Abstract
Background/objectives
Platelet-activating factor receptor (PAFR) activation controls adipose tissue (AT) expansion in animal models. Our objective was twofold: (i) to check whether PAFR signaling is involved in human obesity and (ii) investigate the PAF pathway role in hematopoietic or non-hematopoietic cells to control adipocyte size.
Materials/Subjects and methods
Clinical parameters and adipose tissue gene expression were evaluated in subjects with obesity. Bone marrow (BM) transplantation from wild-type (WT) or PAFR−/− mice was performed to obtain chimeric PAFR-deficient mice predominantly in hematopoietic or non-hematopoietic-derived cells. A high carbohydrate diet (HC) was used to induce AT remodeling and evaluate in which cell compartment PAFR signaling modulates it. Also, 3T3-L1 cells were treated with PAF to evaluate fat accumulation and the expression of genes related to it.
Results
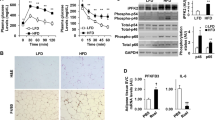
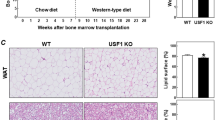
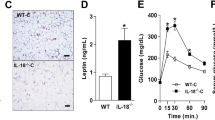
PAFR expression in omental AT from humans with obesity was negatively correlated to different corpulence parameters and more expressed in the stromal vascular fraction than adipocytes. Total PAFR−/− increased adiposity compared with WT independent of diet-induced obesity. Differently, WT mice receiving PAFR−/−-BM exhibited similar adiposity gain as WT chimeras. PAFR−/− mice receiving WT-BM showed comparable augmentation in adiposity as total PAFR−/− mice, demonstrating that PAFR signaling modulates adipose tissue expansion through non-hematopoietic cells. Indeed, the PAF treatment in 3T3-L1 adipocytes reduced fat accumulation and expression of adipogenic genes.
Conclusions
Therefore, decreased PAFR signaling may favor an AT accumulation in humans and animal models. Importantly, PAFR signaling, mainly in non-hematopoietic cells, especially in adipocytes, appears to play a significant role in regulating diet-induced AT expansion.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Hotamisligil GS, Shargill NS, Spiegelman BM. Adipose expression of tumor necrosis factor-alpha: direct role in obesity-linked insulin resistance. Science. 1993;259:87–91.
Belkina AC, Denis GV. Obesity genes and insulin resistance. Curr Opin Endocrinol Diabetes Obes. 2010;17:472–7.
Marcelin G, Silveira ALM, Martins LB, Ferreira AV, Clement K. Deciphering the cellular interplays underlying obesity-induced adipose tissue fibrosis. J Clin Investig. 2019;129:4032–40.
Ye J, McGuinness OP. Inflammation during obesity is not all bad: evidence from animal and human studies. Am J Physiol Endocrinol Metab. 2013;304:E466–77.
Asterholm IW, Rutkowski JM, Fujikawa T, Cho YR, Fukuda M, Tao C, et al. Elevated resistin levels induce central leptin resistance and increased atherosclerotic progression in mice. Diabetologia. 2014;57:1209–18.
Menezes-Garcia Z, Oliveira MC, Lima RL, Soriani FM, Cisalpino D, Botion LM, et al. Lack of platelet-activating factor receptor protects mice against diet-induced adipose inflammation and insulin-resistance despite fat pad expansion. Obesity. 2014;22:663–72.
Brestoff JR, Kim BS, Saenz SA, Stine RR, Monticelli LA, Sonnenberg GF, et al. Group 2 innate lymphoid cells promote beiging of white adipose tissue and limit obesity. Nature. 2015;519:242–6.
Wallenius V, Wallenius K, Ahren B, Rudling M, Carlsten H, Dickson SL, et al. Interleukin-6-deficient mice develop mature-onset obesity. Nat Med. 2002;8:75–9.
Garcia MC, Wernstedt I, Berndtsson A, Enge M, Bell M, Hultgren O, et al. Mature-onset obesity in interleukin-1 receptor I knockout mice. Diabetes. 2006;55:1205–13.
Xu H, Hirosumi J, Uysal KT, Guler AD, Hotamisligil GS. Exclusive action of transmembrane TNF alpha in adipose tissue leads to reduced adipose mass and local but not systemic insulin resistance. Endocrinology. 2002;143:1502–11.
Martins LB, Oliveira MC, Menezes-Garcia Z, Rodrigues DF, Lana JP, Vieira LQ, et al. Paradoxical role of tumor necrosis factor on metabolic dysfunction and adipose tissue expansion in mice. Nutrition. 2018;50:1–7.
Sugatani J, Sadamitsu S, Yamaguchi M, Yamazaki Y, Higa R, Hattori Y, et al. Antiobese function of platelet-activating factor: increased adiposity in platelet-activating factor receptor-deficient mice with age. FASEB J. 2014;28:440–52.
Yamaguchi M, Matsui M, Higa R, Yamazaki Y, Ikari A, Miyake M, et al. A platelet-activating factor (PAF) receptor deficiency exacerbates diet-induced obesity but PAF/PAF receptor signaling does not contribute to the development of obesity-induced chronic inflammation. Biochem Pharmacol. 2015;93:482–95.
Venable ME, Zimmerman GA, McIntyre TM, Prescott SM. Platelet-activating factor: a phospholipid autacoid with diverse actions. J Lipid Res. 1993;34:691–702.
Rios FJ, Koga MM, Ferracini M, Jancar S. Co-stimulation of PAFR and CD36 is required for oxLDL-induced human macrophages activation. PLoS ONE. 2012;7:e36632.
Kajiwara N, Sasaki T, Bradding P, Cruse G, Sagara H, Ohmori K, et al. Activation of human mast cells through the platelet-activating factor receptor. J Allergy Clin Immunol. 2010;125:1137–1145 e6.
Montrucchio G, Lupia E, Battaglia E, Del Sorbo L, Boccellino M, Biancone L, et al. Platelet-activating factor enhances vascular endothelial growth factor-induced endothelial cell motility and neoangiogenesis in a murine matrigel model. Arterioscler Thromb Vasc Biol. 2000;20:80–8.
Prescott SM, Zimmerman GA, Stafforini DM, McIntyre TM. Platelet-activating factor and related lipid mediators. Annu Rev Biochem. 2000;69:419–45.
Ishii S, Shimizu T. Platelet-activating factor (PAF) receptor and genetically engineered PAF receptor mutant mice. Prog Lipid Res. 2000;39:41–82.
Camussi G, Tetta C, Baglioni C. The role of platelet-activating factor in inflammation. Clin Immunol Immunopathol. 1990;57:331–8.
Triggiani M, Schleimer RP, Warner JA, Chilton FH. Differential synthesis of 1-acyl-2-acetyl-sn-glycero-3-phosphocholine and platelet-activating factor by human inflammatory cells. J Immunol. 1991;147:660–6.
Thivierge M, Parent JL, Stankova J, Rola-Pleszczynski M. Modulation of human platelet-activating factor receptor gene expression by protein kinase C activation. J Immunol. 1996;157:4681–7.
Kurano M, Darestani SG, Shinnakasu A, Yamamoto K, Dochi Y, Uemura K, et al. mRNA expression of platelet activating factor receptor (PAFR) in peripheral blood mononuclear cells is associated with albuminuria and vascular dysfunction in patients with type 2 diabetes. Diabetes Res Clin Pract. 2018;136:124–33.
Divoux A, Tordjman J, Lacasa D, Veyrie N, Hugol D, Aissat A, et al. Fibrosis in human adipose tissue: composition, distribution, and link with lipid metabolism and fat mass loss. Diabetes. 2010;59:2817–25.
Aron-Wisnewsky J, Julia Z, Poitou C, Bouillot JL, Basdevant A, Chapman MJ, et al. Effect of bariatric surgery-induced weight loss on SR-BI-, ABCG1-, and ABCA1-mediated cellular cholesterol efflux in obese women. J Clin Endocrinol Metab. 2011;96:1151–9.
Ishii S, Kuwaki T, Nagase T, Maki K, Tashiro F, Sunaga S, et al. Impaired anaphylactic responses with intact sensitivity to endotoxin in mice lacking a platelet-activating factor receptor. J Exp Med. 1998;187:1779–88.
Castor MG, Rezende B, Resende CB, Alessandri AL, Fagundes CT, Sousa LP, et al. The CCL3/macrophage inflammatory protein-1alpha-binding protein evasin-1 protects from graft-versus-host disease but does not modify graft-versus-leukemia in mice. J Immunol. 2010;184:2646–54.
Rodbell M. Metabolism of isolated fat cells. I. Effects of hormones on glucose metabolism and lipolysis. J Biol Chem. 1964;239:375–80.
Chen Z, Torrens JI, Anand A, Spiegelman BM, Friedman JM. Krox20 stimulates adipogenesis via C/EBPbeta-dependent and -independent mechanisms. Cell Metab. 2005;1:93–106.
Zebisch K, Voigt V, Wabitsch M, Brandsch M. Protocol for effective differentiation of 3T3-L1 cells to adipocytes. Anal Biochem. 2012;425:88–90.
Li Y, Zhao X, Feng X, Liu X, Deng C, Hu CH. Berberine alleviates olanzapine-induced adipogenesis via the AMPKalpha-SREBP Pathway in 3T3-L1 cells. Int J Mol Sci. 2016;17:1865.
Mehra A, Macdonald I, Pillay TS. Variability in 3T3-L1 adipocyte differentiation depending on cell culture dish. Anal Biochem. 2007;362:281–3.
Oliveira MC, Menezes-Garcia Z, Henriques MC, Soriani FM, Pinho V, Faria AM, et al. Acute and sustained inflammation and metabolic dysfunction induced by high refined carbohydrate-containing diet in mice. Obesity. 2013;21:E396–406.
Yost CC, Weyrich AS, Zimmerman GA. The platelet activating factor (PAF) signaling cascade in systemic inflammatory responses. Biochimie. 2010;92:692–7.
Li W, McIntyre TM. Platelet-activating factor receptor affects food intake and body weight. Genes Dis. 2015;2:255–60.
Lacerda DR, Soares DD, Costa KA, Nunes-Silva A, Rodrigues DF, Sabino JL, et al. Mechanisms underlying fat pad remodeling induced by fasting: role of PAF receptor. Nutrition. 2020;71:110616.
Caer C, Rouault C, Le Roy T, Poitou C, Aron-Wisnewsky J, Torcivia A, et al. Immune cell-derived cytokines contribute to obesity-related inflammation, fibrogenesis and metabolic deregulation in human adipose tissue. Sci Rep. 2017;7:3000.
Schmidt FM, Weschenfelder J, Sander C, Minkwitz J, Thormann J, Chittka T, et al. Inflammatory cytokines in general and central obesity and modulating effects of physical activity. PLoS ONE. 2015;10:e0121971.
Kudolo GB, Bressler P, DeFronzo RA, Plasma PAF. acetylhydrolase in non-insulin dependent diabetes mellitus and obesity: effect of hyperinsulinemia and lovastatin treatment. J Lipid Mediat Cell Signal. 1997;17:97–113.
Okada T, Miyashita M, Kuromori Y, Iwata F, Harada K, Hattori H. Platelet-activating factor acetylhydrolase concentration in children with abdominal obesity. Arterioscler Thromb Vasc Biol. 2006;26:e40–1.
Tzotzas T, Filippatos TD, Triantos A, Bruckert E, Tselepis AD, Kiortsis DN. Effects of a low-calorie diet associated with weight loss on lipoprotein-associated phospholipase A2 (Lp-PLA2) activity in healthy obese women. Nutr Metab Cardiovasc Dis. 2008;18:477–82.
Campo S, Sardo MA, Bitto A, Bonaiuto A, Trimarchi G, Bonaiuto M, et al. Platelet-activating factor acetylhydrolase is not associated with carotid intima-media thickness in hypercholesterolemic Sicilian individuals. Clin Chem. 2004;50:2077–82.
de Castro SH, Faria Neto HC, Gomes MB. Platelet-activating factor acetylhydrolase (PAF-AH) activity in patients with type 1 diabetes mellitus. Arq Bras Cardiol. 2007;88:179–84.
Pamir N, McMillen TS, Kaiyala KJ, Schwartz MW, LeBoeuf RC. Receptors for tumor necrosis factor-alpha play a protective role against obesity and alter adipose tissue macrophage status. Endocrinology. 2009;150:4124–34.
Jiao P, Feng B, Ma J, Nie Y, Paul E, Li Y, et al. Constitutive activation of IKKbeta in adipose tissue prevents diet-induced obesity in mice. Endocrinology. 2012;153:154–65.
Kosteli A, Sugaru E, Haemmerle G, Martin JF, Lei J, Zechner R, et al. Weight loss and lipolysis promote a dynamic immune response in murine adipose tissue. J Clin Investig. 2010;120:3466–79.
Ahmed M, Gaffen SL. IL-17 inhibits adipogenesis in part via C/EBPalpha, PPARgamma and Kruppel-like factors. Cytokine. 2013;61:898–905.
Torti FM, Dieckmann B, Beutler B, Cerami A, Ringold GM. A macrophage factor inhibits adipocyte gene expression: an in vitro model of cachexia. Science. 1985;229:867–9.
Keay S, Grossberg SE. Interferon inhibits the conversion of 3T3-L1 mouse fibroblasts into adipocytes. Proc Natl Acad Sci USA. 1980;77:4099–103.
Sohn JH, Kim JI, Jeon YG, Park J, Kim JB. Effects of three thiazolidinediones on metabolic regulation and cold-induced thermogenesis. Mol Cells. 2018;41:900–8.
Bogacka I, Xie H, Bray GA, Smith SR. The effect of pioglitazone on peroxisome proliferator-activated receptor-gamma target genes related to lipid storage in vivo. Diabetes Care. 2004;27:1660–7.
Acknowledgements
The authors thank Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES) and Comité français d’Evaluation de la Coopération Universitaire et Scientifique avec le Brésil (COFECUB) grant no 88887.130206/2017-01, Fundação de Amparo à Pesquisa do Estado de Minas Gerais (FAPEMIG), National Council for Scientific and Technological Development (CNPq/Brazil) by financial support and National Agency of Research (Captor program). Clinical investigation was performed at the Human Nutrition Research Center (CRNH Ile de France), Pitié-Salpêtrière Hospital.
Author information
Authors and Affiliations
Contributions
Conceptualization, AVMF; Project Administration, KAC; Methodology, AVMF, CR, GM, VPS, BMR, and AMS; Investigation, KAC, DRL, ALMS, MCO, ZMG, and FLBM; Resources, AVMF, MMT, AMS and KC; Writing – Original Draft, KAC, ALMS, and DRL; Visualization, ALMS, LBM, and MCO; Writing – Review & Editing, AVMF, GM, ALMS, MCO, AMS, KC and CR; Funding Acquisition, AVMF and KC; Guarantor of this work, AVMF.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Costa, K.A., Lacerda, D.R., Silveira, A.L.M. et al. PAF signaling plays a role in obesity-induced adipose tissue remodeling. Int J Obes 46, 68–76 (2022). https://doi.org/10.1038/s41366-021-00961-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-021-00961-9