Abstract
Background
Excessive gestational weight gain (EGWG) closely associates with postpartum obesity. However, the causal role of EGWG in postpartum obesity has not been experimentally verified. The objective of this study was to determine whether and how EGWG causes long-term postpartum obesity.
Methods
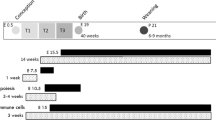
C57BL/6 mice were fed with high-fat diet during gestation (HFFDG) or control chow, then their body composition and energy metabolism were monitored after delivery.
Results
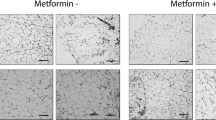
We found that HFFDG significantly increased gestational weight gain. After delivery, adiposity of HFFDG-treated mice (Preg-HF) quickly recovered to the levels of controls. However, 3 months after parturition, Preg-HF mice started to gain significantly more body fat even with regular chow. The increase of body fat of Preg-HF mice was progressive with aging and by 9 months after delivery had increased 2-fold above the levels of controls. The expansion of white adipose tissue (WAT) of Preg-HF mice was manifested by hyperplasia in visceral fat and hypertrophy in subcutaneous fat. Preg-HF mice developed low energy expenditure and UCP1 expression in interscapular brown adipose tissue (iBAT) in later life. Although blood estrogen concentrations were similar between Preg-HF and control mice, a significant decrease in estrogen receptor α (ERα) expression and hypermethylation of the ERα promoter was detected in the fat of Preg-HF mice 9 months after delivery. Interestingly, hypermethylation of ERα promoter and low ERα expression were only detected in adipocyte progenitor cells in both iBAT and WAT of Preg-HF mice at the end of gestation.
Conclusions
These results demonstrate that HFFDG causes long-term postpartum obesity independent of early postpartum fat retention. This study also suggests that HFFDG adversely programs long-term postpartum energy metabolism by epigenetically reducing estrogen signaling in both BAT and WAT.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Cynthia LO, Cheryl DF, Katherine MF. Prevalence of obesity among adults and youth: united states, 2011–2014. In. Hyattsville. MD: National Center for Health Statistics: National Center for Health Statistics; 2015.
Flegal KM, Kruszon-Moran D, Carroll MD, Fryar CD, Ogden CL. TRends in obesity among adults in the united states, 2005 to 2014. JAMA. 2016;315:2284–91.
Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of childhood and adult obesity in the United States, 2011-2012. JAMA. 2014;311:806–14.
Qiao L, Wattez JS, Lee S, Nguyen A, Schaack J, Hay WW, Jr. et al. Adiponectin deficiency impairs maternal metabolic adaptation to pregnancy in mice. Diabetes. 2017;66:1126–35.
Cohen AK, Chaffee BW, Rehkopf DH, Coyle JR, Abrams B. Excessive gestational weight gain over multiple pregnancies and the prevalence of obesity at age 40. Int J Obes. 2014;38:714–8.
Groth SW, Holland ML, Kitzman H, Meng Y. Gestational weight gain of pregnant African American adolescents affects body mass index 18 years later. J Obstet Gynecol Neonatal Nurs. 2013;42:541–50.
McClure CK, Catov JM, Ness R, Bodnar LM. Associations between gestational weight gain and BMI, abdominal adiposity, and traditional measures of cardiometabolic risk in mothers 8 y postpartum. Am J Clin Nutr. 2013;98:1218–25.
Walter JR, Perng W, Kleinman KP, Rifas-Shiman SL, Rich-Edwards JW, Oken E. Associations of trimester-specific gestational weight gain with maternal adiposity and systolic blood pressure at 3 and 7 years postpartum. Am J Obstet Gynecol. 2015;212:499 e1–499 e12.
Mamun AA, Kinarivala M, O’Callaghan MJ, Williams GM, Najman JM, Callaway LK. Associations of excess weight gain during pregnancy with long-term maternal overweight and obesity: evidence from 21 y postpartum follow-up. Am J Clin Nutr. 2010;91:1336–41.
Widen EM, Whyatt RM, Hoepner LA, Ramirez-Carvey J, Oberfield SE, Hassoun A, et al. Excessive gestational weight gain is associated with long-term body fat and weight retention at 7 y postpartum in African American and Dominican mothers with underweight, normal, and overweight prepregnancy BMI. Am J Clin Nutr. 2015;102:1460–7.
Rooney BL, Schauberger CW, Mathiason MA. Impact of perinatal weight change on long-term obesity and obesity-related illnesses. Obstet Gynecol. 2005;106:1349–56.
Linne Y, Dye L, Barkeling B, Rossner S. Long-term weight development in women: a 15-year follow-up of the effects of pregnancy. Obes Res. 2004;12:1166–78.
Yoo HS, Qiao L, Bosco C, Leong L-H, Lytle N, Feng G-S, et al. Intermittent cold exposure enhances fat accumulation in mice. PLoS ONE. 2014;9:e96432.
Qiao L, Yoo HS, Bosco C, Lee B, Feng G-S, Schaack J, et al. Adiponectin reduces thermogenesis by inhibiting brown adipose tissue activation in mice. Diabetologia. 2014;57:1027–36.
Tseng Y-H, Kokkotou E, Schulz TJ, Huang TL, Winnay JN, Taniguchi CM, et al. New role of bone morphogenetic protein 7 in brown adipogenesis and energy expenditure. Nature. 2008;454:1000–4.
Qiao L, MacLean PS, Schaack J, Orlicky DJ, Darimont C, Pagliassotti M, et al. C/EBPalpha regulates human adiponectin gene transcription through an intronic enhancer. Diabetes. 2005;54:1744–54.
Westberry JM, Trout AL, Wilson ME. Epigenetic regulation of estrogen receptor alpha gene expression in the mouse cortex during early postnatal development. Endocrinology. 2010;151:731–40.
Andrews JF, Richard D, Jennings G, Trayhurn P. Brown adipose tissue thermogenesis during pregnancy in mice. Ann Nutr Metab. 1986;30:87–93.
Frontera M, Pujol E, Rodriguez-Cuenca S, Catala-Niell A, Roca P, Garcia-Palmer FJ, et al. Rat brown adipose tissue thermogenic features are altered during mid-pregnancy. Cell Physiol Biochem. 2005;15:203–10.
Martinez de Morentin PB, Lage R, Gonzalez-Garcia I, Ruiz-Pino F, Martins L, Fernandez-Mallo D, et al. Pregnancy induces resistance to the anorectic effect of hypothalamic malonyl-CoA and the thermogenic effect of hypothalamic AMPK inhibition in female rats. Endocrinology. 2015;156:947–60.
Trayhurn P, Douglas JB, McGuckin MM. Brown adipose tissue thermogenesis is /‘suppressed/‘ during lactation in mice. Nature. 1982;298:59–60.
Mercer SW, Trayhurn P. Effect of high fat diets on the thermogenic activity of brown adipose tissue in cold-acclimated mice. J Nutr. 1984;114:1151–8.
Wu MV, Bikopoulos G, Hung S, Ceddia RB. Thermogenic capacity is antagonistically regulated in classical brown and white subcutaneous fat depots by high fat diet and endurance training in rats: impact on whole-body energy expenditure. J Biol Chem. 2014;289:34129–40.
Brooks SL, Rothwell NJ, Stock MJ, Goodbody AE, Trayhurn P. Increased proton conductance pathway in brown adipose tissue mitochondria of rats exhibiting diet-induced thermogenesis. Nature. 1980;286:274–6.
Garcia-Ruiz E, Reynes B, Diaz-Rua R, Ceresi E, Oliver P, Palou A. The intake of high-fat diets induces the acquisition of brown adipocyte gene expression features in white adipose tissue. Int J Obes (Lond). 2015;39:1619–29.
Lee Y-H, Petkova AP, Mottillo EP, Granneman JG. In vivo identification of bipotential adipocyte progenitors recruited by β3-adrenoceptor activation and high-fat feeding. Cell Metab. 2012;15:480–91.
Granneman JG, Li P, Zhu Z, Lu Y. Metabolic and cellular plasticity in white adipose tissue I: effects of beta3-adrenergic receptor activation. Am J Physiol Endocrinol Metab. 2005;289:E608–16.
Palmer BF, Clegg DJ. The sexual dimorphism of obesity. Mol Cell Endocrinol. 2015;402:113–9.
Villena JA, Kralli A. ERRalpha: a metabolic function for the oldest orphan. Trends Endocrinol Metab: TEM. 2008;19:269–76.
Van Pelt RE, Gavin KM, Kohrt WM. Regulation of body composition and bioenergetics by estrogens. Endocrinol Metab Clin North Am. 2015;44:663–76.
Al-Safi ZA, Polotsky AJ. Obesity and menopause. Best Pract Res Clin Obstet Gynaecol. 2015;29:548–53.
Hevener AL, Clegg DJ, Mauvais-Jarvis F. Impaired estrogen receptor action in the pathogenesis of the metabolic syndrome. Mol Cell Endocrinol. 2015;418:306–21.
Watanabe T, Inoue S, Hiroi H, Orimo A, Kawashima H, Muramatsu M. Isolation of estrogen-responsive genes with a CpG island library. Mol Cell Biol. 1998;18:442–9.
Wilson ME, Westberry JM, Prewitt AK. Dynamic regulation of estrogen receptor-alpha gene expression in the brain: a role for promoter methylation? Front Neuroendocrinol. 2008;29:375–85.
Waalkes MP, Liu J, Chen H, Xie Y, Achanzar WE, Zhou YS, et al. Estrogen signaling in livers of male mice with hepatocellular carcinoma induced by exposure to arsenic in utero. J Natl Cancer Inst. 2004;96:466–74.
Lin HF, Hsi E, Liao YC, Chhor B, Hung J, Juo SH, et al. Demethylation of circulating estrogen receptor alpha gene in cerebral ischemic stroke. PLoS ONE. 2015;10:e0139608.
Giacinti L, Claudio PP, Lopez M, Giordano A. Epigenetic information and estrogen receptor alpha expression in breast cancer. Oncologist. 2006;11:1–8.
Matsuda KI. Epigenetic changes in the estrogen receptor alpha gene promoter: implications in sociosexual behaviors. Front Neurosci. 2014;8:344.
Kos M, Reid G, Denger S, Gannon F. Minireview: genomic organization of the human ERalpha gene promoter region. Mol Endocrinol. 2001;15:2057–63.
Berry R, Rodeheffer MS. Characterization of the adipocyte cellular lineage in vivo. Nat Cell Biol. 2013;15:302–8.
Church CD, Berry R, Rodeheffer MS. Isolation and study of adipocyte precursors. Methods Enzymol. 2014;537:31–46.
Berggren EK, Groh-Wargo S, Presley L, Hauguel-De MS, Catalano PM. Maternal fat, but not lean, mass is increased among overweight/obese women with excess gestational weight gain. Am J Obstet Gynecol. 2015;214:745e1–5.
Grove KL, Fried SK, Greenberg AS, Xiao XQ, Clegg DJ. A microarray analysis of sexual dimorphism of adipose tissues in high-fat-diet-induced obese mice. Int J Obes (Lond). 2010;34:989–1000.
Hong J, Stubbins RE, Smith RR, Harvey AE, Nunez NP. Differential susceptibility to obesity between male, female and ovariectomized female mice. Nutr J. 2009;8:11.
Perez PA, DiPatrizio NV. Impact of maternal western diet-induced obesity on offspring mortality and peripheral endocannabinoid system in mice. PLoS ONE. 2018;13:e0205021.
Lichtenbelt WDV, Vanhommerig JW, Smulders NM, Drossaerts JMAFL, Kemerink GJ, Bouvy ND, et al. Cold-activated brown adipose tissue in healthy men. New Engl J Med. 2009;360:1500–8.
Virtanen KA, Lidell ME, Orava J, Heglind M, Westergren R, Niemi T, et al. Functional brown adipose tissue in healthy adults (vol 360, pg 1518, 2009). New Engl J Med. 2009;361:1123–1123.
Cypess AM, Lehman S, Williams G, Tal I, Rodman D, Goldfine AB, et al. Identification and importance of brown adipose tissue in adult humans. New Engl J Med. 2009;360:1509–17.
Rosen ED, Spiegelman BM. What we talk about when we talk about fat. Cell. 2014;156:20–44.
Heine PA, Taylor JA, Iwamoto GA, Lubahn DB, Cooke PS. Increased adipose tissue in male and female estrogen receptor-alpha knockout mice. Proc Natl Acad Sci USA. 2000;97:12729–34.
Cooke PS, Heine PA, Taylor JA, Lubahn DB. The role of estrogen and estrogen receptor-alpha in male adipose tissue. Mol Cell Endocrinol. 2001;178:147–54.
Davis KE, M DN, Sun K, W MS, J DB, J AZ, et al. The sexually dimorphic role of adipose and adipocyte estrogen receptors in modulating adipose tissue expansion, inflammation, and fibrosis. Mol Metab. 2013;2:227–42.
Martinez de Morentin PB, Gonzalez-Garcia I, Martins L, Lage R, Fernandez-Mallo D, Martinez-Sanchez N, et al. Estradiol regulates brown adipose tissue thermogenesis via hypothalamic AMPK. Cell Metab. 2014;20:41–53.
Heim M, Frank O, Kampmann G, Sochocky N, Pennimpede T, Fuchs P, et al. The phytoestrogen genistein enhances osteogenesis and represses adipogenic differentiation of human primary bone marrow stromal cells. Endocrinology. 2004;145:848–59.
Benvenuti S, Cellai I, Luciani P, Deledda C, Saccardi R, Mazzanti B, et al. Androgens and estrogens prevent rosiglitazone-induced adipogenesis in human mesenchymal stem cells. J Endocrinol Invest. 2012;35:365–71.
Gao B, Huang Q, Lin YS, Wei BY, Guo YS, Sun Z, et al. Dose-dependent effect of estrogen suppresses the osteo-adipogenic transdifferentiation of osteoblasts via canonical Wnt signaling pathway. PLoS ONE. 2014;9:e99137.
Pedram A, Razandi M, Blumberg B, Levin ER. Membrane and nuclear estrogen receptor alpha collaborate to suppress adipogenesis but not triglyceride content. FASEB J. 2015;30:230–40.
Acknowledgements
This work was supported by NIH grants HD069634 (J.S.), DK095132 (J.S.), HD007186 (W.W.H.Jr), HD068372(W.W.H.Jr), UL1TR001082(W.W.H.Jr), and American Diabetes grant 1–16-IBS-272 (J.S.). JS is the guarantor of this work and, as such, had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Author Contributions
LQ, KC, JSW, SL, HG and GSF contributed research data. LQ, WWHJr. and JS contributed to research design and manuscript preparation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Qiao, L., Chu, K., Wattez, JS. et al. High-fat feeding reprograms maternal energy metabolism and induces long-term postpartum obesity in mice. Int J Obes 43, 1747–1758 (2019). https://doi.org/10.1038/s41366-018-0304-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-018-0304-x