Abstract
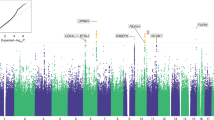
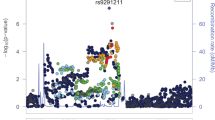
Individuals suffering from chronic pain develop substance use disorders (SUDs) more often than others. Understanding the shared genetic influences underlying the comorbidity between chronic pain and SUDs will lead to a greater understanding of their biology. Genome-wide association statistics were obtained from the UK Biobank for multisite chronic pain (MCP, Neffective = 387,649) and from the Million Veteran Program and the Psychiatric Genomics Consortium meta-analyses for alcohol use disorder (AUD, Neffective = 296,974), cannabis use disorder (CanUD, Neffective = 161,053), opioid use disorder (OUD, Neffective = 57,120), and problematic tobacco use (PTU, Neffective = 270,120). SNP-based heritability was estimated for each of the traits and genetic correlation (rg) analyses were performed to assess MCP-SUD pleiotropy. Bidirectional Mendelian Randomization analyses evaluated possible causal relationships. Finally, to identify and characterize individual loci, we performed a genome-wide pleiotropy analysis and a brain-wide analysis using imaging phenotypes available from the UK Biobank. MCP was positively genetically correlated with AUD (rg = 0.26, p = 7.55 × 10−18), CanUD (rg = 0.37, p = 8.21 × 10−37), OUD (rg = 0.20, p = 1.50 × 10−3), and PTU (rg = 0.29, p = 8.53 × 10−12). Although the MR analyses supported bi-directional relationships, MCP had larger effects on AUD (pain-exposure: beta = 0.18, p = 8.21 × 10−4; pain-outcome: beta = 0.07, p = 0.018), CanUD (pain-exposure: beta = 0.58, p = 2.70 × 10−6; pain-outcome: beta = 0.05, p = 0.014) and PTU (pain-exposure: beta = 0.43, p = 4.16 × 10−8; pain-outcome: beta = 0.09, p = 3.05 × 10−6) than the reverse. The genome-wide analysis identified two SNPs pleiotropic between MCP and all SUD investigated: IHO1 rs7652746 (ppleiotropy = 2.69 × 10−8), and CADM2 rs1248857 (ppleiotropy = 1.98 × 10−5). In the brain-wide analysis, rs7652746 was associated with multiple cerebellum and amygdala imaging phenotypes. When analyzing MCP pleiotropy with each SUD separately, we found 25, 22, and 4 pleiotropic variants for AUD, CanUD, and OUD, respectively. To our knowledge, this is the first large-scale study to provide evidence of potential causal relationships and shared genetic mechanisms underlying MCP-SUD comorbidity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
All data are reported in the manuscript and its supplemental material. For any additional queries, please reach out to the corresponding author. Genome-wide data used in this article are publicly available (MCP: https://researchdata.gla.ac.uk/822/, SUDs: dbGaP phs001672.v1.p1, https://www.ncbi.nlm.nih.gov/gap/).
References
Carvalho AS, Martins Pereira S, Jacomo A, Magalhaes S, Araujo J, Hernandez-Marrero P, et al. Ethical decision making in pain management: a conceptual framework. J Pain Res. 2018;11:967–76.
Dydyk AM, Conermann T. Chronic Pain. StatPearls: Treasure Island (FL), 2023.
Goldberg DS, McGee SJ. Pain as a global public health priority. BMC Public Health. 2011;11:770.
Yong RJ, Mullins PM, Bhattacharyya N. Prevalence of chronic pain among adults in the United States. Pain. 2022;163:e328–e332.
Manchikanti L, Cash KA, Damron KS, Manchukonda R, Pampati V, McManus CD. Controlled substance abuse and illicit drug use in chronic pain patients: An evaluation of multiple variables. Pain Physician. 2006;9:215–25.
Cheatle M, Comer D, Wunsch M, Skoufalos A, Reddy Y. Treating pain in addicted patients: recommendations from an expert panel. Popul Health Manag. 2014;17:79–89.
Barry DT, Cutter CJ, Beitel M, Kerns RD, Liong C, Schottenfeld RS. Psychiatric Disorders Among Patients Seeking Treatment for Co-Occurring Chronic Pain and Opioid Use Disorder. J Clin Psychiatry. 2016;77:1413–9.
Manchikanti L, Helm S 2nd, Fellows B, Janata JW, Pampati V, Grider JS, et al. Opioid epidemic in the United States. Pain Physician. 2012;15:ES9–38.
Gardner EA, McGrath SA, Dowling D, Bai D. The Opioid Crisis: Prevalence and Markets of Opioids. Forensic Sci Rev. 2022;34:43–70.
Turk DC, Wilson HD, Cahana A. Treatment of chronic non-cancer pain. Lancet. 2011;377:2226–35.
Hocking LJ, Generation S, Morris AD, Dominiczak AF, Porteous DJ, Smith BH. Heritability of chronic pain in 2195 extended families. Eur J Pain. 2012;16:1053–63.
Mogil JS. Pain genetics: past, present and future. Trends Genet. 2012;28:258–66.
Johnston KJA, Adams MJ, Nicholl BI, Ward J, Strawbridge RJ, Ferguson A, et al. Genome-wide association study of multisite chronic pain in UK Biobank. PLoS Genet. 2019;15:e1008164.
Toikumo S, Vickers-Smith R, Jinwala Z, Xu H, Saini D, Hartwell E. et al. The genetic architecture of pain intensity in a sample of 598,339 U.S. veterans. medRxiv. 2023; 2023.03.09.23286958.
Haefeli M, Elfering A. Pain assessment. Eur Spine J. 2006;15:S17–24.
Levey DF, Galimberti M, Deak JD, Wendt FR, Bhattacharya A, Koller D, et al. Multi-ancestry genome-wide association study of cannabis use disorder yields insight into disease biology and public health implications. Nat Genet. 2023;55:2094–103.
Kember RL, Vickers-Smith R, Xu H, Toikumo S, Niarchou M, Zhou H, et al. Cross-ancestry meta-analysis of opioid use disorder uncovers novel loci with predominant effects in brain regions associated with addiction. Nat Neurosci. 2022;25:1279–87.
Hatoum AS, Colbert SMC, Johnson EC, et al. Multivariate genome-wide association meta-analysis of over 1 million subjects identifies loci underlying multiple substance use disorders. Nat Ment Health. 2023;1:210–23.
Zhou H, Kember RL, Deak JD, Xu H, Toikumo S, Yuan K et al. Multi-ancestry study of the genetics of problematic alcohol use in >1 million individuals. Nat Med. 2023;29:3184–92.
Farrell SF, Kho PF, Lundberg M, Campos AI, Renteria ME, de Zoete RMJ, et al. A Shared Genetic Signature for Common Chronic Pain Conditions and its Impact on Biopsychosocial Traits. J Pain. 2023;24:369–86.
Lee MC, Wanigasekera V, Tracey I. Imaging opioid analgesia in the human brain and its potential relevance for understanding opioid use in chronic pain. Neuropharmacology. 2014;84:123–30.
Volkow ND, Boyle M. Neuroscience of Addiction: Relevance to Prevention and Treatment. Am J Psychiatry. 2018;175:729–40.
Smallwood RF, Price LR, Campbell JL, Garrett AS, Atalla SW, Monroe TB, et al. Network Alterations in Comorbid Chronic Pain and Opioid Addiction: An Exploratory Approach. Front Hum Neurosci. 2019;13:174.
Gaziano JM, Concato J, Brophy M, Fiore L, Pyarajan S, Breeling J, et al. Million Veteran Program: A mega-biobank to study genetic influences on health and disease. J Clin Epidemiol. 2016;70:214–23.
Sullivan PF, Agrawal A, Bulik CM, Andreassen OA, Borglum AD, Breen G, et al. Psychiatric Genomics: An Update and an Agenda. Am J Psychiatry. 2018;175:15–27.
Turley P, Walters RK, Maghzian O, Okbay A, Lee JJ, Fontana MA, et al. Multi-trait analysis of genome-wide association summary statistics using MTAG. Nat Genet. 2018;50:229–37.
Bulik-Sullivan BK, Loh PR, Finucane HK, Ripke S, Yang J, Schizophrenia Working Group of the Psychiatric Genomics C, et al. LD Score regression distinguishes confounding from polygenicity in genome-wide association studies. Nat Genet. 2015;47:291–5.
Hemani G, Zheng J, Elsworth B, Wade KH, Haberland V, Baird D, et al. The MR-Base platform supports systematic causal inference across the human phenome. Elife. 2018;7:e34408.
Hemani G, Bowden J, Davey Smith G. Evaluating the potential role of pleiotropy in Mendelian randomization studies. Hum Mol Genet. 2018;27:R195–R208.
Verbanck M, Chen CY, Neale B, Do R. Detection of widespread horizontal pleiotropy in causal relationships inferred from Mendelian randomization between complex traits and diseases. Nat Genet. 2018;50:693–8.
von-Berg J, Michelle TD, van-der-Laan SW, de-Ridder J. PolarMorphism enables discovery of shared genetic variants across multiple traits from GWAS summary statistics. Bioinformatics. 2022:38:i212-9.
Purcell S, Neale B, Todd-Brown K, Thomas L, Ferreira MA, Bender D, et al. PLINK: a tool set for whole-genome association and population-based linkage analyses. Am J Hum Genet. 2007;81:559–75.
Mishra A, Macgregor S. VEGAS2: Software for More Flexible Gene-Based Testing. Twin Res Hum Genet. 2015;18:86–91.
Smith SM, Douaud G, Chen W, Hanayik T, Alfaro-Almagro F, Sharp K, et al. An expanded set of genome-wide association studies of brain imaging phenotypes in UK Biobank. Nat Neurosci. 2021;24:737–45.
Consortium GT. The GTEx Consortium atlas of genetic regulatory effects across human tissues. Science. 2020;369:1318–30.
Foley CN, Staley JR, Breen PG, Sun BB, Kirk PDW, Burgess S, et al. A fast and efficient colocalization algorithm for identifying shared genetic risk factors across multiple traits. Nat Commun. 2021;12:764.
Sanchez-Roige S, Palmer AA, Fontanillas P, Elson SL, Me Research Team tSUDWGotPGC, Adams MJ, et al. Genome-Wide Association Study Meta-Analysis of the Alcohol Use Disorders Identification Test (AUDIT) in Two Population-Based Cohorts. Am J Psychiatry. 2019;176:107–18.
Gelernter J, Polimanti R. Genetics of substance use disorders in the era of big data. Nat Rev Genet. 2021;22:712–29.
Zhang Y, Cheng Y, Jiang W, Ye Y, Lu Q, Zhao H. Comparison of methods for estimating genetic correlation between complex traits using GWAS summary statistics. Brief Bioinform. 2021;22:bbaa442.
Johnson EC, Demontis D, Thorgeirsson TE, Walters RK, Polimanti R, Hatoum AS, et al. A large-scale genome-wide association study meta-analysis of cannabis use disorder. Lancet Psychiatry. 2020;7:1032–45.
Cooke ME, Potter KW, Jashinski J, Pascale M, Schuster RM, Tervo-Clemmens B, et al. Development of cannabis use disorder in medical cannabis users: A 9-month follow-up of a randomized clinical trial testing effects of medical cannabis card ownership. Front Psychiatry. 2023;14:1083334.
Riley JL 3rd, King C. Self-report of alcohol use for pain in a multi-ethnic community sample. J Pain. 2009;10:944–52.
Rogers AH, Bakhshaie J, Buckner JD, Orr MF, Paulus DJ, Ditre JW, et al. Opioid and Cannabis Co-Use among Adults With Chronic Pain: Relations to Substance Misuse, Mental Health, and Pain Experience. J Addict Med. 2019;13:287–94.
Zvolensky MJ, McMillan K, Gonzalez A, Asmundson GJ. Chronic pain and cigarette smoking and nicotine dependence among a representative sample of adults. Nicotine Tob Res. 2009;11:1407–14.
Wallis D, Coatsworth JD, Mennis J, Riggs NR, Zaharakis N, Russell MA, et al. Predicting Self-Medication with Cannabis in Young Adults with Hazardous Cannabis Use. Int J Environ Res Public Health. 2022;19:1850.
Osborn LA, Lauritsen KJ, Cross N, Davis AK, Rosenberg H, Bonadio F, et al. Self-Medication of Somatic and Psychiatric Conditions Using Botanical Marijuana. J Psychoact Drugs. 2015;47:345–50.
Bicket MC, Stone EM, McGinty EE. Use of Cannabis and Other Pain Treatments Among Adults With Chronic Pain in US States With Medical Cannabis Programs. JAMA Netw Open. 2023;6:e2249797.
Busse JW, Vankrunkelsven P, Zeng L, Heen AF, Merglen A, Campbell F, et al. Medical cannabis or cannabinoids for chronic pain: a clinical practice guideline. BMJ. 2021;374:n2040.
Brennan PL, Schutte KK, Moos RH. Pain and use of alcohol to manage pain: prevalence and 3-year outcomes among older problem and non-problem drinkers. Addiction. 2005;100:777–86.
Patterson AL, Gritzner S, Resnick MP, Dobscha SK, Turk DC, Morasco BJ. Smoking cigarettes as a coping strategy for chronic pain is associated with greater pain intensity and poorer pain-related function. J Pain. 2012;13:285–92.
Ditre JW, Brandon TH. Pain as a motivator of smoking: effects of pain induction on smoking urge and behavior. J Abnorm Psychol. 2008;117:467–72.
Compton P, Darakjian J, Miotto K. Screening for addiction in patients with chronic pain and “problematic” substance use: evaluation of a pilot assessment tool. J Pain Symptom Manag. 1998;16:355–63.
Morasco BJ, Dobscha SK. Prescription medication misuse and substance use disorder in VA primary care patients with chronic pain. Gen Hosp Psychiatry. 2008;30:93–9.
Ward R, Tang YL, Axon RN, Casarella J, Whitfield N, Rauch SAM. Effectiveness of a substance use treatment program for veterans with chronic pain and opioid use disorder. J Subst Abus Treat. 2022;132:108635.
Savage SR, Kirsh KL, Passik SD. Challenges in using opioids to treat pain in persons with substance use disorders. Addict Sci Clin Pr. 2008;4:4–25.
Turner HN, Oliver J, Compton P, Matteliano D, Sowicz TJ, Strobbe S, et al. Pain Management and Risks Associated With Substance Use: Practice Recommendations. Pain Manag Nurs. 2022;23:91–108.
Hill KP, Palastro MD, Johnson B, Ditre JW. Cannabis and Pain: A Clinical Review. Cannabis Cannabinoid Res. 2017;2:96–104.
Khan JS, Hah JM, Mackey SC. Effects of smoking on patients with chronic pain: a propensity-weighted analysis on the Collaborative Health Outcomes Information Registry. Pain. 2019;160:2374–9.
Girdler SS, Maixner W, Naftel HA, Stewart PW, Moretz RL, Light KC. Cigarette smoking, stress-induced analgesia and pain perception in men and women. Pain. 2005;114:372–85.
Maleki N, Tahaney K, Thompson BL, Oscar-Berman M. At the intersection of alcohol use disorder and chronic pain. Neuropsychology. 2019;33:795–807.
Berrendero F, Mendizabal V, Robledo P, Galeote L, Bilkei-Gorzo A, Zimmer A, et al. Nicotine-induced antinociception, rewarding effects, and physical dependence are decreased in mice lacking the preproenkephalin gene. J Neurosci. 2005;25:1103–12.
Ballantyne JC, Shin NS. Efficacy of opioids for chronic pain: a review of the evidence. Clin J Pain. 2008;24:469–78.
Meyer A, LeClair C, McDonald JV. Prescription Opioid Prescribing in Western Europe and the United States. R I Med J (2013). 2020;103:45–8.
Baselmans BML, Jansen R, Ip HF, van Dongen J, Abdellaoui A, van de Weijer MP, et al. Multivariate genome-wide analyses of the well-being spectrum. Nat Genet. 2019;51:445–51.
Zhong VW, Kuang A, Danning RD, Kraft P, van Dam RM, Chasman DI, et al. A genome-wide association study of bitter and sweet beverage consumption. Hum Mol Genet. 2019;28:2449–57.
Saunders GRB, Wang X, Chen F, Jang SK, Liu M, Wang C, et al. Genetic diversity fuels gene discovery for tobacco and alcohol use. Nature. 2022;612:720–4.
Ruscheweyh R, Kuhnel M, Filippopulos F, Blum B, Eggert T, Straube A. Altered experimental pain perception after cerebellar infarction. Pain. 2014;155:1303–12.
Ranjbar H, Soti M, Banazadeh M, Saleki K, Kohlmeier KA, Shabani M. Addiction and the cerebellum with a focus on actions of opioid receptors. Neurosci Biobehav Rev. 2021;131:229–47.
Hampton WH, Hanik IM, Olson IR. Substance abuse and white matter: Findings, limitations, and future of diffusion tensor imaging research. Drug Alcohol Depend. 2019;197:288–98.
Forster BB, MacKay AL, Whittall KP, Kiehl KA, Smith AM, Hare RD, et al. Functional magnetic resonance imaging: the basics of blood-oxygen-level dependent (BOLD) imaging. Can Assoc Radio J. 1998;49:320–9.
van der Gaag C, Minderaa RB, Keysers C. The BOLD signal in the amygdala does not differentiate between dynamic facial expressions. Soc Cogn Affect Neurosci. 2007;2:93–103.
Kilts CD. Imaging the roles of the amygdala in drug addiction. Psychopharmacol Bull. 2001;35:84–94.
Neugebauer V. Amygdala pain mechanisms. Handb Exp Pharm. 2015;227:261–84.
Tolomeo S, Yu R. Brain network dysfunctions in addiction: a meta-analysis of resting-state functional connectivity. Transl Psychiatry. 2022;12:41.
Kregel J, Meeus M, Malfliet A, Dolphens M, Danneels L, Nijs J, et al. Structural and functional brain abnormalities in chronic low back pain: A systematic review. Semin Arthritis Rheum. 2015;45:229–37.
Stanzione M, Baumann M, Papanikos F, Dereli I, Lange J, Ramlal A, et al. Meiotic DNA break formation requires the unsynapsed chromosome axis-binding protein IHO1 (CCDC36) in mice. Nat Cell Biol. 2016;18:1208–20.
Zhou H, Sealock JM, Sanchez-Roige S, Clarke TK, Levey DF, Cheng Z, et al. Genome-wide meta-analysis of problematic alcohol use in 435,563 individuals yields insights into biology and relationships with other traits. Nat Neurosci. 2020;23:809–18.
Deak JD, Levey DF, Wendt FR, Zhou H, Galimberti M, Kranzler HR, et al. Genome-Wide Investigation of Maximum Habitual Alcohol Intake in US Veterans in Relation to Alcohol Consumption Traits and Alcohol Use Disorder. JAMA Netw Open. 2022;5:e2238880.
Liu M, Jiang Y, Wedow R, Li Y, Brazel DM, Chen F, et al. Association studies of up to 1.2 million individuals yield new insights into the genetic etiology of tobacco and alcohol use. Nat Genet. 2019;51:237–44.
Brazel DM, Jiang Y, Hughey JM, Turcot V, Zhan X, Gong J, et al. Exome Chip Meta-analysis Fine Maps Causal Variants and Elucidates the Genetic Architecture of Rare Coding Variants in Smoking and Alcohol Use. Biol Psychiatry. 2019;85:946–55.
Pasman JA, Verweij KJH, Gerring Z, Stringer S, Sanchez-Roige S, Treur JL, et al. GWAS of lifetime cannabis use reveals new risk loci, genetic overlap with psychiatric traits, and a causal influence of schizophrenia. Nat Neurosci. 2018;21:1161–70.
Morris J, Bailey MES, Baldassarre D, Cullen B, de Faire U, Ferguson A, et al. Genetic variation in CADM2 as a link between psychological traits and obesity. Sci Rep. 2019;9:7339.
Frei JA, Andermatt I, Gesemann M, Stoeckli ET. The SynCAM synaptic cell adhesion molecules are involved in sensory axon pathfinding by regulating axon-axon contacts. J Cell Sci. 2014;127:5288–302.
Sanchez-Roige S, Jennings MV, Thorpe HHA, Mallari JE, van der Werf LC, Bianchi SB, et al. CADM2 is implicated in impulsive personality and numerous other traits by genome- and phenome-wide association studies in humans and mice. Transl Psychiatry. 2023;13:167.
Li S, Ma C, Li Y, Chen R, Liu Y, Wan LP, et al. The schizophrenia-associated missense variant rs13107325 regulates dendritic spine density. Transl Psychiatry. 2022;12:361.
Everitt BJ, Robbins TW. From the ventral to the dorsal striatum: devolving views of their roles in drug addiction. Neurosci Biobehav Rev. 2013;37:1946–54.
Martikainen IK, Nuechterlein EB, Pecina M, Love TM, Cummiford CM, Green CR, et al. Chronic Back Pain Is Associated with Alterations in Dopamine Neurotransmission in the Ventral Striatum. J Neurosci. 2015;35:9957–65.
Vellucci R. Heterogeneity of chronic pain. Clin Drug Investig. 2012;32:3–10.
Treede RD, Rief W, Barke A, Aziz Q, Bennett MI, Benoliel R, et al. Chronic pain as a symptom or a disease: the IASP Classification of Chronic Pain for the International Classification of Diseases (ICD-11). Pain. 2019;160:19–27.
Gkatzionis A, Burgess S. Contextualizing selection bias in Mendelian randomization: how bad is it likely to be? Int J Epidemiol. 2019;48:691–701.
Brumpton B, Sanderson E, Heilbron K, Hartwig FP, Harrison S, Vie GA, et al. Avoiding dynastic, assortative mating, and population stratification biases in Mendelian randomization through within-family analyses. Nat Commun. 2020;11:3519.
Acknowledgements
The authors acknowledge support from the Horizon 2020 Marie Sklodowska-Curie Individual Fellowship from the European Commission (101028810), the National Institutes of Health (R33 DA047527, R21 DC018098, RF1 MH132337, K99 AG078503, T32 MH014276, T32 AA02825, K01 DA051759), Alzheimer’s Association Research Fellowship (AARF-22-967171), and One Mind. We thank the participants and the investigators involved in the UK Biobank, Million Veteran Program, and the Psychiatric Genomics Consortium for making their data publicly available.
Author information
Authors and Affiliations
Contributions
DK and RP designed the study. DK analyzed the data, and wrote the manuscript draft. DFL, HZ, ASH, JDD, RLK, HRK, MBS and JG provided data. All the other authors provided critical feedback, context interpretation, draft revision, and editing. RP supervised the study, reviewed, and edited the manuscript.
Corresponding authors
Ethics declarations
Competing interests
RP reports a research grant from Alkermes. RP and JG are paid for their editorial work in the journal Complex Psychiatry. JG and HRK hold US patent 10,900,082 titled: “Genotype-guided dosing of opioid agonists,” issued January 26, 2021. HRK is a member of advisory boards for Dicerna Pharmaceuticals, Sophrosyne Pharmaceuticals, and Enthion Pharmaceuticals; a consultant to Sobrera Pharmaceuticals; the recipient of research funding and medication supplies for an investigator-initiated study from Alkermes; and a member of the American Society of Clinical Psychopharmacology’s Alcohol Clinical Trials Initiative, which was supported in the past 3 years by Alkermes, Dicerna, Ethypharm, Lundbeck, Mitsubishi, Otsuka, and Pear Therapeutics. MBS has in the past 3 years received consulting income from Actelion, Acadia Pharmaceuticals, Aptinyx, atai Life Sciences, Boehringer Ingelheim, Bionomics, BioXcel Therapeutics, Clexio, Delix Pharmaceuticals, EmpowerPharm, Engrail Therapeutics, GW Pharmaceuticals, Janssen, Jazz Pharmaceuticals, and Roche/Genentech; has stock options in Oxeia Biopharmaceuticals and EpiVario; and has been paid for editorial work on Depression and Anxiety (Editor-in-Chief), Biological Psychiatry (Deputy Editor), and UpToDate (Co-Editor-in-Chief for Psychiatry). The other authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Koller, D., Friligkou, E., Stiltner, B. et al. Pleiotropy and genetically inferred causality linking multisite chronic pain to substance use disorders. Mol Psychiatry (2024). https://doi.org/10.1038/s41380-024-02446-3
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41380-024-02446-3