Abstract
Objective
Examine the risk of preterm birth (PTB, < 37 weeks) and early term birth (37–38 weeks) for women with reported drug abuse/dependence.
Study Design
The population was drawn from singleton livebirths in California from 2007 to 2012. Drug abuse/dependence was determined from maternal diagnostic codes (opioid, cocaine, cannabis, amphetamine, other, or polysubstance). Relative risks, adjusted for maternal factors were calculated for PTB and early term birth.
Result
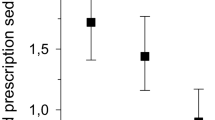
Of the 2,890,555 women in the sample, 1.7% (n = 48,133) had a diagnostic code for drug abuse/dependence. The percentage of PTBs varied from 11.6% (cannabis) to 24.3% (cocaine), compared with 6.7% of women without reported drug abuse/dependence.
Conclusion
Women with reported drug abuse/dependence during pregnancy were at increased risk of having a PTB and all but those using cannabis were at risk of having an early term birth. Women using cocaine and polysubstance were at the highest risk of birth < 32 weeks.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Romero R, Dey SK, Fisher SJ. Preterm labor: one syndrome, many causes. Science. 2014;345:760–5.
Goldenberg RL, Culhane JF, Iams JD, Romero R. Epidemiology and causes of preterm birth. Lancet. 2008;371:75–84.
Machado LC Jr., Passini R Jr., Rosa IR, Carvalho HB. Neonatal outcomes of late preterm and early term birth. Eur J Obstet Gynecol Reprod Biol. 2014;179:204–8.
Reddy UM, Bettegowda VR, Dias T, Yamada-Kushnir T, Ko CW, Willinger M. Term pregnancy: a period of heterogeneous risk for infant mortality. Obstet Gynecol. 2011;117:1279–87.
Bonello MR, Xu F, Li Z, Burns L, Austin MP, Sullivan EA. Mental and behavioral disorders due to substance abuse and perinatal outcomes: a study based on linked population data in New South Wales, Australia. Int J Environ Res Public Health. 2014;11:4991–5005.
Burns L, Mattick RP, Cooke M. The use of record linkage to examine illicit drug use in pregnancy. Addiction. 2006;101:873–82.
Feldman JG, Minkoff HL, McCalla S, Salwen M. A cohort study of the impact of perinatal drug use on prematurity in an inner-city population. Am J Public Health. 1992;82:726–8.
Gorman MC, Orme KS, Nguyen NT, Kent EJ 3rd, Caughey AB. Outcomes in pregnancies complicated by methamphetamine use. Am J Obstet Gynecol. 2014;211:429.e421–27.
Hayatbakhsh MR, Flenady VJ, Gibbons KS, Kingsbury AM, Hurrion E, Mamun AA, et al. Birth outcomes associated with cannabis use before and during pregnancy. Pediatr Res. 2012;71:215–9.
Ladhani NN, Shah PS, Murphy KE. Prenatal amphetamine exposure and birth outcomes: a systematic review and metaanalysis. Am J Obstet Gynecol. 2011;205:219.e211–7.
Brown HL, Graves CR. Smoking and marijuana use in pregnancy. Clin Obstet Gynecol. 2013;56:107–13.
Ganapathy V. Drugs of abuse and human placenta. Life Sci. 2011;88:926–30.
Ganapathy VV, Prasad PD, Ganapathy ME, Leibach FH. Drugs of abuse and placental transport. Adv Drug Deliv Rev. 1999;38:99–110.
Huizink AC. Prenatal cannabis exposure and infant outcomes: overview of studies. Prog Neuropsychopharmacol Biol Psychiatry. 2014;52:45–52.
Kuczkowski KM. The effects of drug abuse on pregnancy. Curr Opin Obstet Gynecol. 2007;19:578–85.
Woods JR Jr, Plessinger MA, Clark KE. Effect of cocaine on uterine blood flow and fetal oxygenation. JAMA. 1987;25:957–61.
Morgan MA, Silavin SL, Randolph M, Payne GG Jr, Sheldon RE, Fishburne JI Jr, et al. Effect of intravenous cocaine on uterine blood flow in the gravid baboon. Am J Obstet Gynecol. 1991;16:1021–7. ; discussion1027-30
Gillogley KM, Evans AT, Hansen RL, Samuels SJ, Batra KK. The perinatal impact of cocaine, amphetamine, and opiate use detected by universal intrapartum screening. Am J Obstet Gynecol. 1990;163(5 Pt 1):1535–42.
Cherukuri R, Minkoff H, Feldman J, Parekh A, Glass L. A cohort study of alkaloidal cocaine (“crack”) in pregnancy. Obstet Gynecol. 1988;72:147–51.
Dekker GA, Lee SY, North RA, McCowan LM, Simpson NA, Roberts CT. Risk factors for preterm birth in an international prospective cohort of nulliparous women. PLoS ONE. 2012;7:e39154.
Saurel-Cubizolles MJ, Prunet C, Blondel B. Cannabis use during pregnancy in France in 2010. BJOG. 2014;121:971–7.
Chouteau M, Namerow PB, Leppert P. The effect of cocaine abuse on birth weight and gestational age. Obstet Gynecol. 1988;72(3 Pt 1):351–4.
American Medical Association. International classification of diseases: ICD-9-CM 2008. Vol. 1, 2. Chicago, IL: American Medical Association; 2007.
Baer RJ, Norton ME, Shaw GM, Flessel MC, Goldman S, Currier RJ, et al. Risk of selected structural abnormalities in infants after increased nuchal translucency measurement. Am J Obstet Gynecol. 2014;211:675 e671–19.
Jelliffe-Pawlowski LL, Baer RJ, Blumenfeld YJ, Ryckman KK, O’Brodovich HM, Gould JB, et al. Maternal characteristics and mid-pregnancy serum biomarkers as risk factors for subtypes of preterm birth. BJOG. 2015;122:1484–93.
Administration SAaMHS. Results from the 2013 National Survey on Drug Use and Health: summary of national findings. Rockville, MD: Substance Abuse and Mental Health Services Administration; 2014.
McCarthy JJ, Leamon MH, Parr MS, Anania B. High-dose methadone maintenance in pregnancy: maternal and neonatal outcomes. Am J Obstet Gynecol. 2005;193(3 Pt 1):606–10.
Wouldes TA, Woodward LJ. Maternal methadone dose during pregnancy and infant clinical outcome. Neurotoxicol Teratol. 2010;32:406–13.
Almario CV, Seligman NS, Dysart KC, Berghella V, Baxter JK. Risk factors for preterm birth among opiate-addicted gravid women in a methadone treatment program. Am J Obstet Gynecol. 2009;201:326.e321–6.
Kotelchuck M. An evaluation of the Kessner adequacy of prenatal care index and a proposed adequacy of prenatal care utilization index. Am J Public Health. 1994;84:1414–20.
El-Mohandes A, Herman AA, Nabil El-Khorazaty M, Katta PS, White D, Grylack L. Prenatal care reduces the impact of illicit drug use on perinatal outcomes. J Perinatol. 2003;23:354–60.
Acknowledgements
This work was supported by the California Preterm Birth Initiative within the University of California, San Francisco.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Baer, R.J., Chambers, C.D., Ryckman, K.K. et al. Risk of preterm and early term birth by maternal drug use. J Perinatol 39, 286–294 (2019). https://doi.org/10.1038/s41372-018-0299-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-018-0299-0
This article is cited by
-
Reduced fetal cerebral blood flow predicts perinatal mortality in a mouse model of prenatal alcohol and cannabinoid exposure
BMC Pregnancy and Childbirth (2024)
-
Prenatal tobacco smoke exposure and risk for cognitive delays in infants born very premature
Scientific Reports (2024)
-
Environmental factors affecting pregnancy outcomes
Endocrine (2023)
-
The epidemiologic characteristics and associated risk factors of preterm birth from 2004 to 2013 in Taiwan
BMC Pregnancy and Childbirth (2020)