Abstract
Premature infants are at risk for lower airway obstruction; however, maturation of reflex pathways regulating lower airway patency is inadequately studied. We hypothesized that postnatal maturation causes developmental change in brainstem efferent airway-related vagal preganglionic neurons (AVPNs) within the rostral nucleus ambiguus (rNA) that project to the airways and in pulmonary afferent fibers that terminate in the nucleus tractus solitarius (NTS). Ferrets aged 7, 14, 21, and 42 d received intrapulmonary injection of cholera toxin (CT)-β subunit, a transganglionic retrograde tracer. Five days later, their brainstem was processed for dual immunolabeling of CT-β and the cholinergic marker, choline acetyl transferase. CT-β–labeled AVPNs and CT-β–labeled afferent fiber optical density (OD) were analyzed. There was a significantly higher CT-β–labeled cell number within the rNA at the youngest compared with older ages. All efferent CT-β–labeled cells expressed choline acetyl transferase. OD of CT-β–labeled afferent fibers was also higher at 7 d compared with 14 d. We conclude that the number of efferent AVPNs and afferent fiber OD both diminish over the second postnatal week. We speculate that exposure to injurious agents in early postnatal life may inhibit natural remodeling and thereby enhance later vulnerability to airway hyperreactivity.
Similar content being viewed by others
Main
Anatomical studies in human premature infants and various animal models have demonstrated a well-developed and well-innervated airway smooth muscle layer in late fetal and early postnatal life (1–5). In combination with the small caliber intrapulmonary airways that are present during early development, this may predispose premature infants to airway obstruction and impaired ventilation. Furthermore, the risk of airway hyperreactivity and need for asthma medication in former premature infants when compared with their term counterparts is increased over 2- to 3-fold, respectively (6–9). Nonetheless, maturational change in reflex pathways regulating control of lower airway patency during early development has not been adequately studied.
Cholinergic outflow to the airways depends on sensory input received from the lungs, which modulates airway-related vagal preganglionic neurons (AVPNs) in the brainstem (10–15). Efferent neural output from AVPNs located in the rostral nucleus ambiguus (rNA) is modulated by afferent input to the nucleus tractus solitarius (NTS) from lung afferents such as slowly adapting stretch receptors, C-fibers, and rapidly adapting receptors (10,12,16–18). However, there is limited information on physiologic and developmental changes in maturation of airway reflex responses from lung afferents to airway smooth muscle. Previous studies have focused on C-fiber influences on ventilatory muscle responses rather than airway regulation (19–21). Haxhiu-Poskurica et al. (22) characterized 2- to 10-wk-old piglets' responses to C-fiber stimulation and the resultant changes in tracheal smooth muscle tone; they documented immaturity of reflex responses of airway smooth muscle tone during early postnatal life when compared with reflex pathways regulating ventilatory responses. These results supported earlier studies demonstrating a diminished hypoxia-induced increase in airway smooth muscle tone in newborn dogs (23), but it is unclear from these physiologic studies whether airway reflex pathways are anatomically intact at an early postnatal age.
Ferrets have proven to be a useful animal model of human viral disease affecting the respiratory system (24,25). Furthermore, similarities between human and ferret development of cholinergic neurons and airway smooth muscle innervation have suggested that this species is a favorable model for studying human respiratory neuronal reflex pathways (13,17,26). In a previous study done in our laboratory (27), the chemical profile of vagal preganglionic motor cells projecting to the airways was characterized in adult ferrets. AVPNs found within the rNA were shown to be cholinergic in nature and their stimulation resulted in a release of acetylcholine leading to contraction of airway smooth muscle. However, it is not known whether these cholinergic traits are expressed at an early postnatal age. Therefore, we sought to test the hypothesis that early postnatal maturation is associated with developmental change in both the density of afferent fibers reaching the NTS and the number of efferent AVPNs within the rNA, which project to the airways.
METHODS
Animal preparation.
Studies were performed in healthy European ferret pups, Mustella putorius furo (Marshall Farm, NY) weighing between 38 and 190 g. All experiments were conducted in accordance with protocols approved by the Institutional Animal Care and Use Committee of Case Western Reserve University. Ferret pups were housed with the mother on a regular day/night cycle (lights on from 06:00 to 18:00 h) at 24°C and 55% relative humidity.
To determine developmental changes of the central sensory and motor innervation of the airways, four groups of ferret pups were injected with 50-μL cholera toxin (CT)-β subunit (List Biological Laboratories, Inc., Campbell, CA), a transganglionic retrograde tracer, dissolved in distilled water (1 mg/mL). Injections were performed on postnatal days 7 (n = 8), 14 (n = 4), 21 (n = 4), and 42 (n = 3) into the upper lobe of the right lung (12,27,28). After the procedure, ferret pups were returned to their mothers and were monitored for any complications. Five days after the CT-β injections, animals were deeply anesthetized with ketamine and xylazine (50 mg/kg and 10 mg/kg, respectively; intraperitoneal), perfused with saline followed by 4% paraformaldehyde made in 0.1 M phosphate buffer (pH 7.4). Brains were removed, postfixed in the same fixative for 2 d, and then transferred to 30% sucrose in 0.1 M phosphate buffer for cryoprotection. Transverse sections of the brainstem were sliced at 40 μm using a Cryostat (Leica CM1850, Leica Microsystems, Heidelberger, Strasse) and stored in 0.2% sodium azide in 0.1 M phosphate buffer. In a second set of experiments following an identical protocol, eight 7-d-old animals were injected with 25 μL of CT-β into the upper lobe of the right lung, to evaluate the effect of a lower CT-β volume on labeled brain cells at the younger age.
Immunohistochemistry.
The immunohistochemical procedures for dual staining of tissue sections for visualization of CT-β–labeled AVPNs have been reported in our previous study (27). Briefly, free floating 1-in-5 series tissue sections were washed in phosphate buffer saline (PBS, pH 7.4) three times for 10 min each followed by incubation in PBS containing 0.3% hydrogen peroxide for 30 min to block endogenous peroxidase activity. Sections were washed in PBS and then incubated two times for 10 min each in 0.3% Triton-X in PBS. Tissues were then placed into a blocking medium containing 1% albumin bovine serum (Sigma Chemical Co., St. Louis, MO) for 30min. Sections were incubated for 24 h at 4°C in goat polyclonal anticholine acetyltransferase (ChAT, Chemicon International, Temecula, CA; 1:500) (27). Sections were washed in 0.3% Triton-X in PBS and incubated for 2 h in a 1:200 solution of donkey anti-goat IgG conjugated with Alexa Fluor 594 (Texas Red, Molecular Probes, Eugene, OR). The sections were then washed in 0.3% Triton-X in PBS three times; each for 10 min. Sequential immunofluorescent detection of CT-β was performed after the ChAT labeling protocol was completed. The sections were incubated in a 1:20,000 dilution of rabbit polyclonal anti-CT-β (Accurate Chemical and Scientific Corporation, Westbury, NY) for 36 h. Sections were washed in 0.3% Triton-X in PBS and incubated for 2 h in a 1:200 solution of donkey anti-rabbit IgG conjugated with fluorescein (Jackson Immunoresearch Laboratories, Inc., West Grove, PA). In control experiments for ChAT and CT-β labeling, primary antibodies were omitted. Sections were then rinsed in PBS three times for 10 min each, mounted on Superfrost/Plus microscope slides and cover-slipped using Vecta Shield (Vector Laboratories Inc., Burlingame, CA).
Data analysis.
One in five sections were carefully selected from 0.0, 1.0, 1.5, 2.0, and 3.5 mm rostral to the obex as defined previously by our group (12). The obex was considered as a zero point. For consistency, the sections from the all the groups were selected and analyzed by the same individual. Slides were viewed with a fluorescent microscope (Leica DMLB, Leica Microsystems, Heidelberger, Strasse). Colocalization of ChAT and CT-β protein was identified by alternating between fluorescent filters. Images were acquired from the same area of the section for both traits, digitized, and stored as TIFF files for data analysis. Data are expressed as mean ± SEM at each age. Statistical comparisons for CT-β–labeled AVPNs between age groups were made by using one-way ANOVA (Student-Neuman-Keuls; significance at p ≤ 0.05).
To determine the CT-β–labeled afferent nerve terminals in the NTS at different levels from the obex, we used the same animals and brainstem slices from 7- and 14-d-old animals that were used in the previous experiment, where animals were injected with 50 μL of CT-β into the right lung. Confocal images (Leica DMIRE2, Leica Microsystems, Heidelberger, Strasse) were taken at 4-μm intervals to avoid double counting and optical stacks of images (Z-sectioning) were acquired from the same section, digitized, and stored as TIFF files. To standardize and unbias the data analysis, gain, and offset were kept at the same level for all age groups. The density of CT-β–labeled axon terminals ending in the NTS region was also counted and the total optical density (OD) per unit volume per level was collated using NIH ImageJ software. Images were analyzed keeping the same threshold parameter for all age groups and the investigator who analyzed the images was blinded to the animals' age.
RESULTS
We initially quantified cells labeled for CT-β only at each age group to characterize neuroanatomic connections between the lungs and cell bodies within the brainstem. In sections selected from 0.0, 1.0, 1.5, 2.0, and 3.5 mm rostral to the obex, retrogradely labeled CT-β cell bodies were located in the dorsal motor nucleus of the vagus and in the rNA. In this study, we focused on the rNA because this is the major site controlling neural output to airways. CT-β–labeled cells within the rNA were found both in the compact and loose portion of the rNA, which lies just below the compact portion. The mean number of CT-β–labeled cells combined for all levels was significantly higher (p < 0.05) at 7-d-old (125 ± 10, n = 8) compared with 14-d-old (60 ± 9, n = 4), 21-d-old (63 ± 5, n = 4), and 42-d-old (38 ± 16, n = 3) pups (Fig. 1). Although sample sizes were small in the older age groups, the assumption of normality of data within groups was met, and hence we used one-way ANOVA for the analysis. There was no statistical significance in the CT-β–labeled cell counts between the older age groups.
As a significant decline in CT-β–labeled cell bodies occurred between 7 and 14 postnatal days, and the weight of ferret pups approximately doubled from 7 to 14 d, one half (25 μL) of the original CT-β dose (50 μL) was injected into the right lung in eight additional 7-d-old ferret pups. This was done to confirm that the increased cell count at the rNA region in the 7-d-old group was not due to a higher CT-β dose per body weight. There were no statistical differences (p = 0.16) between the 7-d-old ferret group injected with 50 μL (125 ± 10, n = 8) and the 7-d-old ferret group injected with 25 μL (101 ± 6, n = 8). Furthermore, the number of CT-β–labeled cells in the 7-d-old ferret groups injected with 25 μL was significantly higher (p < 0.05) than the number of cells in the older groups injected with 50 μL.
To determine the neuraxis level that expressed most cells that projected to the airways, CT-β–labeled cells were counted at different levels (0.0, 1.0, 1.5, 2.0, and 3.5 mm) from the obex in all the animals. The 7-d-old group showed a consistent trend toward more cells at each neuraxis level (Fig. 2). Overall, for all groups, the rNA region at 3.5 mm rostral to the obex showed the densest projection to the airways (Fig. 2).
We subsequently quantified the number of CT-β–labeled cells that were double labeled with ChAT, a cholinergic marker and enzyme that synthesizes acetylcholine. All the CT-β–labeled rNA cells expressed ChAT, confirming that CT-β–labeled AVPNs are cholinergic in nature (Fig. 3).
Finally, we sought to determine whether age-dependent changes in efferent innervation of the airways from the brainstem are also seen in the afferent innervation of the respiratory reflex pathway to the NTS. We used confocal microscope sections of the tissues at 4-μm intervals to determine the total relative number of “puncta” or OD per cubic micrometer within the NTS subnuclei. We analyzed the density of anterogradely-labeled CT-β afferent fiber projection to the NTS at 7 and 14 d. We chose these two critical time frames based on our initial labeling study with the efferent projection to the airways where the data showed significantly higher CT-β–labeled cells in the AVPNs between the 7- and 14-d-old ferret groups. Our data showed afferent labeling in the ventrolateral and commissural subnuclei of the NTS. The density of CT-β–labeled afferent fibers was much higher at the younger age. The 7-d-old animals (n = 4) had an average OD of 1.23 OD/μm3 (SEM = 0.29) compared with 0.13 OD/μm3 (SEM = 0.02) in 14-d-old animals (n = 4). The highest density was observed at 0.0 and 1.5 mm rostral to the obex (p < 0.05) (Fig. 4).
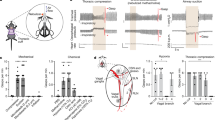
Photomicrograph comparing the OD of CT-β–labeled afferent fibers at the NTS between a 7-d-old ferret (top panel A–C) and a 14-d-old ferret (bottom panel D–F) after microinjection of CT-β into the right lung. Evaluated sections taken at 0.0 (A and D), 1.0 (B and E), and 1.5 (C and F) rostral to the obex. Scale bar: 75 μm.
DISCUSSION
This study was designed to determine whether there is a maturational difference in the number of efferent AVPNs projecting from the rNA to the lungs and whether this change is also observed in the density of afferent fibers projecting from the lungs to the NTS in a ferret model. Using CT-β as a retrograde tracer, we were able to identify the vagal preganglionic neurons projecting to the airways. We chose 7-, 14-, and 21- and 42-d-old ferret pups to study age-dependent changes in airway projection. We found that when animals were injected intrapulmonary with 50 μL CT-β, the number of CT-β–labeled cells is significantly higher in the 7-d-old group when compared with the older groups. Between 7 and 14 d, the number of labeled cells in the 14-d-old group is significantly diminished. When a second group of animals was injected at 7 d with half of the original dose of CT-β to match the CT-β dose/body weight, there was no significant difference in the CT-β–labeled cell count between the 7-d-old groups injected with either 50 or 25 μL of CT-β, indicating that the higher number of CT-β–labeled cells is not related to a higher dose/body weight. Regardless of the CT-β dose injected at 7 d, the number of CT-β–labeled cells was significantly higher than at later ages. These findings strongly suggest that the number of efferent AVPNs is higher at a younger age and diminishes with maturation.
In the adult ferret, AVPNs projecting to the airways were found from 0.0 to 3.5 mm rostral to the obex with the predominance of the labeling at 3.5 mm (11). In this study, we also quantified the number of cells seen at different brainstem levels to determine whether the maturational changes we observed were specific to a given area within the brainstem or more ubiquitous. Regardless of age group, the ferret pups showed the densest projection to the airways at 3.5 mm rostral to the obex. Furthermore, we determined that AVPNs that project to the airways were cholinergic in nature by double immunolabeling with ChAT. This suggests that after their activation AVPNs release acetylcholine in the intrinsic ganglia and thereby regulate airway smooth muscle tone (17).
We also characterized the OD of afferent fibers projecting to the NTS. NTS subnuclei are involved in tracheobronchial and respiratory reflexes as they receive information from airway receptors such as pulmonary C-fibers, rapidly adapting, and slowly adapting receptors. Our study showed afferent labeling in the ventrolateral and commissural subnuclei of the NTS, the primary sensory afferent relay center in the brainstem. The density of CT-β–labeled fibers in the 7-d-old ferret pups was higher than in the 14-d-old ferret group. This suggests that similar maturational changes occur in both afferent innervation to the NTS and efferent AVPN projection to the airways.
Our observation of a decline in efferent cell bodies and afferent fibers is consistent with prior observations of neuronal death accompanying normal development in the CNS (29). These studies described programmed cell death in areas such as the developing trigeminal system, olivocerebral system, cochlear nucleus, and other areas (29–32). To our knowledge, there are no studies related to the evolution of programmed cell death for AVPNs in the rNA, which is part of the central airway reflex pathway. Our findings of a decrease in the number of AVPNs (in addition to the decrease in fiber density) support a role for developmental remodeling of neural circuits involved in autonomic control of airway caliber. Although experiments determining programmed cell death would have substantiated our hypothesis, it was beyond the scope of this project. Further studies using techniques such as TUNEL testing and caspace-3 staining in this or comparable immature animal models are needed to support a role for apoptosis in the developmental remodeling we proposed.
Murphy et al. (33) examined the role maturation serves in airway contractile responses in swine. They found an increase in force generation as well as sensitivity to vagal stimulation in the younger animals, and they suggested that a decrease in contractile response in older animals could be related to parasympathetic neural function and maturation in the activity of acetylcholinesterase. These studies are, however, related to alteration in receptor/transductional changes associated with acetylcholine muscarinic receptor responses. In our study, we have shown that there is also a neuroanatomical change during maturation. The present results showing a higher density of fibers coupled with greater number of cells during early life contrasts with the relatively weak airway smooth muscle contractile response as previously demonstrated at that age (22). We speculate that up-regulation of inhibitory GABAergic interneurons and/or other inhibitory inputs to the common efferent pathway contribute to immature reflex responses in young animals in the face of an intact neuroanatomic reflex pathway. Furthermore, peripheral relaxant responses such as those mediated by prostaglandins may also contribute to relaxation in young animals (34) in response to a strong cholinergic efferent output from the brainstem.
Interspecies differences also complicate the comparison of physiologic and neuroanatomic findings. Ferret airway smooth muscle neurobiology and neural circuitry including the cholinergic system is similar to humans and thereby serves as a good model to study airway control (35). Furthermore, ferrets have been successfully used to study human viral disease affecting the respiratory system (25). We have recently shown that allergen exposure and repeated challenges, presumably causing lung inflammation in the adult ferret, diminish central inhibitory noradrenergic modulation of AVPNs partly via down-regulation of α2A-adrenergic receptors expressed by the AVPNs (36).
There are a few limitations to the methods that we have used in our study. CT-β was used as a retrograde transganglionic tracer and experienced personnel injected CT-β into the lungs; however, we cannot rule out differences in the exact location of CT-β injection within the lung and the effect that this may have on distribution of the labeled cells within the brainstem. It is possible that in the present study, not all vagal preganglionic neurons that innervate the airway system could be labeled and therefore the number of cells reported reflects the labeled AVPNs rather than the actual number of AVPNs that innervate the airways. These results are consistent with previous experiments conducted in adult ferrets in our laboratory (14,19). One must also be cautious when interpreting the distribution of afferent terminations in the NTS. Our confocal microscopy results did not differentiate between synaptic contacts and fibers of passage within the NTS. We used a design that allows morphometric quantification of these structures within the NTS subnuclei while avoiding double counting. Finally, the ferret pup is a useful but fragile animal model for studying airway innervation and our statistical analyses in the older age groups are somewhat limited by small number of animals.
Our data in the immature ferret indicate that neural innervation undergoes maturational change in the second week of life, which constitutes a normal maturational phenomenon. Increased density of both afferent and efferent pathways controlling the airways in early life may enhance the vulnerability of infants to activation of respiratory reflexes. We speculate that exposure to injurious chemical or mechanical stimulation such as exposure to high inhaled oxygen, mechanical injury during intubation, or nicotine inhalation in early life may inhibit the natural remodeling we have observed and even change the phenotype resulting in predisposition to airway hyperreactivity later in life.
Abbreviations
- AVPNs:
-
airway-related vagal preganglionic neurons
- ChAT:
-
choline acetyltransferase
- CT-β:
-
cholera toxin-β subunit
- NTS:
-
nucleus tractus solitarius
- rNA:
-
rostral nucleus ambiguus
References
Cullen AB, Cooke PH, Driska SP, Wolfson MR, Shaffer TH 2006 The impact of mechanical ventilation on immature airway smooth muscle: functional, structural, histological, and molecular correlates. Biol Neonate 90: 17–27
Hershenson MB, Kelleher MD, Naureckas ET, Abe MK, Rubinstein VJ, Zimmermann A, Bendele AM, McNulty JA, Panettieri RA, Solway J 1994 Hyperoxia increases airway cell S-phase traversal in immature rats in vivo. Am J Respir Cell Mol Biol 11: 296–303
Ramchandani R, Shen X, Gunst SJ, Tepper RS 2003 Comparison of elastic properties and contractile responses of isolated airway segments from mature and immature rabbits. J Appl Physiol 95: 265–271
Sparrow MP, Lamb JP 2003 Ontogeny of airway smooth muscle: structure, innervation, myogenesis and function in the fetal lung. Respir Physiol Neurobiol 137: 361–372
Sward-Comunelli SL, Mabry SM, Truog WE, Thibeault DW 1997 Airway muscle in preterm infants: changes during development. J Pediatr 130: 570–576
Doyle LW 2006 Respiratory function at age 8–9 years in extremely low birthweight/very preterm children born in Victoria in 1991–1992. Pediatr Pulmonol 41: 570–576
Gessner BD, Chimonas MA 2007 Asthma is associated with preterm birth but not with small for gestational age status among a population-based cohort of Medicaid-enrolled children <10 years of age. Thorax 62: 231–236
Hack M, Taylor HG, Drotar D, Schluchter M, Cartar L, Andreias L, Wilson-Costello D, Klein N 2005 Chronic conditions, functional limitations, and special health care needs of school-aged children born with extremely low-birth-weight in the 1990s. JAMA 294: 318–325
Jaakkola JJ, Ahmed P, Ieromnimon A, Goepfert P, Laiou E, Quansah R, Jaakkola MS 2006 Preterm delivery and asthma: a systematic review and meta-analysis. J Allergy Clin Immunol 118: 823–830
Dehkordi O, Kc P, Balan KV, Haxhiu MA 2006 Airway-related vagal preganglionic neurons express multiple nicotinic acetylcholine receptor subunits. Auton Neurosci 128: 53–63
Haxhiu MA, Jansen AS, Cherniack NS, Loewy AD 1993 CNS innervation of airway-related parasympathetic preganglionic neurons: a transneuronal labeling study using pseudorabies virus. Brain Res 618: 115–134
Haxhiu MA, Loewy AD 1996 Central connections of the motor and sensory vagal systems innervating the trachea. J Auton Nerv Syst 57: 49–56
Haxhiu MA, Kc P, Moore CT, Acquah SS, Wilson CG, Zaidi SI, Massari VJ, Ferguson DG 2005 Brain stem excitatory and inhibitory signaling pathways regulating bronchoconstrictive responses. J Appl Physiol 98: 1961–1982
Kubin L, Alheid GF, Zuperku EJ, McCrimmon DR 2006 Central pathways of pulmonary and lower airway vagal afferents. J Appl Physiol 101: 618–627
Moore CT, Wilson CG, Mayer CA, Acquah SS, Massari VJ, Haxhiu MA 2004 A GABAergic inhibitory microcircuit controlling cholinergic outflow to the airways. J Appl Physiol 96: 260–270
Andresen MC, Yang MY 1990 Non-NMDA receptors mediate sensory afferent synaptic transmission in medial nucleus tractus solitarius. Am J Physiol 259: H1307–H1311
Haxhiu MA, Yamamoto B, Dreshaj IA, Bedol D, Ferguson DG 2000 Involvement of glutamate in transmission of afferent constrictive inputs from the airways to the nucleus tractus solitarius in ferrets. J Auton Nerv Syst 80: 22–30
Sykes RM, Spyer KM, Izzo PN 1997 Demonstration of glutamate immunoreactivity in vagal sensory afferents in the nucleus tractus solitarius of the rat. Brain Res 762: 1–11
Arsenault J, Moreau-Bussiere F, Reix P, Niyonsenga T, Praud JP 2003 Postnatal maturation of vagal respiratory reflexes in preterm and full-term lambs. J Appl Physiol 94: 1978–1986
Taylor-Clark T, Undem BJ 2006 Transduction mechanisms in airway sensory nerves. J Appl Physiol 101: 950–959
Wilson CG, Zhang Z, Bonham AC 1996 Non-NMDA receptors transmit cardiopulmonary C fibre input in nucleus tractus solitarii in rats. J Physiol 496: 773–785
Haxhiu-Poskurica B, Carlo WA, Miller MJ, DiFiore JM, Haxhiu MA, Martin RJ 1991 Maturation of respiratory reflex responses in the piglet. J Appl Physiol 70: 608–616
Waldron MA, Fisher JT 1988 Differential effects of CO2 and hypoxia on bronchomotor tone in the newborn dog. Respir Physiol 72: 271–282
Kobinger GP, Figueredo JM, Rowe T, Zhi Y, Gao G, Sanmiguel JC, Bell P, Wivel NA, Zitzow LA, Flieder DB, Hogan RJ, Wilson JM 2007 Adenovirus-based vaccine prevents pneumonia in ferrets challenged with the SARS coronavirus and stimulates robust immune responses in macaques. Vaccine 25: 5220–5231
Piazza FM, Carson JL, Hu SC, Leigh MW 1991 Attachment of influenza A virus to ferret tracheal epithelium at different maturational stages. Am J Respir Cell Mol Biol 4: 82–87
Carson JL, Reed W, Moats-Staats BM, Brighton LE, Gambling TM, Hu SC, Collier AM 1998 Connexin 26 expression in human and ferret airways and lung during development. Am J Respir Cell Mol Biol 18: 111–119
Kc P, Mayer CA, Haxhiu MA 2004 Chemical profile of vagal preganglionic motor cells innervating the airways in ferrets: the absence of noncholinergic neurons. J Appl Physiol 97: 1508–1517
Hadziefendic S, Haxhiu MA 1999 CNS innervation of vagal preganglionic neurons controlling peripheral airways: a transneuronal labeling study using pseudorabies virus. J Auton Nerv Syst 76: 135–145
Harris JA, Rubel EW 2006 Afferent regulation of neuron number in the cochlear nucleus: cellular and molecular analyses of a critical period. Hear Res 216–217: 127–137
Davies AM 1997 Studies of neurotrophin biology in the developing trigeminal system. J Anat 191: 483–491
Madalosso SH, Perez-Villegas EM, Armengol JA 2005 Naturally occurring neuronal death during the postnatal development of Purkinje cells and their precerebellar afferent projections. Brain Res Brain Res Rev 49: 267–279
White FA, Keller-Peck CR, Knudson CM, Korsmeyer SJ, Snider WD 1998 Widespread elimination of naturally occurring neuronal death in Bax-deficient mice. J Neurosci 18: 1428–1439
Murphy TM, Mitchell RW, Blake JS, Mack MM, Kelly EA, Munoz NM, Leff AR 1989 Expression of airway contractile properties and acetylcholinesterase activity in swine. J Appl Physiol 67: 174–180
Larsen GL, Loader J, Fratelli C, Kang JK, Dakhama A, Colasurdo GN 2007 Modulation of airway responses by prostaglandins in young and fully grown rabbits. Am J Physiol Lung Cell Mol Physiol 293: L239–L244
Zhu W, Dey RD 2001 Projections and pathways of VIP- and nNOS-containing airway neurons in ferret trachea. Am J Respir Cell Mol Biol 24: 38–43
Wilson CG, Akhter S, Mayer CA, Kc P, Balan KV, Ernsberger P, Haxhiu MA 2007 Allergic lung inflammation affects central noradrenergic control of cholinergic outflow to the airways in ferrets. J Appl Physiol 103: 2095–2104
Acknowledgements
We thank Ms. ShiJian Liu for her technical assistance in animal perfusion and tissue sectioning. We also thank our biostatistician, Dr. Mark Schluchter, for his guidance in choosing the appropriate statistical method to analyze our data.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by a grant from the National Institute of Health, HL 50527 (R.J.M.), INO Therapeutics Advancing Newborn Medicine Grant Program, TRN104882 (A.Z.K.) and K99 HL087620 (P.K.).
Rights and permissions
About this article
Cite this article
Kohn, A., Hoxha, Z., Balan, K. et al. Developmental Changes in Brainstem Neurons Regulating Lower Airway Caliber. Pediatr Res 65, 509–513 (2009). https://doi.org/10.1203/PDR.0b013e31819da270
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e31819da270

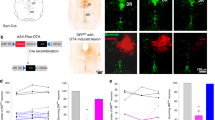


 ), and 42 (
), and 42 ( postnatal days. *p < 0.05.
postnatal days. *p < 0.05.

