Abstract
Objective
The primary aim was to evaluate whether the addition of the posterior lung aided in diagnostic accuracy of predicting bronchopulmonary dysplasia (BPD) vs moderate-severe BPD (msBPD); the secondary aim was to explore the diagnostic accuracy of two protocols for BPD vs msBPD.
Study design
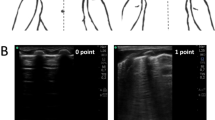
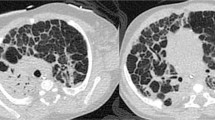
This was a single-center prospective observational study. Preterm infants with a gestational age ≤ 25 weeks were included. Two LUS score protocols were evaluated on the 14th day of life (DOL): (A) evaluating the anterolateral (LUS score-al) lung and (B) the anterolateral combined with posterior (LUS score-alp) lung. The LUS score range for the two protocols was 0–32 and 0–48, respectively.
Results
A total of eighty-nine infants were enrolled. Both the LUS score-al and LUS score-alp were higher in neonates developing BPD and msBPD than in the rest of the cohort (LUS score-al 24 (23,26) vs 22 (20,23); LUS score-alp 36 (34,39) vs 28 (25,32)) (LUS score-al 25 (24,26) vs 23 (21,24); LUS score-alp 40 (39,40) vs 34 (28,36)). The LUS score-al on the 14th DOL showed a moderate diagnostic accuracy to predict BPD and msBPD (AUC 95% CI: 0.797 [0.697–0.896]; 0.811[0.713–0.909]), while the LUS score-alp significantly improved diagnostic accuracy of BPD and msBPD (AUC 95% CI: 0.902 [0.834–0.970]; 0.922 [0.848–0.996]). A cutoff of 25 points in the LUS score-al provided a sensitivity, specificity, positive likelihood ratio, and negative likelihood ratio of 76.9%, 79.4%, 3.7, and 0.3 respectively to predict msBPD. Meanwhile, that of 39 points in the LUS score-alp provided a sensitivity, specificity, positive likelihood ratio, and negative likelihood ratio of 81%, 98.4%, 50.5 and 0.19 to predict msBPD, respectively.
Conclusions
The LUS score on the 14th DOL can predict BPD and msBPD with moderate diagnostic accuracy. Apart from that, scanning posterior enhanced diagnostic accuracy.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Liu J, Copetti R, Sorantin E, Lovrenski J, Rodriguez-Fanjul J, Kurepa D et al. Protocol and guidelines for point-of-care lung ultrasound in diagnosing neonatal pulmonary diseases based on international expert consensus. J Vis Exp. 2019; 145. https://doi.org/10.3791/58990.
Kurepa D, Zaghloul N, Watkins L, Liu J. Neonatal lung ultrasound exam guidelines. J Perinatol. 2018;38:11–22. https://doi.org/10.1038/jp.2017.140.
Brusa G, Savoia M, Vergine M, Bon A, Copetti R, Cattarossi L. Neonatal lung sonography: interobserver agreement between physician interpreters with varying levels of experience. J Ultrasound Med. 2015;34:1549–54. https://doi.org/10.7863/ultra.15.14.08016.
Brat R, Yousef N, Klifa R, Reynaud S, Shankar Aguilera S, et al. Lung ultrasonography score to evaluate oxygenation and surfactant need in neonates treated with continuous positive airway pressure. JAMA Pediatr. 2015;169:e151797. https://doi.org/10.1001/jamapediatrics.2015.1797.
Raimondi F, Cattarossi L, Copetti R. International perspectives: point-of-care chest ultrasound in the neonatal intensive care unit: an Italian perspective. NeoReviews. 2014;15:e2–e6. https://doi.org/10.1542/neo.15-1-e2.
Perri A, Riccardi R, Iannotta R, Di Molfetta DV, Arena R, Vento G, et al. Lung ultrasonography score versus chest X-ray score to predict surfactant administration in newborns with respiratory distress syndrome. Pediatr Pulmonol. 2018;53:1231–6. https://doi.org/10.1002/ppul.24076.
De Martino L, Yousef N, Ben-Ammar R, Raimondi F, Shankar-Aguilera S, De Luca D. Lung ultrasound score predicts surfactant need in extremely preterm neona.tes. Pediatrics. 2018;142:e20180463. https://doi.org/10.1542/peds.2018-0463.
Alonso-Ojembarrena A, Lechuga-Sancho AM, Morales-Arandojo P, Acuñas-Soto S, López-de-Francisco R, Lubián-López SP. Lung ultrasound score and diuretics in preterm infants born before 32 weeks: a pilot study. Pediatr Pulmonol. 2020;55:3312–8. https://doi.org/10.1002/ppul.25098.
Soliman RM, Elsayed Y, Said RN, Abdulbaqi AM, Hashem RH, Aly H. Prediction of extubation readiness using lung ultrasound in preterm infants. Pediatr Pulmonol. 2021;56:2073–80. https://doi.org/10.1002/ppul.25383.
El Amrousy D, Elgendy M, Eltomey M, Elmashad AE. Value of lung ultrasonography to predict weaning success in ventilated neonates. Pediatr Pulmonol. 2020;55:2452–6. https://doi.org/10.1002/ppul.24934.
Raimondi F, Migliaro F, Corsini I, Meneghin F, Dolce P, Pierri L, et al. Lung ultrasound score progress in neonatal respiratory distress syndrome. Pediatrics. 2021;147:e2020030528. https://doi.org/10.1542/peds.2020-030528.
Oulego-Erroz I, Alonso-Quintela P, Terroba-Seara S, Jiménez-González A, Rodríguez-Blanco S. Early assessment of lung aeration using an ultrasound score as a biomarker of developing bronchopulmonary dysplasia: a prospective observational study. J Perinatol. 2021;41:62–68. https://doi.org/10.1038/s41372-020-0724-z.
Loi B, Vigo G, Baraldi E, Raimondi F, Carnielli VP, Mosca F, et al. Lung ultrasound to monitor extremely preterm infants and predict bronchopulmonary dysplasia. a multicenter longitudinal cohort study. Am J Respir Crit Care Med. 2021;203:1398–409. https://doi.org/10.1164/rccm.202008-3131OC.
Raimondi F, Migliaro F, Sodano A, Ferrara T, Lama S, Vallone G, et al. Use of neonatal chest ultrasound to predict noninvasive ventilation failure. Pediatrics. 2014;134:e1089–94. https://doi.org/10.1542/peds.2013-3924.
Lui K, Lee SK, Kusuda S, Adams M, Vento M, Reichman B, et al. International Network for Evaluation of Outcomes (iNeo) of neonates investigators. Trends in outcomes for neonates born very preterm and very low birth weight in 11 high-income countries. J Pediatr. 2019;215:32–40.e14. https://doi.org/10.1016/j.jpeds.2019.08.020.
Cheong JLY, Doyle LW. An update on pulmonary and neurodevelopmental outcomes of bronchopulmonary dysplasia. Semin Perinatol. 2018;42:478–84. https://doi.org/10.1053/j.semperi.2018.09.013.
Ibrahim J, Bhandari V. The definition of bronchopulmonary dysplasia: an evolving dilemma. Pediatr Res. 2018;84:586–8. https://doi.org/10.1038/s41390-018-0167-9.
Onland W, Cools F, Kroon A, Rademaker K, Merkus MP, Dijk PH, et al. Effect of hydrocortisone therapy initiated 7 to 14 days after birth on mortality or bronchopulmonary dysplasia among very preterm infants receiving mechanical ventilation: a randomized clinical trial. JAMA. 2019;321:354–63. https://doi.org/10.1001/jama.2018.21443.
Alvarez-Fuente M, Moreno L, Lopez-Ortego P, Arruza L, Avila-Alvarez A, Muro M, et al. Exploring clinical, echocardiographic and molecular biomarkers to predict bronchopulmonary dysplasia. PLoS ONE. 2019;14:e0213210. https://doi.org/10.1371/journal.pone.0213210.
Álvarez-Fuente M, Moreno L, Mitchell JA, Reiss IK, Lopez P, Elorza D, et al. Preventing bronchopulmonary dysplasia: new tools for an old challenge. Pediatr Res. 2019;85:432–41. https://doi.org/10.1038/s41390-018-0228-0.
Förster K, Sass S, Ehrhardt H, Mous DS, Rottier RJ, Oak P, et al. Early identification of bronchopulmonary dysplasia using novel biomarkers by proteomic screening. Am J Respir Crit Care Med. 2018;197:1076–80. https://doi.org/10.1164/rccm.201706-1218LE.
Rivera L, Siddaiah R, Oji-Mmuo C, Silveyra GR, Silveyra P. Biomarkers for bronchopulmonary dysplasia in the preterm infant. Front Pediatr. 2016;4:33. https://doi.org/10.3389/fped.2016.00033.
Alonso-Ojembarrena A, Serna-Guerediaga I, Aldecoa-Bilbao V, Gregorio-Hernández R, Alonso-Quintela P, Concheiro-Guisán A, et al. The predictive value of lung ultrasound scores in developing bronchopulmonary dysplasia: a prospective multicenter diagnostic accuracy study. Chest. 2021;160:1006–16. https://doi.org/10.1016/j.chest.2021.02.066.
Alonso-Ojembarrena A, Lubián-López SP. Lung ultrasound score as early predictor of bronchopulmonary dysplasia in very low birth weight infants. Pediatr Pulmonol. 2019;54:1404–9.
Louis D, Belen K, Farooqui M, Idiong N, Amer R, Hussain A, et al. Prone versus supine position for lung ultrasound in neonates with respiratory distress. Am J Perinatol. 2021;38:176–81.
Abdelmawla M, Louis D, Narvey M, Elsayed Y. A lung ultrasound severity score predicts chronic lung disease in preterm infants. Am J Perinatol. 2019;36:1357–61. https://doi.org/10.1055/s-0038-1676975.
Higgins RD, Jobe AH, Koso-Thomas M, Bancalari E, Viscardi RM, Hartert TV, et al. Bronchopulmonary dysplasia: executive summary of a workshop. J Pediatr. 2018;197:300–8.
Sweet DG, Carnielli V, Greisen G, Hallman M, Ozek E, Te Pas A, et al. European consensus guidelines on the management of respiratory distress syndrome - 2019 update. Neonatology. 2019;115:432–50. https://doi.org/10.1159/000499361.
Liu J, Guo G, Kurepa D, Volpicelli G, Sorantin E, Lovrenski J, et al. Specification and guideline for technical aspects and scanning parameter settings of neonatal lung ultrasound examination. J Matern Fetal Neonatal Med. 2022;35:1003–16. https://doi.org/10.1080/14767058.2021.1940943.
Mercurio G, D’Arrigo S, Moroni R, Grieco DL, Menga LS, Romano A, et al. Diaphragm thickening fraction predicts noninvasive ventilation outcome: a preliminary physiological study. Crit Care. 2021;25:219. https://doi.org/10.1186/s13054-021-03638-x.
Martínez-Camblor P, Pardo-Fernández JC. The Youden index in the generalized receiver operating characteristic curve context. Int J Biostat (2019);15:/j/ijb.2019.15.issue-1/ijb-2018-0060 /ijb-2018-0060.xml. https://doi.org/10.1515/ijb-2018-0060.
Mojoli F, Bouhemad B, Mongodi S, Lichtenstein D. Lung ultrasound for critically Ill patients. Am J Respir Crit Care Med. 2019;199:701–14. https://doi.org/10.1164/rccm.201802-0236CI.
Zong H, Huang Z, Zhao J, Lin B, Fu Y, Lin Y, et al. The value of lung ultrasound score in neonatology. Front Pediatr. 2022;10:791664. https://doi.org/10.3389/fped.2022.791664.
Woods PL, Stoecklin B, Woods A, Gill AW. Early lung ultrasound affords little to the prediction of bronchopulmonary dysplasia. Arch Dis Child Fetal Neonatal Ed. 2021;106:657–62. https://doi.org/10.1136/archdischild-2020-320830.
Wilson SM, Olver RE, Walters DV. Developmental regulation of lumenal lung fluid and electrolyte transport. Respir Physiol Neurobiol. 2007;159:247–55. https://doi.org/10.1016/j.resp.2007.10.004.
Steinhorn R, Davis JM, Göpel W, Jobe A, Abman S, Laughon M, et al. Chronic pulmonary insufficiency of prematurity: developing optimal endpoints for drug development. J Pediatr. 2017;191:15–21.e1. https://doi.org/10.1016/j.jpeds.2017.08.006.
Liu X, Lv X, Jin D, Li H, Wu H. Lung ultrasound predicts the development of bronchopulmonary dysplasia: a prospective observational diagnostic accuracy study. Eur J Pediatr. 2021;180:2781–9. https://doi.org/10.1007/s00431-021-04021-2.
Acknowledgements
We would like to thank the staff who participated in this study.
Funding
This study is supported by Shenzhen Science and Technology Program (JCYJ20190809170009528 to CX), Shenzhen Fund for Guangdong Provincial High-level Clinical Key Specialties (SZGSP009) and Sanming Project of Medicine in Shenzhen (SZSM201612045).
Author information
Authors and Affiliations
Contributions
Each author made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data. CY conceived and designed the study. ZH, YF, XC, YY, YH, and HY acquired data and analyzed data. The preliminary draft of the manuscript was prepared by HZ, YF, XC, and YY. All authors gave their approval for the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
This study was reviewed by the hospital’s ethics committee (no. SFYLS2019119). Informed consent was provided by each child’s immediate family or guardian before the examination. The study was approved by the Ethics Committee of the Shenzhen Maternity & Child Healthcare Hospital. Oral and written informed consent was obtained from the parents.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zong, H., Huang, Z., Fu, Y. et al. Lung ultrasound score as a tool to predict severity of bronchopulmonary dysplasia in neonates born ≤25 weeks of gestational age. J Perinatol 44, 273–279 (2024). https://doi.org/10.1038/s41372-023-01811-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-023-01811-4