Abstract
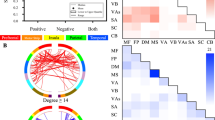
Opioid use disorder is a major public health crisis. While effective treatments are available, outcomes vary widely across individuals and relapse rates remain high. Understanding neural mechanisms of treatment response may facilitate the development of personalized and/or novel treatment approaches. Methadone-maintained, polysubstance-using individuals (n = 53) participated in fMRI scanning before and after substance-use treatment. Connectome-based predictive modeling (CPM)—a recently developed, whole-brain approach—was used to identify pretreatment connections associated with abstinence during the 3-month treatment. Follow-up analyses were conducted to determine the specificity of the identified opioid abstinence network across different brain states (cognitive vs. reward task vs. resting-state) and different substance use outcomes (opioid vs. cocaine abstinence). Posttreatment fMRI data were used to assess network changes over time and within-subject replication. To determine further clinical relevance, opioid abstinence network strength was compared with healthy subjects (n = 38). CPM identified an opioid abstinence network (p = 0.018), characterized by stronger within-network motor/sensory connectivity, and reduced connectivity between the motor/sensory network and medial frontal, default mode, and frontoparietal networks. This opioid abstinence network was anatomically distinct from a previously identified cocaine abstinence network. Relationships between abstinence and opioid and cocaine abstinence networks replicated across multiple brain states but did not generalize across substances. Network connectivity measured at posttreatment related to abstinence at 6-month follow-up (p < 0.009). Healthy comparison subjects displayed intermediate network strengths relative to treatment responders and nonresponders. These data indicate dissociable anatomical substrates of opioid vs. cocaine abstinence. Results may inform the development of novel opioid-specific treatment approaches to combat the opioid epidemic.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
McCarty D, Priest KC, Korthuis PT. Treatment and prevention of opioid use disorder: Challenges and opportunities. Annu Rev Public Health. 2018;39:525–41.
McCabe SE, West BT, Jutkiewicz EM, Boyd CJ. Multiple DSM-5 substance use disorders: a national study of US adults. Hum Psychopharmacol. Clin. 2017;32:e2625.
Van den Brink W, Haasen C. Evidenced-based treatment of opioid-dependent patients. Can J Psychiatry. 2006;51:635–46.
Connery HS. Medication-assisted treatment of opioid use disorder: review of the evidence and future directions. Harv Rev Psychiatry. 2015;23:63–75.
Moningka H, Lichenstein S, Worhunsky PD, DeVito EE, Scheinost D, Yip SW. Can neuroimaging help combat the opioid epidemic? A systematic review of clinical and pharmacological challenge fMRI studies with recommendations for future research. Neuropsychopharmacology. 2019;44:259–73.
Stewart JL, May AC, Aupperle RL, Bodurka J. Forging neuroimaging targets for recovery in opioid use disorder. Front Psychiatry. 2019;10:117.
Castells X, Kosten TR, Capella D, Vidal X, Colom J, Casas M. Efficacy of opiate maintenance therapy and adjunctive interventions for opioid dependence with comorbid cocaine use disorders: a systematic review and meta-analysis of controlled clinical trials. Am J Drug Alcohol Abuse. 2009;35:339–49.
Lorvick J, Browne EN, Lambdin BH, Comfort M. Polydrug use patterns, risk behavior and unmet healthcare need in a community-based sample of women who use cocaine, heroin or methamphetamine. Addict Behav. 2018;85:94–9.
Leri F, Bruneau J, Stewart J. Understanding polydrug use: review of heroin and cocaine co-use. Addiction. 2003;98:7–22.
Moeller SJ, Paulus MP. Toward biomarkers of the addicted human brain: Using neuroimaging to predict relapse and sustained abstinence in substance use disorder. Prog Neuropsychopharmacol Biol Psychiatry. 2018;80(Pt B):143–54.
Shen X, Finn ES, Scheinost D, Rosenberg MD, Chun MM, Papademetris X, et al. Using connectome-based predictive modeling to predict individual behavior from brain connectivity. Nat Protoc. 2017;12:506–18.
Finn ES, Shen X, Scheinost D, Rosenberg MD, Huang J, Chun MM, et al. Functional connectome fingerprinting: identifying individuals using patterns of brain connectivity. Nat Neurosci. 2015;18:1664–71.
Yip SW, Scheinost D, Potenza MN, Carroll KM. Connectome-based prediction of cocaine abstinence. Am J Psychiatry. 2019;175:156–64.
Ahn WY, Vassileva J. Machine-learning identifies substance-specific behavioral markers for opiate and stimulant dependence. Drug Alcohol Depend. 2016;161:247–57.
Epstein DH, Willner-Reid J, Vahabzadeh M, Mezghanni M, Lin JL, Preston KL. Real-time electronic diary reports of cue exposure and mood in the hours before cocaine and heroin craving and use. Arch Gen Psychiatry. 2009;66:88–94.
De Pirro S, Galati G, Pizzamiglio L, Badiani A. The affective and neural correlates of heroin versus cocaine use in addiction are influenced by environmental setting but in opposite directions. J Neurosci. 2018;38:5182–95.
Greene A, Gao S, Scheinost D, Constable R. Task-induced brain state manipulation improves prediction of individual traits. Nat Commun. 2018;9:2807.
Rosenberg MD, Finn ES, Scheinost D, Papademetris X, Shen X, Constable RT, et al. A neuromarker of sustained attention from whole-brain functional connectivity. Nat Neurosci. 2016;19:165–71.
Rosenberg MD, Hsu WT, Scheinost D, Todd Constable R, Chun MM. Connectome-based models predict separable components of attention in novel individuals. J Cogn Neurosci. 2018;30:160–73.
Rosenberg MD, Zhang S, Hsu WT, Scheinost D, Finn ES, Shen X, et al. Methylphenidate modulates functional network connectivity to enhance attention. J Neurosci. 2016;36:9547–57.
Finn ES, Scheinost D, Finn DM, Shen X, Papademetris X, Constable RT. Can brain state be manipulated to emphasize individual differences in functional connectivity? Neuroimage. 2017;160:140–51.
Garavan H, Brennan KL, Hester R, Whelan R. The neurobiology of successful abstinence. Curr Opin Neurobiol. 2013;23:668–74.
Andrews MM, Meda SA, Thomas AD, Potenza MN, Krystal JH, Worhunsky P, et al. Individuals family history positive for alcoholism show functional magnetic resonance imaging differences in reward sensitivity that are related to impulsivity factors. Biol Psychiatry. 2011;69:675–83.
Scheinost D, Noble S, Horien C, Greene AS, Lake EMR, Salehi M, et al. Ten simple rules for predictive modeling of individual differences in neuroimaging. Neuroimage. 2019;193:35–45.
Varoquaux G, Raamana PR, Engemann DA, Hoyos-Idrobo A, Schwartz Y, Thirion B. Assessing and tuning brain decoders: cross-validation, caveats, and guidelines. Neuroimage. 2017;145:166–79.
Badiani A, Belin D, Epstein D, Calu D, Shaham Y. Opiate versus psychostimulant addiction: the differences do matter. Nat Rev Neurosci. 2011;12:685–700.
Vassileva J, Conrod PJ. Impulsivities and addictions: a multidimensional integrative framework informing assessment and interventions for substance use disorders. Philos Trans R Soc Lond B Biol Sci. 2019;374:20180137.
George O, Koob GF. Individual differences in the neuropsychopathology of addiction. Dialogues Clin Neurosci. 2017;19:217–29.
Yalachkov Y, Kaiser J, Naumer MJ. Sensory and motor aspects of addiction. Behav Brain Res. 2010;207:215–22.
Volkow ND, Boyle M. Neuroscience of addiction: relevance to prevention and treatment. Am J Psychiatry. 2018. https://doi.org/10.1176/appi.ajp.2018.17101174.
Shi Z, Jagannathan K, Wang AL, Fairchild VP, Lynch KG, Suh JJ, et al. Behavioral and accumbal responses during an affective go/no-go task predict adherence to injectable naltrexone treatment in opioid use disorder. Int J Neuropsychopharmacol. 2019;22:180–5.
Wang AL, Elman I, Lowen SB, Blady SJ, Lynch KG, Hyatt JM, et al. Neural correlates of adherence to extended-release naltrexone pharmacotherapy in heroin dependence. Transl Psychiatry. 2015;5:e531.
Barreno EM, Dominguez-Salas S, Diaz-Batanero C, Lozano OM, Marin JAL, Verdejo-Garcia A. Specific aspects of cognitive impulsivity are longitudinally associated with lower treatment retention and greater relapse in therapeutic community treatment. J Subst Abus Treat. 2019;96:33–8.
Worhunsky PD, Stevens MC, Carroll KM, Rounsaville BJ, Calhoun VD, Pearlson GD, et al. Functional brain networks associated with cognitive control, cocaine dependence, and treatment outcome. Psychol Addict Behav. 2013;27:477–88.
Acknowledgements
This work was supported by grants K01DA039299, R21DA045969, P50DA09241 T32DA022975, and R01DA035058 from the National Institute on Drug Abuse. Data reported here have been presented at the American College of Neuropsychopharmacology’s 57th Annual Meeting, at the Collaborative Perspectives on Addiction 2019 Annual Meeting, and are scheduled for additional oral presentation at the Society for Biological Psychiatry’s 74th Annual Scientific Meeting, and the College on Problems of Drug Dependence (CPDD) 81st Annual Scientific Meeting.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
SDL, DS, and SWY report no financial relationships with commercial interest. KMC has received multiple grants from NIDA and NIAAA. She is a member of CBT4CBT LLC; this is managed through University. MNP has received financial support or compensation for the following: MNP has consulted for and advised RiverMend Health and Opiant/Lakelight Therapeutics; has received unrestricted research support from Mohegan Sun Casino and grant support from the National Center for Responsible Gaming; and has consulted for legal and gambling entities on issues related to addictive disorders.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Lichenstein, S.D., Scheinost, D., Potenza, M.N. et al. Dissociable neural substrates of opioid and cocaine use identified via connectome-based modelling. Mol Psychiatry 26, 4383–4393 (2021). https://doi.org/10.1038/s41380-019-0586-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41380-019-0586-y
This article is cited by
-
Neuromarkers in addiction: definitions, development strategies, and recent advances
Journal of Neural Transmission (2024)
-
Distinct neural networks predict cocaine versus cannabis treatment outcomes
Molecular Psychiatry (2023)
-
Densely sampled neuroimaging for maximizing clinical insight in psychiatric and addiction disorders
Neuropsychopharmacology (2022)
-
Antagonistic network signature of motor function in Parkinson’s disease revealed by connectome-based predictive modeling
npj Parkinson's Disease (2022)
-
Functional connectivity during frustration: a preliminary study of predictive modeling of irritability in youth
Neuropsychopharmacology (2021)