Abstract
Background
Timing of dietary intake may play a role in obesity. However, previous studies produced mixed findings possibly due to inconsistent approaches to characterize meal timing and not taking into account chronotype and macronutrients. To address the aforementioned limitations, we have defined meal timing relative to sleep/wake timing, investigated the relationship between meal timing and body mass index (BMI) dependent on chronotype, and examined the associations.
Methods
BMI, chronotype, and dietary intakes were measured in 872 middle-to-older-aged adults by six 24-h dietary recalls in 1 year. We defined four time windows of intake relative to sleep timing: morning (within 2 h after getting out of bed), night (within 2 h before bedtime), and two midday periods in between (split by the midpoint of the waking period).
Results
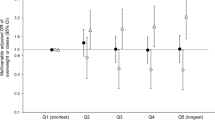
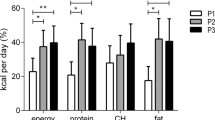
A higher percent of total daily energy intake consumed during the morning window was associated with lower odds of being overweight or obese (odds ratio (95% confidence intervals), 0.53 (0.31, 0.89)). This association was stronger in people with an earlier chronotype (0.32 (0.16, 0.66)). A higher percent of total daily energy intake consumed during the night window was associated with higher odds of being overweight or obese (1.82 (1.07, 3.08)), particularly in people with a later chronotype (4.94 (1.61, 15.14)). These associations were stronger for the intakes of carbohydrates and protein than for fat intake.
Conclusion
Our study suggests that higher dietary consumption after waking up and lower consumption close to bedtime associate with lower BMI, but the relationship differs by chronotype. Furthermore, the data demonstrate a clear relationship between the timing of carbohydrate and protein intake and obesity. Our findings highlight the importance of considering timing of intake relative to sleep timing when studying the associations of meal timing with obesity and metabolic health.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Mattson MP, Allison DB, Fontana L, Harvie M, Longo VD, Malaisse WJ, Mosley M, Notterpek L, Ravussin E, Scheer FA, Seyfried TN, Varady KA, Panda S. Meal frequency and timing in health and disease. Proc Natl Acad Sci U S A. 2014;111:16647–53.
St-Onge MP, Ard J, Baskin ML, Chiuve SE, Johnson HM, Kris-Etherton P, et al. Meal timing and frequency: implications for cardiovascular disease prevention: a scientific statement from the American Heart Association. Circulation. 2017;135:e96–e121.
Deshmukh-Taskar P, Nicklas TA, Radcliffe JD, O'Neil CE, Liu Y. The relationship of breakfast skipping and type of breakfast consumed with overweight/obesity, abdominal obesity, other cardiometabolic risk factors and the metabolic syndrome in young adults. The National Health and Nutrition Examination Survey (NHANES): 1999–2006. Public Health Nutr. 2013;16:2073–82.
Horikawa C, Kodama S, Yachi Y, et al. Skipping breakfast and prevalence of overweight and obesity in Asian and Pacific regions: a meta-analysis. Prev Med. 2011;53:260–7.
Garaulet M, Gomez-Abellan P, Alburquerque-Bejar JJ, Lee YC, Ordovas JM, Scheer FA. Timing of food intake predicts weight loss effectiveness. Int J Obes (Lond). 2013;37:604–11.
Berg C, Lappas G, Wolk A, et al. Eating patterns and portion size associated with obesity in a Swedish population. Appetite. 2009;52:21–26.
Kutsuma A, Nakajima K, Suwa K. Potential association between breakfast skipping and concomitant late-night-dinner eating with metabolic syndrome and proteinuria in the Japanese Population. Science (Cairo). 2014;2014:253581.
Wang JB, Patterson RE, Ang A, Emond JA, Shetty N, Arab L. Timing of energy intake during the day is associated with the risk of obesity in adults. J Hum Nutr Diet. 2014;27 Suppl 2:255–62.
Baron KG, Reid KJ, Horn LV, Zee PC. Contribution of evening macronutrient intake to total caloric intake and body mass index. Appetite. 2013;60:246–51.
McCrory MA, Shaw AC, Lee JA. Energy and nutrient timing for weight control: does timing of ingestion matter? Endocrinol Metab Clin N Am. 2016;45:689–718.
Fong M, Caterson ID, Madigan CD. Are large dinners associated with excess weight, and does eating a smaller dinner achieve greater weight loss? A systematic review and meta-analysis. Br J Nutr. 2017;118:616–28.
Jiang P, Turek FW. Timing of meals: when is as critical as what and how much. Am J Physiol Endocrinol Metab. 2017;312:E369–E380.
McHill AW, Phillips AJ, Czeisler CA, et al. Later circadian timing of food intake is associated with increased body fat. Am J Clin Nutr. 2017;106:1213–9.
Lovato N, Micic G, Gradisar M, et al. Can the circadian phase be estimated from self-reported sleep timing in patients with delayed sleep wake phase disorder to guide timing of chronobiologic treatment? Chronobiol Int. 2016;33:1376–90.
Brown SA, Kunz D, Dumas A, et al. Molecular insights into human daily behavior. Proc Natl Acad Sci USA. 2008;105:1602–7.
Munoz JSG, Canavate R, Hernandez CM, Cara-Salmeron V, Morante JJH. The association among chronotype, timing of food intake and food preferences depends on body mass status. Eur J Clin Nutr. 2017;71:736–42.
Lopez-Minguez J, Dashti HS, Madrid-Valero JJ, et al. Heritability of the timing of food intake. Clin Nutr. 2018. pii: S0261-5614(18)30113-4. https://doi.org/10.1016/j.clnu.2018.03.002.
Jakubowicz D, Barnea M, Wainstein J, Froy O. High caloric intake at breakfast vs. dinner differentially influences weight loss of overweight and obese women. Obesity (Silver Spring). 2013;21:2504–12.
National Cancer Institute Cancer Data Access System. IDATA Homepage. 2016. https://biometry.nci.nih.gov/cdas/idata/. Accessed 6 Sep 2017.
National Cancer Institute Division of Cancer Control & Population Sciences. Automated self-Administered 24-hour (ASA24®) dietary assessment tool. Bethesda, MD: NCI; 2017.
The Worldwide Experimental Platform. https://www.thewep.org/documentations/mctq/item/mctq-variables. Accessed 6 Mar 2018.
Hosmer DW, Lemeshow S. Applied logistic regression. 2nd ed. New York: Wiley; 2000.
van der Heijden AA, Hu FB, Rimm EB, van Dam RM. A prospective study of breakfast consumption and weight gain among U.S. men. Obesity (Silver Spring). 2007;15:2463–9.
Purslow LR, Sandhu MS, Forouhi N, et al. Energy intake at breakfast and weight change: prospective study of 6,764 middle-aged men and women. Am J Epidemiol. 2008;167:188–92.
Baron KG, Reid KJ, Kern AS, Zee PC. Role of sleep timing in caloric intake and BMI. Obesity (Silver Spring). 2011;19:1374–81.
Duffy JF, Dijk DJ, Hall EF, Czeisler CA. Relationship of endogenous circadian melatonin and temperature rhythms to self-reported preference for morning or evening activity in young and older people. J Investig Med. 1999;47:141–50.
Mongrain V, Lavoie S, Selmaoui B, Paquet J, Dumont M. Phase relationships between sleep–wake cycle and underlying circadian rhythms in morningness-eveningness. J Biol Rhythms. 2004;19:248–57.
Scheer FA, Morris CJ, Shea SA. The internal circadian clock increases hunger and appetite in the evening independent of food intake and other behaviors. Obesity (Silver Spring). 2013;21:421–3.
Asher G, Schibler U. Crosstalk between components of circadian and metabolic cycles in mammals. Cell Metab. 2011;13:125–37.
Kessler K, Hornemann S, Petzke KJ, et al. The effect of diurnal distribution of carbohydrates and fat on glycaemic control in humans: a randomized controlled trial. Sci Rep. 2017;7:44170.
Shea SA, Hilton MF, Hu K, Scheer FA. Existence of an endogenous circadian blood pressure rhythm in humans that peaks in the evening. Circ Res. 2011;108:980–4.
Acknowledgements
We thank the National Cancer Institute for access to NCI’s data collected by the Interactive Diet and Activity Tracking in AARP (IDATA) study. The statements contained herein are solely those of the authors and do not represent or imply concurrence or endorsement by NCI. MG was supported in part by The Spanish Government of Investigation, Development and Innovation (SAF2017-84135-R) including FEDER co-funding, and NIH grant R01DK105072 (to MG). FAJLS was supported in part by NIH grants R01HL094806, R01HL118601, R01DK099512, R01DK102696, R01HL140574, and R01DK105072 (to FAJLS).
Author contributions
QX, FAJLS, and MG designed research; QX analyzed data; QX, FAJLS, and MG wrote paper; QX had primary responsibility for final content. All authors read and approved the final manuscript.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
FAJLS received speaker fees from Bayer Healthcare, Sentara Healthcare, Philips, Kellogg Company, Vanda Pharmaceuticals, and Pfizer. The other authors declare that they have no conflict of interest.
Supplementary information
Rights and permissions
About this article
Cite this article
Xiao, Q., Garaulet, M. & Scheer, F.A.J.L. Meal timing and obesity: interactions with macronutrient intake and chronotype. Int J Obes 43, 1701–1711 (2019). https://doi.org/10.1038/s41366-018-0284-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-018-0284-x
This article is cited by
-
The impact of dietary and sleep rhythms on blood pressure in children and adolescents: a cross-sectional study
Hypertension Research (2024)
-
Alignment between timing of ‘highest caloric intake’ and chronotype in relation to body composition during adolescence: the DONALD Study
European Journal of Nutrition (2024)
-
Association of meal timing with body composition and cardiometabolic risk factors in young adults
European Journal of Nutrition (2023)
-
Association between CLOCK 3111 T/C polymorphism with ghrelin, GLP-1, food timing, sleep and chronotype in overweight and obese Iranian adults
BMC Endocrine Disorders (2022)
-
Circadian timing of eating and BMI among adults in the American Time Use Survey
International Journal of Obesity (2022)