Abstract
Objective
NODAL has been implicated in timing of parturition and immune regulation. We investigated the relationship between NODAL polymorphisms, infection/inflammation, and preterm birth.
Study design
For this secondary analysis, 613 women (189 preterm and 424 term) from the Montreal Prematurity Study were genotyped for NODAL polymorphisms and assessed for bacterial vaginosis and placental inflammation.
Result
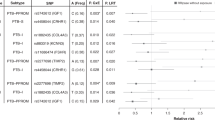
NODAL polymorphisms were not associated with preterm birth. However, the rs2231947(C>T) variant allele was associated with increased risk for preterm birth among women with bacterial vaginosis (odds ratio: 2.76, 95% confidence interval: 1.12−6.85). Among women without placental inflammation, the rs1904589(A>G) variant allele was associated with increased risk of preterm birth (odds ratio: 1.31, 95% confidence interval: 1.02−1.70). Among women with placental inflammation, the rs10999338(C>T) variant allele was associated with reduced risk of preterm birth (odds ratio: 0.50, 95% confidence interval: 0.29−0.87).
Conclusion
The effect of NODAL polymorphisms on preterm birth depends on maternal infection/inflammation status.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Change history
08 March 2022
A Correction to this paper has been published: https://doi.org/10.1038/s41372-021-01246-9
References
Blencowe H, Cousens S, Oestergaard MZ, Chou D, Moller A-B, Narwal R, et al. National, regional, and worldwide estimates of preterm birth rates in the year 2010 with time trends since 1990 for selected countries: a systematic analysis and implications. Lancet. 2012;379:2162–72.
Goldenberg RL, Culhane JF, Iams JD, Romero R. Epidemiology and causes of preterm birth. Lancet. 2008;371:75–84.
Moster D, Lie RT, Markestad T. Long-term medical and social consequences of preterm birth. N Engl J Med. 2008;359:262–73.
Goldenberg RL, Hauth JC, Andrews WW. Intrauterine infection and preterm delivery. N Engl J Med. 2000;342:1500–7.
Bastek JA, Gómez LM, Elovitz MA. The role of inflammation and infection in preterm birth. Clin Perinatol. 2011;38:385–406.
Young A, Thomson AJ, Ledingham M, Jordan F, Greer IA, Norman JE. Immunolocalization of proinflammatory cytokines in myometrium, cervix, and fetal membranes during human parturition at term. Biol Reprod. 2002;66:445–9.
Salafia CM, Vogel CA, Vintzileos AM, Bantham KF, Pezzullo J, Silberman L. Placental pathologic findings in preterm birth. Am J Obstet Gynecol. 1991;165:934–8.
Newton ER, Piper J, Peairs W. Bacterial vaginosis and intraamniotic infection. Am J Obstet Gynecol. 1997;176:672–7.
Kenyon C, Colebunders R, Crucitti T. The global epidemiology of bacterial vaginosis: a systematic review. Am J Obstet Gynecol. 2013;209:505–23.
Mitchell C, Marrazzo J. Bacterial vaginosis and the cervicovaginal immune response. Am J Reprod Immunol. 2014;71:555–63.
Lamont RF. Infection in the prediction and antibiotics in the prevention of spontaneous preterm labour and preterm birth. BJOG. 2003;110:71–75.
Goffinet F, Maillard F, Mihoubi N, Kayem G, Papiernik E, Cabrol D, et al. Bacterial vaginosis: prevalence and predictive value for premature delivery and neonatal infection in women with preterm labour and intact membranes. Eur J Obstet Gynecol Reprod Biol. 2003;108:146–51.
Wang Y, Yang X, Zheng Y, Wu Z-H, Zhang X-A, Li Q-P, et al. The SEPS1 G-105A polymorphism is associated with risk of spontaneous preterm birth in a Chinese population. PLoS ONE. 2013;8:e65657.
Roberts AK, Monzon-Bordonaba F, Van Deerlin PG, Holder J, Macones GA, Morgan MA, et al. Association of polymorphism within the promoter of the tumor necrosis factor α gene with increased risk of preterm premature rupture of the fetal membranes. Am J Obstet Gynecol. 1999;180:1297–302.
Macones GA, Parry S, Elkousy M, Clothier B, Ural SH, Strauss JF. A polymorphism in the promoter region of TNF and bacterial vaginosis: preliminary evidence of gene-environment interaction in the etiology of spontaneous preterm birth. Am J Obstet Gynecol. 2004;190:1504–8.
Iannaccone PM, Zhou X, Khokha M, Boucher D, Kuehn MR. Insertional mutation of a gene involved in growth regulation of the early mouse embryo. Dev Dyn. 1992;194:198–208.
Brennan J, Norris DP, Robertson EJ. Nodal activity in the node governs left-right asymmetry. Genes Dev. 2002;16:2339–44.
Park C, Dufort D. Nodal expression in the uterus of the mouse is regulated by the embryo and correlates with implantation. Biol Reprod. 2011;84:1103–10.
Thulluru HK, Park C, Dufort D, Kleiverda G, Oudejans C, van Dijk M. Maternal nodal inversely affects NODAL and STOX1 expression in the fetal placenta. Front Genet. 2013;4:170.
Park C, Dufort D. Elsevier trophoblast research award lecture: the multifaceted role of nodal signaling during mammalian reproduction. Placenta. 2011;32:S125–S129.
Park C, DeMayo FJ, Lydon J, Dufort D. NODAL in the uterus is necessary for proper placental development and maintenance of pregnancy. Biol Reprod. 2012;86:194.
Wang XF, Wang HS, Zhang F, Guo Q, Wang H, Wang KF, et al. Nodal promotes the generation of M2-like macrophages and downregulates the expression of IL-12. Eur J Immunol. 2014;44:173–83.
Zhang D, Bao YL, Yu CL, Wang Y, Song Z-B. Cripto-1 modulates macrophage cytokine secretion and phagocytic activity via NF-kB signaling. Immunol Res. 2016;64:104–14.
Kramer MS, Goulet L, Lydon J, Séguin L, McNamara H, Dassa C, et al. Socio-economic disparities in preterm birth: causal pathways and mechanisms. Paediatr Perinat Epidemiol. 2001;15 Suppl 2:104–23.
Kramer MS, Wilkins R, Goulet L, Séguin L, Lydon J, Kahn SR, et al. Investigating socio-economic disparities in preterm birth: evidence for selective study participation and selection bias. Paediatr Perinat Epidemiol. 2009;23:301–9.
Libman MD, Kramer MS, Platt RW. Comparison of Gram and Kopeloff stains in the diagnosis of bacterial vaginosis in pregnancy. Diagn Microbiol Infect Dis. 2006;54:197–201.
Nugent RP, Krohn MA, Hillier SL. Reliability of diagnosing bacterial vaginosis is improved by a standardized method of Gram stain interpretation. J Clin Microbiol. 1991;29:297–301.
Kramer MS, Chen MF, Roy I, Dassa C, Lamoureux J, Kahn SR, et al. Intra- and interobserver agreement and statistical clustering of placental histopathologic features relevant to preterm birth. Am J Obstet Gynecol. 2006;195:1674–9.
Luong ML, Libman M, Dahhou M, Chen MF, Kahn SR, Goulet L, et al. Vaginal douching, bacterial vaginosis, and spontaneous preterm birth. J Obstet Gynaecol Can. 2010;32:313–20.
Auton A, Abecasis GR, Altshuler DM, Durbin RM, Bentley DR, Chakravarti A, et al. A global reference for human genetic variation. Nature. 2015;526:68–74.
Peduzzi P, Concato J, Kemper E, Holford TR, Feinstem AR. A simulation study of the number of events per variable in logistic regression analysis. J Clin Epidemiol. 1996;49:1373–9.
Danecek P, Auton A, Abecasis GR, Albers CA, Banks E, DePristo MA, et al. The variant call format and VCFtools. Bioinformatics. 2011;27:2156–8.
Nadeau HCG, Subramaniam A, Andrews WW. Infection and preterm birth. Semin Fetal Neonatal Med. 2016;21:100–5.
Menon R, Dunlop AL, Kramer MR, Fortunato SJ, Hogue CJ. An overview of racial disparities in preterm birth rates: caused by infection or inflammatory response? Acta Obs Gynecol Scand. 2011;90:1325–31.
Stallmach T, Hebisch G, Joller H, Kolditz P, Engelmann M. Expression pattern of cytokines in the different compartments of the feto-maternal unit under various conditions. Reprod Fertil Dev. 1995;7:1573–80.
Imseis HM, Greig PC, Livengood CH, Shunior E, Durda P, Erikson M. Characterization of the inflammatory cytokines in the vagina during pregnancy and labor with bacterial vaginosis. J Soc Gynecol Investig. 1997;4:90–94.
Himes KP, Simhan HN. Genetic susceptibility to infection-mediated preterm birth. Infect Dis Clin NA. 2008;22:741–53.
Karody V, Le M, Nelson S, Meskin K, Klemm S, Simpson P, et al. A TIR domain receptor-associated protein (TIRAP) variant SNP (rs8177374) confers protection against premature birth. J Perinatol. 2013;33:341–6.
Simhan HN, Krohn MA, Roberts JM, Zeevi A, Caritis SN. Interleukin-6 promoter - 174 polymorphism and spontaneous preterm birth. Am J Obstet Gynecol. 2003;189:915–8.
Sheikh IA, Ahmad E, Jamal MS, Rehan M, Assidi M, Tayubi IA, et al. Spontaneous preterm birth and single nucleotide gene polymorphisms: a recent update. BMC Genomics. 2016;17:759.
Muglia LJ, Katz M. The enigma of spontaneous preterm birth. N Engl J Med. 2010;362:529–35.
Roessler E, Pei W, Ouspenskaia M, Karkera JD, Veléz JI, Banerjee-Basu S, et al. Cumulative ligand activity of NODAL mutations and modifiers are linked to human heart defects and holoprosencephaly. Mol Genet Metab. 2009;98:225–34.
Adachi H, Saijoh Y, Mochida K, Ohishi S, Hashiguchi H, Hirao A, et al. Determination of left/right asymmetric expression of nodal by a left side-specific enhancer with sequence similarity to a lefty-2 enhancer. Genes Dev. 1999;13:1589–1600.
Frey HA, Stout MJ, Pearson LN, Tuuli MG, Cahill AG, Strauss JF, et al. Genetic variation associated with preterm birth in African-American women. Am J Obstet Gynecol. 2016;215:235.e1–235.e8.
Findlay SD, Postovit LM. Brief report: common genetic variation in chromosome 10q22.1 shows a strong sex bias in human embryonic stem cell lines and directly controls the novel alternative splicing of human NODAL which is associated with XIST expression in female cell lines. Stem Cells. 2016;34:791–6.
Simmons LE, Rubens CE, Darmstadt GL, Gravett MG. Preventing preterm birth and neonatal mortality: exploring the epidemiology, causes, and interventions. Semin Perinatol. 2010;34:408–15.
Acknowledgements
We thank Michael Kramer, Mourad Dahhou, and the members of the Montreal Prematurity Study Group. We also thank the McGill University and Genome Quebec Innovation Centre (Montreal, Canada) for performing SNP discovery and Sanger sequencing. We thank all of the women for their generous participation in this study.
Funding
This study was funded by March of Dimes Grant No. 21-FY14-130. LMS was supported by a Toronto Dominion Bank Post-Doctoral Fellowship for Child Health Research Excellence. TH was supported by the Ministry of Higher Education of Saudi Arabia. Support for the Montreal Prematurity Study was provided by the Perinatal Epidemiological Research Iniviative Program Grant No 20-FY04-38 from the March of Dimes Birth Defects Foundation. The funders had no role in study design, data collection and analysis, interpretation of data, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Starr, L.M., Ayash, T.A. & Dufort, D. Evidence of a gene–environment interaction of NODAL variants and inflammation in preterm birth. J Perinatol 38, 482–488 (2018). https://doi.org/10.1038/s41372-018-0073-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-018-0073-3