Abstract
Background
Obesity is a chronic disease associated with adverse outcomes and its prevalence is increasing, which makes it a concern. One of the obesity treatment options is bariatric surgery, which effectively reduces calorie absorption and total body mass, but its effects on physical activity (PA) levels need to be clarified, considering the protective effect of the PA against cardiovascular disease, independently of the weight loss alone.
Objectives
To carry out a systematic review and meta-analysis of observational studies that evaluated PA in pre- and post-bariatric surgery periods through objective evaluation.
Methods
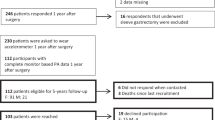
A systematic search was carried out following the PRISMA criteria of studies with adult individuals who underwent bariatric surgery and were objectively evaluated for PA pre- and post-surgery. Studies with interventions were excluded.
Results
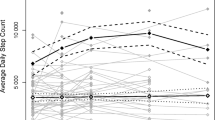
A total of 419 records were found, and after excluding duplicates and applying the eligibility criteria, 10 studies remained. This meta-analysis found a significant increase in the steps by day (MD = 1340; 95% CI = 933.90; 1745.35, p < 0.001) and the light physical activity level (MD = 16.8 min/day; 95% CI = 2.60; 30.98, p = 0.02), but not in moderate to vigorous physical activity (MD = 0.24; 95% CI = −0.08; 1.57, p = 0.92).
Conclusions
Patients undergoing bariatric surgery increased their steps by day and light physical activity but did not increase moderate to vigorous physical activity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Schauer PR, Bhatt DL, Kirwan JP, Wolski K, Aminian A, Brethauer SA. et al. Bariatric surgery versus intensive medical therapy for diabetes – 5-year outcomes. N Engl J Med. 2017;376:641–51.
Sjöström L. Review of the key results from the Swedish Obese Subjects (SOS) trial – a prospective controlled intervention study of bariatric surgery. J Intern Med. 2013;273:219–34.
Ciobârcă DM, Florinela Cătoi A, Copăescu C, Miere D, Crișan G. Nutritional status prior to bariatric surgery for severe obesity: a review. Med Pharm Rep. 2022;95:24–30.
Welbourn R, Hollyman M, Kinsman R, Dixon J, Liem R, Ottosson J. et al. Bariatric surgery worldwide: baseline demographic description and one-year outcomes from the Fourth IFSO Global Registry Report 2018. Obes Surg. 2019;29:782–95.
Kochkodan J, Telem DA, Ghaferi AA. Physiologic and psychological gender differences in bariatric surgery. Surg Endosc. 2018;32:1382–8. https://doi.org/10.1007/s00464-017-5819-z.
Obesity and overweight. https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight. Accessed 20 Oct 2022.
World Obesity Day 2022 – Accelerating action to stop obesity. https://www.who.int/news/item/04-03-2022-world-obesity-day-2022-accelerating-action-to-stop-obesity. Accessed 13 Apr 2023.
Bariatric Surgery Procedures | ASMBS. https://asmbs.org/patients/bariatric-surgery-procedures. Accessed 24 Oct 2022.
Josbeno DA, Jakicic JM, Hergenroeder A, Eid GM. Physical activity and physical function changes in obese individuals after gastric bypass surgery. Surg Obes Relat Dis. 2010;6:361–6.
Kissler HJ, Settmacher U. Bariatric surgery to treat obesity. Semin Nephrol. 2013;33:75–89.
Koshy AA, Bobe AM, Brady MJ. Potential mechanisms by which bariatric surgery improves systemic metabolism. Transl Res. 2013;161:63–72.
Di Lorenzo N, Antoniou SA, Batterham RL, Busetto L, Godoroja D, Iossa A. et al. Clinical practice guidelines of the European Association for Endoscopic Surgery (EAES) on bariatric surgery: update 2020 endorsed by IFSO-EC, EASO and ESPCOP. Surg Endosc. 2020;34:2332–58.
Almeida SS, Zanatta DP, Rezende FF. Imagem corporal, ansiedade e depressão em pacientes obesos submetidos à cirurgia bariátrica. Estudos Psicologia (Natal). 2012;17:153–60.
Langaro F, Vieira APK, Poggere LC, Trentini CM. Características de personalidade de mulheres que se submeteram à cirurgia bariátrica. Avaliação Psicológica. 2011;10:71–9
Tae B, Pelaggi ER, Moreira JG, Waisberg J, De Matos LL, D’Elia G. O impacto da cirurgia bariátrica nos sintomas depressivos e ansiosos, comportamento bulímico e na qualidade de vida. Rev Col Bras Cir. 2014;41:155–60
Fiorani C, Coles SR, Kulendran M, McGlone ER, Reddy M, Khan OA. Long-term quality of life outcomes after laparoscopic sleeve gastrectomy and Roux-en-Y gastric bypass – a comparative study. Obes Surg. 2021;31:1376–80.
Arterburn DE, Telem DA, Kushner RF, Courcoulas AP. Benefits and risks of bariatric surgery in adults: a review. JAMA. 2020;324:879–87.
Diretrizes – Abeso. https://abeso.org.br/diretrizes/. Accessed 13 Apr 2023.
O’Brien PE, McPhail T, Chaston TB, Dixon JB. Systematic review of medium-term weight loss after bariatric operations. Obes Surg. 2006;16:1032–40.
Jassil FC, Carnemolla A, Kingett H, Paton B, O’Keeffe AG, Doyle J, et al. Protocol for a 1-year prospective, longitudinal cohort study of patients undergoing Roux-en-Y gastric bypass and sleeve gastrectomy: the BARI-LIFESTYLE observational study. BMJ Open. 2018;8e020659.
Jacobi D, Ciangura C, Couet C, Oppert JM. Physical activity and weight loss following bariatric surgery. Obes Rev. 2011;12:366–77.
Coen PM, Carnero EA, Goodpaster BH. Exercise and bariatric surgery: an effective therapeutic strategy. Exerc Sport Sci Rev. 2018;46:262–70.
Egberts K, Brown WA, Brennan L, O’Brien PE. Does exercise improve weight loss after bariatric surgery? A systematic review. Obes Surg. 2012;22:355–41.
Lavie CJ, Ozemek C, Carbone S, Katzmarzyk PT, Blair SN. Sedentary behavior, exercise, and cardiovascular health. Circ Res. 2019;124:799–815. https://doi.org/10.1161/CIRCRESAHA.118.312669.
Elagizi A, Kachur S, Carbone S, Lavie CJ, Blair SN. A review of obesity, physical activity, and cardiovascular disease. Curr Obes Rep. 2020;9:571–81.
King WC, Hsu JY, Belle SH, Courcoulas AP, Eid GM, Flum DR, et al. Pre- to postoperative changes in physical activity: report from the Longitudinal Assessment of Bariatric Surgery-2 (LABS-2). Surg Obes Relat Dis. 2012;8:522–32. https://doi.org/10.1016/j.soard.2011.07.018.
King WC, Chen JY, Bond DS, Belle SH, Courcoulas AP, Patterson EJ, et al. Objective assessment of changes in physical activity and sedentary behavior: pre- through 3 years post-bariatric surgery. Obesity. 2015;23:1143–50.
Sellberg F, Possmark S, Willmer M, Tynelius P, Persson M, Berglind D. Meeting physical activity recommendations is associated with health-related quality of life in women before and after Roux-en-Y gastric bypass surgery. Qual Life Res. 2019;28:1497–507.
Nielsen MS, Alsaoodi H, Hjorth MF, Sjödin A. Correction to: Physical activity, sedentary behavior, and sleep before and after bariatric surgery and associations with weight loss outcome. Obes Surg. 2021;31:909
Afshar S, Seymour K, Kelly SB, Woodcock S, van Hees VT, Mathers JC. Changes in physical activity after bariatric surgery: using objective and self-reported measures. Surg Obes Relat Dis. 2017;13:474–83. https://doi.org/10.1016/j.soard.2016.09.012.
Berglind D, Willmer M, Tynelius P, Ghaderi A, Näslund E, Rasmussen F. Accelerometer-measured versus self-reported physical activity levels and sedentary behavior in women before and 9 months after Roux-en-Y gastric bypass. Obes Surg. 2016;26:1463–70.
Bond DS, Jakicic JM, Unick JL, Vithiananthan S, Pohl D, Roye GD. et al. Pre- to postoperative physical activity changes in bariatric surgery patients: self report vs. objective measures. Obesity (Silver Spring). 2010;18:2395–7.
Creel DB, Schuh LM, Reed CA, Gomez AR, Hurst LA, Stote J. et al. A randomized trial comparing two interventions to increase physical activity among patients undergoing bariatric surgery. Obesity (Silver Spring). 2016;24:1660–8.
Marquez DX, Aguiñaga S, Vásquez PM, Conroy DE, Erickson KI, Hillman C, et al. A systematic review of physical activity and quality of life and well-being. Transl Behav Med. 2020;10:1098–109. https://doi.org/10.1093/tbm/ibz198.
van Poppel MN, Chinapaw MJ, Mokkink LB, van Mechelen W, Terwee CB. Physical activity questionnaires for adults: a systematic review of measurement properties. Sports Med. 2010;40:565–600. https://doi.org/10.2165/11531930-000000000-00000.
Page MJ, Moher D, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. PRISMA 2020 explanation and elaboration: updated guidance and exemplars for reporting systematic reviews. BMJ. 2021;372:n160.
Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A. Rayyan—a web and mobile app for systematic reviews. Syst Rev. 2016;5:210.
The Newcastle-Ottawa Scale (NOS) for Assessing the Quality if Nonrandomized Studies in Meta-Analyses – ScienceOpen. https://www.scienceopen.com/document?vid=54b48470-4655-4081-b5d4-e8ebe8d1792e. Accessed 13 Apr 2023.
Koshy L, Jeemon P, Ganapathi S, Madhavan M, Urulangodi M, Sharma M, et al. Association of South Asian-specific MYBPC3Δ25bp deletion polymorphism and cardiomyopathy: a systematic review and meta-analysis. Meta Gene. 2021;28:100883.
Boone DA, Coleman KL. Use of a step activity monitor in determining outcomes. J Prosthet Orthot. 2006;18:P86–92.
Ibacache P, Cano-Cappellacci M, Miranda-Fuentes C, Rojas J, Maldonado P, Bottinelli A. Physical fitness and physical activity in women with obesity: short term effects of sleeve gastrectomy. Nutr Hosp. 2019;36:840–5.
Spadaccini D, Guazzotti S, Goncalves Correia FP, Daffara T, Tini S, Antonioli A, et al. Beyond bariatric surgery and weight loss medicaments. A systematic review of the current practice in obesity rehabilitative inpatient programs in adults and pediatrics. Front Nutr. 2022;9:963709.
Flegal KM, Kruszon-Moran D, Carroll MD, Fryar CD, Ogden CL. Trends in obesity among adults in the United States, 2005 to 2014. JAMA. 2016;315:2284–91.
Chooi YC, Ding C, Magkos F. The epidemiology of obesity. Metabolism. 2019;92:6–10. https://doi.org/10.1016/j.metabol.2018.09.005.
Levorato CD, de Mello LM, da Silva AS, Nunes AA. Fatores associados à procura por serviços de saúde numa perspectiva relacional de gênero. Cien Saude Colet. 2014;19:1263–74.
Herring LY, Stevinson C, Davies MJ, Biddle SJ, Sutton C, Bowrey D. et al. Changes in physical activity behaviour and physical function after bariatric surgery: a systematic review and meta-analysis. Obes Rev. 2016;17:250–61.
Miller GD, Nicklas BJ, You T, Fernandez A. Physical function improvements after laparoscopic Roux-en-Y gastric bypass surgery. Surg Obes Relat Dis. 2009;5:530–7.
Donnelly JE, Blair SN, Jakicic JM, Manore MM, Rankin JW, Smith BK. American College of Sports Medicine Position Stand. Appropriate physical activity intervention strategies for weight loss and prevention of weight regain for adults. Med Sci Sports Exerc. 2009;41:459–71.
Jabbour G, Ibrahim R, Bragazzi N. Preoperative physical activity level and exercise prescription in adults with obesity: the effect on post-bariatric surgery outcomes. Front Physiol. 2022;13:869998.
Goodpaster BH, DeLany JP, Otto AD, Kuller L, Vockley J, South-Paul JE. et al. Effects of diet and physical activity interventions on weight loss and cardiometabolic risk factors in severely obese adults: a randomized trial. JAMA. 2010;304:1795–802.
Mechanick JI, Apovian C, Brethauer S, Garvey WT, Joffe AM, Kim J, et al. Clinical practice guidelines for the perioperative nutrition, metabolic, and nonsurgical support of patients undergoing bariatric procedures − 2019 update: cosponsored by American Association of Clinical Endocrinologists/American College of Endocrinology, The Obesity Society, American Society for Metabolic & Bariatric Surgery, Obesity Medicine Association, and American Society of Anesthesiologists. Surg Obes Relat Dis. 2020;16:175–247.
Svensson PA, Anveden Å, Romeo S, Peltonen M, Ahlin S, Burza MA. et al. Alcohol consumption and alcohol problems after bariatric surgery in the Swedish obese subjects study. Obesity (Silver Spring). 2013;21:2444–51.
King WC, Chen JY, Mitchell JE, Kalarchian MA, Steffen KJ, Engel SG, et al. Prevalence of alcohol use disorders before and after bariatric surgery. JAMA. 2012;307:2516.
Alyahya RA, Alnujaidi MA. Prevalence and outcomes of depression after bariatric surgery: a systematic review and meta-analysis. Cureus. 2022;14e25651.
Molero J, Olbeyra R, Flores L, Jiménez A, de Hollanda A, Andreu A. et al. Prevalence of low skeletal muscle mass following bariatric surgery. Clin Nutr ESPEN. 2022;49:436–41.
Maggisano M, Maeda A, Okrainec A, Wnuk S, Sockalingam S, Jackson TD. Physical activity and its association with psychosocial health following bariatric surgery. Appl Physiol Nutr Metab. 2019;44:1379–82.
Bellicha A, Ciangura C, Poitou C, Portero P, Oppert JM. Effectiveness of exercise training after bariatric surgery – a systematic literature review and meta-analysis. Obes Rev. 2018;19:1544–56.
Paluch AE, Bajpai S, Bassett DR, Carnethon MR, Ekelund U, Evenson KR, et al. Steps for Health Collaborative. Daily steps and all-cause mortality: a meta-analysis of 15 international cohorts. Lancet Public Health. 2022;7:e219–28. https://doi.org/10.1016/S2468-2667(21)00302-9.
Bull FC, Al-Ansari SS, Biddle S, Borodulin K, Buman MP, Cardon G, et al. World Health Organization 2020 guidelines on physical activity and sedentary behaviour. Br J Sports Med. 2020;54:1451–62. https://doi.org/10.1136/bjsports-2020-102955.
Reinmann A, Gafner SC, Hilfiker R, Bruyneel AV, Pataky Z, Allet L. Bariatric surgery: consequences on functional capacities in patients with obesity. Front Endocrinol (Lausanne). 2021;12:646283. https://doi.org/10.3389/fendo.2021.646283.
Sundgot-Borgen C, Bond DS, Sniehotta FF, Kvalem IL, Hansen BH, Bergh I, et al. Associations of changes in physical activity and sedentary time with weight recurrence after bariatric surgery: a 5-year prospective study. Int J Obes. 2023;47:463–70. https://doi.org/10.1038/s41366-023-01284-7.
Author information
Authors and Affiliations
Contributions
MB and CG were the authors responsible for the conceptualization, methodology, search and selection, data extraction and writing of the original draft. BPdA performed the writing and review. TGC performed a written review and meta-analysis. MPdS was the research coordinator and performed the meta-analysis, conceptualization, writing and review of the original draft preparation.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bastos, M., Gonsalves, C., de Almeida, B.P. et al. Do patients with obesity undergoing bariatric surgery modify their objectively measured physical activity? A systematic review and meta-analysis. Int J Obes 48, 315–323 (2024). https://doi.org/10.1038/s41366-023-01452-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-023-01452-9