Abstract
Adiponectin has potent insulin-sensitizing effects, improves lipid metabolism, and potentially protects against the development of metabolic syndrome. Thus, increasing adiponectin levels in preterm infants at risk for developing metabolic syndrome may be of special interest. The aim of this study was to examine the effects of dietary long-chain polyunsaturated fatty acids (LCPUFA) on serum adiponectin and lipid concentrations in preterm infants. Adiponectin and lipid levels of 60 healthy preterm infants [gestational age 32.7 (1.9) wk] randomly assigned to be fed either 1) a formula containing LCPUFA [arachidonic and docosahexanoic] (+LCPUFA group) or 2) the same formula without LCPUFA (−LCPUFA/control group), were determined at mean (SD) 33.8 (11.7) d. Adiponectin and HDL-C concentrations were significantly higher in the +LCPUFA group than in controls (p = 0.002 and p = 0.01, respectively); whereas, triglyceride levels were lower (p = 0.06). Adiponectin correlated positively with HDL-C levels and negatively with triglyceride levels in the +LCPUFA group but not in the controls. In conclusion, circulating adiponectin concentrations were higher in preterm infants fed a formula containing LCPUFA than infants fed an LCPUFA-free formula and they correlated with lipidemic profile.
Similar content being viewed by others
Main
Low birth weight due to poor fetal growth has been identified as a factor contributing to the development of metabolic syndrome (insulin resistance, dislipidemia, hypertension) (1,2). Moreover, preterm infants are also at risk for insulin resistance, and possibly for other components of metabolic syndrome, irrespective of whether they were born appropriate or small for gestational age (3,4). Although the underlying mechanism(s) connecting preterm birth and the development of metabolic syndrome risk are not known, circulating concentrations of adiponectin have been shown to be lower in preterm than in full term infants (5). Adiponectin is an adipocyte-derived protein, which has potent insulin-sensitizing effects, improves lipid metabolism, and potentially protects against the development of insulin resistance and metabolic syndrome (6). High plasma levels of adiponectin are associated with lower incidence of type-2 diabetes and coronary heart disease (7,8). Therefore, a means of increasing circulating concentrations of adiponectin in preterm infants may be of special interest.
N-3 and n-6 long-chain polyunsaturated fatty acids (LCPUFA), mainly docosahexanoic (DHA) and arachidonic (AA) acid, have been added in some, but not all, commercially available infant formulas, in an attempt to mimic the composition of human milk. In animals and human adults, diets enriched with n-3 LCPUFA have been linked to beneficial effects against insulin resistance (9) and to a favorable impact on lipidemic profile (10,11). The influence of dietary n-3 LCPUFA on circulating concentrations of adiponectin has been studied in animals (12–15), in obese adults, and in patients, who have suffered a myocardial infarction (16–18). Dietary n-3 LCPUFA appear to have had a positive effect in the majority of these studies.
In a longitudinal observational study in 62 preterm infants, we found a positive correlation between feeding with n-3 and n-6 LCPUFA-supplemented formula and serum adiponectin levels (5). However, the study included only 9 LCPUFA-supplemented infants, and the results needed to be confirmed in a randomized controlled trial. Moreover, it remains to determine whether the intake of LCPUFA had any effect on serum lipid levels in preterm infants. The aim of the present randomized controlled study was to examine the effects of dietary LCPUFA on serum adiponectin and lipid levels in preterm infants and the associations of adiponectin with the infants' lipidemic profile.
METHODS
Subjects and study protocol.
Eligible participants were preterm infants admitted to our unit after birth, who met the following criteria: gestational age ≥28 wk, birth weight >1000 g, no family history of hyper- or hypo-lipidemias, no congenital malformation, and mothers, who elected formula feeding. The Hospital Ethics Committee approved the study, and informed parental consent was obtained.
Gestational age was estimated from the last menstrual period and was supported by fetal ultrasound measurements and clinical examination of the neonate according to the new Ballard score (19). After matching for gestational age (±1 wk), birth weight (±100 g), and gender by a computer-generated randomization table within clusters of six, 84 infants were initially enrolled for the study. After birth, each was randomly assigned to be fed either 1) a commercial formula containing LCPUFA (AA; 12.0 mg and DHA; 7.1 mg per 100 mL of formula) (+LCPUFA group, n = 42) or 2) a formula without LCPUFA (−LCPUFA/control group, n = 42). The chief-nurse, not involved in care of the trial infants, undertook the allocation and ordering of each test formula for the enrolled infants using sealed opaque randomization envelopes. She kept the randomization list private and disclosed it after the study.
The two formulas were produced by the same manufacturer (S-26, Wyeth Nutritionals, Ireland) and were provided by the hospital food service for feeding of hospitalized infants. The formula-containing bottles were similar in appearance; only the name of the participant to whom the formula was administered was written on them. The nutrient composition of the formulas was identical apart from LCPUFA. The formulas provided 67 Kcal/100 mL when diluted to 15% (wt/vol) and contained 1.5 g/dL protein, 3.6 g/dL fat, 7.2 g/dL carbohydrates and 0.23 g/dL minerals and vitamins. The fatty acid composition of the formulas, according to manufacturer specifications, is shown in Table 1. The amount of formula consumed at each meal was recorded and the infants' growth was evaluated periodically during hospitalization. Body weight was obtained daily using a standard electronic scale. Measurements of birth weight and body weight at discharge were converted to z scores (SD scores from the mean after adjustment for gestational age and gender) (20). Recumbent length and head circumference were measured weekly by the same investigator. Body mass index was calculated (Kg/m2) at discharge.
Infants were dropped from the study if they presented major neonatal morbidity (respiratory distress requiring assisted ventilation for more than 3 d, hypotension with need for inotropes, intraventricular hemorrhage greater than grade I according to the criteria of Volpe, sepsis, necrotizing enterocolitis, bronchopulmonary dysplasia) or did not tolerate full enteral feeding (≥150 mL/Kg/d) by the 10th day of life. Twelve infants in each group were dropped from the study. All the remaining (30 infants in each group) underwent a venipuncture before feeding on the morning of the day of discharge, for routine blood tests, as well as for determining serum adiponectin and lipid [triglycerides, total cholesterol (C), HDL-C, and LDL-C] levels. Neither the care taker who did the feeding nor the person who performed the anthropometric and blood measurements, nor the scientist who did the statistical evaluation of the results, had any knowledge of the infants' diet.
The sample size was calculated using our previous report of adiponectin concentrations in preterm infants (5). Assuming an alpha risk of 0.05, a power of 0.80 and a bilateral test, it was estimated that approximately 20 infants were needed in each group to detect a significant difference of 1 SD in mean adiponectin levels between +LCPUFA and −LCPUFA/control groups.
Adiponectin and lipid assays.
Serum adiponectin levels were assayed using a human adiponectin ELISA kit (Linco Research, MO). According to the manufacturer, the intra- and interassay coefficients of variation were less than 7.4% and 8.4%, respectively; the sensitivity limit of the assay was 0.78 ng/mL and the appropriate range of measurements (standard concentrations) were 1.56 ng/mL to 100 ng/mL. For values greater than 100 ng/mL, the samples were further diluted using assay diluent, and the assay was repeated so that the results fell within the range.
Serum triglycerides, total C, and HDL-C were measured using the Bayer ADVIA 1650 Clinical Chemistry System (Bayer Corporation, Tarrytown, NY), whereas LDL-C values were estimated using the Friedewald formula as follows: LDL-C = total C- (triglycerides/5 + HDL-C).
Statistical analyses.
Data are presented as mean (SD). Groups were compared for quantitative variables by the Student t test. Values of adiponectin and lipid levels were normally distributed, both overall and for +LCPUFA and −LCPUFA/control groups separately, so no transformation was necessary. Correlation analyses and multiple regression analyses were used to examine relations among the variables of interest. Levels of statistical significance were set at p ≤ 0.05. All statistical analyses were performed using the SPSS statistical package (SPSS, version 10.0, Chicago, IL).
RESULTS
The characteristics of the study population are shown in Table 2. Clinical and anthropometric characteristics did not differ significantly between the two groups of infants studied.
Mean (SD) serum adiponectin levels were significantly higher in the +LCPUFA group than in the −LCPUFA/control group (p = 0.002) (Table 3). Serum HDL-C levels were also significantly higher in the +LCPUFA group than in the control group (p = 0.01), whereas serum triglyceride levels tended to be significantly lower in the +LCPUFA group than in the control group (p = 0.06) (Table 3). No difference was recorded in serum total C and LDL-C levels between +LCPUFA group and control group.
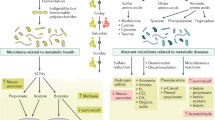
In the entire study population, serum adiponectin concentrations correlated positively with serum HDL-C levels (r = 0.46, p < 0.001); whereas, they correlated negatively with serum triglyceride levels (Fig. 1). No significant correlation between serum adiponectin and total C or between adiponectin and LDL-C levels was found. Serum adiponectin concentrations were also positively associated with HDL-C (r = 0.58, p = 0.001) and negatively associated with serum triglyceride levels (Fig. 1) within the +LCPUFA group; whereas, no significant correlations were found within the −LCPUFA/control group. Thus, the significant correlations found between adiponectin and lipid levels in the entire study population were driven entirely by the supplemented group.
Correlations between serum adiponectin and triglyceride levels. •, infants fed the LCPUFA-supplemented formula (+LCPUFA group); ○, infants fed the LCPUFA-free formula (−LCPUFA/control group). The lines represent the regression slope separately for the +LCPUFA group (– – –; r = −0.58, p = 0.001) and the −LCPUFA/control group (. . . .; r = −0.19, p = 0.29), and for the entire study population (—; r = −0.42, p = 0.001).
Within the +LCPUFA group, significant correlations of adiponectin with total C levels (r = 0.42, p = 0.02) and LDL-C levels (r = 0.48, p = 0.007) were also observed. However, these associations did not remain significant after controlling for HDL-C or triglyceride concentrations by multiple regression analysis; whereas, both HDL-C and triglyceride levels were independently associated with adiponectin concentrations.
DISCUSSION
The present study is the first to indicate that dietary LCPUFA may have a beneficial effect on serum adiponectin in premature infants. The difference in adiponectin levels between infants fed the formula supplemented with DHA and AA, and those fed the LCPUFA-free formula, was not due to the factors previously reported to influence the circulating concentrations of adiponectin in preterm infants, such as adiposity and weight gain (5,21), because anthropometric parameters, including body mass index and weight gain, were similar between groups. In addition, all the infants studied were healthy and their gender, gestational, and postnatal age distribution did not differ significantly between groups. In this trial, we cannot differentiate between the effects of AA and n-3 LCPUFA. However, our findings are consistent with the results of the studies in animals (12–15) and in obese adults (16,18) fed diets supplemented with n-3 LCPUFA. On the contrary, no effect on adiponectin levels was observed after a 3-mo treatment with n-3 LCPUFA in adults who suffered a myocardial infarct (17).
In our study, infants fed the LCPUFA-supplemented formula had significantly higher HDL-C levels than those fed the LCPUFA-free formula and lower triglyceride levels (p = 0.06). These results reflect the well-known favorable effects of n-3 LCPUFA on the blood lipid profile in adults. Linoleic acid (18:2n-6) has well described LDL-C lowering effect, but no specific lipid profile modulating effects has been described for AA, which on a carbon-to-carbon basis is a less potent regulator of lipid metabolism than n-3 LCPUFA (22). N-3 LCPUFA have been shown to lower triglycerides in numerous clinical trials and in a meta-analysis (23). Although this effect is dose-dependent, even low intakes of n-3 LCPUFA have been found to promote a significant reduction in triglycerides (22). The effect of dietary LCPUFA on HDL-C varies; increase, decrease, or a neutral effect on HDL-C levels has been reported in adults, leading to a conclusion that there is no significant impact of n-3 LCPUFA on HDL-C levels (23). In infants, the relation between dietary LCPUFA and lipid profile has been rarely studied. In preterm infants fed a formula supplemented with 0.5% AA and 0.35% DHA, serum total C concentrations were found to be higher, and triglyceride levels lower, than in infants fed an unsupplemented formula (24). In addition, a previous randomized trial in full term infants has shown evidence of an acute plasma triglyceride-lowering effect of fish oil, known to be rich in n-3 LCPUFA, primarily eicosapentanoic acid (EPA) and DHA (25).
The influence of dietary n-3 and n-6 LCPUFA on lipid levels in blood is believed to be mediated via targeted effects on specific transcription factors and nuclear receptors that regulate the expression of genes encoding key regulatory proteins of lipid metabolism (22). The mechanisms how dietary LCPUFA lead to an increase in adiponectin levels are less well known. To our knowledge, no specific role has been suggested for n-6 LCPUFA on the production/release of adiponectin. Stimulation of the expression of the gene encoding adiponectin by dietary n-3 LCPUFA has been shown in animals (12); this could be through the activation of transcription factors in the adipose tissue (26,27). However, no modification, or even inhibition, of adiponectin gene expression was observed in other studies in animals fed a diet supplemented with fish oil (13) or in isolated rat adipocytes cultured with EPA (28). The increase in circulating adiponectin levels by dietary LCPUFA has also been attributed to a lowering effect of n-3 LCPUFA on plasma FFA and triglycerides, which in high concentrations, exert an inhibitory effect on the release of adiponectin by adipocytes (13,14).
It has been reported that adiponectin directly regulates lipid metabolism and exerts a HDL-C-elevating and triglyceride-lowering action (29). Treatment with the globular domain of adiponectin improved fatty utilization in isolated muscle as well as in cultured skeletal muscle cells (6); whereas, disruption of the two receptors of adiponectin (AdipoR1 and R2) resulted in increased tissue triglyceride content (30). Numerous studies in adolescents and adults have shown that adiponectin levels are strongly associated with lipid profile, correlating positively with HDL-C and negatively with triglyceride concentrations (29,31–34).
In our study, the expected correlations between adiponectin and lipid levels were observed in the group of infants fed the LCPUFA-supplemented formula, but not in the group fed the LCPUFA-free diet. The absence of any significant correlation between adiponectin and lipid levels in the unsupplemented group may indicate that there is possibly no mechanistic link between blood lipid profile and adiponectin in preterm infants, but that the observed correlations in the supplemented group reflect parallel effects of dietary LCPUFA on serum adiponectin and lipid levels. In addition, a synergic effect of LCPUFA and adiponectin on lipid profile in the supplemented group cannot be excluded. To our knowledge, the associations between adiponectin and lipid levels in infants have been evaluated in only one study, in umbilical venous blood at birth in newborns between 35 and 42 wk of gestational age. No significant correlation between adiponectin and HDL-C or triglyceride levels in cord blood was found, but a strong inverse relationship between cord adiponectin and LDL-C concentrations was observed (35).
A limitation of this study is that biomarkers of LCPUFA intake, such as the LCPUFA status of the plasma or erythrocytes, were not measured due to the limited amount of blood available from these small preterm infants. It would be useful to know how the LCPUFA status relates to the outcomes of adiponectin and lipid levels in serum. In addition, the AA and DHA content of the LCPUFA-formula were close to the lowest levels of supplementation of other experimental formulas (24,36). It has been reported that a higher content of AA and DHA supplementation (equal or higher than 0.49% AA and 0.35% DHA) is needed to provide sufficient levels of these fatty acids to achieve a fatty acid status in the plasma and erythrocyte membranes similar to that of infants fed breast milk typical of mothers in Western countries (36,37). Whether such a higher content would have stronger effects on adiponectin levels or lipidemic profile in our study population is not known.
Irrespective of the underlying pathophysiological mechanism(s), the higher circulating adiponectin levels in infants fed the LCPUFA-supplemented formula may explain, at least in part, the reported beneficial effect of dietary LCPUFA against insulin resistance in animals and human adults (9). We did not examine whether differences in insulin sensitivity were already present between the two groups of studied infants. However, the protection that the increased adiponectin concentrations may provide against later development of insulin resistance and metabolic syndrome is, in our opinion, of special importance to preterm infants because they are at risk to develop such maladies. Several observations support a programming effect of dietary LCPUFA on later health. In animals, adequate availability of EPA, DHA, and AA during the perinatal period is critical to prevent development of metabolic syndrome in adult life (9). In humans, DHA and AA supplementation in early life is associated with lower blood pressure later in life (38). Notably, there is evidence that breast milk has a beneficial role on the major components of metabolic syndrome (obesity, blood pressure, C metabolism, and insulin resistance) that affect cardiovascular risk (39); this has been attributed, at least in part, to the rich content of breast milk in LCPUFA (40). Follow-up of our study population is needed to examine whether the positive influence of dietary LCPUFA on adiponectin levels and on the lipidemic profile is indicative of a long-term beneficial effect of LCPUFA on the health of these infants in later life.
Abbreviations
- AA:
-
arachidonic acid
- DHA:
-
docosahexanoic acid
- EPA:
-
eicosapentanoic acid
- LCPUFA:
-
long-chain polyunsaturated fatty acids
References
Eriksson JG, Forsen T, Tuomilehto J, Jaddoe VW, Osmond C, Barker DJ 2002 Effects of size at birth and childhood growth on the insulin resistance syndrome in elderly individuals. Diabetologia 45: 342–348
Barker DJ 2002 Fetal programming of coronary heart disease. Trends Endocrinol Metab 13: 364–368
Regan FM, Cutfield WS, Jefferies C, Robinson E, Hofman PL 2006 The impact of early nutrition in premature infants on later childhood insulin sensitivity and growth. Pediatrics 118: 1943–1949
Hofman PL, Regan F, Cutfield WS 2006 Prematurity-another example of perinatal metabolic programming?. Horm Res 66: 33–39
Siahanidou T, Mandyla H, Papassotiriou GP, Papassotiriou I, Chrousos G 2007 Circulating levels of adiponectin in preterm infants. Arch Dis Child Fetal Neonatal Ed 92: F286–F290
Karbowska J, Kochan Z 2006 Role of adiponectin in the regulation of carbohydrate and lipid metabolism. J Physiol Pharmacol 57: 103–113
Spranger J, Kroke A, Mohlig M, Bergmann MM, Ristow M, Boeing H, Pfeiffer AF 2003 Adiponectin and protection against type-2 diabetes mellitus. Lancet 361: 226–228
Kumada M, Kihara S, Sumitsuji S, Kawamoto T, Matsumoto S, Ouchi N, Arita Y, Okamoto Y, Shimomura I, Hiraoka H, Nakamura T, Funahashi T, Matsuzawa Y 2003 Association of hypoadiponectinemia with coronary artery disease in men. Arterioscler Thromb Vasc Biol 23: 85–89
Das UN 2005 Pathophysiology of metabolic syndrome X and its links to the perinatal period. Nutrition 21: 762–773
Simopoulos AP 1991 Omega-3 fatty acids in health and disease and in growth and development. Am J Clin Nutr 54: 438–463
Wijendran V, Hayes KC 2004 Dietary n-6 and n-3 fatty acid balance and cardiovascular health. Annu Rev Nutr 24: 597–615
Flachs P, Mohamed-Ali V, Horakova O, Rossmeisl M, Hosseinzadeh-Attar MJ, Hensler M, Ruzickova J, Kopecky J 2006 Polyunsaturated fatty acids of marine origin induce adiponectin in mice fed a high-fat diet. Diabetologia 49: 394–397
Rossi AS, Lombardo YB, Lacorte JM, Chicco AG, Rouault C, Slama G, Rizkalla SW 2005 Dietary fish oil positively regulates plasma leptin and adiponectin levels in sucrose-fed, insulin-resistant rats. Am J Physiol Regul Integr Comp Physiol 289: R486–R494
Shirouchi B, Nagao K, Inoue N, Ohkubo T, Hibino H, Yanagita T 2007 Effect of dietary omega 3 phosphatidylcholine on obesity-related disorders in obese Otsuka Long-Evans Tokushima fatty rats. J Agric Food Chem 55: 7170–7176
Duda MK, O'Shea KM, Lei B, Barrows BR, Azimzadeh AM, McElfresh TE, Hoit BD, Kop WJ, Stanley WC 2007 Dietary supplementation with omega-3 PUFA increases adiponectin and attenuates ventricular remodeling and dysfunction with pressure overload. Cardiovasc Res 76: 303–310
Itoh M, Suganami T, Satoh N, Tanimoto-Koyama K, Yuan X, Tanaka M, Kawano H, Yano T, Aoe S, Takeya M, Shimatsu A, Kuzuya H, Kamei Y, Ogawa Y 2007 Increased adiponectin secretion by highly purified eicosapentanoic acid in rodent models of obesity and human obese subjects. Arterioscler Thromb Vasc Biol 27: 1918–1925
Patel JV, Lee KW, Tomson J, Dubb K, Hughes EA, Lip GY 2007 Effects of omega-3 polyunsaturated fatty acids on metabolically active hormones in patients post-myocardial infarction. Int J Cardiol 115: 42–45
Krebs JD, Browning LM, McLean NK, Rothwell JL, Mishra GD, Moore CS, Jebb SA 2006 Additive benefits of long-chain n-3 polyunsaturated fatty acids and weight-loss in the management of cardiovascular risk in overweight hyperinsulinaemic women. Int J Obes (Lond) 30: 1535–1544
Ballard JL, Khoury JC, Wedig K, Wang L, Eilers-Walsman BL, Lipp R 1991 New Ballard Score, expanded to include extremely premature infants. J Pediatr 119: 417–423
Oken E, Kleinman KP, Rich-Edwards J, Gillman MW 2003 A nearly continuous measure of birth weight for gestational age using a United States national reference. BMC Pediatr 3: 6
Kajantie E, Hytinantti T, Hovi P, Andersson S 2004 Cord plasma adiponectin: a 20-fold rise between 24 weeks gestation and term. J Clin Endocrinol Metab 89: 4031–4036
Davidson MH 2006 Mechanisms for the hypotriglyceridemic effect of marine omega-3 fatty acids. Am J Cardiol 98: 27i–33i
Hooper L, Thompson RL, Harrison RA, Summerbell CD, Moore H, Worthington HV, Durrington PN, Ness AR, Capps NE, Davey Smith G, Riemersma RA, Ebrahim SB 2004 Omega 3 fatty acids for prevention and treatment of cardiovascular disease. Cochrane Database Syst Rev 4: CD003177
Vanderhoof J, Gross S, Hegyi T, Clandinin T, Porcelli P, DeCristofaro J, Rhodes T, Tsang R, Shattuck K, Cowett R, Adamkin D, McCarton C, Heird W, Hook-Morris B, Pereira G, Chan G, Van Aerde J, Boyle F, Pramuk K, Euler A, Lien EL 1999 Evaluation of a long-chain polyunsaturated fatty acid supplemented formula on growth, tolerance, and plasma lipids in preterm infants up to 48 weeks postconceptional age. J Pediatr Gastroenterol Nutr 29: 318–326
Damsgaard CT, Schack-Nielsen L, Michaelsen KF, Fruekilde MB, Hels O, Lauritzen L 2006 Fish oil affects blood pressure and the plasma lipid profile in healthy Danish infants. J Nutr 136: 94–99
Iwaki M, Matsuda M, Maeda N, Funahashi T, Matsuzawa Y, Makishima M, Shimomura I 2003 Induction of adiponectin, a fat-derived antidiabetic and antiatherogenic factor, by nuclear receptors. Diabetes 52: 1655–1663
Lihn AS, Jessen N, Pedersen SB, Lund S, Richelsen B 2004 AICAR stimulates adiponectin and inhibits cytokines in adipose tissue. Biochem Biophys Res Commun 316: 853–858
Lorente-Cebrian S, Perez-Matute P, Martinez JA, Marti A, Moreno-Aliaga MJ 2006 Effects of eicosapentaenoic acid (EPA) on adiponectin gene expression and secretion in primary cultured rat adipocytes. J Physiol Biochem 62: 61–69
Baratta R, Amato S, Degano C, Farina MG, Patane G, Vigneri R, Frittitta L 2004 Adiponectin relationship with lipid metabolism is independent of body fat mass: evidence from both cross-sectional and intervention studies. J Clin Endocrinol Metab 89: 2665–2671
Yamauchi T, Nio Y, Maki T, Kobayashi M, Takazawa T, Iwabu M, Okada-Iwabu M, Kawamoto S, Kubota N, Kubota T, Ito Y, Kamon J, Tsuchida A, Kumagai K, Kozono H, Hada Y, Ogata H, Tokuyama K, Tsunoda M, Ide T, Murakami K, Awazawa M, Takamoto I, Froguel P, Hara K, Tobe K, Nagai R, Ueki K, Kadowaki T 2007 Targeted disruption of AdipoR1 and AdipoR2 causes abrogation of adiponectin binding and metabolic actions. Nat Med 13: 332–339
Furler SM, Gan SK, Poynten AM, Cisholm DJ, Campbell LV, Kriketos AD 2006 Relationship of adiponectin with insulin sensitivity in humans, independent of lipid availability. Obesity (Silver Spring) 14: 228–234
Martin LJ, Woo JG, Daniels SR, Goodman E, Dolan LM 2005 The relationships of adiponectin with insulin and lipids are strengthened with increasing adiposity. J Clin Endocrinol Metab 90: 4255–4259
Steffes MW, Gross MD, Lee DH, Schreiner PJ, Jacobs DR Jr 2006 Adiponectin, visceral fat, oxidative stress, and early macrovascular disease: the coronary artery risk development in young adults study. Obesity (Silver Spring) 14: 319–326
Matsubara M, Maruoka S, Katayose S 2002 Decreased plasma adiponectin concentrations in women with dyslipidemia. J Clin Endocrinol Metab 87: 2764–2769
Bansal N, Charlton-Menys V, Pemberton P, McElduff P, Oldroyd J, Vyas A, Koudsi A, Clayton PE, Cruickshank JK, Durrington PN 2006 Adiponectin in umbilical cord blood is inversely related to low-density lipoprotein cholesterol but not ethnicity. J Clin Endocrinol Metab 91: 2244–2249
Clandinin MT, Van Aerde JE, Parrott A, Field CJ, Euler AR, Lien E 1999 Assessment of feeding different amounts of arachidonic and docosahexaenoic acids in preterm infant formulas on the fatty acid content of lipoprotein lipids. Acta Paediatr 88: 890–896
Fleith M, Clandinin MT 2005 Dietary PUFA for preterm and term infants: review of clinical studies. Crit Rev Food Sci Nutr 45: 205–229
Forsyth JS, Willatts P, Agostoni C, Bissenden J, Casaer P, Boehm G 2003 Long chain polyunsaturated fatty acid supplementation in infant formula and blood pressure in later childhood: follow up of a randomized controlled trial. BMJ 326: 953–957
Singhal A 2006 Early nutrition and long-term cardiovascular health. Nutr Rev 64: S44–S49
Das UN 2002 The lipids that matter from infant nutrition to insulin resistance. Prostaglandins Leukot Essent Fatty Acids 67: 1–12
Author information
Authors and Affiliations
Corresponding author
Additional information
The study was funded by the School of Medicine, University of Athens, Greece.
Rights and permissions
About this article
Cite this article
Siahanidou, T., Margeli, A., Lazaropoulou, C. et al. Circulating Adiponectin in Preterm Infants Fed Long-Chain Polyunsaturated Fatty Acids (LCPUFA)-Supplemented Formula—A Randomized Controlled Study. Pediatr Res 63, 428–432 (2008). https://doi.org/10.1203/PDR.0b013e31816780e4
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e31816780e4