Abstract
Objective
Bethanechol has demonstrated improvement in trachealis tone in animal models, but no trials have studied efficacy in infants. This study aimed to examine if bethanechol improves a standardized pulmonary severity score (PSS) in infants with severe bronchopulmonary dysplasia with a diagnosis of tracheobronchomalacia (TBM).
Study design
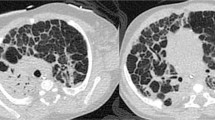
This retrospective cohort study evaluated cases treated with bethanechol matched with controls who did not receive bethanechol. TBM was diagnosed by dynamic computography. Daily PSS was recorded for each infant from 40 to 55 weeks post-menstrual age.
Results
Cases’ mean PSS change was 21% lower than the controls’ mean PSS change pre- and post-bethanechol (95% CI −40%, −2%) by paired t-test (p = 0.03). Matched differences (controls’ PSS – cases’ PSS) demonstrated greater mean PSS difference post-bethanechol compared to pre-bethanechol 0.17, (95% CI 0.05, 0.29) by paired t-test (p = 0.009).
Conclusion
Infants with TBM treated with bethanechol compared to those not treated had a lower PSS reflecting improved respiratory status.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Carden KA, Boiselle PM, Waltz DA, Ernst A. Tracheomalacia and tracheobronchomalacia in children and adults. Chest. 2005;127:984–1005.
Hysinger E, Friedman N, Jensen E, Zhang H, Piccione J. Bronchoscopy in neonates with severe bronchopulmonary dysplasia in the NICU. J Perinatol. 2019;39:263–8.
Bergeron M, Cohen AP, Cotton RT. The management of cyanotic spells in children with oesophageal atresia. Front Pediatr. 2017;5:106.
Wallis C, Alexopoulou E, Antón-Pacheco JL, Bhatt JM, Bush A, Chang AB, et al. ERS statement on tracheomalacia and bronchomalacia in children. Eur Respir J. 2019;54:1900382.
Murgu SD, Colt HG. Tracheobronchomalacia and excessive dynamic airway collapse. Respirology. 2006;11:388–406.
Boiselle PM, O’Donnell CR, Bankier AA, Ernst A, Millet ME, Potemkin A, et al. Tracheal collapsibility in healthy volunteers during forced expiration: assessment with multidetector CT. Radiology 2009;252:255–62.
Gunatilaka CC, Higano NS, Hysinger EB, Gandhi DB, Fleck RJ, Hahn AD, et al. Increased work of breathing due to tracheomalacia in neonates. Ann Am Thorac Soc. 2020;17:1247–56.
Hysinger EB, Friedman NL, Padula MA, Shinohara RT, Zhang H, Panitch HB, et al. Tracheobronchomalacia is associated with increased morbidity in bronchopulmonary dysplasia. Ann Am Thorac Soc. 2017;14:1428–35.
Boogaard R, Huijsmans SH, Pijnenburg MWH, Tiddens HAWM, de Jongste JC, Merkus PJFM. Tracheomalacia and bronchomalacia in children. Chest. 2005;128:3391–7.
Wagner EM, Jacoby DB. Methacholine causes reflex bronchoconstriction. J Appl Physiol. 1999;86:294–7.
Bass R, Santiago M, Smith L, Quinlan C, Panitch H, Giordano T, et al. Bethanechol in Tracheomalacia: two case series and a review of the literature. Pediatr Allergy Immunol Pulmonol. 2018;31:180–3.
Bhutani VK, Koslo RJ, Shaffer TH. The effect of tracheal smooth muscle tone on neonatal airway collapsibility. Pediatr Res. 1986;20:492–5.
Panitch HB, Keklikian EN, Motley RA, Wolfson MR, Schidlow DV. Effect of altering smooth muscle tone on maximal expiratory flows in patients with tracheomalacia. Pediatr Pulmonol. 1990;9:170–6.
Madan A, Brozanski BS, Cole CH, Oden NL, Cohen G, Phelps DL. A pulmonary score for assessing the severity of neonatal chronic lung disease. Pediatrics 2005;115:e450–7.
Ullmann N, Secinaro A, Menchini L, Caggiano S, Verrillo E, Santangelo TP, et al. Dynamic expiratory CT: an effective non-invasive diagnostic exam for fragile children with suspected tracheo-bronchomalacia. Pediatr Pulmonol. 2018;53:73–80.
Ngerncham M, Lee EY, Zurakowski D, Tracy DA, Jennings R. Tracheobronchomalacia in pediatric patients with esophageal atresia: Comparison of diagnostic laryngoscopy/bronchoscopy and dynamic airway multidetector computed tomography. J Pediatr Surg. 2015;50:402–7.
Goo HW. Free-breathing cine CT for the diagnosis of tracheomalacia in young children. Pediatr Radio. 2013;43:922–8.
Greenberg SB. Dynamic pulmonary CT of children. Am J Roentgenol. 2012;199:435–40.
Lee EY, Boiselle PM. Tracheobronchomalacia in infants and children: multidetector CT evaluation. Radiology. 2009;252:7–22.
Lee EY, Zurakowski D, Waltz DA, Mason KP, Riaz F, Ralph A, et al. MDCT evaluation of the prevalence of tracheomalacia in children with mediastinal aortic vascular anomalies. J Thorac Imaging. 2008;23:258–65.
Greenberg SB, Dyamenahalli U. Dynamic pulmonary computed tomography angiography: a new standard for evaluation of combined airway and vascular abnormalities in infants. Int J Cardiovasc Imaging. 2014;30:407–14.
Jensen EA, Dysart K, Gantz MG, McDonald S, Bamat NA, Keszler M, et al. The diagnosis of bronchopulmonary dysplasia in very preterm infants. An evidence-based approach. Am J Respir Crit Care Med. 2019;200:751–9.
Panitch HB, Talmaciu I, Heckman J, Wolfson MR, Shaffer TH. Quantitative bronchoscopic assessment of airway collapsibility in newborn lamb tracheae. Pediatr Res. 1998;43:832–9.
Davis S, Jones M, Kisling J, Angelicchio C, Tepper RS. Effect of continuous positive airway pressure on forced expiratory flows in infants with tracheomalacia. Am J Respir Crit Care Med. 1998;158:148–52.
Nealon E, Rivera BK, Cua CL, Ball MK, Stiver C, Boe BA, et al. Follow-up after percutaneous patent ductus arteriosus occlusion in lower weight infants. J Pediatr. 2019;212:144–50. e3
Pugh CP, Arkansas Children’s Hospital Research Institute. The effect of bethanechol on work of breathing and expiratory tracheal collapse in infants with tracheobronchomalacia measured by electrical activity of the diaphragm and bronchoscopy. (2022). Available from: https://clinicaltrials.gov/ct2/show/NCT05299008.
Author information
Authors and Affiliations
Contributions
All authors composed and edited this manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pugh, C.P., Akmyradov, C., Courtney, S.E. et al. The effect of bethanechol on tracheobronchomalacia in preterm infants with bronchopulmonary dysplasia: a retrospective cohort study. J Perinatol 44, 288–293 (2024). https://doi.org/10.1038/s41372-023-01799-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-023-01799-x