Abstract
Objective
Determine incidence and risk factors for readmissions in early infancy.
Study design
Secondary analysis of data from the Cesarean Section Optimal Antibiotic Prophylaxis trial. All unplanned revisits (unplanned clinic, ER visits, and hospital readmissions) and hospital readmissions (initial discharge to 3-month follow-up) were analyzed.
Results
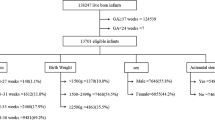
295 (15.9%) of 1850 infants had revisits with risk factors being ethnicity (adjusted odds ratio (aOR): 0.6 for Hispanic), maternal postpartum antibiotics (1.89), azithromycin treatment (1.22), small for gestational age (1.68), apnea (3.82), and hospital stay after birth >90th percentile (0.49). 71 (3.8%) of 1850 infants were readmitted with risk factors being antenatal steroids (aOR 2.49), elective repeat C/section (0.72), postpartum maternal antibiotics (2.22), O2 requirement after delivery room (2.82), and suspected/proven neonatal sepsis (0.55).
Conclusion(s)
Multiple risk factors were identified, suggesting potential impact on the neonatal microbiome (maternal postpartum antibiotics) or issues related to access/cost of care (Hispanic ethnicity associated with fewer revisits).
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Lorch SA. National quality measures in perinatal medicine. Clin Perinatol. 2017;44:485–509.
Toomey SL, Peltz A, Loren S, Tracy M, Williams K, Pengeroth L, et al. Potentially preventable 30-day hospital readmissions at a children’s hospital. Pediatrics. 2016;138:e20154182.
Jonas JA, Devon EP, Ronan JC, Ng SC, Owusu-McKenzie JY, Strausbaugh JT, et al. Determining preventability of pediatric readmissions using fault tree analysis. J Hosp Med. 2016;11:329–35.
Hain PD, Gay JC, Berutti TW, Whitney GM, Wang W, Saville BR. Preventability of early readmissions at a children’s hospital. Pediatrics. 2013;131:e171–81.
Zhou H, Roberts PA, Dhaliwal SS, Della PR. Risk factors associated with paediatric unplanned hospital readmissions: a systematic review. BMJ Open. 2019;9:e020554.
Kuzniewicz MW, Parker SJ, Schnake-Mahl A, Escobar GJ. Hospital readmissions and emergency department visits in moderate preterm, late preterm, and early term infants. Clin Perinatol. 2013;40:753–75.
Underwood MA, Danielsen B, Gilbert WM. Cost, causes and rates of rehospitalization of preterm infants. J Perinatol. 2007;27:614–9.
Dietz PM, Rizzo JH, England LJ, Callaghan WM, Vesco KK, Bruce FC, et al. Early term delivery and health care utilization in the first year of life. J Pediatr. 2012;161:234–9 e231.
Radmacher P, Massey C, Adamkin D. Hidden morbidity with “successful” early discharge. J Perinatol. 2002;22:15–20.
Tomashek KM, Shapiro-Mendoza CK, Weiss J, Kotelchuck M, Barfield W, Evans S, et al. Early discharge among late preterm and term newborns and risk of neonatal morbidity. Semin Perinatol. 2006;30:61–8.
Maisels MJ, Kring E. Length of stay, jaundice, and hospital readmission. Pediatrics. 1998;101:995–8.
Soskolne EI, Schumacher R, Fyock C, Young ML, Schork A. The effect of early discharge and other factors on readmission rates of newborns. Arch Pediatr Adolesc Med. 1996;150:373–9.
Metcalfe A, Mathai M, Liu S, Leon JA, Joseph KS. Proportion of neonatal readmission attributed to length of stay for childbirth: a population-based cohort study. BMJ Open. 2016;6:e012007.
Hensman AM, Erickson-Owens DA, Sullivan MC, Quilliam BJ. Determinants of neonatal readmission in healthy term infants: results from a nested case-control study [published online ahead of print, 2020 Mar 2]. Am J Perinatol. 2020. https://doi.org/10.1055/s-0040-1702936.
Roca A, Oluwalana C, Bojang A, Camara B, Kampmann B, Bailey R, et al. Oral azithromycin given during labour decreases bacterial carriage in the mothers and their offspring: a double-blind randomized trial. Clin Microbiol Infect. 2016;22:565 e561–9.
Chan GJ, Stuart EA, Zaman M, Mahmud AA, Baqui AH, Black RE. The effect of intrapartum antibiotics on early-onset neonatal sepsis in Dhaka, Bangladesh: a propensity score matched analysis. BMC Pediatr. 2014;14:104.
Reed BD, Schibler KR, Deshmukh H, Ambalavanan N, Morrow AL. The impact of maternal antibiotics on neonatal disease. J Pediatr. 2018;197:97–103 e103.
Young PC, Korgenski K, Buchi KF. Early readmission of newborns in a large health care system. Pediatrics. 2013;131:e1538–44.
Tita AT, Szychowski JM, Boggess K, Saade G, Longo S, Clark E, et al. Adjunctive azithromycin prophylaxis for cesarean delivery. N Engl J Med. 2016;375:1231–41.
Patrick SW, Burke JF, Biel TJ, Auger KA, Goyal NK, Cooper WO. Risk of hospital readmission among infants with neonatal abstinence syndrome. Hosp Pediatr. 2015;5:513–9.
Turi KN, Wu P, Escobar GJ, Gebretsadik T, Ding T, Walsh EM, et al. Prevalence of infant bronchiolitis-coded healthcare encounters attributable to RSV. Health Sci Rep. 2018;1:e91.
Toizumi M, Suzuki M, Nguyen HAT, Le MN, Ariyoshi K, Moriuchi H, et al. Viral acute respiratory illnesses in young infants increase the risk of respiratory readmission. Pediatr Infect Dis J. 2018;37:1217–22.
Cox DW, Khoo SK, Zhang G, Lindsay K, Keil AD, Knight G, et al. Rhinovirus is the most common virus and rhinovirus-C is the most common species in paediatric intensive care respiratory admissions. Eur Respir J. 2018;52:2.
Rodriguez VA, Goodman DM, Bayldon B, Budin L, Michelson KN, Garfield CF, et al. Pediatric readmissions within 3 days of discharge: preventability, contributing factors, and necessity. Hosp Pediatr. 2019;9:241–8.
Kogon BE, Oster ME, Wallace A, Chiswell K, Hill KD, Cox ML, et al. Readmission after pediatric cardiothoracic surgery: an analysis of the society of thoracic surgeons database. The. Ann Thorac Surg. 2019;107:1816–23.
Zook HG, Payne NR, Puumala SE, Ziegler KM, Kharbanda AB. Racial/ethnic variation in emergency department care for children with asthma. Pediatr Emerg Care. 2019;35:209–15.
Ju M, Luna N, Park KT. The effect of limited english proficiency on pediatric hospital readmissions. Hosp Pediatr. 2017;7:1–8.
Samuels-Kalow ME, Stack AM, Amico K, Porter SC. Parental language and return visits to the emergency department after discharge. Pediatr Emerg Care. 2017;33:402–4.
Alpern ER, Clark AE, Alessandrini EA, Gorelick MH, Kittick M, Stanley RM, et al. Recurrent and high-frequency use of the emergency department by pediatric patients. Acad Emerg Med. 2014;21:365–73.
Simon TD, Bublitz Emsermann C, Dickinson LM, Hambidge SJ. Lower rates of emergency department injury visits among Latino children in the USA: no association with health insurance. Inj Prev. 2006;12:248–52.
Lee HC, Bardach NS, Maselli JH, Gonzales R. Emergency department visits in the neonatal period in the United States. Pediatr Emerg Care. 2014;30:315–8.
Beniflah JD, Little WK, Simon HK, Sturm J. Effects of immigration enforcement legislation on Hispanic pediatric patient visits to the pediatric emergency department. Clin Pediatr (Philos). 2013;52:1122–6.
Higgins RD, Saade G, Polin RA, Grobman WA, Buhimschi IA, Watterberg K, et al. Evaluation and management of women and newborns with a maternal diagnosis of chorioamnionitis: summary of a workshop. Obstet Gynecol. 2016;127:426–36.
Mathew JL. Effect of maternal antibiotics on breast feeding infants. Postgrad Med J. 2004;80:196–200.
Funding
This study is funded by NIH (R01 HD064729).
C/SOAP Consortium
Rachel LeDuke12, Janatha Grant12, Lee Ann Merin12, Marci Tew12, Gloria Adam12, Zhara Rahman12, Rebecca Quinn12, Yukiko Nakamura Orange13, Christopher Parks13, Richard Mailhot13, Robin Steele13, Sue Cliver13, Ashutosh Tamhane13, Karen Dorman14, Linda Manor14, Sue Pope14, Carmen Beamon15, Beth Morgan15, Ester Godbold16, Cecelia Recabarren16, Maria Bahena16, Brenda Aguillon16, Virginia Huaracha16, Maria Wilson-Jimenez16, Lisa Garcia16, Masoomeh Ehsani16, Sa Tran16, Christine Servay17, Barbara Conley17, Pat Pandya17, Elaine Lofland18, Kim Potthoff18, Vanessa Johnson19, Kedra Wallace19, James N. MartinJr19, Richard Ogletree19, Michael Varner20, Shanna Salmon20, Suzanne Timothy20, Amber Sowles20, Kim Hill20, Winter Redd20, Amanda Behunin21, Sandi Dellerman21, Michael Nunley21, Richard Cox21, Melissa Hofer21, Caroline Torres22, Connie Eng22, M. Hutchison23, Paula Givens23, Felecia Ortiz23, Vu Ta23, Christine Wong23, Michael George23.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Members of the C/SOAP Consortium are listed below Acknowledgements
Rights and permissions
About this article
Cite this article
Ambalavanan, N., Jauk, V., Szychowski, J.M. et al. Epidemiology of readmissions in early infancy following nonelective cesarean delivery. J Perinatol 41, 24–31 (2021). https://doi.org/10.1038/s41372-020-0730-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-020-0730-1