Abstract
Background:
Rhesus (Rh) disease and extreme hyperbilirubinemia (EHB) result in neonatal mortality and long-term neurodevelopmental impairment, yet there are no estimates of their burden.
Methods:
Systematic reviews and meta-analyses were undertaken of national prevalence, mortality, and kernicterus due to Rh disease and EHB. We applied a compartmental model to estimate neonatal survivors and impairment cases for 2010.
Results:
Twenty-four million (18% of 134 million live births ≥32 wk gestational age from 184 countries; uncertainty range: 23–26 million) were at risk for neonatal hyperbilirubinemia-related adverse outcomes. Of these, 480,700 (0.36%) had either Rh disease (373,300; uncertainty range: 271,800–477,500) or developed EHB from other causes (107,400; uncertainty range: 57,000–131,000), with a 24% risk for death (114,100; uncertainty range: 59,700–172,000), 13% for kernicterus (75,400), and 11% for stillbirths. Three-quarters of mortality occurred in sub-Saharan Africa and South Asia. Kernicterus with Rh disease ranged from 38, 28, 28, and 25/100,000 live births for Eastern Europe/Central Asian, sub-Saharan African, South Asian, and Latin American regions, respectively. More than 83% of survivors with kernicterus had one or more impairments.
Conclusion:
Failure to prevent Rh sensitization and manage neonatal hyperbilirubinemia results in 114,100 avoidable neonatal deaths and many children grow up with disabilities. Proven solutions remain underused, especially in low-income countries.
Similar content being viewed by others
Main
Neonatal hyperbilirubinemia and jaundice occur in almost all newborns (1,2,3,4,5,6,7,8,9,10) and may be benign if its progression to extreme hyperbilirubinemia (EHB; total bilirubin (TB) >428 μmol/l in full-term babies) is recognized, monitored, and prevented or managed in a timely manner. Major risk factors include neonatal hemolysis (such as Rhesus (Rh) disease), glucose-6-phosphate dehydrogenase (G6PD) deficiency, infections, and an array of familial and genetic disorders. In addition to conditions such as preterm birth that make the neonate more susceptible to bilirubin neurotoxicity, suboptimal breast milk intake or dehydration may also contribute to EHB (1,2,3,4,5,6,7,8,9,10). At present, once the early stages of hyperbilirubinemic brain damage occur, therapeutic options are limited to the prompt (<8 h) use of exchange transfusion, hence the imperative for preventive approaches. Universal prenatal Rh screening for specific risk of perinatal hemolysis and its prophylaxis with Rh immunoglobulin have been highly effective practices for preventing neonatal morbidities and mortality (11,12,13,14). Countries with universal access to perinatal health services have virtually eliminated severe hyperbilirubinemia (icterus gravis neonatorum), which had been so common in the late 19th century (15,16,17,18,19,20,21,22,23,24,25,26,27,28).
Now with emerging affordable technologies, the worldwide prevention and management of newborn jaundice can more feasibly reach those at risk even in low-income settings (1,2,29,30,31). Yet, there remains a paucity of quality population data on the prevalence of hyperbilirubinemia and related outcomes to inform such a strategy for most countries (8).
In the absence of direct national or regional reporting, we report systematic estimates for the prevalence, mortality, and neurodevelopmental outcomes of Rh disease and EHB due to other causes, e.g., G6PD deficiency, prematurity, neonatal hemolysis, and idiopathic causes. We based these estimates, as described below, on national risks of G6PD deficiency, preterm birth, neonatal hemolysis (not due to Rh disease), and other idiopathic causes, along with measures of the implementation gap for universal Rh prophylaxis.
Methods
Definitions and Measurements
Inconsistent use of definitions and management approaches limit the use of available data at both national and global levels. We used the following definitions shown in Figure 1 , starting from perinatal risk factors, outcomes in terms of mortality, and then impairments (hearing loss and neurodevelopmental impairment, including choreoathetoid cerebral palsy).
Schematic representation of the prenatal and neonatal risk factors for Rhesus (Rh) disease and extreme hyperbilirubinemia and their impact on stillbirths, neonatal death due to kernicterus, and long-term impairment of kernicterus during childhood. In view of the complex confluence of biological risk, interaction with other childhood disease, and social–cultural factors, we did not estimate childhood death due to kernicterus. ABE, acute bilirubin encephalophathy.
Rh disease or Rh hemolytic disease is defined by maternal–fetal Rh (D) antigen incompatibility and the consequences associated with maternal sensitization (see Web appendix I-iii for details and references). This was the most common and severe cause of fetal and neonatal hemolysis in Europe and the United States until about 60 y ago; it is now rare in countries where Rh prophylaxis is used. Women whose erythrocytes are Rh (D)-antigen negative are sensitized (develop anti-Rh (D) antibodies) during a previous pregnancy in which the fetus is Rh (D)-positive or by exposure to Rh antigens from blood products/transfusion. Severe hemolytic disease manifests in utero as progressive anemia and hypoalbuminemia, leading to anasarca (edema) and heart failure (hydrops fetalis), resulting in stillbirths or early neonatal deaths. Surviving infants can present with severe jaundice, anemia, and death from kernicterus or brain damage resulting from EHB. These complications can be treated with timely exchange blood transfusions. In most high-income countries, Rh disease has been eradicated by coordinated obstetrical and neonatal care (32). These prenatal interventions require expert assessment, use of Rh immunoprophylaxis, and diagnosis of fetal anemia, early signs of cardiac failure, or hydrops, in addition to the timely use of intrauterine transfusion to correct hemolytic anemia.
G6PD deficiency is an X-linked inherited enzymopathy (33,34,35,36,37,38,39,40). G6PD deficiency is widespread (450 million people). There are variable data regarding the distribution of individuals at risk for neonatal hemolytic crisis due to G6PD deficiency, partly due to diverse assay methods for enzyme activity or genetic identification and timing of the assay in relation to postnatal and chronological ages. Recent population migration, sample size, and validity of the surveys also limit the accurate representation of a national prevalence (34). Existing published data highlight important limitations due to the use of summarized national levels that can mask subnational variations. Accurate (phenotypic) quantitative identification of deficient G6PD enzyme activity by spectrophotometry is a measure of the condition soon after birth. However, variations due to both partial phenotypic manifestations of diverse genetic mutations and the high enzyme activity of younger red blood cells are significant confounding factors. DNA/polymerase chain reaction screening for specific mutations is ideal to identify female heterozygotes, but this approach is limited by the diversity of known variants and the occasional mismatch with phenotypic expression of enzyme activity. More recently, Luzzatto et al. (37). have suggested estimation of G6PD deficiency allele frequency to predict and generate population-weighted estimates of affected population. Howes et al. (33). have used this approach to propose a Bayesian geostatistical model adapted to the gene’s X-linked inheritance that circumvents the above-mentioned limitations to assess national prevalence. There is paucity of data to estimate a neonate’s risk for G6PD deficiency following exposure to aggravating triggers that may cause unpredictable adverse consequences (35).
Prematurity: Preterm birth is any birth before 37 completed wk of gestation (<259 d since the first day of the woman’s last menstrual period) (41,42). Further subdivisions based on completed GA are as follows: late preterm (34 to <37 wk); moderately preterm (32 to <34 wk); and very preterm (<32 wk). The incidence of kernicterus in 1955, i.e., before the clinical use of phototherapy, was 10.1, 5.7, 3.2, 1.1, and 0.8% for infants at 30, 31–32, 33–34, 35–36, and >36 wk GA, respectively (43). We limited our analysis to the group of preterm births of >32 wk GA because preterm births <32 wk handle hyperbilirubinemia differently, and according to International Classification of Diseases rules, deaths and disability in this group should be allocated to preterm birth as the primary condition to address, so we will not include these here to avoid double counting the burden along with those included in preterm birth direct complications.
Clinical State and Outcome Definitions
EHB is defined as total plasma/serum bilirubin >25 mg/dl (428 µmol/l) or those treated with exchange blood transfusion (44). Kernicterus or CBE has been used as a clinical diagnosis that relies on a history of excessive prolonged hyperbilirubinemia and classical abnormalities of muscle tone, movement disorders, and aberrant processing disorders (26,45,46). Acute signs of extrapyramidal dysfunction may precede CBE. Acute bilirubin encephalopathy (31) includes progressive changes in an infant’s mental (behavioral) status, muscle tone, and distinct cry patterns. Acute clinical signs, initially described in 1955 by Crosse et al. (43), are as follows: “the first 24 to 48 hours of life are the most critical. Signs develop in a baby who is jaundiced… and include head retraction, an expressionless facies, usually with oculogyric movements, changes in muscle tone, cyanotic attacks, refusal to suck, vomiting and hemorrhage prior to death. In severe cases these signs are self-evident but in those less affected they are easily missed …. unless specifically sought.” “Several babies who showed minimal signs have proved to be definite cases of kernicterus.” Thus, neonatal mortality is due to respiratory failure and progressive coma or intractable seizures. An increased signal on magnetic resonance imaging of the globus pallidus and other areas prone to bilirubin neurotoxicity is often evidenced in surviving infants. Posticteric clinical sequelae include irreversible, but static, classic signs of athetoid cerebral palsy, generalized dystonia, paralysis of upward gaze, “kernicteric facies,” and sensorineural hearing impairment. Neuromotor impairment secondary to abnormal muscle tone includes dystonia that is characterized by excessive or sustained contraction of opposing muscles during voluntary movements, in addition to hypertonia or hypotonia. Painful muscle cramps, incoordination of sucking, swallowing, and visuomotor function may manifest during early infancy. Cerebral palsy with choreoathetosis is another classic manifestation of kernicterus, which is characterized by involuntary movements or irregular muscle contractions that manifest as writhing or twisting. Paroxysmal movement disorders are often misdiagnosed and labeled as seizures. Hearing impairment is defined by sensorineural abnormalities ascertained by objective tests. Auditory system abnormalities with hyperbilirubinemia primarily involve brainstem nuclei, leading to abnormalities in auditory brainstem responses and detected by referred hearing screens during infancy. Auditory neuropathy, also called ‘‘auditory dyssynchrony,’’ is often subtler and associated with childhood hearing impairment (47,48,49,50,51,52). Developmental delay or cognitive impairment, ascertained by the Bayley Mental Developmental Index, provides continuous variables to define the extent of aberrations for mental and psychomotor indexes. In addition, infants’ intelligence can be estimated or tested for intelligence quotients of <70 using the Wechsler Intelligence Score for Children (47). Cognitive impairment has been reported and possibly related to associated hearing impairment, neuromotor impairment, or, possibly due to social neglect. Other posticteric sequelae may result from subtle signs either with exposure to TB levels that are lower than EHB or following partial treatment of EHB. These “soft” perturbations of sensory processing disorders have been described as the syndrome of bilirubin-induced neurologic dysfunction or “BIND” (53) but are intentionally not included in this study due to the limited data and consensus in definitions found in the literature.
Data Searches for G6PD Deficiency and Preterm Birth, With Effects on Neonatal Mortality, EHB, and Kernicterus
Systematic reviews of the main electronic literature databases (Ovid Medline, Ovid Medline In-Process and Non-Indexed Citations, PubMed, Cinahl, Global Health, Scopus, and Popline) were undertaken using a combination of medical subject heading and free text words. Search terms used were exchange blood transfusion, kernicterus/bilirubin encephalopathy, death (from jaundice), phototherapy, G6PD deficiency, ABO incompatibility, Rh incompatibility, admission/readmission (for jaundice), sequelae, impairment, and outcomes. Reference lists of all the relevant studies were scanned to further identify studies of interest. We excluded case reports, nonhuman studies, those that did not have the relevant population or age group, those that did not focus on the relevant condition (jaundice, hyperbilirubinemia, and encephalopathy), and those that did not provide relevant primary data (e.g., for prevalence/risk). In addition, we conducted a retrospective review of the historic Rh disease literature, commencing from identification as a clinical disease to the period Rh disease was considered “conquered.” Pivotal studies, cited in Appendix I, allowed for estimation of mortality and disease among survivors. We also identified population-based studies before the use of phototherapy, which reported on the outcome of systematic use of phototherapy. Due to rapid improvement in the access to and quality of specialized/intensive newborn care in countries with low-mortality settings, for mortality, encephalopathy, and long-term impairment risk, we decided to focus on recent literature only and extracted data from studies with birth cohorts having median year of 2005 or later. Where sufficient data were available, standard meta-analysis techniques were used to obtain pooled estimates of the relevant parameter’s risk, which included EHB-related neonatal mortality and bilirubin encephalopathy (acute and/or chronic). Heterogeneity across studies was evaluated using I2 and χ2 tests, and where evidence of heterogeneity was present (I2 > 70% or P < 0.05), a random-effects model was used.
Data Searches for Rh Disease
A systematic review of the published literature using PubMed was performed to establish the prevalence of Rh-negative blood groups by country for all countries with NMR >5. Countries with NMR <5 were presumed to have good Rh prophylaxis and strong health systems, with very low number of cases of Rh disease in these countries. Search terms included “rh, rh blood-group system” (medical subject heading term), “Rhesus,” and “Blood group.” Reference lists of all the relevant studies were scanned to further identify studies of interest and Web-based resources were searched using Internet search engines. For countries with no available data, the prevalence of Rh-negative blood groups was estimated using the regional median prevalence (Web appendix I-iii).
A further systematic review using PubMed (search terms included combinations of “Rhesus,” “rhesus disease,” “erythroblastosis fetalis,” “rhesus h(a)emolytic disease of the newborn,” “outcome,” “neonatal death,” and “stillbirth”) was undertaken to estimate the outcome of Rh disease in the absence of effective treatment and limited to primary studies published before 1960 and to reviews without date limitations.
Pooling of Data by Country Context and Access to Neonatal Services
Data were not available to estimate every parameter for every country. Hence, we sought to use pooled data from countries that are similar in their access to and quality of care as these are closely linked to outcomes. Outcomes of EHB depend on a systematic approach to prevention and management of hyperbilirubinemia. We grouped countries into three NMR bands (NMR/1,000 live births) as follows: Group 1 (NMR <5), Group 2 (NMR 5 to <15), and Group 3 (NMR ≥15), which approximate to high-, middle-, and low-income countries, respectively. Where data were available, we sought to further distinguish the outcomes between those with access to specialized neonatal care if required (including phototherapy and exchange blood transfusion) and those with basic/limited care only at home or in a facility with no access to these specialized services because this will affect the mortality and kernicterus outcomes.
Modeling Approach
A three-step compartmental model was constructed for each country with at least 10,000 live births for the year 2010 (54,55) as follows: Step 1) estimation of the number of cases based on the prevalence of G6PD deficiency, late-preterm birth, and other causes of EHB, not due to Rh disease, in addition to estimating the prevalence of Rh disease; Step 2) estimation of the number of stillbirths, neonatal deaths, and cases of kernicterus by applying the risk data to the estimated cases; and Step 3) estimation of the numbers of survivors with neurodevelopmental impairment ( Figure 2 ). All results are presented by regional grouping according to the Global Burden of Disease Study Group superregions (56,57) (Appendix II). We quantified the uncertainty surrounding these estimates by taking 1,000 random draws of the input parameters at each step, assuming a normal distribution with mean equal to the point estimate of the parameter and SD equal to the estimated SE of the parameter (55). We summed the data at the worldwide or regional level for each draw and present the 2.5th and 97.5th percentiles of the resulting distributions as the uncertainty range.
Schematic representation of the three-compartmental model. This model delineates the serial steps toward input of country-specific parameters, processes, and outputs to estimate prevalence, burden of Rhesus (Rh) disease and extreme hyperbilirubinemia–related mortality, and the number of postneonatal survivors with kernicterus and long-term impairment. A/CBE, acute/chronic bilirubin encephalophathy.
Results
We identified 23,145 relevant titles for the non-Rh disease causes of EHB. Of these, 2,599 abstracts and 185 pertinent publications were selected for full text review. Sixty-two studies (from 30 countries) were screened; 26 met the criteria to provide population source for occurrence of kernicterus (acute and/or chronic) and/or kernicterus-associated neonatal mortality (Web appendix I-vii). We used the observational cohort of 41,324 infants born without Rh disease who were recruited for a multicenter study in the United States in 1959–1975 (58). Extrapolation of these data to the 134 million live births yielded the result that 1.1 million (0.8%) worldwide would develop TB >20 mg/dl (342 µmol/l), 214,400 would progress to TB >25 mg/dl (428 µmol/l), and a total of 1,648,200 newborns would undergo exchange transfusions. Studies excluded because of reported implementation of routine bilirubin screening showed that prophylactic use of phototherapy in 6.6 ± 1.3% (95% confidence interval (CI): 4.4, 8.7) of live births >34 wk gestational age (GA) (3,59,60,61) drastically reduced the need for exchange transfusions.
Step 1: Estimation of Prevalence
Rh hemolytic disease prevalence. Postpartum Rh immunoglobulin administration has been standard therapy for many years in high-income countries and Rh hemolytic disease has been virtually eradicated. Countries with a neonatal mortality rate (NMR) <5 were therefore presumed to have good Rh prophylaxis and strong health systems, with very few cases of Rh disease. It is likely that there are lapses in universal immunoprophylaxis in some of these countries. However, there are inadequate data to estimate the number of protection failures and the numbers would be small in the global perspective; therefore, our focus was on countries with an NMR >5.
Process: The prevalence of Rh-negative blood group was estimated by country (see Methods and Web appendix I-iii) and the total births for 2010 were calculated as the sum of live births (54) and stillbirths (estimated assuming no change in stillbirth rates from 2009 to 2010) (62). These were used to estimate the total number of pregnancies in Rh-negative women in 2010. The number of Rh-positive babies born to those women was calculated knowing the Rh positivity prevalence in the fathers (i.e., the prevalence of Rh positivity in the country). For an Rh-positive baby to be born to an Rh-negative mother, it must receive at least one Rh allele (positive) from an Rh-positive father. The number of Rh-positive pregnancies represents the number of women who should have received Rh immunoglobulin prophylaxis postpartum. The number of women who did receive prophylaxis is based on information on the worldwide distribution of Rh immunoglobulin preparations, obtained through the courtesy of The Marketing Research Bureau (http://marketingresearchbureau.com/; Orange, CT), which has tracked the plasma markets since 1974 through interviews with public organizations and private firms, governmental and nongovernmental organizations, trade associations, patient groups, and opinion leaders. Thus, we determined the number of women who did not receive postpartum protection. Of those unprotected women, it was previously calculated that 15% would develop Rh isoimmunization and their anti-Rh antibodies would enter the circulation of their next baby (11). We calculated the risk of a second baby being Rh positive from the prevalence of the Rh positivity of the father. This risk factor was modified because the fathers in the second pregnancy do not account for the Rh-negative men who could have been fathers in the first pregnancy.
These serial calculations required several assumptions, limiting their absolute accuracy. As will be noted, this results—for the most part—in an underestimation of the severity of the burden. First, all calculations are based on two Rh-positive pregnancies; however, in many countries, the fertility rate (average number of babies per woman) is as high as 7.0; in Nigeria, e.g., in 2010, it was 4.9. With each successive Rh-positive pregnancy, the prevalence of Rh immunization increases. Prevalence data for Rh negativity were not available for all countries and within countries too, they varied. Accordingly, regional median estimates were applied. Second, it is likely that in many countries where Rh immunoglobulin is available, there are many failures of protection. Our calculations are based on the assumption that all the Rh immunoglobulin distributed in a country was used postpartum. That means that none was used during pregnancy or posttermination of pregnancy/miscarriage or for other medical indications and that each vial was used as a single dose and not divided for multiple recipients. Last, we have not included in our calculations that blood type A, B, O incompatibility reduces the likelihood of Rh isoimmunization ( Table 1 ).
Outcome: In 2010, an estimated 373,300 babies were affected with Rh hemolytic disease worldwide. Data inputs are detailed descriptions by country in the Web appendix I-iv. The global estimated prevalence for Rh disease was 276/100,000 live births. Prevalence for specific regions such as Southeast Asia/Pacific countries, Latin America, North Africa/the Middle East, South Asia, sub-Saharan Africa, and Eastern Europe/Central Asia is estimated at 57, 252, 278, 385, 386, and 529/100,000 live births, respectively. These data are in contrast to Rh disease prevalence of 2.5/100,000 live births in countries that have well-established health-care infrastructure that includes coordinated perinatal–neonatal care for virtually all pregnancies.
Prevalence of Risk Factors for EHB
G6PD deficiency prevalence. Process: Country-specific prevalence for overall G6PD deficiency was obtained from (i) a geostatistical model reported for 97 endemic malaria countries (33); (ii) pooled estimates of ≥3 studies for each of these six countries (Croatia, Cyprus, Greece, Italy, Spain, and the United States) and the studies had used diverse methodologies to assay G6PD deficiency; (iii) regional estimates from Nkhoma et al. for the remaining 81 countries (33,34) ( Table 2 , Web appendix I-ii). Howes et al. (33) have provided the most recent report, a continuous evidence-based prevalence and estimate of the affected population that represents a national risk for countries endemic to malaria. Unlike the Nkhoma report (34), the G6PD deficiency phenotype was identified and then used to model the genotype for these countries (35). Prevalence was generally lower across Central and Southeast Asia compared with that in sub-Saharan Africa (usually <20%) but accounted for >60% of the affected general population.
Moderate- and late-preterm birth (32 to <37 wk gestational age) prevalence. Process: Prevalence of preterm birth rates by country was obtained from the data reported by Blencowe et al. (41). The study estimated that 84% of all preterm births occurred after 32 completed wk of gestation.
Estimation of risk for nonpreterm neonates without G6PD deficiency or Rh disease. Process: The population at risk of EHB but without any of the three quantified EHB risk factors (G6PD deficiency, Rh disease, or prematurity) was obtained mathematically by subtracting the sum of the live births with each risk factor from the total population of live births. This subgroup includes infants with risk of undifferentiated, but major, causes of EHB: neonatal hemolysis (including ABO incompatibility and other red blood cell disorders) and an increasingly recognized array of idiopathic causes ( Table 2 ).
Risk of EHB. Process: Two sets of population studies from Canada and Denmark (63,64,65,66,67,68,69) provided data on the number who develop EHB and listed causes for EHB (excluding Rh disease because of effective national Rh prophylaxis programs). We requested Sgro and Ebbesen to provide additional unpublished data to clarify the prevalence for G6PD deficiency and preterm births in a comparable EHB cohort. We relied on the Canadian data (66,67,68) to inform prevalence data estimate because the population and causes of jaundice were more heterogeneous than that in the Danish data (63,64,65,69). The combined Canadian and Danish data set includes unpublished data on outcomes at age >2 y and EHB data for preterm neonates. In the absence of data from other settings, the same risk was applied to all countries. As these studies were undertaken in populations with low rates of infection and intrauterine growth restriction, with access to full prenatal screening and comprehensive neonatal care including prophylactic interventions with phototherapy and/or exchange blood transfusion, the risk of EHB is likely to be lower than that in settings without such access. In particular, for the “global” preterm baby, much of the increased risk of EHB is due to its increased infection vulnerability. In this supplement, to avoid double counting the long-term impairment in these babies, this burden has been included under infection (70). We sought to adjust for the effect of access to phototherapy and the risk of EHB using data for babies of >2 kg weight from a trial of phototherapy to reduce hyperbilirubinemia, where babies without access to phototherapy had 2.45 times the risk of developing EHB (58).
From the Canadian data, we estimated the global risk of EHB without any of the three risk factors and assuming an average 2.37% G6PD prevalence reported in military recruits in the United States (36) and extrapolated it to the Canadian data; we calculated the risk of EHB in G6PD-deficient babies to be 0.13%, as shown in Table 3 . To estimate the EHB prevalence due to G6PD deficiency, we assumed an equivalent biological risk across the different countries and regions and applied this risk to the prevalence of G6PD deficiency in each country to calculate the population of G6PD-deficient babies who would develop EHB.
The Canadian population–based study also reported 19 cases of EHB in preterm babies 34 to <37 wk gestation (66,67,68). This gives a EHB risk of 0.045%, assuming that 6.6% of live births are late preterm in Canada ( Table 3 ). This presents a likely underestimation of the risk because of the following: (i) precise definitions for EHB are not available for preterm infants and bilirubin-associated neurological damage is likely to occur at lower levels than in term babies; and (ii) because there were no surveillance data to quantify the risk of EHB in premature babies GA 32 to <34 wk, we assumed the risk to be the same as in those of GA 34 to <37 wk.
EHB outcome: Globally, we estimated that of the 11 million (uncertainty range: 11–12 million) babies born at risk for G6PD deficiency, an estimated 27,000 cases of EHB occurred in G6PD-deficient babies. Latin America, South Asia, and sub-Saharan Africa account for 2, 33, and 47% of the G6PD-deficient infants with EHB, respectively, for a combined prevalence of 28/100,000 live births. This is in contrast with high-income nations that account for 2.2% of global burden of EHB due to G6PD deficiency, with a prevalence of 5/100,000 live births.
We estimated that of the 13 million (uncertainty range: 12–14 million) babies born at GA 32–37 wk, at least 10,000 developed EHB. Latin America, sub-Saharan Africa, and South Asia account for 4, 32, and 39% of the EHB cases, respectively, for a combined prevalence of 10/100,000 live births. This is in contrast with high-income nations where the 4% moderate and late-preterm live births have an EHB prevalence of 3.5/100,000 live births.
We estimated that of the remaining 111 million babies born at GA >36 wk, at least 70, 000 developed EHB that would be attributed to undifferentiated causes but we combined occurrence of EHB due to neonatal hemolytic and/or idiopathic conditions, but unrelated to Rh disease.
Global prevalence of EHB and Rh disease. We estimated that 373,300 live births (uncertainty range: 271,800–477,500) in 2010 were affected by Rh disease (277/100,000 live births; Table 4 ) and 107,400 live births by EHB due to other causes: 10% moderate and late preterm (8/100,000 live births); 25% G6PD (20/100,000 live births); and 66% due to other hemolysis/idiopathic causes. The majority of the total EHB and Rh disease (80%) occurred in those born in countries with NMR >15 that account for 60% of the global live births.
Step 2: Estimation of Postneonatal Survivors From Rh Disease and EHB
Rh disease–related mortality and kernicterus. Process: It was assumed that infants born with Rh disease without the benefit of prenatal screening and coordinated Rh prophylaxis and intensive treatment (such as serial middle cerebral velocity measurements, recognition and correction of fetal anemia, timing for safe birthing, and postnatal treatment with exchange transfusion or phototherapy) would have an outcome similar to that reported by investigators before the 1950s (before the availability of exchange blood transfusion and phototherapy) for neonatal mortality and before 1970 for stillbirth outcomes (Web appendix I-v).
Walker described a large series of newborns with Rh disease and reported the stillbirth rate at 14% (23). This is consistent with a smaller study where 13% of noninduced pregnancies affected with Rh disease were stillborn (19). The reported neonatal mortality in live births affected by Rh disease was 32% (24/75) in a series from the United States during the period 1928–1945 (15), which is consistent with the results in other retrieved studies (Web appendix I-v). As noted by Vaughan in 1950 (16), these results are not comparable because the population denominator included only clinical cases before the advent of serological testing in the early 1940s and because the numerator frequently included the composite measure of adverse outcome (kernicterus or death) and not death only. In view of these limitations, we used only the 1945–1946 data on live birth outcomes from the Boston Hospital (16), where the population denominator included all cases diagnosed serologically, including mild or subclinical cases, and where it was possible to estimate the mortality rate without including the kernicterus survivors. Because our outcome of interest was the risk of neonatal death out of all births in Rh-sensitized pregnancies (including stillbirths), we adjusted the denominator (assuming the stillbirth rate in the population to be 14%, as above) and estimated that 24% of all Rh-immunized pregnancies would result in neonatal deaths.
In Walker’s large series of pregnancies affected with Rh disease, 33% of newborns required no treatment (23). We have assumed that 14% of Rh disease pregnancies will result in stillbirths and 24% in neonatal deaths and that the remaining 29%, who require treatment, will have severe hyperbilirubinemia. Hsia et al. (20) reported that 50% of untreated infants whose peak TB reached >513 μmol/l (30 mg/dl) developed kernicterus, consistent with observations made by Mollison and Walker (19). We assumed that 50% of babies with Rh disease and hyperbilirubinemia would reach a level greater than 30 mg/dl (513 µmol/l) in keeping with the clear indication for exchange transfusion for babies with Rh disease (as described by Walker) to prevent kernicterus. Overall, we estimated 7.2% of all Rh disease–affected infants who survived had developed subsequent kernicterus ( Table 1 ).
Non-Rh disease EHB mortality and kernicterus adjusted for access to neonatal care. Process: We estimated the number of babies with EHB and/or Rh disease who develop acute kernicterus or die in the neonatal period. The risk for acute (ABE) and chronic bilirubin encephalopathy (CBE; kernicterus) was calculated together to avoid overreporting of cases because many articles had given figures for both without specifying how many babies had both ABE and CBE. If individual data were listed for ABE and CBE (kernicterus), we chose the higher value for our analysis ( Table 2 and Web appendix I-v).
Outcome in countries with “good” access to neonatal care (NMR <5): In these countries, almost all babies requiring care would have access to specialized facilities. The risk of bilirubin encephalopathy in this group was estimated from six relevant articles from four countries (71,72,73,74,75), and it included a large cohort study with 7-y follow-up from the United States (76). The pooled risk of encephalopathy was 23.0% (95% CI: 9.9, 36.1). On the other hand, the pooled mortality data using two data sets specifically from the United States from among the three pooled data sets showed a bilirubin encephalopathy rate of 2.4% (95% CI: 1.0, 5.8).
Outcome in countries with “intermediate” access to neonatal care (NMR 5 to <15): In this group, the majority of the population would have access to neonatal intensive care unit (NICU) care, but the quality of care may be variable. A small proportion would have no access to NICU care or treatment. Pooling results from six studies conducted in NICU settings yielded an encephalopathy risk of 35.0% (95% CI: 12.0, 58.0) for those with access to NICU care, whereas the average NMR derived from two studies was 8.2% (95% CI: 3.3, 13.1). For the small proportion of population with basic or no access to health care, risks of encephalopathy and neonatal mortality derived from the “marginal access” countries were applied.
Outcome countries with “limited” access to neonatal care: This group of countries has the largest and most heterogeneous population, with around 50 million home births with no care, facility births with some care, and a limited number of urban or richer families with variable access to NICU care. We used extensive work published elsewhere to estimate the access to care within these countries (55) (Web appendix II-ii). The neonatal kernicteric mortality for NICU care was estimated by pooling results from 16 studies (eight countries) that included ten countries from Africa. The pooled mortality risk was 16.0% among infants with EHB (95% CI: 10.2, 21.9%). In those without any access to care, we conservatively selected a mortality of 35% based on a study conducted in the late 1940s, when treatment options were limited to exchange blood transfusion at specialized centers. For the risk of encephalopathy at the NICU level, 15 facility-level data sets from seven countries were available, and the pooled estimate was 43.8% (95% CI: 25.5, 62.1).
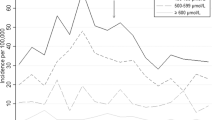
Global estimate of mortality associated with Rh disease and EHB due to other causes. There were 114,000 neonatal deaths associated with these conditions in 2010 (85/100,000 live births (22% or 25,000 deaths with EHB, uncertainty range: 10,000–36,000). There were 89,000 deaths (78%) associated with Rh disease (uncertainty range: 42,000–151,000). Eastern Europe/Central Asia, Latin America, sub-Saharan Africa, and South Asia account for 6, 7, 35, and 39% of the deaths, respectively, for a combined prevalence of 119/100,000 live births compared with 0.1% (n = 94; prevalence 1/100,000 live births) in high-income countries ( Figure 3 ).
Number of stillbirths (due to Rhesus (Rh) disease; white bars) and neonatal deaths/100,000 live births due to kernicterus (black bars) for all live births in 2010. These data are shown for regional geographic distribution. Regional categorization of countries is consistent with the global burden of diseases (54,55).
Global estimated risk of stillbirths due to RH disease. We estimated 52,000 stillbirths due to Rh disease ( Figure 3 ). To investigate the contribution of EHB and/or fetal Rh disease, we relied on data reported from high-income countries from an era before universal Rh immunoprophylaxis. It is unusual for non-Rh disease EHB to present with fetal manifestations. Stillbirths are less likely in pregnancies at risk for EHB without Rh disease. However, we are underestimating both stillbirths and neonatal deaths for remote communities or nations in conflict.
Global estimates of number of babies with kernicterus. There were 75,400 cases (uncertainty range: 43,200–95,800) that represent 24% of the surviving 314,700 neonates with EHB and Rh disease who developed kernicterus, for a prevalence of 56/100,000 live births. Figure 4 illustrates the contributory causes of newborn jaundice that led to kernicterus. There were 48,500 (64%) and 26,900 (36%) cases of kernicterus associated with non-Rh EHB and Rh disease, respectively. Eastern Europe/Central Asia, Latin America, sub-Saharan Africa, and South Asia account for 3.8, 5.8, 35, and 37% of the kernicterus cases, respectively, for a combined prevalence of 73/100,000 live births, compared with 1.6% (n = 1,193; prevalence 10/100,000 live births) from high-income countries.
Estimated rates of kernicterus (per 100,000 live births). Data are presented and attributed to cause of hyperbilirubinemia due to prematurity by yellow bars; G6PD deficiency by green; hemolytic and idiopathic conditions by blue; and Rhesus (Rh) disease by red. These are shown for regional geographic distribution worldwide using global burden of diseases (GBD) categorization (54,55).
Step 3: Estimation of Impairment due to Kernicterus
Global estimate of survivors with NDI following kernicterus. The estimated risk of long-term impairment among survivors, globally, is shown in Figure 5 . We based the risk on a recently published systematic review and data provided by Sgro and Ebbesen (63,64,65,66,67,68), which are more specific than those previously provided by Ip et al. (6). We assumed a constant biologic risk and applied this risk of impairment to all the survivors of kernicterus regardless of the level of care and mortality setting because the effect of bilirubin encephalopathy is not reversible (a global prevalence of 56/100,000 live births) and hence estimated the number of impaired survivors with long-term impairment according to specific global regions ( Table 5 and Figure 6 ).
Outcomes for Rhesus (Rh) disease–affected pregnancies and extreme hyperbilirubinemia (without Rh disease). aStillbirths due to non-Rh disease have not been estimated or included.
Number of infants with major impairments due to kernicterus as presented for hearing loss (white bars) and athetoid cerebral palsy (black bars). Data shown for all live births in 2010 are shown for regional geographic distribution. Regional categorization of countries is consistent with the global burden of diseases (54,55).
Discussion
Our study is the first to provide global estimates of Rh disease and EHB, in addition to the resulting burden, in terms of deaths and impairment. Every year, ~24 million pregnancies and their babies are at risk worldwide. The global burden of EHB and Rh disease is disproportionately heavy for the poorest countries: 11-fold higher for infants born in countries with NMR >15 compared with those with NMR <5 (384,600 vs. 5,600 live births affected, with prevalence of 480 vs. 42 per 100,000 live births). The outcomes are affected by lack of both preventive services and care ( Figure 5 ).
Of the 480,700 live births at risk of Rh disease, 24% were at risk of neonatal death (114,100; uncertainty range: 59,700–172,000), 13% at risk for kernicterus (75,400; uncertainty range: 43,200–95,800), and 11% for stillbirths. Yet, knowledge of Rh disease has been iconic for more than 6 decades and means for its prevention have been established for more than 40 y. There has been an egregious failure to prevent Rh sensitization and its adverse consequences worldwide. The global “know–do” gap can only be bridged if nations assume their responsibility to address these disparities in maternal–child health care. Barriers include low attention to this issue, poor dissemination of evidence-based tools for effective Rh disease prevention, and high cost for the currently available immunoprophylaxis. In addition, prevention and management of EHB is even more neglected.
Our study exposes the variations in risk, and hence national data are important for effective health service planning. Currently, these newborns are born into the following three very different worlds, reflecting a transition from high neonatal mortality to preventable disability in otherwise-healthy newborns:
-
1
Countries with higher NMR (≥15) are at the highest risk for neonatal mortality due to Rh disease and EHB. Here, reduction in Rh sensitization and better care of every newborn, including management of EHB when needed, is an urgent implementation priority. The challenge is to provide unfettered and affordable access to Rh immunoprophylaxis and reach those in remote regions or those dispersed in areas of conflict and postconflict settings.
-
2
Emerging countries with lower NMR (5 to <15) that exhibit variations in the quality of care, with variable penetration of a systems approach for maternal and newborn care, including for Rh disease and EHB management. The management and prevention of Rh sensitization appears to have penetrated clinical practice, but it does not seem to be universal. On the other hand, EHB burden is vastly underestimated for preterm birth, G6PD deficiency, and unrecognized neonatal hemolysis. In addition, causes for underlying neonatal mortality are erroneously labeled and not attributed to kernicterus, which leads to further underestimation of its disease burden. Here, there is an urgent need to strengthen neonatal screening and delivery services and to focus on the outcome of impairment-free survival.
-
3
High-income countries, with NMR <5, have achieved both a near elimination of neonatal mortality associated with kernicterus and reductions in impairment. Here, a better identification of postnatal hemolysis and improved management of idiopathic etiologies remain as challenges.
Our estimates suggest that Rh disease accounts for the majority of the total global EHB burden (uncertainty range: 271,800–477,500). Although it should be underlined that our study vastly underestimates the burden of EHB because we excluded cases of extreme preterm birth (<32 wk GA) and those with infections to avoid double counting with the burden estimates for those conditions because a neonatal death in a very preterm neonate or in one with severe infection and jaundice but no clear cause of hemolysis would be attributed to preterm birth or infections as a cause of death by International Classification of Diseases rules. In addition, given the lack of population-based risk data, we relied on estimates of risk from one low-mortality context in Canada for preterm birth, G6PD deficiency, and unrecognized neonatal hemolysis, including ABO incompatibility, which will be much lower than the reality in many other countries ( Table 2 ).
Estimates from high-income nations reveal benign outcomes for most infants affected by Rh disease. For example, kernicterus mortality trends in the United States from 1979 to 2006 used data from the US National Center for Health Statistics of 108,888,600 live births; the crude kernicterus death rate was estimated at 0.28 (95% CI: 0.25, 0.40) with a significantly higher risk in males (28). In the same retrospective review of kernicterus among children born from 1988 to 1997 in California, the time trend data estimated an incidence of 0.44 cases (95% CI: 0.28, 0.65) per 100,000 annual live births. Incidence of EHB due to conditions other than Rh disease following systematic prevention of Rh disease in the United States, for 4 decades before 2004 was estimated at a prevalence of 169/100,000 live births (76) and has now declined to 40/100,000 live births through implementation of a systems approach (71). Unlike in the United States, the Rh disease burden remains extraordinarily high among countries with NMR ≥5 and overshadows EHB due to other causes.
Lack of Unfettered Access to Neonatal Services and Risk of Impairment
The “screen and prevent approach,” which implements a systems approach, has started to transform the EHB burden, particularly in countries with NMR <10. The current prevalence of EHB-related mortality in nations with good access to neonatal services (>90% access to NICU) compared with those having marginal care (a combination of basic and NICU care) shows extraordinary disparity. Data availability and inconsistent definitions varied, with the least data coming from the highest-burden settings. From a global perspective, we estimate that among countries with NMR >15, infants with EHB were least likely to be admitted to a facility where they can receive the required specialized and coordinated perinatal-NICU care. Overall, 46/100,000 live births (83% of survivors with kernicterus) were estimated to have long-term neurodevelopmental impairment ( Table 5 ). Our estimates of 36,000 cases of cerebral palsy (uncertainty range: 15,000–55,000) globally is undoubtedly an underestimate because of our reliance on the Canadian data for risk of impairment, apart from the exclusion of those with extreme preterm birth and infections. Indeed, a newborn who is preterm, with infection and jaundice, is at the highest risk of impairment (77). Here, South Asia and sub-Saharan Africa were estimated at 26,000 (37/100,000) vs. 560 cases (5/100,000 live births) from high-income countries (approximately an eightfold higher burden). Low coverage and the quality of pre- and postnatal coordination for “health services” is specifically exemplified by the ineffective Rh immunoprophylaxis in low- and middle-income countries. The transition of health services in certain Eastern Europe/Central Asian countries illustrates the high prevalence of Rh sensitization, but a much lower prevalence of Rh disease adverse outcomes, compared with the situation in South Asia and sub-Saharan Africa.
Data Limitations
Presently, no single replicable test exists to further measure the risks for EHB. Hence, we sought to estimate burden as conservatively as possible, including ABO incompatibility in other causes of EHB because ABO hemolytic disease alone has not been shown to cause neonatal death (1,6,8,27). A recent retrospective review suggests a statistically significant interaction between a positive Coombs test, EHB, and lower intelligence quotient during childhood (61), but more population-based data are needed to define the magnitude of this risk. G6PD deficiency prevalence data are limited, especially regarding defined enzyme level activity adjusted for gender. Adverse exacerbations by exposures to drugs, toxins, infections, and dietary agents add to the unpredictable risk of EHB due to G6PD deficiency (35) and are underestimated in our study due to reliance on the risk data from Canada alone. The EHB risk among late and moderate preterm birth we applied was minimal (about 5% or less) because we used a very high bilirubin threshold to define EHB and the risk from the Danish and Canadian data, which are in the context of very high–capacity neonatal care. Adjustment for risk for developing bilirubin neurotoxicity among preterm infants is more complex (2). Thus, we believe that we have significantly underestimated the prevalence of neonatal hemolysis, G6PD deficiency, and prematurity-related EHB. Similarly, race and ethnicity often affect bilirubin elimination disorders due to an array of genetic conditions masking as idiopathic factors (1,2). In developing nations, vulnerability to EHB continues to be confounded by comorbidities that include sepsis, intrauterine growth restriction, and unscreened inborn errors. We also did not study infants who received an exchange blood transfusion at lower TB values in the absence of acute kernicterus, those who were too moribund to receive an exchange blood transfusion, or for whom there were no resources to perform the procedure. We did not include children with the subtler form of bilirubin-induced neurologic dysfunction, and hence the results presented are likely to be an underestimate of the total burden of impairment following hyperbilirubinemia. In view of insufficient data and the likely preponderance of newborn female discrimination at birth and gender-selective referrals to tertiary care, we elected to forgo the highlighting of gender differences in our model.
Data Improvement and Programmatic Implications
Coupled with promotion of maternal and newborn care, inclusion of essential newborn care—particularly breastfeeding—and better care of preterm babies, including kangaroo mother care and safer management of neonatal jaundice, are key to public policies that engender better neonatal survival, improved long-term development, and reduced disability (78).
Important “know–do” gaps that need attention include the following:
-
1
Primary prevention, especially operationalizing systems strategies, including national identification of all Rh-negative women before or during pregnancy and ensuring that they receive Rh immunoprophylaxis postpartum and ideally at the 28th wk of pregnancy with coordinated obstetric and neonatal care. This will necessitate building partnerships with families and mobilizing community awareness.
-
2
Secondary prevention through care of affected pregnancies and neonates, harnessing and implementing affordable and proven-effective technologies for identification of and improved newborn care, as being promoted by the Every Newborn Action Plan (79).
-
3
Tertiary prevention through early identification and care of affected survivors to address long-term medical and scholastic impairments among those exposed to severe hyperbilirubinemia.
-
4
Improved data and use of data, including consistent definitions of risk and outcomes to be measured during routine data collection and in special cohort studies.
Conclusions
The failure to prevent Rh sensitization and manage EHB results in the global burden of neonatal hyperbilirubinemia falling most heavily on the world’s poorest countries, especially in South Asia and sub-Saharan Africa. Knowledge gained to prevent Rh disease 6 decades ago in high-income countries has not been consistently implemented. The very fact that we are forced to rely on data from Europe and the United States, now 70 y old, shows the low priority given to this condition. Global and national leadership is needed to mobilize action and embed proven systems approaches, policies, and programs to substantially and sustainably reduce newborn deaths and disability, including jaundice-related mortality and disabilities.
Statement of Financial Support
The study was funded in part by the March of Dimes Prematurity Research Center at Stanford University School of Medicine. This article is published as part of a supplement sponsored by The Bill and Melinda Gates Foundation to the Child Health Epidemiology Reference Group (CHERG) through the US Fund for UNICEF and to Save the Children’s Saving Newborn Lives program.
Disclosure
V.K.B. has received grant support from the National Institutes of Health (NIH). H.B. and S.C. have received grant support from the Bill and Melinda Gates Foundation through the Child Health Epidemiology Reference Group. T.S. has received grant support from the NIH and Thrasher Research Fund. J.L. has received grant support from the Bill and Melinda Gates Foundation through Save the Children’s Saving Newborn Lives program. The authors declared no conflict of interest.
References
American Academy of Pediatrics Subcommittee on H. Management of hyperbilirubinemia in the newborn infant 35 or more weeks of gestation. Pediatrics 2004;114:297–316.
Maisels MJ, Bhutani VK, Bogen D, Newman TB, Stark AR, Watchko JF . Hyperbilirubinemia in the newborn infant > or =35 weeks’ gestation: an update with clarifications. Pediatrics 2009;124:1193–8.
Bhutani VK, Stark AR, Lazzeroni LC, et al.; Initial Clinical Testing Evaluation and Risk Assessment for Universal Screening for Hyperbilirubinemia Study Group. Predischarge screening for severe neonatal hyperbilirubinemia identifies infants who need phototherapy. J Pediatr 2013;162:477–482.e1.
Keren R, Tremont K, Luan X, Cnaan A . Visual assessment of jaundice in term and late preterm infants. Arch Dis Child Fetal Neonatal Ed 2009;94:F317–22.
Johnson LH, Bhutani VK, Brown AK . System-based approach to management of neonatal jaundice and prevention of kernicterus. J Pediatr 2002;140:396–403.
Ip S, Chung M, Kulig J, et al.; American Academy of Pediatrics Subcommittee on Hyperbilirubinemia. An evidence-based review of important issues concerning neonatal hyperbilirubinemia. Pediatrics 2004;114:e130–53.
Fetus and Newborn Committee CPSC. Guidelines for detection, management and prevention of hyperbilirubinemia in term and late preterm newborn infants (35 or more weeks’ gestation). J Paediatr Child Health 2007;1B-12B:FN07–2.
Trikalinos TA, Chung M, Lau J, Ip S . Systematic review of screening for bilirubin encephalopathy in neonates. Pediatrics 2009;124:1162–71.
Rennie J, Burman-Roy S, Murphy MS ; Guideline Development Group. Neonatal jaundice: summary of NICE guidance. BMJ 2010;340:c2409.
Bratlid D, Nakstad B, Hansen TW . National guidelines for treatment of jaundice in the newborn. Acta Paediatr 2011;100:499–505.
Zipursky A . The universal prevention of Rh immunization. Clin Obstet Gynecol 1971;14:869–84.
Zipursky A . Prevention of Rh immunization. Can Med Assoc J 1975;113:227.
Zipursky A . Rh hemolytic disease of the newborn–the disease eradicated by immunology. Clin Obstet Gynecol 1977;20:759–72.
Zipursky A . The conquest of Rh disease. Can Med Assoc J 1978;118:609–10.
Vaughan VC . Kernicterus in erythroblastosis fetalis. J Pediatr 1946;29:462–73.
Vaughan VC 3rd, Allen FH Jr, Diamond LK . Erythroblastosis fetalis. I. Problems in the interpretation of changing mortality in erythroblastosis fetalis. Pediatrics 1950;6:173–82.
Mollison PL, Cutbush M . Exchange transfusion in haemolytic disease of the newborn. Lancet 1948;2:522–7.
Mollison PL, Cutbush M . Haemolytic disease of the newborn; criteria of severity. Br Med J 1949;1:123–30.
Mollison PL, Walker W . Controlled trials of the treatment of haemolytic disease of the newborn. Lancet 1952;1:429–33.
Hsia DY, Allen FH Jr, Gellis SS, Diamond LK . Erythroblastosis fetalis. VIII. Studies of serum bilirubin in relation to kernicterus. N Engl J Med 1952;247:668–71.
Allen FH Jr . Selection of blood for exchange transfusion in erythroblastosis fetalis. Bibl Haematol 1968;29:241–6.
Armitage P, Mollison PL . Further analysis of controlled trials of treatment of haemolytic disease of the newborn. J Obstet Gynaecol Br Emp 1953;60:605–20.
Walker WC . Haemolytic Disease of the Newborn in Recent Advances in Paediatrics, 4th edn. London, UK: J.A. Churchill, 1970.
Diamond I, Odell GB, Johnson L, Boggs TR, Lucey JF . Kernicterus: revised concepts of pathogenesis and management. Pediatrics 1966;38:539–46.
Ip S, Lau J, Chung M, et al. Hyperbilirubinemia and kernicterus: 50 years later. Pediatrics 2004;114:263–4.
Johnson L, Bhutani VK, Karp K, Sivieri EM, Shapiro SM . Clinical report from the pilot USA Kernicterus Registry (1992 to 2004). J Perinatol 2009;29:Suppl 1:S25–45.
Kuzniewicz MW, Escobar GJ, Newman TB . Impact of universal bilirubin screening on severe hyperbilirubinemia and phototherapy use. Pediatrics 2009;124:1031–9.
Brooks JC, Fisher-Owens SA, Wu YW, Strauss DJ, Newman TB . Evidence suggests there was not a “resurgence” of kernicterus in the 1990s. Pediatrics 2011;127:672–9.
Bhutani VK, Stevenson DK . The need for technologies to prevent bilirubin-induced neurologic dysfunction syndrome. Semin Perinatol 2011;35:97–100.
Slusher TM, Zipursky A, Bhutani VK . A global need for affordable neonatal jaundice technologies. Semin Perinatol 2011;35:185–91.
Cline BK, Vreman HJ, Faber K, et al. Phototherapy device effectiveness in Nigeria: irradiance assessment and potential for improvement. J Trop Pediatr 2013;59:321–5.
Moise KJ Jr . Management of rhesus alloimmunization in pregnancy. Obstet Gynecol 2002;100:600–11.
Howes RE, Piel FB, Patil AP, et al. G6PD deficiency prevalence and estimates of affected populations in malaria endemic countries: a geostatistical model-based map. PLoS Med 2012;9:e1001339.
Nkhoma ET, Poole C, Vannappagari V, Hall SA, Beutler E . The global prevalence of glucose-6-phosphate dehydrogenase deficiency: a systematic review and meta-analysis. Blood Cells Mol Dis 2009;42:267–78.
Watchko JF, Kaplan M, Stark AR, Stevenson DK, Bhutani VK . Should we screen newborns for glucose-6-phosphate dehydrogenase deficiency in the United States? J Perinatol 2013;33:499–504.
Chinevere TD, Murray CK, Grant E Jr, Johnson GA, Duelm F, Hospenthal DR . Prevalence of glucose-6-phosphate dehydrogenase deficiency in U.S. Army personnel. Mil Med 2006;171:905–7.
Luzzatto L, Notaro R . Malaria. Protecting against bad air. Science 2001;293:442–3.
Kaplan M, Beutler E, Vreman HJ, et al. Neonatal hyperbilirubinemia in glucose-6-phosphate dehydrogenase-deficient heterozygotes. Pediatrics 1999;104(1 Pt 1):68–74.
WHO Working Group. WHO, glucose-6-phosphate dehydrogenase deficiency. Bull World Health Organ 1981;67:61–7.
Kaplan M, Hammerman C . The need for neonatal glucose-6-phosphate dehydrogenase screening: a global perspective. J Perinatol 2009;29:Suppl 1:S46–52.
Blencowe H, Cousens S, Oestergaard MZ, et al. National, regional, and worldwide estimates of preterm birth rates in the year 2010 with time trends since 1990 for selected countries: a systematic analysis and implications. Lancet 2012;379:2162–72.
Engle WA, Tomashek KM, Wallman C ; Committee on Fetus and Newborn, American Academy of Pediatrics. “Late-preterm” infants: a population at risk. Pediatrics 2007;120:1390–401.
Crosse VM, Meyer TC, Gerrard JW . Kernicterus and prematurity. Arch Dis Child 1955;30:501–8.
Bhutani VK, Maisels MJ, Stark AR, Buonocore G ; Expert Committee for Severe Neonatal Hyperbilirubinemia; European Society for Pediatric Research; American Academy of Pediatrics. Management of jaundice and prevention of severe neonatal hyperbilirubinemia in infants >or=35 weeks gestation. Neonatology 2008;94:63–7.
Perlstein MA . Neurologic sequelae of erthroblastosis fetalis. Am J Dis Child 1950;79:605–6.
Shapiro SM . Definition of the clinical spectrum of kernicterus and bilirubin-induced neurologic dysfunction (BIND). J Perinatol 2005;25:54–9.
Scheidt PC, Graubard BI, Nelson KB, et al. Intelligence at six years in relation to neonatal bilirubin levels: follow-up of the National Institute of Child Health and Human Development Clinical Trial of Phototherapy. Pediatrics 1991;87:797–805.
Olusanya BO, Okolo AA . Adverse perinatal conditions in hearing-impaired children in a developing country. Paediatr Perinat Epidemiol 2006;20:366–71.
Vohr BR, Lester B, Rapisardi G, et al. Abnormal brain-stem function (brain-stem auditory evoked response) correlates with acoustic cry features in term infants with hyperbilirubinemia. J Pediatr 1989;115:303–8.
Matkin ND, Carhart R . Hearing acuity and Rh incompatibility. Electrodermal thresholds. Arch Otolaryngol 1968;87:383–8.
Byers RK, Paine RS, Crothers B . Extrapyramidal cerebral palsy with hearing loss following erythroblastosis. Pediatrics 1955;15:248–54.
Perlman M, Fainmesser P, Sohmer H, Tamari H, Wax Y, Pevsmer B . Auditory nerve-brainstem evoked responses in hyperbilirubinemic neonates. Pediatrics 1983;72:658–64.
Johnson L, Bhutani VK . The clinical syndrome of bilirubin-induced neurologic dysfunction. Semin Perinatol 2011;35:101–13.
United Nations Population Division. 2010. (http://hdr.undp.org/en/statistics/.) Accessed October 2011.
Blencowe H, Vos T, Lee AC, et al. Estimates of neonatal morbidities and disabilities at regional and global levels for 2010: introduction, methods overview, and relevant findings from the Global Burden of Disease study. Pediatr Res 2013 (this issue).
Liu L, Johnson H, Cousens S, et al. Global, regional and national causes of child mortality: an updated systematic analysis for 2010 with time trends since 2000. Lancet 2012;379:2151–61.
Murray CJ, Ezzati M, Flaxman AD, et al. GBD 2010: design, definitions, and metrics. Lancet 2012;380:2063–6.
Brown AK, Kim MH, Wu PY, Bryla DA . Efficacy of phototherapy in prevention and management of neonatal hyperbilirubinemia. Pediatrics 1985;75(2 Pt 2):393–400.
Mah MP, Clark SL, Akhigbe E, et al. Reduction of severe hyperbilirubinemia after institution of predischarge bilirubin screening. Pediatrics 2010;125:e1143–8.
Eggert LD, Wiedmeier SE, Wilson J, Christensen RD . The effect of instituting a prehospital-discharge newborn bilirubin screening program in an 18-hospital health system. Pediatrics 2006;117:e855–62.
Kuzniewicz M, Newman TB . Interaction of hemolysis and hyperbilirubinemia on neurodevelopmental outcomes in the collaborative perinatal project. Pediatrics 2009;123:1045–50.
Cousens S, Blencowe H, Stanton C, et al. National, regional, and worldwide estimates of stillbirth rates in 2009 with trends since 1995: a systematic analysis. Lancet 2011;377:1319–30.
Ebbesen F . Recurrence of kernicterus in term and near-term infants in Denmark. Acta Paediatr 2000;89:1213–7.
Ebbesen F, Andersson C, Verder H, et al. Extreme hyperbilirubinaemia in term and near-term infants in Denmark. Acta Paediatr 2005;94:59–64.
Ebbesen F, Bjerre JV, Vandborg PK . Relation between serum bilirubin levels =450 µmol/L and bilirubin encephalopathy; a Danish population-based study. Acta Paediatr 2012;101:384–9.
Sgro M, Campbell D, Barozzino T, Shah V . Acute neurological findings in a national cohort of neonates with severe neonatal hyperbilirubinemia. J Perinatol 2011;31:392–6.
Sgro M, Campbell D, Shah V . Incidence and causes of severe neonatal hyperbilirubinemia in Canada. CMAJ 2006;175:587–90.
Sgro M, Campbell DM, Kandasamy S, Shah V . Incidence of chronic bilirubin encephalopathy in Canada, 2007-2008. Pediatrics 2012;130:e886–90.
Vandborg PK, Hansen BM, Greisen G, Jepsen M, Ebbesen F . Follow-up of neonates with total serum bilirubin levels = 25 mg/dL: a Danish population-based study. Pediatrics 2012;130:61–6.
Seale AC, Blencowe H, Zaidi A, et al. Neonatal severe bacterial infection impairment estimates in South Asia, sub-Saharan Africa, and Latin America for 2010. Pediatr Res 2013 (this issue).
Christensen RD, Lambert DK, Henry E, et al. Unexplained extreme hyperbilirubinemia among neonates in a multihospital healthcare system. Blood Cells Mol Dis 2013;50:105–9.
Kaplan M, Bromiker R, Schimmel MS, Algur N, Hammerman C . Evaluation of discharge management in the prediction of hyperbilirubinemia: the Jerusalem experience. J Pediatr 2007;150:412–7.
Facchini FP, Mezzacappa MA, Rosa IR, Mezzacappa Filho F, Aranha-Netto A, Marba ST . Follow-up of neonatal jaundice in term and late premature newborns. J Pediatr (Rio J) 2007;83:313–22.
Newman TB, Xiong B, Gonzales VM, Escobar GJ . Prediction and prevention of extreme neonatal hyperbilirubinemia in a mature health maintenance organization. Arch Pediatr Adolesc Med 2000;154:1140–7.
Manning D, Todd P, Maxwell M, Jane Platt M . Prospective surveillance study of severe hyperbilirubinaemia in the newborn in the UK and Ireland. Arch Dis Child Fetal Neonatal Ed 2007;92:F342–6.
Newman TB, Klebanoff MA . Neonatal hyperbilirubinemia and long-term outcome: another look at the Collaborative Perinatal Project. Pediatrics 1993;92:651–7.
Mwaniki MK, Atieno M, Lawn JE, Newton CR . Long-term neurodevelopmental outcomes after intrauterine and neonatal insults: a systematic review. Lancet 2012;379:445–52.
Bhutani VK . Public Policy to Prevent Severe Neonatal Hyperbilirubinemia. New York, NY: McGraw Hill Professional, 2012.
Every newborn: an action plan to end preventable deaths. (http://www.globalnewbornaction.org.)
Acknowledgements
Global Prevent Kernicterus Network: Lois Johnson (USA); Martin Castillo Cuadrado (Life Science Research Assistant, Stanford University); Ronald J. Wong (Stanford University); Iman Seoud and Iman Iskander (Cairo, Egypt); Hameed Numan Alhamdani (Baghdad, Iraq); Joshua Owa (Ife-Ife, Nigeria); Priscilla Joe (Children’s Hospital of Oakland, CA); Margaret Manley (PGPR), Adam Miller (PGPR), Sharmilaa Kandasamy (Research Coordinator, Inner City Health Research, St. Michael’s Hospital, Toronto, Ontario, Canada), and Judith Stanke, Tara Zamora, Kathleen Warner, Elizabeth Keating, and Shane Richardson (University of Minnesota).
Author information
Authors and Affiliations
Corresponding author
Supplementary information
Web appendix
(DOC 1313 kb)
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Bhutani, V., Zipursky, A., Blencowe, H. et al. Neonatal hyperbilirubinemia and Rhesus disease of the newborn: incidence and impairment estimates for 2010 at regional and global levels. Pediatr Res 74 (Suppl 1), 86–100 (2013). https://doi.org/10.1038/pr.2013.208
Published:
Issue Date:
DOI: https://doi.org/10.1038/pr.2013.208
This article is cited by
-
Validity of BiliDx as a point-of-care bilirubin measurement device to diagnose and monitor neonatal jaundice at Muhimbili National Hospital, an observational study
BMC Pediatrics (2024)
-
Acceptability and operational feasibility of community health worker-led home phototherapy treatment for neonatal hyperbilirubinemia in rural Bangladesh
BMC Pediatrics (2024)
-
Predictive and diagnostic measures for kernicterus spectrum disorder: a prospective cohort study
Pediatric Research (2024)
-
Chemoprevention of bilirubin encephalopathy with a nanoceutical agent
Pediatric Research (2023)
-
Advances to diminish global newborn kernicterus mortality
Journal of Perinatology (2023)