Abstract
In the first phase 3 study in relapsed/refractory AL amyloidosis (TOURMALINE-AL1 NCT01659658), 168 patients with relapsed/refractory AL amyloidosis after 1–2 prior lines were randomized to ixazomib (4 mg, days 1, 8, 15) plus dexamethasone (20 mg, days 1, 8, 15, 22; n = 85) or physician’s choice (dexamethasone ± melphalan, cyclophosphamide, thalidomide, or lenalidomide; n = 83) in 28-day cycles until progression or toxicity. Primary endpoints were hematologic response rate and 2-year vital organ deterioration or mortality rate. Only the first primary endpoint was formally tested at this interim analysis. Best hematologic response rate was 53% with ixazomib–dexamethasone vs 51% with physician’s choice (p = 0.76). Complete response rate was 26 vs 18% (p = 0.22). Median time to vital organ deterioration or mortality was 34.8 vs 26.1 months (hazard ratio 0.53; 95% CI, 0.32–0.87; p = 0.01). Median treatment duration was 11.7 vs 5.0 months. Adverse events of clinical importance included diarrhea (34 vs 30%), rash (33 vs 20%), cardiac arrhythmias (26 vs 15%), nausea (24 vs 14%). Despite not meeting the first primary endpoint, all time-to-event data favored ixazomib–dexamethasone. These results are clinically relevant to this relapsed/refractory patient population with no approved treatment options.
Similar content being viewed by others

Introduction
Immunoglobulin light chain systemic light-chain (AL) amyloidosis is a rare clonal plasma-cell disorder that produces misfolded immunoglobulin light-chain proteins, which aggregate and deposit as amyloid fibrils in tissues/organs, leading to multi-organ dysfunction [1,2,3]. The most frequently involved organs are the heart and kidney [1, 4]. Prognosis is generally poor: in patients with advanced cardiac involvement, survival is limited to 4–6 months [4, 5]. Among all patients, 24% will die within 6 months of diagnosis and only 5–31% will survive for 10 years [6,7,8,9,10]. Autologous stem cell transplant achieves the best long-term outcomes for AL amyloidosis patients, although most patients are ineligible due to poor physical condition [11,12,13,14,15].
When this trial was designed, there were no approved or standard-of-care treatments for AL amyloidosis. Since completion of this trial, daratumumab has been approved as part of a cyclophosphamide, bortezomib, dexamethasone treatment for newly diagnosed patients [16]. No drug is approved for AL amyloidosis as second line therapy. Management of AL amyloidosis is primarily based on off-label use of therapies for multiple myeloma (MM) [11, 17], and with these treatments, deeper hematologic responses have been associated with organ responses and prolonged overall survival (OS) [3, 11, 18, 19]. Proteasome inhibitor (PI)-based combinations have demonstrated activity in newly diagnosed and relapsed/refractory AL amyloidosis [12, 15, 20]; however, treatment with certain PIs may be challenging due to burden of administration, comorbidities, organ dysfunction, or toxicity concerns [12, 15]. New, active treatments that are tolerable in the context of multi-organ dysfunction are needed.
TOURMALINE-AL1 is the first phase 3 study in relapsed/refractory AL amyloidosis and investigates ixazomib–dexamethasone vs physician’s choice of treatment. The oral PI ixazomib is approved in more than 65 countries in combination with lenalidomide–dexamethasone to treat MM after ≥1 prior therapy [21,22,23]. In a phase 1/2 study in relapsed/refractory AL amyloidosis, ixazomib appeared active and well tolerated in 27 patients (10 of whom received added dexamethasone) with a hematologic response rate of 52% (100% in PI-naïve patients [n = 5]) and organ response rate of 56% [24]. Here we report results of TOURMALINE-AL1 in order to further our understanding of treatment of this rare disease.
Patients and methods
Study design
TOURMALINE-AL1 is a phase 3, randomized, open-label study conducted in 68 sites across 19 countries in Europe, North America, Latin America, and Asia-Pacific. Adult patients with biopsy-proven AL amyloidosis and major organ (cardiac and/or renal) involvement by International Society of Amyloidosis (ISA) criteria [25] were eligible. Patients had to have relapsed/refractory disease after 1–2 prior therapies. Patients could have prior exposure but not be refractory to PI therapy. Full eligibility criteria are in the Supplementary Appendix.
The study was conducted in accordance with Good Clinical Practice and applicable regulatory requirements. Local ethics committees/institutional review boards approved the protocol. Patients provided written informed consent. Data were analyzed by the sponsor; authors had access to the data. During the study, the sponsor and the trial-monitoring component of the contract research organization, and the Independent Review Committee remained blinded to the efficacy data. The trial was registered at ClinicalTrials.gov as NCT01659658.
Procedures
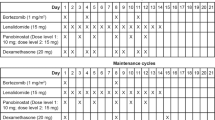
Patients were randomized 1:1 to receive oral ixazomib (4 mg) on days 1, 8, and 15 plus oral dexamethasone 20 mg/day on days 1, 8, 15, and 22, or physician’s choice in 28-day cycles.
For physician’s choice, investigators selected a dexamethasone-based non-PI-containing regimen from a prespecified list; the choice for each screened patient was made prior to randomization. The choices included dexamethasone alone 20 mg/day by mouth (PO), days 1–4, 9–12, and 17–20; dexamethasone 20 mg/day PO, days 1–4, plus melphalan 0.22 mg/kg PO, days 1–4; dexamethasone 20 mg/day PO, days 1, 8, 15, and 22, plus cyclophosphamide 500 mg PO, days 1, 8, and 15; dexamethasone 20 mg/day PO, days 1, 8, 15, and 22, plus thalidomide 50–200 mg/day PO (starting dose 50 mg/day, increased as tolerated); dexamethasone 20 mg/day PO, days 1, 8, 15, and 22, plus lenalidomide 15 mg/day, days 1–21. Regimens were given in 28-day cycles with dose adjustments based on toxicities; dexamethasone could be increased up to 40 mg/day on days 1, 8, 15, and 22 after 4 weeks, if the lower dose was tolerated without grade >2 dexamethasone-related toxicities.
Patients were treated until disease progression/death or unacceptable toxicity, or study termination, whichever occurred first. Patients receiving melphalan–dexamethasone were treated until best response (defined as a the deepest response achieved) plus 2 additional cycles, or to a maximum of 18 months of therapy or 600 mg total dose of melphalan, given the increased risk of second primary malignancies with prolonged melphalan use noted in the melphalan package insert [26]. Crossover from physician’s choice to ixazomib–dexamethasone was not permitted.
Conduct was overseen by a steering committee. Randomization was stratified by Mayo 2004 cardiac risk stage (1 vs 2 vs a subgroup of 3, based on cardiac biomarkers) [5], relapsed vs refractory disease, and prior PI exposure (naïve vs exposed). The randomization scheme was generated by an independent statistician, with treatment assignment via an Interactive Voice Response System.
Outcomes and assessments
The original co-primary endpoints were best overall hematologic response rate (partial response or better), based on central laboratory results and 2010 ISA criteria [19], and OS. After discussion with regulatory agencies, and considering the methods by which patients are treated and the intention to demonstrate a meaningful measure of clinical benefit, OS was replaced by the novel endpoint of 2-year vital organ (heart and kidney) deterioration or mortality rate as the co-primary endpoint. Cardiac deterioration was defined as the need for hospitalization for heart failure; kidney deterioration was defined as progression to end-stage renal disease requiring maintenance dialysis or renal transplantation. Key secondary endpoints were OS, and hematologic complete response (CR) rate by central laboratory results and ISA criteria. Other secondary endpoints included: hematologic progression-free survival (PFS), vital organ (heart/kidney) PFS, overall (hematologic and/or vital organ) PFS, time to vital organ deterioration and mortality, vital organ best response, duration of hematologic response, time to treatment failure (death, hematologic or major organ progression, hematologic response with stable but clinically morbid organ disease requiring additional therapy, or withdrawal for any reason) time to subsequent anticancer treatment, adverse events (AEs), and serious AEs (SAEs). Full details are provided in the Supplementary Appendix.
Response was evaluated according to central laboratory results and the ISA’s Revised Consensus Response Criteria, as evaluated by a blinded adjudication committee [19]. Hematologic response was assessed every cycle from the date of first dose until end of treatment and every 6 weeks thereafter until documented progression or initiation of subsequent therapy. Organ response was assessed after cycles 3, 6, 9, and 12 and then every 3 cycles thereafter until disease progression or the initiation of subsequent therapy. Best response was defined as a plateau in deepest response achieved. After disease progression, patients were followed for overall survival and subsequent therapy at least every 12 weeks. AEs were graded according to the National Cancer Institute’s Common Terminology Criteria for Adverse Events, version 4.03. AEs were assessed from first dose through 30 days after administration of the last dose of study drug or the start of subsequent anticancer therapy, whichever occurred first. After consultation with regulatory authorities, the protocol was amended in July 2015 to exclude enrollment of PI-exposed patients, to balance the treatment arms, with a target ratio of approximately 50:50 PI-exposed vs PI-naïve patients.
Statistical analysis
The 2 primary endpoints and key secondary endpoints were planned to be tested sequentially to control family-wise error rate. Assuming a hazard ratio (HR) of 0.63, a total sample size of 248 (145 death events) was determined to give 80% power to test OS at a 2-sided alpha of 0.05. As this sample size also gave adequate power to test the endpoints of overall hematologic response rate and 2-year vital organ deterioration or mortality rate, which later became the co-primary endpoints, sample size based on the OS endpoint was retained as the final sample size for the study. There were two planned interim analyses (IA) and one final analysis. The first IA (IA1) was planned when ~176 patients (power was 90%, assuming 65 and 40% responses in ixazomib–dexamethasone and physicians’ choice arms; see Supplementary methods for justification of assumptions) had completed 6 cycles or had discontinued beforehand to test hematologic response at 0.04 alpha and 2-year vital organ deterioration and mortality rate at 0.01. The second IA was planned when 218 patients had completed 2 years of treatment or discontinued, to test 2-year vital organ deterioration and mortality rate with appropriate alpha carried over from IA1. The final IA was to test OS followed by hematologic CR rate with appropriate alpha carried over from the second IA. As the study did not meet the first primary endpoint at IA1, conducted with data from 168 patients, enrollment was stopped on June 5, 2019.
All efficacy data are reported for the intent-to-treat population. For binary endpoints, arms were compared using an unstratified Cochran–Mantel–Haenszel (CMH) test; a logistic regression model was used to estimate treatment effect and two-sided 95% confidence intervals (CIs). For time-to-event endpoints, arms were compared using a two-sided, stratified log-rank test; an unadjusted stratified Cox model was used to estimate HRs and two-sided 95% CIs. Safety data are reported descriptively in the safety population (patients who received ≥1 dose). Missing data were treated as missing with no data imputation; for the primary endpoints, missing data were counted as failures. SAS version 9.1 (or higher) was used for all analyses.
Results
Patients
Between December 2012 and August 2018, 168 patients were randomized to receive ixazomib–dexamethasone (n = 85) or physician’s choice (n = 83) (Supplementary Fig. 1). Physician’s choice regimens were lenalidomide–dexamethasone (n = 47), melphalan–dexamethasone (n = 24), cyclophosphamide–dexamethasone (n = 10), and thalidomide–dexamethasone (n = 2); no patients received dexamethasone alone. Baseline characteristics were well balanced between treatment arms (Table 1).
Efficacy
At data cut-off (February 20, 2019), all patients had completed 6 cycles of treatment or discontinued beforehand, and IA1 was performed. Best hematologic responses were seen in 53% (45/85; 95% CI, 41.8–63.9) of ixazomib–dexamethasone vs 51% (42/83; 95% CI, 39.4–61.8) of physician’s choice patients (unstratified CMH p = 0.76); the first primary endpoint was therefore not met. Hematologic CR rate (key secondary endpoint) was 26% (22/85) vs 18% (15/83) (odds ratio, 1.58; 95% CI, 0.76–3.32, p = 0.22; Table 2). Hematologic responses by physician’s choice of treatment are presented in Supplementary Table 1 and by baseline characteristics in Fig. 1. Response rate was 63% (29/46) vs 50% (22/44) in PI-naïve patients (favoring ixazomib–dexamethasone) and 41% (16/39) vs 51% (20/39) (favoring physician’s choice) in PI-exposed patients (Table 3). Among all patients, median duration of hematologic response was 46.5 months (ixazomib–dexamethasone) vs 20.2 months (physician’s choice) (HR, 0.55; 95% CI, 0.26–1.18; p = 0.12).
Best vital organ responses occurred in 36% (31/85) of ixazomib–dexamethasone and 11% (9/83) of physician’s choice patients; cardiac-only response rate was 18% (15/85) vs 5% (4/83) and renal-only response rate was 28% (24/85) vs 7% (6/83) (Table 2). Two-year vital organ deterioration and mortality rate (second primary endpoint) data were immature; 47 (30%) patients had not yet completed 2-year follow-up. Time to vital organ deterioration or mortality was longer with ixazomib–dexamethasone than physician’s choice (median, 34.8 vs 26.1 months; HR, 0.53; 95% CI, 0.32–0.87; p = 0.01) (Fig. 2a and by stratification factors in Fig. 2b). Among the subset of patients with 2 years of follow-up, 40% (26/65) of ixazomib–dexamethasone and 45% (25/56) of physician’s choice patients had a vital organ deterioration or mortality event.
a Time to vital organ deterioration or mortality (investigator assessed)—defined as time from randomization to vital organ (heart or kidney) deterioration (evaluated according to central laboratory results and International Society of Amyloidosis criteria) or death, whichever occurred first. Cardiac deterioration was defined as the need for hospitalization for heart failure. Kidney deterioration was defined as progression to end-stage renal disease with the need for maintenance dialysis or renal transplantation. Patients without documentation of organ deterioration or death were censored at the date of the last assessment. b Time to vital organ deterioration and mortality by randomization stratification factors (investigator assessed). CI confidence interval, HR hazard ratio, NE not estimable.
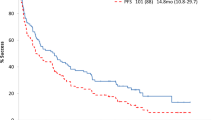
Median time to treatment failure was 10.1 months (ixazomib–dexamethasone) vs 5.2 months (physician’s choice) (HR, 0.60; 95% CI, 0.42–0.86; p = 0.005) (Fig. 3a); median time to subsequent therapy was 26.5 vs 12.5 months (HR, 0.61; 95% CI, 0.40–0.95; p = 0.03) (Fig. 3b). Median overall PFS was 11.2 vs 7.4 months (HR, 0.67; 95% CI, 0.46–0.99; p = 0.04) (Fig. 4a), hematologic PFS was 29.5 vs 27.7 months (HR, 0.76; 95% CI, 0.48–1.21; p = 0.24), and organ PFS was 18.0 vs 11.0 months (HR, 0.62; 95% CI, 0.41–0.93; p = 0.02). After 45.3 months median OS follow-up for ixazomib–dexamethasone and 43.4 months for physician’s choice, median OS was not reached vs 40.8 months (HR, 0.84; 95% CI, 0.51–1.37; p = 0.48) (Fig. 4b).
a Time to treatment failure—defined as time from randomization to death due to any cause, hematologic or major organ progression (evaluated according to central laboratory results and International Society of Amyloidosis criteria), clinically morbid organ disease requiring additional therapy, or withdrawal for any reason. Patients without documentation of treatment failure were censored at the date of last response assessment. b Time to subsequent therapy—defined as time from randomization to the start of subsequent anticancer treatment. Patients without subsequent anticancer therapy were censored at the date of death or the last date they were known to be alive. CI confidence interval, HR hazard ratio.
a Overall (hematologic and/or vital organ) progression-free survival (investigator assessed)—defined as time from randomization to first documentation of hematologic disease progression or vital organ (heart or kidney) progression, or death due to any cause, whichever occurred first. Patients without documentation of hematologic disease progression and organ progression were censored at the date of last hematologic response assessment that was stable disease or better, or the date of last organ assessment of stable disease or better, whichever occurred last. b Overall survival—defined as time from randomization to date of death. Patients without documentation of death at the time of analysis were censored at the date last known to be alive. CI confidence interval, HR hazard ratio, NE not estimable.
Time-to-event outcomes by prior PI exposure are shown in Supplementary Fig. 2. Median time to vital organ deterioration or mortality in PI-naïve patients was 44.9 months (ixazomib–dexamethasone n = 46) vs 28.0 months (physician’s choice n = 44) (HR, 0.53) and 27.0 vs 26.1 months in PI-exposed patients (n = 39 vs n = 39; HR, 0.52). Median OS in PI-naïve patients was not reached (ixazomib–dexamethasone) vs 71.1 months (physician’s choice) (HR, 0.81), and 40.9 vs 32.4 months in PI-exposed patients (HR, 0.85). HRs were 0.46–0.85 in favor of ixazomib–dexamethasone vs physician’s choice in both PI-naïve and PI-exposed patients.
Safety
Median treatment duration was 11.7 months (ixazomib–dexamethasone) vs 5.0 months (physician’s choice) (HR, 0.46; 95% CI, 0.32–0.67). Of 24 patients receiving melphalan–dexamethasone, 4 stopped treatment according to protocol for melphalan. The safety population comprised all ixazomib–dexamethasone patients and 81 physician’s choice patients (Supplementary Fig. 1). Safety is summarized in Supplementary Table 2; grade ≥3 AEs were experienced by 62% (53/85) of ixazomib–dexamethasone and 56% (45/81) of physician’s choice patients. Any-grade AEs of clinical importance in ixazomib–dexamethasone versus physician’s choice patients included diarrhea (34 vs 30%), rash (33 vs 20%), cardiac arrhythmias (26 vs 15%, of which 8 vs 1% were due to non-drug-related atrial fibrillation), nausea (24 vs 14%), pneumonia (21 vs 16%), and peripheral neuropathy (19 vs 15%) (Table 4). The most common (>5% overall) grade ≥3 AEs were fatigue (9% in both arms), anemia (2 vs 11%), and cardiac failure and dyspnea (each 6 vs 4%). Events by total person years on treatment were 544 with ixazomib–dexamethasone vs 1400 with physician’s choice.
SAEs were reported in 47% (40/85) of ixazomib–dexamethasone vs 33% (27/81) of physician’s choice patients; SAEs occurring in ≥5% of patients in either arm were pneumonia (5 vs 5%) and dyspnea (5 vs 1%). AEs resulting in discontinuation were reported in 26% (22/85) vs 20% (16/81) of patients. Five patients (6%) receiving ixazomib–dexamethasone and 4 (5%) receiving physician’s choice died on-study (Supplementary Table 2); all deaths were considered related to AL amyloidosis or complications thereof, and all patients had pre-existing cardiac disease.
Discussion
Randomized controlled trials in AL amyloidosis are scarce due to the rarity of the disease, and there are no standard primary endpoints for AL amyloidosis. TOURMALINE-AL1 is the first randomized phase 3 trial to be conducted in relapsed/refractory AL amyloidosis. It provides clinically meaningful data for patients and physicians that can inform treatment choices and further scientific understanding of this rare disease, and it also highlights the challenges associated with clinical trial design and recruitment in this setting. All time-to-event data favored ixazomib–dexamethasone over physician’s choice regimens. Ixazomib–dexamethasone was well tolerated (no new safety signals seen compared to prior studies in AL amyloidosis and relapsed/refractory MM) [24, 27], enabling twice as long a treatment duration vs physician’s choice.
As the first phase 3 trial in this setting, several elements of the study design are noteworthy. This trial was designed in 2012, working collaboratively with regulatory agencies and the amyloidosis medical community to design a clinically meaningful study for this patient population. The novel composite endpoint of 2-year vital organ deterioration and mortality rate was formulated despite a lack of historical data on which to base statistical assumptions. Assumptions relating to power had to be based on data from small, single-arm studies, many of which had enrolled both treatment-naïve and relapsed/refractory patients. Furthermore, hematologic response rate was chosen as the first primary endpoint based on feedback from experts in the field, as an endpoint believed to be a surrogate for clinical benefit. At the time of study design, however, hematologic response rate was being validated in newly diagnosed rather than relapsed/refractory AL amyloidosis. This study could have helped validate it in relapsed/refractory patients [28]. The choice of control arm was complicated by the absence of agreed standards of care because there were no preceding randomized trials in the relapsed setting. The choice of control arm was determined based upon the consensus of the best available options, globally, at the time of trial design, according to amyloidosis experts’ advice. Thus, an additive trial design per those conventionally used in multiple myeloma—of investigating novel doublet versus single-agent, or novel triplet versus standard-of-care doublet—was not feasible at the time in this setting. Over the course of the trial, which was prolonged due to the rarity of the disease and the difficulty in recruiting patients who were bortezomib-naïve hindering accrual, the widespread and increased application of approved multiple myeloma regimens may have in part affected outcomes. The benefit and tolerability ixazomib–dexamethasone demonstrated in PI-exposed patients suggest that this regimen may represent a valid option in relapsed-refractory patients previously exposed to daratumumab and bortezomib.
In the treatment of newly diagnosed AL amyloidosis, deeper hematologic responses are associated with improved organ response and OS, and organ responses are linked with improved prognosis [3, 11, 18, 19, 29, 30]. Responses were deeper (CR, 26 vs 18%) and more durable (median, 46.5 vs 20.2 months) with ixazomib–dexamethasone vs physicians’ choice, although the overall hematologic response rate was similar between arms (53 vs 51%). Consistently, best vital organ response rates were higher with ixazomib–dexamethasone vs physician’s choice (36 vs 11%), although organ response assessment based on NT-proBNP levels per ISA criteria may have underestimated rates in patients receiving lenalidomide–dexamethasone due to NT-proBNP-increases observed with immunomodulatory drugs [31].
Notably, the hematologic response reported with ixazomib–dexamethasone is consistent with the 52% rate reported in the phase 1/2 study of ixazomib in relapsed/refractory AL amyloidosis in which patients with less than a partial response after 3 cycles received added dexamethasone [24]. Historically, hematologic response rates with dexamethasone alone are 35–40% (albeit using different response criteria and including both newly diagnosed and pretreated patients [32, 33]), suggesting a clear treatment effect with ixazomib. For comparison, hematologic response rates of 39–69% have been reported for single-agent bortezomib in PI-naïve relapsed AL amyloidosis [34]. In this phase 3 study, hematologic responses by regimen in the physician’s choice arm were consistent (range, 50–58%), except for cyclophosphamide–dexamethasone (30%), although the small numbers of patients preclude meaningful conclusions. Similarly, small subgroups and wide confidence intervals did not allow confirmation of any differences in hematologic response rates according to patients’ baseline characteristics. The statistical assumption of a 40% hematologic response rate for physician’s choice was based on data from single-arm studies [35,36,37,38,39,40,41] (which often included a mix of newly diagnosed and relapsed patients) and assumed equal enrollment across all regimens. The fact that no patients received a physician’s choice of dexamethasone alone and that nearly a third of patients received the melphalan and dexamethasone combination, which resulted in a 58% response rate (predominant in countries where melphalan would not have been available outside of this clinical trial), and over half of patients received lenalidomide plus dexamethasone, which resulted in a 51% response rate (predominant in countries where lenalidomide would not have been available outside of this clinical trial) could account for the higher-than-expected response rate. Since an additive trial design was not feasible at the time of study design, this resulted in the ixazomib–dexamethasone doublet being compared against two effective doublets, melphalan plus dexamethasone and lenalidomide plus dexamethasone, as a result of the evolving standards of care in the relapsed/refractory AL amyloidosis setting.
The second primary endpoint of the rate of 2-year vital organ deterioration and mortality was lower with ixazomib–dexamethasone vs physician’s choice (40 vs 45%) in evaluable patients. Further, time to vital organ deterioration and mortality was numerically longer with ixazomib–dexamethasone vs physician’s choice (events 37 vs 40; HR, 0.53; 95% CI, 0.32–0.87). With only 40% of OS events reached, there was a trend for an improvement in OS (HR, 0.84; 95% CI, 0.51–1.37). While the hematologic response rate in PI-exposed patients favored treatment with physician’s choice, the HRs for longer-term outcomes of time to vital organ deterioration and mortality and OS favored ixazomib–dexamethasone in both PI-naïve and PI-exposed populations. The magnitude of benefit with ixazomib–dexamethasone vs physician’s choice was greater in PI-naïve patients vs PI-exposed patients, which is expected based on the previous phase 1/2 study of ixazomib (± dexamethasone) in relapsed/refractory AL amyloidosis in which PI-naïve patients had a median hematologic PFS of 25.8 months compared with 10.7 months in PI-exposed patients [24]. It is also consistent with a phase 2 study of ixazomib–dexamethasone in relapsed MM in which the median event-free survival in bortezomib-naïve patients was double that in bortezomib-exposed patients [42]. The benefit demonstrated with ixazomib–dexamethasone vs physician’s choice in PI-exposed patients in this phase 3 study, provides important information for patients who have previously received a PI and their treating physicians. This represents a clinically relevant benefit in this setting, given the paucity of treatment options with no standard of care available. Across all patients, all other time-to-event endpoints including overall and organ PFS, time-to-treatment failure, and time to subsequent therapy were numerically longer with ixazomib–dexamethasone over physician’s choice.
Safety was similar between the 2 arms, with AEs reported for ixazomib–dexamethasone consistent with the known ixazomib safety profile [24, 42, 43]. Rash and peripheral neuropathy were more common with ixazomib–dexamethasone, but events were mainly low-grade. The increase in cardiac arrhythmias in the ixazomib–dexamethasone arm (26 vs 15%) is thought to be a result of the higher frequency of non-drug-related atrial fibrillation in patients with cardiac involvement (8 vs 1%) or longer exposure to drug. Numerically higher rates of SAEs and AEs resulting in discontinuation were reported with ixazomib–dexamethasone vs physician’s choice; however, this was not surprising given that patients received ixazomib–dexamethasone for twice as long as physician’s choice. On-study deaths were similar between arms; none were considered related to treatment.
Long-term treatment with certain PIs may be challenging for some patients due to burden of administration, comorbidities, organ dysfunction, or toxicity [12, 15]. Peripheral neuropathy is a known side effect with bortezomib and, as such, bortezomib is not recommended for patients with existing grade 3–4 neuropathy [15]; although rates of such events appear reduced with subcutaneous dosing [44]. Carfilzomib has been investigated in a phase 1/2 study in relapsed/refractory AL amyloidosis. Hematologic response rate was 63%; however, cardiac, pulmonary, and renal toxicities were common, and may limit the use of carfilzomib in this setting [45]. Data from TOURMALINE-AL1 demonstrate that ixazomib–dexamethasone is generally well tolerated in AL amyloidosis with a clinically relevant treatment duration (enabling deeper hematologic responses and higher organ response rates than physician’s choice), thereby providing patients with a potential longer-term PI-based treatment option.
TOURMALINE-AL1, the first phase 3 trial in relapsed/refractory AL amyloidosis, demonstrates outcome improvements with ixazomib–dexamethasone vs physician’s choice in evaluable patients. Ixazomib–dexamethasone prolonged time to vital organ deterioration and mortality, PFS, and time to subsequent therapy vs physician’s choice in patients with relapsed/refractory AL amyloidosis. Ixazomib–dexamethasone also improved the depth and duration of response, although the first primary endpoint of overall hematologic response rate was not met. Treatment with ixazomib–dexamethasone was generally well tolerated, enabling patients to receive treatment for twice as long as physician’s choice. The time-to-event data suggest that ixazomib–dexamethasone may benefit patients with relapsed/refractory AL amyloidosis who have limited treatment options.
Data availability
The datasets, including the redacted study protocol, redacted statistical analysis plan, and individual participants’ data supporting the results reported in this article, will be made available within three months from initial request, to researchers who provide a methodologically sound proposal. The data will be provided after its de-identification, in compliance with applicable privacy laws, data protection and requirements for consent and anonymization.
References
Grogan M, Dispenzieri A, Gertz MA. Light-chain cardiac amyloidosis: strategies to promote early diagnosis and cardiac response. Heart. 2017;103:1065–72.
Kastritis E, Dimopoulos MA. Recent advances in the management of AL Amyloidosis. Br J Haematol. 2016;172:170–86.
Merlini G, Seldin DC, Gertz MA. Amyloidosis: pathogenesis and new therapeutic options. J Clin Oncol. 2011;29:1924–33.
Palladini G, Milani P, Merlini G. Novel strategies for the diagnosis and treatment of cardiac amyloidosis. Expert Rev Cardiovasc Ther. 2015;13:1195–211.
Dispenzieri A, Gertz MA, Kyle RA, Lacy MQ, Burritt MF, Therneau TM, et al. Serum cardiac troponins and N-terminal pro-brain natriuretic peptide: a staging system for primary systemic amyloidosis. J Clin Oncol. 2004;22:3751–7.
Gillmore JD, Wechalekar A, Bird J, Cavenagh J, Hawkins S, Kazmi M, et al. Guidelines on the diagnosis and investigation of AL amyloidosis. Br J Haematol. 2015;168:207–18.
Kyle RA, Gertz MA, Greipp PR, Witzig TE, Lust JA, Lacy MQ, et al. Long-term survival (10 years or more) in 30 patients with primary amyloidosis. Blood. 1999;93:1062–6.
Merlini G, Palladini G. Amyloidosis: is a cure possible? Ann Oncol. 2008;19:iv63–6.
Muchtar E, Gertz MA, Kumar SK, Lacy MQ, Dingli D, Buadi FK, et al. Improved outcomes for newly diagnosed AL amyloidosis between 2000 and 2014: cracking the glass ceiling of early death. Blood. 2017;129:2111–19.
Muchtar E, Gertz MA, Lacy MQ, Go RS, Buadi FK, Dingli D, et al. Ten-year survivors in AL amyloidosis: characteristics and treatment pattern. Br J Haematol. 2019;187:588–94.
Dispenzieri A, Buadi F, Kumar SK, Reeder CB, Sher T, Lacy MQ, et al. Treatment of immunoglobulin light chain amyloidosis: mayo stratification of myeloma and risk-adapted therapy (mSMART) consensus statement. Mayo Clin Proc. 2015;90:1054–81.
Gertz MA. Immunoglobulin light chain amyloidosis: 2018 update on diagnosis, prognosis, and treatment. Am J Hematol. 2018. https://doi.org/10.1002/ajh.25149.
Sidana S, Sidiqi MH, Dispenzieri A, Buadi FK, Lacy MQ, Muchtar E et al. Fifteen year overall survival rates after autologous stem cell transplantation for AL amyloidosis. Am J Hematol. 2019. https://doi.org/10.1002/ajh.25566.
Sidiqi MH, Aljama MA, Buadi FK, Warsame RM, Lacy MQ, Dispenzieri A, et al. Stem cell transplantation for light chain amyloidosis: Decreased early mortality over time. J Clin Oncol. 2018;36:1323–29.
Wechalekar AD, Gillmore JD, Bird J, Cavenagh J, Hawkins S, Kazmi M, et al. Guidelines on the management of AL amyloidosis. Br J Haematol. 2015;168:186–206.
Palladini G, Kastritis E, Maurer MS, Zonder J, Minnema MC, Wechalekar AD, et al. Daratumumab plus CyBorD for patients with newly diagnosed AL amyloidosis: safety run-in results of ANDROMEDA. Blood. 2020;136:71–80.
Palladini G, Merlini G. What is new in diagnosis and management of light chain amyloidosis? Blood. 2016;128:159–68.
Kaufman GP, Dispenzieri A, Gertz MA, Lacy MQ, Buadi FK, Hayman SR, et al. Kinetics of organ response and survival following normalization of the serum free light chain ratio in AL amyloidosis. Am J Hematol. 2015;90:181–6.
Palladini G, Dispenzieri A, Gertz MA, Kumar S, Wechalekar A, Hawkins PN, et al. New criteria for response to treatment in immunoglobulin light chain amyloidosis based on free light chain measurement and cardiac biomarkers: impact on survival outcomes. J Clin Oncol. 2012;30:4541–9.
Jelinek T, Kryukova E, Kufova Z, Kryukov F, Hajek R. Proteasome inhibitors in AL amyloidosis: focus on mechanism of action and clinical activity. Hematol Oncol. 2017;35:408–19.
Millennium Pharmaceuticals Inc. NINLARO® (ixazomib) capsules, for oral use. United States prescribing information (2016). https://www.ninlaro.com/downloads/prescribing-information.pdf.
Takeda Pharma a/S. NINLARO European Product Assessment Report – Summary of Product Characteristics. (2018).
Takeda Pharmaceutical Company. Takeda announces results from phase 3 clinical trial evaluating NINLARO™ (ixazomib) in newly diagnosed multiple myeloma. Takeda news release. (2020). https://www.takeda.com/newsroom/newsreleases/.
Sanchorawala V, Palladini G, Kukreti V, Zonder JA, Cohen AD, Seldin DC, et al. A phase 1/2 study of the oral proteasome inhibitor ixazomib in relapsed or refractory AL amyloidosis. Blood. 2017;130:597–605.
Sipe JD, Benson MD, Buxbaum JN, Ikeda SI, Merlini G, Saraiva MJ, et al. Amyloid fibril proteins and amyloidosis: chemical identification and clinical classification International Society of Amyloidosis 2016 Nomenclature Guidelines. Amyloid. 2016;23:209–13.
GlaxoSmithKline. ALKERAN®(melphalan) Tablets. United States prescribing information. 2007.
Moreau P, Masszi T, Grzasko N, Bahlis NJ, Hansson M, Pour L, et al. Oral Ixazomib, Lenalidomide, and Dexamethasone for Multiple Myeloma. N. Engl J Med. 2016;374:1621–34.
Comenzo RL, Reece D, Palladini G, Seldin D, Sanchorawala V, Landau H, et al. Consensus guidelines for the conduct and reporting of clinical trials in systemic light-chain amyloidosis. Leukemia. 2012;26:2317–25.
Kastritis E, Gavriatopoulou M, Roussou M, Migkou M, Fotiou D, Ziogas DC, et al. Renal outcomes in patients with AL amyloidosis: Prognostic factors, renal response and the impact of therapy. Am J Hematol. 2017;92:632–39.
Palladini G, Hegenbart U, Milani P, Kimmich C, Foli A, Ho AD, et al. A staging system for renal outcome and early markers of renal response to chemotherapy in AL amyloidosis. Blood. 2014;124:2325–32.
Dispenzieri A, Dingli D, Kumar SK, Rajkumar SV, Lacy MQ, Hayman S, et al. Discordance between serum cardiac biomarker and immunoglobulin-free light-chain response in patients with immunoglobulin light-chain amyloidosis treated with immune modulatory drugs. Am J Hematol. 2010;85:757–9.
Gertz MA, Lacy MQ, Lust JA, Greipp PR, Witzig TE, Kyle RA. Phase II trial of high-dose dexamethasone for untreated patients with primary systemic amyloidosis. Med Oncol. 1999;16:104–9.
Palladini G, Anesi E, Perfetti V, Obici L, Invernizzi R, Balduini C, et al. A modified high-dose dexamethasone regimen for primary systemic (AL) amyloidosis. Br J Haematol. 2001;113:1044–6.
Reece DE, Hegenbart U, Sanchorawala V, Merlini G, Palladini G, Blade J, et al. Long-term follow-up from a phase 1/2 study of single-agent bortezomib in relapsed systemic AL amyloidosis. Blood. 2014;124:2498–506.
Dispenzieri A, Lacy MQ, Geyer SM, Greipp PR, Witzig TE, Lust JA, et al. Low dose single agent thalidomide is tolerated in patients with primary systemic amyloidosis, but responses are limited. Blood. 2004;104:4920–20.
Dispenzieri A, Lacy MQ, Rajkumar SV, Geyer SM, Witzig TE, Fonseca R, et al. Poor tolerance to high doses of thalidomide in patients with primary systemic amyloidosis. Amyloid. 2003;10:257–61.
Dispenzieri A, Lacy MQ, Zeldenrust SR, Hayman SR, Kumar SK, Geyer SM, et al. The activity of lenalidomide with or without dexamethasone in patients with primary systemic amyloidosis. Blood. 2007;109:465–70.
Palladini G, Milani P, Foli A, Vidus Rosin M, Basset M, Lavatelli F, et al. Melphalan and dexamethasone with or without bortezomib in newly diagnosed AL amyloidosis: a matched case-control study on 174 patients. Leukemia. 2014;28:2311–6.
Palladini G, Perfetti V, Perlini S, Obici L, Lavatelli F, Caccialanza R, et al. The combination of thalidomide and intermediate-dose dexamethasone is an effective but toxic treatment for patients with primary amyloidosis (AL). Blood. 2005;105:2949–51.
Palladini G, Russo P, Foli A, Milani P, Lavatelli F, Obici L, et al. Salvage therapy with lenalidomide and dexamethasone in patients with advanced AL amyloidosis refractory to melphalan, bortezomib, and thalidomide. Ann Hematol. 2012;91:89–92.
Sanchorawala V, Wright DG, Rosenzweig M, Finn KT, Fennessey S, Zeldis JB, et al. Lenalidomide and dexamethasone in the treatment of AL amyloidosis: results of a phase 2 trial. Blood. 2007;109:492–6.
Kumar SK, Laplant BR, Reeder CB, Roy V, Halvorson AE, Buadi F, et al. Randomized phase 2 trial of ixazomib and dexamethasone in relapsed multiple myeloma not refractory to bortezomib. Blood. 2016;128:2415–22.
Dimopoulos MA, Gay F, Schjesvold F, Beksac M, Hajek R, Weisel KC, et al. Oral ixazomib maintenance following autologous stem cell transplantation (TOURMALINE-MM3): a double-blind, randomised, placebo-controlled phase 3 trial. Lancet. 2019;393:253–64.
Sidana S, Narkhede M, Elson P, Hastings D, Faiman B, Valent J, et al. Neuropathy and efficacy of once weekly subcutaneous bortezomib in multiple myeloma and light chain (AL) amyloidosis. PLoS One. 2017;12:e0172996.
Cohen AD, Landau H, Scott EC, Liedtke M, Kaufman JL, Rosenzweig M, et al. Safety and efficacy of carfilzomib (CFZ) in previously-treated systemic light-chain (AL) amyloidosis. Blood. 2016;128:645.
Acknowledgements
This study was supported by Millennium Pharmaceuticals, Inc., Cambridge, MA, USA, a wholly owned subsidiary of Takeda Pharmaceutical Company Limited. We thank the participants and their families, as well as the physicians, nurses, study coordinators, and research staff for participation in the trial. Helen Wilkinson, PhD, of FireKite (an Ashfield Company, part of UDG Healthcare plc), provided medical writing support for this manuscript, which was funded by Millennium Pharmaceuticals, Inc., Cambridge, MA, USA, a wholly owned subsidiary of Takeda Pharmaceutical Company Limited in compliance with Good Publication Practice 3 ethical guidelines (Battisti et al, Ann Intern Med 2015;163:461–4), and also Renda H. Ferrari, PhD, (Millennium Pharmaceuticals, Inc., Cambridge, MA, USA, a wholly owned subsidiary of Takeda Pharmaceutical Company Limited) for her editorial support.
Author information
Authors and Affiliations
Contributions
A.D., G.M. D.B., G.L., A.K., and D.V.F drafted the manuscript; all authors conceived and/or designed the work that led to the submission, acquired data, and/or played an important role in interpreting the results, revised the manuscript, approved the final version and agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Competing interests
AD, reports grants from Takeda, Celgene, Alnylam, and Pfizer for trial support, and research support from Janssen, outside the submitted work. EK, reports personal fees from Takeda, during the conduct of the study; grants and personal fees from Amgen, personal fees and non-financial support from Genesis Pharma, grants, personal fees and non-financial support from Janssen, personal fees from Prothena, personal fees from Pfizer, outside the submitted work. ADW, reports research funding from Amgen and Honoraria from Janssen-Cilag, Takeda, GSK, and Celgene. SOS, reports grants, personal fees and non-financial support from Janssen, grants, personal fees and non-financial support from Prothena, grants and non-financial support from Sanofi, non-financial support from MSD, personal fees and non-financial support from Takeda, outside the submitted work. KK, reports grants and personal fees from Celgene, for honoraria, consulting or advisory roles and personal fees from Takeda, Amgen, and Janssen, for honoraria, consulting or advisory role outside the submitted work. VS, reports grants from Takeda, Celgene, Prothena, Janssen, and consulting or advisory role from AbbVie, Proclara, Caleum, during the conduct of the study. HJL, reports grants from Genzyme Corporation, Amgen, Takeda Pharmaceuticals, Janssen Scientific Affairs LLC, HCA Healthcare, Spectrum Pharmaceuticals, Inc, Caelum Biosciences, Inc, Celgene, Clinical Care Options, Karyopharm, outside the submitted work. FK, has nothing to disclose. KS, reports research funding from BMS and honoraria from Takeda, BMS, Janssen and Celgene. RLC, received steering committee personal fees from Takeda, during the conduct of the study; grants to institution and personal steering committee fees from Janssen, personal DSCM fees from Sanofi, grants for laboratory research and personal DSCM fees from UNUM, grants to institution for clinical trial and personal steering committee fees from Takeda, grants to institution for clinical trial and personal fees for an advisory board from Karyopharm, personal fees for an advisory board from Amgen, grants to institution for clinical trial and personal steering committee fees from Prothena, personal fees for an advisory board from Caelum Biosciences, outside the submitted work. DB, is an employee of Millennium Pharmaceuticals, Inc., Cambridge, MA, USA, a wholly owned subsidiary of Takeda Pharmaceutical Company Limited. GL, is an employee of Millennium Pharmaceuticals, Inc., Cambridge, MA, USA, a wholly owned subsidiary of Takeda Pharmaceutical Company Limited. AK, is an employee of Millennium Pharmaceuticals, Inc., Cambridge, MA, USA, a wholly owned subsidiary of Takeda Pharmaceutical Company Limited. DVF, is an employee of Millennium Pharmaceuticals, Inc., Cambridge, MA, USA, a wholly owned subsidiary of Takeda Pharmaceutical Company Limited. GM has nothing to disclose.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Dispenzieri, A., Kastritis, E., Wechalekar, A.D. et al. A randomized phase 3 study of ixazomib–dexamethasone versus physician’s choice in relapsed or refractory AL amyloidosis. Leukemia 36, 225–235 (2022). https://doi.org/10.1038/s41375-021-01317-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41375-021-01317-y
This article is cited by
-
Safety and efficacy of teclistamab in systemic immunoglobulin light chain amyloidosis
Blood Cancer Journal (2023)
-
Diagnosis and Treatment of AL Amyloidosis
Drugs (2023)
-
Molecular Cardiotoxic Effects of Proteasome Inhibitors Carfilzomib and Ixazomib and Their Combination with Dexamethasone Involve Mitochondrial Dysregulation
Cardiovascular Toxicology (2023)
-
The management of light chain (AL) amyloidosis in Europe: clinical characteristics, treatment patterns, and efficacy outcomes between 2004 and 2018
Blood Cancer Journal (2023)
-
Global epidemiology of amyloid light-chain amyloidosis
Orphanet Journal of Rare Diseases (2022)