Abstract
Background/Objective
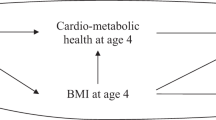
Adiposity may mediate the effect of dietary glycemic load (GL) on lipid profiles in children, as studies have shown an association between dietary GL and adiposity and between adiposity and lipid profiles. Our objective was to evaluate the role of adiposity as a mediator in the association between dietary GL and lipid profiles after 2 years.
Subjects/Methods
The Quebec Adipose and Lifestyle InvesTigation in Youth study included 630 children, 8–10 years old at recruitment with at least one parent with overweight or obesity with 2-year follow-up. Three baseline 24-h dietary recalls were administered by a dietitian at baseline. Child and parent characteristics were obtained through direct measurement (blood lipids, anthropometrics) or questionnaires (socio-economic characteristics). Indicators of adiposity, including body mass index (BMI) z-score and percent body fat, were the mediators of interest. A conventional approach using the Baron and Kenny method was used. A causal approach using marginal structural models (MSM) was used to estimate the controlled direct effect.
Results
Mean age at baseline was 9.6 years and 33% were overweight or obese. Both methods revealed that the effect of GL on blood lipids was mediated by adiposity. The weighted MSM did not show evidence of a direct effect (TG: β =;0.01, 95% CI = −0.01,0.02; HDL: β = 0.005, 95%CI = −0.002,0.01), whereas the conventional method did for TG but not HDL (TG:β = 0.04, 95%CI = 0.01,0.07; HDL: β = −0.01, 95%CI = −0.03,0.01).
Conclusion
Adiposity contributes substantially to the association between GL and blood lipids. The choice of approach for mediation analysis should be based on the fulfilment of conditions of each method.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Sahoo K, Sahoo B, Choudhury AK, Sofi NY, Kumar R, Bhadoria AS. Childhood obesity: causes and consequences. J Family Med Prim Care. 2015;4:187–92.
Friedemann C, Heneghan C, Mahtani K, Thompson M, Perera R, Ward AM. Cardiovascular disease risk in healthy children and its association with body mass index: systematic review and meta-analysis. BMJ. 2012;345:e4759.
Juhola J, Magnussen CG, Viikari JS, Kahonen M, Hutri-Kahonen N, Jula A, et al. Tracking of serum lipid levels, blood pressure, and body mass index from childhood to adulthood: the Cardiovascular Risk in Young Finns Study. J Pediatr. 2011;159:584–90.
Baker JL, Olsen LW, Sorensen TI. Childhood body-mass index and the risk of coronary heart disease in adulthood. N Engl J Med. 2007;357:2329–37.
Morrison JA, Glueck CJ, Horn PS, Yeramaneni S, Wang P. Pediatric triglycerides predict cardiovascular disease events in the fourth to fifth decade of life. Metabolism. 2009;58:1277–84.
Shikany JM, Tinker LF, Neuhouser ML, Ma Y, Patterson RE, Phillips LS, et al. Association of glycemic load with cardiovascular disease risk factors: the Women’s Health Initiative Observational Study. Nutrition. 2010;26:641–7.
McKeown NM, Meigs JB, Liu S, Saltzman E, Wilson PW, Jacques PF. Carbohydrate nutrition, insulin resistance, and the prevalence of the metabolic syndrome in the Framingham Offspring Cohort. Diabetes Care. 2004;27:538–46.
Song S, Lee JE, Song WO, Paik HY, Song Y. Carbohydrate intake and refined-grain consumption are associated with metabolic syndrome in the Korean adult population. J Acad Nutr Diet. 2014;114:54–62.
Ford ES, Liu S. Glycemic index and serum high-density lipoprotein cholesterol concentration among us adults. Arch Internal Med. 2001;161:572–6.
Zhang X, Zhu Y, Cai L, Ma L, Jing J, Guo L, et al. Dietary glycemic index and glycemic load and their relationship to cardiovascular risk factors in Chinese children. Appl Physiol Nutr Metab. 2016;41:391–6.
Slyper A, Jurva J, Pleuss J, Hoffmann R, Gutterman D. Influence of glycemic load on HDL cholesterol in youth. Am J Clin Nutr. 2005;81:376–9.
Baron RM, Kenny DA. The moderator-mediator variable distinction in social psychological research: conceptual, strategic, and statistical considerations. J Pers Soc Psychol. 1986;51:1173–82.
Cole SR, Platt RW, Schisterman EF, Chu H, Westreich D, Richardson D, et al. Illustrating bias due to conditioning on a collider. Int J Epidemiol. 2009;39:417–20.
Cole SR, Hernan MA. Fallibility in estimating direct effects. Int J Epidemiol. 2002;31:163–5.
Kaufman JS, Maclehose RF, Kaufman S. A further critique of the analytic strategy of adjusting for covariates to identify biologic mediation. Epidemiol Perspect Innov. 2004;1:4.
Nandi A, Glymour MM, Kawachi I, VanderWeele TJ. Using marginal structural models to estimate the direct effect of adverse childhood social conditions on onset of heart disease, diabetes, and stroke. Epidemiology. 2012;23:223–32.
Van der Wal WM, Geskus RB. An R package for inverse probability weighting. J Stat Softw. 2011;43:1–23.
Lambert M, Van Hulst A, O’Loughlin J, Tremblay A, Barnett TA, Charron H, et al. Cohort profile: the Quebec adipose and lifestyle investigation in youth cohort. Int J Epidemiol. 2012;41:1533–44.
Suissa K, Benedetti A, Henderson M, Gray-Donald K, Paradis G. Effects of dietary glycemic index and load on children’s cardiovascular risk factors. Ann Epidemiol. 2019;40:e3.
Centers for Disease Control and Prevention, National Center for Health Statistics. CDC growth charts: United States. http://www.cdc.gov/growthcharts/. In, May 30, 2000.
World Health Organization (WHO). BMI-for-age (5-19 years). Accessed on September 15, 2020 from https://www.who.int/growthref/who2007_bmi_for_age/en/. In.
Friedewald WT, Levy RI, Fredrickson DS. Estimation of the concentration of low-density lipoprotein cholesterol in plasma, without use of the preparative ultracentrifuge. Clin Chem. 1972;18:499–502.
Colley R, Connor Gorber S, Tremblay MS. Quality control and data reduction procedures for accelerometry-derived measures of physical activity. Health Reports. 2010;21:63–9.
Henderson M, Gray-Donald K, Mathieu ME, Barnett TA, Hanley JA, O’Loughlin J, et al. How are physical activity, fitness, and sedentary behavior associated with insulin sensitivity in children? Diabetes Care. 2012;35:1272–8.
Marshall WA, Tanner JM. Variations in pattern of pubertal changes in girls. Arch Dis Child. 1969;44:291–303.
Marshall WA, Tanner JM. Variations in the pattern of pubertal changes in boys. Arch Dis Child. 1970;45:13–23.
Shim JS, Oh K, Kim HC. Dietary assessment methods in epidemiologic studies. Epidemiol Health. 2014;36:e2014009.
Johnson RK, Driscoll P, Goran MI. Comparison of multiple-pass 24-hour recall estimates of energy intake with total energy expenditure determined by the doubly labeled water method in young children. J Am Diet Assoc. 1996;96:1140–4.
Louie JC, Flood V, Turner N, Everingham C, Gwynn J. Methodology for adding glycemic index values to 24-hour recalls. Nutrition. 2011;27:59–64.
Atkinson FS, Foster-Powell K, Brand-Miller JC. International tables of glycemic index and glycemic load values: 2008. Diabetes Care. 2008;31:2281–3.
Olendzki BC, Ma Y, Culver AL, Ockene IS, Griffith JA, Hafner AR, et al. Methodology for adding glycemic index and glycemic load values to 24-hour dietary recall database. Nutrition. 2006;22:1087–95.
Willett WC, Howe GR, Kushi LH. Adjustment for total energy intake in epidemiologic studies. Am J Clin Nutr. 1997;65:1220S–1228S. 4 Suppldiscussion 1229S-1231S
Suissa K, Benedetti A, Henderson M, Gray-Donald K, Paradis G. The cardiometabolic risk profile of underreporters of energy intake differs from that of adequate reporters among children at risk of obesity. J Nutr. 2019;149:123–30.
Nandi A, VanderWeele TJ. Mediation analysis in social epidemiology. Methods in social epidemiology. Hoboken: John Wiley & Sons; 2006. p. 398–430.
VanderWeele TJ. Marginal structural models for the estimation of direct and indirect effects. Epidemiology. 2009;20:18–26.
Valeri L, Lin X, VanderWeele TJ. Mediation analysis when a continuous mediator is measured with error and the outcome follows a generalized linear model. Stat Med. 2014;33:4875–90.
Robins JM, Hernan MA, Brumback B. Marginal structural models and causal inference in epidemiology. Epidemiology. 2000;11:550–60.
Ludwig DS. The glycemic index: physiological mechanisms relating to obesity, diabetes, and cardiovascular disease. JAMA. 2002;287:2414–23.
Te Morenga LA, Howatson AJ, Jones RM, Mann J. Dietary sugars and cardiometabolic risk: systematic review and meta-analyses of randomized controlled trials of the effects on blood pressure and lipids. Am J Clin Nutr. 2014;100:65–79.
Song S, Paik HY, Song WO, Park M, Song Y. Three distinct clustering patterns in metabolic syndrome abnormalities are differentially associated with dietary factors in Korean adults. Nutr Res. 2014;34:383–90.
Becker GF, Passos EP, Moulin CC. Short-term effects of a hypocaloric diet with low glycemic index and low glycemic load on body adiposity, metabolic variables, ghrelin, leptin, and pregnancy rate in overweight and obese infertile women: a randomized controlled trial. Am J Clin Nutr. 2015;102:1365–72.
Murakami K, McCaffrey TA, Livingstone MB. Dietary glycaemic index and glycaemic load in relation to food and nutrient intake and indices of body fatness in British children and adolescents. Br J Nutr. 2013;110:1512–23.
Barba G, Sieri S, Russo MD, Donatiello E, Formisano A, Lauria F, et al. Glycaemic index and body fat distribution in children: the results of the ARCA project. Nutr Metab Cardiovascular Dis. 2012;22:28–34.
Gopinath B, Flood VM, Rochtchina E, Baur LA, Louie JC, Smith W, et al. Carbohydrate nutrition and development of adiposity during adolescence. Obesity. 2013;21:1884–90.
Nielsen BM, Bjornsbo KS, Tetens I, Heitmann BL. Dietary glycaemic index and glycaemic load in Danish children in relation to body fatness. Br J Nutr. 2005;94:992–7.
Schwingshackl L, Hobl LP, Hoffmann G. Effects of low glycaemic index/low glycaemic load vs. high glycaemic index/ high glycaemic load diets on overweight/obesity and associated risk factors in children and adolescents: a systematic review and meta-analysis. Nutr J. 2015;14:87.
Thomas DE, Elliott EJ, Baur L Low glycaemic index or low glycaemic load diets for overweight and obesity. Cochrane Database Syst Rev. 2007: Cd005105. https://doi.org/10.1002/14651858.CD005105.pub2.
Luma GB, Spiotta RT. Hypertension in children and adolescents. Am Fam Phys. 2006;73:1558–68.
Plourde G. Impact of obesity on glucose and lipid profiles in adolescents at different age groups in relation to adulthood. BMC Family Pract. 2002;3:18.
Berenson GS, Wattigney WA, Bao W, Srinivasan SR, Radhakrishnamurthy B. Rationale to study the early natural history of heart disease: the Bogalusa Heart Study. Am J Med Sci. 1995;310:S22–8. Suppl 1
Tracy RE, Newman WP,3rd, Wattigney WA, Berenson GS. Risk factors and atherosclerosis in youth autopsy findings of the Bogalusa Heart Study. Am J Med Sci. 1995;310 Suppl 1:S37–41.
Stoner L, Weatherall M, Skidmore P, Castro N, Lark S, Faulkner J, et al. Cardiometabolic risk variables in preadolescent children: a factor analysis. J Am Heart Assoc. 2017;6:10.
Pires A, Martins P, Pereira AM, Marques M, Castela E, Sena C, et al. Childhood adiposity: being male is a potential cardiovascular risk factor. Eur J Pediatr. 2016;175:63–9.
Telford RD, Cunningham RB, Waring P, Telford RM, Potter JM, Hickman PE, et al. Sensitivity of blood lipids to changes in adiposity, exercise, and diet in children. Med Sci Sports Exerc. 2015;47:974–82.
Dong JY, Zhang YH, Wang P, Qin LQ. Meta-analysis of dietary glycemic load and glycemic index in relation to risk of coronary heart disease. Am J Cardiol. 2012;109:1608–13.
Valeri L, Vanderweele TJ. Mediation analysis allowing for exposure-mediator interactions and causal interpretation: theoretical assumptions and implementation with SAS and SPSS macros. Psychological Methods. 2013;18:137–50.
Cole SR, Hernan MA. Constructing inverse probability weights for marginal structural models. Am J Epidemiol. 2008;168:656–64.
Williamson T, Ravani P. Marginal structural models in clinical research: when and how to use them?. Nephrol Dial Transpl. 2017;32 Suppl 2:ii84–ii90.
Hernan MA. A definition of causal effect for epidemiological research. J Epidemiol Commun Health. 2004;58:265–71.
Acknowledgements
The QUALITY study is funded by the Canadian Institutes of Health Research (CIHR), the Heart and Stroke Foundation of Canada (HFSC), as well as the Fonds de la recherche du Québec en santé (FRQS). The authors wish to thank the QUALITY research team and especially Louise Johnson-Down for her help with the dietary data. Dr. Marie Lambert passed away on 20 February 2012, her leadership and devotion to the QUALITY study will always be remembered and appreciated.
Author information
Authors and Affiliations
Contributions
KS designed the research question for this project, conducted the analysis, interpreted results and wrote the manuscript. AB, MH, KGD and GP participated in the research question design (defining outcomes, identifying confounders, determining appropriate analysis methods), reviewed and edited the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Suissa, K., Benedetti, A., Henderson, M. et al. A mediation analysis on the relationship between dietary glycemic load, obesity and cardiovascular risk factors in children. Int J Obes 46, 774–781 (2022). https://doi.org/10.1038/s41366-021-00958-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-021-00958-4