Abstract
Objective
To compare the incidence of bronchopulmonary dysplasia (BPD) based on the 1988 Vermont Oxford Network (VON) criteria, National Institutes of Health (NIH) 2001 definition, and NIH 2018 definition.
Methods
BPD incidence by each definition was compared in premature infants born at a single center between 2016 and 2018. Comorbidities were compared between those with and without BPD according to the newest definition.
Results
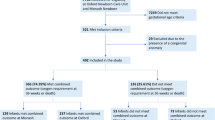
Among 352 survivors, BPD incidence was significantly different at 9%, 28% and 34% according to VON, NIH 2001 and NIH 2018 definitions, respectively (p < 0.05). According to the newest definition, any grade of BPD was associated with more co-morbidities than those without BPD (P < 0.001).
Conclusion
At a center that emphasizes use of early noninvasive respiratory support, the incidence of BPD was significantly higher according to the NIH 2018 definition compared to other two definitions. The relationship between BPD diagnosis and long-term clinical outcomes remains unclear.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Change history
07 September 2021
A Correction to this paper has been published: https://doi.org/10.1038/s41372-021-01140-4
References
Stoll BJ, Hansen NI, Bell EF, Shankaran S, Laptook AR, Walsh MC, et al. Neonatal outcomes of extremely preterm infants from the NICHD Neonatal Research Network. Pediatrics. 2010;126:443–56.
Ibrahim J, Bhandari V. The definition of bronchopulmonary dysplasia: an evolving dilemma. Pediatr Res. 2018;84:586–8.
Jensen EA, Schmidt B. Epidemiology of bronchopulmonary dysplasia. Birth Defects Res A Clin Mol Teratol. 2014;100:145–57.
Trembath A, Laughon MM. Predictors of bronchopulmonary dysplasia. Clin Perinatol. 2012;39:585–601.
Padula MA, Grover TR, Brozanski B, Zaniletti I, Nelin LD, Asselin JM, et al. Therapeutic interventions and short-term outcomes for infants with severe bronchopulmonary dysplasia born at <32 weeks’ gestation. J Perinatol. 2013;33:877–81.
Jobe AH, Bancalari E. Bronchopulmonary dysplasia. Am J Respir Crit Care Med. 2001;163:7.
National Institutes of Health. Report of workshop on bronchopulmonary dysplasia; NIH publication No. 80-1660. Washington (DC): National Institutes of Health; 1979.
Shennan T, Dunn S, Hoskins M. Abnormal pulmonary outcomes in premature infants: prediction from oxygen requirement in the neonatal period. Pediatrics. 1988;82:527–32.
Walsh MC, Yao Q, Gettner PA, Hale E, Collins M, Hensman A, et al. Impact of a physiologic definition on bronchopulmonary dysplasia rates. Pediatrics. 2004;114:1305–11.
Ehrenkranz RA. Validation of the National Institutes of Health Consensus Definition of bronchopulmonary dysplasia. Pediatrics. 2005;116:1353–60.
Northway WH Jr, Rosan RC, Porter DY. Pulmonary disease following respiratory therapy of hyaline-membrane disease: bronchopulmonary dysplasia. N. Engl J Med. 1967;276:357–68.
Poindexter BB, Feng R, Schmidt B, Aschner JL, Ballard RA, Hamvas A, et al. Comparisons and limitations of current definitions of bronchopulmonary dysplasia for the prematurity and respiratory outcomes program. Ann Am Thorac Soc. 2015;12:1822–30.
Higgins RD, Jobe AH, Koso-Thomas M, Bancalari E, Viscardi RM, Hartert TV, et al. Bronchopulmonary dysplasia: executive summary of a workshop. J Pediatr. 2018;197:300–8.
Polin RA, Sahni R. Newer experience with CPAP. Semin Neonatol. 2002;7:379–89.
Vermont Oxford Network. VLBW/Expanded Databases - 2020 Data Definitions, Forms, and Materials. [Internet]. [updated 2021 Jan 7; cited 2020 Jun 1]. Available from: https://public.vtoxford.org/.
Abman SH, Collaco JM, Shepherd EG, Keszler M, Cuevas-Guaman M, Welty SE, et al. Interdisciplinary care of children with severe bronchopulmonary dysplasia. J Pediatr. 2017;181:12–28.e1.
Committee on Obstetric Practice. Committee Opinion No. 712: Intrapartum management of intraamniotic infection. Obstet Gynecol. 2017;130:e95–101.
R Core Team. R: a language and environment for statistical computing. Vienna, Austria: R Foundation for Statistical Computing; 2013. http://www.R-project.org.
Papile L-A, Burstein J, Burstein R, Koffler H. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr. 1978;92:529–34.
Zhang S, Garbutt V, McBride JT. Strain-induced growth of the immature lung. J Appl Physiol. 1996;81:1471–6.
Bamat N, Jensen EA, Kirpalani H. Duration of continuous positive airway pressure in premature infants. Semin Fetal Neonatal Med. 2016;21:189–95.
Sahni R, Schiaratura M, Polin RA. Strategies for the prevention of continuous positive airway pressure failure. Semin Fetal Neonatal Med. 2016;21:196–203.
Sahni R, Ammari A, Suri MS, Milisavljevic V, Ohira-Kist K, Wung JT, et al. Is the new definition of bronchopulmonary dysplasia more useful? J Perinatol. 2005;25:41–46.
Stroustrup A, Trasande L. Epidemiological characteristics and resource use in neonates with bronchopulmonary dysplasia: 1993-2006. Pediatrics. 2010;126:291–7.
Anderson PJ, Doyle LW. Neurodevelopmental outcome of bronchopulmonary dysplasia. Semin Perinatol. 2006;30:227–32.
Davidson L, Berkelhamer S. Bronchopulmonary dysplasia: chronic lung disease of infancy and long-term pulmonary outcomes. J Clin Med. 2017;6:4.
vom Hove M, Prenzel F, Uhlig HH, Robel-Tillig E. Pulmonary outcome in former preterm, very low birth weight children with bronchopulmonary dysplasia: a case-control follow-up at school age. J Pediatr. 2014;164:40–45.e4.
Jensen EA, Dysart K, Gantz MG, McDonald S, Bamat NA, Keszler M, et al. The diagnosis of bronchopulmonary dysplasia in very preterm infants. An evidence-based approach. Am J Respir Crit Care Med. 2019;200:751–9.
Malavolti AM, Bassler D, Arlettaz-Mieth R, Faldella G, Latal B, Natalucci G. Bronchopulmonary dysplasia—impact of severity and timing of diagnosis on neurodevelopment of preterm infants: a retrospective cohort study. BMJ Paediatr Open. 2018;2:e000165.
Palta M, Sadek M, Barnet JH, Evans M, Weinstein MR, McGuinness G, et al. Evaluation of criteria for chronic lung disease in surviving very low birth weight infants. J Pediatr. 1998;132:7.
Weinstein MR, Peters ME, Sadek M, Palta M, For The Newborn Lung Project. A new radiographic scoring system for bronchopulmonary dysplasia. Pediatr Pulmonol. 1994;18:284–9.
Higano NS, Spielberg DR, Fleck RJ, Schapiro AH, Walkup LL, Hahn AD, et al. Neonatal pulmonary magnetic resonance imaging of bronchopulmonary dysplasia predicts short-term clinical outcomes. Am J Respir Crit Care Med. 2018;198:1302–11.
Acknowledgements
We would like to thank Kiyoko Ohira-Kist for her time and effort in collecting and inputting our institution’s data into the Vermont Oxford Network Database.
Author information
Authors and Affiliations
Contributions
FK and AW-S conceptualized and designed the study, designed the data collection instruments, collected data and drafted the initial manuscript and reviewed and revised the manuscript. DAB and NG carried out secondary analyses and reviewed and revised the manuscript. RS and JTW reviewed and revised the manuscript. All authors approved the final manuscript and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: Table 3 was corrected.
Rights and permissions
About this article
Cite this article
Kim, F., Bateman, D.A., Goldshtrom, N. et al. Revisiting the definition of bronchopulmonary dysplasia in premature infants at a single center quaternary neonatal intensive care unit. J Perinatol 41, 756–763 (2021). https://doi.org/10.1038/s41372-021-00980-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-021-00980-4
This article is cited by
-
Current Controversies and Advances in Non-invasive Respiratory Support for Preterm Infants
Current Treatment Options in Pediatrics (2022)