Abstract
The ultimate goal of neonatal nutrition care is optimal growth, neurodevelopment, and long-term health for preterm babies. International consensus is that increased energy and protein intakes in the neonatal period improve growth and neurodevelopment, but after more than 100 y of research the optimum intakes of energy and protein remain unknown. We suggest an important factor contributing to the lack of progress is the lack of a standardized approach to reporting nutritional intake data and growth in the neonatal literature. We reviewed randomized controlled trials and observational studies documented in MEDLINE and the Web of Science from 2008 to 2015 that compared approximately 3 vs. 4 g.kg–1.d–1 protein for preterm babies in the first month after birth. Consistency might be expected in the calculation of nutritional intake and assessment of growth outcomes in this relatively narrow scope of neonatal nutrition research. Twenty-two studies were reviewed. There was substantial variation in methods used to estimate and calculate nutritional intakes and in the approaches used in reporting these intakes and measures of infant growth. Such variability makes comparisons amongst studies difficult and meta-analysis unreliable. We propose the StRONNG Checklist—Standardized Reporting Of Neonatal Nutrition and Growth to address these issues.
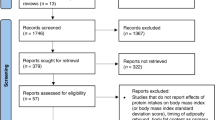
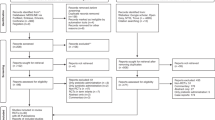
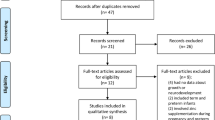
Similar content being viewed by others
Main
For preterm babies, nutrition in early life is now recognized as a key determinant of improving neonatal outcomes: survival; optimal growth; neurodevelopment, and long-term health (1). Ever since the “gavage” feeding of preterm babies began in the late 19th century and nutritional intake could be determined by neonatal staff rather than the baby, we have faced the dilemma of the nutrition required to achieve these goals (2).
Early 20th century metabolic studies estimated the energy and protein requirements of late preterm babies, but despite over 1,000 publications on neonatal nutrition and growth, a 2014 review of clinical trials on parenteral nutrition for extremely preterm babies concluded that the “cardinal unresolved questions are the optimal protein and energy intakes and the growth velocity that is predictive of optimal long-term health (3).” There is broad consensus that the target for growth of the preterm baby should be to match intrauterine growth of the normal human fetus. To achieve this, we need to know, first, what this growth looks like in terms of not only weight but also other measures of growth, including body composition, and, secondly, the nutritional requirements needed for this growth to be realized. This review will consider these critical questions and will propose that a standardized approach to reporting data will aid progress toward answering these unresolved questions.
The many different approaches taken to reporting nutritional intake data and growth in the neonatal literature make addressing these questions through interpretation of the data difficult. To investigate the variability in reporting, we identified and reviewed recent randomized controlled trials and observational studies documented in MEDLINE and the Web of Science from 2008 to 2015 that compared approximately 3 vs. 4 g.kg–1.d–1 protein for preterm babies in the first month after birth. Consistency might be expected in the calculation of nutritional intake and assessment of growth outcomes in this relatively narrow scope of research. Twenty-two studies were reviewed. Many of the studies did not cite the reference for the breast-milk nutrient composition data used to calculate nutritional intakes or, in some cases, even what these figures were ( Table 1 ). Where composition data were provided, there was a range of different figures for the composition of breast milk and intravenous nutrition and intakes were presented in a variety of ways ( Table 1 ). Assessment of growth also was undertaken over varied time periods, using different growth references and several methods of calculating growth ( Table 2 and Supplementary Table S1 online). It is difficult to find even two studies where the same references or methods have been used to determine nutritional intake or growth outcomes ( Tables 1 and 2 ; Supplementary Table S1 online). These differences make the body of neonatal nutrition research challenging to interpret and meta-analysis difficult to perform. Given that many studies are of small size, meta-analysis and Individual Participant Data meta-analysis would enhance interpretation of these data. Meta-analysis would be much more robust if there were an agreed upon set of international guidelines for standardized methodology and reporting of neonatal nutrition and growth outcomes. In this review, we present further analysis of the differences, discussion of potential solutions, and a standardization checklist for neonatal nutrition research.
What do we need to know?
Determining the optimal nutritional requirements of preterm babies requires an agreed reference standard for growth and other outcomes. In 1977, the recommendation of the American Academy of Pediatrics was “to achieve postnatal growth and body composition equivalent to those of normally growing, healthy human fetuses of the same gestational age” (4). Some doubt remains as to whether this is the appropriate goal; however, in the absence of an alternative based on evidence, this remains a reasonable target, albeit one that is not met by the majority of preterm babies (5).
For research to address the best means of achieving this goal, we need to know:
-
1. The growth that would have occurred in utero
-
2. The body composition the baby would have had if he/she had remained in utero
-
3. The nutrient intake required to achieve the first two
The Growth That Would Have Occurred In Utero
Babies born preterm are more likely to be growth-restricted compared with their gestational-age matched peers who remain in utero and are born at term (6), with up to 40% of preterm babies having some evidence of intrauterine growth restriction (7). Therefore, postnatal growth of preterm babies ideally should be monitored against a standard based on measurements of normally growing fetuses in utero at the same gestational age, rather than cross-sectional data from preterm births. Various methods have been developed for estimating fetal weight in utero with at least 35 different formulae available. These estimates have been found to be relatively accurate at predicting birth weight up to 3,500 g with 80% of estimated fetal weights within 10% of birthweight (8). Fetal head circumference and biparietal diameter can be measured by ultrasound; however, there are no reliable references for fetal length.
The INTERGROWTH 21st study (9) provides the most consistent standards for fetal growth and size at birth, using data from carefully selected and standardized participants in eight geographically defined urban populations in whom health and nutritional needs were met and adequate antenatal care was provided. Fetal growth and newborn size were measured using prespecified markers and the same methods, equipment, and selection criteria. However, as few data from babies born between 23 and 33 wk were available, the INTERGROWTH-21st curves begin at 33 wk postmenstrual age and even in the moderately preterm gestations the numbers of babies born at each gestational age is small. Thus, these charts are not suitable for the monitoring of growth in babies born at moderately preterm or earlier gestations.
Customized centile charts for intrauterine growth, adjusting for maternal size, ethnicity, and other variables such as prior birth weight, have been developed to improve the detection of intrauterine growth restriction. There is considerable debate over whether such charts are preferable to international standards (10). Furthermore, customized charts only provide a customized fetal weight centile, ignoring the very important length and head circumference variables, and were not developed to assess birthweight or longitudinal postnatal growth. Given the importance of linear growth in preterm babies to ensure proportional growth and head circumference growth, which is correlated with brain growth (11), it is difficult to support the use of customized fetal growth charts for monitoring postnatal growth.
Comparison of Potential Growth Curves. In practice, therefore, the postnatal growth of most preterm babies is monitored using growth charts derived from cross-sectional data of babies born preterm. Two international standards commonly used for assessing the growth of preterm infants from around 23 wk postmenstrual age (PMA) and for calculation of Z-scores are the UK 1990 (12) and Fenton 2013 (13) datasets. The essential features of these datasets and INTERGROWTH 21st are summarized in Table 3 . Both the UK 1990 and Fenton 2013 datasets have been developed based on cross-sectional data from preterm births and linked to the World Health Organization (WHO) post-term growth standard (14). The UK-WHO growth curves were designed for assessing preterm infants from 23 wk postmenstrual age to 2 y corrected age using a combination of UK 1990 and WHO data (15). The Fenton 2013 growth curves use a more recent and much larger sample of cross-sectional data of preterm births which link to the WHO growth data from birth to 10 wk post-term (16).
For weight, the UK-WHO, INTERGROWTH 21st and Fenton 2013 data sets are similar. The slightly lower Fenton 2013 curves may be explained by the Fenton data being derived from actual PMA in weeks and days and the UK–1990 for completed weeks. Thus, fewer babies would be classified as small-for-gestational-age (SGA) between 24 and 34 wk PMA compared with the WHO curves. The Fenton dataset for weight is over 400 times larger than the UK-WHO dataset which includes few data for births from 32–35 wk PMA. From approximately 38–42 wk, the slope of the INTERGROWTH-21st and UK-WHO curves dip in comparison with Fenton 2013 reflecting the slower growth in utero that occurs just prior to term (17). The Fenton data have been statistically smoothed as they link to WHO data around 40 wk to avoid this dip. Given that the slowing of intrauterine growth prior to term is a feature of the birth-related maturational and hormonal changes, (18) there is no good reason why babies born preterm should follow this dip in growth trajectory and a smoothed transition is perhaps more appropriate for both clinical practice and research purposes (13).
The more striking difference for length and head circumference amongst the Fenton 2013, INTERGROWTH-21st and UK-1990 curves may be contributed to by a substantially larger sample, especially at lower gestations (12,13) in the Fenton dataset (e.g., for babies <30 wk gestation n = 12,000 vs. 146 in the UK-WHO), more accurate estimation of gestational age at birth and more contemporary data in the Fenton dataset.
Use of SD (Z-Scores or ΔZ-Scores). Z-scores express an anthropometric value such as weight, length, or head circumference for age or weight for height as a number of SDs below or above the reference population mean or median value. The Z-score is widely recognized as the best system for presentation and analysis of anthropometric data (19).
The recommended formula for calculating the Z-score is the Lambda Mu Sigma method using data from an appropriate published dataset (20). A negative Z-score change indicates a decline in growth status, a positive Z-score change is an increase in growth status, or a Z-score change of zero is a stable or unchanged growth status. Therefore, Z-score change rather than Z-score alone is preferable to evaluate the effect of nutrition interventions on growth (21). The potential effect of the choice of dataset on the evaluation of growth is demonstrated in Figure 1 comparing Z-scores for the same lengths calculated with the UK-WHO vs. Fenton 2013 dataset. Linear growth in this case would be considered appropriate if using the UK-WHO data but faltering if using the Fenton 2013 dataset.
Comparison of Z-score change between the UK-WHO and Fenton 2013 datasets. Linear growth would be considered appropriate with the UK-WHO data (squares: no change in z-score) but faltering with the Fenton 2013 dataset (circles: a decrease of ~1 z-score). Differences below 30 wk postmenstrual age (PMA) are likely due to more recent data with better estimation of gestational age and a substantially larger sample size in the Fenton data (<30 wk PMA 12,000 vs. 146 in UK-WHO). Differences near term are likely to be due to the smoothing of the Fenton charts from prenatal growth to postnatal growth data, taking account of the slowing of intrauterine growth near term that one would not expect to see in preterm babies at the same corrected gestational age.
However, if z-scores are used to report growth, it is important to be cognisant of the entry criteria for babies to be enrolled in the study. Studies in extremely preterm babies often use either a GA criterion, a birthweight criterion or both (below a certain GA AND/OR below a certain birthweight). If a GA criterion alone is used, one would expect the z score distribution to approximate normality; however, if birthweight alone or a combined criterion are used, this may not be the case as smaller, more mature babies will be included and larger, less mature babies will not, skewing the z-score distribution.
It also is important to note the normal contraction of the extracellular fluid space after birth means that some downward tracking of z-score between birth and a later time point is expected. This has led some researchers to report change in growth from the nadir in weight, or from regain in birthweight, or from birth. However, unless babies are weighed daily to delineate accurately the day of maximum weight loss or of regain in birthweight, these approaches will lead to further inaccuracies. Further, postnatal weight loss and duration of poor growth immediately after birth is minimized with optimal nutrition. Some researchers report growth from birth, while others report growth from the day birthweight is regained ( Table 2 ). Therefore, for consistency of reporting, we recommend reporting growth from birth, a clearly defined, consistent time-point, with the understanding that for weight loss of ECF fluid should be borne in mind.
Choice of a Reference Dataset. For consistency in attribution of SGA status, determination of Z-scores, and assessment of Z-score change over time, an agreed international dataset would be of great value. Given that INTERGROWTH-21st does not have data prior to 33 wk, and small numbers at 33 and 34 wk, and that the UK-WHO data are older and also based on much smaller numbers, beginning at 24 wk when there are increasing numbers of survivors at gestations below that, the Fenton 2013 dataset may be the best currently available option. It also has the benefit of smoothing at term gestations to avoid a dip at this time.
Recommendations:
-
Measure growth from birth, rather than from a nadir or from the time when birthweight was regained
-
Growth reference for preterm infants—Fenton 2013
-
Growth reported as Z-scores and Z-score change to indicate growth status alterations over time
Reporting of Weight Velocity. Currently, there is no standardized approach to the calculation of growth velocity, generally reported as weight gain in g.kg−1.d−1. Thirteen of the 22 studies in Table 2 reported Z-scores and seven reported Z-score change rather than weight gain. Fourteen studies reported weight velocity in g.kg−1.d−1 but seven did not specify how this was calculated.
Seven specified how weight velocity was calculated but used three different methods:
-
1. Net weight gain over the time interval divided by the time interval and birth weight
-
2. Net weight gain over the time interval divided by the time interval and the mean of birth weight and weight at day x
-
3. Exponential method for calculation of weight velocity reported by Patel (22)
The difference between these methods has been estimated to be 42% over 39 d (23). Researchers should state the method used when reporting weight gain. Patel’s method is validated to assess the growth of ELBW and VLBW infants and provides a simple-to-use and consistent approach (13).
Recommendation:
-
Exponential method for calculation of weight velocity (22)
The Body Composition the Baby Would Have Had If He/She Had Remained In Utero
Growth patterns in early postnatal life and body composition have important consequences for metabolic and cardiovascular health in later life (24,25). At term-corrected age, preterm babies are significantly shorter, lighter, and have smaller head circumferences than those born at full-term (6,26). Several studies now have demonstrated that very preterm babies also have a different body composition at term-corrected age when compared with babies born at term (6,27,28), with substantially less lean body mass (mean difference, 460 g) but a similar fat mass (6). Thus, they also have a higher per cent fat mass. Both body size and composition relate to the risk of noncommunicable diseases in later life (29); therefore, understanding how the growth of preterm infants can be modified to aim for a body composition at term-corrected age that is similar to that of babies born at term may be important for optimizing life-long health (30,31).
Body composition and particularly changes in lean body mass are difficult to measure accurately in very small preterm babies. Several indirect in vivo techniques have been evaluated including bioelectrical impedance analysis, dual-energy x-ray absorptiometry, MRI and use of stable isotopes, such as deuterium oxide dilution (32). Issues of complexity, expense, and ease of use that are beyond the scope of this article mean that none of these is practical for routine measurement of preterm babies. However, recently, it has become possible to measure fat or lean body mass routinely in the neonatal intensive care unit using air displacement plethysmography (ADP) (33); this now is standard practice in some neonatal units, although infants need to be free from significant interventions such as CPAP or ventilation. With ADP, measurements of infant mass and volume, determined by air displacement, are used to estimate whole-body density (i.e., mass/volume). Published reference models for the densities of lean body mass and fat mass from multi-component studies and standard assumptions about the densities of fat and lean tissue are used to derive the fraction of fat in body weight (34).
However, even ADP is not available in most units, meaning that weight gain is therefore often used as a proxy for growth, with much less consideration paid to length and head growth. It is relatively easy to improve the postnatal weight gain of preterm babies with additional energy in the form of glucose polymers or fat added to enteral feeds, but this may only increase fat mass rather than the intended increase in lean body mass (35,36). At present, simple anthropometric measurements using all three growth parameters and not just weight are the most reliable and readily available growth parameters for preterm babies (37).
Recommendation:
-
Weight, length, and head circumference reported weekly
-
Raw data for lean body mass, fat mass, and other measurements should be reported.
-
In future, an agreed upon lean body/ fat mass index would be useful
The Nutrient Intake Required To Achieve the Growth and Body Composition That Would Have Occurred If the Baby Had Remained In Utero
Recommended Energy and Protein Intakes. The primary modifiable influence on postnatal growth is nutrition, although other factors such as disease, environment, and genetics also play a role (38,39). Research to date has focused on the energy and protein intake required to achieve intrauterine growth and international consensus groups have made recommendations based on this research ( Table 4 ). These recommendations are based on studies that showed increased protein accretion with increased protein intake and that even a small deficit in protein intake impairs both lean body mass accretion and linear growth (40), although the level of evidence is not high.
In reality, many neonatal units (41) and even clinical trials (42) struggle to reach these recommendations, and therefore, it is important that actual intakes are always reported in addition to prescribed or intended intake. Similarly, it is important that the source used to calculate nutritional intakes is referenced.
Basis for the Calculation of Energy and Protein Intake Parenteral Solutions. The nutrient composition figures used to calculate energy and amino acid intake from parenteral solutions often are not reported, with the consequence that there may be variation that is not apparent. For example, including the energy content of glycerol and added vitamins in the energy calculation for lipid gives 10 rather than 9 kcal/ g lipid; some authors use 9 kcal per g for enteral fat and 10 kcal per g for parenteral fat (43). For carbohydrate (dextrose) some authors use 3.4 kcal per g because dextrose datasheets state that 1 g of dextrose contains 3.4 kcal, whereas others use the Atwater factor of 4 kcal per gm (44).
Further inaccuracy can occur in the conversion of lipid emulsion to fat, with 5 ml lipid emulsion often considered to provide 1 g fat. However, vitamin solutions commonly added to 20% lipid emulsions are in 10% lipid; therefore, addition of 25 ml vitamins to 100 ml of 20% lipid emulsion effectively reduces the solution to a 17.5% lipid emulsion containing 0.88 g fat/5 ml and not 1 g fat/5 ml.
Recommendation: All figures used for calculations are specified and suggest:
-
Enteral protein: 4 kcal.g–1
-
Enteral carbohydrate: 4 kcal.g–1
-
Enteral fat: 9 kcal.g–1
-
Parenteral amino acids: 4 kcal.g–1
-
Parenteral dextrose: 3.4 kcal.g–1
-
Parenteral lipid: 10 kcal.g–1
-
Parenteral lipid with vitamins as per manufacturer (e.g., 0.88 g fat per 5 ml lipid emulsion)
Enteral Solutions. In the 22 studies reviewed, various assumptions were made when calculating nutrient intake:
Bioavailability of Enteral vs. Parenteral Nutrients
Parenteral nutrition bypasses the usual process of eating and digestion. As the intestines consume a significant proportion of the diet for the growth and energy of the intestines themselves, the recommended intakes of parenteral nutrition are usually lower than for enteral nutrition, e.g., 3.5 to 4 g.kg−1.d−1 parenteral vs. 4–4.5 g.kg−1.d−1enteral protein for ELBW babies ( Table 4 ). In the first week after birth, parenteral nutrition provides the majority of nutritional intake but up to 50% may be enteral. For statistical analysis of total protein intake in the first week where a comparison with the recommended parenteral protein intake for instance is required, some researchers use a bioavailability factor to convert enteral protein intake to a parenteral equivalent to compare total intake (parenteral + enteral) with parenteral recommendations. According to some authors, this factor ranges from 81 to 87% for fortified human milk and from 86 to 94% for infant formula (45). Fanaro assumed 88% (46), but Tan et al. (47) and Rochow et al. (48) all assumed 85% absorption of enteral protein. However, stable isotope studies have shown that protein digestion and absorption is almost 100% in infants (49), but that fecal nitrogen is derived from endogenous synthesized (glycol-) proteins, sloughed-off cells and bacterial products. There is variation in the bioavailability of different nutrients, i.e., energy vs. protein vs. micronutrients, which is also affected by the nature of the enteral solution, e.g., breast milk vs. fortified breast milk vs. infant formula. In many cases, the actual bioavailability is unknown; therefore, we suggest no adjustment is made for this until there is definitive evidence of the bioavailability of specific nutrients in breast milk and other milks and nutritional supplements for preterm infants.
Loss of Enteral Feed Volume in Feeding Tubes and Via Gastric Reflux
This refers to the proportion of enteral intake that is actually available for digestion by the gut. It takes into account enteral absorption, loss of milk in feeding tubes, and gastric reflux. Some authors consider 100% of enteral feeds to be absorbed and others only 75% (including 85% bioavailability of enteral vs. parenteral nutrients) (48). There is little evidence to support this practice and it would be difficult to measure accurately the volume of feed that is digested and absorbed; therefore, it may be better just to report the total enteral volume administered.
Recommendation:
-
Calculation and reporting of parenteral and enteral protein and energy intakes separately where possible
-
Enteral protein and energy should be considered 100% bioavailable, and calculations should be based on administered volumes
Nutritional Composition of Breast Milk. Own mothers’ breast milk is the feed of choice for preterm babies. However, the composition of breast milk is dynamic. The concentration of both energy and protein in expressed breast milk is highly variable throughout lactation and between individuals (50). The analysis of human milk can also be influenced by methods of expression and storage and pasteurization. Published studies of breast-milk composition involve nonstandardized collection with varying attention to storage and processing conditions resulting in substantial variation in reported nutritional composition (50,51). Any calculation of energy and protein intake from breast milk is merely an estimation (52).
Table 1 shows the variation in breast-milk composition figures used in recent neonatal nutrition and growth studies. The energy range is from 64 to 72 kcal.100 ml−1. The range for protein was even larger (0.8–2.4 g.100 ml-1).
Although the precise nutritional content of the breast milk administered to each baby in each study is unknown, the use of standardized figures for breast-milk composition would improve both the comparability of studies and the likelihood of finding optimal protein and energy intakes for preterm babies.
Recommendation:
-
The energy, protein, carbohydrate, and fat concentrations per 100 ml of breast milk used to calculate nutritional intakes are reported
-
Energy and protein intakes are calculated and reported using either actual breastmilk analysis figures (stating the methodology used) or standardized preterm transitional breastmilk composition for 14 d (65 kcal and 1.5 g protein.100 ml−1) and mature breastmilk composition thereafter (72 kcal and 1.2 g protein.100 ml−1) (53,54,55,56,57)
We have formulated our recommendations into a the StRONNG Checklist - Standardized Reporting Of Neonatal Nutrition and Growth, which provides guidelines for standardized reporting of nutritional intakes and growth in neonatal populations ( Table 5 ).
Conclusion
Methodological heterogeneity underlies the body of neonatal nutrition and growth literature. Before we can determine accurately the effects of nutritional interventions and whether or not the observed anthropometric or body composition differences reflect improved short- and long-term outcomes, standardization of nutritional composition, statistical methods, growth standards, and reporting of outcomes is required. This is essential to improve the quality and usefulness of clinical trials in neonatal nutrition and enable true meta-analysis of the results.
Author Contributions
B.C. conceived the review and F.B. participated in its design. B.C. and F.B. drafted the manuscript and all authors contributed to and approved the final manuscript.
Statement of Financial Support
B.C. is supported by a grant from Gravida: National Centre for Growth and Development, Auckland, New Zealand. The authors have no other conflicts of interest to disclose.
Disclosure
The authors declare that they have no competing interests.
References
Ong KK. Catch-up growth in small for gestational age babies: good or bad? Curr Opin Endocrinol Diabetes Obes 2007;14:30–4.
Dunn PM. Stéphane Tarnier (1828-1897), the architect of perinatology in France. Arch Dis Child Fetal Neonatal Ed 2002;86:F137–9.
Uthaya S, Modi N. Practical preterm parenteral nutrition: systematic literature review and recommendations for practice. Early Hum Dev 2014;90:747–53.
American Academy of Pediatrics, Committee on Nutrition. Nutritional needs of low-birth-weight infants. Pediatrics 1977;60:519–30.
Horbar JD, Ehrenkranz RA, Badger GJ, et al. Weight growth velocity and postnatal growth failure in infants 501 to 1500 grams: 2000–2013. Pediatrics 2015;136:e84–92.
Johnson MJ, Wootton SA, Leaf AA, Jackson AA. Preterm birth and body composition at term equivalent age: a systematic review and meta-analysis. Pediatrics 2012;130:e640–9.
Cooke RJ. Postnatal growth and development in the preterm and small for gestational age infant. In: Lucas A, Makrides M, Ziegler EE, eds. Importance of Growth for Health and Development. Basel: Nestle´ Nutrition Institute; 2010:85–95.
Scioscia M, Vimercati A, Ceci O, Vicino M, Selvaggi LE. Estimation of birth weight by two-dimensional ultrasonography: a critical appraisal of its accuracy. Obstet Gynecol 2008;111:57–65.
Villar J, Cheikh Ismail L, Victora CG, et al.; International Fetal and Newborn Growth Consortium for the 21st Century (INTERGROWTH-21st). International standards for newborn weight, length, and head circumference by gestational age and sex: the Newborn Cross-Sectional Study of the INTERGROWTH-21st Project. Lancet 2014;384:857–68.
Bertino E, Milani S, Fabris C, De Curtis M. Neonatal anthropometric charts: what they are, what they are not. Arch Dis Child Fetal Neonatal Ed 2007;92:F7–F10.
Cooke RW, Lucas A, Yudkin PL, Pryse-Davies J. Head circumference as an index of brain weight in the fetus and newborn. Early Hum Dev 1977;1:145–9.
Cole TJ, Williams AF, Wright CM ; RCPCH Growth Chart Expert Group. Revised birth centiles for weight, length and head circumference in the UK-WHO growth charts. Ann Hum Biol 2011;38:7–11.
Fenton TR, Kim JH. A systematic review and meta-analysis to revise the Fenton growth chart for preterm infants. BMC Pediatr 2013;13:59.
de Onis M, Onyango AW. WHO child growth standards. Lancet 2008;371:204.
Cole TJ, Wright CM, Williams AF ; RCPCH Growth Chart Expert Group. Designing the new UK-WHO growth charts to enhance assessment of growth around birth. Arch Dis Child Fetal Neonatal Ed 2012;97:F219–22.
Fenton TR. A new growth chart for preterm babies: Babson and Benda’s chart updated with recent data and a new format. BMC Pediatr 2003;3:13.
Rosso P, Cramoy C. Nutrition and Pregnancy. In: Willick M, ed. Nutrition Pre-and Postnatal Development. 1st edn. New York: Plenum Press; 1979:143–4.
Fenton TR, Nasser R, Eliasziw M, Kim JH, Bilan D, Sauve R. Validating the weight gain of preterm infants between the reference growth curve of the fetus and the term infant. BMC Pediatr 2013;13:92.
Physical status: the use and interpretation of anthropometry. Report of a WHO Expert Committee. WHO Technical Report Series No. 854. Geneva: World Health Organization, 1995.
Cole TJ, Green PJ. Smoothing reference centile curves: the LMS method and penalized likelihood. Stat Med 1992;11:1305–19.
de Onis M, Blossner M. The Z-Score or Standard Classification System. WHO Global Database on Child Growth and Malnutrition, Geneva. 1997:56–9.
Patel AL, Engstrom JL, Meier PP, Kimura RE. Accuracy of methods for calculating postnatal growth velocity for extremely low birth weight infants. Pediatrics 2005;116:1466–73.
Senterre T, Rigo J. Reduction in postnatal cumulative nutritional deficit and improvement of growth in extremely preterm infants. Acta Paediatr 2012;101:e64–70.
Hofman PL, Regan F, Jackson WE, et al. Premature birth and later insulin resistance. N Engl J Med 2004;351:2179–86.
Wells JC. The thrifty phenotype: An adaptation in growth or metabolism? Am J Hum Biol 2011;23:65–75.
Uthaya S, Thomas EL, Hamilton G, Doré CJ, Bell J, Modi N. Altered adiposity after extremely preterm birth. Pediatr Res 2005;57:211–5.
Roggero P, Giannì ML, Amato O, et al. Is term newborn body composition being achieved postnatally in preterm infants? Early Hum Dev 2009;85:349–52.
Ramel SE, Gray HL, Ode KL, Younge N, Georgieff MK, Demerath EW. Body composition changes in preterm infants following hospital discharge: comparison with term infants. J Pediatr Gastroenterol Nutr 2011;53:333–8.
Li Y, Ley SH, Tobias DK, et al. Birth weight and later life adherence to unhealthy lifestyles in predicting type 2 diabetes: prospective cohort study. BMJ 2015;351:h3672.
Wells JC, Chomtho S, Fewtrell MS. Programming of body composition by early growth and nutrition. Proc Nutr Soc 2007;66:423–34.
Eriksson JG, Forsén T, Tuomilehto J, Osmond C, Barker DJ. Early growth and coronary heart disease in later life: longitudinal study. BMJ 2001;322:949–53.
Demerath EW, Fields DA. Body composition assessment in the infant. Am J Hum Biol 2014;26:291–304.
Ellis KJ, Yao M, Shypailo RJ, Urlando A, Wong WW, Heird WC. Body-composition assessment in infancy: air-displacement plethysmography compared with a reference 4-compartment model. Am J Clin Nutr 2007;85:90–5.
Butte NF, Hopkinson JM, Wong WW, Smith EO, Ellis KJ. Body composition during the first 2 years of life: an updated reference. Pediatr Res 2000;47:578–85.
Romera G, Figueras J, Rodríguez-Miguélez JM, Ortega J, Jiménez R. Energy intake, metabolic balance and growth in preterm infants fed formulas with different nonprotein energy supplements. J Pediatr Gastroenterol Nutr 2004;38:407–13.
Kashyap S, Ohira-Kist K, Abildskov K, et al. Effects of quality of energy intake on growth and metabolic response of enterally fed low-birth-weight infants. Pediatr Res 2001;50:390–7.
Koo WW. Body composition measurements during infancy. Ann N Y Acad Sci 2000;904:383–92.
Embleton NE, Pang N, Cooke RJ. Postnatal malnutrition and growth retardation: an inevitable consequence of current recommendations in preterm infants? Pediatrics 2001;107:270–3.
Stoltz Sjöström E, Öhlund I, Ahlsson F, et al. Nutrient intakes independently affect growth in extremely preterm infants: results from a population-based study. Acta Paediatr 2013;102:1067–74.
Wauben I, Westerterp K, Gerver WJ, Blanco C. Effect of varying protein intake on energy balance, protein balance and estimated weight gain composition in premature infants. Eur J Clin Nutr 1995;49:11–6.
Lapillonne A, Kermorvant-Duchemin E. A systematic review of practice surveys on parenteral nutrition for preterm infants. J Nutr 2013;143(12 Suppl):2061S–5S.
Burattini I, Bellagamba MP, Spagnoli C, et al.; Marche Neonatal Network. Targeting 2.5 versus 4 g/kg/day of amino acids for extremely low birth weight infants: a randomized clinical trial. J Pediatr 2013;163:1278–82.e1.
Moltu SJ, Blakstad EW, Strømmen K, et al. Enhanced feeding and diminished postnatal growth failure in very-low-birth-weight infants. J Pediatr Gastroenterol Nutr 2014;58:344–51.
Miller J, Makrides M, Gibson RA, et al. Effect of increasing protein content of human milk fortifier on growth in preterm infants born at <31 wk gestation: a randomized controlled trial. Am J Clin Nutr 2012;95:648–55.
Rigo J. Nutritional needs of prermature infants: current issues J Pediatr 2006;149:S80–S8.
Fanaro S, Ballardini E, Vigi V. Different pre-term formulas for different pre-term infants. Early Hum Dev 2010;86 Suppl 1:27–31.
Tan MJ, Cooke RW. Improving head growth in very preterm infants–a randomised controlled trial I: neonatal outcomes. Arch Dis Child Fetal Neonatal Ed 2008;93:F337–41.
Rochow N, Fusch G, Mühlinghaus A, et al. A nutritional program to improve outcome of very low birth weight infants. Clin Nutr 2012;31:124–31.
Shulman RJ, Gannon N, Reeds PJ. Cereal feeding and its impact on the nitrogen economy of the infant. Am J Clin Nutr 1995;62:969–72.
Zachariassen G, Fenger-Gron J, Hviid MV, Halken S. The content of macronutrients in milk from mothers of very preterm infants is highly variable. Dan Med J 2013;60:A4631.
Ballard O, Morrow AL. Human milk composition: nutrients and bioactive factors. Pediatr Clin North Am 2013;60:49–74.
Weber A, Loui A, Jochum F, Bührer C, Obladen M. Breast milk from mothers of very low birthweight infants: variability in fat and protein content. Acta Paediatr 2001;90:772–5.
Lönnerdal B, Forsum E, Hambraeus L. A longitudinal study of the protein, nitrogen, and lactose contents of human milk from Swedish well-nourished mothers. Am J Clin Nutr 1976;29:1127–33.
Anderson GH, Atkinson SA, Bryan MH. Energy and macronutrient content of human milk during early lactation from mothers giving birth prematurely and at term. Am J Clin Nutr 1981;34:258–65.
Fomon SJ. Requirements and recommended dietary intakes of protein during infancy. Pediatr Res 1991;30:391–5.
Butte NF, Garza C, Johnson CA, Smith EO, Nichols BL. Longitudinal changes in milk composition of mothers delivering preterm and term infants. Early Hum Dev 1984;9:153–62.
Arslanoglu S, Moro GE, Ziegler EE. Preterm infants fed fortified human milk receive less protein than they need. J Perinatol 2009;29:489–92.
Morgan C, McGowan P, Herwitker S, Hart AE, Turner MA. Postnatal head growth in preterm infants: a randomized controlled parenteral nutrition study. Pediatrics 2014;133:e120–8.
Schanler R, Atkinson SA. Human milk. In: Tsang RC, ed. Nutrition of the Preterm Infant: Scientific Basis and Practical Guidelines. 2nd edn. Cincinnati, OH: Digital Education Publishing; 2005:333–56.
Olsen IE, Harris CL, Lawson ML, Berseth CL. Higher protein intake improves length, not weight, z scores in preterm infants. J Pediatr Gastroenterol Nutr 2014;58:409–16.
Gross SJ. Growth and biochemical response of preterm infants fed human milk or modified infant formula. N Engl J Med 1983;308:237–41.
Bolisetty S, Pharande P, Nirthanakumaran L, et al. Improved nutrient intake following implementation of the consensus standardised parenteral nutrition formulations in preterm neonates–a before-after intervention study. BMC Pediatr 2014;14:309.
Vlaardingerbroek H, Vermeulen MJ, Rook D, et al. Safety and efficacy of early parenteral lipid and high-dose amino acid administration to very low birth weight infants. J Pediatr 2013;163:638–44.e1–5.
Loui A, Bührer C. Growth of very low birth weight infants after increased amino acid and protein administration. J Perinat Med 2013;41:735–41.
Aguayo J. Maternal lactation for preterm newborn infants. Early Hum Dev 2001;65 Suppl:S19–29.
Cormack BE, Bloomfield FH. Increased protein intake decreases postnatal growth faltering in ELBW babies. Arch Dis Child Fetal Neonatal Ed 2013;98:F399–404.
Xyris Software (Australia) Pty Ltd. FoodWorks Professional Version 5 Service pack 1 Build 1376. New Zealand 2007.
Scattolin S, Gaio P, Betto M, et al. Parenteral amino acid intakes: possible influences of higher intakes on growth and bone status in preterm infants. J Perinatol 2013;33:33–9.
Berseth CL, Van Aerde JE, Gross S, Stolz SI, Harris CL, Hansen JW. Growth, efficacy, and safety of feeding an iron-fortified human milk fortifier. Pediatrics 2004;114:e699–706.
Balasubramanian H, Nanavati RN, Kabra NS. Effect of two different doses of parenteral amino acid supplementation on postnatal growth of very low birth weight neonates, a randomized controlled trial. Indian Pediatr 2013;50:1131–6.
Ditzenberger GR, Wallen LD, Phelan L, Escoe S, Collins SD. Supplemental protein and postnatal growth of very low birth weight infants: a randomized trial. J Neonatal Perinatal Med 2013;6:285–94.
Biasini A, Marvulli L, Neri E, China M, Stella M, Monti F. Growth and neurological outcome in ELBW preterms fed with human milk and extra-protein supplementation as routine practice: do we need further evidence? J Matern Fetal Neonatal Med 2012;25 Suppl 4:72–4.
Moya F, Sisk PM, Walsh KR, Berseth CL. A new liquid human milk fortifier and linear growth in preterm infants. Pediatrics 2012;130:e928–35.
Blanco CL, Gong AK, Schoolfield J, et al. Impact of early and high amino acid supplementation on ELBW infants at 2 years. J Pediatr Gastroenterol Nutr 2012;54:601–7.
Can E, Bülbül A, Uslu S, Cömert S, Bolat F, Nuhoğlu A. Effects of aggressive parenteral nutrition on growth and clinical outcome in preterm infants. Pediatr Int 2012;54:869–74.
Newburg D, Neubauer S. Carbohydrates in milks: analysis, quantities and significance. In: Jensen R, ed. Handbook of Milk Composition. San Diago, CA: Academic Press; 1995:273–350.
Roggero P, Giannì ML, Orsi A, et al. Implementation of nutritional strategies decreases postnatal growth restriction in preterm infants. PLoS One 2012;7:e51166.
Costa-Orvay JA, Figueras-Aloy J, Romera G, Closa-Monasterolo R, Carbonell-Estrany X. The effects of varying protein and energy intakes on the growth and body composition of very low birth weight infants. Nutr J 2011;10:140.
Atkinson SA, Radde IC, Chance GW, Bryan MH, Anderson GH. Macro-mineral content of milk obtained during early lactation from mothers of premature infants. Early Hum Dev 1980;4:5–14.
Smolkin T, Diab G, Shohat I, et al. Standardized versus individualized parenteral nutrition in very low birth weight infants: a comparative study. Neonatology 2010;98:170–8.
Koletzko B, Goulet O, Hunt J, Krohn K, Shamir R ; Parenteral Nutrition Guidelines Working Group; European Society for Clinical Nutrition and Metabolism; European Society of Paediatric Gastroenterology, Hepatology and Nutrition (ESPGHAN); European Society of Paediatric Research (ESPR). 1. Guidelines on Paediatric Parenteral Nutrition of the European Society of Paediatric Gastroenterology, Hepatology and Nutrition (ESPGHAN) and the European Society for Clinical Nutrition and Metabolism (ESPEN), Supported by the European Society of Paediatric Research (ESPR). J Pediatr Gastroenterol Nutr 2005;41 Suppl 2:S1–87.
Tsang RC, Uauy R, Koletzko B, Zlotkin SH. Nutrition of the Preterm Infant: Scientific Basis and Practical Guidelines. 2nd edn.Cincinnati: Digital Education Publishing, Inc.; 2005;415–6.
Agostoni C, Buonocore G, Carnielli VP, et al.; ESPGHAN Committee on Nutrition. Enteral nutrient supply for preterm infants: commentary from the European Society of Paediatric Gastroenterology, Hepatology and Nutrition Committee on Nutrition. J Pediatr Gastroenterol Nutr 2010;50:85–91.
Koletzko B, Poindexter B, Uauy R. Recommended Nutrient Intake Levels for Stable, Fully Enterally Fed Very Low Birth Weight Infants. In: Koletzko B, Poindexter B, Uauy R, eds. Nutritional Care of Preterm Infants Scientific Basis and Practical Guidelines. Basel: Karger; 2014:297–9.
Author information
Authors and Affiliations
Corresponding author
Supplementary information
Supplementary Table
(DOC 137 kb)
PowerPoint slides
Rights and permissions
About this article
Cite this article
Cormack, B., Embleton, N., van Goudoever, J. et al. Comparing apples with apples: it is time for standardized reporting of neonatal nutrition and growth studies. Pediatr Res 79, 810–820 (2016). https://doi.org/10.1038/pr.2016.26
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pr.2016.26
This article is cited by
-
Intratracheal budesonide mixed with surfactant to increase survival free of bronchopulmonary dysplasia in extremely preterm infants: study protocol for the international, multicenter, randomized PLUSS trial
Trials (2023)
-
The influence of nutrition on white matter development in preterm infants: a scoping review
Pediatric Research (2023)
-
Body composition of extremely preterm infants fed protein-enriched, fortified milk: a randomized trial
Pediatric Research (2022)
-
Racial differences in growth rates and body composition of infants born preterm
Journal of Perinatology (2022)
-
Nephrocalcinosis in very low birth weight infants: incidence, associated factors, and natural course
Pediatric Nephrology (2022)