Abstract
Objective
To examine changes in prevalence of overeating behaviors in a comparative effectiveness study of two pediatric weight management interventions.
Methods
Four-hundred and seven children, ages 6–12 years, with a BMI ≥ 85th percentile were enrolled in a comparative effectiveness trial of two pediatric weight management interventions. Prevalence of “sneaking, hiding or hoarding food”, and ‘eating in the absence of hunger’ was evaluated at baseline and 12 months. Statistical methods included McNemar’s test and longitudinal logistic regression.
Results
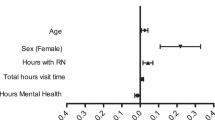
Prevalence of “sneak, hide, or hoard food” significantly decreased in all participants from 29.1% to 20.7% at 12 months. The prevalence of “eating in the absence of hunger” decreased in all participants from 46.7% to 22.4% at 12 months. Use of SNAP benefits, free/reduced meals at school, parental stress, housing, and food insecurity at baseline were associated with an increased likelihood of endorsing overeating behaviors at 12 months. Conversely, those who engaged in at least one session of the pediatric weight management intervention were significantly less likely to endorse “eating in the absence of hunger” at 12 months.
Conclusions
Participation in pediatric weight management interventions improves the prevalence of overeating behaviors and is associated with participant engagement and social determinants of health, specifically food security status. Efforts to engage populations impacted by food insecurity and other social determinants of health risk factors will be critical for success of weight management interventions.
Clinical trial registration
This trial has been registered at ClinicalTrials.gov (identifier: NCT03012126).
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
US Preventive Services Task F, Grossman DC, Bibbins-Domingo K, Curry SJ, Barry MJ, Davidson KW, et al. Screening for obesity in children and adolescents. JAMA. 2017;317:2417–26. https://doi.org/10.1001/jama.2017.6803
US Preventive Services Task Force. Screening for obesity in children and adolescents: recommendation statement. JAMA. 2017;317:2417–26. https://doi.org/10.1001/jama.2017.6803
Kumar S, Kelly AS. Review of childhood obesity: from epidemiology, etiology, and comorbidities to clinical assessment and treatment. Mayo Clin Proc. 2017;92:251–65. https://doi.org/10.1016/j.mayocp.2016.09.017
Skelton JA, Palakshappa D, Moore JB, Irby MB, Montez K, Rhodes SD. Community engagement and pediatric obesity: Incorporating social determinants of health into treatment. J Clin Transl Sci. 2019;4:279–85. https://doi.org/10.1017/cts.2019.447
Graham H, White PCL. Social determinants and lifestyles: integrating environmental and public health perspectives. Public Health. 2016;141:270–8. https://doi.org/10.1016/j.puhe.2016.09.019
Hanson KL, Connor LM. Food insecurity and dietary quality in US adults and children: a systematic review. Am J Clin Nutr. 2014;100:684–92. https://doi.org/10.3945/ajcn.114.084525
Leung CW, Epel ES, Ritchie LD, Crawford PB, Laraia BA. Food insecurity is inversely associated with diet quality of lower-income adults. J Acad Nutr Diet. 2014;114:1943–e2. https://doi.org/10.1016/j.jand.2014.06.353
Bruening M, MacLehose R, Loth K, Story M, Neumark-Sztainer D. Feeding a family in a recession: food insecurity among Minnesota parents. Am J Public Health. 2012;102:520–6. https://doi.org/10.2105/AJPH.2011.300390
Seligman HK, Berkowitz SA. Aligning programs and policies to support food security and public health goals in the United States. Annu Rev Public Health. 2019;40:319–37. https://doi.org/10.1146/annurev-publhealth-040218-4132
Tester JM, Lang TC, Laraia BA. Disordered eating behaviors and food insecurity: a qualitative study about children with obesity in low-income households. Obes Res Clin Pract. 2016;10:544–52. https://doi.org/10.1016/j.orcp.2015.11.007
Hooper L, Telke S, Larson N, Mason SM, Neumark-Sztainer D. Household food insecurity: associations with disordered eating behaviours and overweight in a population-based sample of adolescents. Public Health Nutr. 2020;23:3126–35. https://doi.org/10.1017/S1368980020000464
Fiechtner L, Perkins M, Biggs V, Langhans N, Sharifi M, O'connor G, et al. Rationale and design of the clinic and community approaches to healthy weight randomized trial. Contemp Clin Trials. 2018;67:16–22. https://doi.org/10.1016/j.cct.2018.01.002
Giuse NB, Koonce TY, Kusnoor SV, Prather AA, Gottlieb LM, Huang LC, et al. Institute of medicine measures of social and behavioral determinants of health: a feasibility study. Am J Prev Med. 2017;52:199–206. https://doi.org/10.1016/j.amepre.2016.07.033
Elo AL, Leppänen A, Jahkola A. Validity of a single-item measure of stress symptoms. Scand J Work Environ Health. 2003;29:444–51. https://doi.org/10.5271/sjweh.752
Atkins M, Castro I, Sharifi M, Perkins M, O'connor G, Sandel M, et al. Unmet social needs and adherence to pediatric weight management interventions: Massachusetts, 2017–-9. Am J Public Health. 2020;110:S251–S257. https://doi.org/10.2105/AJPH.2020.305772
Urban Institute and Child Trends. National Survey of America’s Familities (NASF); 2002
Hager ER, Quigg AM, Black MM, Coleman SM, Heeren T, Rose-Jacobs R, et al. Development and validity of a 2-item screen to identify families at risk for food insecurity. Pediatrics. 2010;126:e26–e32
Nobles JD, Perez A, Skelton JA, Spence ND, Ball GD. The engagement pathway: a conceptual framework of engagement-related terms in weight management. Obes Res Clin Pract. 2018;12:133–8. https://doi.org/10.1016/j.orcp.2017.12.005
Khanal S, Choi L, Innes-Hughes C, Rissel C. Dose response relationship between program attendance and children’s outcomes in a community based weight management program for children and their families. BMC Public Health. 2019;19:716 https://doi.org/10.1186/s12889-019-7094-5
Sonneville KR, Horton NJ, Micali N, Crosby RD, Swanson SA, Solmi F, et al. Longitudinal associations between binge eating and overeating and adverse outcomes among adolescents and young adults: does loss of control matter? JAMA Pediatr. 2013;167:149–55. https://doi.org/10.1001/2013.jamapediatrics.12
Russell H, Oliver C. The assessment of food-related problems in individuals with Prader-Willi syndrome. Br J Clin Psychol. 2003;42:379–92. https://doi.org/10.1348/014466503322528928
Yanovski SZ, Marcus MD, Wadden TA, Walsh BT. The Questionnaire on Eating and Weight Patterns-5: an updated screening instrument for binge eating disorder. Int J Eat Disord. 2015;48:259–61. https://doi.org/10.1002/eat.22372
Johnson WG, Grieve FG, Adams CD, Sandy J. Measuring binge eating in adolescents: adolescent and parent versions of the questionnaire of eating and weight patterns. Int J Eat Disord. 1999;26:301–14. 10.1002/(sici)1098-108x(199911)26:3<301::aid-eat8>3.0.co;2-m
Fairburn CG. Overcoming binge eating, Second Edition: The proven program to learn why you binge and how you can stop. Guilford Publications; 2013
Rasmusson G, Lydecker JA, Coffino JA, White MA, Grilo CM. Household food insecurity is associated with binge-eating disorder and obesity. Int J Eat Disord. 2019;52:28–35. https://doi.org/10.1002/eat.22990
West CE, Goldschmidt AB, Mason SM, Neumark‐Sztainer D. Differences in risk factors for binge eating by socioeconomic status in a community‐based sample of adolescents: findings from Project EAT. Int J Eat Disord. 2019;52:659–68
Leung CW, Stewart AL, Portela-Parra ET, Adler NE, Laraia BA, Epel ES. Understanding the psychological distress of food insecurity: a qualitative study of children’s experiences and related coping strategies. J Acad Nutr Diet. 2020;120:395–403. https://doi.org/10.1016/j.jand.2019.10.012
West CE, Goldschmidt AB, Mason SM, Neumark‐Sztainer D. Differences in risk factors for binge eating by socioeconomic status in a community‐based sample of adolescents: Findings from Project EAT. Int J Eat Disord. 2019;52:659–68
Fram MS, Frongillo EA, Jones SJ, Williams RC, Burke MP, DeLoach KP, et al. Children are aware of food insecurity and take responsibility for managing food resources. J Nutr. 2011;141:1114–9. https://doi.org/10.3945/jn.110.135988
Brown AGM, Esposito LE, Fisher RA, Nicastro HL, Tabor DC, Walker JR. Food insecurity and obesity: research gaps, opportunities, and challenges. Transl Behav Med. 2019;9:980–7. https://doi.org/10.1093/tbm/ibz117
Berger AT, Widome R, Erickson DJ, Laska MN, Harnack LJ. Changes in association between school foods and child and adolescent dietary quality during implementation of the Healthy, Hunger-Free Kids Act of 2010. Ann Epidemiol. 2020;47:30–36. https://doi.org/10.1016/j.annepidem.2020.05.013
Tester JM, Leung CW, Crawford PB, Revised WIC. Food package and children’s diet quality. Pediatrics. 2016;137:e20153557 https://doi.org/10.1542/peds.2015-3557
Eicher-Miller HA. A review of the food security, diet and health outcomes of food pantry clients and the potential for their improvement through food pantry interventions in the United States. Physiol Behav. 2020;220:112871 https://doi.org/10.1016/j.physbeh.2020.112871
Trude ACB, Kharmats AY, Hurley KM, Anderson Steeves E, Talegawkar SA, Gittelsohn J. Household, psychosocial, and individual-level factors associated with fruit, vegetable, and fiber intake among low-income urban African American youth. BMC Public Health. 2016;16:872 https://doi.org/10.1186/s12889-016-3499-6
Nightingale CM, Rudnicka AR, Ram B, Shankar A, Limb ES, Procter D, et al. Housing, neighbourhood and sociodemographic associations with adult levels of physical activity and adiposity: baseline findings from the ENABLE London study. BMJ Open. 2018;8:e021257 https://doi.org/10.1136/bmjopen-2017-021257
Nobari TZ, Whaley SE, Blumenberg E, Prelip ML, Wang MC. Severe housing-cost burden and obesity among preschool-aged low-income children in Los Angeles County. Prev Med Rep. 2019;13:139–45. https://doi.org/10.1016/j.pmedr.2018.12.003
Lohman BJ, Stewart S, Gundersen C, Garasky S, Eisenmann JC. Adolescent overweight and obesity: links to food insecurity and individual, maternal, and family stressors. J Adolesc Health. 2009;45:230–7. https://doi.org/10.1016/j.jadohealth.2009.01.003
Parks EP, Kumanyika S, Moore RH, Stettler N, Wrotniak BH, Kazak A. Influence of stress in parents on child obesity and related behaviors. Pediatrics. 2012;130:e1096–104. https://doi.org/10.1542/peds.2012-0895
Shankardass K, McConnell R, Jerrett M, Lam C, Wolch J, Milam J, et al. Parental stress increases body mass index trajectory in pre-adolescents. Pediatr Obes. 2014;9:435–42. https://doi.org/10.1111/j.2047-6310.2013.00208.x
Parks EP, Kazak A, Kumanyika S, Lewis L, Barg FK. Perspectives on stress, parenting, and children’s obesity-related behaviors in black families. Health Educ Behav. 2016;43:632–40. https://doi.org/10.1177/1090198115620418
Baskind MJ, Taveras EM, Gerber MW, Fiechtner L, Horan C, Sharifi M. Parent-perceived stress and its association with children’s weight and obesity-related behaviors. Prev Chronic Dis. 2019;16:180368 https://doi.org/10.5888/pcd16.180368
Adam TC, Epel ES. Stress, eating and the reward system. Physiol Behav. 2007;91:449–58. https://doi.org/10.1016/j.physbeh.2007.04.011
Tomiyama AJ, Dallman MF, Epel ES. Comfort food is comforting to those most stressed: evidence of the chronic stress response network in high-stress women. Psychoneuroendocrinology. 2011;36:1513–9. https://doi.org/10.1016/j.psyneuen.2011.04.005
Torres SJ, Nowson CA. Relationship between stress, eating behavior, and obesity. Nutrition. 2007;23:887–94. https://doi.org/10.1016/j.nut.2007.08.008
Goulding AN, Rosenblum KL, Miller AL, Peterson KE, Chen YP, Kaciroti N, et al. Associations between maternal depressive symptoms and child feeding practices in a cross-sectional study of low-income mothers and their young children. Int J Behav Nutr Phys Act. 2014;11:75 https://doi.org/10.1186/1479-5868-11-75
Bronte-Tinkew J, Zaslow M, Capps R, Horowitz A, McNamara M. Food insecurity works through depression, parenting, and infant feeding to influence overweight and health in toddlers. J Nutr. 2007;137:2160–5. https://doi.org/10.1093/jn/137.9.2160
Tate EB, Wood W, Liao Y, Dunton GF. Do stressed mothers have heavier children? A meta-analysis on the relationship between maternal stress and child body mass index. Obes Rev. 2015;16:351–61. https://doi.org/10.1111/obr.12262
Golan M, Kaufman V, Shahar DR. Childhood obesity treatment: targeting parents exclusively v. parents and children. Br J Nutr. 2006;95:1008–15. https://doi.org/10.1079/bjn20061757
Wrotniak BH, Epstein LH, Paluch RA, Roemmich JN. The relationship between parent and child self-reported adherence and weight loss. Obes Res. 2005;13:1089–96. https://doi.org/10.1038/oby.2005.127
Saelens BE, McGrath AM. Self-monitoring adherence and adolescent weight control efficacy. Child Health Care. 2003;32:137–52. https://doi.org/10.1207/S15326888CHC3202_5
Germann JN, Kirschenbaum DS, Rich BH. Child and parental self-monitoring as determinants of success in the treatment of morbid obesity in low-income minority children. J Pediatr Psychol. 2007;32:111–21. https://doi.org/10.1093/jpepsy/jsl007
Steele MM, Steele RG, Hunter HL. Family adherence as a predictor of child outcome in an intervention for pediatric obesity: different outcomes for self-report and objective measures. Child Health Care. 2009;38:64–75. https://doi.org/10.1080/02739610802615898
Theim KR, Sinton MM, Goldschmidt AB, Van Buren DJ, Doyle AC, Saelens BE, et al. Adherence to behavioral targets and treatment attendance during a pediatric weight control trial. Obesity. 2013;21:394–7. https://doi.org/10.1002/oby.20281
Cena H, Stanford FC, Ochner L, Fonte ML, Biino G, De Giuseppe R, et al. Association of a history of childhood-onset obesity and dieting with eating disorders. Eat Disord. 2017;25:216–29. https://doi.org/10.1080/10640266.2017.1279905
Fairburn CG, Wilson GT, Schleimer K. Binge eating: nature, assessment, and treatment. Guilford Press; 1993
Gormally J, Black S, Daston S, Rardin D. The assessment of binge eating severity among obese persons. Addict Behav. 1982;7:47–55. https://doi.org/10.1016/0306-4603(82)90024-7
Goldschmidt AB. Are loss of control while eating and overeating valid constructs? A critical review of the literature. Obes Rev. 2017;18:412–49. https://doi.org/10.1111/obr.12491
Acknowledgements
This study was supported by the Centers for Disease Control and Prevention National Center for Chronic Disease Prevention and Health Promotion (Award no.: U18DP006259). Dr Fiechtner is supported by grant number K23HD090222 from the Eunice Kennedy Shriver National Institute of Child Health and Human Development. Dr Harshman is supported by grant number F32MH118824 from the National Institute of Mental Health. Dr Taveras is supported by grant K24 DK10589 from the National Institute of Diabetes and Digestive and Kidney Diseases. The content is solely the responsibility of the authors and does not necessarily represent the official views of the Centers for Disease Control, or the National Institutes of Health.
Author information
Authors and Affiliations
Contributions
LF and ET were involved in all parts of the study, including study concept and design, obtaining funding, data collection, analysis, and writing of manuscript; MP was involved in administrative, technical, and material support of the study as well as design of the analysis; ML conducted the data analysis, SGH and SP, KBM, HC, IC, and BR were involved in the data analysis plan development and execution, and manuscript preparation; all authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Harshman, S.G., Castro, I., Perkins, M. et al. Pediatric weight management interventions improve prevalence of overeating behaviors. Int J Obes 46, 630–636 (2022). https://doi.org/10.1038/s41366-021-00989-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-021-00989-x