Abstract
Purpose
To investigate in-hospital mortality and hospital length of stay (LOS) in infants requiring tracheostomy with bronchopulmonary dysplasia (BPD).
Methods
We explored the correlation between tracheostomy with in-hospital mortality and LOS in infant patients hospitalized with BPD, using the data from Nationwide Inpatient Sample between 2008 and 2017 in the United States. In-hospital mortality and LOS was compared in patients who underwent tracheostomy with those patients who did not after propensity-score matching.
Results
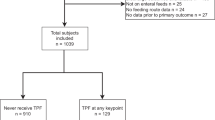
A total of 10,262 children ≤2 years old hospitalized with BPD, 847 (8%) underwent tracheostomy, and 821 patients underwent tracheostomy were matched with 1602 patients without tracheostomy. Tracheostomy group was correlated with higher in-hospital mortality(OR(95%CI):2.98(2.25–3.95)) and prolonged LOS(absolute difference(95%CI):97.0(85.6–108.4)).
Conclusions
Tracheostomy was correlated with increased in-hospital mortality and prolonged LOS. Such information may contribute to better decision-making process between clinicians and parents regarding tracheostomy to manage parent expectations, as well as better interdisciplinary teamwork.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
The data we used in the study is publicly available.
References
Higgins RD, Jobe AH, Koso-Thomas M, Bancalari E, Viscardi RM, Hartert TV, et al. Bronchopulmonary dysplasia: executive summary of a workshop. J Pediatr. 2018;197:300–8.
Stoll BJ, Hansen NI, Bell EF, Walsh MC, Carlo WA, Shankaran S, et al. Trends in care practices, morbidity, and mortality of extremely preterm neonates, 1993–2012. JAMA. 2015;314:1039–51.
Nakashima T, Inoue H, Sakemi Y, Ochiai M, Yamashita H, Ohga S, et al. Trends in bronchopulmonary dysplasia among extremely preterm infants in Japan, 2003–2016. J Pediatr. 2021;230:119–125.e117.
Jobe AH, Bancalari E. Bronchopulmonary dysplasia. Am J Respir Crit Care Med. 2001;163:1723–9.
Hayes D Jr, Feola DJ, Murphy BS, Shook LA, Ballard HO. Pathogenesis of bronchopulmonary dysplasia. Respiration. 2010;79:425–36.
Muller RG, Mamidala MP, Smith SH, Smith A, Sheyn A. Incidence, epidemiology, and outcomes of pediatric tracheostomy in the United States from 2000 to 2012. Otolaryngol Head Neck Surg. 2019;160:332–8.
DeMauro SB, Wei JL, Lin RJ. Perspectives on neonatal and infant tracheostomy. Semin Fetal Neonatal Med. 2016;21:285–91.
Cammack B, Noel-MacDonnell J, Cuna A, Manimtim W. Impact of tracheostomy on language and cognitive development in infants with severe bronchopulmonary dysplasia. J Perinatol. 2020;40:299–305.
Luo J, Shepard S, Nilan K, Wood A, Monk HM, Jensen EA, et al. Improved growth and developmental activity post tracheostomy in preterm infants with severe BPD. Pediatr Pulmonol. 2018;53:1237–44.
Annesi CA, Levin JC, Litt JS, Sheils CA, Hayden LP. Long-term respiratory and developmental outcomes in children with bronchopulmonary dysplasia and history of tracheostomy. J Perinatol. 2021;41:2645–50.
Upadhyay K, Vallarino DA, Talati AJ. Outcomes of neonates with tracheostomy secondary to bronchopulmonary dysplasia. BMC Pediatr. 2020;20:414.
Hatch LD 3rd, Clark RH, Carlo WA, Stark AR, Ely EW, Patrick SW. Changes in use of respiratory support for preterm infants in the US, 2008-2018. JAMA Pediatr. 2021;175:1017–24.
Greenland S. Basic methods for sensitivity analysis of biases. Int J Epidemiol. 1996;25:1107–16.
House M, Nathan A, Bhuiyan MAN, Ahlfeld SK. Morbidity and respiratory outcomes in infants requiring tracheostomy for severe bronchopulmonary dysplasia. Pediatr Pulmonol. 2021;56:2589–96.
Mandy G, Malkar M, Welty SE, Brown R, Shepherd E, Gardner W, et al. Tracheostomy placement in infants with bronchopulmonary dysplasia: safety and outcomes. Pediatr Pulmonol. 2013;48:245–9.
Abman SH, Collaco JM, Shepherd EG, Keszler M, Cuevas-Guaman M, Welty SE, et al. Interdisciplinary care of children with severe bronchopulmonary dysplasia. J Pediatr. 2017;181:12–28.e11.
D’Souza JN, Levi JR, Park D, Shah UK. Complications following pediatric tracheotomy. JAMA Otolaryngol Head Neck Surg. 2016;142:484–8.
Edwards JD, Kun SS, Keens TG. Outcomes and causes of death in children on home mechanical ventilation via tracheostomy: an institutional and literature review. J Pediatr. 2010;157:955–9.e952.
Padula MA, Grover TR, Brozanski B, Zaniletti I, Nelin LD, Asselin JM, et al. Therapeutic interventions and short-term outcomes for infants with severe bronchopulmonary dysplasia born at <32 weeks’ gestation. J Perinatol. 2013;33:877–81.
DeMauro SB, D’Agostino JA, Bann C, Bernbaum J, Gerdes M, Bell EF, et al. Developmental outcomes of very preterm infants with tracheostomies. J Pediatr. 2014;164:1303–10.e1302.
Murthy K, Porta NFM, Lagatta JM, Zaniletti I, Truog WE, Grover TR, et al. Inter-center variation in death or tracheostomy placement in infants with severe bronchopulmonary dysplasia. J Perinatol. 2017;37:723–7.
Murthy K, Savani RC, Lagatta JM, Zaniletti I, Wadhawan R, Truog W, et al. Predicting death or tracheostomy placement in infants with severe bronchopulmonary dysplasia. J Perinatol. 2014;34:543–8.
Windsor AM, Kiell EP, Sobol SE. Predictors of the need for tracheostomy in the neonatal intensive care unit. Int J Pediatr Otorhinolaryngol. 2020;135:110122.
Overman AE, Liu M, Kurachek SC, Shreve MR, Maynard RC, Mammel MC, et al. Tracheostomy for infants requiring prolonged mechanical ventilation: 10 years’ experience. Pediatrics. 2013;131:e1491–96.
Hysinger EB, Friedman NL, Padula MA, Shinohara RT, Zhang H, Panitch HB, et al. Tracheobronchomalacia is associated with increased morbidity in bronchopulmonary dysplasia. Ann Am Thorac Soc. 2017;14:1428–35.
Sisk EA, Kim TB, Schumacher R, Dechert R, Driver L, Ramsey AM, et al. Tracheotomy in very low birth weight neonates: indications and outcomes. Laryngoscope. 2006;116:928–33.
Radford PJ, Stillwell PC, Blue B, Hertel G. Aspiration complicating bronchopulmonary dysplasia. Chest. 1995;107:185–8.
Wang LJ, Hu Y, Wang W, Zhang CY, Bai YZ, Zhang SC. Gastroesophageal reflux poses a potential risk for late complications of bronchopulmonary dysplasia: a prospective Cohort Study. Chest. 2020;158:1596–605.
Jensen EA, Munson DA, Zhang H, Blinman TA, Kirpalani H. Anti-gastroesophageal reflux surgery in infants with severe bronchopulmonary dysplasia. Pediatr Pulmonol. 2015;50:584–7.
Kurata H, Ochiai M, Inoue H, Ichiyama M, Yasuoka K, Fujiyoshi J, et al. A nationwide survey on tracheostomy for very-low-birth-weight infants in Japan. Pediatr Pulmonol. 2019;54:53–60.
Koltsida G, Konstantinopoulou S. Long term outcomes in chronic lung disease requiring tracheostomy and chronic mechanical ventilation. Semin Fetal Neonatal Med. 2019;24:101044.
Baker CD. Chronic respiratory failure in bronchopulmonary dysplasia. Pediatr Pulmonol. 2021;56:3490–8.
Acknowledgements
The authors thank Dr. Xiaotian Chen (Children’s Hospital of Fudan University, Shanghai, China) for reviewing the manuscript.
Funding
This work is supported by the Three-Year Action Plan for Strengthening Public Health System in Shanghai (2020–2022) Subject Chief Scientist (GWV-10.2-XD05), Pilot Program of Naval Medical University (Cheng WU), National Key Research and Development Program of China (2021YFC2701800, 2021YFC2701805).
Author information
Authors and Affiliations
Contributions
RZ and YX designed the work. RZ, YX and YQ drafted the work. JX, RW, SW, YC, XL, YT, CC and JH critically reviewed the work for intellectual content. SW and CW were the guarantors. All authors approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
Because the NIS is a de-identified inpatient health-care database for public availability, our study was exempted by the Committee on Ethics of Medical Research at Naval Medical University.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhu, R., Xu, Y., Qin, Y. et al. In-hospital mortality and length of hospital stay in infants requiring tracheostomy with bronchopulmonary dysplasia. J Perinatol (2023). https://doi.org/10.1038/s41372-023-01840-z
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41372-023-01840-z