Abstract
Background:
Phototherapy using blue light is the treatment of choice worldwide for neonatal hyperbilirubinemia. However, treatment with turquoise light may be a desirable alternative. Therefore, the aim of this randomized, controlled study was to compare the bilirubin isomer distribution in serum of jaundiced neonates after 24 h of therapy with narrow-band (LED) light centered at 497 nm (turquoise) vs. 459 nm (blue), of essentially equal irradiance.
Materials:
Eighty-three neonates (≥33 wk gestational age) with uncomplicated hyperbilirubinemia were included in the study. Forty neonates were exposed to light centered at 497 nm and 43 infants with light centered at 459 nm. Irradiances were 5.2 × 1015 and 5.1 × 1015 photons/cm2/s, respectively.
Results:
After 24 h of treatment no significant differences in serum concentrations of total bilirubin isomers and Z,Z-bilirubin were observed between the 2 groups. Interestingly, concentrations of Z,E-bilirubin, and thus also total bilirubin isomers formed during therapy, were highest for infants receiving light centered at 459 nm, while the concentration of E,Z-bilirubin was highest for those receiving light centered at 497 nm. No significant difference was found between concentrations of E,Z-lumirubin.
Conclusion:
Therapy with LED light centered at 497 nm vs. 459 nm, applied with equal irradiance on the infants, resulted in a different distribution of bilirubin isomers in serum.
Similar content being viewed by others
Main
Jaundice occurs in the majority of neonates. The total serum bilirubin concentration (TSB) is a dynamic balance between bilirubin production, distribution, and excretion by the liver and kidneys. In late preterm and term neonates the hyperbilirubinemia is generally harmless and culminates most often from the third to the sixth day of life.
Phototherapy using blue light is the treatment of choice for neonatal hyperbilirubinemia, and it is administered to prevent acute and chronic bilirubin encephalopathy (kernicterus). This condition is rare in the industrialized world, but it is still common in many developing countries (1).
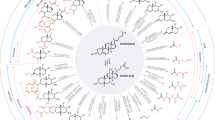
Absorption of light by bilirubin in the skin transforms it from the native nonpolar and toxic Z,Z-bilirubin to more polar bilirubin isomers: the configurational isomers Z,E- and E,Z-bilirubin and structural isomers E,Z- and E,E-lumirubin, which can then be excreted into the bile and urine without conjugation. Configurational isomerization is reversible, whereas formation of lumirubins is irreversible ( Figure 1 ) (2). In addition, small amounts of oxidation products are formed (6).
Photochemical reactions of Z,Z-bilirubin in neonates. McDonagh et al. (3,4) propose that E,Z-lumirubin is formed from both Z,Z- and E,Z-bilirubin, whereas Onishi et al. (5) propose that E,Z-bilirubin is an obligate intermediate in the formation of E,Z-lumirubin. The serum concentrations of E,E-lumirubin were too low to be identified and quantified with certainty and therefore, are not reported.
Blue light, matching the absorption spectrum of serum bilirubin in vitro with a maximum of 459 nm, is used in standard phototherapy worldwide (7). However, treatment with higher wavelength turquoise light may be a desirable alternative. Using optical models of the skin, Agati et al. (8) and Lamola et al. (9) suggested that for equal irradiance, the greatest decrease of the Z,Z-bilirubin concentration would occur with exposure of the infants to turquoise light with peak irradiance within the wavelength range of 485 to 505 nm or 475 to 480 nm, respectively. In our first clinical study using broad spectrum fluorescent light with equal irradiance on the infants, the decrease of TSB was 20% greater for turquoise light with peak irradiance at 490 nm than for blue light with peak irradiance at 452 nm in treatment of preterm infants (10). In our subsequent clinical investigation, also with equal irradiance on the infants, we then compared the effects of light emitted from narrow-band light emitting diodes (LEDs) centered at 497 nm (turquoise) and 459 nm (blue), respectively. The same decrease in the TSB concentration was observed in both groups of late preterm and term infants (11). An extension of this randomized, controlled, nonblinded clinical study was done to compare the levels of bilirubin isomers in the infant’s serum, the results of which we report below.
Results
Table 1 shows no significant differences in the demographic and clinical data between the infants exposed to LED light centered at 497 nm vs. 459 nm.
As expected, there was a significant decrease in the serum concentration of Z,Z-bilirubin and a significant increase in the concentrations of the bilirubin isomers Z,E-bilirubin, E,Z-bilirubin and E,Z-lumirubin, both in infants treated with light centered at 497 nm and 459 nm, respectively (P < 0.001, for all statistical analyses). Z,E-bilirubin accounted for the greatest fraction of the bilirubin isomers formed during the therapy ( Table 2 ).
Table 2 shows that after 24 h of phototherapy, there was no significant difference in the concentrations of total bilirubin isomers and Z,Z-bilirubin between the two groups. Furthermore, the concentrations of Z,E-bilirubin, and thus also total bilirubin isomers formed during light exposure (Z,E-bilirubin, E,Z-bilirubin, and E,Z-lumirubin), were highest in infants treated with LED light centered at 459 nm, while the concentration of E,Z-bilirubin was highest in infants treated with LED light centered at 497 nm. In addition, no significant difference was found between the concentrations of E,Z-lumirubin.
Table 3 shows the concentrations of bilirubin isomers produced during light exposure in relation to total bilirubin isomers, expressed as percentage. After 24 h of treatment the percentage of Z,E-bilirubin, and thus also total bilirubin isomers formed during therapy, were highest for the group exposed to light centered at 459 nm. In contrast, the percentage of E,Z-bilirubin was highest for the group exposed to light centered at 497 nm. No significant difference was found between the percentages of E,Z-lumirubin.
Discussion
This study shows, that after 24 h of treatment, the serum concentrations of total bilirubin isomers and Z,Z-bilirubin were the same in the infants treated either with LED light centered at 497 nm or 459 nm, applied with equal irradiance on the infants. The concentrations of Z,E-bilirubin, and thus also total bilirubin isomers formed during the treatment, were highest for infants exposed to light centered at 459 nm, while the concentration of E,Z-bilirubin was highest for those exposed to light centered at 497 nm.
Z,E-bilirubin accumulates in plasma (12). The concentration of Z,E-bilirubin increases until equilibrium with Z,Z-bilirubin is reached, which occurs after approximately 4–6 h of exposure to light (13,14,15). Thereafter, the percentage of Z,E-bilirubin to the sum of Z,Z- and Z,E-bilirubin only depends on the emission spectrum of the light (15). After 24 h of phototherapy, the percentage of Z,E-bilirubin to total bilirubin isomers was higher for infants treated with light centered at 459 nm than for those treated with light centered at 497 nm (23% vs. 14%), and thus also the percentage of total bilirubin isomers formed during treatment to total bilirubin isomers was highest for the infants treated with light centered at 459 nm (26% vs. 18%) ( Table 3 ). This is in agreement with previous in vitro studies, which showed that after equilibrium between Z,Z- and Z,E-isomers is reached, the percentage of Z,E-bilirubin decreases with longer wavelengths (4,16).This observation has also been confirmed in earlier clinical studies, where the reported percentages of Z,E-bilirubin to total bilirubin isomers were: 24% to 27% (10,13,14), 16% (10) and 9% (14) in children exposed to light of wavelengths ~460, 490, and 528 nm, respectively.
In this study, we found that the concentrations of E,Z-bilirubin were much lower than those of Z,E-bilirubin, but in contrast to Z,E-bilirubin, it was highest for the group treated with light centered at 497 nm. This is in accordance with the formation of E,Z-bilirubin in vitro, which increased with longer wavelengths of the light (5,16). E,Z-bilirubin has been studied less than the Z,E-isomer, presumably because configurational isomerization highly favors formation of Z,E-bilirubin.
After 24 h of treatment there was no significant difference in the E,Z-lumirubin concentration between infants exposed to light centered at 497 nm or 459 nm, respectively ( Table 2 ). However, it was difficult to detect the presence of a small difference of E,Z-lumirubin between the two treatments, due to the low concentrations. In vitro studies have shown, that the formation of lumirubin increases at longer wavelengths of light (3,5,16).
At the initiation of the phototherapy, the sum of Z,E-bilirubin, E,Z-bilirubin, and E,Z-lumirubin comprised ~5% of the total bilirubin isomers ( Table 2 ). The reasons might be that the neonates had been exposed to the ambient light and perhaps that the blood accidentally might have been exposed to light during sampling. Thus, the fact that before phototherapy the concentrations of Z,E-bilirubin, and thus also the sum of Z,E-bilirubin, E,Z-bilirubin, and E,Z-lumirubin, were highest in the group of neonates later receiving light centered at 459 nm, was a coincidence.
This study confirms the results of our previous study (10) using fluorescent light, in which the concentration of Z,E-bilirubin was the highest in infants treated with light with peak emission at 452 nm. However, in that study we only found a trend toward a higher E,Z-bilirubin concentration in infants exposed to light with peak emission at 490 nm.
Non-albumin bound Z,Z-bilirubin in plasma is able to cross the blood-brain barrier as it is nonpolar and lipid-soluble (17). Because the bilirubin isomers formed during phototherapy are more polar and less lipid soluble, it was hypothesized that the unbound fraction of these isomers might be less able to pass through the blood-brain barrier (3,18). Furthermore, isolated bilirubin isomers formed in vitro during light exposure seem to be biologically inert and do not exert any negative biological effects on human neuroblastoma cells (19). If the above was the case, it would be of greatest importance to the very sick extremely preterm infants. Even though their TSB is low, their concentration of unbound Z,Z-bilirubin might be high, which involves a considerable risk of bilirubin encephalopathy (20). Production of Z,E-bilirubin, E,Z-bilirubin, and E,Z-lumirubin start immediately after initiation of phototherapy, and after 60 min of therapy with blue light, ~20% of the serum bilirubin isomers consist of Z,E-bilirubin (13), i.e., a decrease in the risk of neuropathy might occur already short time after start of phototherapy.
It should be pointed out that Z,E-bilirubin and E,Z bilirubin can be converted back to Z,Z-bilirubin in the dark, which is thought to occur in the bile (21). If this also occurs in the intracellular environment, it will reduce the effect of phototherapy.
We know that no other studies of bilirubin isomers during phototherapy with turquoise and blue LED light. This is important, because it is clear that LEDs will be the phototherapy light source of the future, because, in contrast to fluorescent light, they deliver light of narrower wavelength range (fewer noneffective wavelengths), generate significantly less radiant heat, and their irradiance decreases more slowly with time.
Finally, this study in addition with our earlier study (10), are the only investigations exposing infants to light of different peak emission wavelengths at equal irradiances.
We find several strengths of the study: (i) the use of LEDs as the only light source, (ii) the light irradiances were measured by a radiometer with constant sensitivity, which made it possible to expose the two groups of infants to equal irradiance, thereby making the results of the treatments comparable, and (iii) the patient population was homogeneous.
A limitation of the study was that 15% of the randomized infants were either withdrawn or excluded from the investigation. However, as the drop-out was neither related to exposure nor outcome, the risk of selection bias was very small (22).
Conclusion
Distribution of bilirubin isomers in serum was different in neonates treated with LED light centered at 497 nm vs. 459 nm, of essentially equal irradiance.
Perspectives
In future clinical studies comparing the effect of lamps with different emission spectra, the individual bilirubin isomers should be measured. More studies are needed both on the ability of the bilirubin isomers formed during phototherapy to pass through the blood-brain barrier and/or of their toxicity. The first hours after start of phototherapy will be of greatest interest.
Methods
Study Groups
The study groups and treatments have been described in detail previously (11). Briefly, infants were enrolled in the study at the neonatal intensive care unit at Aalborg University Hospital, Denmark between 1 January 2013 and 31 December 2013. All infants were ≥33 wk gestational age with uncomplicated hyperbilirubinemia. They were randomized either to be exposed to light centered at 497 nm or 459 nm, emitted from LEDs. They were treated for 24 h from above. The irradiances were 5.2 × 1015 and 5.1 × 1015 photons/cm2/s, respectively. The irradiance was measured using an Ocean Optics spectrometer (Model 2000+, Dunedin, FL), with a constant sensitivity over the wavelength range of 200 to 1100 nm. The irradiance of the light centered at 459 nm was 30 µW/cm2/nm measured by a handheld clinical radiometer (neoBLUE, Natus Medical, San Carlos, Ca).
The LED light centered at 497 nm had bandwidth of 484–511 nm and emission range 450–575 nm; and the LED light centered at 459 nm had bandwidth of 449–469 nm and emission range 416–524 nm, respectively.
Of the 104 infants who were eligible for the study, parents of 6 infants refused participation. As a result, a total of 98 infants were randomized to receive either LED light centered at 497 nm (n = 50) or 459 nm (n = 48). In the 497 nm group 2, infants were withdrawn from the study, 1 infant because of a high initial TSB and suspicion of blood type ABO immune hemolytic disease, the other infant due to communication issues with the mother. Furthermore, 8 infants were excluded because of liver disease (n = 1) or due to problems either with blood sampling or transportation of the samples from the neonatal intensive care unit to the Department of Clinical Biochemistry during evening and night (n = 7). In the 459 nm group, 1 infant was withdrawn from the study because of a high initial TSB and suspicion of blood type ABO immune hemolytic disease, and 4 infants were excluded due to either problems with blood sampling or sample transportation. Thus, a total of 40 infants receiving LED light centered at 497 nm and 43 infants light centered at 459 nm, were included in the study.
Measurements
The concentrations of bilirubin isomers were measured in serum from capillary blood drawn by a heel stick at initiation of phototherapy (time, 0 h) and 24 h after start of the phototherapy (time, 24 h). Sampling occurred under subdued light and the blood was drawn into tubes wrapped with aluminum foil to avoid light exposure. The blood samples were immediately centrifuged and the serum stored at −20°C in the dark. The bilirubin isomers were identified and quantitated using isocratic reversed phase high performance liquid chromatography (23). The imprecision of the method expressed as coefficients of variation was 2.4% for the concentration of total bilirubin isomers; 3.3% for total bilirubin isomers formed during phototherapy; Z,Z-bilirubin and Z,E-bilirubin, 3.5% for E,Z-bilirubin; and 5.1% for E,Z-lumirubin.
The total bilirubin isomers are defined as the sum of the following bilirubin isomers shown in Figure 1 : Z,Z-bilirubin, Z,E-bilirubin, E,Z-bilirubin, and E,Z-lumirubin. Likewise, the total bilirubin isomers formed during phototherapy is defined as the sum of bilirubin isomers Z,E-bilirubin, E,Z-bilirubin, and E,Z-lumirubin.
The TSB is the sum of all bilirubin derivatives in serum, both unconjugated and conjugated. It was determined by a diazo-method (24). This method is used routinely in our department, and the inclusion of infants in the study was based on such a determination of TSB according to our guidelines for phototherapy.
Ethics
This study was approved by the Committee for Biomedical Research Ethics in Region North Jutland, Denmark. Verbal and written informed consents were obtained from the parents.
The study was registered with number NCT 02154165 in the Clinical Trial Registry.
Data Analysis
Fisher’s exact test for contingency tables was used to calculate significant differences between medians of the two groups. A two-by-two table was obtained by computing the overall median for the entire study group and then for each treatment group counting the number of infants with a value lower or higher than the overall median value. To calculate confidence intervals (CI) for the medians of each group, we applied an approximation relying on the quantiles of the binomial distribution as implemented in the ci.median function from the R-package asbio. Comparisons of categorical variables between the groups were also conducted using Fisher’s exact test. For all analyses the statistical software program R (version 3.2.1) was used. Significance level was set at P < 0.05.
Presentation of Data
The content in serum of Z,E-bilirubin, E,Z-bilirubin, and E,Z-lumirubin is not only presented in absolute values (µmol/l) ( Table 2 ), but also as a fraction of total bilirubin isomers ( Table 3 ). This is due to two reasons: (i) After 24 h of treatment equilibrium exists between Z,E- and Z,Z-bilirubin (13,14,15). Perhaps an equilibrium also exists between E,Z- and Z,Z-bilirubin, but this has not been investigated and (ii) To compare our results with earlier studies, in which the results most often are presented as fractions (10,13,14).
Statement of Financial Support
No financial assistance was received to support this study.
Disclosure
The authors have no conflicts of interest.
References
Bhutani VK, Zipursky A, Blencowe H, et al. Neonatal hyperbilirubinemia and Rhesus disease of the newborn: incidence and impairment estimates for 2010 at regional and global levels. Pediatr Res 2013;74 Suppl 1:86–100.
Maisels MJ, McDonagh AF. Phototherapy for neonatal jaundice. N Engl J Med 2008;358:920–8.
McDonagh AF. Controversies in bilirubin biochemistry and their clinical relevance. Semin Fetal Neonatal Med 2010;15:141–7.
McDonagh AF, Agati G, Fusi F, Pratesi R. Quantum yields for laser photocyclization of bilirubin in the presence of human serum albumin. Dependence of quantum yield on excitation wavelength. Photochem Photobiol 1989;50:305–19.
Onishi S, Itoh S, Isobe K. Wavelength-dependence of the relative rate constants for the main geometric and structural photoisomerization of bilirubin IX alpha bound to human serum albumin. Demonstration of green light at 510 nm as the most effective wavelength in photochemical changes from (ZZ)-bilirubin IX alpha to (EZ)-cyclobilirubin IX alpha via (EZ)-bilirubin. Biochem J 1986;236:23–9.
Lightner DA, Linnane WP 3rd, Ahlfors CE. Bilirubin photooxidation products in the urine of jaundiced neonates receiving phototherapy. Pediatr Res 1984;18:696–700.
American Academy of Pediatrics. Management of hyperbilirubinemia in the newborn infant 35 or more weeks of gestation. Pediatr 2004;114:297–316.
Agati G, Fusi F, Donzelli GP, Pratesi R. Quantum yield and skin filtering effects on the formation rate of lumirubin. J Photochem Photobiol B 1993;18:197–203.
Lamola AA, Bhutani VK, Wong RJ, Stevenson DK, McDonagh AF. The effect of hematocrit on the efficacy of phototherapy for neonatal jaundice. Pediatr Res 2013;74:54–60.
Ebbesen F, Madsen P, Støvring S, Hundborg H, Agati G. Therapeutic effect of turquoise versus blue light with equal irradiance in preterm infants with jaundice. Acta Paediatr 2007;96:837–41.
Ebbesen F, Vandborg PK, Madsen PH, Trydal T, Jakobsen LH, Vreman HJ. Effect of phototherapy with turquoise vs. blue LED light of equal irradiance in jaundiced neonates. Pediatr Res 2016;79:308–12.
Ennever JF, Knox I, Denne SC, Speck WT. Phototherapy for neonatal jaundice: in vivo clearance of bilirubin photoproducts. Pediatr Res 1985;19:205–8.
Mreihil K, Madsen P, Nakstad B, Benth JŠ, Ebbesen F, Hansen TW. Early formation of bilirubin isomers during phototherapy for neonatal jaundice: effects of single vs. double fluorescent lamps vs. photodiodes. Pediatr Res 2015;78:56–62.
Agati G, Fusi F, Pratesi S, Galvan P, Donzelli GP. Bilirubin photoisomerization products in serum and urine from a Crigler-Najjar type I patient treated by phototherapy. J Photochem Photobiol B 1998;47:181–9.
Costarino AT, Ennever JF, Baumgart S, Speck WT, Paul M, Polin RA. Bilirubin photoisomerization in premature neonates under low- and high-dose phototherapy. Pediatr 1985;75:519–22.
Itoh S, Onishi S, Isobe K, Manabe M, Yamakawa T. Wavelength dependence of the geometric and structural photoisomerization of bilirubin bound to human serum albumin. Biol Neonate 1987;51:10–7.
Saunders NR, Liddelow SA, Dziegielewska KM. Barrier mechanisms in the developing brain. Front Pharmacol 2012;3:1–18.
Ruud Hansen TW. Phototherapy for neonatal jaundice–therapeutic effects on more than one level? Semin Perinatol 2010;34:231–4.
Jasprova J, Dal Ben M, Vianello E, et al. The biological effects of bilirubin photoisomers. PLoS One 2016;11:e0148126.
Cashore WJ, Oh W. Unbound bilirubin and kernicterus in low-birth-weight infants. Pediatr 1982;69:481–5.
Onishi S, Isobe K, Itoh S, et al. Metabolism of bilirubin and its photoisomers in newborn infants during phototherapy. J Biochem 1986;100:789–95.
Pearce N, Checkoway H, Kriebel D. Bias in occupational epidemiology studies. Occup Environ Med 2007;64:562–8.
Itoh S, Isobe K, Onishi S. Accurate and sensitive high-performance liquid chromatographic method for geometrical and structural photoisomers of bilirubin IX alpha using the relative molar absorptivity values. J Chromatogr A 1999;848:169–77.
Doumas BT, Kwok-Cheung PP, Perry BW, et al. Candidate reference method for determination of total bilirubin in serum: development and validation. Clin Chem 1985;31:1779–89.
Acknowledgements
We thank Stephanie Kourula, PhD and Benjamin K. Cline, MS for technical assistance and valuable discussions. Ronald J. Wong, BA, is thanked for critical review of the manuscript. We are grateful to Rami Vardi of Bright Light LED, (Canoga Park, CA) for technical support and donation of the LED tubes and driver.
Author information
Authors and Affiliations
Corresponding author
PowerPoint slides
Rights and permissions
About this article
Cite this article
Ebbesen, F., Madsen, P., Vandborg, P. et al. Bilirubin isomer distribution in jaundiced neonates during phototherapy with LED light centered at 497 nm (turquoise) vs. 459 nm (blue). Pediatr Res 80, 511–515 (2016). https://doi.org/10.1038/pr.2016.115
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pr.2016.115
This article is cited by
-
Urinary lumirubin excretion in jaundiced preterm neonates during phototherapy with blue light-emitting diode vs. green fluorescent lamp
Scientific Reports (2023)
-
Characteristics of bilirubin photochemical changes under green light-emitting diodes in humans compared with animal species
Scientific Reports (2021)
-
Sixty years of phototherapy for neonatal jaundice – from serendipitous observation to standardized treatment and rescue for millions
Journal of Perinatology (2020)
-
A novel accurate LC-MS/MS method for quantitative determination of Z-lumirubin
Scientific Reports (2020)
-
The effect of light wavelength on in vitro bilirubin photodegradation and photoisomer production
Pediatric Research (2019)