Abstract
Current guidelines strongly recommend the identification of genetic forms of hypercholesterolemia (HC) during childhood. The usefulness of non–cholesterol sterols (NCS) in the diagnosis of genetic HC has not been fully explored. Plasma NCS were measured by gas chromatography/mass spectrometry (GC/MS) in 113 children with hypercholesterolemia affected by: autosomal dominant hypercholesterolemia (ADH), familial combined hyperlipidemia (FCHL), polygenic hypercholesterolemia (PHC), and in 79 controls to evaluate: i) plasma NCS profile in different genetic HC and ii) the usefulness of NCS for the diagnosis of HC beyond current clinical criteria. ADH was characterized by raised lathosterol/total cholesterol (TC) and reduced phytosterols/TC ratios, indicative of increased cholesterol synthesis. FCHL showed a slight increase of lathosterol/TC ratio, whereas PHC showed increased phytosterols/TC ratios, indicative of increased cholesterol absorption. In a post hoc discriminant analysis of patients with HC, lipid values correctly classified the 73% (14 of 19) of ADH, whereas the inclusion of plasma sterols allowed the correct identification of all 19 patients with ADH. FCHL was not differentiated from PHC (62 versus 69%). In conclusion, NCS measurement showed that cholesterol plasma levels are related to the cholesterol synthesis in ADH and to cholesterol absorption in PHC. NCS improve the detection of ADH in pediatric patients, whereas FCHL diagnosis is not improved.
Similar content being viewed by others
Main
Inherited hypercholesterolemias (HC) are burdened by premature cardio- and cerebrovascular (CV) events (1). An early identification of genetic HC (2,3) allows the prescription of lifestyle changes and/or drug therapy even in childhood, thus increasing the probability to prevent future CV events (4). The clinical diagnosis of these genetic HC in childhood is not a simple task because of the variability of plasma lipids levels used as diagnostic criteria and of the unclear transmission of the inherited trait (5). As a consequence, the DNA sequencing of the candidate genes LDLR, APOB, and PCSK9 remains the gold standard for autosomal dominant hypercholesterolemia (ADH) diagnosis. To date, no genes responsible for familial combined hyperlipidemia (FCHL) or polygenic hypercholesterolemia (PHC) have been identified.
Plasma cholesterol homeostasis relies mainly on two physiologic mechanisms: intestinal cholesterol absorption and liver cholesterol synthesis, which are cross-regulated to maintain plasma cholesterol levels (6). Measurable plasma markers of these two processes have been identified. Liver cholesterol synthesis has been found to be related to plasma levels of lathosterol (7), a precursor sterol in the cholesterol synthetic chain, whereas cholesterol intestinal absorption is proportional to plasma levels of phytosterols (mainly campesterol and sitosterol), which are plant-derived sterols that cannot be synthesized but only absorbed by the intestine (6). Subjects can be classified on the basis of their plasma non–cholesterol sterols profile in “high absorbers” when cholesterol absorption prevails on synthesis and “high producers” when synthesis is prevalent. Cholesterol absorption contributes significantly to plasma cholesterol levels, as demonstrated by population studies showing that polymorphic variants of the NPC1L1 gene, encoding for the protein responsible for cholesterol absorption, associate with lower levels of plasma LDL cholesterol (8).
The aim of this study is to explore the spectrum of non–cholesterol sterols profiles in children with the three major forms of genetic HC: ADH (OMIM 143890), FCHL (OMIM 144250), and PHC, defined on the basis of the combination of family data and molecular analysis. In addition, we evaluated whether the measurement of plasma non–cholesterol sterols may represent a useful biochemical tool able to support the clinical diagnosis of genetic HC.
METHODS
Index subjects were recruited from children with HC referred to two outpatient Lipid Clinics: the “Lipid Clinic” of the Department of Pediatrics, University of Rome “La Sapienza,” Rome, Italy and the “Inherited Dyslipidemias Clinic” of the Department of Clinical Medicine and Emerging Diseases, University of Palermo. At their first visit, lipids and lipoproteins were measured in index children and in available siblings and in their parents. Informed consent was obtained from parents and the study was approved by the University of Rome “La Sapienza,” and University of Palermo Ethical Committees. Demographic and clinical information were collected in all family members. A physical examination including the evaluation of tendon xanthomas and a collection of antrophometrical measurements were also included in the study protocol.
Exclusion criteria in this study included age younger than 2 y or older than 18 y, hypothyroidism, renal diseases, malignancy, and any acute illness. All children with dyslipidemia currently on drug therapy (including statins, dietary stanols, or resins) were excluded. Children with HC were also excluded if their available plasma samples showed total cholesterol (TC) concentrations lower than the 85% of the maximum value filed in their clinical records.
One hundred thirteen patients with HC were included in the study and characterized as follows:
Autosomal dominant hypercholesterolemia.
ADH was diagnosed in children with LDL (C) levels >90th age-related percentile and plasma triglyceride (TG) <75th age-related percentile, with at least one of the parents showing the same phenotype (9). The molecular defect was identified in ADH probands by sequencing the LDLR, APOB, and PCSK9 genes. First-degree relatives of ADH probands with identified gene mutations underwent DNA sequencing regardless the LDL (C) plasma levels. The heterozygous ADH (HeADH) group consisted of 17 patients identified as carriers of 12 different mutations of the LDLR gene (c.515 A>G, c.671 A>G, c.1118 G>A, c.1162 del C, c.1166 C>T, c.1257 C>G, c.1381 G>T, c.1567 G>A, c.1593 del GTAC, c.1646 G>A, c.2024 del G, c.2390–1 G>A) and two patients with clinical diagnosis of definite ADH but negative for mutations of candidate genes. The homozygous ADH (HoADH) group consisted of two probands carrying three mutations of the LDLR gene (c.671 A>G in a homozygous patient and c.1618 G>A/ c.1775 G>A in a compound heterozygous patient).
Familial combined hyperlipidemia.
FCHL was diagnosed in 39 children with TC >90th percentile and/or TG >75th percentile with at least a first-degree relative showing a similar lipid profile (9). Because a previous report (10) demonstrated that ADH probands can be found among FCHL kindred by molecular analysis of candidate genes, we performed the analysis of candidate genes in those FCHL probands showing increased TG values possibly due to nongenetic causes, such as overweight or obesity. None of the patients with ADH were identified by this approach.
Polygenic hypercholesterolemia.
PHC was diagnosed in 63 children with LDL (C) levels between the 75th and the 90th age- and sex-related percentiles and TG <75th percentile.
Normolipidemic controls.
Seventy-nine healthy normolipidemic controls (NC) were recruited among nonaffected members of the families with dyslipidemia, showing TC and TG plasma levels <75th age- and gender-adjusted percentiles.
Plasma lipids were measured by standard colorimetric assays. LDL (-C) was calculated by the Friedewald formula. Plasma non–cholesterol sterols were assayed by gas chromatography/mass spectrometry (GC/MS) as published by others (11) with some modifications. Briefly, a plasma volume containing 70 μg of cholesterol was processed. This procedure normalized the amount of cholesterol loaded into the chromatographic column because the different TC concentrations between patients with NC and ADH could have affected the analysis of the chromatograms. After the addition of 5β-Cholestan-3a-ol (epicoprostanol) as internal standard, sterols were derivatized in N, O–bis(trimethylsilyl) (trifluoracetamide) (BSTFA): trimethylchlorosilane (TMCS): Pyridine (99:1:100) and loaded through a refrigerated ALS100 autosampler (Agilent Technologies, Santa Clara, CA) on a HP1313 low-polarity column (Agilent Technologies) in a Agilent HP5890 gas chromatograph. The m/z ratios were collected by an Agilent HP5973N mass spectrometer in single-ion monitoring (SIM) mode. Characteristics ions for each sterol were chosen by injecting true standards spiked on a plasma matrix and selecting all the ions exhibiting the best peak purity. The following m/z ratios were selected: epicoprostanol (IS): 355 and 370, cholesterol: 458, lathosterol: 255 and 458, campesterol: 255 and 472, and sitosterol: 396 and 486. Calibration curves were built spiking plasma replicates with increasing amounts of true sterols standards. All curves were highly linear (Pearson's R > 0.99) between 0.5 μg/L and 25 μg/L of sterols plasma concentrations (data not shown). All standards and reagents were purchased from Sigma Chemical Co.-Aldrich (St. Louis, MO).
The analysis of the ADH candidate genes (LDLR, APOB, and PCSK9) was carried out by direct sequencing as previously described (12). When possible, the identified sequence variations were confirmed by restriction fragment length polymorphism (RFLP) analysis using appropriate restriction enzymes. Gene rearrangements were excluded by Southern blotting (12).
Sterols to TC ratios, as measures of cholesterol synthesis and absorption, were multiplied by a 103 factor. Plasma sterols levels distributions were slightly right skewed, data are presented as median (min value−max value). One-to-one differences between HC and NC groups were assessed by the Kruskal-Wallis rank test. Suspicious significance values obtained in a condition of lack of sample numerosity were recalculated by the Mann-Whitney test followed by a “post hoc” Bonferroni adjustment of probability values.
Variables were log transformed and checked for normality by the one-sample Kolmogorov-Smirnov using the Lillefort variant. After log transform, the power of plasma sterols to discriminate the different hyperlipoproteinemias (HLPs) was assessed by a multivariate discriminant analysis using a first model that excluded plasma sterols and a second model that included the sterols. Backward removal of noncontributing variables was used. Simultaneous correlations between plasma lipids and non–cholesterol sterols were evaluated as partial correlations, to adjust for age and male gender as covariates.
All calculations were performed using either the SYSTAT 10 (SPSS Inc, CA) or the CRUNCH 4.0 (Crunch Corporation, CA) statistical software packages.
RESULTS
One hundred thirteen children with HC and 79 NC were included in the study. Table 1 shows data of age, sex, and plasma lipids. As expected, all patients with HC had higher plasma TC and LDL (C) levels compared with NC, whereas patients with FCHL also had higher plasma TG values. Patients with PHC showed higher plasma HDL (C) levels compared with NC.
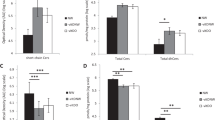
Table 2 reports data on sterols concentrations presented as median (min−max values) and the ratios of sterols/TC. Plasma non–cholesterol sterols absolute concentrations were increased in patients HC versus NC, except campesterol in HeADH. The main cholesterol synthesis index (lathosterol/TC) was higher in all patients with HC with the exception of patients with PHC. The main cholesterol absorption index (campesterol/TC) was lower in ADH versus NC but higher in patients with PHC versus NC, and also the sitosterol/TC ratio showed a similar behavior.
The lathosterol/campesterol and lathosterol/sitosterol ratios are not affected by the different TC values in children with HC and NC, measuring the unbiased synthesis/absorption balance. These ratios are higher only in ADH, suggesting a predominance of cholesterol synthesis over absorption. Children with HoADH showed an index of cholesterol synthesis 2-fold higher the value of subjects with HeADH (2.15 ± 1.7 versus 1.04 ± 0.5). Also, the absorption indexes were higher in HoADH (campe/TC 0.96 ± 0.3 versus 0.83 ± 0.5, sito/TC 1.85 ± 0.3 versus 1.20 ± 0.7), so that the resulting sterol balance is similar in the two ADH groups. Conversely, elevated values of cholesterol absorption indexes led to a decreased lathosterol/sitosterol ratio in patients with PHC.
Table 3 reports the results of the post hoc multivariate discriminant analyses designed to evaluate the power of plasma non–cholesterol sterols to distinguish between different forms of HC. Patients with HeADH, FCHL, and PHC were included in the two models while HoADH were excluded because of the very elevated cholesterol levels compared with the other groups. Model 1 considered only the plasma lipids and model 2 also included absolute plasma concentrations of non–cholesterol sterols, sterols/TC ratios, and sterol/sterol ratios. The plasma lipids alone were able to correctly classify the 67% of the patients with HC, whereas the addition of the plasma sterols increased the percent of correctly classified cases to 86%. Moreover, the model 2 was very powerful in identifying ADH (19 of 19 correctly allocated patients), whereas FCHL and PCH were still misclassified (18 of 29 correctly allocated patients with FCHL and 50 of 63 correctly allocated patients with PCH).
To investigate the relationships of cholesterol synthesis and absorption with plasma lipids levels in children without monogenic disorders, we evaluated the correlations of cholesterol absorption and synthesis indexes with TC, TG, and HDL (C) in the whole study sample (N = 171 subjects) with the exclusion of 21 children with ADH. The results of Table 4 show that TC, HDL (C), and LDL (C) plasma levels were correlated mainly to the cholesterol absorption indexes, whereas TG levels were correlated mainly to cholesterol synthesis index. TG and HDL (C) levels correlated inversely with plasma non–cholesterol sterols indexes.
DISCUSSION
Detection and treatment of genetic HC in childhood have been strongly advocated to prevent atherosclerosis (13,14). ADH, due to mutations of the LDLR gene, represents the most common genetic hyperlipidemia detectable in childhood. An accepted guideline for the diagnosis of ADH is based on the presence of vertically inherited very high LDL (C) levels (5,13), but the chosen LDL (C) cutoffs have been proven to be very specific but not enough sensitive. Population average cholesterol levels are affected by genetic and environmental factors. As a consequence, LDL (C) percentile-related cutoffs differ among populations, making different screening programs hardly comparable (13). A LDL (C) level >3.5 mmol/L detected FH probands with a 98% chance in a Dutch population (15), whereas a higher cutoff [LDL (C) >3.9 mmol/L] showed a 79% sensitivity and 71% specificity in an Italian population (9) and a LDL (C) >4.0 mM cutoff caused a 21% of uncorrected classification among pediatric FH from an Austrian population (16). Among the clinical criteria, the presence of xanthoma may be useful, but this sign is rarely found in children with HeADH. A molecular test based on the screening of candidate genes (LDLR, APOB, and PCSK9) supports the clinical diagnosis of ADH. However, about one third of patients with a clinical diagnosis of ADH do not have detectable mutations (17).
In this context, the identification of new diagnostic tools able to integrate the current diagnostic criteria is a relevant task. In this study, we evaluated whether the measurement of plasma non–cholesterol sterols concentrations may be useful to this purpose. We have shown that the different forms of HC are characterized by different patterns of plasma non–cholesterol sterols. Patients with ADH behave as “high producers” (high lathosterol/cholesterol ratio) and as “low absorbers” (low campesterol/TC ratio). This finding is consistent with the decreased liver uptake of LDL particles due to a reduced activity of LDL receptors on the surface of cell membranes (18). The reduced influx of lipoprotein cholesterol stimulates the cholesterol synthesis, resulting in an increase of the lathosterol/TC ratio also shown by others (19) and reverted by the administration of statins (18). In patients with ADH, the intestinal absorption is decreased through a feedback mechanism (20). It is noteworthy that this peculiar plasma sterols pattern is present only in ADH, allowing us to elaborate a discriminant function able to distinguish HeADH from PCH (Table 3). Data regarding the two subjects with HoADH show that the cholesterol synthesis index (lathosterol/TC) is 2-fold higher than the HeADH value (Table 2), but the HoADH cholesterol absorption indexes are not as decreased as in HeADH. The high cholesterol absorption index in patients with HoADH of this study is supported by a recent report (20) showing much higher levels of phytosterols in an adult subject with HoADH compared with his heterozygous parents. A possible explanation of this finding may reside in the virtual absence of LDL receptors in hoADH intestinal cells in comparison with the 50% reduction of HeADH cells. The absence of LDL receptors in patients with HoADH may be able to trigger an increase of cholesterol absorption not evident in patients with HeADH.
Children with FCHL are characterized by a moderate increase of cholesterol synthesis (as suggested by the high lathosterol/TC ratio). This finding is in agreement with the increased liver apolipoprotein B-containing lipoproteins production demonstrated by kinetic studies (3). Nevertheless, the non–cholesterol sterols pattern of FCHL is not very different from PHC, causing a misclassification in the discriminant analysis reported in Table 3.
Finally, another interesting finding of this study is that children classified as PHC show an increased absorption of intestinal cholesterol. To support this finding, correlations of Table 4 show that all subjects, excluding the ones carrying a monogenic form of HC, are characterized by significant positive correlations between plasma cholesterol levels and markers of cholesterol absorption. These results suggest that genetic determinants of cholesterol absorption affect plasma cholesterol levels more than genetic determinants of cholesterol synthesis. A possible explanation of this finding is that that cholesterol synthesis might be regulated by strict feedback mechanisms, whereas cholesterol absorption might be more “deregulated,” as suggested by recent reports on polymorphic variants of the NPC1L1 and ABCG5/G8 genes able to significantly affect cholesterol and phytosterols plasma levels (8,21). Interestingly, increased cholesterol absorption indexes have been found in patients with clinical diagnosis of ADH but negative for the molecular analysis of the candidate genes (22). A growing body of evidence suggests that novel genetic determinants of cholesterol levels are yet to be found among genes controlling the cholesterol absorption process.
In evaluating these results, possible limitations must be highlighted. First of all, the definition of familial HC in our children was based on arbitrary lipid percentile cutoffs. However, similar pediatric criteria have been used by others (23). As a consequence, we cannot completely rule out the possibility that some children defined as PHC might carry LDLR gene mutations. Finally, the correct diagnosis of FCHL in childhood is still controversial. We used well-established consensus criteria for FCHL diagnosis that have been used also in other pediatric studies (9,23,24). We also refined the FCHL diagnosis by molecular analysis in those cases with possible ADH, as suggested by a recent study (10).
In conclusion, we found that the various forms of HC show distinct patterns of plasma non–cholesterol sterols. The addition of non–cholesterol sterols to plasma lipids measurement improves the identification of ADH probands. Patients with FCHL do not show a peculiar non–cholesterol sterols pattern and cannot be correctly identified by sterols analysis. Interestingly, in our pediatric sample (excluding monogenic ADH), cholesterol absorption seems to be the main determinant of plasma cholesterol levels. Further studies are necessary to test whether the plasma non–cholesterol sterols measurement may be included among the current diagnostic criteria of definite ADH.
Abbreviations
- ADH:
-
autosomal dominant hypercholesterolemia
- FCHL:
-
familial combined hyperlipidemia
- HC:
-
hypercholesterolemia
- HeADH:
-
heterozygous ADH
- HoADH:
-
homozygous ADH
- NC:
-
normolipidemic controls
- PHC:
-
polygenic hypercholesterolemia
- TC:
-
total cholesterol
References
1991 Risk of fatal coronary heart disease in familial hypercholesterolemia. Scientific Steering Committee on behalf of the Simon Broome Register Group. BMJ 303: 893–896
Rahalkar AR, Hegele RA 2008 Monogenic pediatric dyslipidemias: classification, genetics and clinical spectrum. Mol Genet Metab 93: 282–294
Venkatesan S, Cullen P, Pacy P, Halliday D, Scott J 1993 Stable isotopes show a direct relation between VLDL apoB overproduction and serum triglyceride levels and indicate a metabolically and biochemically coherent basis for familial combined hyperlipidemia. Arterioscler Thromb 13: 1110–1118
Jaeger BR, Tsobanelis T, Bengel F, Schwaiger M, Seidel D 2002 Long-term prevention of premature coronary atherosclerosis in homozygous familial hypercholesterolemia. J Pediatr 141: 125–128
Kavey RE, Allada V, Daniels SR, Hayman LL, McCrindle BW, Newburger JW, Parekh RS, Steinberger J, American Heart Association Expert Panel on Population and Prevention Science American Heart Association Council on Cardiovascular Disease in the Young American Heart Association Council on Epidemiology and Prevention American Heart Association Council on Nutrition Physical Activity and Metabolism American Heart Association Council on High Blood Pressure Research American Heart Association Council on Cardiovascular Nursing American Heart Association Council on the Kidney in Heart Disease Interdisciplinary Working Group on Quality of Care and Outcomes Research 2006 Cardiovascular risk reduction in high-risk pediatric patients: a scientific statement from the American Heart Association Expert Panel on Population and Prevention Science; the Councils on Cardiovascular Disease in the Young, Epidemiology and Prevention, Nutrition, Physical Activity and Metabolism, High Blood Pressure Research, Cardiovascular Nursing, and the Kidney in Heart Disease; and the Interdisciplinary Working Group on Quality of Care and Outcomes Research: endorsed by the American Academy of Pediatrics. Circulation 114: 2710–2738
Brown AJ 2002 Atherosclerosis: cell biology and lipoproteins: cholesterol absorption inhibitors: gateway therapy for hypercholesterolemia. Curr Opin Lipidol 13: 701–703
Miettinen TA, Tilvis RS, Kesäniemi YA 1990 Serum plant sterols and cholesterol precursors reflect cholesterol absorption and synthesis in volunteers of a randomly selected male population. Am J Epidemiol 131: 20–31
Cohen JC, Pertsemlidis A, Fahmi S, Esmail S, Vega GL, Grundy SM, Hobbs HH 2006 Multiple rare variants in NPC1L1 associated with reduced sterol absorption and plasma low-density lipoprotein levels. Proc Natl Acad Sci USA 103: 1810–1815
Campagna F, Martino F, Bifolco M, Montali A, Martino E, Morrone F, Antonini R, Cantafora A, Verna R, Arca M 2008 Detection of familial hypercholesterolemia in a cohort of children with hypercholesterolemia: results of a family and DNA-based screening. Atherosclerosis 196: 356–364
Civeira F, Jarauta E, Cenarro A, García-Otín AL, Tejedor D, Zambón D, Mallen M, Ros E, Pocoví M 2008 Frequency of low-density lipoprotein receptor gene mutations in patients with a clinical diagnosis of familial combined hyperlipidemia in a clinical setting. J Am Coll Cardiol 52: 1546–1553
Ahmida HS, Bertucci P, Franzò L, Massoud R, Cortese C, Lala A, Federici G 2006 Simultaneous determination of plasmatic phytosterols and cholesterol precursors using gas chromatography-mass spectrometry (GC-MS) with selective ion monitoring (SIM). J Chromatogr B Analyt Technol Biomed Life Sci 842: 43–47
Bertolini S, Cantafora A, Averna M, Cortese C, Motti C, Martini S, Pes G, Postiglione A, Stefanutti C, Blotta I, Pisciotta L, Rolleri M, Langheim S, Ghisellini M, Rabbone I, Calandra S 2000 Clinical expression of familial hypercholesterolemia in clusters of mutations of the LDL receptor gene that cause a receptor-defective or receptor-negative phenotype. Arterioscler Thromb Vasc Biol 20: E41–E52
McCrindle BW, Urbina EM, Dennison BA, Jacobson MS, Steinberger J, Rocchini AP, Hayman LL, Daniels SR, American Heart Association Atherosclerosis Hypertension Obesity in Youth Committee American Heart Association Council of Cardiovascular Disease in the Young American Heart Association Council on Cardiovascular Nursing 2007 Drug therapy of high-risk lipid abnormalities in children and adolescents: a scientific statement from the American Heart Association Atherosclerosis, Hypertension, and Obesity in Youth Committee, Council of Cardiovascular Disease in the Young, with the Council on Cardiovascular Nursing. Circulation 115: 1948–1967
Starr B, Hadfield SG, Hutten BA, Lansberg PJ, Leren TP, Damgaard D, Neil HA, Humphries SE 2008 Development of sensitive and specific age- and gender-specific low-density lipoprotein cholesterol cutoffs for diagnosis of first-degree relatives with familial hypercholesterolemia in cascade testing. Clin Chem Lab Med 46: 791–803
Widhalm K, Dirisamer A, Lindemayr A, Kostner G 2007 Diagnosis of families with familial hypercholesterolemia and/or Apo B-100 defect by means of DNA analysis of LDL-receptor gene mutations. J Inherit Metab Dis 30: 239–247
Umans-Eckenhausen MA, Defesche JC, Sijbrands EJ, Scheerder RL, Kastelein JJ 2001 Review of first 5 years of screening for familial hypercholesterolemia in the Netherlands. Lancet 357: 165–168
Hedman M, Miettinen TA, Gylling H, Ketomäki A, Antikainen M 2006 Serum noncholesterol sterols in children with heterozygous familial hypercholesterolemia undergoing pravastatin therapy. J Pediatr 148: 241–246
Sudhop T, Lütjohann D, Kodal A, Igel M, Tribble DL, Shah S, Perevozskaya I, von Bergmann K 2002 Inhibition of intestinal cholesterol absorption by ezetimibe in humans. Circulation 106: 1943–1948
Ketomäki A, Gylling H, Siimes MA, Vuorio A, Miettinen TA 2003 Squalene and noncholesterol sterols in serum and lipoproteins of children with and without familial hypercholesterolemia. Pediatr Res 53: 648–653
Ketomaki A, Gylling H, Miettinen TA 2004 Effects of plant stanol and sterol esters on serum phytosterols in a family with familial hypercholesterolemia including a homozygous subject. J Lab Clin Med 143: 255–262
Zhao HL, Houweling AH, Vanstone CA, Jew S, Trautwein EA, Duchateau GS, Jones PJ 2008 Genetic variation in ABC G5/G8 and NPC1L1 impact cholesterol response to plant sterols in hypercholesterolemic men. Lipids 43: 1155–1164
García-Otín AL, Cofán M, Junyent M, Recalde D, Cenarro A, Pocoví M, Ros E, Civeira F 2007 Increased intestinal cholesterol absorption in autosomal dominant hypercholesterolemia and no mutations in the low-density lipoprotein receptor or apolipoprotein B genes. J Clin Endocrinol Metab 92: 3667–3673
Lapinleimu J, Nuotio IO, Lapinleimu H, Simell OG, Rask-Nissila L, Viikari JS 2002 Recognition of familial dyslipidemias in 5-year-old children using the lipid phenotypes of parents. The STRIP project. Atherosclerosis 160: 417–423
Cortner JA, Coates PM, Gallagher PR 1990 Prevalence and expression of familial combined hyperlipidemia in childhood. J Pediatr 116: 514–519
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Noto, D., Cefalù, A., Barraco, G. et al. Plasma Non–cholesterol Sterols: A Useful Diagnostic Tool in Pediatric Hypercholesterolemia. Pediatr Res 67, 200–204 (2010). https://doi.org/10.1203/PDR.0b013e3181c8f035
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e3181c8f035
This article is cited by
-
Cholesterol metabolism in mice models of genetic hypercholesterolemia
Journal of Physiology and Biochemistry (2020)