Abstract
Objective
Infants with severe bronchopulmonary dysplasia (sBPD) have complex medical courses. We developed the clinician-rated Optimal State Scoring Tool (OSST) that measures factors relevant to clinical improvement of sBPD and investigated preliminary validity using linear growth outcome and OSST scores in sBPD patients.
Methods
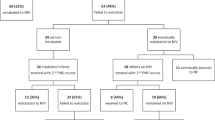
Tool development process and pilot findings are provided for 13 patients evaluated longitudinally. OSST scores, length measurements, and steroid dependency values were obtained. Changes in OSST scores and lengths were examined using linear mixed-effect models.
Results
OSST scores were significantly correlated with linear growth (95% CI 0.36, 0.57). The steroid-dependent group showed significantly slower rate of linear growth (95% CI 0.74, 1.05) and slower rate of increase in OSST scores (95% CI 0.99, 2.13) compared to the non-steroid-dependent group, with the OSST showing the largest effect size.
Conclusion
Pilot data reflect promising evidence for OSST construct validity in monitoring clinical outcomes in sBPD patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article [and its supplementary information files]. Research data are confidential.
References
Poindexter BB, Feng R, Schmidt B, Aschner JL, Ballard RA, Hamvas A, et al. Comparisons and limitations of current definitions of bronchopulmonary dysplasia for the prematurity and respiratory outcomes program. Ann Am Thorac Soc. 2015;12:1822–30.
Higgins RD, Jobe AH, Koso-Thomas M, Bancalari E, Viscardi RM, Hartert TV, et al. Bronchopulmonary dysplasia: executive summary of a workshop. J Pediatr. 2018;197:300–8.
Ramel SE, Demerath EW, Gray HL, Younge N, Boys C, Georgieff MK. The relationship of poor linear growth velocity with neonatal illness and two-year neurodevelopment in preterm infants. Neonatology. 2012;102:19–24.
Guaman MC, Gien J, Baker CD, Zhang H, Austin ED, Collaco JM. Point prevalence, clinical characteristics, and treatment variation for infants with severe bronchopulmonary dysplasia. Am J Perinatol. 2015;32:960–7.
Logan JW, Burdo-Hartman W, Lynch SK. Optimizing neurodevelopment in severe bronchopulmonary dysplasia. NeoReviews. 2017;18:e598–605.
Bauer SE, Schneider L, Lynch SK, Malleske DT, Shepherd EG, Nelin LD. Factors associated with neurodevelopmental impairment in bronchopulmonary dysplasia. J Pediatr. 2020;218:22–7.e2.
Logan JW, Lynch SK, Curtiss J, Shepherd EG. Clinical phenotypes and management concepts for severe, established bronchopulmonary dysplasia. Paediatr Respir Rev. 2019;31:58–63.
Keilt MJ, Logan JW, Backes CH, Reber KM, Nelin LD, Shepherd EG. In-hospital outcomes of later referrals for established bronchopulmonary dysplasia. J Perinatol. 2021;41:1972–82.
Vento G, Tirone C, Paladini A, Lio A, Tana M. Weaning from the ventilator in bronchopulmonary dysplasia. Clin Perinatol. 2021;48:895–906.
Pfister KM, Ramel SE. Linear growth and neurodevelopmental outcomes. Clin Perinatol. 2014;41:309–21.
Sanchez-Solis M, Perez-Fernandez V, Bosch-Gimenez V, Quesada JJ, Garcia-Marcos L. Lung function gain in preterm infants with and without bronchopulmonary dysplasia. Pediatr Pulmonol. 2016;51:936–42.
Abman SH, Collaco JM, Shepherd EG, Keszler M, Cuevas-Guaman M, Welty SE, et al. Interdisciplinary care of children with severe bronchopulmonary dysplasia. J Pediatr. 2017;181:12–28.e1.
Boateng GO, Neilands TB, Frongillo EA, Melgar-Quiñonez HR, Young SL. Best practices for developing and validating scales for health, social, and behavioral research: a primer. Front Public Health. 2018;6:149 https://doi.org/10.3389/fpubh.2018.00149.
Natarajan G, Johnson YR, Brozanski B, Farrow KN, Zaniletti I, Padula MA, et al. Postnatal weight gain in preterm infants with severe bronchopulmonary dysplasia. Am J Perinatol. 2014;31:223–30.
Meyers JM, Tan S, Bell EF, Duncan AF, Guillet R, Stoll BJ, et al. Neurodevelopmental outcomes among extremely premature infants with linear growth restriction. J Perinatol. 2019;39:193–202.
Lagatta JM, Hysinger EB, Zaniletti I, Wymore EM, Vyas-Read S, Yallapragada S, et al. The impact of pulmonary hypertension in preterm infants with severe bronchopulmonary dysplasia through 1 year. J Pediatr. 2018;203:218–24.e3.
Cuestas E, Aguilera B, Cerutti M, Rizzotti A. Sustained neonatal inflammation is associated with poor growth in infants born very preterm during the first year of life. J Pediatr. 2019;205:91–7.
Stavrou S, Nicolaides NC, Critselis E, Darviri C, Charmandari E, Chrousos GP. Paediatric stress: from neuroendocrinology to contemporary disorders. Eur J Clin Investig. 2017;47:262–9.
Gardelis JG, Hatzis TD, Stamogiannou LN, Dona AA, Fotinou AD, Brestas PS, et al. Activity of the growth hormone/insulin-like growth factor-I axis in critically ill children. J Pediatr Endocrinol Metab. 2005;18:363–72.
Gelato MC. The growth hormone/insulin-like growth factor axis in critical illness. J Pediatr Endocrinol Metab. 2000;13:S1023–9.
Van Dokkum NH, de Kroon MLA, Reijneveld SA, Bos AF. Neonatal stress, health, and development in preterms: a systematic review. Pediatrics. 2021;148:e202105414.
Yaribeygi H, Panahi Y, Sahraei H, Johnston TP, Sahebkar A. The impact of stress on body function: a review. EXCLI J. 2017;16:1057–72.
Halliday HL. The effect of postnatal steroids on growth and development. J Perinat Med. 2001;29:281–5.
Balany J, Bhandari V. Understanding the impact of infection, inflammation, and their persistence in the pathogenesis of bronchopulmonary dysplasia. Front Med. 2015;2:90.
Thekkeveedu KR, Guaman MC, Shivanna B. Bronchopulmonary dysplasia: a review of pathogenesis and pathophysiology. Respir Med. 2017;132:170–7.
Curtiss J, Zhang H, Griffiths P, Shepherd EG, Lynch S. Nutritional management of the infant with severe bronchopulmonary dysplasia. NeoReviews. 2015;16:e674–9.
Shepherd EG, Knupp AM, Welty SE, Susey KM, Gardner WP, Gest AL. An interdisciplinary bronchopulmonary dysplasia program is associated with improved neurodevelopmental outcomes and fewer rehospitalizations. J Perinatol. 2012;32:33–8.
Acknowledgements
We would like to thank Tara Benninger Ph.D., Emily Bingham RD, Jillane Downs MS, APRN, and Melissa Hanin MOT/L for their support and contributions.
Author information
Authors and Affiliations
Contributions
Each author made substantial contributions to conception and design. JC, TP, BLG, LL, MM, LP, KS, MS, and SL collected and contributed to the interpretation of the data. KGS analyzed and interpreted the data and reviewed and revised the final manuscript. JC drafted the initial manuscript and reviewed and revised the final manuscript. PG and TP reviewed and revised the initial draft. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Curtiss, J., Griffiths, P., Stephenson, K.G. et al. The Optimal State Scoring Tool: guidance for interdisciplinary care of infants with severe bronchopulmonary dysplasia and its relation to linear growth. J Perinatol 43, 1301–1307 (2023). https://doi.org/10.1038/s41372-023-01680-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-023-01680-x