Abstract
In hyperprostaglandin E syndrome (HPGES) and classic Bartter syndrome (cBS), tubular salt and water losses stimulate renin secretion, which is dependent on enhanced cyclooxygenase-2 (COX-2) enzymatic activity. In contrast to other renal COX metabolites, only prostaglandin E2 (PGE2) is selectively up-regulated in these patients. To determine the intrarenal source of PGE2 synthesis, we analyzed the expression of microsomal PGE2 synthase (mPGES; EC: 5.3.99.3), whose product PGE2 has been shown to stimulate renin secretion in vitro. Expression of mPGES was analyzed by immunohistochemistry in eight patients with HPGES, in two patients with cBS, and in six control subjects. Expression of mPGES immunoreactive protein was observed in cells of the macula densa in five of eight HPGES patients and in one of two cBS patients. Expression of mPGES immunoreactive protein was not observed in cells associated with the macula densa in kidneys from control subjects without a history consistent with activation of the renin angiotensin system. Co-induction of COX-2 and mPGES in cells of the macula densa suggests that PGE2 activates renin secretion in humans.
Similar content being viewed by others
Main
Hyperprostaglandin E syndrome (HPGES) or antenatal Bartter syndrome with and without sensorineural hearing loss and classic Bartter syndrome (cBS) belong to the heterogeneous group of hypokalemic salt-losing tubulopathies (SLTs) (1). The term hyperprostaglandin E syndrome was introduced to emphasize the critical role of prostaglandin E2 (PGE2) in both pathogenesis and treatment of these congenital tubulopathies (2). Patients who have HPGES show massive salt and water losses closely resembling chronic furosemide treatment (3, 4). At the molecular level, loss of function mutations have been identified in genes essential for salt reabsorption in the thick ascending limb of Henle's loop (TAL): two gene products, namely NKCC2 (5, 6) and ROMK (7, 8), are expressed in the luminal membrane of the TAL. NKCC2 is the furosemide-sensitive sodium-potassium-chloride co-transporter, which is dependent on the recycling of potassium into the luminal compartment mediated by ROMK potassium channel. A third gene product shown to be mutated in cBS, namely ClCKb (9, 10), allows basolateral exit of chloride into the interstitium. Finally, loss of function mutations in the gene encoding Barttin, a β-subunit of CLCKa and CLCKb, have recently been shown to cause HPGES associated with sensorineural deafness (11–13).
Similar to normal subjects who are treated with furosemide (3, 4), patients with HPGES show increased urinary excretion of PGE2(2). Inhibition of PGE2 synthesis by nonsteroidal anti-inflammatory drugs such as indomethacin effectively reduce salt and water losses in these patients and is therefore standard treatment (2).
PG synthesis is initiated by the bifunctional enzyme cyclooxygenase (COX) (14). Two COX isoforms are known: COX-1, which is expressed constitutively in almost all organs, and COX-2, which can be induced by various stimuli (15). In contrast to healthy control subjects (16), patients with HPGES or cBS show enhanced expression of the inducible COX-2 in the macula densa (17). The macula densa is a specialized segment of the TAL and is thought to sense the luminal salt concentration (18). In salt-depleted animals, COX-2-derived products have been shown to mediate the compensatory activation of renin secretion, which ultimately results in salt and water retention (19). Our finding of enhanced expression of COX-2 in the macula densa in patients with hypokalemic SLT and studies in salt-depleted animals provided the rationale for switching patients with hypokalemic SLT from their standard medication with the COX-unselective nonsteroidal anti-inflammatory drug indomethacin to the COX-2 selective inhibitor rofecoxib. Rofecoxib turned out be as effective as the unselective inhibitor indomethacin in ameliorating renal disturbances as well as in suppressing the activated renin-angiotensin system (RAS), proving that renin secretion is accompanied by and dependent on enhanced COX-2 enzymatic activity (20).
In contrast to ample evidence showing that COX-2 activity stimulates renin secretion, little information exists on the nature of prostanoids synthesized in the macula densa by COX-2 and stimulating secretion of renin from the juxtaglomerular cells. Because the intrarenal synthesis of PGE2 is selectively up-regulated in this group of congenital SLTs and PGE2 has been shown to stimulate renin secretion in vitro(21), we determined the intracellular source of PGE2 synthesis in these patients. Various pathways result in PGE2 generation: the immediate product of COX activity PGH2 is rapidly converted nonenzymatically into PGE2 and PGD2(14). Alternatively, selective formation of PGE2 is ensured by two enzymes namely a cytosolic PGE synthase (22) and a microsomal PGE synthase (mPGES; EC: 5.3.99.3) (23), which both have recently been cloned. Whereas the cytosolic PGE synthase is thought to couple preferentially to COX-1, the mPGES and prostacyclin synthase are functionally dependent on COX-2 in vitro(22, 24). In adult mouse kidney, mPGES is expressed in collecting ducts (25). In human kidney, Northern blot analysis shows moderate expression of mPGES (23); however, a detailed analysis of the intrarenal distribution of human mPGES has not been performed yet. To analyze further the signaling pathway from the macula densa COX-2 to renin secretion, we mapped the intrarenal distribution of mPGES in control and hypokalemic SLT subjects.
METHODS
Patients.
Renal biopsies were performed in 1997 and 1998 during an indomethacin-free interval in children with genetically and clinically defined HPGES or cBS to evaluate the renal side effects of long-term indomethacin treatment. Written informed parental consent and oral assessment of the children were obtained before enrollment (26). The genetic analysis of the patients has been described elsewhere (6, 8, 9, 27); the patient characteristics are shown in Table 1.
Biochemical analysis.
For evaluating a possible relationship between renal PGE2 synthesis and plasma renin levels, long-term indomethacin treatment was discontinued 3 d before renal biopsy, as described previously (20). Blood samples and cooled 24-h urine collections were obtained before and 3 d after withdrawal of indomethacin. Radioimmunologic standard assays were used for analysis of plasma renin concentration. Renal prostanoid levels were determined by gas chromatography/tandem-mass spectrometry using a stable isotope dilution assay, as described elsewhere (28). Reference intervals for the excretion of PGs were previously described (29).
Histochemical analysis.
Renal biopsies from patients with congenital SLTs were routinely fixed in formalin. In addition, we analyzed renal tissue (n = 6) from kidneys deemed unsuitable for kidney transplantation. Kidney were excluded from transplantation because of vascular problems. Donor age ranged between 39 to 58 y. Medical history did not indicate conditions associated with salt or volume depletion in five cases. One patient had congestive heart failure and required multiple drugs, including furosemide, and an aortic balloon pump for pressure support before death. Approval by the local ethics committee was obtained (17).
Specificity of the antibodies.
The specificity of the polyclonal anti–COX-2 antibodies using routinely formalin-fixed human tissue has been shown in our previous studies (17). To characterize the polyclonal anti-mPGES antibodies (Cayman Chemical Company, Ann Arbor, MI, U.S.A.), we performed various control experiments. Specificity of the anti-mPGES antibodies was analyzed by Western blotting as described previously (25). Briefly, human embryonic kidney cells (HEK293) were transiently transfected with an expression vector encoding murine microsomal PGES (pCDNA3.1hmPGES) (25). Two micrograms of each cell lysate (mock and pCDNA3.1hmPGES transfected cells) and 10 μg of a human lung cancer cell line A549 known to abundantly express mPGES (23) were separated on a 10% SDS-PAGE minigel. After transfer to a nitrocellulose membrane, the membrane was washed three times with TBST [50 mM of Tris (pH 7.5), 150 mm of NaCl, and 0.05% Tween 20] and then incubated in blocking buffer (TBST and 5% Carnation nonfat dry milk) for 1 h at room temperature. The membrane was then incubated with the polyclonal anti-murine mPGES antibodies diluted 1:2000 in blocking buffer overnight at 4°C. After three washings in TBST, the membrane was incubated with a horseradish peroxidase-conjugated anti-rabbit secondary antibody (diluted 1:20,000 in TBST with 0.5% BSA; Jackson Immuno-Research Laboratories, West Grove, PA, U.S.A.) for 1 h at room temperature, followed by three 30-min washings. Antibody labeling was visualized by addition of chemiluminescence reagent (Renaissance; DuPont NEN, Boston, MA, U.S.A.), and the membrane was exposed to Kodak XAR-5 film.
Immunohistochemistry.
Sections obtained from routinely formalin-fixed tissue specimen were cut at 2- to 5-μm thickness, deparaffinized in xylene, and incubated for 30 min in methanol containing 0.3% H2O2 to block endogenous peroxidase activity. Processing of paraformaldehyde-fixed adult mouse kidney sections with the mPGES antibodies resulted in specific labeling of collecting ducts, as shown in our previous study (25) (data not shown). Preincubation of the mPGE antibodies with the peptide used as immunogen at a concentration of 2 μg/mL for 1 h at room temperature completely blocked staining on mouse and human renal tissue (data not shown). Anti–COX-2 antibodies were obtained from Santa Cruz (Santa Cruz, CA, U.S.A.; goat polyclonal anti-human cox-2: c-20, sc#1745, lot #J151). Antibodies required antigen retrieval by microwaving slides for 3 min in PBS containing 0.1 M of sodium citrate (pH 6.0). Polyclonal anti-mPGES and anti–COX-2 were diluted 1:200 and 1:1000, respectively, in TBST [50 mM of Tris (pH 7.5), 300 mM of NaCl, and 0.05% Tween 20] containing 1% BSA, 5% normal horse serum, and 1% nonfat dry milk. Sections were incubated at room temperature overnight. Immunolabeling was detected using biotinylated rabbit anti-goat or donkey anti-rabbit antibodies followed by visualization with an avidin-biotin horseradish peroxidase labeling kit (Vectastain ABC Elite kit) and diaminobenzidine staining. To co-localize both COX-2 and mPGES, we attempted to visualize primary antibodies with immunofluorescent secondary antibodies. However, they failed because of the low sensitivity of this approach compared with the enzymatic procedure described above. Pictures were captured with a digital camera (RT-Spot-Cam; Diagnostic Instruments, Visitron-System, Munich, Germany), and color composites were generated by using Adobe Photoshop v6.0 on a Power Macintosh.
Statistical analysis.
To analyze the correlation between the percentage of indomethacin-induced inhibition of renal PGE2 synthesis with the degree of inhibition of plasma renin activity by indomethacin as shown in Figure 1, we used the Spearman correlation coefficient for nonparametric variables (SSPS for Windows, v. 11.0).
RESULTS
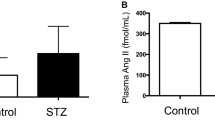
The urinary excretion of PGE2 (patients: median, 29 ng · h−1 · 1.73m−2, range, 22–169 ng· h−1 · 1.73m−2; normal: range, 4–27 ng· h−1 · 1.73m−2) and its major metabolite PGE-M (patients: median, 963 ng· h−1 · 1.73m−2, range, 536–4610 ng· h−1 · 1.73m−2; normal: range, 62–482 ng· h−1 · 1.73m−2) was elevated during the indomethacin-free interval immediately before the biopsy. This elevation of PGE excretion was paralleled by a rise in plasma renin levels (patients: median, 338 SU/mL, range, 148–1424 SU/mL; normal: range, 5–50 SU/mL). Statistical analysis indicates that the extent of indomethacin-induced inhibition of both intrarenal PGE2 levels and plasma renin levels are significantly correlated (r = 0.8;Fig. 1).
The prostacyclin metabolites 6-keto-PGF1α (median, 10 ng· h−1 · 1.73m−2, range, 3–25 ng· h−1 · 1.73m−2; normal: range, 2–12 ng· h−1 · 1.73m−2) and 2,3-dinor-6-keto-PGF1α (median, 6 ng· h−1 · 1.73m−2, range, 1–14 ng· h−1 · 1.73m−2) remained within the normal range. Similarly, no changes were observed in the renal synthesis of thromboxane and PGF2α between control subjects (29) and patients affected by either HPES or cBS, respectively.
The specificity of the polyclonal anti-mPGES antibodies was initially analyzed by immunoblotting. No signal was seen in mock-transfected HEK293 cells. Specific labeling of a product migrating at 16 kD consistent with the calculated molecular weight for microsomal PGES was seen in lysates from HEK293 cells transiently transfected with a murine mPGES expression vector. This band co-migrated with a product synthesized constitutively in a human lung cancer cell line A549 consistent with the original identification of mPGES by Jakobsson et al.(23). These result demonstrate that the mPGES antibodies used in this study selectively react with both the murine and the human mPGES protein (data not shown).
Immunohistochemistry using mPGES selective antibodies was performed on renal tissue deemed unsuitable for transplantation. In one patient with congestive heart failure, mPGES ir-protein was observed in cells of the macula densa (Fig. 2A). Five to 15% of maculae densa in one section showed labeling. Typically, mPGES ir-protein was restricted to 5–10 cells. Serial sections processed with anti-PGES (Fig. 2A) and COX-2 antibodies (Fig. 2B) showed co-localization of the proteins within distinct cells of the macula densa.
Expression of mPGES immunoreactive protein. Serial sections of renal cortex from a patient with congestive heart failure were processed with anti–COX-2 (top) and anti-mPGES antibodies (bottom). COX-2 immunoreactive protein is expressed in the cells of the macula densa but not in the surrounding cells of the TAL. Serial sections reveal that expression of COX-2 immunoreactive protein co-localizes with expression of mPGES immunoreactive protein. G, glomerulus; A, arteriole; MD, macula densa.
In patients with HPGES or cBS, mPGES immunoreactivity in the macula densa was observed in five of eight or one of two biopsies, respectively. In contrast to the control tissue, cells of the macula densa seemed to contain less cytoplasm. The underlying mutations in these patients are given in Table 1. Figure 3A shows expression of mPGES in a patient with a genetic defect in the gene encoding RomK;Figure 3B and C, demonstrate mPGES in a patient with a genetic defect in the gene encoding the furosemide-sensitive NaK2Cl transporter NKCC2 and the kidney chloride channel ClCkB, respectively. Typically, mPGES expression was not very abundant. Hyperplasia of the juxtaglomerular apparatus was also seen (Fig. 3A and C, arrows). MPGES immunoreactivity was absent in renal tissue from patients without evidence of an activation of the RAS (data not shown). In contrast to adult mouse kidney, mPGES expression was not observed in collecting ducts.
Expression of mPGES in patients with HPGES and cBS. Expression of mPGES immunoreactive protein was also observed in a HPGES patient with a genetic defect in the gene encoding ROMK (A), in a patient with a genetic defect in the gene encoding the furosemide-sensitive NaK2Cl transporter (B), and in a patient with a genetic defect in the ClCKb gene (C). Hyperplasia of the juxtaglomerular apparatus is seen in Fig. 3A and C (arrows).
DISCUSSION
Recent studies in humans and rodents have established a key role of macula densa COX-2 in stimulating renin secretion (19). The prostanoids acting downstream of COX-2 have not been identified yet. Enhanced renal PGE2 synthesis in congenital hypokalemic SLTs and in furosemide-treated subjects as shown by us and others indicates that this prostanoid may result from macula densa COX-2 activity (3, 4, 30). In this study, we confirm that renal PGE2 synthesis is selectively up-regulated in patients with HPGES and cBS. Furthermore, the extent of indomethacin-induced inhibition of both intrarenal PGE2 levels and plasma renin levels is significantly, albeit weakly, correlated (R = 0.80, p < 0.01). The correlation may be flawed by the relatively low number of patients in this study. In addition, whereas plasma renin levels reflect a given time point, PGE2 levels result from a collection period of 24 h in this study. Collectively, the correlation is compatible with the notion that PGE2 may stimulate renin secretion in humans.
The key new finding of this study is that mPGES is expressed in the macula densa in subjects with HPGES or cBS. Expression of mPGES immunoreactivity was not detected in subjects without evidence of activation of the RAS. This pattern of gene expression parallels the expression of COX-2 in the macula densa. Indeed, using serial sections, we could show that mPGES and COX-2 co-localize in specific cells of the macula densa. Two recent studies have also demonstrated co-expression of mPGES and COX-2 in the macula densa in mice, rabbits, and rats (31, 32). This may suggest that both genes are regulated in a similar way in the macula densa. In contrast to COX-2, however, little information exists regarding the regulation of mPGES gene expression. Both genes can be induced by inflammatory cytokines, and both are suppressed by glucocorticoids (15, 33). Whether mPGES gene expression in TAL cells is also induced by the protein kinase p38 upon depletion of extracellular chloride as shown for COX-2 in rabbit TAL cells in vitro remains to be shown (34).
Similar to the expression of COX-2 in renal biopsies from patients with HPES or cBS (17), nPGES expression was not observed in all biopsies examined. Harris et al.(35) showed that in salt-depleted rats, only 20% of all maculae densa showed expression of COX-2 in this nephron segment. We speculate that absence of mPGES expression in four of nine biopsies may reflect the paucity of glomeruli in renal biopsies rather than complete absence of mPGES expression in these patients.
Co-expression of COX-2 and mPGES in the macula densa may suggest that PGE2 is the major metabolite synthesized in the macula densa and, more important, that this prostanoid may stimulate renin secretion. Co-expression of the two enzymes also ensures preferential formation of PGE2 from PGH2, which is observed in patients with HPGES and cBS (2). Because renin secretion is stimulated by agents that increase the intracellular cAMP levels, including PGE2(21), candidate PGE2 receptors are EP2 and EP4, which both activate adenylate cyclase (36). The latter has been shown to be expressed intraglomerularly by in situ hybridization (36). To directly address involvement of these EP receptors, studies in knockout mice and/or studies with specific inhibitors of EP receptors (37) will be necessary.
In adult mouse kidney, mPGES mRNA and immunoreactive protein are expressed in collecting ducts as shown previously by Guan et al.(25). This finding was confirmed in mouse tissue in the present study (data not shown) and has recently also been demonstrated for adult rat kidney (38). No labeling was detected in the present study in human collecting ducts in the kidneys deemed unsuitable for transplantation.
The specificity of our mPGES labeling procedure is strongly suggested by the following observations: in addition to the complete overlap of mPGES and COX-2 immunoreactive protein in cells of the human macula densa (Fig. 2A and B), two other experiments demonstrate the specificity of the mPGES antibodies. First, the mPGES antibodies specifically recognize both murine and human mPGES in Western blot experiments (data not shown). Second, preincubation of the mPGES antibodies with the peptide used as the immunogen completely blocked immunohistochemical staining (data not shown).
CONCLUSION
In summary, we have shown that mPGES is expressed in the macula densa in patients with HPGES or cBS and in a patient with congestive heart failure. This finding is compatible with the notion that PGE2 generated by the concerted action of COX-2 and mPGES activity stimulates renin secretion in these subjects. As specific inhibitors of prostanoid receptors are currently successfully tested in animals and may be available for patients in the future, our speculation may be confirmed. Further studies are needed to dissect the signaling pathway leading to the induction of mPGES expression as well as the events downstream from PGE2 generation.
Abbreviations
- cBS:
-
classic Bartter syndrome
- COX:
-
cyclooxygenase
- HPGES:
-
hyperprostaglandin e syndrome
- mPGES:
-
microsomal prostaglandin E2 synthase
- PG:
-
prostaglandin
- RAS:
-
renin-angiotensin system
- SLT:
-
salt-losing tubulopathy
- TAL:
-
thick ascending limb of Henle's loop
References
Peters M, Jeck N, Reinalter S, Leonhardt A, Tonshoff B, Klaus GG, Konrad M, Seyberth HW 2002 Clinical presentation of genetically defined patients with hypokalemic salt-losing tubulopathies. Am J Med 112: 183–190
Seyberth HW, Rascher W, Schweer H, Kühl PG, Mehls O, Schärer K 1985 Congenital hypokalemia with hypercalciuria in preterm infants: a hyperprostaglandinuric tubular syndrome different from Bartter syndrome. J Pediatr 107: 694–701
Ciabattoni G, Pugliese F, Cinotti GA, Stirati G, Ronci R, Castrucci G, Pierucci A, Patrono C 1979 Characterization of furosemide-induced activation of the renal prostaglandin system. Eur J Pharmacol 60: 181–187
Stichtenoth DO, Wagner B, Frolich JC 1998 Effect of selective inhibition of the inducible cyclooxygenase on renin release in healthy volunteers. J Investig Med 46: 290–296
Simon DB, Karet FE, Hamdan JM, DiPietro A, Sanjad SA, Lifton RP 1996 Bartter's syndrome, hypokalaemic alkalosis with hypercalciuria, is caused by mutations in the Na-K-2Cl cotransporter NKCC2. Nat Genet 13: 183–188
Vargas-Poussou R, Feldmann D, Vollmer M, Konrad M, Kelly L, van den Heuvel LP, Tebourbi L, Brandis M, Karolyi L, Hebert SC, Lemmink HH, Deschenes G, Hildebrandt F, Seyberth HW, Guay-Woodford LM, Knoers NV, Antignac C 1998 Novel molecular variants of the Na-K-2Cl cotransporter gene are responsible for antenatal Bartter syndrome. Am J Hum Genet 62: 1332–1340
Simon DB, Karet FE, Rodriguez-Soriano J, Hamdan JH, DiPietro A, Trachtman H, Sanjad SA, Lifton RP 1996 Genetic heterogeneity of Bartter's syndrome revealed by mutations in the K+ channel, ROMK. Nat Genet 14: 152–156
Karolyi L, Konrad M, Köckerling A, Ziegler A, Zimmermann DK, Roth B, Wieg C, Grzeschik KH, Koch MC, Seyberth HW, Vargas R, Forestier L, Jean G, Deschaux M, Rizzoni GF, Niaudet P, Antignac C, Feldmann D, Lorridon F, Cougoureux E, Laroze F, Alessandri JL, David L, Saunier P, Deschenes G, Hildebrandt F, Vollmer M, Proesmans W, Brandis M, Vandenheuvel LPJ, Lemmink HH, Nillesen W, Monnens LAH, Knoers N, Guaywoodford LM, Wright CJ, Madrigal G, Hebert SC 1997 Mutations in the gene encoding the inwardly-rectifying renal potassium channel, ROMK, cause the antenatal variant of Bartter syndrome: evidence for genetic heterogeneity. Hum Mol Genet 6: 17–26
Konrad M, Vollmer M, Lemmink HH, van den Heuvel LP, Jeck N, Vargas-Poussou R, Lakings A, Ruf R, Deschenes G, Antignac C, Guay-Woodford L, Knoers NV, Seyberth HW, Feldmann D, Hildebrandt F 2000 Mutations in the chloride channel gene CLCNKB as a cause of classic Bartter syndrome. J Am Soc Nephrol 11: 1449–1459
Simon DB, Bindra RS, Mansfield TA, Nelson-Williams C, Mendonca E, Stone R, Schurman S, Nayir A, Alpay H, Bakkaloglu A, Rodriguez-Soriano J, Morales JM, Sanjad SA, Taylor CM, Pilz D, Brem A, Trachtman H, Griswold W, Richard GA, John E, Lifton RP 1997 Mutations in the chloride channel gene, CLCNKB, cause Bartter's syndrome type III. Nat Genet 17: 171–178
Waldegger S, Jeck N, Barth P, Peters M, Vitzthum H, Wolf K, Kurtz A, Konrad M, Seyberth HW 2002 Barttin increases surface expression and changes current properties of ClC-K channels. Pflugers Arch 444: 411–418
Birkenhager R, Otto E, Schurmann MJ, Vollmer M, Ruf EM, Maier-Lutz I, Beekmann F, Fekete A, Omran H, Feldmann D, Milford DV, Jeck N, Konrad M, Landau D, Knoers NV, Antignac C, Sudbrak R, Kispert A, Hildebrandt F 2001 Mutation of BSND causes Bartter syndrome with sensorineural deafness and kidney failure. Nat Genet 29: 310–314
Estevez R, Boettger T, Stein V, Birkenhager R, Otto E, Hildebrandt F, Jentsch TJ 2001 Barttin is a Cl- channel beta-subunit crucial for renal Cl- reabsorption and inner ear K+ secretion. Nature 414: 558–561
Smith W 1992 Prostanoid biosynthesis and mechanism of action. Am J Physiol 263: F181–F191
Herschman HR 1996 Prostaglandin synthase 2. Biochim Biophys Acta 1299: 125–140
Komhoff M, Grone HJ, Klein T, Seyberth HW, Nusing RM 1997 Localization of cyclooxygenase-1 and -2 in adult and fetal human kidney: implication for renal function. Am J Physiol 272: F460–F468
Komhoff M, Jeck ND, Seyberth HW, Grone HJ, Nusing RM, Breyer MD 2000 Cyclooxygenase-2 expression is associated with the renal macula densa of patients with Bartter-like syndrome. Kidney Int 58: 2420–2424
Schlatter E, Salomonsson M, Persson AE, Greger R 1989 Macula densa cells sense luminal NaCl concentration via furosemide sensitive Na+2Cl-K+ cotransport. Pflugers Arch 414: 286–290
Breyer MD, Harris RC 2001 Cyclooxygenase 2 and the kidney. Curr Opin Nephrol Hypertens 10: 89–98
Reinalter S, Jeck N, Brochhausen C, Watzer B, Nüsing RM, Seyberth HW, Kömhoff M 2002 Role of cyclooxygenase-2 in hyperprostaglandin E syndrome/antenatal Bartter syndrome (HPS/aBS). Kidney Int 62: 253–260
Jensen BL, Schmid C, Kurtz A 1996 Prostaglandins stimulate renin secretion and renin mRNA in mouse renal juxtaglomerular cells. Am J Physiol 271: F659–F669
Tanioka T, Nakatani Y, Semmyo N, Murakami M, Kudo I 2000 Molecular identification of cytosolic prostaglandin E2 synthase that is functionally coupled with cyclooxygenase-1 in immediate prostaglandin E2 biosynthesis. J Biol Chem 275: 32775–32782
Jakobsson PJ, Thoren S, Morgenstern R, Samuelsson B 1999 Identification of human prostaglandin E synthase: a microsomal, glutathione-dependent, inducible enzyme, constituting a potential novel drug target. Proc Natl Acad Sci U S A 96: 7220–7225
Ueno N, Murakami M, Tanioka T, Fujimori K, Tanabe T, Urade Y, Kudo I 2001 Coupling between cyclooxygenase, terminal prostanoid synthase, and phospholipase A2. J Biol Chem 276: 34918–34927
Guan Y, Zhang Y, Schneider A, Riendeau D, Mancini JA, Davis L, Komhoff M, Breyer RM, Breyer MD 2001 Urogenital distribution of a mouse membrane-associated prostaglandin E(2) synthase. Am J Physiol 281: F1173–F1177
Reinalter SC, Grone HJ, Konrad M, Seyberth HW, Klaus G 2001 Evaluation of long-term treatment with indomethacin in hereditary hypokalemic salt-losing tubulopathies. J Pediatr 139: 398–406
Jeck N, Derst C, Wischmeyer E, Ott H, Weber S, Rudin C, Seyberth HW, Daut J, Karschin A, Konrad M 2001 Functional heterogeneity of ROMK mutations linked to hyperprostaglandin E syndrome. Kidney Int 59: 1803–1811
Schweer H, Watzer B, Seyberth HW 1994 Determination of seven prostanoids in 1 ml of urine by gas chromatography-negative ion chemical ionization triple stage quadruple mass spectrometry. J Chromatogr 652: 221–227
Leonhardt A, Busch C, Schweer H, Seyberth HW 1992 Reference intervals and developmental changes in urinary prostanoid excretion in healthy newborns, infants and children. Acta Paediatr 81: 191–196
Kockerling A, Reinalter SC, Seyberth HW 1996 Impaired response to furosemide in hyperprostaglandin E syndrome: evidence for a tubular defect in the loop of Henle. J Pediatr 129: 519–528
Campean V, Theilig F, Paliege A, Breyer M, Bachman S 2003 Key enzymes for renal prostaglandin synthesis—site-specific expression in rodent kidney (rat, mouse). Am J Physiol 285: F19–F32
Fuson AL, Komlosi P, Unlap TM, Bell PD, Peti-Peterdi J 2003 Immunolocalization of a microsomal prostaglandin R synthase in rabbit kidney. Am J Physiol 285: F558–F564
Stichtenoth DO, Thoren S, Bian H, Peters-Golden M, Jakobsson PJ, Crofford LJ 2001 Microsomal prostaglandin E synthase is regulated by proinflammatory cytokines and glucocorticoids in primary rheumatoid synovial cells. J Immunol 167: 469–474
Cheng HF, Wang JL, Zhang MZ, McKanna JA, Harris RC 2000 Role of p38 in the regulation of renal cortical cyclooxygenase-2 expression by extracellular chloride. J Clin Invest 106: 681–688
Harris RC, McKanna JA, Akai Y, Jacobson HR, Dubois RN, Breyer MD 1994 Cyclooxygenase-2 is associated with the macula densa of rat kidney and increases with salt restriction. J Clin Invest 94: 2504–2510
Breyer MD, Breyer RM 2000 Prostaglandin E receptors and the kidney. Am J Physiol 279: F12–F23
Narumiya S, Sugimoto Y, Ushikubi F 1999 Prostanoid receptors: structures, properties, and functions. Physiol Rev 79: 1193–1226
Vitzthum H, Abt I, Einhellig S, Kurtz A 2002 Gene expression of prostanoid forming enzymes along the rat nephron. Kidney Int 62: 1570–1581
Acknowledgements
We thank Matthew D. Breyer for providing pCDNA3.1mPGES expression vector and control tissue and Claudia Schmidt for excellent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by Stiftung P. E. Kempkes, Marburg (19-2000 & 26-2001) and Deutsche Forschungsgemeinschaft (KO 1855/2-1) to M.K.
Rights and permissions
About this article
Cite this article
Kömhoff, M., Reinalter, S., Gröne, H. et al. Induction of Microsomal Prostaglandin E2 Synthase in the Macula Densa in Children with Hypokalemic Salt-Losing Tubulopathies. Pediatr Res 55, 261–266 (2004). https://doi.org/10.1203/01.PDR.0000101747.09626.6B
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/01.PDR.0000101747.09626.6B
This article is cited by
-
Disease modeling in genetic kidney diseases: mice
Cell and Tissue Research (2017)
-
Hereditäre hypokaliämische Salzverlusttubulopathien
Der Nephrologe (2017)
-
Ionenkanalerkrankungen der Niere und Nebenniere
Medizinische Genetik (2013)
-
Microsomal prostaglandin E synthase-1 and blood pressure regulation
Kidney International (2007)