Abstract
Objective
To study the growth and neurodevelopmental outcome of very and moderate preterm infants (VMPT) compared to term appropriate-for-age (term AGA) infants at 18-months corrected age.
Methods
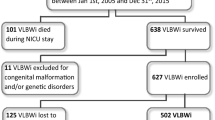
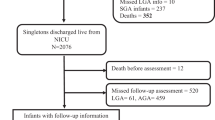
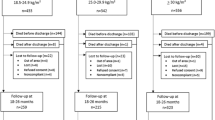
This prospective cohort study enrolled consecutively born 212 VMPT infants and 250 term AGA controls delivered during study period.
Outcome measures
Major neurodevelopmental impairment (NDI) defined as any one of cerebral palsy, motor (MoDQ) or mental developmental quotient (MoDQ) <70 on Developmental Assessment Scale for Indian infants, visual or hearing impairment, or epilepsy, and growth outcomes.
Results
Among 195 VMPT and 240 term AGA infants who completed follow-up, the frequency of major NDI was 12.8% and 2.5% respectively (RR 5.1; 95% CI [2.13–12.19]). Major NDI was higher among infants <28 weeks gestation (39%) and birthweight <1000 grams (27%). A quarter of VMPT infants exhibited wasting and 18% stunting than 7% each among controls.
Conclusion
VMPT infants had a higher frequency of major NDI and growth failure at 18-months.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
Dataset can be requested by writing to the corresponding author.
References
Blencowe H, Lee AC, Cousens S, Bahalim A, Narwal R, Zhong N, et al. Preterm birth-associated neurodevelopmental impairment estimates at regional and global levels for 2010. Pediatr Res. 2013;74:17–34.
Council on Children With Disabilities; Section on Developmental Behavioral Pediatrics; Bright Futures Steering Committee; Medical Home Initiatives for Children With Special Needs Project Advisory Committee. Identifying infants and young children with developmental disorders in the medical home: an algorithm for developmental surveillance and screening. Pediatrics 2006;118:405–20.
Allotey J, Zamora J, Cheong-See F, Kalidindi M, Arroyo-Manzano D, Asztalos E, et al. Cognitive, motor, behavioural and academic performances of children born preterm: a meta-analysis and systematic review involving 64 061 children. BJOG. 2018;125:16–25.
Chaudhari S, Kulkarni S, Pandit A, Deshmukh S. Mortality and morbidity in high risk infants during a six year follow-up. Indian Pediatr. 2000;37:1314–20.
Chaudhari S, Otiv M, Chitale A, Pandit A, Hoge M. Pune low birth weight study−cognitive abilities and educational performance at twelve years. Indian Pediatr. 2004;41:121–8.
Chaudhari S, Otiv M, Khairnar B, Pandit A, Hoge M, Sayyad M. Pune low birth weight study - birth to adulthood - cognitive development. Indian Pediatr. 2013;50:853–7.
Chaudhari S, Otiv M, Khairnar B, Pandit A, Hoge M, Sayyad M. Pune low birth weight study, growth from birth to adulthood. Indian Pediatr. 2012;49:727–32.
Modi M, Saluja S, Kler N, Batra A, Kaur A, Garg P, et al. Growth and neurodevelopmental outcome of VLBW infants at 1 year corrected age. Indian Pediatr. 2013;50:573–7.
Mukhopadhyay K, Mahajan R, Malhi P, Kumar A. Neurodevelopmental outcome of extremely low birth weight children at corrected age of two years. Indian Pediatr. 2016;53:391–3.
Murki S, Kallem VR, Gururaj J, Bashir T, Oleti TP, Kiran S. Growth and neurodevelopmental outcomes at 12 to 18 months of corrected age in preterm infants born small for gestational age. Indian Pediatr. 2020;57:301–4.
Surveillance of Cerebral Palsy in Europe. Surveillance of cerebral palsy in Europe: a collaboration of cerebral palsy surveys and registers. Surveillance of Cerebral Palsy in Europe (SCPE). Dev Med Child Neurol. 2000;42:816–24.
WHO Multicentre Growth Reference Study Group. WHO child growth standards based on length/height, weight and age. Acta Paediatr Suppl. 2006;450:76–85.
Serenius F, Källén K, Blennow M, Ewald U, Fellman V, Holmström G, et al. Neurodevelopmental outcome in extremely preterm infants at 2.5 years after active perinatal care in Sweden. JAMA. 2013;309:1810–20.
Fenton TR, Kim JH. A systematic review and meta-analysis to revise the Fenton growth chart for preterm infants. BMC Pediatr. 2013;13:59.
Sharma PK, Sankar MJ, Sapra S, Saxena R, Karthikeyan CV, Deorari A, et al. Growth and neurosensory outcomes of preterm very low birth weight infants at 18 months of corrected age. Indian J Pediatr. 2011;78:1485–90.
Mukhopadhyay K, Malhi P, Mahajan R, Narang A. Neurodevelopmental and behavioral outcome of very low birth weight babies at corrected age of 2 years. Indian J Pediatr. 2010;77:963–7.
Oommen SP, Santhanam S, John H, Roshan R, Swathi TO, Padankatti C, et al. Neurodevelopmental outcomes of very low birth weight infants at 18–24 months, corrected gestational age in a Tertiary Health Centre: a prospective cohort study. J Trop Pediatr. 2019;65:552–60.
Ballot DE, Potterton J, Chirwa T, Hilburn N, Cooper PA. Developmental outcome of very low birth weight infants in a developing country. BMC Pediatr. 2012;12:11.
Guillén U, DeMauro S, Ma L, Zupancic J, Roberts R, Schmidt B, et al. Relationship between attrition and neurodevelopmental impairment rates in extremely preterm infants at 18 to 24 months: a systematic review. Arch Pediatr Adolesc Med. 2012;166:178–84.
Twilhaar ES, Wade RM, de Kieviet JF, van Goudoever JB, van Elburg RM, Oosterlaan J. Cognitive outcomes of children born extremely or very preterm since the 1990s and associated risk factors: a meta-analysis and meta-regression. JAMA Pediatr. 2018;172:361–7.
Brydges CR, Landes JK, Reid CL, Campbell C, French N, Anderson M. Cognitive outcomes in children and adolescents born very preterm: a meta-analysis. Dev Med Child Neurol. 2018;60:452–68.
Arpi E, D’Amico R, Lucaccioni L, Bedetti L, Berardi A, Ferrari F. Worse global intellectual and worse neuropsychological functioning in preterm-born children at preschool age: a meta-analysis. Acta Paediatr. 2019;108:1567–79.
Draper ES, Zeitlin J, Manktelow BN, Piedvache A, Cuttini M, Edstedt Bonamy AK, et al. EPICE cohort: two-year neurodevelopmental outcomes after very preterm birth. Arch Dis Child Fetal Neonatal Ed. 2020;105:350–6.
Pierrat V, Marchand-Martin L, Arnaud C, Kaminski M, Resche-Rigon M, Lebeaux C, et al. Neurodevelopmental outcome at 2 years for preterm children born at 22 to 34 weeks’ gestation in France in 2011: EPIPAGE-2 cohort study. BMJ. 2017;358:j3448.
Burnett AC, Cheong JLY, Doyle LW. Biological and social influences on the neurodevelopmental outcomes of preterm infants. Clin Perinatol. 2018;45:485–500.
Dusick AM, Poindexter BB, Ehrenkranz RA, Lemons JA. Growth failure in the preterm infant: can we catch up? Semin Perinatol. 2003;27:302–10.
Chan SH, Johnson MJ, Leaf AA, Vollmer B. Nutrition and neurodevelopmental outcomes in preterm infants: a systematic review. Acta Paediatr. 2016;105:587–99.
de Kieviet JF, Piek JP, Aarnoudse-Moens CS, Oosterlaan J. Motor development in very preterm and very low-birth-weight children from birth to adolescence: a meta-analysis. JAMA. 2009;302:2235–42.
Phatak P. Developmental Assessment Scales for Indian Infants (DASII) – Revised Baroda Norms Manual, 1997.
Wolke D, Ratschinski G, Ohrt B, Riegel K. The cognitive outcome of very preterm infants may be poorer than often reported: an empirical investigation of how methodological issues make a big difference. Eur J Pediatr. 1994;153:906–15.
Acknowledgements
Ajay, Reena, Faizan, Sukhram Babu, Manju Saxena, Farha, Suresh, Nisha, Sant, Meenakshi, Anuja Aggarwala, AK Gupta, Kanak, Alok Thakkar, Garima, Sandhya.
Funding
This work was supported by the Indian Council of Medical Research (ICMR) Grant Number 5/7/305/08-RHN.
Author information
Authors and Affiliations
Contributions
SS and TS contributed to interpretation of data, data analysis, drafting of the manuscript, and critical revisions of the manuscript. SG conceptualized and designed the study, contributed to data collection and data analyses, and critically reviewed the manuscript. RS, KS, SG, AK, MJ coordinated and supervised data collection and critically reviewed the manuscript. SS, SG, and MB coordinated and supervised data collection. CPY and VS contributed to data analyses and critically reviewed the manuscript. AT and VKP conceptualized and designed the study and critically reviewed the manuscript. RA and MJS conceptualized and designed the study, supervised the initial analyses, reviewed and revised the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
The study has been approved by Institutional ethics committee of All India Institute of Medical Sciences, New Delhi (Ref: IEC/P-05/04.01.2010). Written informed consent was obtained from one or both parents prior to enrollment. The study was performed in accordance with the Declaration of Helsinki.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sivanandan, S., Gupta, S., Sahoo, T. et al. Short-term neurodevelopment and growth outcomes of very and moderate preterm Indian infants. J Perinatol 42, 1489–1495 (2022). https://doi.org/10.1038/s41372-022-01519-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-022-01519-x