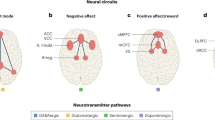
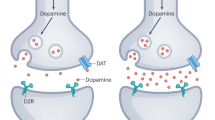
Abstract
Despite advances in neuroscience, limited progress has been made in developing new and better medications for psychiatric disorders. Available treatments in psychiatry rely on a few classes of drugs that have a broad spectrum of activity across disorders with limited understanding of mechanism of action. While the added value of more targeted therapies is apparent, a dearth of pathophysiologic mechanisms exists to support targeted treatments, and where mechanisms have been identified and drugs developed, results have been disappointing. Based on serendipity and early successes that led to the current drug armamentarium, a haunting legacy endures that new drugs should align with outdated and overinclusive diagnostic categories, consistent with the idea that “one size fits all”. This legacy has fostered clinical trial designs focused on heterogenous populations of patients with a single diagnosis and non-specific outcome variables. Disturbingly, this approach likely contributed to missed opportunities for drugs targeting the hypothalamic-pituitary-adrenal axis and now inflammation. Indeed, cause-and-effect data support the role of inflammatory processes in neurotransmitter alterations that disrupt specific neurocircuits and related behaviors. This pathway to pathology occurs across disorders and warrants clinical trial designs that enrich for patients with increased inflammation and use primary outcome variables associated with specific effects of inflammation on brain and behavior. Nevertheless, such trial designs have not been routinely employed, and results of anti-inflammatory treatments have been underwhelming. Thus, to accelerate development of targeted therapeutics including in the area of inflammation, regulatory agencies and the pharmaceutical industry must embrace treatments and trials focused on pathophysiologic pathways that impact specific symptom domains in subsets of patients, agnostic to diagnosis. Moreover, closer collaboration among basic and clinical investigators is needed to apply neuroscience knowledge to reveal disease mechanisms that drive psychiatric symptoms. Together, these efforts will support targeted treatments, ultimately leading to new and better therapeutics in psychiatry.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Hyman SE. Psychiatric drug development: diagnosing a crisis. Cerebrum. 2013;2013:5.
Hyman SE. Revolution stalled. Sci Transl Med. 2012;4:155cm111.
Cuthbert BN. Research Domain Criteria: toward future psychiatric nosologies. Dialogues Clin Neurosci. 2015;17:89–97.
Clementz BA, Sweeney JA, Hamm JP, Ivleva EI, Ethridge LE, Pearlson GD, et al. Identification of Distinct Psychosis Biotypes Using Brain-Based Biomarkers. Am J Psychiatry. 2016;173:373–84.
Holsboer F. Antidepressant drug discovery in the postgenomic era. World J Biol Psychiatry. 2001;2:165–77.
Moncrieff J, Cooper RE, Stockmann T, Amendola S, Hengartner MP, Horowitz MA. The serotonin theory of depression: a systematic umbrella review of the evidence. Mol Psychiatry. 2022. https://doi.org/10.1038/s41380-022-01661-0. Online ahead of print
New JP, Hanrahan C. Antidepressant medications: The FDA-approval process and the need for updates. Ment Health Clin. 2014;4:11–6.
DeVita VT Jr., Chu E. A history of cancer chemotherapy. Cancer Res. 2008;68:8643–53.
Correll CU, Rubio JM, Kane JM. What is the risk-benefit ratio of long-term antipsychotic treatment in people with schizophrenia? World Psychiatry. 2018;17:149–60.
Photopoulos J. The future of tissue-agnostic drugs. Nature. 2020;585:S16–S18.
Luoh SW, Flaherty KT. When Tissue Is No Longer the Issue: Tissue-Agnostic Cancer Therapy Comes of Age. Ann Intern Med. 2018;169:233–9.
Seligson ND, Knepper TC, Ragg S, Walko CM. Developing Drugs for Tissue-Agnostic Indications: A Paradigm Shift in Leveraging Cancer Biology for Precision Medicine. Clin Pharm Ther. 2021;109:334–42.
Rizzo A, Mollica V, Santoni M, Massari F. Cancer Immunotherapy: Current and Future Perspectives on a Therapeutic Revolution. J Clin Med. 2021;10:5246.
Healy D. The Discovery of Antidepressants. The Antidepressant Era. Cambridge, MA:Harvard University Press;1997. p. 43–77.
Hyman SE. Can neuroscience be integrated into the DSM-V? Nat Rev Neurosci. 2007;8:725–32.
Insel T, Cuthbert B, Garvey M, Heinssen R, Pine DS, Quinn K, et al. Research domain criteria (RDoC): toward a new classification framework for research on mental disorders. Am J Psychiatry. 2010;167:748–51.
https://reporter.nih.gov/search/IjOHtpuaY0KulajqirwxQA/projects/charts. Accessed Date Accessed.
Owens MJ, Nemeroff CB. The role of corticotropin-releasing factor in the pathophysiology of affective and anxiety disorders: laboratory and clinical studies. Ciba Found Symp. 1993;172:296–308. discussion 308-216
Nemeroff CB. The corticotropin-releasing factor (CRF) hypothesis of depression: new findings and new directions. Mol Psychiatry. 1996;1:336–42.
Bremner JD, Licinio J, Darnell A, Krystal JH, Owens MJ, Southwick SM, et al. Elevated CSF corticotropin-releasing factor concentrations in posttraumatic stress disorder. Am J Psychiatry. 1997;154:624–9.
Banki CM, Bissette G, Arato M, O’Connor L, Nemeroff CB. CSF corticotropin-releasing factor-like immunoreactivity in depression and schizophrenia. Am J Psychiatry. 1987;144:873–7.
Spierling SR, Zorrilla EP. Don’t stress about CRF: assessing the translational failures of CRF(1)antagonists. Psychopharmacol (Berl). 2017;234:1467–81.
Dwyer JB, Aftab A, Radhakrishnan R, Widge A, Rodriguez CI, Carpenter LL, et al. Hormonal Treatments for Major Depressive Disorder: State of the Art. Am J Psychiatry. 2020;177:686–705.
Block T, Petrides G, Kushner H, Kalin N, Belanoff J, Schatzberg A. Mifepristone Plasma Level and Glucocorticoid Receptor Antagonism Associated With Response in Patients With Psychotic Depression. J Clin Psychopharmacol. 2017;37:505–11.
The dexamethasone suppression test: an overview of its current status in psychiatry. The APA Task Force on Laboratory Tests in Psychiatry. Am J Psychiatry. 1987;144:1253–62.
Rush AJ, Giles DE, Schlesser MA, Orsulak PJ, Parker CR Jr., Weissenburger JE, et al. The dexamethasone suppression test in patients with mood disorders. J Clin Psychiatry. 1996;57:470–84.
Calhoun V. The Promise of Big Data Imaging for Mental Health. Cerebrum. 2021;2021:cer-01-21.
Levey DF, Stein MB, Wendt FR, Pathak GA, Zhou H, Aslan M, et al. Bi-ancestral depression GWAS in the Million Veteran Program and meta-analysis in >1.2 million individuals highlight new therapeutic directions. Nat Neurosci. 2021;24:954–63.
Hoehe MR, Morris-Rosendahl DJ. The role of genetics and genomics in clinical psychiatry. Dialogues Clin Neurosci. 2018;20:169–77.
Ermers NJ, Hagoort K, Scheepers FE. The Predictive Validity of Machine Learning Models in the Classification and Treatment of Major Depressive Disorder: State of the Art and Future Directions. Front Psychiatry. 2020;11:472.
Chekroud AM, Bondar J, Delgadillo J, Doherty G, Wasil A, Fokkema M, et al. The promise of machine learning in predicting treatment outcomes in psychiatry. World Psychiatry. 2021;20:154–70.
Schwabe I, Milaneschi Y, Gerring Z, Sullivan PF, Schulte E, Suppli NP, et al. Unraveling the genetic architecture of major depressive disorder: merits and pitfalls of the approaches used in genome-wide association studies. Psychol Med. 2019;49:2646–56.
Kendler KS, Ohlsson H, Sundquist J, Sundquist K. Risk for Mood, Anxiety, and Psychotic Disorders in Individuals at High and Low Genetic Liability for Bipolar Disorder and Major Depression. JAMA Psychiatry. 2022;79:1102–9.
Tam V, Patel N, Turcotte M, Bossé Y, Paré G, Meyre D. Benefits and limitations of genome-wide association studies. Nat Rev Genet. 2019;20:467–84.
Zannas AS, Jia M, Hafner K, Baumert J, Wiechmann T, Pape JC, et al. Epigenetic upregulation of FKBP5 by aging and stress contributes to NF-kappaB-driven inflammation and cardiovascular risk. Proc Natl Acad Sci USA. 2019;116:11370–9.
Menke A, Klengel T, Rubel J, Brückl T, Pfister H, Lucae S, et al. Genetic variation in FKBP5 associated with the extent of stress hormone dysregulation in major depression. Genes Brain Behav. 2013;12:289–96.
Zannas AS, Wiechmann T, Gassen NC, Binder EB. Gene-Stress-Epigenetic Regulation of FKBP5: Clinical and Translational Implications. Neuropsychopharmacology. 2016;41:261–74.
Binder EB. The role of FKBP5, a co-chaperone of the glucocorticoid receptor in the pathogenesis and therapy of affective and anxiety disorders. Psychoneuroendocrinology. 2009;34:S186–195.
Binder EB, Salyakina D, Lichtner P, Wochnik GM, Ising M, Putz B, et al. Polymorphisms in FKBP5 are associated with increased recurrence of depressive episodes and rapid response to antidepressant treatment. Nat Genet. 2004;36:1319–25.
Klengel T, Mehta D, Anacker C, Rex-Haffner M, Pruessner JC, Pariante CM, et al. Allele-specific FKBP5 DNA demethylation mediates gene-childhood trauma interactions. Nat Neurosci. 2013;16:33–41.
Rao S, Yao Y, Ryan J, Li T, Wang D, Zheng C, et al. Common variants in FKBP5 gene and major depressive disorder (MDD) susceptibility: a comprehensive meta-analysis. Sci Rep. 2016;6:32687.
Hartmann J, Wagner KV, Gaali S, Kirschner A, Kozany C, Ruhter G, et al. Pharmacological Inhibition of the Psychiatric Risk Factor FKBP51 Has Anxiolytic Properties. J Neurosci. 2015;35:9007–16.
Baker RE, Peña JM, Jayamohan J, Jérusalem A. Mechanistic models versus machine learning, a fight worth fighting for the biological community? Biol Lett. 2018;14:20170660.
Scangos KW, Khambhati AN, Daly PM, Makhoul GS, Sugrue LP, Zamanian H, et al. Closed-loop neuromodulation in an individual with treatment-resistant depression. Nat Med. 2021;27:1696–700.
Zandvakili A, Philip NS, Jones SR, Tyrka AR, Greenberg BD, Carpenter LL. Use of machine learning in predicting clinical response to transcranial magnetic stimulation in comorbid posttraumatic stress disorder and major depression: A resting state electroencephalography study. J Affect Disord. 2019;252:47–54.
Arulpragasam AR, van ‘t Wout-Frank M, Barredo J, Faucher CR, Greenberg BD, Philip NS. Low Intensity Focused Ultrasound for Non-invasive and Reversible Deep Brain Neuromodulation-A Paradigm Shift in Psychiatric Research. Front Psychiatry. 2022;13:825802.
Miller AH, Raison CL. Are Anti-inflammatory Therapies Viable Treatments for Psychiatric Disorders?: Where the Rubber Meets the Road. JAMA Psychiatry. 2015;72:527–8.
Miller AH, Raison CL. The role of inflammation in depression: from evolutionary imperative to modern treatment target. Nat Rev Immunol. 2016;16:22–34.
Lucido MJ, Bekhbat M, Goldsmith DR, Treadway MT, Haroon E, Felger JC, et al. Aiding and Abetting Anhedonia: Impact of Inflammation on the Brain and Pharmacological Implications. Pharm Rev. 2021;73:1084–117.
Miller AH, Pariante CM. Trial failures of anti-inflammatory drugs in depression. Lancet Psychiatry. 2020;7:837.
Harrison NA, Voon V, Cercignani M, Cooper EA, Pessiglione M, Critchley HD. A Neurocomputational Account of How Inflammation Enhances Sensitivity to Punishments Versus Rewards. Biol Psychiatry. 2016;80:73–81.
Davies KA, Cooper E, Voon V, Tibble J, Cercignani M, Harrison NA. Interferon and anti-TNF therapies differentially modulate amygdala reactivity which predicts associated bidirectional changes in depressive symptoms. Mol Psychiatry. 2021;26:5150–60.
Capuron L, Pagnoni G, Drake DF, Woolwine BJ, Spivey JR, Crowe RJ, et al. Dopaminergic mechanisms of reduced basal ganglia responses to hedonic reward during interferon alfa administration. Arch Gen Psychiatry. 2012;69:1044–53.
Eisenberger NI, Berkman ET, Inagaki TK, Rameson LT, Mashal NM, Irwin MR. Inflammation-induced anhedonia: endotoxin reduces ventral striatum responses to reward. Biol Psychiatry. 2010;68:748–54.
Lee Y, Mansur RB, Brietzke E, Carmona NE, Subramaniapillai M, Pan Z, et al. Efficacy of adjunctive infliximab vs. placebo in the treatment of anhedonia in bipolar I/II depression. Brain Behav Immun. 2020;88:631–9.
Salvadore G, Nash, A, Bleys, C, Hsu, B, Saad, Z, Gause, A, et al. A Double-Blind, Placebo-Controlled, Multicenter Study of Sirukumab as Adjunctive Treatment to a Monoaminergic Antidepressant in Adults With Major Depressive Disorder. 57th Annual Meeting of the American College of Neuropsychopharmacology in Hollywood Florida. Hollywood, FL: American College of Neuropsychopharmacology; 2018.
Raison CL, Rutherford RE, Woolwine BJ, Shuo C, Schettler P, Drake DF, et al. A randomized controlled trial of the tumor necrosis factor antagonist infliximab for treatment-resistant depression: the role of baseline inflammatory biomarkers. JAMA Psychiatry. 2013;70:31–41.
Majd M, Saunders EFH, Engeland CG. Inflammation and the dimensions of depression: a review. Front Neuroendocrinol. 2020;56:100800.
Kappelmann N, Arloth J, Georgakis MK, Czamara D, Rost N, Ligthart S, et al. Dissecting the Association Between Inflammation, Metabolic Dysregulation, and Specific Depressive Symptoms: A Genetic Correlation and 2-Sample Mendelian Randomization Study. JAMA Psychiatry. 2021;78:161–70.
Barnes J, Mondelli V, Pariante CM. Genetic Contributions of Inflammation to Depression. Neuropsychopharmacology. 2017;42:81–98.
Goldsmith DR, Rapaport MH, Miller BJ. A meta-analysis of blood cytokine network alterations in psychiatric patients: comparisons between schizophrenia, bipolar disorder and depression. Mol Psychiatry. 2016;21:1696–709.
Yang JJ, Jiang W. Immune biomarkers alterations in post-traumatic stress disorder: a systematic review and meta-analysis. J Affect Disord. 2020;268:39–46.
Osimo EF, Pillinger T, Rodriguez IM, Khandaker GM, Pariante CM, Howes OD. Inflammatory markers in depression: a meta-analysis of mean differences and variability in 5,166 patients and 5,083 controls. Brain Behav Immun. 2020;87:901–9.
Kohler-Forsberg O, Nicolaisen Lydholm C, Hjorthoj C, Nordentoft M, Mors O, Benros ME. Efficacy of anti-inflammatory treatment on major depressive disorder or depressive symptoms: Meta-analysis of clinical trials. Acta Psychiatr Scand. 2019;139:404–19.
Savitz JB, Teague TK, Misaki M, Macaluso M, Wurfel BE, Meyer M, et al. Treatment of bipolar depression with minocycline and/or aspirin: an adaptive, 2x2 double-blind, randomized, placebo-controlled, phase IIA clinical trial. Transl Psychiatry. 2018;8:27.
Nettis MA, Lombardo G, Hastings C, Zajkowska Z, Mariani N, Nikkheslat N et al. Augmentation therapy with minocycline in treatment-resistant depression patients with low-grade peripheral inflammation: results from a double-blind randomised clinical trial. Neuropsychopharmacology. 2021;46:939–48.
Husain MI, Chaudhry IB, Khoso AB, Husain MO, Hodsoll J, Ansari MA, et al. Minocycline and celecoxib as adjunctive treatments for bipolar depression: a multicentre, factorial design randomised controlled trial. Lancet Psychiatry. 2020;7:515–27.
Hellmann-Regen J, Clemens V, Grozinger M, Kornhuber J, Reif A, Prvulovic D, et al. Effect of Minocycline on Depressive Symptoms in Patients With Treatment-Resistant Depression: A Randomized Clinical Trial. JAMA Netw Open. 2022;5:e2230367.
Butler D. Translational research: crossing the valley of death. Nature. 2008;453:840–2.
Back SE, Book SW, Santos AB, Brady KT. Training physician-scientists: a model for integrating research into psychiatric residency. Acad Psychiatry. 2011;35:40–5.
Milewicz DM, Lorenz RG, Dermody TS, Brass LF. Rescuing the physician-scientist workforce: the time for action is now. J Clin Investig. 2015;125:3742–7.
Greek R, Greek J. Is the use of sentient animals in basic research justifiable? Philos Ethics Humanit Med. 2010;5:14.
Graziane J, Graziane N. Neuroscience Milestones: Developing Standardized Core-Competencies for Research-Based Neuroscience Trainees. J Neurosci. 2022;42:7332–8.
Arbuckle MR, Gordon JA, Pincus HA, Oquendo MA. Bridging the gap: supporting translational research careers through an integrated research track within residency training. Acad Med. 2013;88:759–65.
Gilbert AR, Tew JD Jr., Reynolds CF 3rd, Pincus HA, Ryan N, Nash K, et al. A developmental model for enhancing research training during psychiatry residency. Acad Psychiatry. 2006;30:55–62.
Miller G. Psychiatry. Beyond DSM: seeking a brain-based classification of mental illness. Science. 2010;327:1437.
Iyer G, Hanrahan AJ, Milowsky MI, Al-Ahmadie H, Scott SN, Janakiraman M, et al. Genome sequencing identifies a basis for everolimus sensitivity. Science. 2012;338:221.
Chokhawala K, Stevens L. Antipsychotic Medications. StatPearls. Treasure Island (FL): StatPearls Publishing Copyright © 2022, StatPearls Publishing LLC; 2022.
Del Casale A, Bonanni L, Bargagna P, Novelli F, Fiaschè F, Paolini M, et al. Current Clinical Psychopharmacology in Borderline Personality Disorder. Curr Neuropharmacol. 2021;19:1760–79.
Garakani A, Murrough JW, Freire RC, Thom RP, Larkin K, Buono FD, et al. Pharmacotherapy of Anxiety Disorders: Current and Emerging Treatment Options. Focus (Am Psychiatr Publ). 2021;19:222–42.
Meltzer HY. The mechanism of action of novel antipsychotic drugs. Schizophr Bull. 1991;17:263–87.
Kapur S, Zipursky R, Jones C, Remington G, Houle S. Relationship between dopamine D(2) occupancy, clinical response, and side effects: a double-blind PET study of first-episode schizophrenia. Am J Psychiatry. 2000;157:514–20.
Schatzberg AF. New indications for antidepressants. J Clin Psychiatry. 2000;61:9–17.
Popper CW. Antidepressants in the treatment of attention-deficit/hyperactivity disorder. J Clin Psychiatry. 1997;58:14–29.
Leonard BE. Mechanisms of Action of Antidepressants. CNS Drugs. 1995;4:1–12.
Nayak R, Rosh I, Kustanovich I, Stern S. Mood Stabilizers in Psychiatric Disorders and Mechanisms Learnt from In Vitro Model Systems. Int J Mol Sci. 2021;22:9315.
Canitano R. Mood Stabilizers in Children and Adolescents With Autism Spectrum Disorders. Clin Neuropharmacol. 2015;38:177–82.
Schloesser RJ, Martinowich K, Manji HK. Mood-stabilizing drugs: mechanisms of action. Trends Neurosci. 2012;35:36–46.
McAllister TW, Zafonte R, Jain S, Flashman LA, George MS, Grant GA, et al. Randomized Placebo-Controlled Trial of Methylphenidate or Galantamine for Persistent Emotional and Cognitive Symptoms Associated with PTSD and/or Traumatic Brain Injury. Neuropsychopharmacology. 2016;41:1191–8.
Hardy SE. Methylphenidate for the treatment of depressive symptoms, including fatigue and apathy, in medically ill older adults and terminally ill adults. Am J Geriatr Pharmacother. 2009;7:34–59.
Gaillard C, Lago TR, Gorka AX, Balderston NL, Fuchs BA, Reynolds RC, et al. Methylphenidate modulates interactions of anxiety with cognition. Transl Psychiatry. 2021;11:544.
Faraone SV. The pharmacology of amphetamine and methylphenidate: Relevance to the neurobiology of attention-deficit/hyperactivity disorder and other psychiatric comorbidities. Neurosci Biobehav Rev. 2018;87:255–70.
Feder A, Costi S, Rutter SB, Collins AB, Govindarajulu U, Jha MK, et al. A Randomized Controlled Trial of Repeated Ketamine Administration for Chronic Posttraumatic Stress Disorder. Am J Psychiatry. 2021;178:193–202.
Williams NR, Heifets BD, Bentzley BS, Blasey C, Sudheimer KD, Hawkins J, et al. Attenuation of antidepressant and antisuicidal effects of ketamine by opioid receptor antagonism. Mol Psychiatry. 2019;24:1779–86.
Zanos P, Gould TD. Mechanisms of ketamine action as an antidepressant. Mol Psychiatry. 2018;23:801–11.
Dos Santos RG, Bouso JC, Rocha JM, Rossi GN, Hallak JE. The Use of Classic Hallucinogens/Psychedelics in a Therapeutic Context: Healthcare Policy Opportunities and Challenges. Risk Manag Health Policy. 2021;14:901–10.
Sarris J, Sinclair J, Karamacoska D, Davidson M, Firth J. Medicinal cannabis for psychiatric disorders: a clinically-focused systematic review. BMC Psychiatry. 2020;20:24.
Silva EADJ, Medeiros WMB, Torro N, Sousa JMM, Almeida I, Costa FBD, et al. Cannabis and cannabinoid use in autism spectrum disorder: a systematic review. Trends Psychiatry Psychother. 2022;44:e20200149.
Wright M, Di Ciano P, Brands B. Use of cannabidiol for the treatment of anxiety: a short synthesis of pre-clinical and clinical evidence. Cannabis Cannabinoid Res. 2020;5:191–6.
Author information
Authors and Affiliations
Contributions
AHM and CLR were responsible for the conceptualization of the paper and paper preparation including writing and editing.
Corresponding author
Ethics declarations
Competing interests
AHM is a paid consultant for Cerevel Therapeutics, and CLR is a paid consultant for Novartis, Alfasigma, Usona Institute and Emory Healthcare.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Miller, A.H., Raison, C.L. Burning down the house: reinventing drug discovery in psychiatry for the development of targeted therapies. Mol Psychiatry 28, 68–75 (2023). https://doi.org/10.1038/s41380-022-01887-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41380-022-01887-y
This article is cited by
-
The why, when, where, how, and so what of so-called rapidly acting antidepressants
Neuropsychopharmacology (2024)
-
Transcriptomic dysregulation and autistic-like behaviors in Kmt2c haploinsufficient mice rescued by an LSD1 inhibitor
Molecular Psychiatry (2024)
-
Serum autoantibodies against α7-nicotinic receptors in subgroups of patients with bipolar disorder or schizophrenia: clinical features and link with peripheral inflammation
Translational Psychiatry (2024)
-
Elevated body temperature is associated with depressive symptoms: results from the TemPredict Study
Scientific Reports (2024)
-
Psychedelics and ketamine are a symptom of psychiatry’s woes, not a cure
Molecular Psychiatry (2023)