic rhinosinusitis with nasal polyps. Int. Forum Allergy Rhinol. 7, 963–972 (2017).
Chen, Z. et al. Th2 and eosinophil responses suppress inflammatory arthritis. Nat. Commun. 7, 11596 (2016).
Arnold, I. C. et al. Eosinophils suppress Th1 responses and restrict bacterially induced gastrointestinal inflammation. J. Exp. Med. 215, 2055–2072 (2018).
Heredia, J. E. et al. Type 2 innate signals stimulate fibro/adipogenic progenitors to facilitate muscle regeneration. Cell 153, 376–388 (2013).
Yang, H. et al. Identification of CD163 as an antiinflammatory receptor for HMGB1-haptoglobin complexes. JCI Insight 1, pii: 126617 (2016).
Lee, S. J. et al. Mannose receptor-mediated regulation of serum glycoprotein homeostasis. Science 295, 1898–1901 (2002).
Liu, J. Z. et al. Association analyses identify 38 susceptibility loci for inflammatory bowel disease and highlight shared genetic risk across populations. Nat. Genet. 47, 979–986 (2015).
Madhankumar, A. B., Mintz, A. & Debinski, W. Alanine-scanning mutagenesis of alpha-helix D segment of interleukin-13 reveals new functionally important residues of the cytokine. J. Biol. Chem. 277, 43194–43205 (2002).
Zuo, L. et al. IL-13 induces esophageal remodeling and gene expression by an eosinophil-independent, IL-13R alpha 2-inhibited pathway. J. Immunol. 185, 660–669 (2010).
Weigmann, B. et al. Isolation and subsequent analysis of murine lamina propria mononuclear cells from colonic tissue. Nat. Protoc. 2, 2307–2311 (2007).
Acknowledgements
This project was funded and supported by the Intramural Research Program of the National Institutes of Health, National Institute of Allergy and Infectious Diseases, and Pfizer Inc. We would like to thank Elizabeth A. Connor and the CCR Genomics Core for assistance with Nanostring. We would also like to thank Patrick Lin, Sandra White, Byunghyun Kang, Tina Vaziri, Pedro Gazzinelli-Guimaraes, Bridget Donnelly, and Kevin Hart for assistance with animal work and thoughtful scientific discussion. We thank Ginger Chen for assistance with IL-13Rα2 KD experiments. Lastly, we thank the National Institute of Allergy and Infectious Diseases Veterinary Services team for animal care and weighing mice throughout the studies. Erik P. Karmele is a predoctoral student in The George Washington University-National Institutes of Health Graduate Partnerships Program. This work is presented to the above program in partial fulfillment of the requirements for the Ph.D. degree.
Members of the 23andMe Research Team
Michelle Agee (magee@23andme.com), Babak Alipanahi (bpanahi@gmail.com), Adam Auton (aauton@23andme.com), Robert K. Bell (rbell@23andme.com), Katarzyna Bryc (kbryc@23andme.com), Sarah L. Elson (selson@23andme.com), Pierre Fontanillas (pfontanillas@23andme.com), Nicholas A. Furlotte (nfurlotte@23andme.com), Karen E. Huber (kbrenneman@23andme.com), Nadia K. Litterman (nlitterman@23andme.com), Matthew H. McIntyre (mmcintyre@23andme.com), Joanna L. Mountain (joanna@23andme.com), Elizabeth S. Noblin (lnoblin@23andme.com), Carrie A.M. Northover (cnorthover@23andme.com), Steven J. Pitts (spitts@23andme.com), J. Fah Sathirapongsasuti (fsathirapongsasuti@23andme.com), Olga V. Sazonova (osazonova@23andme.com), Janie F. Shelton (jshelton@23andme.com), Suyash Shringarpure (sshringarpure@23andme.com), Chao Tian (ctian@23andme.com), Joyce Y. Tung (joyce@23andme.com), Vladimir Vacic (vvacic@23andme.com), and Catherine H. Wilson (cwilson@23andme.com).
Author information
Authors and Affiliations
Consortia
Contributions
E.P.K., T.A.W. and K.M.V. conceived and designed the experiments; E.P.K., T.S.P., T.R.R., R.W.T., K.J.K., T.A.P., R.d.Q.P. and K.M.V. performed the experiments; E.P.K., T.S.P., T.R.R., R.W.T., R.L.G. III, K.J.K., A.K., D.A.H., 23andMe. R.T., T.A.P., R.d.Q.P. and N.B. analyzed the data; M.H., M.F., F.J., L.T. and M.T.K. provided reagents; E.P.K., T.A.W. and K.M.V. wrote the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
R.L.G. III, M.H., M.F., F.J., R.deQ.P., N.B., L.T., M.T.K., and T.A.W. are the employees of Pfizer Inc. A.K., D.A.H., and the 23andMeResearch Team are the employees of 23andMe. All other authors have no disclosures.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Members of the 23andMe Research Team are listed below Acknowledgements.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Karmele, E.P., Pasricha, T.S., Ramalingam, T.R. et al. Anti-IL-13Rα2 therapy promotes recovery in a murine model of inflammatory bowel disease. Mucosal Immunol 12, 1174–1186 (2019). https://doi.org/10.1038/s41385-019-0189-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41385-019-0189-6
This article is cited by
-
Transferrin modified PEG–PLGA nanoparticles: highly effective notoginsenoside R1 formulations for the treatment of ulcerative colitis
Journal of Pharmaceutical Investigation (2024)
-
Cellular mechanotransduction in health and diseases: from molecular mechanism to therapeutic targets
Signal Transduction and Targeted Therapy (2023)
-
Combined effect of vitamin C and vitamin D3 on intestinal epithelial barrier by regulating Notch signaling pathway
Nutrition & Metabolism (2021)
-
Intestinal eosinophils: multifaceted roles in tissue homeostasis and disease
Seminars in Immunopathology (2021)
-
The reduction of DSS-induced colitis severity in mice exposed to cigarette smoke is linked to immune modulation and microbial shifts
Scientific Reports (2020)