Abstract
Objective
The primary objectives were to compare body mass index (BMI) Z-score (Z), systolic blood pressure (SBP), serum leptin:adiponectin (L:A) ratio and estimated glomerular filtration rate (eGFR) at ~3 years adjusted age between two arms of a randomized controlled trial (RCT) comparing two modes of human milk fortification for very low-birthweight infants in the neonatal intensive care unit.
Study design
Follow-up of RCT at 33–48 months.
Results
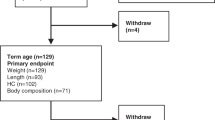
Follow-up data are available in 82/120 infants. Infants in the experimental arm have anthropometric data consistent with central obesity and higher serum L:A ratio (sensitivity analysis adjusting for sex and using all available data), but have similar eGFR and SBP at follow-up compared with controls. Serum L:A ratio is strongly correlated with anthropometric measurements suggesting central obesity.
Conclusions
Infants in the experimental arm have central obesity and higher serum L:A ratio compared with controls. Notably, serum L:A ratio is strongly correlated with weight gain.
Trial registration
This randomized controlled trial was registered at ClinicalTrials.gov NCT02372136.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Kumar VHS. Cardiovascular morbidities in adults born preterm: getting to the heart of the matter! Children. 2022;9:1843.
Duncan AF, Heyne RJ, Morgan JS, Ahmad N, Rosenfeld CR. Elevated systolic blood pressure in preterm very-low-birth-weight infants ≤3 years of life. Pediatr Nephrol. 2011;26:1115–21.
Beltowski J. Role of leptin in blood pressure regulation and arterial hypertension. J Hypertens. 2006;24:789–801.
Kim DH, Kim C, Ding EL, Townsend MK, Lipsitz LA. Adiponectin levels and the risk of hypertension. A systematic review and meta-analysis. Hypertension. 2013;62:27–32.
Diamond FB Jr, Cuthbertson D, Hanna S, Eichler D. Correlates of adiponectin and the leptin/adiponectin ratio in obese and non-obese children. J Pediatr Endocrinol Metab. 2004;17:1069–75.
Diamond F, Dharamraj C, Luther S, Eichler D. The leptin/adiponectin ratio in mid-infancy correlates with weight gain in healthy term infants, but is unrelated to serum insulin concentrations, body mass index, or skin fold thickness. J Pediatr Endocrinol Metab. 2008;21:1133–8.
Santana-Meneses JF, Suano-Souza FI, Franco MDC, Fonseca FL, Strufaldi MWL. Leptin and adiponectin concentrations in infants with low birthweight: relationship with maternal health and postnatal growth. J Dev Orig Health Dis. 2022;13:338–44.
Tylutka A, Morawin B, Walas Ł, Michałek M, Gwara A, Zembron-Lacny A. Assessment of metabolic syndrome predictors in relation to inflammation and visceral fat tissue in older adults. Sci Rep. 2023;13:89.
Kondo H, Abe I, Gotoh K, Fukui A, Takanari H, Ishii Y, et al. Interleukin 10 treatment ameliorates high-fat diet-induced inflammatory atrial remodeling and fibrillation. Circ Arrhythm Electrophysiol. 2018;11:e006040.
Esposito K, Pontillo A, Giugliano F, Giugliano G, Marfella R, Nicoletti G, et al. Association of low interleukin-10 levels with the metabolic syndrome in obese women. J Clin Endocrinol Metab. 2003;88:1055–8.
Frankfurt JA, Duncan AF, Heyne RJ, Rosenfeld CR. Renal function and systolic blood pressure in very-low-birth-weight infants 1-3 years of age. Pediatr Nephrol. 2012;27:2285–91.
Duncan AF, Frankfurt JA, Heyne RJ, Rosenfeld CR. Biomarkers of adiposity are elevated in preterm very-low-birth-weight infants at 1, 2 and 3 y of age. Pediatr Res. 2017;81:780–6.
Wickland J, Brown LS, Blanco V, Heyne R, Turer C, Rosenfeld CR. Persistent high blood pressure and renal dysfunction in preterm infants during childhood. Pediatr Res. 2023;93:217–25.
Brion LP, Rosenfeld CR, Heyne R, Brown LS, Lair C, Burchfield P, et al. Adjustable feedings plus accurate serial length measurements decrease weight-length disproportion in very preterm infants. J Perinatol. 2019;39:1131–9. Corrected and republished from: J Perinatol. 2019; 39:1694.
Brion LP, Rosenfeld CR, Heyne R, Brown LS, Lair CS, Heyne E, et al. Association of age of initiation and type and of complementary foods with body mass index and weight-length at twelve months of age in preterm infants. J Perinatol. 2020;40:1394–404.
Simon L, Hadchouel A, Arnaud C, Frondas-Chauty A, Marret S, Flamant C, et al. Growth trajectory during the first 1000 days and later overweight in very preterm infants. Arch Dis Child Fetal Neonatal Ed. 2023;108:149–55.
Brion LP, Rosenfeld CR, Heyne R, Brown LS, Lair CS, Petrosyan E, et al. Optimizing individual nutrition in preterm very low birthweight infants: double-blinded randomized controlled trial. J Perinatol. 2020;40:655–65.
Reis RD, Tolentino-Plata K, Caraig M, Heyne R, Rosenfeld CR, Brown LS, et al. Double-blinded randomized controlled trial of optimizing nutrition in preterm very low birthweight infants: Bayley scores at 18-38 months of age. J Perinatol. 2023;43:81–5.
Filler G, Lepage N. Should the Schwartz formula for estimation of GFR be replaced by cystatin C formula? Pediatr Nephrol. 2003;18:981–5.
Olsen IE, Lawson ML, Ferguson AN, Cantrell R, Grabich SC, Zemel BS, et al. BMI curves for preterm infants. Pediatrics. 2015;135:e572–81.
Olsen IE, Groveman SA, Lawson ML, Clark RH, Zemel BS. New intrauterine growth curves based on United States data. Pediatrics. 2010;125:e214–24.
WHO Multicentre Growth Reference Study Group. WHO Child Growth Standards based on length/height, weight and age. Acta Paediatr Suppl. 2006;450:76–85.
WHO Multicentre Growth Reference Study Group. WHO child growth standards: length/height-for-age, weight-for-age, weight-for-length, weight-for-height and body mass index-for-age: methods and development. Geneva: World Health Organization; 2006. https://www.who.int/publications/i/item/924154693X. Accessed 20 Jun 2023.
Clark RH, Olsen IE, Spitzer AR. Assessment of neonatal growth in prematurely born infants. Clin Perinatol. 2014;41:295–307.
WHO Multicentre Growth Reference Study Group. WHO child growth standards: head circumference-for-age, arm circumference-for-age, triceps skinfold-for-age and subscapular skinfold-for-age: methods and development. Geneva: World Health Organization; 2007. https://www.who.int/publications/i/item/9789241547185. Accessed 20 Jun 2023.
Hampl SE, Hassink SG, Skinner AC, Armstrong SC, Barlow SE, Bolling CF, et al. Clinical practice guideline for the evaluation and treatment of children and adolescents with obesity. Pediatrics. 2023;151:e2022060640.
Schwartz GJ, Schneider MF, Maier PS, Moxey-Mims M, Dharnidharka VR, Warady BA, et al. Improved equations estimating GFR in children with chronic kidney disease using an immunonephelometric determination of cystatin C. Kidney Int. 2012;82:445–53.
Flynn, JT, Kaelber DC, Baker-Smith CM, Blowey D, Carroll AE, Daniels SR, et al. Subcommittee on screening and management of high blood pressure in children. Clinical practice guideline for screening and management of high blood pressure in children and adolescents. Pediatrics. 2017;140:e20171904. Erratum in: Pediatrics. 2017 Nov 30;: Erratum in: Pediatrics. 2018 Sep;142.
Erhardt E, Foraita R, Pigeot I, Barba G, Veidebaum T, Tornaritis M, et al. IDEFICS consortium. Reference values for leptin and adiponectin in children below the age of 10 based on the IDEFICS cohort. Int J Obes. 2014;38:S32–8.
Li G, Taljaard M, Van den Heuvel ER, Levine MA, Cook DJ, Wells GA, et al. An introduction to multiplicity issues in clinical trials: the what, why, when and how. Int J Epidemiol. 2017;46:746–55.
Perneger TV. What’s wrong with Bonferroni adjustments. BMJ. 1998;316:1236–8.
Zhu Y, Lin Q, Zhang Y, Deng H, Hu X, Yang X, et al. Mid-upper arm circumference as a simple tool for identifying central obesity and insulin resistance in type 2 diabetes. PLoS ONE. 2020;15:e0231308.
López-Jaramillo P, Gómez-Arbeláez D, López-López J, López-López C, Martínez-Ortega J, Gómez-Rodríguez A, et al. The role of leptin/adiponectin ratio in metabolic syndrome and diabetes. Horm Mol Biol Clin Investig. 2014;18:37–45.
Pan L, Li R, Park S, Galuska DA, Sherry B, Freedman DS. A longitudinal analysis of sugar-sweetened beverage intake in infancy and obesity at 6 years. Pediatrics. 2014;134:S29–35.
Heyman MB, Abrams SA. AAP section on gastroenterology, hepatology, and nutrition; AAP Committee on Nutrition. Fruit juice in infants, children, and adolescents: current recommendations. Pediatrics. 2017;139:e20170967.
Baldassarre ME, Giannì ML, Di Mauro A, Mosca F, Laforgia N. Complementary feeding in preterm infants: where do we stand? Nutrients. 2020;12:1259.
Vissers KM, Feskens EJ, van Goudoever JB, Janse AJ. The timing of initiating complementary feeding in preterm infants and its effect on overweight: a systematic review. Ann Nutr Metab. 2018;72:307–15.
Salvatori G, Martini L, The Study Group on Neonatal Nutrition and Gastroenterology-Italian Society of Neonatology OBO. Complementary feeding in the preterm infants: summary of available macronutrient intakes and requirements. Nutrients. 2020;12:3696.
Brenner BM, Garcia DL, Anderson S. Glomeruli and blood pressure. Less of one, more the other? Am J Hypertens. 1988;11:335–47.
Luyckx VA, Brenner BM. Low birthweight, nephron number, and kidney disease. Kidney Int Suppl. 2005;97:S68–77.
Carmody JB, Charlton JR. Short-term gestation, long-term risk: prematurity and chronic kidney disease. Pediatrics 2013;131:1168–79.
Funding
Children’s Medical Center Clinical Advisory Committee (CCRAC) – Senior Investigator Research Award – Direction (L.P. Brion); National Grant from the Gerber Foundation (L.P. Brion); George L. MacGregor Professorship (C.R. Rosenfeld) UTSW consolidated account (R. Heyne) Crystal Charity Ball (CCB) UT Foundation (Lina Chalak). Funding/Financial Support: The RCT was supported by a National Grant from the Gerber Foundation (LP Brion), George L. MacGregor Professorship (CR Rosenfeld), a Children’s Medical Center Clinical Advisory Committee (CCRAC) – Senior Investigator Research Award – New Direction (LP Brion), a UTSW consolidated account (R. Heyne) and by the Crystal Charity Ball (CCB) UT Foundation (Lina Chalak). The follow-up was supported by the latter four sources. The study sponsors had no role in design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, and approval of the manuscript, and decision to submit the manuscript for publication. One of the originally planned outcomes, body composition by Dexascan, was not performed for lack of funding.
Author information
Authors and Affiliations
Contributions
DJR, RH, CRR, and LPB conceptualized and designed the study. MC, RN was the research coordinator for the QI project. SB, MS conducted statistical analyses. Measurements of cystatin-C were obtained at the clinical laboratory at Children’s Medical Center. Measurements of adipokines and cytokines were obtained at UT Southwestern Medical Center. All authors participated in the interpretation of the data, critically reviewed the revisions, and approved the final manuscript as submitted.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Reis, J.D., Heyne, R., Rosenfeld, C.R. et al. Follow-up of a randomized trial optimizing neonatal nutrition in preterm very low birthweight infants: growth, serum adipokines, renal function and blood pressure. J Perinatol 44, 78–86 (2024). https://doi.org/10.1038/s41372-023-01821-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-023-01821-2