Abstract
Objective
To characterize demographics and trends in length of stay (LOS), morbidities, and mortality in late preterm infants.
Study design
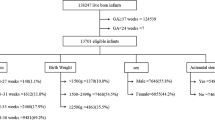
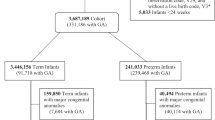
Cohort study of infants born between 34 0/7 and 36 6/7 weeks gestation between 1999 and 2018 without major congenital anomalies at Pediatrix Medical Group neonatal intensive care units (NICUs).
Results
307,967 infants from 410 NICUs met inclusion criteria. The median (25th–75th percentile) LOS was 11 (8–16) days in the entire period. Postmenstrual age (PMA) at discharge increased during the cohort for all gestational ages (p < 0.001). There was a decrease in invasive ventilation, receipt of phototherapy, and reflux medications observed (p < 0.001).
Conclusion
In this large cohort, given 20 years of time for medical advancement, there was no significant improvement in the LOS of late preterm infants. All infants had an increased PMA at discharge, despite multiple practice changes that were observed.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The data that support the findings of this study are available from Pediatrix Clinical Data Warehouse but restrictions apply to the availability of these data, which were used under license for the current study, and so are not publicly available. Data are however available from the authors upon reasonable request and with permission of Pediatrix Clinical Data Warehouse.
References
Raju TNK. The problem of late-preterm (near-term) births: a workshop summary. Pediatr Res. 2006;60:775–6.
Williams JE, Pugh Y. The Late Preterm: A Population at Risk. Crit Care Nurs Clin North Am. 2018;30:431–43.
Tomashek KM, Shapiro-Mendoza CK, Weiss J, Kotelchuck M, Barfield W, Evans S, et al. Early Discharge Among Late Preterm and Term Newborns and Risk of Neonatal Morbidity. Semin Perinatol. 2006;30:61–8.
Pulver LS, Denney JM, Silver RM, Young PC. Morbidity and discharge timing of late preterm newborns. Clin Pediatrics. 2010;49:1061–7.
Martin JA, Hamilton BE, Osterman MJK, Driscoll AK. Births: Final Data for 2019. Natl Vital- Stat Rep. 2021;70:1–51.
Hamilton BE, Martin JA, Osterman MJK, Curtin SC, Matthews TJ. Births: Final Data for 2014. Natl Vital- Stat Rep. 2015;64:1–64.
Mally PV, Bailey S, Hendricks-Muñoz KD. Clinical Issues in the Management of Late Preterm Infants. Curr Probl Pediatr Adolesc Health Care. 2010;40:218–33.
Horgan MJ. Management of the late preterm infant: not quite ready for prime time. Pediatr Clin North Am. 2015;62:439–51.
Karnati S, Kollikonda S, Abu-Shaweesh J. Late preterm infants—Changing trends and continuing challenges. Int J Pediatr Adolesc Med. 2020;7:36–44.
Spitzer AR, Ellsbury D, Clark RH. The Pediatrix BabySteps® Data Warehouse–a unique national resource for improving outcomes for neonates. Indian J Pediatr. 2015;82:71–9.
Olsen IE, Groveman SA, Lawson ML, Clark RH, Zemel BS. New intrauterine growth curves based on United States data. Pediatrics 2010;125:e214–24.
Stoll BJ, Hansen NI, Sánchez PJ, Faix RG, Poindexter BB, Van Meurs KP, et al. Early onset neonatal sepsis: the burden of group B Streptococcal and E. coli disease continues. Pediatrics 2011;127:817–26.
Hornik CP, Fort P, Clark RH, Watt K, Benjamin DK, Smith PB, et al. Early and late onset sepsis in very-low-birth-weight infants from a large group of neonatal intensive care units. Early Hum Dev. 2012;88:S69–74.
Jefferies AL, Lyons ER, Shah PS, Shah V. Impact of late preterm birth on neonatal intensive care resources in a tertiary perinatal center. Am J Perinatol. 2013;30:573–8.
Wang ML, Dorer DJ, Fleming MP, Catlin EA. Clinical outcomes of near-term infants. Pediatrics. 2004;114:372–6.
Aly H, Hoffman H, El-Dib M, Said L, Mohamed M. Factor affecting length of stay in late preterm infants: an US national database study. J Matern Fetal Neonatal Med. 2015;28:598–604.
Celik IH, Demirel G, Canpolat FE, Dilmen U. A common problem for neonatal intensive care units: late preterm infants, a prospective study with term controls in a large perinatal center. J Matern Fetal Neonatal Med. 2013;26(Mar):459–62.
Edwards EM, Horbar JD. Variation in Use by NICU Types in the United States. Pediatrics. 2018;142:e20180457.
Boyle EM, Johnson S, Manktelow B, Seaton SE, Draper ES, Smith LK, et al. Neonatal outcomes and delivery of care for infants born late preterm or moderately preterm: a prospective population-based study. Arch Dis Child Fetal Neonatal Ed. 2015;100:F479–85.
Edwards EM, Greenberg LT, Ehret DEY, Lorch SA, Horbar JD. Discharge Age and Weight for Very Preterm Infants: 2005-2018. Pediatrics 2021;147:e2020016006.
Kitsommart R, Janes M, Mahajan V, Rahman A, Seidlitz W, Wilson J, et al. Outcomes of late-preterm infants: a retrospective, single-center, Canadian study. Clin Pediatr. 2009;48:844–50.
Melamed N, Klinger G, Tenenbaum-Gavish K, Herscovici T, Linder N, Hod M, et al. Short-term neonatal outcome in low-risk, spontaneous, singleton, late preterm deliveries. Obstet Gynecol. 2009;114:253–60.
Moyer LB, Goyal NK, Meinzen-Derr J, Ward LP, Rust CL, Wexelblatt SL, et al. Factors associated with readmission in late-preterm infants: a matched case-control study. Hosp Pediatr. 2014;4:298–304.
Goyal N, Zubizarreta JR, Small DS, Lorch SA. Length of stay and readmission among late preterm infants: an instrumental variable approach. Hosp Pediatr. 2013;3:7–15.
Montenegro BL, Amberson M, Veit L, Freiberger C, Dukhovny D, Rhein LM. Economics of Home Monitoring for Apnea in Late Preterm Infants. Respir Care. 2017;62:42–8.
Joyce AH, Sengupta A, Garfield CF, Myers P. When is My Baby Going Home? Moderate to Late Preterm Infants are Discharged at 36 Weeks Based on Admission Data. Am J Perinatol. 2021;38:773–8.
Lau C. Development of infant oral feeding skills: what do we know?123. Am J Clin Nutr. 2016;103:616S–21S.
Simpson C, Schanler RJ, Lau C. Early Introduction of Oral Feeding in Preterm Infants. Pediatrics 2002;110:517–22.
Gyamfi-Bannerman C, Thom EA, Blackwell SC, Tita ATN, Reddy UM, Saade GR, et al. Antenatal Betamethasone for Women at Risk for Late Preterm Delivery. N. Engl J Med. 2016;374:1311–20.
Committee on Obstetric Practice. Committee Opinion No. 713: Antenatal Corticosteroid Therapy for Fetal Maturation. Obstet Gynecol. 2017;130:e102–9.
COMMITTEE ON FETUS AND NEWBORN, Papile LA, Baley JE, Benitz W, Cummings J, Eichenwald E, et al. Respiratory Support in Preterm Infants at Birth. Pediatrics. 2014;133:171–4.
Wheatley E, Kennedy KA. Cross-over trial of treatment for bradycardia attributed to gastroesophageal reflux in preterm infants. J Pediatr. 2009;155:516–21.
Slaughter JL, Stenger MR, Reagan PB, Jadcherla SR. Neonatal Histamine-2 Receptor Antagonist and Proton Pump Inhibitor Treatment at United States Children’s Hospitals. J Pediatrics. 2016;1:63–70.
Beck-Sague CM, Azimi P, Fonseca SN, Baltimore RS, Powell DA, Bland LA, et al. Bloodstream infections in neonatal intensive care unit patients: results of a multicenter study. Pediatr Infect Dis J. 1994;13:1110–6.
Maisels MJ, Watchko JF, Bhutani VK, Stevenson DK. An approach to the management of hyperbilirubinemia in the preterm infant less than 35 weeks of gestation. J Perinatol. 2012;32:660–4.
Palma JP, Arain YH. Development of a Web-Based Decision Support Tool to Operationalize and Optimize Management of Hyperbilirubinemia in Preterm Infants. Clin Perinatol. 2016;43:375–83.
Braun D, Edwards EM, Schulman J, Profit J, Pursley DM, Goodman DC. Choosing wisely for the other 80%: What we need to know about the more mature newborn and NICU care. Semin Perinatol. 2021;45:151395.
Acknowledgements
This research was supported in part by the Duke Pediatric Research Scholars Program, Department of Pediatrics, and Duke University School of Medicine.
Author information
Authors and Affiliations
Contributions
All authors were involved in the study design, analysis, and manuscript revision. All authors read and approved the final manuscript. CL contributed to the conception and design of the study, the data interpretation, the manuscript drafting, and the critical revision of the manuscript. KC contributed to the conception and design of the study, the data interpretation, and the critical revision of the manuscript. RHC contributed to the conception and design of the study, the data acquisition, the data interpretation, and the critical revision of the manuscript. RGG contributed to the conception and design of the study, the data analysis and interpretation, and the critical revision of the manuscript. SA had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. SA contributed to the conception and design of the study, the data analysis, the data interpretation, and the critical revision of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lockyear, C., Coe, K., Greenberg, R.G. et al. Trends in morbidities of late preterm infants in the neonatal intensive care unit. J Perinatol 43, 1379–1384 (2023). https://doi.org/10.1038/s41372-023-01705-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-023-01705-5