Abstract
Background/objectives
We hypothesized that physical activity (PA) improves insulin sensitivity in adolescents with severe obesity beyond that attributable to metabolic bariatric surgery (MBS).
Subjects/methods
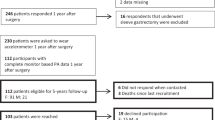
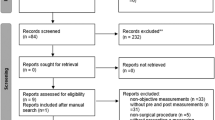
StepWatchTM monitors objectively measured PA in 88 participants in the Teen Longitudinal Assessment of Bariatric Surgery (Teen-LABS) study. Primary outcomes included absolute change in fasting insulin, HOMA-IR, and fasting glucose from pre-surgery (baseline) to 6, 12, 24, and 36 months post-MBS. SAS PROC TRAJ generated activity trajectories based on probability and individual participant step count trajectories. Linear regression models were used, adjusted for baseline value, visit, surgical procedure, sex, and percent change in BMI. Additional models adjusted for percent change in iliac waist circumference (IWC) or percent body fat (BF), measured by bio-impedance.
Results
Two activity trajectories were identified: more active (MA, n = 13) and less active (LA, n = 75). MA baseline mean daily step count was >6000, increasing to >9000 at 2 years. LA mean daily step count remained at ~4000. Few participants recorded moderate step activity (cadence >80 steps/minute). Still, fasting insulin and HOMA-IR differed in association with activity trajectoy. MA was associated with a greater absolute decrease in fasting insulin (−7.8 μU/ml [95% CI: (−11.8, −3.7)], p ≤ 0.001) and a greater decrease in HOMA-IR (−1.9 [95% CI: (−3.0, −0.7)], p = 0.001), when adjusted for percent change in BMI. The significant independent effect of MA remained when adjusted for percent change in IWC or percent BF. Clinically, 100% of MA trajectory participants normalized fasting insulin, HOMA-IR, and fasting glucose by 6 months and normalization remained throughout the 36 months follow up. In contrast, 76.3 and 65.8% of LA trajectory participants normalized fasting insulin and HOMA-IR, respectively, by 12 months with 28.6% of both remaining normalized at 36 months.
Conclusions
PA is independently associated with improved insulin sensitivity beyond that attributable to MBS in adolescents with severe obesity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Pinhas-Hamiel O, Dolan LM, Daniels SR, Standiford D, Khoury PR, Zeitler P. Increased incidence of non-insulin-dependent diabetes mellitus among adolescents. J Pediatr. 1996;128:608–15.
Burns SF, Bacha F, Lee SJ, Tfayli H, Gungor N, Arslanian SA. Declining beta-cell function relative to insulin sensitivity with escalating OGTT 2-h glucose concentrations in the nondiabetic through the diabetic range in overweight youth. Diabetes Care. 2011;34:2033–40.
Pareek M, Schauer PR, Kaplan LM, Leiter LA, Rubino F, Bhatt DL. Metabolic surgery: weight loss, diabetes, and beyond. J Am Coll Cardiol. 2018;71:670–87.
Michalsky MP, Inge TH, Jenkins TM, Xie C, Courcoulas A, Helmrath M. et al. Cardiovascular risk factors after adolescent bariatric surgery. Pediatrics. 2018;141:e20172485.
Eckardt K, Taube A, Eckel J. Obesity-associated insulin resistance in skeletal muscle: role of lipid accumulation and physical inactivity. Rev Endocr Metab Disord. 2011;12:163–72.
Nadeau KJ, Zeitler PS, Bauer TA, Brown MS, Dorosz JL, Draznin B, et al. Insulin resistance in adolescents with type 2 diabetes is associated with impaired exercise capacity. J Clin Endocrinol Metab. 2009;94:3687–95.
Berglind D, Willmer M, Tynelius P, Ghaderi A, Naslund E, Rasmussen F. Women undergoing Roux-en-Y gastric bypass surgery: family resemblance in pre- to postsurgery physical activity and sedentary behavior in children and spouses. Surg Obes Relat Dis. 2015;11:690–6.
Lent MR, Bailey-Davis L, Irving BA, Wood GC, Cook AM, Hirsch AG, et al. Bariatric surgery patients and their families: health, physical activity, and social support. Obes Surg. 2016;26:2981–8.
Inge TH, Zeller M, Harmon C, Helmrath M, Bean J, Modi A, et al. Teen-longitudinal assessment of bariatric surgery: methodological features of the first prospective multicenter study of adolescent bariatric surgery. J Pediatr Surg. 2007;42:1969–71.
Price PH, Kaizer AM, Daniels SR, Jenkins TM, Inge TH, Eckel RH. Physical activity improves lipid and weight-loss outcomes after metabolic bariatric surgery in adolescents with severe obesity. Obesity. 2019;27:989–96.
Andruff H, Carraro N, Thompson A, Gaudreau P, Louvet B. Latent class growth modelling: a tutorial. tutorials in quantitative methods for psychology. 2009;5:11–24.
R: a language and environment for statistical computing. Vienna, Austria: R Foundation for Statistical Computing; 2018. https://www.R-project.org/.
Services UDoHaH. Physical activity guidelines for Americans. 2nd ed. Washington, DC: US Department of Health and Human Services; 2018.
Tudor-Locke C, Craig CL, Beets MW, Belton S, Cardon GM, Duncan S. et al. How many steps/day are enough? For children and adolescents. Int J Behav Nutr Phys Act. 2011;8:78–91.
Tudor-Locke C, Craig CL, Brown WJ, Clemes SA, De Cocker K, Giles-Corti B, et al. How many steps/day are enough? For adults. Int J Behav Nutr Phys Act. 2011;8:79.
Xanthakos SA, Jenkins TM, Kleiner DE, Boyce TW, Mourya R, Karns R, et al. High prevalence of nonalcoholic fatty liver disease in adolescents undergoing bariatric surgery. Gastroenterology. 2015;149:623–34.
Algooneh A, Almazeedi S, Al-Sabah S, Ahmed M, Othman F. Non-alcoholic fatty liver disease resolution following sleeve gastrectomy. Surg Endosc. 2016;30:1983–7.
da Cruz MRR, Branco-Filho AJ, Zaparolli MR, Wagner NF, de Paula Pinto JS, Campos ACL, et al. Predictors of success in bariatric surgery: the role of bmi and pre-operative comorbidities. Obes Surg. 2018;28:1335–41.
Inge TH, Courcoulas AP, Jenkins TM, Michalsky MP, Helmrath MA, Brandt ML, et al. Weight loss and health status 3 years after bariatric surgery in adolescents. N Engl J Med. 2016;374:113–23.
Schenk S, Saberi M, Olefsky JM. Insulin sensitivity: modulation by nutrients and inflammation. J Clin Investig. 2008;118:2992–3002.
D’Adamo E, Caprio S. Type 2 diabetes in youth: epidemiology and pathophysiology. Diabetes Care. 2011;34 (Suppl 2):S161–5.
Hannon TS, Rao G, Arslanian SA. Childhood obesity and type 2 diabetes mellitus. Pediatrics. 2005;116:473–80.
Mayer-Davis EJ, Lawrence JM, Dabelea D, Divers J, Isom S, Dolan L, et al. Incidence trends of type 1 and type 2 diabetes among youths, 2002-2012. N Engl J Med. 2017;376:1419–29.
Caprio S, Perry R, Kursawe R. Adolescent obesity and insulin resistance: roles of ectopic fat accumulation and adipose inflammation. Gastroenterology. 2017;152:1638–46.
Smith JD, Mills E, Carlisle SE. Treatment of pediatric type 2 diabetes. Ann Pharmacother. 2016;50:768–77.
Hannon TS, Arslanian SA. The changing face of diabetes in youth: lessons learned from studies of type 2 diabetes. Ann N Y Acad Sci. 2015;13531:113–37.
Berman LJ, Weigensberg MJ, Spruijt-Metz D. Physical activity is related to insulin sensitivity in children and adolescents, independent of adiposity: a review of the literature. Diabetes Metab Res Rev. 2012;28:395–408.
Takahashi H, Kotani K, Tanaka K, Egucih Y, Anzai K. Therapeutic approaches to nonalcoholic fatty liver disease: exercise intervention and related mechanisms. Front Endocrinol. 2018;9:588.
Bordenave S, Brandou F, Manetta J, Fédou C, Mercier J, Brun JF. Effects of acute exercise on insulin sensitivity, glucose effectiveness and disposition index in type 2 diabetic patients. Diabetes Metab. 2008;34:250–7.
Aadland E, Robertson L. Physical activity is associated with weight loss and increased cardiorespiratory fitness in severely obese men and women undergoing lifestyle treatment. J Obes. 2012;2012:810594.
Look ARG. Eight-year weight losses with an intensive lifestyle intervention: the look AHEAD study. Obesity. 2014;22:5–13.
Pownall HJ, Bray GA, Wagenknecht LE, Walkup MP, Heshka S, Hubbard VS, et al. Changes in body composition over 8 years in a randomized trial of a lifestyle intervention: the look AHEAD study. Obesity. 2015;23:565–72.
Herman KM, Carver TE, Christou NV, Andersen RE. Keeping the weight off: physical activity, sitting time, and weight loss maintenance in bariatric surgery patients 2 to 16 years postsurgery. Obes Surg. 2014;24:1064–72.
Fernandes RA, Vaz Ronque ER, Venturini D, Barbosa DS, Silva DP, Cogo CT, et al. Resting heart rate: its correlations and potential for screening metabolic dysfunctions in adolescents. BMC Pediatr. 2013;13:48.
Onofre T, Carlos R, Oliver N, Felismino A, Fialho D, Corte R, et al. Effects of a physical activity program on cardiorespiratory fitness and pulmonary function in obese women after bariatric surgery: a pilot study. Obes Surg. 2017;27:2026–33.
Funding
The Teen-LABS consortium is funded by cooperative agreements with the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), through grants UM1DK072493 (PI, Dr Thomas Inge, University of Colorado, Denver, CO), and UM1DK095710 (PI, Dr Changchun Xie, University of Cincinnati). Dr Paula Holland Price was supported by the National Heart, Lung and Blood Institute (NHLBI): 5T32HL116276-05.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Price, P.H., Kaizer, A.M., Inge, T.H. et al. Physical activity impacts insulin sensitivity post metabolic bariatric surgery in adolescents with severe obesity. Int J Obes 44, 1479–1486 (2020). https://doi.org/10.1038/s41366-020-0585-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-020-0585-8