Abstract
This report deals with the possible mechanism by which IL-18 can contribute to the control and resolution of inflammatory lesions in the cornea caused by herpes simplex virus infection. Our results demonstrate that the expression of the IL-18R by both regulatory T cells (Treg) and effector T cells was a pivotal event that influenced lesion pathogenesis. The engagement of IL-18R on Treg with its cytokine ligand resulted in Amphiregulin expression a molecule associated with tissue repair. In support of this scheme of events, lesion severity became more severe in animals unable to express the IL-18R because of gene knockout and was reduced in severity when IL-18 was overexpressed in the cornea. These changes in lesion severity correlated with the frequency and number of both Treg and Teff that expressed Amphiregulin. Additional experiments indicated that IL-12 and IL-18 acted synergistically to enhance Amphiregulin expression in Treg, an event partly dependent on P38 MAPK activity. Finally, sub-conjunctival administration of Amphiregulin resulted in resolution of both developing and developed lesions. Thus, overall our results imply that IL-18 may participate in controlling the severity of SK and contribute to tissue repair by converting both Treg and effector T cells into those that produce Amphiregulin.
Similar content being viewed by others
Introduction
Viruses may cause disease in many ways but few do so solely by their uncontrolled replication.1 More often lesions are the consequence of host inflammatory reactions to the infection and this can lead to chronic tissue damage. Resolving chronic reactions is problematic and these may persist even after the inciting virus is no longer replicating. Resolution of chronic lesions may require a change in the balance of cellular participants along with a change in the cytokines that dominate lesions.2 Cell types involved in limiting tissue damage include CD4 T cells that express the Foxp3 transcription factor (regulatory T cells -Treg).3,4 Such Treg express a range of regulatory functions and can act against several targets in inflammatory responses.5,6 Indeed, there is a spectrum of Treg in terms of functional activities and the spectrum may differ according to location in the body and the stage of lesion development.7,8 Additionally, Treg function may be unstable and under some circumstances the cells lose their regulatory activities and may even take on a pro-inflammatory role in tissues.9,10 An objective for control of chronic infections is to expand and maintain subsets of Treg with functions that counteract tissue damaging events and even contribute to lesion repair.
The idea that Treg can participate in the repair of damaged tissues was realized recently,7,11 but so far has received limited investigation. A critical report on the reparative function of Treg came from studies on a muscle damage model,12 where the Treg population present during muscle lesion repair was dominated by cells which produced Amphiregulin (Amp).13 Amp is a ligand for the epidermal growth factor receptor expressed mainly on epithelial cells and stem cells and its binding can result in the activation of downstream signaling kinases resulting in growth, proliferation, and migration of cells.13,14,15 The mechanism that drives the expression of Treg reparative molecules such as Amp involves cytokines produced by innate immune cells or epithelial cells. For instance, both IL-33 and IL-18 were shown to cause the expression of Amp by Treg.15,16 However, whereas the participation of IL-33 in tissue repair has been well established,17,18,19,20 the role played by IL-18 needs to be further substantiated.
IL-18 is a member of the IL-1 family and is mainly produced at barrier tissues and inflammatory sites when a variety of cell types, which includes epithelial and innate immune cells, are exposed to microbial products.21,22 Whereas, some reports advocate a pathogenic role of IL-18 during infections and autoimmunity,23,24,25 others demonstrate a tissue protective role such as occurs following intestinal and ocular injury.26,27,28,29,30 One potential mechanism for the tissue protective function of IL-18 involves Treg. Thus, expression of the IL-18 receptor (IL-18R) on Treg appeared necessary for their suppressive function.31,32 However the role of IL-18 induced signaling events in Treg involved in the tissue repair process requires to be clarified.
The present report focuses on events that result in the expression of IL-18R and how its binding to IL-18 results in Amp expression especially in Treg. We also explored the participation of IL-18 and Amp expression during the course of an inflammatory response caused by herpes simplex virus (HSV) infection in the mouse cornea. We demonstrate that when lesions were at their peak the majority of Treg in the cornea expressed IL-18R along with several suppressive markers compared with Treg in lymphoid organs. The expression of IL-18R was independent of TCR stimulation but was dependent on the pro-inflammatory cytokine IL-12. IL-12 signaling in Treg resulted in reduced expression of the enzyme DNA methyltransferase 3a (DNMT3a), which correlated with enhanced expression of the IL-18R. Thus, knockdown of DNMT3a in CD4 T cells expanded both Treg and effector T cell population that became IL-18R expressers. In fact, IL-18 signaling led to the expression of Amp and, together with IL-12, synergistically enhanced the expression of Amp. Moreover, IL-18R knockout animals displayed enhanced corneal lesion severity and had far fewer Treg and effector T cells that were Amp producers. In contrast, overexpression of IL-18 caused reduced lesion severity, an effect which correlated with higher numbers of Amp expressing Treg and effector T cells. Taken together, our results indicate that IL-18 plays a tissue protective role in the cornea during SK acting via effects on Treg and effector T cells. This effect occurred by binding to the IL-18R and induced the expression of the tissue repair molecule - Amp. Consequently, IL-18 therapy could represent a valuable strategy to shorten the duration of chronic inflammatory reactions to a viral pathogen.
Results
Treg in cornea upregulate IL-18R and Amp expression
To evaluate the phenotypic and functional status of Treg at different locations after HSV infection, single cell suspensions of pooled corneas and individual DLN were collected at 15 days postinfection (pi) and the cell populations were analyzed by flow cytometry for multiple phenotypic markers. Day 15 pi is the time when lesions caused by HSV in the cornea are fully developed and the inflammation is at its peak. Differences between the two populations were evident. While the majority of the Treg in corneas displayed activation and functional suppressive markers (which included Ki-67, CD44, GITR, OX40, Helios, Nrp1, CD25, CTLA-4) only a minority of the Treg in DLN expressed those markers (Fig. 1a). Additionally, a higher proportion of corneal Treg expressed IL-33R (ST2) and IL-18R compared with the DLN Treg (Fig. 1b). Since, the expression of IL-18R in the corneal Treg was greater than ST2, we focused on the potential relevance of IL-18R. We could show that around day 15pi 80% of corneal Treg expressed IL-18R compared with about 46% which expressed ST2 (Fig. 1c).
Corneal Treg have higher functional markers including IL-18R and Amphiregulin. C57BL/6 animals were infected with 1 × 104 PFU of HSV-RE and at day 15 pi, of individual draining Lymph nodes (dLN) and pooled corneas were stained for flow cytometric analysis. a, b Representative histograms depicting the expression of markers related to Treg (CD4+ Foxp3+) function and activation on corneal Tregs40 and dLN Tregs (blue). c Representative flow plots showing the expression of IL-18R and ST2 (IL-33R) on corneal Treg at day 15pi. d, e Single cells suspension of dLN and cornea were stimulated with PMA/Ionomycin. d Representative flow cytometry plots and histogram showing the Amphiregulin (Amp) expression in corneal and dLN Treg. e Representative flow cytometry plots showing the IL-18R expression on Amphiregulin (Amp) expressing Treg (gated on live cells). Data represents the mean ± SEM of three independent experiments (n = 3 mice/group). **P ≤ 0.01
The expression of the tissue repair molecule Amp was also measured in day 15 samples. About 50% of the corneal Treg were shown to express Amp, whereas less than 25% of DLN Treg were Amp positive (Fig. 1d, Supp Fig. 1A). Curiously, about 70% of the corneal Treg expressing Amp were also IL-18R positive (Fig. 1e). Collectively, these data indicate that the Treg in the cornea are functionally more activated than the Treg in lymph nodes, and the expression of IL-18R by corneal Treg might play a role in driving the production of Amp.
IL-18R and Amp expressing Treg increase with duration of lesion development
To evaluate the potential relevance of IL-18R and Amp expression on Treg following ocular infection, corneas were isolated at different time points pi that included the time of early lesion development (D8), its peak (D15) and the time when most lesions were decreased in severity (D21). The isolated corneal cells were stimulated with PMA/Ionomycin to enumerate Treg that expressed IL-18R and/or Amp. At day 8, ~60 % of the Treg population expressed IL-18R. This increased to about 80% by day 15pi. By day 21, the Treg that expressed IL-18R was reduced to about 60% (similar differences in number were also observed) (Fig. 2a). In the case of Amp expressing Treg, at day 8 ~30% of corneal Treg expressed Amp, but Amp expressing Treg increased to about 50% by day 15 and remained the same at day 21 (Fig. 2a). Whereas at day 15 the majority of Amp expressors were IL-18R positive, by day 21 the majority of Amp expressors no longer expressed IL-18R (Fig. 2a). While, the expression of IL-18R increased from about 60% at day 8pi to about 90% at day 15pi, the majority of the IL-18R expressing T effectors did not express Amp (with less than 7% were Amp+ IL-18R+ at any given time point) (Fig. 2b). The results indicate that the population of IL-18R expressing Treg varies during the course of infection and most of the IL-18R expressing Treg but only a small minority of T effectors made Amp. The high frequency of Amp expressing Treg (IL-18R pos and neg) when lesions were declining might mean that such cells were participating in lesion repair.
IL-18R and Amphiregulin expression on Treg change over the course of infection. C57BL/6 animals were infected with 1 × 104 PFU of HSV-RE and at various time points post infection (Day 8, 15, 21) single cell suspension of pooled corneas were stimulated with PMA/Ionomycin. a Representative flow cytometry plots and bar graphs showing frequency and number of IL-18R and/or Amphiregulin (Amp) expressing Treg. b Representative flow cytometry plots and bar graphs showing frequency and number of IL-18R and/or Amphiregulin (Amp) expressing T effectors (Teff). Data represents the mean ± SEM of three independent experiments (n = 3 mice/group). ****P ≤ 0.0001, ***P ≤ 0.001, **P ≤ 0.01, *P ≤ 0.05
IL-12 and IL-18 synergistically induce the expression of IL-18R and Amp
To account for the observed changes in Treg phenotype over time, various cytokines were measured by multiplex assay and ELISA in the corneas at different time points pi. While, cytokines such as IL-12, IL-6, and IL-33 peaked at day 8 pi (Supp Fig. 1B), the levels of IL-18 peaked at day 15 pi and this was followed by a modest reduction at day 21pi (Fig. 3a). We hypothesized that the expression changes in one or more of these cytokines might have influenced the expression of the IL-18R on Treg. To evaluate this, Treg were differentiated in vitro (iTreg) from naïve CD4 T cells isolated from uninfected C57BL/6 animals. Of note, a low percentage of those iTreg expressed the IL-18R (<5%). This iTreg population was used as the cell source to test the effects of changing the cytokine environment on the expression of the IL-18R. The population was stimulated with IL-2 in the presence or absence of different inflammatory cytokines known to be present in corneal lesions and anti-CD3+ anti-CD28 to mimic TCR stimulation. These cytokines included IL-2, IL-18, IL-6, IL-12, IFN-g, and IL-33 and after 5 days of exposure, the proportion of Treg that expressed IL-18R and Amp was measured. Surprisingly, of all the cytokines tested, only IL-12 caused a significant increase (from 3 to 20%) in the frequency of IL-18R positive Treg compared with controls (Fig. 3b, Supp Fig. 1C). Of note, stimulation with anti-CD3+ CD28, or IL-18 alone, did not influence the frequency of Treg that expressed IL-18R (Fig. 3b). However, when a combination of both IL-12 and IL-18 cytokines was used to stimulate Treg, the number of cells that became IL-18R positive was increased to 60%, well beyond the increase caused by IL-12 stimulation alone (20%) (Fig. 3b). Additionally, while IL-12 alone stimulation did not increase the number of Treg that also expressed Amp, the combination of IL-12 and IL-18 caused a large percentage of cells (~4-fold) to become Amp positive (Fig. 3c). Thus, the cytokines IL-12 and IL-18, whose levels were maximal in the cornea at day 8 and day 15 pi, respectively, appeared to act synergistically to induce the expression of IL-18R and Amp by Treg.
IL-18 and IL-12 synergistically induce the expression of Amphiregulin in Treg. a C57BL/6 animals were infected with 1 × 104 PFU of HSV-RE. Bar graphs showing IL-18 protein levels in the corneas at various time points post infection (Day 0, 8, 15, and 21) quantified by ELISA. b, c iTreg were differentiated from naïve CD4 T cells followed by culturing with either IL-2 alone or with IL-2 in combination with indicated cytokines for 5 days. Representative flow cytometry plots and bar graph showing frequency of b IL-18R expressing or c Amphiregulin (Amp) expressing Treg (gated on live CD4+ Foxp3+). Data represents the mean ± SEM of two independent experiments for (A) n = 4 samples/group or at least three independent experiments for b, c, where n = 3–4 samples/group). ****P ≤ 0.0001, ***P ≤ 0.001, *P ≤ 0.05
DNMT3a can regulate the expression of Amp in CD4 T cells via IL-18R
To evaluate the potential mechanism by which IL-12 could induce the expression of IL-18R, the levels of STAT4 and DNMT3a enzymes were measured in Treg generated in vivo. This analysis was chosen since, previous observations with Th1 cells indicated that IL-12 stimulation induced STAT4 mediated downregulation of DNA methyltransferase-3a (DNMT3a).33,34 This resulted in demethylation of the IL-18R gene and hence the expression of IL-18R.33 In these experiments, iTreg were exposed to IL-2 with or without IL-12 for 3 days after which the levels of STAT4 phosphorylation were measured using flow cytometry. Additionally, mRNA levels of DNMT3a were quantified by QRT-PCR. The results showed that Treg exposed to IL-12 alone significantly induced the phosphorylation of STAT4 (Fig. 4a), but reduced DNMT3a mRNA levels (Fig. 4b) compared with Treg stimulated with IL-2 or IL-18 alone. However, Amp mRNA levels increased when exposed to IL-18 or IL-12 and IL-18 combined, but remained unchanged by exposure to IL-12 or IL-2 alone (Fig. 4b).
DNMT3a may regulate IL-18R expression in Treg. a, b iTreg were differentiated from naïve CD4 T cells followed by culturing with either IL-2 alone or with IL-2 in combination with indicated cytokines for 5 days. a Representative flow cytometry plots and bar graphs showing phosphorylated STAT4 levels in Treg (gated on live CD4+ Foxp3+). b Representative line graph showing relative gene expression levels of DNMT3a and Amp compared with beta-actin, quantified by QRT-PCR. c, d WT (DNMT3a flx/flx) and DNMT3a KO (CD4 Cre+ DNMT3a flx/flx) mice were ocularly infected with HSV-RE and at day 8pi corneas were collected. Single cell suspensions of pooled corneas were stimulated with PMA/Ionomycin followed by ICS assay. c Representative flow cytometry plots and bar graph showing the frequency and number of Amphiregulin expressing Treg (gated on Live CD4+ Foxp3+) and effector T cells (gated on Live CD4+ Foxp3−). d Representative flow cytometry plots and bar graphs showing frequency and number of Treg double positive for IL-18R and Amp. e Bar graph showing MFI of IL-18R on Treg. f Scatter plot showing SK scores at day 15pi. Data represents the mean ± SEM of three independent experiments where n = 3 samples/group. ****P ≤ 0.0001, **P ≤ 0.01, *P ≤ 0.05
To evaluate if DNMT3a could influence IL-18R and subsequently Amp expression in vivo, corneal lesion responses was compared following HSV infection in DNMT3a KO and WT animals. Pools of corneas were stimulated with PMA/Ionomycin at day 15pi and the proportion of Treg that expressed Amp was measured. The results indicate that the frequencies and numbers of Amp producing Treg and effector T cells were higher (2–3 fold) in the corneas of DNMT3aKO animals compared to the control animals (Fig. 4c). In addition, the frequency and numbers of Amp expressing IL-18R pos Treg the were higher in DNMT3a KO compared with WT animals (Fig. 4d). The expression of IL-18R (at per cell basis) within Treg was also higher in the DNMT3a KO compared with WT animals (Fig. 4e). However, SK lesion severity was only moderately reduced in DNMT3a KO mice (Fig. 4f). Taken together, the results indicate that DNMT3a may negatively regulate IL-18R expression and subsequently Amp expression.
Amp induction by IL-12 and IL-18 is P38 MAP kinase dependent
To evaluate the possible mechanism by which IL-18 induced Amp expression, a lead was taken from previous studies on Th2, Th1, or NK cells where P38 MAP Kinase was involved in IL-18 induced expression of IL-5 and IFN-γ, respectively.35,36,37 The levels of phosphorylated P38 MAP kinase (p-P38) were compared between IL-18R positive and negative Treg isolated from the DLN of day 15pi animals. As shown in Fig. 5a, IL-18R positive Treg had 2-fold higher expression of p-P38 compared with IL-18R negative cells. Experiments were also done on in vitro generated Treg wherein iTreg were exposed to IL-2 in the presence or absence of IL-12, or IL-18, or together for 30 min followed by measurement of p-P38. As shown in Fig. 5b, exposure of IL-12 and IL-18 together enhanced the expression of p-P38, while the levels of p-P38 remained unchanged when exposed either to IL-12 or IL-18, or IL-2 alone (Fig. 5b). To evaluate whether activation of P38 MAP kinase was essential for IL-12 and IL-18 induced Amp expression, Treg were exposed to IL-12 and IL-18 for 5 days in the presence or absence of various doses of SB203580, a specific inhibitor of mitogen-activated protein kinase p38. The results indicated that SB203580 dose dependently inhibited Amp expression without influencing the survival of Treg (Fig. 5c). Additionally, P38 MAPK inhibition had minimal effects on the differentiation or proliferation of Treg in vitro (Supp Fig. 1D). Since IL-18 also induces NF-kB along with P38 MAPK, NF-kB was also inhibited using a cell permeable inhibitor (SN50) at various concentrations. However, NF-kB inhibition did not influence Amp expression in Treg (Supp Fig. 1E). These data indicate that IL-12 and IL-18 induced Amp expression in Treg may require MAP kinase P38 phosphorylation.
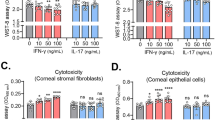
IL-12 and IL-18 induced Amphiregulin expression may be P38 MAPK dependent. a C57BL/6 animals were infected with 1 × 104 PFU of HSV-RE and dLN were isolated at day 15pi. Representative flow cytometry plots and bar graph showing gating strategy and MFI of phosphorylated P38 in IL-18R high and IL-18R low Treg (gated on Live CD4+ Foxp3+) in dLN. b iTreg were differentiated from naïve CD4 T cells followed by culturing with either IL-2 alone or with IL-2 in combination with indicated cytokines for 30 min. Representative histograms and bar graphs showing phopsho-P38 levels and phosphor-P38 MFI respectively. c iTreg were cultured with IL-12 and IL-18 for 5 days in the presence or absence of P38 inhibitor SB 202190 at different concentrations and DMSO as control. Representative flow cytometry plots and bar graph showing the frequency of Amp expressing Treg and % live cells. Data represents the mean ± SEM of three independent experiments where n = 3 samples/group. ****P ≤ 0.0001, **P ≤ 0.01, *P ≤ 0.05
IL-18 signaling is critical for controlling lesion severity
To further evaluate a role for IL-18 in driving the expression of Amp in vivo, IL18r1 knockout mice (IL-18R KO) were used wherein a subunit of the receptor-IL18R1 was deleted. Both WT (C57BL/6) and IL-18R KO mice were ocularly infected with HSV-1 and lesion severity was compared. The results indicate that IL-18R KO animals displayed enhanced lesion severity when compared with WT animals at day 8pi (Fig. 6a). Pools of corneas were collected and evaluated from both groups to measure the frequency and number of Amp expressing Treg in the cornea. It was evident that the Treg and T effector population that were Amp positive was significantly decreased in the IL-18R KO populations (Fig. 6b). Of note, no significant differences in the number and frequency of Th1 and Amp expressing Treg was observed in the DLN of WT and IL-18R KO animals (Fig. 6c). In addition, the knockout of IL-18R did not influence the expression of various activation markers on Treg in the DLN that included GITR, CTLA4, and CD25 (Fig. 6d). Together, these data indicate that the lack of IL-18R signaling can result in enhanced tissue damage and this was accompanied by a diminished number of Treg and effector that expressed Amp.
IL-18R KO animals show higher lesion severity and reduced Amp Treg in cornea (a-d) WT (C57BL/6) and IL18RKO animals were infected with 1 × 104 PFU of HSV-RE (a) line graph showing comparison of SK lesion severity scores at different time points day 5 and day 8 post infection between WT and IL18RKO. b, c Representative FACS plots and histogram showing frequency and number of Treg, Amp Treg and Amp Teffector cells in cornea (b) and Amp Treg and Th1 cells in DLN (c) at day 8 pi. d Histogram showing MFI of key suppressor molecules CTLA4, GITR, and CD25 in DLN of WT and IL18RKO animals at day 8pi. Data represents the mean ± SEM of three independent experiments where n = 8 samples/group (a), n = 3 samples/group (b–d). **P ≤ 0.01, *P ≤ 0.05
Over-expression of IL-18 diminishes SK lesions and expand Amp Treg
Finally, the therapeutic potential of IL-18 in driving the generation of Amp expressing Treg in the cornea was evaluated. For this, an IL-18 overexpressing plasmid which was previously shown to inhibit the development of SK lesions in mice,30 was used. C57BL/6 animals were ocularly injected with the IL-18 overexpressing plasmid 4 and 2 days before ocular infection with HSV. Control animals received empty vector at the same time points. As reported previously,30 animals that received the IL-18 plasmid showed significantly reduced (p < 0.01) SK lesions at day 15pi compared to controls (Fig. 7a). Single cell suspensions of corneas were stimulated with PMA/Ionomycin at day 8 to compare with empty plasmid recipients the numbers of Treg that were Amp positive. As a consequence of IL-18 plasmid exposure all cell types was reduced in number. However, the frequency of Amp expressing Treg and effector CD4 T cells (CD4+ Foxp3−) were both significantly increased at day 8pi (Fig. 7b) compared with the empty plasmid control group. Collectively, these data indicate that IL-18 may play a tissue protective role during ocular lesions and it may be acting by inducing the expression of Amp in Treg and effectors.
IL-18 expression plasmid increases the resolution of SK lesions and Amp Treg in cornea. (A-B) C57BL/6 mice were ocularly infected with 4 × 104 PFU of HSV-1 after administering IL-18 expressing plasmid 4 and 2 days before infection. a SK lesion severity scores as measured at day 15pi. b Representative FACS plots and bar graph showing Amp expressing Treg and Amp expressing effector T cells at day 8pi. Data represents the mean ± SEM of three independent experiments, where n = 8 samples/group (a) and n = 4 samples/group (b). **P ≤ 0.01, *P ≤ 0.05
Amphiregulin accelerates lesion resolution
To evaluate whether Amphiregulin in the cornea had the potential to accelerate lesion resolution, animals were treated with Amphiregulin protein starting at different time points post infection. Firstly, C57BL/6 animals were ocularly infected with HSV and sub-conjunctively treated with recombinant mouse Amphiregulin (rmAmp) every other day starting from day 8 pi to day 14pi. Control animals were treated with PBS at the indicated time points. Animals were scored at different time points during treatment (day 12pi and day 15pi) to enumerate the progression of lesion severity. The results indicated that rmAmp administration from the time when lesion were appearing (day 8pi) significantly reduced lesion severity (p < 0.01) (Fig. 8a). In a separate set of experiments, C57BL/6 animals that were infected with HSV and showing lesions scores ≥ 3 were either treated with rmAmp or PBS (control) every other day starting from day 15pi. At day 21pi, the animals were scored for lesions severity. The results indicated that the animals that received rmAmp had significantly reduced lesion severity compared with the PBS control group (p < 0.0001) and some of the Amp responders resolved their lesions (Fig. 8b). Collectively, these results indicate that Amp expression in the cornea can reduce the progression of lesions and contributes to lesion resolution.
Amp reduces SK lesion severity and accelerates lesion resolution. a C57BL/6 mice were ocularly infected with HSV-1 and were treated with recombinant mouse Amp (rmAmp) every other day sub-conjunctively starting from day 8pi. Line graph showing SK lesion scores at different time points (day 12 and day 15pi) and scatter plot showing lesion severity at day15pi. b Day 15 post infected C57BL/6 animals showing lesion score or ≥3 were treated sub-conjunctively with rmAmp every other day starting from day 15pi. Scatter plot showing lesion severity at day15pi (before) and day21pi (after). Data represents the mean ± SEM of three independent experiments, where n = 10–14 samples/group. ****P ≤ 0.0001, **P ≤ 0.01
Discussion
Stromal keratitis is an inflammatory reaction that occurs in the cornea in response to HSV infection. Lesion severity is known to be influenced by the relative abundance of the pro-inflammatory, mainly CD4 type Th1 cells, and regulatory T cells.38,39 The later cell type appears to limit tissue damage caused by the activities of Th1 cells along with the cells recruited to the cornea such as neutrophils and macrophages.39 Currently, it is not clear how Treg exert their anti-inflammatory function, or if they actively contribute to tissue repair. However, the results in this report support the idea that the expression of the IL-18R by Treg is a relevant event and that the engagement of IL-18R with its cytokine ligand results in the expression of Amphiregulin, a molecule associated with tissue repair in several situations.15 Our results also show that when mice were unable to express IL-18R, SK lesions became more severe and that overexpression of IL-18 in the eye using an expression plasmid was an effective means of limiting lesions. The later outcome correlated with the increased proportion of Treg and effector cells that were Amp producers. Thus, overall our results imply that IL-18 may participate in controlling the severity of SK and contribute to tissue repair by converting into Treg and effector cells that produce Amphiregulin.
Past studies had clearly associated the presence of Treg with diminished tissue damage caused by ocular infection with HSV.5,40,41 Treg may express numerous regulatory functions and it is not clear which ones participate in limiting the corneal damage caused by the effects of T cells and other inflammatory cells. In addition to constraining the pro-inflammatory activities of several cell types, evidence accumulates from studies in other systems that Treg may also participate in the repair of tissue damage.12,16 Tissue repair is a particularly relevant topic with an organ whose function is totally dependent on maintaining tissue clarity along the visual axis from the cornea to the retina. Thus, it would be valuable to discover how any cell type could orchestrate repair of the damaged cornea. Corneal tissue repair involves numerous events and one of these could be Amphiregulin production.42 Amphiregulin engages the epidermal growth factor receptor expressed on corneal epithelial cells and stem cells and causes cell proliferation, differentiation, and migration to participate in tissue repair.43,44,45 Several cell types, such as innate lymphoid cells and mast cells can mediate repair of some tissues via their production of Amp,46,47 but their contributions to the resolution of corneal lesions is yet to be established. However, Treg are numerous in corneal lesions and, as was recently shown in repairing muscle and lung lesions,12,16 these Treg were in large part Amp-producers, unlike Treg at other non-inflamed sites. These observations on repairing muscle and lung inspired the present investigations to determine how Treg could participate in corneal repair in response to a chronic viral induced inflammatory event.
Our studies revealed that an essential event leading up to Amp production by Treg was expression of the IL-18R and engagement by its cytokine ligand IL-18. Previous studies by Rudensky and colleagues had noted that a consequence of triggering the IL-18R on Treg was their conversion to become Amp producers.16 Of many cytokines evaluated for inducing Amp, only IL-18 and IL-33 were effective. Our studies focused on the IL-18R since Treg that expressed this receptor were around two-fold more frequent that those that expressed the IL-33R. We could demonstrate that the frequency of Treg that expressed IL-18R increased as lesions progressed but then declined after lesions diminished. This raised the question of what caused Treg to express IL-18R. Many cytokines were tested but IL-12 appeared to be the most likely candidate. Prior studies had shown that IL-12 is prominently expressed during SK lesion development, perhaps driven by viral components with TLR ligand activity48 or by produces released by damaged cells. In addition to IL-12, we also showed that IL-12 along with IL-18 appeared to act together to cause more Treg to become IL-18R and Amp expressers but the detailed mechanism that explained this apparent synergism needs further study.
The mechanism by which IL-12 caused the expression of IL-18R was associated with STAT4 phosphorylation and down regulation of DNMT3a gene expression. Previous results supported a role for DNMT3a in controlling IL-18R gene expression with it acting by methylating the promoter region.33 Additionally, the knockdown of DNMT3a in CD4 T cells led to the enhancement of Amp and IL-18R expressing Treg in the cornea. Hence, inhibitors targeting DNA methyltransferases such as 5-Azacytidine could have potential therapeutic implications to enhance both the suppressive function and tissue reparative function of Treg. In fact, we recently observed that 5-Azacytidine therapy did inhibit the progression of SK and acted by enhancing the activity of Treg.40 However, it remains to be evaluated whether 5-Azacytidine treatment was also associated with an increased expression of IL-18R and Amp by Treg. Another mechanism by which IL-18 induced Amp expression was activation of P38 MAPK kinase. Thus inhibition of MAP kinase activity using a specific inhibitor led to a dose dependent reduction in Amp expression in the presence of IL-18. These data did not come as a surprise since P38 MAPK activity is known to be required for IL-18 induced Th2 cytokines (IL-4 and IL-13) in basophils and IFN-gamma in NK and Th1 cells.35,36,37 Hence, it is possible that IL-18 and P38 MAPK play a cell specific role in orchestrating the production of cell specific cytokines. An additional mechanism of P38 MAPK mediated inhibition of Amp expression could be via regulating the expression of DNMT3a which in turn regulates the expression of IL18R or Amp itself. However, this issue received minimal attention and further studies are warranted.
A critical event for Treg to become Amp-producers and contribute to lesion resolution was the expression of IL-18R. Thus knockout mice unable to express IL-18R developed more severe SK lesions than did intact control animals and a major consequence of IL-18R KO was a significant reduction in the frequency of Treg that produced Amp. Since the IL-18R KO could still produce IL-33, this might argue that if the IL-33/IL-33R axis is also involved in Amp expression its role is likely to be minor. In addition, previous report32 has shown that IL-18R KO animals harbor Treg with minimal suppressive abilities and display a defect in the expression of various other key effector molecules. This could indicate that IL-18R expression by Treg is critical for both Amp expression and its suppressive functions.
A final approach which implicated a critical role for IL-18 in controlling lesion severity involved using an expression plasmid encoding IL-18. As reported previously,30 use of this plasmid inhibited the severity of SK lesions and in the present study we could show that a consequence of IL-18 plasmid therapy was expansion of the Treg population that were Amp producing cells. However, since IL-18 can have effects on immune cells other than Treg such as neutrophils and macrophages,49 studies using IL-18R flox and Amphiregulin flox mice are needed to further depict the role of IL-18 induced Amp expression by Treg.
In conclusion, our results support the idea that the ongoing events that occur during HSV–induced ocular lesions serve to cause Treg to express IL-18R and this event is necessary to subsequently express Amp, a molecule involved in tissue repair. So far we have been unable to fully verify the concept since we lack access to mice which lack expression of Amp specifically in Treg. Regardless of the source, subconjunctival administration of Amp resulted in the repair of developing or fully developed lesions indicating the importance of Amp in corneal repair process.
Materials and Methods
Mice and virus
C57BL/6 mice (Female) were purchased from Envigo, Inc. (Indianapolis, IN), IL-18R Knockout, CD4 Cre mice were purchased from Jackson and DNMT3a flox mice were a kind gift from Dr. Igor Nasonkin (University of Pittsburg Medical center) all were kept in pathogen free facility where food, water, bedding, and instruments were autoclaved. CD4 cre mice were bred with DNMT3a flox mice and cre mice homozygous for flox was used for the experiments as DNMT3aKO. All the animals were housed in American Association of Laboratory Animal Care–approved facilities at the University of Tennessee, Knoxville, Tennessee. All investigations followed guidelines of the Institutional Animal Care and Use Committee, and adhered to the ARVO Statement for the Use of Animals in Ophthalmic and Vision Research. HSV-l RE strain was used in all procedures. Virus was grown in Vero cell monolayers (American Type Culture Collection, Manassas, VA), titrated, and stored in aliquots at −80 °C until used.
HSV-1 ocular infection and clinical scoring
Ocular infections with HSV-1 was done as previously described.40 Briefly, mice were kept under deep anesthesia by administering an intra peritoneal (i.p) injection of tribromoethanol (Avertin). Later, the mice eyes were scarified with 27-gauge needle and and a 3-µl drop containing 1 × 104 plaque-forming units (PFU) of HSV-1 RE was applied to the eye. The eyes were examined on different days after infection for the development of clinical lesions by slit-lamp biomicroscope (Kawa Co., Nagoya, Japan), and the clinical severity of keratitis of individually scored mice was recorded by a blinded observer. The scoring system was as follows: 0, normal cornea; +1, mild corneal haze; +2, moderate corneal opacity or scarring; +3, severe corneal opacity but iris visible; +4, opaque cornea and corneal ulcer; +5, corneal rupture and necrotizing keratitis.
Flow cytometric analysis
Flow cytometric analysis on tissue and lymph node samples were described previously.10 Briefly, cornea were excised at indicated time points, pooled, and digested with liberase (Roche) for 45 min at 37 °C in a humidified atmosphere of 5% CO2. Single cell suspensions were made by grinding the digested tissue and stained for different cell surface molecules for fluorescence-activated cell sorting (FACS) analyses. Draining cervical lymph nodes were isolated from mice at indicated time points and single cell suspensions were used for FACS analyses. To determine the Amp producing T cells, single cell suspensions were stimulated with PMA (50 ng) and Ionomycin (500 ng) for 3 h in the presence of brefeldin A (10 μg/mL) in U-bottom 96-well plates.16 After this period, Live/Dead staining was performed to gate out the dead population followed by cell surface and intracellular cytokine staining using Foxp3 intracellular staining kit (ebioscience) in accordance with the manufacturer’s recommendations. The stained samples were acquired with a FACS LSR II (BD Biosciences, San Jose, CA) and the data were analyzed using FlowJo software (Tree Star, Inc., Ashland, OR).
Reagents and antibodies
All the staining CD4 (RM4-5), CD45 (53-6.7), CD11b (M1/70), Ly6G (1A8), F4/80 (BM8), IFN-γ (XMG1.2), CD25 (PC61), CD44 (IM7), Foxp3 (FJK-16S), anti-CD3 (145-2C11), anti-CD28 (37.51), IL-18Ra (P3TUNYA) phosphor p38 (4NIT4KK) from Thermofisher. Phorbol myristate acetate (PMA) and Ionomycin from Sigma. Live/Dead staining kit (Life Technologies), anti-mouse Amphiregulin (R&D), GolgiPlug (brefeldin A) and Stat4 (pY693) from BD biosciences. Recombinant mouse IL-2, IL-12, IL-6, IFN-γ, IL-33, IL-18, Amphiregulin, and TGF-β from R&D systems. P38 inhibitor-SB202190 (Tocris) and NF-kB inhibitor-SN50 (emdmillipore).
In vitro Treg differentiation and Treg cultures
Treg were generated in vitro as previously described.40 Briefly, 1 × 106 naïve CD4 T cells were cultured in the presence of plate bound anti-CD3/CD28 Ab (1 µg/ml) and complete RPMI media containing rmIL-2 (100 U/ml) and TGFβ (5 ng/ml) for 5 days at 37 °C in a 5% CO2 incubator. After 5 days, Foxp3, IL18Ra, and Amp expression was determined by flow cytometry as described above. For inducing IL18Ra expression, in vitro generated Treg were cultured with either IL-12 (5 ng/ml) or IL-18 (100 ng/ml) orIL-33 (100 ng/ml) or IFN-gamma (10 ng/ml) or IL-6 (25 ng/ml) for 24 h. For Amp induction experiments, iTreg cells were cultured in the presence of IL-12 (5 ng/ml) or IL-18 (100 ng/ml) or together. For P38 MAPK inhibitor experiments, iTreg were cultured in the presence of IL-12 (5 ng/ml) and IL-18 (100 ng/ml) in the presence or absence of SB 202190 (P38 inhibitor) at doses indicated. After 5 days cells were re-stimulated with PMA/Ionomycin and analyzed for Amp expression using flow cytometer.
Quantitative PCR (qPCR)
Taqman gene expression assays for DNMT3a from Applied Biosystems were performed on iTreg populations using 7500 Fast Real-Time PCR system (Applied Biosystems) as described previously.40
Cytokine level measurements
Corneas were pooled (three corneas per sample) and collected in PBS containing anti-protease cocktail. Corneas were homogenized with tissue homogenizer (Kontes Pellet Pestle mortar). Levels of IL-18 were measured using Mouse IL-18 and Mouse Amphiregulin (Amp) ELISA (R&D); other cytokines were measured using multiplex analysis (Eve technologies).
Purification of CD4+ T cells
Naïve CD4+ T cells were purified using a mouse naïve CD4+ T cell isolation kit (Miltenyi Biotec, Auburn, CA). The purity was achieved at least to an extent of 90%.
Over-expression plasmid preparation
IL-18 over expression plasmid was kindly provided by Dr. Seong Kug Eo, Chonbuk National University and empty plasmid (PCDNA3.1) from Thermosfisher. Plasmid was cloned and purified using Qiagen Maxi kit and 5 µg/eye was administered at 4 and 2 days before infection.
Amphiregulin treatment
Recombinant mouse Amphiregulin (R&D) was sub-conjunctively administered every other day at the dose of 1 μg/mouse at indicated time points. As a control PBS (5 μl) was administered.
Statistical analysis
The statistical significance between the two groups was determined using unpaired, 1-tailed Student’s t-test. For experiments involving more than two groups, one-way ANOVA with Tukey’s multiple comparison tests was used to calculate the level of significance. GraphPad Prism software (GraphPad Software, La Jolla, CA, USA) was used to calculate the statistical significance.
References
Rouse, B. T. & Sehrawat, S. Immunity and immunopathology to viruses: what decides the outcome? Nat. Rev. Immunol. 10, 514 (2010).
Ortega‐Gómez, A., Perretti, M. & Soehnlein, O. Resolution of inflammation: an integrated view. EMBO Mol. Med. 5, 661–674 (2013).
Keynan, Y. et al. The role of regulatory T cells in chronic and acute viral infections. Clin. Infect. Dis. 46, 1046–1052 (2008).
Veiga‐Parga, T., Sehrawat, S. & Rouse, B. T. Role of regulatory T cells during virus infection. Immunol. Rev. 255, 182–196 (2013).
Foulsham, W. et al. The function of regulatory T cells at the ocular surface. Ocul. Surf. 15, 652–659 (2017).
Schmidt, A., Oberle, N., & Krammer, P.H. Molecular mechanisms of treg-mediated T cell suppression. Front. Immunol. 3, 51 (2012).
Panduro, M., Benoist, C. & Mathis, D. Tissue tregs. Annu. Rev. Immunol. 34, 609–633 (2016).
Zhou, X., Tang, J., Cao, H., Fan, H. & Li, B. Tissue resident regulatory T cells: novel therapeutic targets for human disease. Cell. & Mol. Immunol. 12, 543–552 (2015).
Sakaguchi, S., Vignali, D. A., Rudensky, A. Y., Niec, R. E. & Waldmann, H. The plasticity and stability of regulatory T cells. Nat. Rev. Immunol. 13, 461–467 (2013).
Bhela, S. et al. The plasticity and stability of regulatory T cells during viral-induced inflammatory lesions. J. Immunol. 199, 1342–1352 (2017).
Burzyn, D., Benoist, C. & Mathis, D. Regulatory T cells in nonlymphoid tissues. Nat. Immunol. 14, 1007–1013 (2013).
Burzyn, D. et al. A special population of regulatory T cells potentiates muscle repair. Cell 155, 1282–1295 (2013).
Berasain C, Avila MA. Amphiregulin; 2014. Elsevier. pp. 31–41.
Avraham, R. & Yarden, Y. Feedback regulation of EGFR signalling: decision making by early and delayed loops. Nat. Rev. Mol. Cell Biol. 12, 104–117 (2011).
Zaiss, D. M., Gause, W. C., Osborne, L. C. & Artis, D. Emerging functions of amphiregulin in orchestrating immunity, inflammation, and tissue repair. Immunity 42, 216–226 (2015).
Arpaia, N. et al. A distinct function of regulatory T cells in tissue protection. Cell 162, 1078–1089 (2015).
Schmitz, J. et al. IL-33, an interleukin-1-like cytokine that signals via the IL-1 receptor-related protein ST2 and induces T helper type 2-associated cytokines. Immunity 23, 479–490 (2005).
Monticelli, L. A. et al. IL-33 promotes an innate immune pathway of intestinal tissue protection dependent on amphiregulin–EGFR interactions. Proc. Natl Acad. Sci. 112, 10762–10767 (2015).
Liew, F. Y., Girard, J.-P. & Turnquist, H. R. Interleukin-33 in health and disease. Nat. Rev. Immunol. 16, 676–689 (2016).
Schiering, C. et al. The alarmin IL-33 promotes regulatory T-cell function in the intestine. Nature 513, 564–568 (2014).
Dinarello, CA., Novick, D., Kim, S., & Kaplanski, G. Interleukin-18 and IL-18 binding protein. Front. Immunol. 4, 289 (2013).
Kaplanski, G. Interleukin‐18: biological properties and role in disease pathogenesis. Immunol. Rev. 281, 138–153 (2018).
Nowarski, R. et al. Epithelial IL-18 equilibrium controls barrier function in colitis. Cell 163, 1444–1456 (2015).
Boraschi, D. & Dinarello, C. A. IL-18 in autoimmunity. Eur. Cytokine Netw. 17, 224–252 (2006).
Sedimbi, S. K., Hägglöf, T. & Karlsson, M. C. IL-18 in inflammatory and autoimmune disease. Cell. Mol. life Sci. 70, 4795–4808 (2013).
Levy, M. et al. Microbiota-modulated metabolites shape the intestinal microenvironment by regulating NLRP6 inflammasome signaling. Cell 163, 1428–1443 (2015).
Holmkvist, P., Pool, L., Hägerbrand, K., Agace, W. W. & Rivollier, A. IL‐18Rα‐deficient CD4+ T cells induce intestinal inflammation in the CD45RBhi transfer model of colitis despite impaired innate responsiveness. Eur. J. Immunol. 46, 1371–1382 (2016).
Doyle, SL. et al. IL-18 attenuates experimental choroidal neovascularization as a potential therapy for wet age-related macular degeneration. Sci. Transl. Med. 6, 230ra244 (2014).
Salcedo, R. et al. MyD88-mediated signaling prevents development of adenocarcinomas of the colon: role of interleukin 18. J. Exp. Med. 207, 1625–1636 (2010).
Kim, B., Lee, S., Suvas, S. & Rouse, B. T. Application of plasmid DNA encoding IL-18 diminishes development of herpetic stromal keratitis by antiangiogenic effects. J. Immunol. 175, 509–516 (2005).
Oertli, M. et al. DC-derived IL-18 drives Treg differentiation, murine Helicobacter pylori–specific immune tolerance, and asthma protection. J. Clin. Investig. 122, 1082 (2012).
Harrison, O. et al. Epithelial-derived IL-18 regulates Th17 cell differentiation and Foxp3+ Treg cell function in the intestine. Mucosal Immunol. 8, 1226–1236 (2015).
Yu, Q., Thieu, V. T. & Kaplan, M. H. Stat4 limits DNA methyltransferase recruitment and DNA methylation of the IL‐18Rα gene during Th1 differentiation. EMBO J. 26, 2052–2060 (2007).
Pham, D. et al. Opposing roles of STAT4 and Dnmt3a in Th1 gene regulation. J. Immunol. 191, 902–911 (2013).
Kroeger, K. M., Sullivan, B. M. & Locksley, R. M. IL-18 and IL-33 elicit Th2 cytokines from basophils via a MyD88-and p38α-dependent pathway. J. Leukoc. Biol. 86, 769–778 (2009).
Yang, J., Zhu, H., Murphy, T. L., Ouyang, W. & Murphy, K. M. IL-18–stimulated GADD45β required in cytokine-induced, but not TCR-induced, IFN-γ production. Nat. Immunol. 2, 157–164 (2001).
Mavropoulos, A., Sully, G., Cope, A. P. & Clark, A. R. Stabilization of IFN-γ mRNA by MAPK p38 in IL-12–and IL-18–stimulated human NK cells. Blood 105, 282–288 (2005).
Biswas, P. S. & Rouse, B. T. Early events in HSV keratitis – setting the stage for a blinding disease. Microbes Infect. 7, 799–810 (2005).
Rajasagi N.K, Rouse B.T. Application of our understanding of pathogenesis of herpetic stromal keratitis for novel therapy. Microbes Infect (2018). https://doi.org/10.1016/j.micinf.2017.12.014
Varanasi, S. K. et al. Azacytidine treatment inhibits the progression of herpes stromal keratitis by enhancing regulatory T cell function. J. Virol. 91, e02367–02316 (2017).
Gaddipati, S., Estrada, K., Rao, P., Jerome, A. D. & Suvas, S. IL-2/Anti–IL-2 antibody complex treatment inhibits the development but not the progression of herpetic stromal keratitis. J. Immunol. 194, 273–282 (2015).
Ljubimov, A. V. & Saghizadeh, M. Progress in corneal wound healing. Progress. Retin. Eye Res. 49, 17–45 (2015).
Zieske, J. D., Takahashi, H., Hutcheon, A. E. & Dalbone, A. C. Activation of epidermal growth factor receptor during corneal epithelial migration. Invest. Ophthalmol. Vis. Sci. 41, 1346–1355 (2000).
Morita S-i, et al. (2007) Human corneal epithelial cell proliferation by epiregulin and its cross-induction by other EGF family members.
Peterson, J. L., Phelps, E. D., Doll, M. A., Schaal, S. & Ceresa, B. P. The role of endogenous epidermal growth factor receptor ligands in mediating corneal epithelial homeostasis EGFR ligands in corneal wound healing. Invest. Ophthalmol. Vis. Sci. 55, 2870–2880 (2014).
Monticelli, L. A. et al. Innate lymphoid cells promote lung-tissue homeostasis after infection with influenza virus. Nat. Immunol. 12, 1045–1054 (2011).
Okumura, S., Sagara, H., Fukuda, T., Saito, H. & Okayama, Y. FcεRI-mediated amphiregulin production by human mast cells increases mucin gene expression in epithelial cells. J. Allergy Clin. Immunol. 115, 272–279 (2005).
Kumaraguru, U. & Rouse, B. The IL-12 response to herpes simplex virus is mainly a paracrine response of reactive inflammatory cells. J. Leukoc. Biol. 72, 564–570 (2002).
Yano, T. et al. The pathological role of IL-18Rα in renal ischemia/reperfusion injury. Lab. Investig. 95, 78–91 (2015).
Acknowledgements
This study was supported by National Institutes of Health Grant EY 005093. We thank Dr. Igor Nasonkin of University of Pittsburg Medical center for providing DNMT3a flox mice and Dr. Seong Kug Eo of Chonbuk National University for providing IL-18 expression plasmid.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Varanasi, S.K., Rajasagi, N., Jaggi, U. et al. Role of IL-18 induced Amphiregulin expression on virus induced ocular lesions. Mucosal Immunol 11, 1705–1715 (2018). https://doi.org/10.1038/s41385-018-0058-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41385-018-0058-8
This article is cited by
-
The amphiregulin/EGFR axis has limited contribution in controlling autoimmune diabetes
Scientific Reports (2023)