Abstract
Intestinal alkaline sphingomyelinase (Alk-SMase) and neutral ceramidase may catalyze the hydrolysis of endogenous sphingomyelin (SM) and milk SM in human-milk fed infants. The enzymes generate sphingolipid metabolites that may influence gut maturation. Alk-SMase also inactivates platelet-activating factor (PAF) that is involved in the pathogenesis of necrotizing enterocolitis (NEC). We examined whether the two enzymes are expressed in both preterm and term infants and analyzed Alk-SMase, neutral ceramidase, SM, and sphingolipid metabolites in meconium. Meconium was collected from 46 preterm (gestational ages 23–36 wk) and 38 term infants (gestational ages 37–42 wk) and analyzed for Alk-SMase using 14C-choline–labeled SM and for neutral ceramidase using 14C-octanoyl-sphingosine as substrates. Molecular species of SM, ceramide, and sphingosine were analyzed by high-performance liquid chromatography mass spectroscopy. Meconium contained significant levels of Alk-SMase and ceramidase at all gestational ages. It also contained 16–24 carbon molecular species of SM, palmitoyl- and stearoyl-sphingosine, and sphingosine. There were positive correlations between levels of SM and ceramide and between ceramide and sphingosine levels. In conclusion, Alk-SMase and ceramidase are expressed in the gut of both preterm and term newborn infants and may generate bioactive sphingolipid messengers.
Similar content being viewed by others
Main
Sphingolipids are important constituents of cell membranes, particularly plasma and lysosomal membranes, and the enteral mucosal brush border. SM consists of a long-chain sphingoid base, linked with an amide bond to a long-chain fatty acid and the polar head group phosphocholine. Sphingomyelinases (SMases) catalyze the hydrolysis of SM to phosphocholine and ceramide and ceramidases catalyze the hydrolysis of ceramide to free fatty acids and sphingoid bases, primarily sphingosine (Fig. 1) (1). Different SMases and ceramidases are designated by their pH optimum as acid, neutral, and alkaline (2,3). Mucosal Alk-SMase and neutral ceramidase are key enzymes of SM and ceramide metabolism in the gut (1,4–6). Ceramide and sphingosine and sphingosine-1-phosphate (S-1-P), which is formed after the absorption of sphingosine into mucosal cells, are signaling substances with multiple effects acting through several activation pathways (7–9).
The human milk–fed infant ingests about 150 mg of SM per day because SM is a major polar milk lipid accounting for 40% of the milk fat globule membrane (10,11). Furthermore, the mucosal brush border contains significant amounts of SM, ceramides, and glycosphingolipids, which are alternative substrates for intestinal sphingolipid hydrolyzing enzymes. Unlike dietary glycerolipids, sphingolipids are not degraded by pancreatic enzymes. SM is sequentially hydrolyzed by Alk-SMase and neutral ceramidase acting at the brush border of the intestinal epithelium and in the gut lumen (6,11). Alk-SMase is a tissue-specific enzyme that is expressed in the gut with highest levels in the middle and lower small intestine and in humans also in bile (1,12,13). The enzyme was cloned and identified as a novel member of the nucleotide phosphodiesterase (NPP) family (13). Furthermore, it was shown that Alk-SMase inactivates the potent proinflammatory lipid messenger PAF (1-alken-2-acetyl-glycerophosphocholine) (14). PAF can be produced in the intestine and has been ascribed a pathogenic role in neonatal NEC (15).
Neutral ceramidase of the gut (5) has been purified and characterized in both rat (16) and human tissue (L. Ohlsson et al., Abstract OP-G-283, EUGW, Copenhagen 2005), and was found to have extensive homology to neutral ceramidase of other tissues. The crucial role of neutral ceramidase in ceramide digestion in the gut was recently confirmed by studies on gene-targeted mice lacking active neutral ceramidase 2 (17).
Both Alk-SMase and intestinal ceramidase are highly glycosylated and resistant to proteases and remain active in the gut lumen (13,16,18). They are released in active form by bile salts and, in the case of Alk-SMase, by tryptic cleavage of an anchoring C-terminal fragment (19). These features made it possible to use ileostomy content as starting material for purification of both enzymes (13,16,18), and to use fecal levels as a measure of Alk-SMase expression (20).
In the fetal rat, the gut epithelium undergoes rapid transformation with formation of mature villus cells and distinct villus and crypt structures around d 18 of gestation i.e. soon before birth at d 23 (21). Expression of Alk-SMase coincides with this differentiation (22). In human fetal life differentiation of the epithelium is extended over a longer time period. Brush border enzymes characteristic of the mature villus cells develop progressively from the 13th gestational week (23). However, no previous study has measured activity of Alk-SMase and neutral ceramidase and sphingolipid metabolites in human newborns.
This study examines the levels of Alk-SMase, neutral ceramidase, and key sphingolipid metabolites in meconium of newborn preterm and term infants, for three reasons: First, milk SM or its bioactive metabolites may influence intestinal maturation (24). Second, it is important to know whether the ability to inactivate PAF via Alk-SMase is developed in the most preterm infants who are most susceptible to NEC. Third, the analyses concern enzymes and metabolites that may trigger sphingolipid signaling during lung epithelial and alveolar cell apoptosis and inflammation that characterizes meconium aspiration syndrome (25).
METHODS
Subjects.
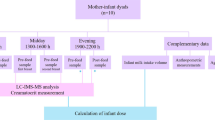
The study population consisted of 46 preterm infants (gestational ages 23–36 wk) treated in the neonatal intensive care unit of Lund University Hospital, Sweden, and 38 healthy term infants in the maternity unit of the Department of Obstetrics and Gynecology. Infants were stratified in five groups according to gestational age: 23–25 wk, 26–28 wk, 29–32 wk, 33–36 wk, and 37–42 wk. Patient characteristics are given in Table 1. A majority of the preterm infants needed surfactant and mechanical ventilation. All preterm infants, except for one infant who had gastrochisis, received oral feedings with human milk (donor or mother's own), usually within the first hours of life (26). Five of the full-term infants received milk replacement formulations. All the others were breast-fed.
Sample collection and preparation. The study was approved by the Lund University Research Ethics Committee, written informed parental consent was obtained before inclusion in the study. Meconium was collected soon after birth and frozen in test tubes (Table 1). Before determination, samples were weighed and suspended in 0.15 mol/L NaCl containing 1 mmol/L benzamidine to a concentration about 0.25 g/mL. The samples were stirred vigorously and then centrifuged at 3000 rpm for 10 min. The supernatant was saved for biochemical analysis and lipid extraction.
SMase assay.
The activities of different types of SMase activity were analyzed as described (27). The buffers used were 50 mmol/L of Tris-maleate buffer pH 5.0 containing 0.15 mol/L NaCl and 0.12% Triton X-100 for acid SMase, 50 mmol/L of Tris-HCl buffer pH 7.5 containing 4 mmol/L Mg2+ and 0.12% Triton X-100 for neutral SMase, and 50 mmol/L of Tris-HCl pH 9.0 containing 2 mmol/L ethylenediamine tetraacetic acid, 0.15 mol/L NaCl, and 6 mmol/L taurocholate for Alk-SMase. For each determination, a 10-μL sample was mixed with 90 μL of buffer containing 80 pmole [14C]SM (8000 dpm) and incubated at 37°C for 30 min. The reaction was terminated by adding 0.4 mL chloroform/methanol (2/1, vol/vol) followed by centrifugation at 10,000× g for 5 s. An aliquot of the upper phase was taken and the production of 14C-phosphocholine was determined by liquid scintillation.
Neutral ceramidase assay.
Neutral ceramidase was assayed as described (16). 14C-octanoyl-sphingosine was used as substrate, and the incubation buffer was 50 mmol/L of Tris-maleate pH 7.0 containing 10 mmol/L of sodium taurocholate. The assay was started by adding 10 μL of the sample containing the enzyme with 90 μL of the assay buffer with substrate, and the samples were incubated at 37°C for 1 h. The reaction was interrupted by adding 0.6 mL methanol-chloroform-heptane in proportions of 28:25:20 (vol/vol/vol) and 0.2 mL of 0.05 mol/L K2CO3-K2B2O2, pH 10. After mixing, the tubes were centrifuged at 10,000 rpm for 10 s. An aliquot of 200 μL of upper phase was taken for liquid scintillation counting, and the rate of hydrolysis was calculated from the proportion of the radioactive substrate that had been hydrolyzed (28).
Analysis of SM, ceramide, and sphingosine.
Ceramide was determined by liquid chromatography tandem mass spectrometry (LC-MS-MS) as described (29). 18-d-erythro-sphingosine, C-22-SM, C-23-SM, and C-24-SM were analyzed by the same method. The fragments analyzed were for 18-d-erythro-sphingosine m/z 300.1/264.4 [collision energy (CE) 28 V], for C-22-SM m/z 787.9/183.8 (CE 39 V), for C-23-SM m/z 801.9/183.8 (CE 39 V), and for C-24-SM m/z 815.9/183.8 (CE 39 V). Weighed standards C-16- and C-18-ceramide were used for preparation of calibration curves. For C-22-SM, C-23-SM, and C-24-SM milk, SM containing a mixture of several molecular species of SM was used as the standard. Thus, the content of each individual C-22-SM through C-24-SM species in the standard sample was calculated from the total SM mass and the known fatty acid composition of milk SM (30).
C-16-SM (palmitoyl-SM) is abundant among intestinal epithelial and bile SM species that also contain 18 carbon d-erythro-sphingosine, whereas longer fatty acids (more than 20 carbons) are abundant in SM species containing 4-hydroxysphinganine as a sphingoid base and in glycolipids (31). Comparison of C-16-SM and C-16-ceramide levels would therefore be expected to best reflect SM hydrolysis, and analyses were focused on C-16 and C-18 species of ceramide, for which authentic synthetic standards are also available. Because SM of most tissues contains high proportions of longer chain SM species, we analyzed also meconium for C-22:0, C-23:0, and C-24:0 SM species to see whether the fatty acid composition reflects intestinal tissue SM rather than bile SM.
Statistical analysis.
Apart from the individual values shown in some figures, most of the data are presented as mean ± standard error. The correlation was performed by linear regression analysis using the program GraphPad Prism 4; p < 0.05 was considered significant for the correlation.
RESULTS
Alk-SMase and neutral ceramidase in meconium.
Alk-SMase was the predominant SMase at all gestational ages, being much higher than the other SMase activities, i.e. acid and neutral SMase. Values for the activity of the different SMases in all meconium samples, expressed as pmole/h/mg meconium [mean (SEM)] were 30,160 (3010) for Alk-SMase, 7.43 (0.92) for acid SMase, and 5.03 (0.47) for neutral SMase. Significant Alk-SMase activity was found in all meconium samples, i.e. also in those from the most preterm children. If anything, the activity per gram of meconium was higher in samples from preterm than in samples from term infants (Fig. 2A). Because Alk-SMase and neutral intestinal ceramidase catalyze the sequential degradation of SM to sphingosine and free fatty acids, we asked whether the ceramidase and the Alk-SMase are simultaneously expressed. As shown in Figure 2B, ceramidase was present in all meconium samples. The relationship of ceramidase activity to gestational age was similar to that of Alk-SMase, i.e. the enzyme was present also in the most preterm infants and the activity per weight of meconium was not lower than in the term infants. There was a strong positive correlation between the levels of the two enzymes (Fig. 3). However, with the assay methods used, the activity of Alk-SMase was found to be about 10 times higher than that of neutral ceramidase.
Because most of the preterm infants had received treatment with antenatal corticosteroids, antibiotics, and surfactant, it was not possible to examine possible effects from these interventions on Alk-SMase and ceramidase levels. The premature child with gastrochisis was among those infants who had low Alk-SMase values. The five term infants who received milk replacement formulations did not differ significantly from the breast-fed children on any of the parameters.
Sphingolipids in meconium.
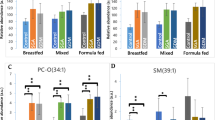
Levels of C-16- and C-18-SM and of the corresponding ceramide species are summarized in Figure 4. The levels of C-16 species of both SM and ceramide exceeded the levels of C-18 species. The average C-16-ceramide/C-16-SM wt/wt ratio was 0.6 and the average mol/mol ratio was 0.8, indicating that hydrolysis of C-16-SM had occurred. Individual data for C-16-SM and C-16-ceramide in relation to gestational age are shown in Figure 5A and B. Both compounds were present in all samples examined, but individual values for each compound or for the C-16-ceramide/C-16-SM ratio did not correlate with gestational age or gender.
Palmitoyl and stearoyl species of SM and ceramide and sphingosine in meconium. The figure shows ) for concentration [mean (SEM)] in meconium of C-16-SM, C-16-ceramide, C-18-SM, C-18-ceramide, and sphingosine (sph). Values are given as mass per wet weight of meconium. The average molar ratio of C-16-ceramide to C-16-SM was 0.79.
SM, ceramide, and sphingosine in meconium. (A) Individual values for C-16-SM. Four outlying values are not shown: 283.3 at 23 wk, 178.8 at 24 wk, 311.6 at 26 wk, and 414.6 at 28 wk. Values for C-16-ceramide (B) and for sphingosine (C). (C) Four outlying values are not shown: 15.5 at 25 wk, 23.1 at 28 wk, 44.4 at 29 wk, and 26.8 at 34 wk. There was no significant correlation between SM or any of the two metabolites with gestational age.
(C-18-d-erythro-)sphingosine levels are shown in Figure 5C. The sphingosine levels were lower than the ceramide levels and did not correlate with gestational age or gender, but sphingosine was found in all samples examined. When the correlations between related metabolites were examined, we found that the sum of C-16- SM + C-18-SM was positively correlated with that of C-16-ceramide + C-18-ceramide, and the levels of these ceramides are positively related to those of sphingosine (Fig. 6A and B).
Correlations between SM, ceramide, and sphingosine levels in meconium. (A) The correlation between SM (sum of C-16-SM + C-18-SM) and of ceramide (sum of C-16-ceramide + C-18-ceramide) (r2 = 0.2691 and p < 0.001). (B) The correlation between C-16-ceramide + C-18-ceramide and sphingosine (r2 = 0.3749 and p < 0.0001). Thus, the levels of ceramide and sphingosine correlated strongly with the levels of the substrates from which these metabolites are formed.
Meconium also contained long-chain (C-22:0, C-23:0, and C-24:0) SM species (data not shown).
DISCUSSION
This study shows that Alk-SMase and neutral ceramidase are present in significant amounts in meconium of newborn human infants. Both enzymes were expressed even in the most premature children born at 23–26 gestational weeks. Slightly higher values per gram meconium were actually found in the samples from the preterm infants, which may reflect the amount of enzymes produced as well as dilution factors. The levels are comparable to those found in adult feces, in feces from 3-wk-old pigs, and in duodenal and jejunal content from a few measurements in newborns (1).
The findings are in line with those of studies on other brush border enzymes as alkaline phosphatase and lactase that are expressed from 17 gestational weeks (23), i.e. when mature villi differentiate in humans. By 20 wk of gestation, the anatomic differentiation of the fetal gut has progressed to the extent that it resembles that of a newborn (23). Thus, the presence of both neutral ceramidase and Alk-SMase probably reflects the formation of mature epithelium expressing brush border enzymes. This interpretation is in line with our finding in fetal rat that Alk-SMase was promptly expressed around d 20 as the appearance of mature differentiated epithelium occurs before delivery at d 23 (22). As the Alk-SMase increased, the acid SMase decreased promptly in the rat. In the present study, acid and neutral SMase activities were far lower than those of Alk-SMase, which may reflect either a similar down-regulation of acid SMase in humans or differences in stability between the SMases. Whereas Alk-SMase is protease resistant and survives in active form in intestinal and fecal environments, this is not the case for acid and neutral SMase (32). The ratios between acid or neutral and alkaline SMase may therefore be higher in intestinal epithelium than is reflected in meconium. Intestinal neutral ceramidase is as stable to proteases as Alk-SMase (16). The strong correlation between Alk-SMase and neutral ceramidase (Fig. 3) thus most likely reflects coexpression of both enzymes. They may enter the meconium both by sloughing of mucosal cells and by release from intact villus cells by bile salts or trypsin (16,18,19).
Corticosteroid treatment is known to enhance intestinal maturation and expression of brush border enzymes and transporters (23). Because most of the premature infants had been exposed to antenatal treatment with corticosteroids, Alk-SMase and ceramidase expression may thus have been influenced by this treatment.
Three pieces of evidence indicate that Alk-SMase and neutral ceramidase are key enzymes in digestion of SM (1,5,6,16,18,19). First, enzymes hydrolyzing SM are absent in pancreatic juice (5). Second, SM digestion occurs mainly in the middle and lower small intestine where Alk-SMase and neutral ceramidase are preferentially located (1,28). Third, Alk-SMase is specifically dependent on certain bile salts, primarily taurocholate and taurochenodeoxycholate (18). Human milk bile salt–stimulated lipase (BSSL) has some ceramidase activity (33), but is active primarily in the proximal intestine and is not active against ceramide in the presence of other competing substrates such as glycerolipids (34). Furthermore, gene-targeted mice lacking BSSL exhibited normal ceramidase activity except in the uppermost part of the gut (34), whereas neutral ceramidase 2 gene knockout mice exhibited decreased ceramide digestion with increased levels of ceramide in feces (17).
By the action of Alk-SMase and neutral ceramidase on SM of the polar lipids in the milk fat globule membrane, the human milk–fed infant may thus use both the phosphocholine and the hydrophobic components of SM. Furthermore, the sphingolipid metabolites that these enzymes generate may influence cellular growth and differentiation in the fetal and neonatal gut. It is recognized that mothers' milk is important for the normal maturation of the infant gut mucosa, but the factors involved are only partly known. Moutori et al. (24) fed newborn rat pups milk replacement formulas with and without SM, resulting in differences in lactase activity, distribution of vacuolated cells, and Auerbach nerve plexus area, indicating that SM intake influenced neonatal gut maturation. Our data indicate that if this effect requires hydrolysis of SM, it may be exerted both in premature and full-term children who are breast-fed.
A novel function of Alk-SMase was recently discovered. PAF, a strong proinflammatory lipid messenger (1-alken.2-acetyl-3-phosphocholine glycerol), was found to be hydrolyzed and inactivated by Alk-SMase (14). Because PAF is known to be present in meconium and found in increased amounts in infants with NEC (15), the finding of Alk-SMase in the meconium of preterm infants provides a potential novel anti-inflammatory mechanism that may counteract NEC.
Milk feeding is associated with a lower risk of NEC (35). The reasons are unknown. Carlson et al. (36) reported a lower incidence of NEC in infants fed a preterm formula with egg phospholipids and emphasized the supply of polyunsaturated fatty acids, in particular of arachidonic acid, as a precursor of eicosanoids. Because about 70% of egg phospholipids are phosphatidylcholine and 3% is SM, the supply of choline may be important as well. Combined with our data, the findings emphasize that polar milk lipids are potential protective agents against NEC. Such an action may be exerted by the intact polar lipids or by metabolites with anti-inflammatory action (e.g. ceramide and sphingosine) or the ability to stimulate regeneration or survival of mucosal epithelial cells (S-1-P, prostaglandins, lysophosphatidic acid).
Because Alk-SMase and ceramidase may generate bioactive sphingolipid metabolites from endogenous SM during fetal development, we examined the levels of key SM and ceramide species and of sphingosine. Meconium contained both C-16-SM, C-18-SM, and SM with very long chain fatty acids. High levels of C-22-SM through C-24-SM indicated that much of the meconium SM originates from intestinal tissue rather than bile. Meconium also contained C-16-ceramide and C-18-ceramide and free sphingosine. Palmitic acid, with sphingosine as a base, is abundant in SM of intestinal epithelial cells and bile, whereas longer fatty acids are abundant in glycolipids and in SM containing 4-hydroxysphinganine (31). The C-16-ceramide/C-16-SM ratio is therefore likely to indicate the degree of hydrolysis of C-16-SM and was found to be much higher than is normally found in tissues. There was a positive correlation between C-16-SM and C-18 SM and ceramide species, which further supports that these ceramides in meconium are derived mainly from hydrolysis of SM. Obviously, C-16-ceramide and C-18-ceramide are not likely to be the only ceramide species in meconium. Hydrolysis of long-chain SM and of glycosphingolipids, as cerebroside, hematoside, and blood group active fucolipids known to be present in meconium (37–39), may generate molecular ceramide species containing very long chain and hydroxylated fatty acids.
All meconium samples also contained sphingosine. Sphingosine is derived from delta-4-desaturation of dihydrosphingosine in ceramide. Free sphingosine in meconium must therefore be formed by hydrolysis of ceramide. Accordingly, we found a positive correlation between the levels of ceramide (C-16 and C-18) and of sphingosine. The level of sphingosine was lower than that of ceramide, probably due to absorption and metabolism of sphingosine by the gut (4). Yet, the amount may be highly significant, considering that ceramide and sphingosine are lipid messengers that exert biologic effects at low concentrations. Thus, ceramide and sphingosine are present in meconium and may be generated by Alk-SMase and ceramidase. Further studies of their biologic effects during the gut maturation and differentiation are therefore highly motivated. Based on our findings, Alk-SMase, ceramidase, and the sphingolipid metabolites should also be added to the list of compounds that might exert biologic effects in the lungs during meconium aspiration (40).
In conclusion, we studied the levels of Alk-SMase and neutral ceramidase in meconium at different gestational ages and found that both enzymes are expressed early. We also found that meconium contains significant amounts of SM, ceramide, and free sphingosine. We postulate that the two enzymes are important in the metabolism of milk and mucosal sphingolipids and generate sphingolipid metabolites with important biologic effects during intestinal maturation.
Abbreviations
- Alk-SMase:
-
alkaline sphingomyelinase
- NEC:
-
necrotizing enterocolitis
- PAF:
-
platelet- activating factor
- SM:
-
sphingomyelin
References
Nilsson A, Duan RD 2006 Absorption and lipoprotein transport of sphingomyelin. J Lipid Res 47: 154–171
Pettus BJ, Chalfant CE, Hannun YA 2002 Ceramide in apoptosis: an overview and current perspectives. Biochim Biophys Acta 1585: 114–125
Levade T, Andrieu-Abadie N, Segui B, Auge N, Chatelut M, Jaffrezou JP, Salvayre R 1999 Sphingomyelin-degrading pathways in human cells role in cell signalling. Chem Phys Lipids 102: 167–178
Nilsson A 1968 Metabolism of sphingomyelin in the intestinal tract of the rat. Biochim Biophys Acta 164: 575–584
Nilsson A 1969 The presence of spingomyelin- and ceramide-cleaving enzymes in the small intestinal tract. Biochim Biophys Acta 176: 339–347
Nilsson A, Duan RD 1999 Alkaline sphingomyelinases and ceramidases of the gastrointestinal tract. Chem Phys Lipids 102: 97–105
Hannun YA, Luberto C, Argraves KM 2001 Enzymes of sphingolipid metabolism: from modular to integrative signaling. Biochemistry 40: 4893–4903
Pyne S 2002 Cellular signaling by sphingosine and sphingosine 1-phosphate. Their opposing roles in apoptosis. Subcell Biochem 36: 245–268
Cuvillier O 2002 Sphingosine in apoptosis signaling. Biochim Biophys Acta 1585: 153–162
Zeisel SH, Mar MH, Howe JC, Holden JM 2003 Concentrations of choline-containing compounds and betaine in common foods. J Nutr 133: 1302–1307
Vesper H, Schmelz EM, Nikolova-Karakashian MN, Dillehay DL, Lynch DV, Merrill AH Jr 1999 Sphingolipids in food and the emerging importance of sphingolipids to nutrition. J Nutr 129: 1239–1250
Duan RD, Nilsson A 1997 Purification of a newly identified alkaline sphingomyelinase in human bile and effects of bile salts and phosphatidylcholine on enzyme activity. Hepatology 26: 823–830
Duan RD, Bergman T, Xu N, Wu J, Cheng Y, Duan J, Nelander S, Palmberg C, Nilsson A 2003 Identification of human intestinal alkaline sphingomyelinase as a novel ecto-enzyme related to the nucleotide phosphodiesterase family. J Biol Chem 278: 38528–38536
Wu J, Nilsson A, Jonsson BA, Stenstad H, Agace W, Cheng Y, Duan RD 2006 Intestinal alkaline sphingomyelinase hydrolyses and inactivates platelet-activating factor by a phospholipase C activity. Biochem J 394: 299–308
Amer MD, Hedlund E, Rochester J, Caplan MS 2004 Platelet-activating factor concentration in the stool of human newborns: effects of enteral feeding and neonatal necrotizing enterocolitis. Biol Neonate 85: 159–166
Olsson M, Duan RD, Ohlsson L, Nilsson A 2004 Rat intestinal ceramidase: purification, properties, and physiological relevance. Am J Physiol Gastrointest Liver Physiol 287: G929–G937
Kono M, Dreier JL, Ellis JM, Allende ML, Kalkofen DN, Sanders KM, Bielawski J, Bielawska A, Hannun YA, Proia RL 2006 Neutral ceramidase encoded by the Asah2 gene is essential for the intestinal degradation of sphingolipids. J Biol Chem 281: 7324–7331
Duan RD, Cheng Y, Hansen G, Hertervig E, Liu JJ, Syk I, Sjostrom H, Nilsson A 2003 Purification, localization, and expression of human intestinal alkaline sphingomyelinase. J Lipid Res 44: 1241–1250
Wu J, Liu F, Nilsson A, Duan RD 2004 Pancreatic trypsin cleaves intestinal alkaline sphingomyelinase from mucosa and enhances the sphingomyelinase activity. Am J Physiol Gastrointest Liver Physiol 287: G967–G973
Di Marzio L, Di Leo A, Cinque B, Fanini D, Agnifili A, Berloco P, Linsalata M, Lorusso D, Barone M, De Simone C, Cifone MG 2005 Detection of alkaline sphingomyelinase activity in human stool: proposed role as a new diagnostic and prognostic marker of colorectal cancer. Cancer Epidemiol Biomarkers Prev 14: 856–862
Trier JS, Moxey PC 1979 Morphogenesis of the small intestine during fetal development. Ciba Found Symp Jan 16-: 3–29.
Lillienau J, Cheng Y, Nilsson A, Duan RD 2003 Development of intestinal alkaline sphingomyelinase in rat fetus and newborn rat. Lipids 38: 545–549
Montgomery RK, Mulberg AE, Grand RJ 1999 Development of the human gastrointestinal tract: twenty years of progress. Gastroenterology 116: 702–731
Motouri M, Matsuyama H, Yamamura J, Tanaka M, Aoe S, Iwanaga T, Kawakami H 2003 Milk sphingomyelin accelerates enzymatic and morphological maturation of the intestine in artificially reared rats. J Pediatr Gastroenterol Nutr 36: 241–247
Zagariya A, Bhat R, Chari G, Uhal B, Navale S, Vidyasagar D 2005 Apoptosis of airway epithelial cells in response to meconium. Life Sci 76: 1849–1858
Bellander M, Ley D, Polberger S, Hellstrom-Westas L 2003 Tolerance to early human milk feeding is not compromised by indomethacin in preterm infants with persistent ductus arteriosus. Acta Paediatr 92: 1074–1078
Duan RD, Nilsson A 2000 Sphingolipid hydrolyzing enzymes in the gastrointestinal tract. Methods Enzymol 311: 276–286
Lundgren P, Nilsson A, Duan RD 2001 Distribution and properties of neutral ceramidase activity in rat intestinal tract. Dig Dis Sci 46: 765–772
Wu J, Cheng Y, Jonsson BA, Nilsson A, Duan RD 2005 Acid sphingomyelinase is induced by butyrate but does not initiate the anticancer effect of butyrate in HT29 and HepG2 cells. J Lipid Res 46: 1944–1952
Malmsten M, Bergenstahl B, Nyberg L, Oldham G 1994 Sphingomyelin from milk—characterization of crystalline, liposome and emulsion properties. J Am Oil Chem Soc 71: 1021–1026
Bouhours JF, Guignard H 1979 Free ceramide, sphingomyelin, and glucosylceramide of isolated rat intestinal cells. J Lipid Res 20: 879–907
Duan RD, Nyberg L, Nilsson A 1995 Alkaline sphingomyelinase activity in rat gastrointestinal tract: distribution and characteristics. Biochim Biophys Acta 1259: 49–55
Nyberg L, Farooqi A, Blackberg L, Duan RD, Nilsson A, Hernell O 1998 Digestion of ceramide by human milk bile salt-stimulated lipase. J Pediatr Gastroenterol Nutr 27: 560–567
Kirby RJ, Zheng S, Tso P, Howles PN, Hui DY 2002 Bile salt-stimulated carboxyl ester lipase influences lipoprotein assembly and secretion in intestine: a process mediated via ceramide hydrolysis. J Biol Chem 277: 4104–4109
McGuire W, Anthony MY 2003 Donor human milk versus formula for preventing necrotising enterocolitis in preterm infants: systematic review. Arch Dis Child Fetal Neonatal Ed 88: F11–F14
Carlson SE, Montalto MB, Ponder DL, Werkman SH, Korones SB 1998 Lower incidence of necrotizing enterocolitis in infants fed a preterm formula with egg phospholipids. Pediatr Res 44: 491–498
Karlsson KA, Larson G 1978 Molecular characterization of cell-surface antigens of human fetal tissue: meconium, a rich source of epithelial blood-group glycolipids. FEBS Lett 87: 283–287
Larson G, Watsfeldt P, Falk P, Leffler H, Koprowski H 1987 Fecal excretion of intestinal glycosphingolipids by newborns and young children. FEBS Lett 214: 41–44
Taki T, Rokukawa C, Kasama T, Kon K, Ando S, Abe T, Handa S 1992 Human meconium gangliosides. Characterization of a novel I-type ganglioside with the NeuAc alpha 2-6Gal structure. J Biol Chem 267: 11811–11817
Holopainen R, Aho H, Laine J, Peuravuori H, Soukka H, Kaapa P 1999 Human meconium has high phospholipase A2 activity and induces cellular injury and apoptosis in piglet lungs. Pediatr Res 46: 626–632
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was supported by the Swedish Research Council (grants 03969 to Å.N. and 0037 to L.H.W.), the Swedish Cancer Society (grant 4845 to R.-D.D.), and the Albert Påhlssons Foundation, Research Funds of the Lund University Hospital.
Rights and permissions
About this article
Cite this article
Duan, RD., Cheng, Y., Jönsson, B. et al. Human Meconium Contains Significant Amounts of Alkaline Sphingomyelinase, Neutral Ceramidase, and Sphingolipid Metabolites. Pediatr Res 61, 61–66 (2007). https://doi.org/10.1203/01.pdr.0000250534.92934.c2
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/01.pdr.0000250534.92934.c2