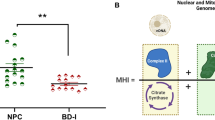
Abstract
Recent studies have suggested that mitochondrial dysfunction and dysregulated neuroinflammatory pathways are involved in the pathophysiology of major depressive disorder (MDD). Here, we aimed to assess the differences in markers of mitochondrial dynamics, mitophagy, general autophagy, and apoptosis in peripheral blood mononuclear cells (PBMCs) of MDD patients (n = 77) and healthy controls (HCs, n = 24). Moreover, we studied inflammation engagement as a moderator of mitochondria dysfunctions on the severity of depressive symptoms. We found increased levels of Mfn-2 (p < 0.001), short Opa-1 (S-Opa-1) (p < 0.001) and Fis-1 (p < 0.001) in MDD patients, suggesting an increase in the mitochondrial fragmentation. We also found that MDD patients had higher levels of Pink-1 (p < 0.001), p62/SQSTM1 (p < 0.001), LC3B (p = 0.002), and caspase-3 active (p = 0.001), and lower levels of parkin (p < 0.001) compared with HCs. Moreover, we showed that that MDD patients with higher CRP levels had higher levels of Mfn-2 (p = 0.001) and LC3B (p = 0.002) when compared with MDD patients with low CRP. Another notable finding was that the severity of depressive symptoms in MDD is associated with changes in protein levels in pathways related to mitochondrial dynamics and mitophagy, and can be dependent on the inflammatory status. Overall, our study demonstrated that a disruption in the mitochondrial dynamics network could initiate a cascade of abnormal changes relevant to the critical pathological changes during the course of MDD and lead to poor outcomes.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Disease GBD, Injury I, Prevalence C. Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: A systematic analysis for the global burden of disease study 2017. Lancet. 2018;392:1789–858.
Liu Q, He H, Yang J, Feng X, Zhao F, Lyu J. Changes in the global burden of depression from 1990 to 2017: Findings from the global burden of disease study. J Psychiatr Res. 2020;126:134–40.
Kim YK. Molecular neurobiology of major depressive disorder. Prog Neuro-Psychopharmacol Biol Psychiatry. 2016;64:275–6.
Zhang G, Xu S, Zhang Z, Zhang Y, Wu Y, An J, et al. Identification of key genes and the pathophysiology associated with major depressive disorder patients based on integrated bioinformatics analysis. Front Psychiatry. 2020;11:192.
Allen J, Romay-Tallon R, Brymer KJ, Caruncho HJ, Kalynchuk LE. Mitochondria and mood: Mitochondrial dysfunction as a key player in the manifestation of depression. Front Neurosci. 2018;12:386.
Belenguer P, Duarte JMN, Schuck PF, Ferreira GC. Mitochondria and the Brain: Bioenergetics and beyond. Neurotox Res. 2019;36:219–38.
Spinelli JB, Haigis MC. The multifaceted contributions of mitochondria to cellular metabolism. Nat Cell Biol. 2018;20:745–54.
Kornmann B. Quality control in mitochondria: Use it, break it, fix it, trash it. F1000Prime Rep. 2014;6:15.
Boveris A, Oshino N, Chance B. The cellular production of hydrogen peroxide. Biochem J. 1972;128:617–30.
Fischer F, Hamann A, Osiewacz HD. Mitochondrial quality control: An integrated network of pathways. Trends Biochem Sci. 2012;37:284–92.
Evans CS, Holzbaur ELF. Quality control in neurons: Mitophagy and other selective autophagy mechanisms. J Mol Biol. 2020;432:240–60.
Palikaras K, Tavernarakis N. Regulation and roles of mitophagy at synapses. Mech Ageing Dev. 2020;187:111216.
Sedlackova L, Korolchuk VI. Mitochondrial quality control as a key determinant of cell survival. Biochim Biophys Acta Mol Cell Res. 2019;1866:575–87.
Panchal K, Tiwari AK. Mitochondrial dynamics, a key executioner in neurodegenerative diseases. Mitochondrion. 2019;47:151–73.
Alexiou A, Nizami B, Khan FI, Soursou G, Vairaktarakis C, Chatzichronis S, et al. Mitochondrial dynamics and proteins related to neurodegenerative diseases. Curr Protein Pept Sci. 2018;19:850–7.
Scaini G, Barichello T, Fries GR, Kennon EA, Andrews T, Nix BR, et al. TSPO upregulation in bipolar disorder and concomitant downregulation of mitophagic proteins and NLRP3 inflammasome activation. Neuropsychopharmacol: Off Publ Am Coll Neuropsychopharmacol. 2019;44:1291–9.
Scaini G, Fries GR, Valvassori SS, Zeni CP, Zunta-Soares G, Berk M, et al. Perturbations in the apoptotic pathway and mitochondrial network dynamics in peripheral blood mononuclear cells from bipolar disorder patients. Transl Psychiatry. 2017;7:e1111.
Scaini G, Quevedo J, Velligan D, Roberts DL, Raventos H, Walss-Bass C. Second generation antipsychotic-induced mitochondrial alterations: Implications for increased risk of metabolic syndrome in patients with schizophrenia. Eur Neuropsychopharmacol: J Eur Coll Neuropsychopharmacol. 2018;28:369–80.
Cataldo AM, McPhie DL, Lange NT, Punzell S, Elmiligy S, Ye NZ, et al. Abnormalities in mitochondrial structure in cells from patients with bipolar disorder. Am J Pathol. 2010;177:575–85.
Mertens J, Wang QW, Kim Y, Yu DX, Pham S, Yang B, et al. Differential responses to lithium in hyperexcitable neurons from patients with bipolar disorder. Nature. 2015;527:95–99.
Inuwa IM, Peet M, Williams MA. QSAR modeling and transmission electron microscopy stereology of altered mitochondrial ultrastructure of white blood cells in patients diagnosed as schizophrenic and treated with antipsychotic drugs. Biotech Histochem. 2005;80:133–7.
Rosenfeld M, Brenner-Lavie H, Ari SG, Kavushansky A, Ben-Shachar D. Perturbation in mitochondrial network dynamics and in complex I dependent cellular respiration in schizophrenia. Biol Psychiatry. 2011;69:980–8.
Atkin TA, MacAskill AF, Brandon NJ, Kittler JT. Disrupted in Schizophrenia-1 regulates intracellular trafficking of mitochondria in neurons. Mol Psychiatry. 2011;16:122–4. 121
Chen C, Wang Y, Zhang J, Ma L, Gu J, Ho G. Contribution of neural cell death to depressive phenotypes of streptozotocin-induced diabetic mice. Dis Model Mech. 2014;7:723–30.
Gulbins A, Schumacher F, Becker KA, Wilker B, Soddemann M, Boldrin F, et al. Antidepressants act by inducing autophagy controlled by sphingomyelin-ceramide. Mol Psychiatry. 2018;23:2324–46.
Trivedi MH, Chin Fatt CR, Jha MK, Cooper CM, Trombello JM, Mason BL, et al. Comprehensive phenotyping of depression disease trajectory and risk: Rationale and design of Texas resilience against depression study (T-RAD). J Psychiatr Res. 2020;122:22–32.
Montgomery SA, Asberg M. A new depression scale designed to be sensitive to change. Br J Psychiatry: J Ment Sci. 1979;134:382–9.
Demarest TG, McCarthy MM. Sex differences in mitochondrial (dys)function: Implications for neuroprotection. J Bioenerg Biomembr. 2015;47:173–88.
Scaini G, Maggi DD, De-Nes BT, Goncalves CL, Ferreira GK, Teodorak BP, et al. Activity of mitochondrial respiratory chain is increased by chronic administration of antidepressants. Acta neuropsychiatrica. 2011;23:112–8.
Chistiakov DA, Sobenin IA, Revin VV, Orekhov AN, Bobryshev YV. Mitochondrial aging and age-related dysfunction of mitochondria. Biomed Res Int. 2014;2014:238463.
Hayes A Introduction to Mediation, Moderation, and Conditional Process Analysis. 2nd ed A Regression-Based Approach. 2nd edition edn. Guilford Press: New York, 2018, pp 692.
Scaini G, Santos PM, Benedet J, Rochi N, Gomes LM, Borges LS, et al. Evaluation of Krebs cycle enzymes in the brain of rats after chronic administration of antidepressants. Brain Res Bull. 2010;82:224–7.
Kageyama Y, Kasahara T, Kato M, Sakai S, Deguchi Y, Tani M, et al. The relationship between circulating mitochondrial DNA and inflammatory cytokines in patients with major depression. J Affect Disord. 2018;233:15–20.
Busch KB, Kowald A, Spelbrink JN. Quality matters: how does mitochondrial network dynamics and quality control impact on mtDNA integrity? Philos Trans R Soc Lond B Biol Sci. 2014;369:20130442.
MacVicar T, Langer T. OPA1 processing in cell death and disease - the long and short of it. J Cell Sci. 2016;129:2297–306.
Sood A, Jeyaraju DV, Prudent J, Caron A, Lemieux P, McBride HM, et al. A Mitofusin-2-dependent inactivating cleavage of Opa1 links changes in mitochondria cristae and ER contacts in the postprandial liver. Proc Natl Acad Sci USA. 2014;111:16017–22.
Frezza C, Cipolat S, Martins de Brito O, Micaroni M, Beznoussenko GV, Rudka T, et al. OPA1 controls apoptotic cristae remodeling independently from mitochondrial fusion. Cell. 2006;126:177–89.
Jin SM, Youle RJ. PINK1- and Parkin-mediated mitophagy at a glance. J Cell Sci. 2012;125:795–9.
Kaminskyy VO, Zhivotovsky B. Free radicals in cross talk between autophagy and apoptosis. Antioxid Redox Signal. 2014;21:86–102.
Chung Y, Lee J, Jung S, Lee Y, Cho JW, Oh YJ. Dysregulated autophagy contributes to caspase-dependent neuronal apoptosis. Cell Death Dis. 2018;9:1189.
Deus CM, Yambire KF, Oliveira PJ, Raimundo N. Mitochondria-lysosome crosstalk: From physiology to neurodegeneration. Trends Mol Med. 2020;26:71–88.
Amidfar M, Kim YK, Scaini G, Quevedo J. Evidence for additionally increased apoptosis in the peripheral blood mononuclear cells of major depressive patients with a high risk for suicide. Am J Med Genet Part B, Neuropsychiatr Genet: Off Publ Int Soc Psychiatr Genet. 2018;177:388–96.
Shelton RC, Claiborne J, Sidoryk-Wegrzynowicz M, Reddy R, Aschner M, Lewis DA, et al. Altered expression of genes involved in inflammation and apoptosis in frontal cortex in major depression. Mol Psychiatry. 2011;16:751–62.
Szuster-Ciesielska A, Slotwinska M, Stachura A, Marmurowska-Michalowska H, Dubas-Slemp H, Bojarska-Junak A, et al. Accelerated apoptosis of blood leukocytes and oxidative stress in blood of patients with major depression. Prog neuro-Psychopharmacol Biol psychiatry. 2008;32:686–94.
Nakahira K, Haspel JA, Rathinam VA, Lee SJ, Dolinay T, Lam HC, et al. Autophagy proteins regulate innate immune responses by inhibiting the release of mitochondrial DNA mediated by the NALP3 inflammasome. Nat Immunol. 2011;12:222–30.
Pinti M, Cevenini E, Nasi M, De Biasi S, Salvioli S, Monti D, et al. Circulating mitochondrial DNA increases with age and is a familiar trait: Implications for “inflamm-aging”. Eur J Immunol. 2014;44:1552–62.
Wu G, Zhu Q, Zeng J, Gu X, Miao Y, Xu W, et al. Extracellular mitochondrial DNA promote NLRP3 inflammasome activation and induce acute lung injury through TLR9 and NF-kappaB. J Thorac Dis. 2019;11:4816–28.
Biasizzo M, Kopitar-Jerala N. Interplay Between NLRP3 Inflammasome and Autophagy. Front Immunol. 2020;11:591803.
Funding
The T-RAD study is generously supported by The Hersh Foundation, Jordan E. Harris Foundation, W. W. Caruth, Jr. Fund, Evelyn Rose, M2G Ventures, and support for the use of REDCap (CTSA NIH Grant UL1TR001105). The research funding support from the University of Texas health science centre at Houston, the Louis A. Faillace, MD Endowment Funds and the Translational Psychiatry Program to GS and JQ are acknowledged. Translational Psychiatry Program (USA) is funded by the Department of Psychiatry and Behavioral Sciences, McGovern Medical School at UTHealth and Linda Gail Behavioral Health Research Fund. Center of Excellence on Mood Disorders (USA) is funded by the Pat Rutherford Jr Chair in Psychiatry, John S. Dunn Foundation and Anne and Don Fizer Foundation Endowment for Depression Research. Translational Psychiatry Laboratory (Brazil) is funded by grants from Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq), Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES), Fundação de Amparo à Pesquisa e Inovação do Estado de Santa Catarina (FAPESC), Instituto Cérebro e Mente and University of Southern Santa Catarina (UNESC).
Author information
Authors and Affiliations
Contributions
GS, BLM, MHT, and JQ contribute to conception and design, analysis and interpretation of clinical data, and final approval of the version to be published. GS performed biochemical assessments, data analysis and wrote the paper with input from all authors. APD assisted with statistical analysis and manuscript preparation. MKJ and JCS revised the paper critically for relevant intellectual content.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests, and the funding body had no role in the design of the study, collection and analysis of data, or decision to publish.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Scaini, G., Mason, B.L., Diaz, A.P. et al. Dysregulation of mitochondrial dynamics, mitophagy and apoptosis in major depressive disorder: Does inflammation play a role?. Mol Psychiatry 27, 1095–1102 (2022). https://doi.org/10.1038/s41380-021-01312-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41380-021-01312-w
This article is cited by
-
Morinda officinalis oligosaccharides mitigate depression-like behaviors in hypertension rats by regulating Mfn2-mediated mitophagy
Journal of Neuroinflammation (2023)
-
Identification of mitophagy-related biomarkers and immune infiltration in major depressive disorder
BMC Genomics (2023)
-
BNIP3L/NIX-mediated mitophagy alleviates passive stress-coping behaviors induced by tumor necrosis factor-α
Molecular Psychiatry (2023)
-
Does decreased autophagy and dysregulation of LC3A in astrocytes play a role in major depressive disorder?
Translational Psychiatry (2023)
-
Mitochondria-wide association study observed significant interactions of mitochondrial respiratory and the inflammatory in the development of anxiety and depression
Translational Psychiatry (2023)