Abstract
Objective
We sought to identify associations between prenatal care coordination (PNC) and outcomes in hypoplastic left heart syndrome (HLHS).
Study design
We hypothesized that suboptimal PNC is associated with worse pre-operative status. HLHS patients from 2016 through 2019 were identified using a multicenter registry. Optimal PNC was defined as (1) a completed interdisciplinary conference and (2) closed-loop communication with the obstetric team. Associations between PNC and outcomes were identified.
Results
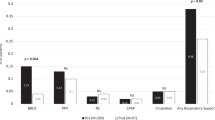
Of 1441 patients, 1242 (86%) had prenatal diagnosis. Among those with a prenatal diagnosis, PNC was achieved in only 845 (68%). Suboptimal PNC was associated with adverse events (50% vs 40%, p < 0.001), inotrope need (19% vs 13%, p = 0.007), mechanical ventilation (22% vs 16%, p = 0.016), and parenteral feeding (60% vs 46%, p < 0.001). African–American race and non-commercial insurance were associated with a lower likelihood of optimal PNC (p = 0.006 and p < 0.001, respectively).
Conclusion
Improving PNC and overcoming racial and socioeconomic barriers are important targets to improve HLHS perinatal care.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
All data are presented in the main manuscript.
References
Donofrio MT, Levy RJ, Schuette JJ, Skurow-Todd K, Sten M-BB, Stallings C, et al. Specialized delivery room planning for fetuses with critical congenital heart disease. Am J Cardiol. 2013;111:737–47.
Brown DW, Cohen KE, O’Brien P, Gauvreau K, Klitzner TS, Beekman RH, et al. Impact of prenatal diagnosis in survivors of initial palliation of single ventricle heart disease: analysis of the national pediatric cardiology quality improvement collaborative database. Pediatr Cardiol. 2014;36:314–21.
Kumar RK, Newburger JW, Gauvreau K, Kamenir SA, Hornberger LK. Comparison of outcome when hypoplastic left heart syndrome and transposition of the great arteries are diagnosed prenatally versus when diagnosis of these two conditions is made only postnatally. Am J Cardiol. 1999;83:1649–53.
Rychik J, Donaghue DD, Levy S, Fajardo C, Combs J, Zhang X, et al. Maternal psychological stress after prenatal diagnosis of congenital heart disease. J Pediatr. 2013;162:302–307.e1.
Sanapo L, Pruetz JD, Słodki M, Goens MB, Moon-Grady AJ, Donofrio MT. Fetal echocardiography for planning perinatal and delivery room care of neonates with congenital heart disease. Echocardiography. 2017;34:1804–21.
Kugler JD, Beekman Iii RH, Rosenthal GL, Jenkins KJ, Klitzner TS, Martin GR, et al. Development of a pediatric cardiology quality improvement collaborative: from inception to implementation. From the Joint Council on Congenital Heart Disease Quality Improvement Task Force. Congenit Heart Dis. 2009;4:318–28.
Roux AVD, Merkin SS, Arnett D, Chambless L, Massing M, Nieto FJ, et al. Neighborhood of residence and incidence of coronary heart disease. N. Engl J Med. 2001;345:99–106.
Jabrayilov R, Vermeulen KM, Detzel P, Dainelli L, van Asselt ADI, Krabbe PFM. Valuing health status in the first year of life: the infant health-related quality of life instrument. Value Health. 2019;22:721–7.
Krishnan AN, Jacobs M, Bhat A, Chelliah A, Chiu J, Cuneo B, et al. Identifying socioeconomic and geographic barriers to prenatal detection of hypoplastic left heart syndrome and transposition of the great arteries. J Am Coll Cardiol. 2019;73:587.
Author information
Authors and Affiliations
Contributions
DS, EB, AB, TL, JP, CR, JV, and DB contributed to the design of the work and interpretation of the data. KG and EB performed data analysis. All authors participated in drafting and critically revising the manuscript for important intellectual content. All authors approved the final version of this manuscript and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Schidlow, D.N., Gauvreau, K., Bucholz, E.M. et al. Prenatal care coordination, racial and socioeconomic inequities, and pre- and post-operative outcomes in hypoplastic left heart syndrome. J Perinatol 43, 378–384 (2023). https://doi.org/10.1038/s41372-022-01571-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-022-01571-7
This article is cited by
-
Social Determinants of Health and Health Equity in Pediatric Cardiology Outcomes
Current Treatment Options in Pediatrics (2023)