Abstract
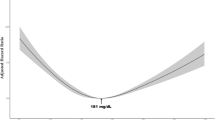
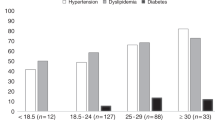
This study investigated the relationships between HDL-C and major types of blood cancers. Competing risks regression was used to examine the hazard ratios of hematologic malignancies in 9,596,145 individuals (≥20 years) using data from the Korean National Health Insurance Service (2009–2017). The incidence of the following hematologic cancers was determined based on the International Classification of Diseases 10th revision: Multiple Myeloma (MM), Hodgkin Lymphoma (HL), Non-Hodgkin Lymphoma (NHL), Lymphoid Leukemia (LL), and Myeloid Leukemia (ML). During an average of 8.3 years of follow-up (79,179,225 person-years), 15,864 incident hematologic malignancies were identified. Compared to those in the highest HDL-C quartile, subjects in the lowest HDL-C quartile had the highest risk of all hematologic cancers combined (adjusted hazard ratio [HR], 95% confidence interval [95% CI] = 1.31, 1.25–1.37) and of each respective type of blood cancer, as follows: MM (HR 1.61, 95% CI, 1.46–1.76), HL (HR 1.35, 95% CI 1.07–1.70), NHL (HR 1.12, 95%CI 1.04–1.21), LL (HR 1.36, 95% CI 1.16–1.61), and ML (HR 1.33, 95% CI 1.22–1.45). Low HDL-C level was significantly associated with increased risk of hematologic malignancy, suggesting that a low HDL-C level is an independent risk factor and preclinical marker for hematologic malignancy.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Collaboration GBoDC. Global, Regional, and National Cancer Incidence, Mortality, Years of Life Lost, Years Lived With Disability, and Disability-Adjusted Life-Years for 29 Cancer Groups, 1990 to 2016: a Systematic Analysis for the Global Burden of Disease Study. JAMA Oncol. 2018;4:1553–68.
Costa LJ, Xavier AC, Wahlquist AE, Hill EG. Trends in survival of patients with Burkitt lymphoma/leukemia in the USA: an analysis of 3691 cases. Blood. 2013;121:4861–6.
Shah A, Andersson TM, Rachet B, Bjorkholm M, Lambert PC. Survival and cure of acute myeloid leukaemia in England, 1971–2006: a population-based study. Br J Haematol. 2013 Aug;162:509–16.
Kansagra A, Dahiya S, Litzow M. Continuing challenges and current issues in acute lymphoblastic leukemia. Leuk Lymphoma. 2018;59:526–41.
Howlader N, Noone AM, Krapcho M, Miller D, Brest A, Yu M, et al. SEER Cancer Statistics Review, 1975-2016, National Cancer Institute. Bethesda, MD, https://seer.cancer.gov/csr/1975_2016/, based on November 2018 SEER data submission, posted to the SEER web site, April 2019.
Krause MR, Regen SL. The structural role of cholesterol in cell membranes: from condensed bilayers to lipid rafts. Acc Chem Res. 2014;47:3512–21.
Long J, Zhang C-J, Zhu N, Du K, Yin Y-F, Tan X, et al. Lipid metabolism and carcinogenesis, cancer development. Am J Cancer Res. 2018;8:778–91.
Yang C, Tian G, Mi J, Wei X, Li X, Li X, et al. Causal relevance of circulating high-density lipoprotein cholesterol with cancer: a Mendelian randomization meta-analysis. Sci Rep. 2015;5:9495.
Knekt P, Reunanen A, Aromaa A, Heliövaara M, Hakulinen T, Hakama M. Serum cholesterol and risk of cancer in a cohort of 39,000 men and women. J Clin Epidemiol. 1988;41:519–30.
Benn M, Tybjærg-Hansen A, Stender S, Frikke-Schmidt R, Nordestgaard BG. Low-Density Lipoprotein Cholesterol and the Risk of Cancer: A Mendelian Randomization Study. JNCI: J Natl Cancer Inst. 2011;103:508–19.
Lim U, Gayles T, Katki HA, Stolzenberg-Solomon R, Weinstein SJ, Pietinen P, et al. Serum High-Density Lipoprotein Cholesterol and Risk of Non-Hodgkin Lymphoma. Cancer Res. 2007;67:5569–74.
Wang L, Chi P-d, Chen H, Xiang J, Xia Z-j, Zhang Y-j. Low level of high-density lipoprotein cholesterol correlates with poor prognosis in extranodal natural killer/T cell lymphoma. Tumour Biol. 2014;35:2141–9.
Alford SH, Divine G, Chao C, Habel LA, Janakiraman N, Wang Y, et al. Serum cholesterol trajectories in the 10 years prior to lymphoma diagnosis. Cancer Causes Control. 2018;29:143–56.
Cheol Seong S, Kim YY, Khang YH, Heon Park J, Kang HJ, Lee H, et al. Data Resource Profile: The National Health Information Database of the National Health Insurance Service in South Korea. Int J Epidemiol. 2017;46:799–800.
Jeong S-M, Han K, Kim D, Rhee SY, Jang W, Shin DW. Body mass index, diabetes, and the risk of Parkinson’s disease. Mov Disord. 2020;35:236–44.
Agarwal DP. Cardioprotective effects of light-moderate consumption of alcohol: a review of putative mechanisms. Alcohol Alcohol (Oxf, Oxfs). 2002;37:409–15.
Fine JP, Gray RJ. A Proportional Hazards Model for the Subdistribution of a Competing Risk. J Am Stat Assoc. 1999;94:496–509.
Kuliszkiewicz-Janus M, Małecki R, Mohamed A. Lipid changes occuring in the course of hematological cancers. Cell Mol Biol Lett. 2008;13:465–74.
Moschovi M, Trimis G, Apostolakou F, Papassotiriou I, Tzortzatou-Stathopoulou F. Serum Lipid Alterations in Acute Lymphoblastic Leukemia of Childhood. J Pediatr Hematol Oncol. 2004;26:289–93.
Negre-Salvayre A, Dousset N, Ferretti G, Bacchetti T, Curatola G, Salvayre R. Antioxidant and cytoprotective properties of high-density lipoproteins in vascular cells. Free Radic Biol Med. 2006;41:1031–40.
Krawczyk J, O’Dwyer M, Swords R, Freeman C, Giles FJ. The role of inflammation in leukaemia. In: Aggarwal BB, Sung B, Gupta SC, editors. Inflammation and Cancer. Basel:Springer Basel; 2014. p. 335–60.
Yvan-Charvet L, Pagler T, Gautier EL, Avagyan S, Siry RL, Han S, et al. ATP-binding cassette transporters and HDL suppress hematopoietic stem cell proliferation. Sci (N. Y, NY). 2010;328:1689–93.
Yui Y, Aoyama T, Morishita H, Takahashi M, Takatsu Y, Kawai C. Serum prostacyclin stabilizing factor is identical to apolipoprotein A-I (Apo A-I). A novel function of Apo A-I. J Clin Investig. 1988;82:803–7.
Halton JM, Nazir DJ, McQueen MJ, Barr RD. Blood lipid profiles in children with acute lymphoblastic leukemia. Cancer. 1998;83:379–84.
Dong F, Mo Z, Eid W, Courtney KC, Zha X. Akt inhibition promotes ABCA1-mediated cholesterol efflux to ApoA-I through suppressing mTORC1. PloS ONE. 2014;9:e113789.
Tosi MR, Tugnoli V. Cholesteryl esters in malignancy. Clin Chim Acta. 2005;359:27–45.
Yuan B, Wu C, Wang X, Wang D, Liu H, Guo L, et al. High scavenger receptor class B type I expression is related to tumor aggressiveness and poor prognosis in breast cancer. Tumour Biol. 2016;37:3581–8.
Kornblau SM, Banker DE, Stirewalt D, Shen D, Lemker E, Verstovsek S, et al. Blockade of adaptive defensive changes in cholesterol uptake and synthesis in AML by the addition of pravastatin to idarubicin + high-dose Ara-C: a phase 1 study. Blood. 2007;109:2999–3006.
Desai P, Mencia-Trinchant N, Savenkov O, Simon MS, Cheang G, Lee S, et al. Somatic mutations precede acute myeloid leukemia years before diagnosis. Nat Med. 2018;24:1015–23.
Larsson SC, Wolk A. Overweight and obesity and incidence of leukemia: a meta-analysis of cohort studies. Int J Cancer. 2008;122:1418–21.
Tilg H, Moschen AR. Adipocytokines: mediators linking adipose tissue, inflammation and immunity. Nat Rev Immunol. 2006;6:772–83.
Sassano A, Katsoulidis E, Antico G, Altman JK, Redig AJ, Minucci S, et al. Suppressive effects of statins on acute promyelocytic leukemia cells. Cancer Res. 2007;67:4524–32.
Acknowledgements
This study was performed using a database from the National Health Insurance System (NHIS).
Author information
Authors and Affiliations
Contributions
Conception and design: TC, KH, DWS. Acquisition of data: DK, KH. Analysis and interpretation of data: DK, KH, SMJ. Writing, review, and/or revision of the paper: SMJ, TC, SJK, SYR, ELG. Study supervision: DWS.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Jeong, SM., Choi, T., Kim, D. et al. Association between high-density lipoprotein cholesterol level and risk of hematologic malignancy. Leukemia 35, 1356–1364 (2021). https://doi.org/10.1038/s41375-020-01081-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41375-020-01081-5
This article is cited by
-
Low serum total cholesterol levels predict inferior prognosis of patients with POEMS syndrome
Discover Oncology (2024)
-
Altered serum lipid levels are associated with prognosis of diffuse large B cell lymphoma and influenced by utility of rituximab
Annals of Hematology (2023)
-
High-density lipoprotein (HDL) has an impact on myeloma outcome: Lower HDL associates with worse progression-free survival
Wiener klinische Wochenschrift (2023)